Abstract
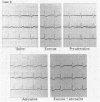
The clinical and haemodynamic effects of adrenaline infusion (30 ng kg-1 min-1) producing plasma adrenaline concentrations in the range seen during acute myocardial infarction and of placebo were investigated in a crossover design in 14 patients with stable coronary heart disease. Adrenaline infusion resulted in electrocardiographic evidence of myocardial ischaemia (greater than or equal to 1 mm (0.1 mV) horizontal or downsloping ST segment depression) in 10 patients and angina in four, although the mean (SEM) increase in heart rate was modest (14 (2) beats/min) and mean coronary vascular resistance fell from 1.56 (0.21) to 1.16 (0.14) mm Hg min ml-1 (p less than 0.005). New or increasingly frequent or complex ventricular arrhythmias occurred in five patients. Placebo infusion had no effect on the variables measured. Supine bicycle exercise during infusion of the saline placebo was associated with a similar degree of ST segment depression (0.9 (0.2) mm) as adrenaline infusion at rest (0.9 (0.1) mm) but exercise performed during adrenaline infusion (10 patients) resulted in more pronounced ST segment depression (1.9 (0.3) mm) (p less than 0.005) than either intervention alone. Angina occurred in three of 11 patients during control exercise and in six of 10 during the combination of adrenaline infusion and exercise. Such potentially adverse consequences of low dose adrenaline infusion in patients with stable coronary heart disease are consistent with the suggestion that adrenal activation is detrimental during acute myocardial infarction, being both arrhythmogenic and proischaemic.
Full text
PDF



Images in this article
Selected References
These references are in PubMed. This may not be the complete list of references from this article.
- Arisaka H., Ikeda U., Takayasu T., Takeda K., Natsume T., Hosoda S. Ouabain inhibits intracellular pH recovery from acidosis in cultured mouse heart cells. J Mol Cell Cardiol. 1988 Jan;20(1):1–3. doi: 10.1016/s0022-2828(88)80173-1. [DOI] [PubMed] [Google Scholar]
- Armbrecht J. J., Buxton D. B., Brunken R. C., Phelps M. E., Schelbert H. R. Regional myocardial oxygen consumption determined noninvasively in humans with [1-11C]acetate and dynamic positron tomography. Circulation. 1989 Oct;80(4):863–872. doi: 10.1161/01.cir.80.4.863. [DOI] [PubMed] [Google Scholar]
- Benedict C. R., Grahame-Smith D. G. Plasma adrenaline and noradrenaline concentrations and dopamine-beta-hydroxylase activity in myocardial infarction with and without cardiogenic shock. Br Heart J. 1979 Aug;42(2):214–220. doi: 10.1136/hrt.42.2.214. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Camici P., Marraccini P., Marzilli M., Lorenzoni R., Buzzigoli G., Puntoni R., Boni C., Bellina C. R., Klassen G. A., L'Abbate A. Coronary hemodynamics and myocardial metabolism during and after pacing stress in normal humans. Am J Physiol. 1989 Sep;257(3 Pt 1):E309–E317. doi: 10.1152/ajpendo.1989.257.3.E309. [DOI] [PubMed] [Google Scholar]
- Corr P. B., Witkowski F. X., Sobel B. E. Mechanisms contributing to malignant dysrhythmias induced by ischemia in the cat. J Clin Invest. 1978 Jan;61(1):109–119. doi: 10.1172/JCI108908. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cryer P. E. Physiology and pathophysiology of the human sympathoadrenal neuroendocrine system. N Engl J Med. 1980 Aug 21;303(8):436–444. doi: 10.1056/NEJM198008213030806. [DOI] [PubMed] [Google Scholar]
- Feigl E. O. The paradox of adrenergic coronary vasoconstriction. Circulation. 1987 Oct;76(4):737–745. doi: 10.1161/01.cir.76.4.737. [DOI] [PubMed] [Google Scholar]
- Fellows I. W., MacDonald I. A., Bennett T., O'Donoghue D. P. Effect of intravenous infusion of adrenaline on the cardiovascular responses to distal body subatmospheric pressure in man. Clin Sci (Lond) 1988 Oct;75(4):389–394. doi: 10.1042/cs0750389. [DOI] [PubMed] [Google Scholar]
- Freyschuss U., Hjemdahl P., Juhlin-Dannfelt A., Linde B. Cardiovascular and metabolic responses to low dose adrenaline infusion: an invasive study in humans. Clin Sci (Lond) 1986 Feb;70(2):199–206. doi: 10.1042/cs0700199. [DOI] [PubMed] [Google Scholar]
- Halter J. B., Stratton J. R., Pfeifer M. A. Plasma catecholamines and hemodynamic responses to stress states in man. Acta Physiol Scand Suppl. 1984;527:31–38. [PubMed] [Google Scholar]
- Herbaczyńska-Cedro K. The influence of adrenaline secretion on the enzymes in heart muscle after acute coronary occlusion in dogs. Cardiovasc Res. 1970 Apr;4(2):168–175. doi: 10.1093/cvr/4.2.168. [DOI] [PubMed] [Google Scholar]
- Karlsberg R. P., Cryer P. E., Roberts R. Serial plasma catecholamine response early in the course of clinical acute myocardial infarction: relationship to infarct extent and mortality. Am Heart J. 1981 Jul;102(1):24–29. doi: 10.1016/0002-8703(81)90408-7. [DOI] [PubMed] [Google Scholar]
- McAlpine H. M., Morton J. J., Leckie B., Rumley A., Gillen G., Dargie H. J. Neuroendocrine activation after acute myocardial infarction. Br Heart J. 1988 Aug;60(2):117–124. doi: 10.1136/hrt.60.2.117. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McCance A. J., Forfar J. C. Cardiac and whole body [3H]noradrenaline kinetics in ischaemic heart disease: contrast between unstable anginal syndromes and pacing induced ischaemia. Br Heart J. 1989 Mar;61(3):238–247. doi: 10.1136/hrt.61.3.238. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McCance A. J., Forfar J. C. Cardiac and whole-body [3H]noradrenaline kinetics during adrenaline infusion in man. Clin Sci (Lond) 1991 Mar;80(3):227–233. doi: 10.1042/cs0800227. [DOI] [PubMed] [Google Scholar]
- Rona G. Catecholamine cardiotoxicity. J Mol Cell Cardiol. 1985 Apr;17(4):291–306. doi: 10.1016/s0022-2828(85)80130-9. [DOI] [PubMed] [Google Scholar]