Abstract
This case report presents a young male patient with a 3-month history of a rapidly growing lower abdominal mass associated with lower urinary tract symptoms and recurrent urinary tract infection. Pelvic magnetic resonance imaging showed a large congenital cyst in the right seminal vesicle having a mass effect on the urinary bladder, rectum, and left ureter. Histopathologic findings from exploratory laparotomy showed an epidermal inclusion cyst with secondary inflammation and suppuration. This report adds to the literature by describing this unique location of an epidermoid cyst within the seminal vesicle.
Keywords: Epidermal inclusion cyst, Epidermoid cyst, Seminal vesicle, Case report
1. Introduction
An epidermoid cyst is a rare cystic lesion in the male pelvis. These cysts are typically asymptomatic; however, they may lead to the compression of the adjacent pelvic organs and more rarely present as an abdominal mass, or both conditions may coexist, as in the current case.1 Such cystic lesions may include epidermoid, dermoid, and enteric cysts with malignant pathologies, such as teratoma, teratocarcinoma, and yolk sac tumor.2 Axial imaging pelvic computed tomography and magnetic resonance imaging (MRI) are the gold standard for diagnosis. This case report presents a young male patient with a rapidly growing pelvic epidermoid cyst.
2. Case presentation
A 20-year-old man with no significant medical history presented for outpatient evaluation of a painless, large, lower abdominal swelling below the umbilicus. The patient first noticed this swelling incidentally 3 months before presentation, and it has grown rapidly since. He reported no change in bowel habits, no history of travel, and no previous trauma. He described the swelling as associated with dysuria and recurrent urinary tract infection. Vital signs were normal, with heart rate, blood pressure, and temperature of 76 beat/min, 123/74 mmHg, and 36.6 °C respectively. On physical examination, the abdomen was soft, with laxity and a visible infraumbilical swelling approximately 15 cm × 15 cm that was firm, not tender, and not mobile. Laboratory findings were unremarkable.
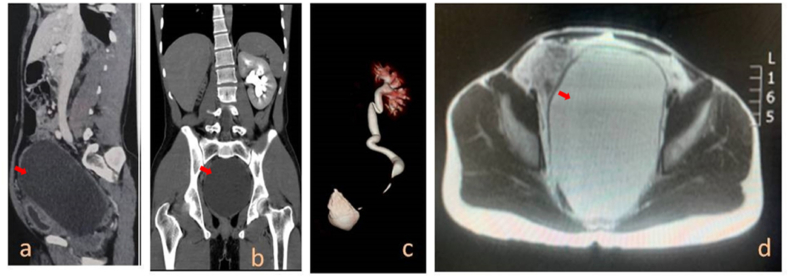
Pelvic-abdominal MRI (Fig. 1) revealed a homogeneous, well-demarcated, giant cystic mass 17 cm × 11 cm × 11 cm posterior to the urinary bladder and prostate, displacing them anteriorly and the rectum posteriorly, and compressing the distal left ureter with moderate proximal ureteric dilatation. The cystic mass was hypointense on T1-and significantly hyperintense on T2-weighted imaging with a thin regular wall. No solid components or restricted diffusion were reported. The mass was attached via a narrow tract with the right seminal vesicles. Computed tomography urography showed a normal left kidney, renal pelvis, and ureter; the right ureter was traced up to the renal pelvis with no ipsilateral renal parenchyma. The prostate was so markedly compressed by the mass that it could not be evaluated. The urinary bladder was also compressed and showed no mural thickening, masses, or diverticular outpouching. Pelvic lymph nodes were not enlarged. The patient was admitted and prepared for exploratory laparotomy.
Fig. 1.
Computed tomography urography (a, b, and c) shows no ipsilateral renal parenchyma. Computed tomography urography and Pelvic magnetic resonance imaging (Red Arrow) (a, b, and d) show a homogeneous giant cystic mass, posterior to the urinary bladder and prostate. (For interpretation of the references to colour in this figure legend, the reader is referred to the Web version of this article.)
The patient underwent exploratory laparotomy through a lower midline incision. A pelvic mass (15 cm × 17 cm) was identified that was adherent to the adjacent structures of the ureter, bladder, and iliac vessels. When the mass was released, the cyst was punctured and turbid fluid was aspirated around 1120ml, and around 30ml was sent for the lab. Next, a meticulous dissection was performed to separate the wall of the cyst from the adherent structures and excise the entire cyst. The patient recovered well and was discharged on postoperative day 4.
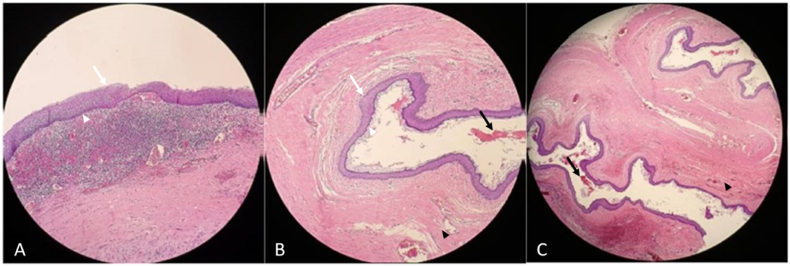
The mass was diagnosed as an epidermal inclusion cyst with secondary inflammation and suppuration. Histopathology (Fig. 2) shows that the cyst wall was lined by keratinizing stratified squamous epithelium with lamellated hyperkeratosis without adnexal structures. No atypia was noted. Areas of acute inflammation were evident. Skeletal muscle and fibrous tissue were also seen below the cyst lining. No hooklets or lamellated membranes were seen.
Fig. 2.
Epidermal inclusion cyst with secondary inflammation and suppuration on low-power microscopy (hematoxylin and eosin stain). (A, B) The cyst wall is lined with stratified squamous epithelium with no evidence of adnexal structure consistent with the epidermoid cyst (white arrow) with the inner wall showing a granular layer (white arrowhead). (B, C) The central lumen contains laminated keratin accumulation (black arrow) and skeletal muscle and fibrous tissue are seen below the cyst lining (black arrowhead).
3. Discussion
Epidermoid cysts are either congenital or acquired. The most accepted etiology is early intrauterine abnormal closure of the neural groove or epithelial fusion lines.3,4 These cystic lesions occur in the midline of any region from the cranium to the anus.4,5 Extratesticular epidermoid cysts are very rare, and they are extremely rare in the male pelvis.3,6,7 Gelderen et al. reported a case of an epidermoid cyst arising from the posterior aspect of the prostate and seminal vesicles. Symptoms on presentation were urinary retention associated with suprapubic fullness, and suprapubic tube insertion revealed “caseous material instead of urine”.7 Another case report described a scrotal epidermoid cyst attached to the anterior aspect of the seminal vesicles in the midline.8
Herein, the cyst originated from the left seminal vesicle and was rapidly growing, causing clinical symptoms of pressure on the bladder and left ureter. Pelvic MRI was the key to diagnosis to differentiate such cystic lesions from the full bladder and other pelvic cystic lesions. Ultrasound is not typically conclusive for central pelvic cystic lesions.7 Other important data from axial imaging MRI include the nature and extent of the lesion, its relation to important vessels and viscera, and its content. This imaging also provides surgeons with a surgical “road map”.7 Herein, open surgical exploration and excision were performed due to the large size of the mass. For this surgery, it is critical to identify the adjacent organs, such as the bladder, bowel, ureter, and iliac vessels, and to safely dissect those structures from the mass when it is tense. Next, aspirating the cyst content allowed careful dissection of hidden areas and organs from the cyst and the creation of sufficient space in the pelvis to safely remove such a large cyst.
4. Conclusion
Among other central pelvic cystic lesions, pelvic epidermoid cysts in men are challenging for diagnosis and treatment. Pelvic MRI is the gold standard for diagnosis and is essential to identify the relationship of the mass to the adjacent organs and to plan the surgical approach. Surgery should include safe surgical dissection of the mass to avoid organ or vessel injuries and good judgment regarding when to aspirate the cyst content to facilitate cyst dissection and excision.
Author contributions
Conceptualization, Abdulaziz M Almalki; Validation, S.O.A., Abdulaziz M Almalki, and M.A.A.; Investigation, S.O.A., Abdulaziz M Almalki, and M.A.A.; Resources, Abdulaziz M Almalki, and K.A.A.; Data curation, S.O.A., Abdulaziz M Almalki, and K.A.A.; Writing—original draft preparation, A.M.A., K.A.A., S.M.A., Arwa M Aljuhani, S.A.A and M.A.A.; Writing—review and editing, M.A.A.; Visualization, S.O.A., and Abdulaziz M Almalki; Supervision, S.O.A. Project administration, Abdulaziz M Almalki; Funding acquisition, S.O.A. All authors have read and agreed to the published version of the manuscript.
Informed consent
Written informed consent was obtained from the patient.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Declaration of competing interest
The authors declare no conflict of interest.
Acknowledgments
None.
Contributor Information
Siraj O. AlSulimani, Email: serajalsulimani@gmail.com.
Abdulaziz M. Almalki, Email: dr.almalki.uro@gmail.com.
Khalid A. Alzahrani, Email: khAlzahrani@outlook.com.
Samia M. Almutairi, Email: samia.almutairi@hotmail.com.
Arwa M. Aljuhani, Email: arwa.4aljuhani@outlook.com.
Sondos A. Alqahtani, Email: sno.s@hotmail.com.
Faisal A. Alruqi, Email: faisal17034@gmail.com.
Meshari A. Alzahrani, Email: ma.alzahrani@mu.edu.sa.
References
- 1.Jain P., Pal D.K. Pelvic epidermoid cyst: a rare cause of lower urinary tract symptoms. BMJ Case Rep. 2018;2018 doi: 10.1136/bcr-2017-223258. bcr2017223258. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Dahan H., Arrivé L., Wendum D., Docou le Pointe H., Djouhri H., Tubiana J.M. Retrorectal developmental cysts in adults: clinical and radiologic-histopathologic review, differential diagnosis, and treatment. Radiographics. 2001;21:575–584. doi: 10.1148/radiographics.21.3.g01ma13575. [DOI] [PubMed] [Google Scholar]
- 3.Lee S.J., Lee J.H., Jeon S.H., Kim M.J. Multiple epidermoid cysts arising from the extratesticular scrotal, spermatic cord and perineal area. Korean J Urol. 2010;51:505–507. doi: 10.4111/kju.2010.51.7.505. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Pear B.L. Epidermoid and dermoid sequestration cysts. Am J Roentgenol Radium Ther Nucl Med. 1970;110:148–155. doi: 10.2214/ajr.110.1.148. [DOI] [PubMed] [Google Scholar]
- 5.Suwa M., Takeda M., Bilim V., Takahashi K. Epidermoid cyst of the penis: a case report and review of the literature. Int J Urol. 2000;7:431–433. doi: 10.1046/j.1442-2042.2000.00219.x. [DOI] [PubMed] [Google Scholar]
- 6.Huang A., Palmer L.S., Levitt S.B. Epidermoid cyst of the scrotum extending into the true pelvis. Urology. 1999;54:561. doi: 10.1016/s0090-4295(99)00197-1. [DOI] [PubMed] [Google Scholar]
- 7.Van Gelderen W.F., Al-Hindawi M., Archibald C.G., Merrie A.E., Cheng K.S. Radiological imaging of a massive dermoid in the male pelvis. Australas Radiol. 1995;39:408–410. doi: 10.1111/j.1440-1673.1995.tb00324.x. [DOI] [PubMed] [Google Scholar]
- 8.Sağlam H.S., Kumsar S., Köse O., Adsan O. A unique scrotal extratesticular epidermod cyst attached to the seminal vesicles. Can Urol Assoc J. 2013;7:E244–E247. doi: 10.5489/cuaj.546. [DOI] [PMC free article] [PubMed] [Google Scholar]