Abstract
目的
探讨加速康复外科(enhanced recovery after surgery,ERAS)对高合并症患者人工全髋关节置换术(total hip arthroplasty,THA)术后功能及疼痛的影响。
方法
以2020年1月—2022年1月拟行THA患者作为研究对象,共223例高合并症患者符合选择标准纳入研究。采用随机信封法将患者分为两组,其中112例围术期按照ERAS方案处理(ERAS组),111例采用传统方案处理(对照组)。两组患者性别、年龄、身体质量指数、Charlson合并症指数以及术前诊断、合并症类型及数量、术前疼痛视觉模拟评分(VAS)等基线资料比较,差异均无统计学意义(P>0.05);但术前ERAS组Harris评分低于对照组,差异有统计学意义(P<0.05)。记录患者术前及术后住院时间。术前、术后1 d、术后首次下床、出院当天、术后2周,采用VAS评分评估疼痛程度;术前以及术后 2 周,1、3、6、12个月,采用Harris评分评价髋关节功能;记录患者术后1年内并发症及死亡发生率、30 d内再入院率以及患者满意度。
结果
ERAS组术前住院时间较对照组缩短(P<0.05),但术后住院时间差异无统计学意义(P>0.05)。两组患者均获随访12个月。两组组内术后VAS评分较术前降低,且随时间延长呈逐步下降趋势,各时间点间差异均有统计学意义(P<0.05);术后各时间点ERAS组VAS评分均低于对照组(P<0.05)。两组组内术后Harris评分均较术前提高,且随时间延长呈逐步增加趋势,各时间点间差异均有统计学意义(P<0.05);同时术后2周及1、3个月ERAS组Harris评分高于对照组,差异有统计学意义(P<0.05)。ERAS组2例(1.79%)、对照组6例(5.41%)发生并发症,并发症发生率差异无统计学意义(P>0.05)。对照组1例术后30 d内再入院、1例1年内因重症肺炎死亡,ERAS组无再入院及死亡患者;两组术后30 d内再入院率、1年内死亡率差异均无统计学意义(P>0.05)。末次随访时,ERAS组患者满意率高于对照组,但差异无统计学意义(P>0.05)。
结论
高合并症THA患者实施ERAS方案能缩短术前等待时间,更好地减轻患者疼痛,改善患者髋关节功能。
Keywords: 高合并症, 人工全髋关节置换术, 加速康复外科, 围术期
Abstract
Objective
To investigate the effects of enhanced recovery after surgery (ERAS) on postoperative function and pain in total hip arthroplasty (THA) patients with high comorbidity.
Methods
Patients with THA who were admitted between January 2020 and January 2022 were selected as the study objects, and a total of 223 patients with high comorbidity met the selection criteria. Patients were randomly divided into two groups using the random envelope method. During perioperative period, 112 cases in the ERAS group were treated according to the ERAS protocol and 111 cases in the control group with the traditional protocol. There was no significant difference in gender, age, body mass index, Charlson comorbidity index, preoperative diagnosis, the type and number of the comorbidities, preoperative visual analogue scale (VAS) score between the two groups (P>0.05). However, the Harris score of ERAS group was significantly lower than that of control group before operation (P<0.05). Preoperative and postoperative hospital stays were recorded. The VAS score was used to evaluate the pain before operation, at 1 day after operation, at the leaving bed time, at the day after discharge, and at 2 weeks after operation. Harris score was used to evaluate hip function before operation and at 2 weeks, 1 month, 3 months, 6 months, and 12 months after operation. The incidence of complications, 30-day readmission rate, mortality rate, and patient’s satisfaction were recorded.
Results
The length of preoperative hospital stay in ERAS group was significantly shorter than that in control group (P<0.05). But there was no significant difference in the length of postoperative hospital stay between groups (P>0.05). All patients in the two groups were followed up 12 months. The VAS score in the two groups after operation was lower than that before operation, and showed a gradually trend with the extension of time, with significant differences between different time points (P<0.05). VAS scores of ERAS group were significantly lower than those of control group at different time points after operation (P<0.05). The postoperative Harris scores in both groups were higher than those before operation, and showed a gradually increasing trend with the extension of time, with significant differences between different time points (P<0.05). Harris scores of ERAS group at 2 weeks, 1 month, and 3 months after operation were significantly higher than those of control group (P<0.05). Complications occurred in 2 cases (1.79%) of the ERAS group and 6 cases (5.41%) of the control group, with no significant difference in incidence (P>0.05). In the control group, 1 case was readmitted within 30 days after operation, and 1 case died of severe pneumonia within 1 year of follow-up. There was no readmission or death in ERAS group, and there was no significant difference in the above indexes between the two groups (P>0.05). At last follow-up, the satisfaction rate of patients in ERAS group was slightly higher than that in control group, but the difference was not significant (P>0.05).
Conclusion
For THA patients with high comorbidity, ERAS protocol can shorten preoperative waiting time, better reduce pain, and improve hip function.
Keywords: High comorbidity, total hip arthroplasty, enhanced recovery after surgery, perioperative period
随着人口寿命延长,骨关节炎患者日渐增多,因此接受人工关节置换术治疗的患者也不断增加[1-2]。人工关节置换术可以有效改善终末期关节疾病患者的生活质量,但此类患者大多为老年人,常合并1种或多种慢性疾病,国外一项研究显示接受人工髋关节或膝关节置换术的患者中83.7%存在合并症[3],而合并症可能影响置换手术疗效[4-5]。因此,术者需重视人工关节置换术患者的合并症。目前,临床采用Charlson合并症指数(Charlson comorbidity index,CCI)评估患者合并症的严重程度,对不同合并症赋予相应分值,分值总和即为CCI,如CCI≥3则判定为高合并症患者[2]。
加速康复外科(enhanced recovery after surgery,ERAS)是经循证医学证据证明的有效围术期处理措施,能降低人工全髋关节置换术(total hip arthroplasty,THA)创伤应激反应、减少并发症、提高手术安全性,缩短平均住院时间、改善预后,从而达到快速康复、提高患者满意度的目的[6-13]。但是上述研究大多基于整体患者,对于高合并症患者是否仍具有积极影响,相关文献报道较少。为此,我们进行了一项前瞻性临床对比研究,探讨ERAS用于高合并症患者THA的有效性。报告如下。
1. 临床资料
1.1. 一般资料
患者纳入标准:① 收治且接受单侧初次THA,由同一主任医师完成手术;② 术前CCI≥3;③ 患者知情同意治疗方案且配合随访研究。排除标准:① 合并凝血功能障碍或下肢深静脉血栓形成;② 存在局部感染灶;③ 存在影响术后髋关节功能评定的其他疾病。
2020年1月—2022年1月,共223例患者符合选择标准纳入研究。采用随机信封法将患者分为两组,其中112例围术期按照ERAS方案处理(ERAS组),111例采用传统方案处理(对照组)。两组患者性别、年龄、身体质量指数、CCI以及术前诊断、合并症类型及数量、术前疼痛视觉模拟评分(VAS)等基线资料比较,差异均无统计学意义(P>0.05)。但术前ERAS组Harris评分低于对照组,差异有统计学意义(P<0.05)。见表1。
表 1.
Comparison of baseline data between groups
两组患者基线资料比较
| 基线资料 Baseline data |
ERAS组 ERAS group |
对照组 Control group |
统计量 Statistical value |
P值 P value |
年龄(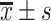 ,岁) ,岁) |
66.9±7.6 | 66.6±7.6 | t=0.275 | 0.783 |
| 性别(男/女,例) | 74/38 | 64/47 | χ2=1.673 | 0.196 |
身体质量指数(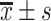 , kg/m2) , kg/m2) |
23.77±3.12 | 23.32±3.09 | t=1.082 | 0.280 |
| CCI [M(Q1,Q3)] | 4(3,5) | 4(3,5) | Z=–0.551 | 0.582 |
| 术前诊断 (骨关节炎/股骨颈骨折/股骨头坏死/炎性髋关节病/ 髋关节发育不良,例) |
56/25/11/14/6 | 53/23/10/17/8 | χ2=0.785 | 0.940 |
| 术前合并症类型 [心力衰竭/周围血管疾病/心、脑血管疾病/慢性肺部疾病/消化性溃疡/肝功能异常/偏瘫/肾功能异常/糖尿病(不伴合并症)/糖尿病(伴合并症),例] | 34/19/89/83/36/ 27/69/12/38/22 |
38/21/85/87/29/ 30/73/10/35/19 |
χ2=2.053 | 0.991 |
| 术前合并症数量(2种/3种/4种/5种,例) | 38/65/22/14 | 35/67/19/16 | χ2=0.492 | 0.921 |
| 术前Harris评分 [M(Q1,Q3),分] | 49(45,52) | 51(48,54) | Z=−2.658 | 0.008 |
| 术前VAS评分 [M(Q1,Q3),分] | 5(5,6) | 5(5,6) | Z=−0.243 | 0.808 |
1.2. 治疗方法
1.2.1. 手术方法
两组手术方法一致。患者采用椎管内麻醉,取后外侧入路。3例采用骨水泥型假体(ERAS组1例、对照组2例),均为美国史塞克公司假体;220例采用非骨水泥型假体(ERAS组111例、对照组109例),其中美国史塞克公司假体181例、美国强生公司假体39例。
1.2.2. 围术期处理方法
ERAS组:① 健康宣教:指导患者心理及心肺功能锻炼,详细介绍ERAS理念及流程、围术期注意事项。② 营养支持:指导患者高蛋白饮食,必要时营养科会诊配置营养餐。③ 血液管理:如患者血红蛋白(hemoglobin,Hb)<70 g/L时输注红细胞;70~120 g/L时应用重组人促红细胞生成素联合蔗糖铁,具体为术前3 d开始应用重组人促红细胞生成素 150 U/kg、静脉补充蔗糖铁100 mg,每周3次,持续至术后出院。术中常规使用止血药,切开皮肤时静脉滴注氨甲环酸1 g,关闭切口时局部应用氨甲环酸1 g。④ 镇痛及麻醉管理:术前3 d采用超前镇痛;术中选用椎管内麻醉,控制性降压;术后多模式镇痛方案。⑤ 导管管理:术中常规不留置尿管;术后24 h内尽早去除引流管及其他各种导管。⑥ 抗凝治疗:术后8 h开始给予低分子肝素4 000~6 000 U/d,出院后改为口服利伐沙班10 mg/d,持续2周。⑦ 功能锻炼:术后6 h在康复技师指导下开始锻炼,待引流管拔除后试行床边坐位过渡至下地站立,如无不适后即在助行器协助下下床活动等。
对照组:术前30 min静脉滴注氨甲环酸1 g,术中置导尿管并于术后24 h内拔除,出院时告知锻炼方式及禁止事项。
1.3. 疗效评价指标
记录患者术前以及术后住院时间,出院标准[13]:切口正常愈合,口服止痛药物效果满意,助行器辅助安全行走,知道并能够进行正确功能锻炼,生活基本自理,愿意并且接受出院。
术前、术后1 d、术后首次下床、出院当天、术后2周,采用VAS评分评估疼痛程度;术前以及术后 2 周,1、3、6、12个月,采用Harris评分评价髋关节功能;记录患者术后1年内并发症及死亡发生率、30 d内再入院率以及患者满意度(满意、不满意)。
1.4. 统计学方法
采用SPSS21.0统计软件进行分析。计量资料行正态性检验,如符合正态分布,以均数±标准差表示,组间比较采用独立样本t检验;不符合正态分布,以M(Q1,Q3)表示,两组多时间点比较选择广义估计方程,组间比较采用Mann-Whitney U检验。计数资料组间比较采用χ2检验或Fisher确切概率法。检验水准α=0.05。
2. 结果
ERAS组术前住院时间较对照组缩短,差异有统计学意义(P<0.05),但两组术后住院时间差异无统计学意义(P>0.05)。除对照组1例于术后12个月死亡外,其余两组患者均获随访12个月。
两组组内术后VAS评分较均术前降低,且随时间延长呈逐步下降趋势,各时间点间差异均有统计学意义(P<0.05)。ERAS组术后各时间点VAS评分均低于对照组,差异均有统计学意义(P<0.05)。见图1。
图 1.
Change trends of VAS scores in the two groups
两组VAS评分变化趋势
两组组内术后Harris评分均较术前提高,且随时间延长呈逐步增加趋势,各时间点间差异均有统计学意义(P<0.05)。ERAS组术后2周及1、3个月 Harris评分高于对照组,差异有统计学意义(P<0.05);但术后6、12个月组间差异无统计学意义(P>0.05)。见图2。
图 2.
Change trends of Harris scores in the two groups
两组Harris评分变化趋势
术后1年内并发症发生情况:ERAS组2例(1.79%)、对照组6例(5.41%)发生并发症,发生率差异无统计学意义(P>0.05)。其中,ERAS组术后8 d发现切口感染1例、10 d发现下肢深静脉血栓形成1例,对照组术后5 d发生低钠血症 1 例、7 d发现切口感染1例、22 d发生髋关节脱位1例、1个月内下肢深静脉血栓形成3例。下肢深静脉血栓形成患者于血管外科治疗后痊愈;切口感染患者给予口服抗生素及换药处理后愈合,未发展为关节内感染;低钠血症患者给予口服药物治疗后纠正;髋关节脱位患者再入院手法复位、下肢皮牵引2周,随访期间未发生再次脱位。
对照组1例术后30 d内再入院,为上述髋关节脱位患者;1例术后12个月因重症肺炎死亡。ERAS组无术后30 d 内再入院及死亡患者。两组术后30 d内再入院率以及术后1年内死亡率差异无统计学意义(P>0.05)。末次随访时,两组患者满意率差异无统计学意义(P>0.05)。见表2。
表 2.
Comparison of outcome indicators between the two groups
两组结局指标比较
| 指标 Indicator |
ERAS组(n=112) ERAS group (n=112) |
对照组(n=111) Control group (n=111) |
效应值(95%CI) Effect value (95%CI) |
P值 P value |
| 术前住院时间 [M(Q1,Q3),d] | 3(3,4) | 4(3,4) | MD=0(−1,0) | <0.001 |
| 术后住院时间 [M(Q1,Q3),d] | 5(4,6) | 5(5,6) | MD=0(0,0) | 0.056 |
| 术后1年内并发症(发生/不发生,例) | 2/110 | 6/105 | RR=0.318(0.063,1.612) | 0.146 |
| 术后30 d内再入院(发生/不发生,例) | 0/112 | 1/110 | RR=2.018(1.767,2.305) | 0.498 |
| 术后1年内死亡(发生/不发生,例) | 0/112 | 1/110 | RR=2.018(1.767,2.305) | 0.498 |
| 患者满意度(满意/不满意,例) | 105/7 | 98/13 | RR=1.990(0.762,5.193) | 0.154 |
3. 讨论
手术延迟会增加骨科手术术后并发症、死亡率和成本[14]。研究发现CCI每增加1分,THA手术延迟风险增加52%,进而导致并发症发生率增高[15]。ERAS方案则能减少关节置换患者术后并发症发生率,缩短住院时间,改善预后[16-18]。本研究结果也发现高合并症 THA 患者围术期应用 ERAS 方案后术前等待时间缩短,不增加并发症发生率,提示ERAS方案对降低入院后手术延迟率有积极影响;但是对术后住院时间无明显优势。
再入院会增加患者医疗费用[19],临床可采用CCI评估关节成形术、手和上肢手术、脊柱手术和创伤手术后再入院风险[20],高合并症意味着高再入院率。既往研究报道ERAS方案对术后30 d内再入院率无显著影响[21]。本研究中仅对照组1例因髋关节脱位于术后30 d内再入院, 进一步验证ERAS方案在此方面无明显优势。
随着关节置换技术的发展,置换术后患者死亡率从1997年的1%下降至2011年的0.6%[22],但对于中等或较高合并症患者其死亡率风险没有下降[2]。Kreder等[23]发现与无合并症患者相比,存在合并症的患者死亡率增加了24倍。研究显示ERAS方案能显著降低关节置换患者死亡率[11]。本研究中对照组1例患者死亡,ERAS组无患者死亡,但组间差异无统计学意义,提示ERAS方案在高合并症THA患者死亡率方面无明显优势。此外,由于ERAS方案的应用使患者卧床时间缩短,也减少了并发症的发生,促进了患者康复锻炼进度,在患者对手术满意度方面有积极作用。本研究ERAS组患者满意度相较对照组无明显优势,可能与样本量较少有一定关系,有待扩大样本量进一步明确。
综上述,高合并症患者THA围术期实施ERAS方案能有效减轻患者疼痛,缩短术前等待时间,有利于髋关节功能康复。但本研究存在以下局限性:① 仅纳入初次单侧置换患者;② 患者例数有限;③ 随访时间短。因此,ERAS方案在关节翻修和双髋置换患者中的应用效果以及对远期疗效的影响,均有待进一步研究。
利益冲突 在课题研究和文章撰写过程中不存在利益冲突;经费支持没有影响文章观点和对研究数据客观结果的统计分析及其报道
伦理声明 研究方案经德阳市人民医院伦理委员会批准(2020-04-040-K01)
作者贡献声明 兰平文:研究设计、数据分析及文章撰写;张明、刘海龙、邓富元:临床数据收集;张建军:文章审校
Funding Statement
德阳市科技计划项目(19SZ040);四川省卫生健康委员会科研课题(20PJ249)
Science and Technology Project of Deyang City (19SZ040); Research Project of Sichuan Provincial Health Commission (20PJ249)
References
- 1.Bülow E, Rolfson O, Cnudde P, et al Comorbidity does not predict long-term mortality after total hip arthroplasty. Acta Orthop. 2017;88(5):472–477. doi: 10.1080/17453674.2017.1341243. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Glassou EN, Pedersen AB, Hansen TB. Is decreasing mortality in total hip and knee arthroplasty patients dependent on patients’ comorbidity? Acta Orthop, 2017, 88(3): 288-293.
- 3.Hustedt JW, Goltzer O, Bohl DD, et al Calculating the cost and risk of comorbidities in total joint arthroplasty in the United States. J Arthroplasty. 2017;32(2):355–361. doi: 10.1016/j.arth.2016.07.025. [DOI] [PubMed] [Google Scholar]
- 4.Ritter MA, Albohm MJ, Keating EM, et al Comparative outcomes of total joint arthroplasty. J Arthroplasty. 1995;10(6):737–741. doi: 10.1016/S0883-5403(05)80068-3. [DOI] [PubMed] [Google Scholar]
- 5.Ethgen O, Bruyère O, Richy F, et al Health-related quality of life in total hip and total knee arthroplasty. A qualitative and systematic review of the literature. J Bone Joint Surg (Am) 2004;86(5):963–974. doi: 10.2106/00004623-200405000-00012. [DOI] [PubMed] [Google Scholar]
- 6.Christelis N, Wallace S, Sage CE, et al An enhanced recovery after surgery program for hip and knee arthroplasty. Med J Aust. 2015;202(7):363–368. doi: 10.5694/mja14.00601. [DOI] [PubMed] [Google Scholar]
- 7.Chiung-Jui Su D, Yuan KS, Weng SF, et al Can early rehabilitation after total hip arthroplasty reduce its major complications and medical expenses? Report from a nationally representative cohort. Biomed Res Int. 2015;2015:641958. doi: 10.1155/2015/641958. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Van Egmond JC, Verburg H, Mathijssen NM The first 6 weeks of recovery after total knee arthroplasty with fast track. Acta Orthop. 2015;86(6):708–713. doi: 10.3109/17453674.2015.1081356. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Di Martino A, Brunello M, Pederiva D, et al Fast track protocols and early rehabilitation after surgery in total hip arthroplasty: A narrative review. Clin Pract. 2023;13(3):569–582. doi: 10.3390/clinpract13030052. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Vendittoli PA, Pellei K, Desmeules F, et al Enhanced recovery short-stay hip and knee joint replacement program improves patients outcomes while reducing hospital costs. Orthop Traumatol Surg Res. 2019;105(7):1237–1243. doi: 10.1016/j.otsr.2019.08.013. [DOI] [PubMed] [Google Scholar]
- 11.Deng QF, Gu HY, Peng WY, et al Impact of enhanced recovery after surgery on postoperative recovery after joint arthroplasty: results from a systematic review and meta-analysis. Postgrad Med J. 2018;94(1118):678–693. doi: 10.1136/postgradmedj-2018-136166. [DOI] [PubMed] [Google Scholar]
- 12.白伟侠, 卢连君, 田晓霞, 等 老年人全髋关节置换围手术期快速康复护理. 中国矫形外科杂志. 2020;28(11):928–932. [Google Scholar]
- 13.欧阳鹏辉, 黄宇, 刘文辉, 等 快速康复外科理念在老年患者全髋关节置换术中的应用效果探讨. 中国临床新医学. 2020;13(3):244–249. doi: 10.3969/j.issn.1674-3806.2020.03.08. [DOI] [Google Scholar]
- 14.Cantu RV, Graves SC, Spratt KF In-hospital mortality from femoral shaft fracture depends on the initial delay to fracture fixation and Injury Severity Score: a retrospective cohort study from the NTDB 2002-2006. J Trauma Acute Care Surg. 2014;76(6):1433–1440. doi: 10.1097/TA.0000000000000230. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Phruetthiphat OA, Gao Y, Anthony CA, et al Incidence of and preoperative risk factors for surgical delay in primary total hip arthroplasty: Analysis from the american college of surgeons national surgical quality improvement program. J Arthroplasty. 2016;31(11):2432–2436. doi: 10.1016/j.arth.2016.05.054. [DOI] [PubMed] [Google Scholar]
- 16.Ripollés-Melchor J, Abad-Motos A, Díez-Remesal Y, et al Association between use of enhanced recovery after surgery protocol and postoperative complications in total hip and knee arthroplasty in the postoperative outcomes within enhanced recovery after surgery protocol in elective total hip and knee arthroplasty study (POWER2) JAMA Surg. 2020;155(4):e196024. doi: 10.1001/jamasurg.2019.6024. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Khan SK, Malviya A, Muller SD, et al Reduced short-term complications and mortality following Enhanced Recovery primary hip and knee arthroplasty: results from 6,000 consecutive procedures. Acta Orthop. 2014;85(1):26–31. doi: 10.3109/17453674.2013.874925. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Li J, Zhu H, Liao R Enhanced recovery after surgery (ERAS) pathway for primary hip and knee arthroplasty: study protocol for a randomized controlled trial. Trials. 2019;20(1):599. doi: 10.1186/s13063-019-3706-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Wurtz LD, Feinberg JR, Capello WN, et al Elective primary total hip arthroplasty in octogenarians. J Gerontol A Biol Sci Med Sci. 2003;58(5):M468–M471. doi: 10.1093/gerona/58.5.M468. [DOI] [PubMed] [Google Scholar]
- 20.Bjorgul K, Novicoff WM, Saleh KJ Evaluating comorbidities in total hip and knee arthroplasty: available instruments. J Orthop Traumatol. 2010;11(4):203–209. doi: 10.1007/s10195-010-0115-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Zhu S, Qian W, Jiang C, et al Enhanced recovery after surgery for hip and knee arthroplasty: a systematic review and meta-analysis. Postgrad Med J. 2017;93(1106):736–742. doi: 10.1136/postgradmedj-2017-134991. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Pedersen AB, Mehnert F, Sorensen HT, et al The risk of venous thromboembolism, myocardial infarction, stroke, major bleeding and death in patients undergoing total hip and knee replacement: a 15-year retrospective cohort study of routine clinical practice. Bone Joint J. 2014;96-B(4):479–485. doi: 10.1302/0301-620X.96B4.33209. [DOI] [PubMed] [Google Scholar]
- 23.Kreder HJ, Grosso P, Williams JI, et al Provider volume and other predictors of outcome after total knee arthroplasty: a population study in Ontario. Can J Surg. 2003;46(1):15–22. [PMC free article] [PubMed] [Google Scholar]




