Abstract
BACKGROUND
Cervical spondyloptosis is a serious condition scarcely encountered by spine surgeons. Few cases have been reported in the literature. There are no general guidelines for their management, especially in delayed cases. The authors describe their surgical technique for the management of cervical spondyloptosis 45 days after the trauma.
OBSERVATIONS
A 28-year-old patient was admitted 45 days after head and cervical trauma leading to quadriplegia with muscular strength at the C5 level. Cervical computed tomography scanning and magnetic resonance imaging revealed C6–7 spondyloptosis with complete slippage of the C6 vertebral body in front of C7. Posterior and anterior cervical spine approaches during the same surgery allowed decompression and stabilization, leading to a dramatic improvement in the neurological deficit. The patient was able to walk 18 months later with near normal balance.
LESSONS
Traumatic cervical spondyloptosis requires early management to increase the possibility of decompression through anatomical realignment and stabilization. In delayed cases, a combined anterior and posterior cervical spine approach according to our technique allows decompression and stabilization with a good postoperative outcome possible.
Keywords: spondyloptosis, spinal cord, cervical spine, vertebral artery, trauma, surgery
ABBREVIATIONS: ASIA = American Spinal Injury Association, CT = computed tomography, MRI = magnetic resonance imaging
Cervical spondyloptosis is a very rare condition and describes total slippage of vertebral bodies anteriorly or posteriorly to another one.1–3 Only 29 cases have been reported in the English-language literature. The condition usually results from high velocity trauma, and its management is challenging regardless of whether the patient is neurologically intact.4 A surgical approach remains the cornerstone of treatment in these patients and aims at decompression, realignment, and stabilization, especially in cases of recent trauma. However, realignment in delayed cases requires caution because of a physiological consolidation on a spondyloptotic spine. Thus, a closed or intraoperative reduction presents a high risk of spinal cord and vertebral artery injury. Herein, we describe a patient with complete telescoping of the C6 vertebral body in front of C7, who was admitted to our institution 45 days after a road traffic accident.
Illustrative Case
A 28-year-old male without a remarkable past medical history was admitted to our department for posttraumatic quadriplegia that had occurred 45 days earlier. He was a helmeted motorcycle driver who experienced a fall during excessive speed in an attempt to avoid an obstacle. His head hit the road violently with an immediate loss of consciousness. He had previously been managed at another institution where radiological imaging revealed cerebral contusion associated with C6–7 spondyloptosis. He woke from a coma a few days later but remained quadriplegic with an American Spinal Injury Association (ASIA) grade A (complete sensory and motor function along the C5 level). Because of the modest technical capabilities and lack of a neurosurgeon at the institution, no specific treatment was suggested for the cervical spine dislocation apart from a rigid cervical collar. Thus, 45 days later the patient was sent to our department for further management. On admission, neurological examination revealed ASIA grade A corresponding to a complete C5 motor level with 1/5 strength in the bilateral biceps and triceps. His sensation was diminished to light touch and pinprick along and below the dermatome of C5, C6, and C7, with brisk jerk of the extensor plantar reflexes and a bilateral Hoffman’s sign. There was also dysphagia and dysphonia. Cervical computed tomography (CT) and magnetic resonance imaging (MRI) showed the persistence of spondyloptosis with a winding, pinched spinal cord at the level of C5, C6, and C7. Intramedullary hyperintensity on T2-weighted images was shown at the level of the dislocation (Fig. 1). Vertebral arteries as well as main cervical vessels were normal and patent on CT angiography (Fig. 2). Because of the extended time from the trauma and the risk of spinal cord injury by a sudden realignment due to a brisk disruption of the bony bridge of consolidation, we did not attempt a closed reduction. A surgical approach with a combination of posterior laminectomy followed by an anterior corporectomy was suggested. Exposure of the bony elements demonstrated a C6 lamina fracture. Laminectomy was performed beyond the limit of the dislocation above and below C6 (C4, C5, C6, and C7) to avoid traction or a winding shape of the spinal cord. Careful intraoperative traction was applied to attempt realignment, but no mobility was noticed, forecasting the beginning of consolidation between the dislocated vertebrae. On a bone window CT scan, there was no consolidation between facets, and this made us believe that the consolidation should be between the bodies of C6 and C7. However, laminectomy allowed decompression of the spinal cord, which returned to a near normal shape.
FIG. 1.

Cervical CT (A–C) and short tau inversion recovery MRI (D) showing complete slippage of C6 in front of C7 and a winding, pinched spinal cord with intramedullary hyperintensity. Note that C6 facet joints were jumped and locked over the C7 facet joints (right facet, A; left facet, B).
FIG. 2.

Preoperative CT angiography showing patency of the vertebral arteries (left vertebral artery, A; right vertebral artery, B).
Then the patient was placed supine, and an anterior approach was performed. A second attempt at intraoperative reduction either by traction or by Caspar retractor did not allow slight mobility of the spine. Thus, a C6 and C7 corporectomy was done with an iliac bone graft and C5–T1 plate fixation (Fig. 3). After 10 hours, the surgical procedure from the beginning of the posterior approach to the end of the anterior approach was completed. The postoperative period was uneventful, and frank improvement was noticed. Dysphagia and dysphonia disappeared within 2 days, which made us suspect that these symptoms occurred as the result of tracheal and esophageal compression by the dislocated cervical spine beyond C7, and muscular strength increased to 3/5 during the first week. The patient was discharged at hospital day 10 and was referred to the physical therapy department. At the 12-month follow-up, the patient was able to stand up without support and to walk but with obvious disbalance (Video 1). After 18 months, he had an ASIA grade E and was able to walk without any support. His gait was still normal 3 years postoperatively, with mild spasticity (Video 2).
FIG. 3.
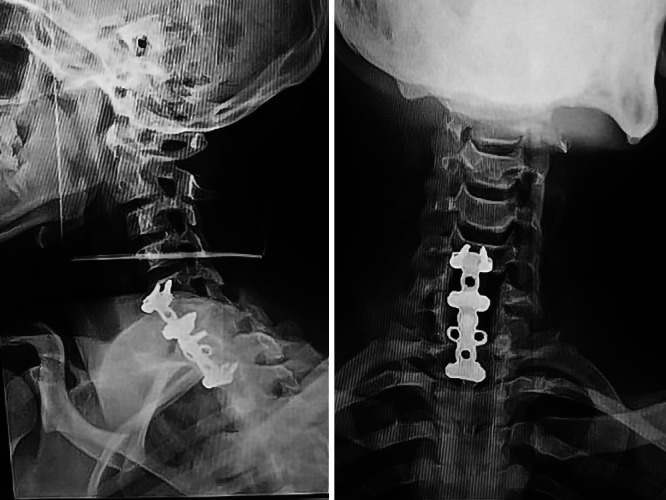
Postoperative radiographs.
VIDEO 1. Clip showing the patient at the 12-month postoperative follow-up. Click here to view.
VIDEO 2. Clip showing the patient at the 3-year follow-up. The patient has been walking without any support since 18 months postoperatively. Click here to view.
Patient Informed Consent
The necessary patient informed consent was obtained in this study.
Discussion
Observations
Neugebaeur first described spondyloptosis in 1882, and since then, it has most often been encountered in the lumbar spine.5 The first reported cases of cervical spine spondyloptosis appeared in 1951, and none were traumatic.6 It was only in 1992 that Bhojraj et al. revealed the first case of traumatic cervical spondyloptosis, and to date, 29 cases can be found in the English-language literature (Table 1).5,7 Most of these patients were managed in the early stage or refused surgery when they were seen after a delayed period. Herein, we describe the surgical management of delayed traumatic cervical spondyloptosis at the C6–7 level. As spondyloptosis represents the last grade of dislocation, it is commonly associated with spinal cord compression and thus requires decompression, realignment, and stabilization.4 This realignment can be done through closed reduction by traction or open reduction either when traction fails or neurological complication appears during this procedure.8 This complication can result from disc herniation, overdistraction, spinal cord edema, or a more rostral noncontiguous injury.4,8,9 Delayed dislocation displays various degrees of consolidation between the dislocated vertebrae. This increases the risk of neurological complication during closed reduction by a brisk rupture of this misalignment consolidation under the incremental weight of the traction. This potential event made us choose an open reduction. There is no consensus in the literature for the surgical management of cervical spondyloptosis.10 Some authors have used a single anterior or posterior approach for decompression, realignment, and instrumentation.10,11 Others have used combined approaches in the same surgery (anterior then posterior, posterior then anterior, or anterior then posterior then anterior).9 We first chose a posterior laminectomy (C5, C6, C7) to decompress the spinal cord and suppress its winding shape, then to try a reduction after resection of the C6 articular facets. Indeed, the spinal cord returned to near normal lordosis after the laminectomy. The closeness of the vertebral arteries to the dislocated articular facets (Fig. 2) exposed them to a high risk of injury during facectomy.12 We did not perform facectomy in our case given the concern that there was a lack of slight mobility under careful traction after the laminectomy despite the appearance of any consolidation between dislocated facets on bone window CT (Fig. 1A and B), resulting in a high probability of consolidation of the body of C6 and C7. The fracture of the posterior elements (pedicle and lamina) is supposed to prevent the spinal cord from great compression.4,8,13 However, fracture of the C6 lamina in our patient did not preclude the winding shape of the spinal cord associated with an intramedullary hyperintensity on T2-weighted images, which was seen 45 days after the trauma. This highlighted the violence of the trauma and the importance of compression on the spinal cord. The second step of our surgery was the anterior approach with a C6 and C7 corporectomy to optimize spinal cord decompression, followed by iliac crest graft fusion and instrumentation. Therefore, we suggest that in delayed cervical spondyloptosis, a balance between the benefits and the risks of an anatomical reduction of the dislocation and injury to the spinal cord or vertebral arteries must be made. Two authors attempted in situ noninstrumented fusion through a single anterior approach; however, postoperative bed rest of 8 to 12 weeks was necessary.7,13 In our case, in situ fusion after the C6 and C7 corporectomy with instrumentation was chosen for early mobilization of the patient to prevent bedsores and begin physical therapy. We suggest a previous laminectomy for posterior decompression to prevent the risk of spinal cord injury during the anterior approach.
TABLE 1.
Literature review of posttraumatic cervical spondyloptosis
| Case No. | Authors & Year | Age (yrs)/Sex | Injury Event | Preop Symptoms | Delay | Imaging | Approach | FU & Outcome |
|---|---|---|---|---|---|---|---|---|
| 1 | Bhojraj & Shahane, 19927 | 8/F | Congenital (home birth: full vaginal delivery w/ breech presentation) | ASIA C | 6 mos | C6–7 | Ant C6 & C7 corporectomy w/in situ fixation | ASIA D at 3 mos, stand & walk independently w/ minimal support |
| 2 | Menku et al., 20049 | 35/M | Not mentioned | ASIA E | Not mentioned | C6–7 | Ant approach + instrumentation + pst instrumentation | ASIA E |
| 3 | Shah & Rajshekhar, 200413 | 40/M | Fall from height (20 ft) | ASIA D | 7 days | C7–T1 | Ant approach (C6 & C7) + tricortical iliac crest bone graft w/o instrumentation | ASIA E at 5-mo FU |
| 4 | Tumialán et al., 20094 | 48/M | Rollover motor vehicle accident | ASIA E | Immediate | C7–T1 | Closed reduction + ant fusion + pst instrumentation | ASIA E |
| 5 | Dahdaleh et al., 201311 | 61/M | Motor vehicle accident | ASIA C | Immediate | C7–T1 | Closed reduction + pst instrumentation | ASIA C (diagnosis w/ lung adenocarcinoma stage IV & died shortly) |
| 6 | 48/F | Fall off staircase (intoxicated) | ASIAC | Immediate | C6–7 (epidural hematoma) | Ant approach & fusion | ASIA D postop, ASIA E at 12-mo FU | |
| 7 | 51/M | Motor vehicle accident (self extrication) | ASIA E | Immediate | C7–T1 | Closed reduction + pst instrumentation | ASIA E | |
| 8 | 48/M | Motor vehicle accident | ASIA C | Immediate | C6–7 | Closed reduction + pst instrumentation | ASIA E at 5-yr FU | |
| 9 | 42/M | Motorcycle accident | ASIA C | Immediate | C7–T1 | Closed reduction + pst instrumentation | ASIA D | |
| 10 | Dhall & Sribnick, 201410 | 28/F | Fall from 2nd floor balcony | ASIA B | Not mentioned | C6–7 | Failure of closed reduction, pst approach + instrumentation | ASIA B postop at discharge, ASIA D at 6-mo FU, ASIA E |
| 11 | Manjila et al., 20145 | 39/M | Motorcycle accident | ASIA A | Immediate | C2–3 lat spondyloptosis + VA injury (bypass) | Pst + posterolat + ant approach | ASIA A at 22-mo FU |
| 12 | Modi et al., 20168 | 35/M | Not mentioned | ASIA A | — | C6–7 | Closed reduction + ant approach + fusion | ASIA A |
| 13 | 8/M | ASIA A | Old injury w/ in situ fusion | C7–T1 | Patient treated conservatively (patient not willing to have surgery) | ASIA A (severe spasticity w/ multiple bed sores & totally dependent) | ||
| 14 | 70/M | C7–T1 | Closed reduction (not operated on due to comorbidities) | Died of multisystem failure | ||||
| 15 | Padwal et al., 20163 | 50/F | Fall of heavy object over head | ASIA C | 8 hrs | C6–7 | Closed reduction + ant approach + fusion | ASIA D postop, ASIA E at 24-mo FU |
| 16 | 40/M | Road traffic accident | ASIA C | Not mentioned | C7–T1 | Closed reduction + ant approach + fusion + pst approach w/ instrumentation | ASIA C postop, ASIA D at 15-mo FU | |
| 17 | 40/M | Road traffic accident | ASIA D | Not mentioned | C7–T1 | Closed reduction + ant approach + fusion + pst approach w/ instrumentation | ASIA D post op, FU not available | |
| 18 | 45/M | Fall from bullock cart | ASIA E | Not mentioned | C6–7 | Closed reduction + ant approach + fusion | ASIA E postop, FU not available | |
| 19 | 64/M | Fall from height | ASIA D | Not mentioned | C6–7 | Closed reduction + ant approach + fusion + pst approach w/ instrumentation | ASIA E at 4-mo FU | |
| 20 | 24/M | Fall from height due to electrocution | ASIA D | Not mentioned | C6–7 | Closed reduction + ant approach + fusion + pst approach w/ instrumentation | ASIA D postop, ASIA E at 6-mo FU | |
| 21 | 45/M | Fall w/ load over head | ASIA C | Not mentioned | C6–7 | Closed reduction + ant approach+ fusion | ASIA D postop | |
| 22 | 55/M | Fall w/ load over head | ASIA E | Not mentioned | C6–7 | Refuse surgery | Not available | |
| 23 | Wong et al., 201712 | 49/F | Motor vehicle accident | ASIA A | Not mentioned | C5–6 | Closed reduction + ant approach + fusion | ASIA A at 6-mo FU (postop angiography showed lt VA dissection treated w/ aspirin) |
| 24 | Feigenbaum et al., 199714 | 15/F | Motor vehicle accident | ASIA A | 3 wks | C5–6 (pst dislocation) + pseudotraumatic aneurysm of lt VA | Ant approach | ASIA A at 7 mos |
| 25 | Kim et al., 20192 | 60/M | Fall | ASIA A | 1 day | C7–T1 | Pst approach + instrumentation | ASIA D |
| 26 | 39/M | Diving + wrong maneuver during rehabilitation | ASIA D | 14 hrs | C7–T1 | Pst approach + instrumentation | ASIA E | |
| 27 | Tsujimoto et al., 20201 | 69/M | Motor vehicle accident | ASIA B | 6 hrs | C6–7 | Pst approach + instrumentation | ASIA D |
| 28 | 73/M | Fall from height (1 m) | ASIA D | 5 hrs | C7–T1 | Preop closed reduction on Mayfield head holder under general anesthesia + pst approach + instrumentation | ASIA E at 6-mo FU | |
| 29 | Alharbi et al., 202215 | 56/M | Motor vehicle accident | ASIA E | Not mentioned | C7–T1 | Pst approach reduction +ant approach + instrumentation (pst + ant) | ASIA E |
| 30 | Present Case | 28/M | Motorcycle accident | ASIA A | 45 days (still ASIA A w/ muscular strength 1/5 at C5 level) | C6–7 | Pst approach (C4–7 laminectomy) + ant approach (C6 & C7 corporectomy) + instrumentation | ASIA E at 18-mo FU |
ant = anterior; FU = follow-up; pst = posterior; VA = vertebral artery.
Lessons
Cervical spondyloptosis is a rare and devastating dislocation of the spine.14,15 Twenty-nine cases have been reported over a period of 28 years. There is no clear guideline for its management especially in delayed cases, which have a high potential for intraoperative complications because of the previous physiological consolidation on a misaligned spine. For the latter, we suggest intraoperative reduction through a posterior approach with laminectomy. If this procedure succeeds, an anterior discectomy with fusion and instrumentation can be achieved. In case of failure, in situ fusion with instrumentation is required for early mobilization of the patient for physical therapy and to avoid long bed rest complications.
Author Contributions
Conception and design: Dao, Ouattara, Sanou, Zabsonré. Acquisition of data: Dao, Napon, Nassoum. Analysis and interpretation of data: Dao, Ouattara. Drafting the article: Dao, Kabré. Critically revising the article: Dao. Reviewed submitted version of manuscript: Dao. Approved the final version of the manuscript on behalf of all authors: Dao. Statistical analysis: Dao. Administrative/technical/material support: Dao. Study supervision: Dao.
Supplemental Information
Videos
Video 1. https://vimeo.com/884423215.
Video 2. https://vimeo.com/884427089.
Previous Presentations
Lecture given at the 2nd meeting of Burkinabé Society of Surgeons, January 29–30, 2021, Bobo Dioulasso, Burkina Faso. Lecture given at the 3rd Congress of Ivorian Society of Neurosurgery, June 22–23, 2022, Bingerville, Ivory Coast.
References
- 1. Tsujimoto T, Suda K, Harmon SM, et al. Two case reports of ‘locked spondyloptosis’: the most severe traumatic cervical spondyloptosis with locked spinous process and vertebral arch into the spinal canal. Spinal Cord Ser Cases. 2020;6(1):10. doi: 10.1038/s41394-020-0259-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Kim MW, Lee SB, Park JH. Cervical spondyloptosis successfully treated with only posterior short segment fusion using cervical pedicle screw fixation. Neurol Med Chir (Tokyo) 2019;59(1):33–38. doi: 10.2176/nmc.tn.2018-0213. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Padwal A, Shukla D, Bhat DI, Somanna S, Devi BI. Post-traumatic cervical spondyloptosis: a rare entity with multiple management options. J Clin Neurosci. 2016;28:61–66. doi: 10.1016/j.jocn.2015.05.074. [DOI] [PubMed] [Google Scholar]
- 4. Tumialán LM, Dadashev V, Laborde DV, Gupta SK. Management of traumatic cervical spondyloptosis in a neurologically intact patient: case report. Spine (Phila Pa 1976) 2009;34(19):E703–E708. doi: 10.1097/BRS.0b013e3181b1fc3a. [DOI] [PubMed] [Google Scholar]
- 5. Manjila S, Chowdhry SA, Bambakidis NC, Hart DJ. Traumatic, high-cervical, coronal-plane spondyloptosis with unilateral vertebral artery occlusion: treatment using a prophylactic arterial bypass graft, open reduction, and instrumented segmental fusion. J Neurosurg Spine. 2014;20(2):183–190. doi: 10.3171/2013.10.SPINE13115. [DOI] [PubMed] [Google Scholar]
- 6. Perlman R, Hawes LE. Cervical spondylolisthesis. J Bone Joint Surg Am. 1951;33-A(4):1012–1013. [PubMed] [Google Scholar]
- 7. Bhojraj SY, Shahane SM. Posttraumatic cervical spondyloptosis at C6-7 with late-onset cord compression: a new clinical entity. Case report. J Neurosurg. 1992;77(5):792–794. doi: 10.3171/jns.1992.77.5.0792. [DOI] [PubMed] [Google Scholar]
- 8. Modi JV, Soman SM, Dalal S. Traumatic cervical spondyloptosis of the subaxial cervical spine: a case series with a literature review and a new classification. Asian Spine J. 2016;10(6):1058–1064. doi: 10.4184/asj.2016.10.6.1058. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Menku A, Kurtsoy A, Tucer B, Oktem IS, Akdemir H. The surgical management of traumatic C6 - C7 spondyloptosis in a patient without neurological deficits. Minim Invasive Neurosurg. 2004;47(4):242–244. doi: 10.1055/s-2004-818496. [DOI] [PubMed] [Google Scholar]
- 10. Dhall SS, Sribnick EA. Significant neurologic recovery after traumatic cervical spondyloptosis and spinal cord injury. Spine J. 2014;14(1):194–195. doi: 10.1016/j.spinee.2013.08.002. [DOI] [PubMed] [Google Scholar]
- 11. Dahdaleh NS, Dlouhy BJ, Greenlee JD, Smoker WR, Hitchon PW. An algorithm for the management of posttraumatic cervical spondyloptosis. J Clin Neurosci. 2013;20(7):951–957. doi: 10.1016/j.jocn.2012.08.008. [DOI] [PubMed] [Google Scholar]
- 12. Wong KE, Chang PS, Monasky MS, Samuelson RM. Traumatic spondyloptosis of the cervical spine: A case report and discussion of worldwide treatment trends. Surg Neurol Int. 2017;8:89. doi: 10.4103/sni.sni_434_16. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13. Shah KC, Rajshekhar V. Successful management of post-traumatic C7-T1 spondyloptosis with uninstrumented ventral surgery. Surg Neurol. 2004;62(5):431–434. doi: 10.1016/j.surneu.2003.12.012. [DOI] [PubMed] [Google Scholar]
- 14. Feigenbaum F, Sulmasy DP, Pellegrino ED, Henderson FC. Spondyloptotic fracture of the cervical spine in a pregnant, anemic Jehovah’s Witness: technical and ethical considerations. Case report. J Neurosurg. 1997;87(3):458–463. doi: 10.3171/jns.1997.87.3.0458. [DOI] [PubMed] [Google Scholar]
- 15. Alharbi HN, Alsager GA, Abdulaziz M, Bhat R, Surur S. Surgical management of traumatic cervicothoracic junction spondyloptosis without neurological injury: a case report and review of the literature. Cureus. 2022;14(10) doi: 10.7759/cureus.30813. [DOI] [PMC free article] [PubMed] [Google Scholar]


