Abstract
Background:
Few studies have examined how parenting influences the associations between prenatal maternal stress and children’s mental health. The objectives of this study were to examine the sex-specific associations between prenatal maternal stress and child internalizing and externalizing symptoms, and to assess the moderating effects of parenting behaviors on these associations.
Methods:
This study is based on 15,963 mother-child dyads from the Norwegian Mother, Father and Child Cohort Study (MoBa). A broad measure of prenatal maternal stress was constructed using 41 self-reported items measured during pregnancy. Three parenting behaviors (positive parenting, inconsistent discipline, positive involvement) were assessed by maternal report at child age 5 years. Child symptoms of internalizing and externalizing disorders (depression, anxiety, attention deficit hyperactivity disorder, conduct disorder, oppositional defiant disorder) were assessed by maternal report at age 8. Analyses were conducted using structural equation modeling techniques.
Results:
Prenatal maternal stress was associated with child internalizing and externalizing symptoms at age 8; associations with externalizing symptoms differed by sex. Associations between prenatal maternal stress and child depression, and conduct disorder and oppositional defiant disorder in males, became stronger as levels of inconsistent discipline increased. Associations between prenatal maternal stress and symptoms of attention-deficit hyperactivity disorder in females were attenuated as levels of parental involvement increased.
Conclusions:
This study confirms associations between prenatal maternal stress and children’s mental health outcomes, and demonstrates that these associations may be modified by parenting behaviors. Parenting may represent an important intervention target for improving mental health outcomes in children exposed to prenatal stress.
Keywords: prenatal stress, internalizing, externalizing, parenting, fetal programming, MoBa
According to the developmental origins of health and disease hypothesis, exposure to maternal stress during critical developmental windows can lead to enduring alterations of fetal endocrine, nervous, and immune systems, which can have long-term consequences for children’s health and development (Barker, 1990; Glover, O’Connor, & O’Donnell, 2010). In line with this hypothesis, maternal stress during pregnancy is associated with children’s risk of depression, externalizing disorders, and other mental health disorders (Kingsbury et al., 2016; MacKinnon, Kingsbury, Mahedy, Evans, & Colman, 2018; Van den Bergh et al., 2017).
Sex differences in the consequences of exposure to prenatal maternal stress are well-documented (Sutherland & Brunwasser, 2018). Animal studies demonstrate sex-specific alterations to neural structures and the hypothalamic–pituitary–adrenal (HPA) axis in response to prenatal maternal stress (Glover & Hill, 2012). Evolutionary explanations posit that female fetuses adapt to intrauterine stress exposures through growth modulation and greater stress responsiveness, which can improve viability but give rise to depressed or anxious phenotypes (Bale, 2011; Glover & Hill, 2012). Conversely, male fetuses tend to prioritize growth and physical development in response to adversity; after birth, males may be better adapted to explore new environments and compete with other males, but these adaptations can lead to greater aggression (Bale, 2011; Glover & Hill, 2012). These differences are reflected in the developmental literature, as several studies demonstrate stronger associations between prenatal maternal stress and internalizing symptoms in females and externalizing symptoms in males (Sutherland & Brunwasser, 2018), emphasizing the need to evaluate sex-specific effects of prenatal maternal stress on children’s development.
A wide range of stressors can activate the maternal stress response system. In line with this, the measurement of maternal stress during pregnancy varies substantially among existing studies; measures ranging from adverse events to maternal depression have been used to assess stress (Nast, Bolten, Meinlschmidt, & Hellhammer, 2013), and have demonstrated associations with children’s mental health (Plant, Pariante, Sharp, & Pawlby, 2015; Van Den Bergh & Marcoen, 2004). Several studies have examined these stressors in isolation; however, co-occurrence is common, and experiencing multiple forms of stress can further amplify children’s risk of adverse outcomes (Appleyard, Egeland, van Dulmen, & Sroufe, 2005). Many stress measures overlap conceptually and phenotypically (O’Donnell, O’Connor, & Glover, 2009), thus, it may be more valuable to focus on broad representations of prenatal maternal stress that capture the shared variance across stress measures (Nast et al., 2013). This view is supported by recent studies that have found associations between broad conceptualizations of prenatal maternal stress and children’s intelligence, autistic traits, and callous-unemotional behaviors (Cecil et al., 2014; Cortes Hidalgo et al., 2018; Rijlaarsdam et al., 2016).
The long-term burden of early life stress exposure on mental health is not limited to exposures during fetal life. Emerging research has examined the impacts of postnatal exposures, including attachment and adversity, on the development of mental disorders in light of prenatal maternal stress exposure (Bergman, Sarkar, Glover, & O’Connor, 2010; Costello, Worthman, Erkanli, & Angold, 2007); this has broad implications given that several aspects of the postnatal environment may be modifiable (Yap et al., 2016). In particular, parenting behaviors may be a target of intervention, as positive and negative parenting behaviors are associated with prenatal stress and children’s mental health (Clayborne et al., 2020; Huizink et al., 2017). For example, positive parental involvement has been associated with lower risk of incident depression in early adulthood (Cong, Hosler, Tracy, & Appleton, 2020), whereas harsh parenting and inconsistent discipline have been associated with increased externalizing problems and depressive symptoms (Feehan, McGee, Stanton, & Silva, 1991; Kingsbury, Sucha, Manion, Gilman, & Colman, 2020). To our knowledge, few studies have examined whether parenting behaviors moderate the effects of prenatal maternal stress on developmental outcomes. As a result, there is a need for research that investigates the moderating role of parenting behaviors on these associations.
The aims of our study were two-fold. Our first aim was to examine the associations between a broad measure of prenatal maternal stress and children’s internalizing and externalizing symptoms in a longitudinal sample, and to ascertain potential sex differences of the associations. Our second aim was to examine the moderating roles of positive parenting, positive parental involvement, and inconsistent discipline on these associations.
Methods
Sample
The current study utilizes data from the Norwegian Mother, Father and Child Cohort Study (MoBa), a population-based pregnancy cohort study conducted by the Norwegian Institute of Public Health. Participants were recruited from across Norway between 1999 and 2008, and women consented to participation in 41% of pregnancies. The cohort now includes over 114,500 children, 95,200 mothers and 75,200 fathers (Magnus et al., 2016). Maternal questionnaire response rates at the 17th and 30th week of gestation, and at 18 months and 5 years after birth were 95.1%, 91.4%, 87.0% and 54.0%, respectively (Schreuder & Alsaker, 2014). The current study is based on version 12 of the quality-assured data files released for research in 2020. The establishment of MoBa and initial data collection was based on a license from the Norwegian Data Protection Agency and approval from The Regional Committees for Medical and Health Research Ethics. The MoBa cohort is now based on regulations related to the Norwegian Health Registry Act. This study includes 15,963 participants with available data on study exposure and outcome variables (see Figure S1). This study was approved by The Regional Committees for Medical and Health Research Ethics (#2013/2061).
Measures
Prenatal Maternal Stress.
A total of 41 items, collected via maternal questionnaire at 17 and/or 30 weeks’ gestation, were used to create a broad measure of prenatal maternal stress. This measure was constructed using methods developed by Cecil et al. (2014), which uses confirmatory factor analysis to account for the shared variance across prenatal stress measures, and has been implemented with good model fit in other studies (Cortes Hidalgo et al., 2018; Rijlaarsdam et al., 2016). The prenatal stress measure categorizes items in relation to four domains that account for different manifestations of stress: life stress, contextual stress, personal stress, and interpersonal stress. Items from each domain were summed and divided by the number of items to generate mean scores, which were used as indicators to extract a single, latent prenatal maternal stress factor. We excluded maternal education from the personal stress domain, because maternal education may impact child development by pathways independent of maternal prenatal stress (Cortes Hidalgo et al., 2018). We included occupational stress-related items into the contextual stress domain, and removed maternal hospitalizations during pregnancy from the life stress domain to improve fit of the measurement model, and required participants to have complete data on at least two out of four stress domains to improve stability of the latent variable. A list of included items is provided in the Appendix.
Parenting Behaviors.
Maternal parenting behaviors at child age 5 years were examined using the Alabama Parenting Questionnaire 9-item short-form version (APQ-9), which was developed to assess parenting practices in clinical and research settings (Elgar, Waschbusch, Dadds, & Sigvaldason, 2007). The APQ-9 was collected in version B of the 5 year questionnaire, which was provided to 64.3% of study participants (remaining participants received version A and thus were not eligible for study inclusion). The APQ-9 measures three dimensions of parenting that are relevant to the etiology and treatment of child internalizing and externalizing problems, including positive parenting (e.g., “you let your child know when they are doing a good job with something”), inconsistent discipline (e.g., “you threaten to punish your child and then do not actually punish him/her”), and positive parental involvement (e.g., “you have a friendly talk with your child”). All answers were scored on a 5-point Likert scale ranging from 1 (never) to 5 (always), with mean scores generated for each dimension. The APQ-9 demonstrates good construct and convergent validity, and is strongly correlated with scores from the complete APQ scale (Elgar et al., 2007). Scores from the APQ have also demonstrated moderate to strong correlations with observational data (Hawes & Dadds, 2006).
Child Mental Health Outcomes
Internalizing symptoms.
Mother-reported symptoms of child depression and anxiety were examined using total scores from short versions of the Mood and Feelings Questionnaire (SMFQ) and the Screen for Child Anxiety Related Disorders (SCARED) at child age 8 years (Birmaher et al., 1999, 1997). The SMFQ comprises 13 items assessing depressive symptoms experienced over the past two weeks, rated from 0 (not true) to 2 (true), resulting in a total sum score of 0–26, with higher scores representing increased depressive symptoms. The SCARED comprises five items rated on a 3-point Likert scale from 1 (not true) to 3 (true). Total scores were calculated by summing values of all items, resulting in a possible score range of 5–15, with higher scores representing increased symptoms of anxiety. Both the SMFQ and SCARED measures have demonstrated high internal consistency in several population‐based studies (Birmaher et al., 1999; Lundervold, Breivik, Posserud, Stormark, & Hysing, 2013).
Externalizing symptoms.
Mother-reported symptoms of attention deficit hyperactivity disorder, conduct disorder, and oppositional defiant disorder were assessed using the Parent/Teacher Rating Scale for Disruptive Behavior Disorders (RS-DBD) at child age 8 years (Silva et al., 2005). The scale consists of 34 items describing the child’s behavior during the last six to twelve months. This includes 18 items reflecting symptoms of attention deficit hyperactivity disorder (e.g., “Has difficulty sustaining attention in tasks or play activities”), 8 items related to conduct disorder (e.g., “Initiates physical fights”), and 8 items related to oppositional defiant disorder (e.g., “Argues with adults”). Items were rated on a 4-point Likert scale from 1 (never/rarely) to 4 (very often). For each disorder, item scores were summed into total scores, with higher scores representing increased symptoms. Items included in the RS-DBD reflect those presented in the Diagnostic and Statistical Manual of Diseases – 4th revision (DSM‐IV-TR), and the measure demonstrates good construct and instrument validity when compared to other parent- and teacher-rated measures of externalizing symptoms (Silva et al., 2005).
Covariates.
Child sex (male or female) was examined as a potential stratification variable and used as a covariate where sex differences were not statistically significant. A number of potential confounding variables were also identified a priori based on the existing literature and investigated in analyses. This included maternal and paternal education (postsecondary and above, high school and below); smoking during the first trimester of pregnancy (yes or no); drinking during the first trimester of pregnancy (never, 1–3 times per month, 1 time per week or more); and parity (no prior births, 1+ prior births). Maternal symptoms of depression at child age 5, measured using the Hopkins Symptom Checklist-8 (Strand, Dalgard, Tambs, & Rognerud, 2003), and cumulative maternal adverse events up to child age 5, were adjusted for in sensitivity analyses.
Statistical Analyses
Reporting of participant characteristics and attrition analyses comparing those included and excluded from the study sample on key study variables were performed using Stata version 15 (StataCorp, College Station, TX). Remaining analyses were conducted using MPlus version 8 (Muthén & Muthén, Los Angeles, CA). Estimation of the associations between prenatal maternal stress and child internalizing and externalizing symptoms was performed using structural equation modelling, with multiple group analyses performed to ascertain potential sex differences. Next, interaction terms were added to the structural equation models to assess moderation by positive parenting, positive parental involvement, and inconsistent discipline. To account for potential non-normality of data and missing values on prenatal stress items and covariates, all models were estimated using full information maximum likelihood estimation (FIML) with robust standard errors (MLR), which is a valid analytic approach to dealing with missing data and is robust to the assumption that data are missing at random (Enders & Bandalos, 2001). Sensitivity analyses were then conducted by adjusting for cumulative maternal stressful life events and maternal depression at child age 5 years for all interaction analyses. Examples of the models assessed in this study are provided in Figures S2 and S3, and details on main analyses conducted are presented below.
Associations between prenatal maternal stress and child internalizing and externalizing symptoms.
Confirmatory factor analysis was used to estimate a latent factor of prenatal maternal stress using mean scores from the four calculated prenatal stress domains as indicators, and analyses of the associations between latent prenatal maternal stress and child internalizing and externalizing symptoms were performed simultaneously. Latent prenatal maternal stress was standardized by scaling its variance to 1, with standardized parameter estimates reported representing changes in the standard deviations of child mental health variables per one standard deviation increase in latent prenatal maternal stress. Unstandardized parameter estimates are also reported, and represent changes in child mental health variables per one unit increase in the latent prenatal maternal stress variable. Unadjusted and adjusted models were estimated. Measures examining internalizing and externalizing disorders were allowed to correlate in all models. Fit of the measurement and structural models were assessed using the comparative fit index (CFI) and the root mean square error of approximation (RMSEA), where good fit was categorized as a value of 0.90 and above or 0.06 and below (Hu & Bentler, 1999; McDonald & Ho, 2002), respectively.
Sex differences were ascertained through multiple group analyses, whereby models examining the associations between prenatal maternal stress and child internalizing or externalizing symptoms were stratified by sex and examined simultaneously. Constrained (all factor loadings held equal) and unconstrained (free estimation of paths between prenatal stress and child internalizing or externalizing symptoms) models were compared using likelihood ratio tests to ascertain whether or not unconstrained estimates significantly differed by sex (p < .05); if significant, analyses were stratified by sex.
Moderating effects of parenting.
To examine moderation by parenting measures, interaction terms were created between prenatal maternal stress and each parenting measure using the XWITH procedure in MPlus, in accordance with the latent moderated structural equations approach (Klein & Moosbrugger, 2000). We considered moderation to be present if interaction terms were significantly associated with symptoms of internalizing or externalizing disorders at a threshold of p < .05. Statistically significant interactions were probed using the Johnson-Neyman technique in MPlus (Johnson & Neyman, 1936), which plots the unstandardized effect (slope) of latent prenatal maternal stress on symptoms of internalizing or externalizing disorders and their 95% confidence intervals (CI) on the y-axis, against the complete range of values for the moderator variables on the x-axis. For continuous moderators, the Johnson-Neyman technique in MPlus provides a visual representation of the values of the moderating variables (on the X-axis) at which the associations between prenatal maternal stress and child internalizing and externalizing symptoms are statistically significant (i.e., where the effect line and its 95% CI do not overlap with zero on the Y-axis), and highlight the strength of the associations across values of the moderating variables.
Results
The majority of mothers included in the sample were married or cohabiting, had some level of post-secondary education, and were pregnant with their first child. Approximately 3.5% of women reported smoking (sometimes or daily), and 8% of women reported alcohol use (1 drink per month or greater) at 17 weeks’ gestation. Descriptive characteristics of the sample, including information on missing data, are summarized in Table 1.
Table 1.
Descriptive characteristics of sample at 17 weeks’ gestation (N = 15,963)
| Characteristic | Mean ± SD or n (%) |
|---|---|
| Maternal age | 30.48 ± 4.37 |
| Parity | |
| 0 | 8,080 (50.62) |
| 1+ Missing |
7,753 (48.57) 130 (0.81) |
| Marital status | |
| Married | 7,722 (48.37) |
| Cohabiting | 7,820 (48.99) |
| Single | 354 (2.22) |
| Missing | 67 (0.42) |
| Maternal education | |
| > High school | 11,960 (74.92) |
| High school and below | 3,306 (20.71) |
| Missing | 697 (4.37) |
| Paternal education | |
| > High school | 9,076 (56.86) |
| High school and below | 5,668 (35.51) |
| Missing | 1,219 (7.64) |
| Smoking | |
| None | 15,025 (94.12) |
| Sometimes | 250 (1.57) |
| Daily | 312 (1.95) |
| Missing | 376 (2.36) |
| Alcohol use | |
| None | 12,836 (80.41) |
| 1–3 drinks per month | 1,257 (7.87) |
| 1+ drinks per week | 50 (0.31) |
| Missing | 1,820 (11.40) |
Note. SD = standard deviation
Associations between prenatal maternal stress and child internalizing and externalizing symptoms
The measurement model for latent prenatal maternal stress (Figure S4) had excellent fit (RMSEA = .00, 90% CI = .000, .014; CFI = 1.000), and all stress domains and outcomes were significantly correlated (Table S1). The likelihood-ratio test to assess for sex differences was not statistically significant for symptoms of internalizing disorders, χ2(2) = 3.614, p = .16, suggesting that the associations between prenatal maternal stress and symptoms of depression and anxiety were similar for males and females. The associations between prenatal maternal stress and symptoms of depression and anxiety were statistically significant prior to and after adjustment for covariates including sex (Table 2), and model fit was good (RMSEA = .043, 90% CI = .040, .045; CFI = 0.901).
Table 2.
Models of associations between prenatal maternal stress, parenting behaviours at age 5, and their interactions, and symptoms of internalizing disorders at age 8 (N = 15,963)
| Symptoms of Depression | Symptoms of Anxiety | |||
|---|---|---|---|---|
| b (SE) | β (95% CI) | b (SE) | β (95% CI) | |
| Individual models | ||||
| Prenatal maternal stress (unadjusted) | 21.039 (1.318)*** | .291 (.268, .31416) | 6.104 (.505)*** | .166 (.144, .189) |
| Prenatal maternal stress (adjusted) | 20.383 (1.344)*** | .301 (.276, .327) | 6.147 (0.514)*** | .179 (.154, .203) |
| Positive parenting model | ||||
| Prenatal maternal stress | 38.760 (11.064)*** | .576 (.260, .891) | 10.687 (4.234)* | .313 (.073, .553) |
| Positive parenting | −.421 (.044)*** | −.077 (−.092, −.061) | −.078 (.022)*** | −.028 (−.044, −.012) |
| Prenatal maternal stress × Positive parenting | −4.073 (2.389) | −.026 (−.056, .004) | −1.009 (.918) | −.013 (−.036, .010) |
| Inconsistent discipline model | ||||
| Prenatal maternal stress | 5.463 (3.593) | .080 (−.024, .192) | 3.741 (1.486)* | .108 (.024, .192) |
| Inconsistent discipline | .366 (.030)*** | .094 (.078, .109) | .048 (.016)** | .024 (.009, .040) |
| Prenatal maternal stress × Inconsistent discipline | 7.099 (1.878) *** | .064 (.032, .095) | 1.094 (.693) | .019 (−.005, .043) |
| Positive parental involvement model | ||||
| Prenatal maternal stress | 40.511 (11.218)*** | .600 (.282, .919) | 10.865 (4.913)* | .317 (.039, .594) |
| Positive parental involvement | −.476 (.051)*** | −.072 (−.088, −.057) | −.110 (.026)*** | −.033 (−.048, −.018) |
| Prenatal maternal stress × Positive parental involvement | −4.593 (2.486) | −.025 (−.051, .001) | −1.078 (1.103) | −.011 (−.034, .011) |
Note.
p < .05,
p < .01,
p < .001.
Significant moderation effects also bolded. b = unstandardized regression coefficient, SE = standard error, β = standardized regression coefficient, CI = confidence interval. Symptoms of depression and anxiety were included together in models. Models were adjusted for the following covariates: maternal education, paternal education, maternal alcohol use, maternal smoking, parity, and sex.
For the associations between prenatal maternal stress and symptoms of externalizing disorders, the likelihood-ratio test to assess for sex differences was statistically significant, χ2(3) = 37.966, p < .001, and analyses were sex-stratified. Prenatal maternal stress was associated with symptoms of all externalizing disorders in males and females. However, the associations with symptoms of conduct disorder and oppositional defiant disorder appeared slightly stronger for males compared to females (Tables 3 and 4), and associations with symptoms of attention deficit hyperactivity disorder appeared stronger for females compared to males. Model fit was excellent for both male (RMSEA = .036, 90% CI = .032, .039; CFI = 0.963) and female (RMSEA = .039, 90% CI = .036, .043; CFI = 0.945) models.
Table 3.
Models of associations between prenatal maternal stress, parenting behaviours at age 5, and their interactions, and symptoms of externalizing disorders at age 8 (males, n = 8,083)
| Symptoms of Attention-Deficit Hyperactivity Disorder | Symptoms of Conduct Disorder | Symptoms of Oppositional Defiant Disorder | ||||
|---|---|---|---|---|---|---|
| b (SE) | β (95% CI) | b (SE) | β (95% CI) | b (SE) | β (95% CI) | |
| Individual models | ||||||
| Prenatal maternal stress (unadjusted, full sample) | 47.336 (3.143)*** | .234 (.211, .256) | 5.305 (.536)*** | .125 (.102, .148) | 17.438 (1.296)*** | .192 (.170, .214) |
| Prenatal maternal stress (adjusted, full sample) | 44.776 (3.207)*** | .234 (.208, .259) | 5.075 (.564)*** | .126 (.101, .152) | 17.385 (1.335)*** | .202 (.177, .227) |
| Prenatal maternal stress (unadjusted, males) | 48.375 (3.561)*** | .231 (.202, .259) | 6.713 (.738)*** | .141 (.112, .170) | 17.686 (1.490)*** | .195 (.167, .223) |
| Prenatal maternal stress (adjusted, males) | 45.560 (3.647)*** | .229 (.198, .260) | 6.454 (.774)*** | .143 (.111, .175) | 17.881 (1.554)*** | .208 (.176, .240) |
| Positive parenting model | ||||||
| Prenatal maternal stress | 52.511 (35.388) | .266 (−.084, .617) | 22.416 (8.555)** | .501 (.127, .875) | 30.369 (13.993)* | .356 (.035, .677) |
| Positive parenting | −1.409 (.193)*** | −.083 (−.105, −.060) | −.422 (.044)*** | −.109 (−.131, −.087) | −.758 (.081)*** | −.103 (−.124, −.081) |
| Prenatal maternal stress × Positive parenting | −1.602 (7.785) | −.004 (−.037, .030) | −3.500 (1.831) | −.034 (−.069, .001) | −2.814 (3.081) | −.014 (−.045, .017) |
| Inconsistent discipline model | ||||||
| Prenatal maternal stress | 22.649 (12.397) | .114 (−.009, .236) | −1.535 (2.570) | −.034 (−.145, .077) | 1.643 (5.160) | .019 (−.099, .137) |
| Inconsistent discipline | 1.606 (.136)*** | .132 (.110, .154) | .353 (.030)*** | .128 (.107, .148) | .898 (.059)*** | .171 (.149, .192) |
| Prenatal maternal stress × Inconsistent discipline | 10.222 (5.931) | .032 (−.004, .067) | 3.763 (1.367) ** | .051 (.016, .087) | 7.345 (2.644) ** | .053 (.017, .088) |
| Positive parental involvement model | ||||||
| Prenatal maternal stress | 103.318 (47.399)* | .521 (.059, .982) | 20.670 (11.221) | .459 (−.029, .947) | 24.603 (17.277) | .286 (−.107, .680) |
| Positive parental involvement | −2.649 (.236)*** | −.129 (−.152, −.107) | −.626 (.236)*** | −.135 (−.157, −.113) | −1.118 (.099)*** | −.126 (−.148, −.104) |
| Prenatal maternal stress × Positive parental involvement | −13.240 (10.509) | −.024 (−.062, .013) | −3.248 (2.469) | −.024 (−.062, .013) | −1.556 (3.902) | −.007 (−.039, .026) |
Note.
p < .05,
p < .01,
p < .001.
Significant moderation effects also bolded. b = unstandardized regression coefficient, SE = standard error, β = standardized regression coefficient, CI = confidence interval. Symptoms of attention deficit hyperactivity disorder, conduct disorder, and oppositional defiant disorder were included together in models. Models were adjusted for the following covariates: maternal education, paternal education, maternal alcohol use, maternal smoking, and parity.
Table 4.
Models of associations between prenatal maternal stress, parenting behaviours at age 5, and their interactions, and symptoms of externalizing disorders at age 8 (females, n = 7,754)
| Symptoms of Attention-Deficit Hyperactivity Disorder | Symptoms of Conduct Disorder | Symptoms of Oppositional Defiant Disorder | ||||
|---|---|---|---|---|---|---|
| b (SE) | β (95% CI) | b (SE) | β (95% CI) | b (SE) | β (95% CI) | |
| Individual models | ||||||
| Prenatal maternal stress (unadjusted, full sample) | 47.336 (3.143)*** | .234 (.211, .256) | 5.305 (.536)*** | .125 (.102, .148) | 17.438 (1.296)*** | .192 (.170, .214) |
| Prenatal maternal stress (adjusted, full sample) | 44.776 (3.207)*** | .234 (.208, .259) | 5.075 (.564)*** | .126 (.101, .152) | 17.385 (1.335)*** | .202 (.177, .227) |
| Prenatal maternal stress (unadjusted) | 45.903 (3.542)*** | .248 (.218, .278) | 3.601 (.539)*** | .109 (.078, .141) | 16.938 (1.608)*** | .188 (.158, .219) |
| Prenatal maternal stress (adjusted) | 43.636 (3.603)*** | .250 (.217, .284) | 3.400 (.561)*** | .110 (.075, .144) | 16.618 (1.655)*** | .196 (.162, .230) |
| Positive parenting model | ||||||
| Prenatal maternal stress | 35.582 (37.712) | .208 (−.224, .641) | 15.907 (9.677) | .522 (−.099, 1.144) | 20.288 (15.924) | .244 (−.133, .621) |
| Positive parenting | −1.328 (.159)*** | −.094 (−.116, −.072) | −.251 (.030)*** | −.100 (−.122, −.078) | −.794 (.077)*** | −.116 (−.138, −.094) |
| Prenatal maternal stress × Positive parenting | 1.569 (8.263) | .004 (−.037, .045) | −2.689 (2.005) | −.038 (−.094, .018) | −.815 (3.485) | −.046 (−.040, .031) |
| Inconsistent discipline model | ||||||
| Prenatal maternal stress | 23.474 (13.426) | .134 (−.017, .285) | −2.099 (3.017) | −.067 (−.255, .121) | 4.769 (6.084) | .056 (−.084, .196) |
| Inconsistent discipline | 1.292 (.116)*** | .128 (.106, .151) | .188 (.020)*** | .105 (.083, .126) | .860 (.056)*** | .176 (.154, .199) |
| Prenatal maternal stress × Inconsistent discipline | 8.329 (6.518) | .029 (−.015, .073) | 2.611 (1.694) | .051 (−.013, .115) | 4.910 (2.968) | .035 (−.006, .077) |
| Positive parental involvement model | ||||||
| Prenatal maternal stress | 157.264 (44.195)*** | .910 (.412, 1.407) | 16.018 (13.459) | .523 (−.343, 1.388) | 33.560 (19.281) | .400 (−.055, .854) |
| Positive parental involvement | −2.110 (.183)*** | −.125 (−.146, −.104) | −.336 (.033)*** | −.112 (−.133, −.091) | −1.085 (.091)*** | −.132 (−.154, −.110) |
| Prenatal maternal stress × Positive parental involvement | −25.909 (9.695)** | −.054 (−.094, −.014) | −2.841 (2.889) | −.034 (−.101, .034) | −3.919 (4.295) | −.017 (−.053, .020) |
Note.
p < .05,
p < .01,
p < .001.
Significant moderation effects also bolded. b = unstandardized regression coefficient, SE = standard error, β = standardized regression coefficient, CI = confidence interval. Symptoms of attention deficit hyperactivity disorder, conduct disorder, and oppositional defiant disorder were included together in models. Models were adjusted for the following covariates: maternal education, paternal education, maternal alcohol use, maternal smoking, and parity.
Moderation by parenting behaviors
The interaction term between prenatal maternal stress and inconsistent discipline was small but statistically significant and positively associated with symptoms of depression (β =.063, 95% CI: .032, .094). The association between prenatal maternal stress and symptoms of depression was significant at all values of inconsistent discipline (i.e., the effect and 95% confidence intervals were above 0 across values of inconsistent discipline), however, the strength of the association increased with increasing levels of inconsistent discipline (Figure 1A). Interaction terms between prenatal maternal stress and positive parenting and positive parental involvement in structural models examining symptoms of depression or anxiety were not statistically significant (Table 2).
Figure 1.
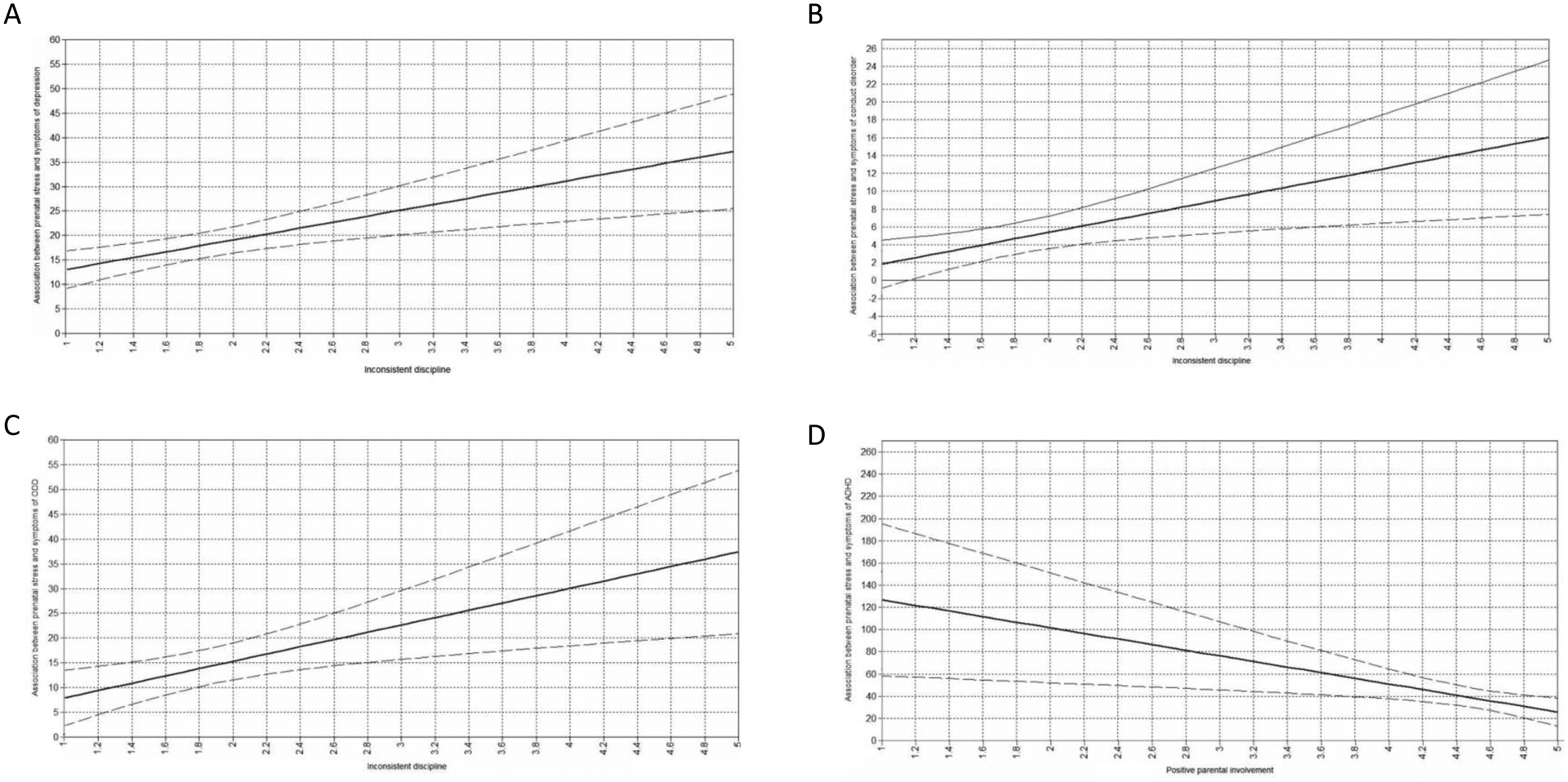
Johnson-Neyman plots of significant interactions between prenatal maternal stress and parenting behaviours at age 5 on child internalizing and externalizing symptoms at age 8. A) Moderating role of inconsistent discipline on the association between prenatal maternal stress and symptoms of depression. B) Moderating role of inconsistent discipline on the association between prenatal maternal stress and symptoms of conduct disorder in males. C) Moderating role of inconsistent discipline on the association between prenatal maternal stress and symptoms of oppositional defiant disorder (ODD) in males. D) Moderating role of positive parental involvement on the association between prenatal maternal stress and symptoms of attention deficit hyperactivity disorder (ADHD) in females. Plot lines represent effect (solid line) and 95% confidence interval of effect (dashed lines).
For males and females, interactions between prenatal maternal stress and positive parenting were not significantly associated with symptoms of externalizing disorders (Tables 3 and 4). For males, the interaction terms between prenatal maternal stress and inconsistent discipline were small but positively associated with higher symptoms of conduct disorder (β = .049, 95% CI = .014, .085) and oppositional defiant disorder (β =.049, 95% CI = .014, .085); interaction terms were not significant for females. The association between prenatal maternal stress and symptoms of conduct disorder was significant at most values of inconsistent discipline, and not statistically significant at the lowest values of inconsistent discipline (Figure 1B). The association between prenatal maternal stress and symptoms of oppositional defiant disorder in males was significant at all values of inconsistent discipline (Figure 1C). Strength of the associations between prenatal maternal stress and symptoms of conduct disorder and oppositional defiant disorder increased as levels of inconsistent discipline increased. For females, the interaction between prenatal maternal stress and positive parental involvement was small but negatively associated with symptoms of attention-deficit hyperactivity disorder (β = −.053, 95% CI: −.093, −.013); interaction terms were not significant for males. The association between prenatal maternal stress and symptoms of attention-deficit hyperactivity disorder in females was significant at all values of positive parental involvement, however, strength of the association was attenuated as positive parental involvement increased (Figure 1D).
Attrition and sensitivity analyses
Comparisons between those included in the study sample and those excluded from analysis are presented in Table S2, as well as detailed information on missing data. Excluded participants, on average, were younger, were less likely to have postsecondary education, and were more likely to have at least one child, smoke during pregnancy, report higher levels of all four prenatal stress domains, and report higher internalizing and externalizing symptoms for children at age 5. Sensitivity analyses adjusting for maternal stressful life events from birth to child age 5 years, and symptoms of depression at child age 5 years are presented in Tables S3 to S5; all interaction effects remained statistically significant after these additional adjustments.
Discussion
Our prospective study of almost 16,000 mother-child dyads demonstrates associations between a broad measure of prenatal maternal stress and subsequent symptoms of internalizing and externalizing disorders in children at 8 years of age; associations between prenatal maternal stress and externalizing disorders also differed by sex. Our findings further demonstrate that several of these associations are moderated by parenting behaviors. Higher levels of inconsistent discipline indicated stronger associations between prenatal maternal stress and child depression in both sexes, and conduct disorder and oppositional defiant disorder in males, and higher levels of positive parental involvement attenuated the association between prenatal maternal stress and symptoms of attention-deficit hyperactivity disorder in girls. These effects also persisted after adjustment for postnatal maternal depression and stressful life events.
Our findings are in line with prior studies on prenatal maternal stress and children’s internalizing and externalizing disorders (Van den Bergh et al., 2017), and expand the evidence base by demonstrating the effects of a broad measure of prenatal maternal stress. We tested for potential sex differences, and in line with the extant literature (Sutherland & Brunwasser, 2018), observed sex differences in the associations between prenatal maternal stress and symptoms of externalizing disorders. Contrary to expectations, we did not observe any statistically significant sex differences for models with internalizing symptoms. A potential explanation for this finding is that these sex differences may appear later in development. Animal models suggest that prenatal maternal stress may disrupt sex-specific development of the prefrontal cortex during adolescence, which differentially influences vulnerability to psychiatric disorders among males and females (Markham, Mullins, & Koenig, 2013); several observational studies demonstrate that females are at greater risk for internalizing disorders compared to males into adolescence and adulthood (Bale & Epperson, 2015).
Emerging evidence further suggests that the associations between prenatal stress and offspring outcomes may be conditional on the postnatal environment, whereby prenatal stress promotes postnatal “developmental plasticity” (Costello et al., 2007; Pluess & Belsky, 2011). This hypothesis of differential susceptibility suggests that exposure to prenatal stress can increase offspring sensitivity to positive and negative postnatal influences, thus either reducing or amplifying risk towards adverse outcomes. A growing number of experimental and observational studies support the role of postnatal environmental factors in moderating the associations between prenatal stress exposure and children’s development in line with differential susceptibility. For example, research suggests that among offspring born to prenatally anxious mothers, higher exposure to postnatal maternal stroking in the first few weeks of life imparts a protective effect on internalizing symptoms at 2.5 years of age, whereas lower exposure is associated with increased internalizing symptoms.(Sharp, Hill, Hellier, & Pickles, 2015). In addition, research conducted in prairie voles suggests that prenatally stressed voles are more responsive to postnatal rearing environments than non-stressed voles.(Hartman, Freeman, Bales, & Belsky, 2018)
There has been limited research examining the moderating role of parenting behaviors in the associations between prenatal maternal stress and child developmental outcomes; among existing studies, findings have been inconsistent (Grant, McMahon, Reilly, & Austin, 2010; McLean et al., 2020; Schechter et al., 2017). Our findings support small interaction effects of inconsistent discipline and positive parental involvement in a manner such that the strength of the associations between prenatal maternal stress and internalizing and externalizing outcomes are amplified when levels of inconsistent discipline are high (or levels of positive parental involvement are low), and vice versa. Elucidating how parenting behaviours moderate these associations based on differential susceptibility can have substantial public health implications (Hartman & Belsky, 2018). Parenting behaviors are potentially modifiable (Yap, Cheong, Zaravinos-Tsakos, Lubman, & Jorm, 2017), and child regulation of stress hormones and other physiological systems implicated in the later onset of psychiatric disorders are responsive to parenting and other psychosocial interventions (Slopen, McLaughlin, & Shonkoff, 2014; Traub & Boynton-Jarrett, 2017). Intervention research also suggests that children who have been affected by adversity tend to benefit most from supportive interventions targeting parenting, in line with models of differential susceptibility (Belsky & van Ijzendoorn, 2017). Research by Pitzer et al. (2011) examining interactions between temperament, parenting, and externalizing problems also partially supports differential susceptibility, and suggests that the influence of parenting behaviours among fearful-inhibited children may be gender-specific (i.e., boys may be more responsive to sensitive parenting, whereas girls may respond more to restrictive parenting). Thus, parenting behaviors may represent a valuable target of intervention in order to enhance resilience among children exposed to early adversity (Traub & Boynton-Jarrett, 2017).
Findings from the current study should be interpreted in light of a number of limitations. First, measures were collected by maternal report, and reporting bias cannot be ruled out. However, many of the included measures have been validated and widely used in epidemiological and psychiatric research (see Appendix for prenatal stress items). Second, parenting behaviors were only reported for mothers, and the role of paternal parenting was not examined. Paternal parenting has demonstrated effects on child behaviour, and paternal involvement may moderate the association between maternal depression and child internalizing symptoms (Mezulis, Hyde, & Clark, 2004); thus, paternal parenting may benefit from further study. Third, we were limited to the parenting measures collected in the MoBa study, however, other parenting behaviours, including parental sensitivity, have demonstrated associations with children’s mental health (Kok et al., 2013), and warrant further analysis. Furthermore, the associations between parenting and children’s behaviour are often bidirectional and parenting can vary throughout childhood depending on both parent and child factors ((Reitz, Deković, & Meijer, 2006; Williford, Calkins, & Keane, 2007)); future researchers may seek to examine the moderating effects of parenting throughout development, and to examine how parenting and children’s behaviour interact over time. Fourth, we did not include genetic information in analyses, and cannot rule out the potential for genetic confounding; more research is needed to determine the role that genetics may play in the observed associations. Fifth, over 99% of MoBa participants report European ancestry, and most are of higher socioeconomic status. Our findings may not generalize to regions with greater socioeconomic or ethnic diversity, and highlight the need to further examine these associations in diverse samples. Sixth, although the assessed stress domains loaded onto a single latent factor, their intercorrelations were small-to-moderate; thus, it may be of interest for future researchers to measure the effects of these domains separately to ascertain the specific effects of early-life stress exposure on children’s development. Finally, substantial attrition was observed over the study follow-up period, which may potentially bias observed associations; however, prior MoBa analyses suggest that this attrition may not substantially impact general estimates of exposure-outcome associations (Nilsen et al., 2009).
These limitations are offset by strengths. The construction of a broad prenatal stress measure addresses limitations inherent to many previous developmental programming studies (Nast et al., 2013), and directly incorporates the shared variance across stress domains; thus, this measure may be of relevance for public health (Appleyard et al., 2005). In addition, the use of data from a prospective study with a large sample size allowed for the adjustment of several confounding variables, including measures reflective of postnatal adversity, with sufficient statistical power to evaluate sex differences and the moderating role of parenting behaviors on several children’s behavioural outcomes.
The current study provides evidence of associations between a broad measure of prenatal maternal stress and symptoms of internalizing and externalizing disorders in children, and highlights the role of positive and negative parenting behaviors in amplifying and reducing the effects of prenatal maternal stress on these outcomes respectively, partly supporting differential susceptibility. Findings may have implications for public health and research, and reinforce the need to develop and promote strategies aimed at reducing stress and reinforcing positive parenting in expecting and new mothers in order to cultivate intergenerational resilience and wellbeing.
Supplementary Material
Acknowledgements:
The Norwegian Mother, Father and Child Cohort Study is supported by the Norwegian Ministry of Health and Care Services and the Ministry of Education and Research. We are grateful to all the participating families in Norway who take part in this on-going cohort study. The consent given by the participants does not allow for storage of data on an individual level in repositories or journals. Researchers who want access to data sets for replication should submit an application to www.helsedata.no. Access to data sets requires approval from The Regional Committee for Medical and Health Research Ethics in Norway and an agreement with MoBa.
Funding Statement:
The present study was partially supported by the Research Council of Norway (RCN; project # 218373) and through RCN’s Centres of Excellence funding scheme, project # 262700, RCN’s guest research program, and the Canada Research Chairs program for Dr. Colman. Dr. Nilsen was supported by RCN (project # 296770). Dr. Torvik was supported by RCN (project #300668). Dr. Bekkhus was supported by RCN (project # 301004 and 288083). Dr. Gilman’s contribution to this research was supported by the Intramural Research Program of the Eunice Kennedy Shriver National Institute of Child Health and Human Development. Dr. Khandaker acknowledges funding support from the Wellcome Trust, UK (grant code: 201486/Z/16/Z), the MQ: Transforming Mental Health, UK (grant code: MQDS17/40), the Medical Research Council, UK (grant code: MC_PC_17213 and grant code: MR/S037675/1), and the BMA Foundation, UK (J Moulton grant 2019).
Footnotes
Conflicts of Interest: None
Ethical Standards: The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional committees on human experimentation and with the Helsinki Declaration of 1975, as revised in 2008.
References
- Appleyard K, Egeland B, van Dulmen MHM, & Sroufe LA (2005). When more is not better: the role of cumulative risk in child behavior outcomes. Journal of Child Psychology and Psychiatry and Allied Disciplines, 46(3), 235–245. doi: 10.1111/j.1469-7610.2004.00351.x [DOI] [PubMed] [Google Scholar]
- Bale TL (2011). Sex differences in prenatal epigenetic programing of stress pathways. Stress, 14(4), 348–356. doi: 10.3109/10253890.2011.586447 [DOI] [PubMed] [Google Scholar]
- Bale TL, & Epperson CN (2015). Sex differences and stress across the lifespan. Nature Neuroscience, 18(10), 1413–1420. doi: 10.1038/nn.4112 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Barker DJP (1990). The fetal and infant origins of adult disease. British Medical Journal, 301(6761), 1111. doi: 10.1136/bmj.301.6761.1111 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Belsky J, & van IJzendoorn MH (2017). Genetic differential susceptibility to the effects of parenting. Current Opinion in Psychology, 15, 125–130. doi: 10.1016/J.COPSYC.2017.02.021 [DOI] [PubMed] [Google Scholar]
- Bergman K, Sarkar P, Glover V, & O’Connor TG (2010). Maternal prenatal cortisol and infant cognitive development: moderation by infant-mother attachment. Biological Psychiatry, 67(11), 1026–1032. doi: 10.1016/j.biopsych.2010.01.002 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Birmaher B, Brent DA, Chiappetta L, Bridge J, Monga S, & Baugher M (1999). Psychometric properties of the screen for child anxiety related emotional disorders (SCARED): a replication study. Journal of the American Academy of Child and Adolescent Psychiatry, 38(10), 1230–1236. doi: 10.1097/00004583-199910000-00011 [DOI] [PubMed] [Google Scholar]
- Birmaher B, Khetarpal S, Brent D, Cully M, Balach L, Kaufman J, & Neer SMK (1997). The Screen for Child Anxiety Related Emotional Disorders (SCARED): scale construction and psychometric characteristics. Journal of the American Academy of Child and Adolescent Psychiatry, 36(4), 545–553. doi: 10.1097/00004583-199704000-00018 [DOI] [PubMed] [Google Scholar]
- Cecil CAM, Lysenko LJ, Jaffee SR, Pingault JB, Smith RG, Relton CL, … Barker ED (2014). Environmental risk, Oxytocin Receptor Gene (OXTR) methylation and youth callous-unemotional traits: a 13-year longitudinal study. Molecular Psychiatry, 19(10), 1071–1077. doi: 10.1038/mp.2014.95 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Clayborne ZM, Kingsbury M, Sampasa-Kinyaga H, Sikora L, Lalande KM, & Colman I (2020). Parenting practices in childhood and depression, anxiety, and internalizing symptoms in adolescence: a systematic review. Social Psychiatry and Psychiatric Epidemiology, 56(4), 619–638. doi: 10.1007/s00127-020-01956-z [DOI] [PubMed] [Google Scholar]
- Cortes Hidalgo AP, Neumann A, Bakermans-Kranenburg MJ, Jaddoe VWV, Rijlaarsdam J, Verhulst FC, … Tiemeier H (2018). Prenatal maternal stress and child IQ. Child Development, 91(2), 347–365. doi: 10.1111/cdev.13177 [DOI] [PubMed] [Google Scholar]
- Costello EJ, Worthman C, Erkanli A, & Angold A (2007). Prediction from low birth weight to female adolescent depression: a test of competing hypotheses. Archives of General Psychiatry, 64(3), 338–344. doi: 10.1001/archpsyc.64.3.338 [DOI] [PubMed] [Google Scholar]
- Elgar FJ, Waschbusch DA, Dadds MR, & Sigvaldason N (2007). Development and validation of a short form of the Alabama Parenting Questionnaire. Journal of Child and Family Studies, 16(2), 243–259. doi: 10.1007/s10826-006-9082-5 [DOI] [Google Scholar]
- Enders CK, & Bandalos DL (2001). The relative performance of full information maximum likelihood estimation for missing data in structural equation models. Structural Equation Modeling, 8(3), 430–457. doi: 10.1207/S15328007SEM0803_5 [DOI] [Google Scholar]
- Feehan M, McGee R, Stanton WR, & Silva PA (1991). Strict and inconsistent discipline in childhood: consequences for adolescent mental health. British Journal of Clinical Psychology, 30(4), 325–331. doi: 10.1111/j.2044-8260.1991.tb00953.x [DOI] [PubMed] [Google Scholar]
- Glover V, & Hill J (2012). Sex differences in the programming effects of prenatal stress on psychopathology and stress responses: An evolutionary perspective. Physiology and Behavior, 106(5), 736–740. doi: 10.1016/j.physbeh.2012.02.011 [DOI] [PubMed] [Google Scholar]
- Glover V, O’Connor TG, & O’Donnell K (2010). Prenatal stress and the programming of the HPA axis. Neuroscience & Biobehavioral Reviews, 35(1), 17–22. doi: 10.1016/J.NEUBIOREV.2009.11.008 [DOI] [PubMed] [Google Scholar]
- Grant KA, McMahon C, Reilly N, & Austin MP (2010). Maternal sensitivity moderates the impact of prenatal anxiety disorder on infant mental development. Early Human Development, 86(9), 551–556. 10.1016/j.earlhumdev.2010.07.004 [DOI] [PubMed] [Google Scholar]
- Hartman S, & Belsky J (2018). Prenatal programming of postnatal plasticity revisited—and extended. Development and Psychopathology, 30(3), 825–842. doi: 10.1017/S0954579418000548 [DOI] [PubMed] [Google Scholar]
- Hartman S, Freeman SM, Bales KL, & Belsky J (2018). Prenatal stress as a risk—and an opportunity—factor. Psychological Science, 29(4), 572–580. doi: 10.1177/0956797617739983 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hawes DJ, & Dadds MR (2006). Assessing parenting practices through parent-report and direct observation during parent-training. Journal of Child and Family Studies, 15(5), 554–567. doi: 10.1007/s10826-006-9029-x [DOI] [Google Scholar]
- Hu L, & Bentler PM (1999). Cutoff criteria for fit indexes in covariance structure analysis: conventional criteria versus new alternatives. Structural Equation Modeling, 6(1), 1–55. doi: 10.1080/10705519909540118 [DOI] [Google Scholar]
- Huizink AC, Menting B, De Moor MHM, Verhage ML, Kunseler FC, Schuengel C, & Oosterman M (2017). From prenatal anxiety to parenting stress: a longitudinal study. Archives of Women’s Mental Health, 20(5), 663–672. doi: 10.1007/s00737-017-0746-5 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Johnson PO, & Neyman J (1936). Tests of certain linear hypotheses and their application to some educational problems. Statistical Research Memoirs, 1, 57–93. [Google Scholar]
- Kingsbury M, Sucha E, Manion I, Gilman SE, & Colman I (2020). Adolescent mental health following exposure to positive and harsh parenting in childhood. Canadian Journal of Psychiatry, 65(6), 392–400. doi: 10.1177/0706743719889551 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kingsbury M, Weeks M, MacKinnon N, Evans J, Mahedy L, Dykxhoorn J, & Colman I (2016). Stressful life events during pregnancy and offspring depression: evidence from a prospective cohort study. Journal of the American Academy of Child and Adolescent Psychiatry, 55(8), 709–716. doi: 10.1016/j.jaac.2016.05.014 [DOI] [PubMed] [Google Scholar]
- Klein A, & Moosbrugger H (2000). Maximum likelihood estimation of latent interaction effects with the LMS method. Psychometrika, 65(4), 457–474. doi: 10.1007/BF02296338 [DOI] [Google Scholar]
- Kok R, Linting M, Bakermans-Kranenburg MJ, van IJzendoorn MH, Jaddoe VWV, Hofman A, … Tiemeier H (2013). Maternal sensitivity and internalizing problems: evidence from two longitudinal studies in early childhood. Child Psychiatry & Human Development, 44(6), 751–765. doi: 10.1007/s10578-013-0369-7 [DOI] [PubMed] [Google Scholar]
- Lundervold AJ, Breivik K, Posserud MB, Stormark KM, & Hysing M (2013). Symptoms of depression as reported by Norwegian adolescents on the Short Mood and Feelings Questionnaire. Frontiers in Psychology, 4, 313. doi: 10.3389/fpsyg.2013.00613 [DOI] [PMC free article] [PubMed] [Google Scholar]
- MacKinnon N, Kingsbury M, Mahedy L, Evans J, & Colman I (2018). The association between prenatal stress and externalizing symptoms in childhood: evidence from the Avon Longitudinal Study of Parents and Children. Biological Psychiatry, 83(2), 100–108. doi: 10.1016/j.biopsych.2017.07.010 [DOI] [PubMed] [Google Scholar]
- Magnus P, Birke C, Vejrup K, Haugan A, Alsaker E, Daltveit AK, … Stoltenberg C (2016). Cohort profile update: the Norwegian Mother and Child Cohort Study (MoBa). International Journal of Epidemiology, 45(2), 382–388. doi: 10.1093/ije/dyw029 [DOI] [PubMed] [Google Scholar]
- Markham JA, Mullins SE, & Koenig JI (2013). Periadolescent maturation of the prefrontal cortex is sex-specific and is disrupted by prenatal stress. Journal of Comparative Neurology, 521(8), 1828–1843. doi: 10.1002/cne.23262 [DOI] [PMC free article] [PubMed] [Google Scholar]
- McDonald RP, & Ho MHR (2002). Principles and practice in reporting structural equation analyses. Psychological Methods, 7(1), 64–82. 10.1037/1082-989X.7.1.64 [DOI] [PubMed] [Google Scholar]
- McLean MA, Cobham VE, Simcock G, Lequertier B, Kildea S, & King S (2020). Childhood anxiety: prenatal maternal stress and parenting in the QF2011 cohort. Child Psychiatry and Human Development. Advance online publication. doi: 10.1007/s10578-020-01024-2 [DOI] [PubMed] [Google Scholar]
- Mezulis AH, Hyde JS, & Clark R (2004). Father involvement moderates the effect of maternal depression during a child’s infancy on child behavior problems in kindergarten. Journal of Family Psychology, 18(4), 575–588. doi: 10.1037/0893-3200.18.4.575 [DOI] [PubMed] [Google Scholar]
- Nast I, Bolten M, Meinlschmidt G, & Hellhammer DH (2013). How to measure prenatal stress? A systematic review of psychometric instruments to assess psychosocial stress during pregnancy. Paediatric and Perinatal Epidemiology, 27(4), 313–322. doi: 10.1111/ppe.12051 [DOI] [PubMed] [Google Scholar]
- Nilsen RM, Vollset SE, Gjessing HK, Skjærven R, Melve KK, Schreuder P, … Magnus P (2009). Self-selection and bias in a large prospective pregnancy cohort in Norway. Paediatric and Perinatal Epidemiology, 3(6), 597–608. doi: 10.1111/j.1365-3016.2009.01062.x [DOI] [PubMed] [Google Scholar]
- O’Donnell K, O’Connor TG, & Glover V (2009). Prenatal stress and neurodevelopment of the child : focus on the HPA Axis and role of the placenta prenatal stress or anxiety predicts neurodevelopmental outcomes in the child. Dev Neurosci, 31(4), 285–292. doi: 10.1159/000216539 [DOI] [PubMed] [Google Scholar]
- Pitzer M, Jennen-Steinmetz C, Esser G, Schmidt MH, & Laucht M (2011). Differential susceptibility to environmental influences: the role of early temperament and parenting in the development of externalizing problems. Comprehensive Psychiatry, 52(6), 650–658. doi: 10.1016/j.comppsych.2010.10.017 [DOI] [PubMed] [Google Scholar]
- Plant DT, Barker ED Waters CS Pawlby S& Pariante CM (2013). Intergenerational transmission of maltreatment and psychopathology: the role of antenatal depression. Psychological Medicine, 43(3), 519–528. doi: 10.1017/S0033291712001298 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Plant Dominic T, Pariante CM Sharp D& Pawlby S(2015). Maternal depression during pregnancy and offspring depression in adulthood: role of child maltreatment. The British Journal of Psychiatry, 207(3), 213–220. doi: 10.1192/bjp.bp.114.156620 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Reitz E, Deković M, & Meijer AM (2006). Relations between parenting and externalizing and internalizing problem behaviour in early adolescence: Child behaviour as moderator and predictor. Journal of Adolescence, 29(3), 419–436. doi: 10.1016/j.adolescence.2005.08.003 [DOI] [PubMed] [Google Scholar]
- Rijlaarsdam J, Pappa I, Walton E, Bakermans-Kranenburg MJ, Mileva-Seitz VR, Rippe RCA, … van IJzendoorn MH (2016). An epigenome-wide association meta-analysis of prenatal maternal stress in neonates: a model approach for replication. Epigenetics, 11(2), 140–149. doi: 10.1080/15592294.2016.1145329 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Schechter JC, Brennan PA, Smith AK, Stowe ZN, Newport DJ, & Johnson KC (2017). Maternal prenatal psychological distress and preschool cognitive functioning: the protective role of positive parental engagement. Journal of Abnormal Child Psychology, 45(2), 249–260. doi: 10.1007/s10802-016-0161-9 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Schreuder P, & Alsaker E (2014). The Norwegian mother and child cohort study (MoBa) – MoBa recruitment and logistics. Norsk Epidemiologi, 24(1–2), 23–27. doi: 10.5324/nje.v24i1-2.1754 [DOI] [Google Scholar]
- Sharp H, Hill J, Hellier J, & Pickles A (2015). Maternal antenatal anxiety, postnatal stroking and emotional problems in children: outcomes predicted from pre- and postnatal programming hypotheses. Psychological Medicine, 45(2), 269–283. doi: 10.1017/S0033291714001342 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Silva RR, Alpert M, Pouget E, Silva V, Trosper S, Reyes K, & Dummit S (2005). A rating scale for disruptive behavior disorders, based on the DSM-IV item pool. Psychiatric Quarterly, 76(4), 327–339. doi: 10.1007/s11126-005-4966-x [DOI] [PubMed] [Google Scholar]
- Slopen N, McLaughlin KA, & Shonkoff JP (2014). Interventions to improve cortisol regulation in children: a systematic review. Pediatrics, 133(2), 312–326. doi: 10.1542/peds.2013-1632 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Strand BH, Dalgard OS, Tambs K, & Rognerud M (2003). Measuring the mental health status of the Norwegian population: Aacomparison of the instruments SCL-25, SCL-10, SCL-5 and MHI-5 (SF-36). Nordic Journal of Psychiatry, 57(2), 113–118. doi: 10.1080/08039480310000932 [DOI] [PubMed] [Google Scholar]
- Sutherland S, & Brunwasser SM (2018). Sex differences in vulnerability to prenatal stress: a review of the recent literature. Current Psychiatry Reports, 20(11), 1–12 doi: 10.1007/s11920-018-0961-4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Traub F, & Boynton-Jarrett R (2017). Modifiable resilience factors to childhood adversity for clinical pediatric practice. Pediatrics, 139(5), e20162569. doi: 10.1542/PEDS.2016-2569 [DOI] [PubMed] [Google Scholar]
- Van den Bergh BRH, van den Heuvel MI, Lahti M, Braeken M, de Rooij SR, Entringer S, … Schwab M (2017). Prenatal developmental origins of behavior and mental health: the influence of maternal stress in pregnancy. Neuroscience and Biobehavioral Reviews, 117, 26–64. doi: 10.1016/j.neubiorev.2017.07.003 [DOI] [PubMed] [Google Scholar]
- Van Den Bergh BRH, & Marcoen A (2004). High antenatal maternal anxiety is related to ADHD symptoms, externalizing problems, and anxiety in 8- and 9-year-olds. Child Development, 75(4), 1085–1097. doi: 10.1111/j.1467-8624.2004.00727.x [DOI] [PubMed] [Google Scholar]
- Williford AP, Calkins SD, & Keane SP (2007). Predicting change in parenting stress across early childhood: child and maternal factors. Journal of Abnormal Child Psychology, 35(2), 251–263. doi: 10.1007/s10802-006-9082-3 [DOI] [PubMed] [Google Scholar]
- Yap MBH, Cheong TWK, Zaravinos-Tsakos F, Lubman DI, & Jorm AF (2017). Modifiable parenting factors associated with adolescent alcohol misuse: a systematic review and meta-analysis of longitudinal studies. Addiction, 112(7), 1142–1162. doi: 10.1111/add.13785 [DOI] [PubMed] [Google Scholar]
- Yap MBH, Morgan AJ, Cairns K, Jorm AF, Hetrick SE, & Merry S (2016). Parents in prevention: a meta-analysis of randomized controlled trials of parenting interventions to prevent internalizing problems in children from birth to age 18. Clinical Psychology Review, 50, 138–158. doi: 10.1016/j.cpr.2016.10.003 [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.


