Abstract
Background:
Contraception is a strategy to meet the family planning goals of women living with human immunodeficiency virus (WLHIV) as well as to reduce the transmission of HIV. There is limited data from Nigeria, where HIV prevalent is the second-largest in the world. This study aimed to examine contraceptive use and identify factors influencing its use among sexually active WLHIV in Ibadan, Nigeria.
Methods:
A facility-based cross-sectional study was conducted among 443 sexually active WLHIV across three HIV treatment centers in Ibadan, Oyo State. The inclusion criteria were WLHIV, aged 18–49 years, who asserted being fecund and sexually active. An adopted questionnaire was used to collect data, and the data was analyzedusing the Statistical Package for Social Sciences (SPSS) Windows version 25. Statistical significance was set at p < 0.05.
Results:
Among sexually active WLHIV (n = 443), 73.1% used contraceptives, with 26.9% having unmet needs. The results revealed a significant association between employment status and the use of contraceptives (AOR = 2.150; 95% CI 1.279–3.612 p=0.004); accessibility to contraceptive methods and the use of contraceptives (AOR = 21.483; 95% CI 7.279–63.402 p=0.00). Also, a significant association was found between payment for service and contraceptive use (AOR = 14.343; 95% CI 2.705–76.051; p = 0.003). Previous reactions towards contraceptive use were also significantly associated with contraceptive use (AOR = 14.343; 95% CI 2.705–76.051 p = 0.003). The dual contraceptives usage rate was 30.7%.
Conclusions:
Although contraceptive use among sexually active WLHIV was high, the study highlighted the need for increased adoption of dual contraceptive methods to mitigate the risk of unintended pregnancy and HIV re-infection among this population. It emphasized the importance of continuous sensitization and counseling services healthcare providers provide to promote contraceptive use among WLHIV.
Keywords: Contraceptive, Sexually Active Women, Human Immunodeficiency Virus
INTRODUCTION
Globally, there are about 37.7 million Human Immunodeficiency Virus (HIV)-positive individuals worldwide, of which 20.2 million are women living with HIV. [1, 2] It has been determined that Sub-Saharan Africa is the area most severely affected by the HIV epidemic, accounting for more than two-thirds of all HIV infections worldwide. Nigeria has the second-largest HIV epidemic in the world and the region’s highest incidence of new infections. In Nigeria, 1.7 million people lived with HIV (PLHIV) in 2020. [3] Women can make independent choices about having children and having sex, regardless of their HIV status. Women living with HIV (WLHIV) must be informed, given the freedom to choose a safe, effective method of contraception, and provided with it at nearby health centers.[4] Because it prevents unplanned pregnancies, contraception may also be essential for preventing Mother-to-Child Transmission of HIV. [5] Strengthening contraceptive programs is therefore essential to lower the high incidence of unintended pregnancies, which could contribute to the elimination of HIV/AIDS outbreaks by 2030 (Sustainable Development Goal 3.3). [6, 7]
There appears to be a substantial unmet need for contraception among WLHIV and contraceptive failure due to the high incidence of unwanted pregnancy and abortion.[8] Nigeria accounts for 70% of sexually active WLHIV, 5.5 million WLHIV births annually, and 15% of the world’s low contraceptive uptake.[9] Furthermore, prior research found that Nigerian WLHIV had a high level of awareness about contraception, but that knowledge did not match their use of contraceptives, which was linked to a high proportion of unwanted pregnancies.[10] Women who are fecund, sexually active, and who report not wanting any more children or wishing to delay the next child are considered to have unmet needs, according to the WHO.[11] Because ART has increased the overall survival rate of PLHIV, WLHIV must have defined reproductive life plans that include accessible access to contraception. Most of the research that has been done on contraceptive use among WLHIV has focused on married women. [12] Because of this, sexual activity among sexually active unmarried women puts them at a higher risk of having an unexpected child because of the idea that sex can only take place within the setting of a married relationship. Therefore, there is a lack of reproductive plans for these women through health services. [13–15]
Although the WHO has recommended that WLHIV have the right to choose any method of contraception, similar to HIV-negative women, the choice of contraception in the presence of HIV appears to be more complicated because WLHIV is required to strike a balance between the prevention of unintended pregnancy and HIV transmission. [16, 17] Sexually active WLHIV can also plan their reproductive lives to avoid unwanted pregnancies and enjoy parenthood like their counterparts who are not living with HIV. Hence, this study aims to identify key predictors of contraceptive use among sexually active WLHIV in Ibadan, Oyo State, Nigeria.
MATERIALS AND METHODS
Study Design and Setting
Design Overview
The research employed a facility-based cross-sectional survey approach. In a cross-sectional survey, researchers observe and collect data from participants simultaneously rather than over a prolonged period. This study design is beneficial for understanding the prevalence of a phenomenon, condition, or opinion at a given moment. [18]
Target Population
The study specifically focused on sexually active women living with WLHIV. By targeting this particular group, the research aimed to gain insights relevant to their experiences, challenges, and needs.
Geographical Setting
The study was conducted in Ibadan, Oyo State, Nigeria. Oyo State, located in the southwestern part of Nigeria, is one of the country’s significant states, with a rich cultural heritage and diverse population. Understanding the experiences of WLHIV in this region could provide insights that might reflect broader trends within the state or even the country, given its diverse demographic makeup.
Facility Details
Three prominent HIV treatment centers in Oyo State were chosen as the study sites:
Adeoyo Maternity Hospital Yemetu: Located in the Yemetu area, this maternity hospital is a haven for expectant mothers and a pivotal center providing HIV treatments and counseling services. It’s a reputable institution known for its comprehensive care for women, especially those living with HIV.
State Hospital Adeoyo Ring Road: Situated on the bustling Ring Road, this state hospital is one of the primary healthcare providers in the region. It caters to a wide range of medical needs, with a particular unit dedicated to HIV treatments, ensuring patients receive both medical and emotional support.
St. Annes Anglican Hospital Molete: A faith-based institution in Molete, St. Annes Anglican Hospital balances spiritual and medical care. Their commitment to serving those living with HIV makes them a crucial part of the healthcare landscape in Oyo State.
Study Timeline
This study’s data collection and observations were carried out over three months, from September to November 2022. This timeframe was chosen to ensure comprehensive data collection while minimizing seasonal or temporal biases that might affect the participants’ responses.
Study population and sampling
Purposive Sampling for Facilities
A purposive sampling technique was utilized for this study. Purposive sampling is a non-probabilistic method where researchers select particular groups or individuals for their specific qualities or characteristics. [19] In this case, the health facilities were chosen based on antiretroviral therapy (ART) treatment availability. Not all health facilities offer ART treatment; hence, selecting those that specifically provide this service was vital to ensure the study’s participants were relevant to the research objectives.
Random Selection of Participants
Once the facilities were determined, the actual participants for the study were chosen through a random sampling process within each facility. This method ensures that each eligible participant in the selected health facilities has an equal chance of being chosen for the study, minimizing biases and ensuring the results represent the target population within those facilities. [20]
Inclusion Criteria
Participants were included in the study based on the following set of criteria:
They identified as WLHIV.
They were aged between 18 and 49 years, ensuring the study focused on the reproductive age group.
They had been sexually active within the last six months.
This criterion was crucial to understanding the current sexual behaviors and practices among WLHIV.
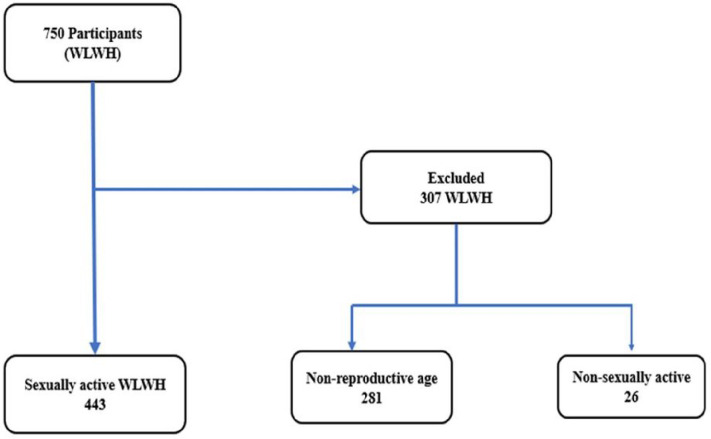
Study Flowchart and Numbers
A comprehensive flowchart was designed to map out the participant selection process. Initially, 750 WLHIV from the selected facilities were approached and interviewed. However, after applying the inclusion criteria, particularly the requirement of recent sexual activity, the final sample size was narrowed down. Out of the initial 750 participants, 443 sexually active WLHIV were found to meet all the study’s criteria and were subsequently analyzed in-depth.
Data Collection
Data was collected using adapted questionnaires from a previous study on contraceptive use among sexually active WLHIV. [17] The questionnaire was divided into three sections: Socio-Demography Data Questionnaire among sexually active WLHIV, Contraceptive Use Questionnaire among sexually active WLHIV, and Perceived factors influencing Contraceptive Use Questionnaire among sexually active WLHIV. Before the main study, the adapted questionnaire was pretested on a representative sample, feedback on clarity and relevance was collected, and statistical analyses, including Cronbach’s Alpha, affirmed their internal solid consistency (α = 0.85) and validity, ensuring their suitability for the research objectives. [21] The selected participants were those who voluntarily consented to participate. All research assistants were trained before the commencement of the study on the research tools, interviewing skills, data management, and clarifications of ethical issues in research. The research assistants administered the questionnaires in English or the local language to participants who could neither read nor write. The questionnaires were administered privately, and clarification and assistance were provided where necessary. The interviews took approximately 20 minutes to complete.
Statistical Analysis
The data gathered from the comprehensive questionnaires was diligently processed and meticulously analyzed utilizing the Statistical Package for Social Science (SPSS) version 25. SPSS is a widely recognized and powerful software for handling and analyzing statistical data, particularly in social sciences research. Variables in the dataset were assessed to determine if they were normally distributed or not to determine the appropriate statistical analysis to be used. Mean was used to describe the customarily distributed variables, while the median was used for the non-normally distributed variables. Linear regression was used to assess the statistical association between variables that had categorized outcomes more than 3.
Meanwhile, logistic regression assessed the statistical association between selected variables and variables with dichotomized outputs such as contraceptive use: Yes/No, True/False. The adjusted regression models included covariates such as age, education level, marital status, income level, and others. The strength of the association was assessed by setting a significance level at p-value < 0.05.
Ethical Considerations
The Health Department of Planning Research & Statistics Division, Oyo State Ministry of Health, provided the Ethics Approval for this study (AD 13/479/44542A). Official permission was obtained from hospitals included in this study. The verbal/written consent procedure was conducted in a separate and private room, administered by trained data collectors. The study participants were assured that their involvement was entirely voluntary, and they retained the right to decline participation or revoke their consent at any juncture.
Significantly, it was stressed that their participation would not impact the medical care they received. Participants were also apprised that the survey might entail sensitive or personal inquiries related to reproductive health concerns, which could be uncomfortable or distressing. Also, participants were explicitly informed that they were under no obligation to answer any question that they found uncomfortable and had the liberty to withdraw from the study or choose not to respond to specific questions at any point. In cases where participants required emotional support, female nurses were available to offer psychological assistance. All collected data were transformed into an anonymized format and stored on laptops protected by passwords throughout the data collection. Furthermore, the data was stored on secure, password-protected computers to ensure confidentiality and security.
RESULTS
Socio-demographic Characteristics of Participants
Table 1 provides a detailed overview of the socio-demographic characteristics of the study participants of 433 individuals. Among the participants, 324 (73.1%) were contraceptive users, while 119 (26.9%) were non-users of contraceptives. Regarding age, the average age of contraceptive users was 36.62 years, with a standard deviation of 6.70 years. In contrast, non-users had a slightly higher average age of 37.59 years with a standard deviation of 7.20 years. When examining marital status, a majority of contraceptive users were married, accounting for 74.6% (290 individuals). The proportions of divorced, widowed, separated, and single users were 70.0%, 56.2%, 66.7%, and 62.5%, respectively. On the other hand, among non-users, 99 (25.4%) were married, 3 (30.0%) were divorced, 7 (43.8%) were widowed, 4 (33.3%) were separated, and 6 (37.5%) were single.
Table 1.
Socio-demographic Characteristics of Study Participants (n =433)
| Contraceptive User N=324 [73.1%] | Non-users of Contraceptives N=119 [26.9%] | |
|---|---|---|
|
| ||
| Variable | N [%] | N [%] |
|
| ||
| Age | ||
|
| ||
| Mean ± SD | 36.62±6.70 | 37.59 ± 7.20 |
|
| ||
| Marital Status | ||
|
| ||
| Married | 290 [74.6] | 99 [25.4] |
| Divorce | 7 [70.0] | 3 [30.0] |
| Widowed | 9 [56.2] | 7 [43.8] |
| Separated | 8 [66.7] | 4 [33.3] |
| Single | 10 [62.5] | 6 [37.5] |
|
| ||
| Ethnic Group | ||
|
| ||
| Yoruba | 285 [75.0] | 95 [25.0] |
| Igbo | 25 [62.5] | 15 [37.5] |
| Hausa | 6 [50.0] | 6 [50.0] |
| Others | 8 [72.7] | 3 [27.3] |
|
| ||
| Religion | ||
|
| ||
| Christianity | 188 [72.0] | 73 [28.0] |
| Islam | 136 [74.7] | 46 [25.3] |
|
| ||
| Educational Level | ||
|
| ||
| Primary level | 93 [78.8] | 25 [21.2] |
| Secondary level | 135 [67.8] | 64 [32.2] |
| Tertiary level | 65 [78.3] | 18 [21.7] |
| None | 31 [72.1] | 12 [27.9] |
|
| ||
| Employment Status | ||
|
| ||
| Employed | 273 [76.5] | 84 [23.5] |
| Unemployed | 51 [59.3] | 35 [40.7] |
|
| ||
| Type of Partner | ||
|
| ||
| Spouse | 269 [74.9] | 90 [25.1] |
| Steady | 32 [80.0] | 8 [20.0] |
| Causal | 14 [53.8] | 12 [46.2] |
| None | 9 [50.0] | 9 [50.0] |
|
| ||
| Monthly Income | ||
|
| ||
| < 44.71 USD (NGN 33,000) | 225(77.6) | 65(22.4) |
| ≥ 44.71 USD (NGN 33,000) | 99(64.7) | 54(35.3) |
|
| ||
| Know Partner’s Status | ||
|
| ||
| Yes | 276 [76.9] | 83 [23.1] |
| No | 48 [57.1] | 36 [42.9] |
|
| ||
| If Yes, Partner Status | ||
|
| ||
| Positive | 111 [77.1] | 33 [22.9] |
| Negative | 161 [78.2] | 45 [21.8] |
| Not Applicable | 52 [55.9] | 41 [44.1] |
Ethnic distribution showed that the Yoruba ethnic group constituted the majority of contraceptive users at 75.0% (285 individuals). Other ethnic groups among users were Igbo at 62.5%, Hausa at 50.0%, and others at 72.7%. For non-users, the Yoruba, Igbo, Hausa, and other ethnic groups constituted 25.0%, 37.5%, 50.0%, and 27.3%, respectively. In terms of religion, 188 (72.0%) of the contraceptive users identified as Christians, and 136 (74.7%) identified as Muslims. Among the non-users, 73 (28.0%) were Christians, and 46 (25.3%) were Muslims. For educational level, among contraceptive users, 93 (78.8%) had primary education, 135 (67.8%) had secondary education, 65 (78.3%) had tertiary education, and 31 (72.1%) had no formal education. Among non-users, the percentages for primary, secondary, tertiary, and none were 21.2%, 32.2%, 21.7%, and 27.9%, respectively.
Regarding employment status, a substantial proportion of contraceptive users, 273 (76.5%), were employed, whereas 51 (59.3%) were unemployed. In contrast, 84 (23.5%) of non-users were employed, and 35 (40.7%) were unemployed. About the type of partner, 269 (74.9%) of contraceptive users had a spouse, 32 (80.0%) had a steady partner, 14 (53.8%) had a casual partner, and 9 (50.0%) had no partner. For non-users, the distribution was 90 (25.1%) with a spouse, 8 (20.0%) with a steady partner, 12 (46.2%) with a casual partner, and 9 (50.0%) with no partner. Considering the monthly income of the participants, 77.6% of contraceptive users (N=225) reported earning less than 44.71 USD (NGN 33,000), while 22.4% of non-users (N=65) fell within this income bracket. On the other hand, 64.7% of contraceptive users (N=99) earned 44.71 USD (NGN 33,000) or more, compared to 35.3% of non-users (N=54) with a similar income level. (See Table 1)
Level of Dual Contraceptive Utilization
Table 2 presents data on the contraceptive utilization patterns among the participants. Out of the participants, 30.7% (N=136) reported using dual contraceptives. Meanwhile, 42.4% (N=188) indicated that they use a single contraceptive method. Notably, 26.9% (N=119) of the participants mentioned that they do not use any contraceptives at all.
Table 2:
Level of Dual Contraceptive Utilization
| Variable | N [%] |
|---|---|
| Dual Contraceptives Usage | 136 [30.7] |
| Single Contraceptive Usage | 188 [42.4] |
| No Usage | 119 [26.9] |
Factors Associated with Contraceptive Use among Sexually Active WLHIV
After adjusting for the seven significant variables in the logistic regression analysis, only four risk factors had a statistically significant association with contraceptive use among sexually active WLHIV. Regarding religion, while women identifying with Islam showed a reduced likelihood of contraceptive use compared to their Christian counterparts, this difference was not statistically significant (Adjusted Odd Ratio (AOR): 0.461, 95% CI: 0.176–1.213, p=0.117). Educational background played a role, with women without formal education being less inclined to use contraceptives compared to those with primary education (AOR: 0.518, 95% CI: 0.162–1.651, p=0.266). The study results show that women with tertiary or secondary education also showed differences in contraceptive use when compared to those with primary education, though these results were not statistically significant.
In terms of marital status, single women had a higher likelihood of contraceptive use than divorced, widowed, or married women; however, this difference did not attain statistical significance. Separated women, on the other hand, were more likely to use contraceptives than single women, but again, this difference was not statistically significant (AOR: 1.799, 95% CI: 0.184–17.619, p=0.614). Employment emerged as a significant factor: employed women were more inclined to use contraceptives than their unemployed counterparts (AOR: 2.150, 95% CI: 1.279–3.612, p=0.004).
Regarding the type of partner, women with steady partners were less likely to use contraceptives than those married, with the difference nearing statistical significance (AOR: 0.102, 95% CI: 0.022–0.485, p=0.067). Yet, women with casual or no partners showed reduced contraceptive use compared to married women, without a significant difference. Notably, the source of contraceptives was influential: women obtaining contraceptives outside the ART center demonstrated a significantly higher tendency to use them compared to those who did not (AOR: 21.483, 95% CI: 7.279–63.402, p=0.00).
Distance to health facilities also influenced contraceptive use, with an increase in usage as the distance from these facilities grew. Specifically, the distance between 2 and 3 kilometers from the health facilities was significant compared to the reference (AOR: 4.021, 95% CI: 1.343–12.036, p=0.020). Additionally, payment for services was a determinant: women paying for services showed a significantly higher likelihood of using contraceptives (AOR: 14.343, 95% CI: 2.705–76.051, p=0.020). Lastly, concerning adverse reactions to contraceptives, the odds ratio indicated a diminished likelihood of experiencing an adverse reaction (AOR: 0.006, 95% CI: 0.002–0.20), suggesting that women not reporting adverse reactions had significantly lower odds of having them compared to the reference group. (See Table 3)
Table 3:
Factors Affecting the Use of Contraceptives among Sexually Active Women Living with HIV
| Variables | Adjusted Odd Ratio (95% CI) | P value |
|---|---|---|
|
| ||
| Religion | ||
|
| ||
| Christianity | 0.461(0.176, 1.213) | 0.117 |
| Islam | Ref | Ref |
|
| ||
| Education Level | ||
|
| ||
| Primary Level | 0.518 (0.162, 1.651) | 0.266 |
| Secondary Level | 1.405(0.438, 4.511) | 0.380 |
| Tertiary Level | 0.354(0.086,1.448) | 0.058 |
| None | Ref | |
|
| ||
| Marital status | ||
|
| ||
| Married | 0.661(0.162,1.651) | 0.266 |
| Divorce | 0.490(0.100,2.410) | 0.380 |
| Widowed | 0.184(0.032,1.062) | 0.585 |
| Separated | 1.799(0.184,17.619) | 0.614 |
| Single | Ref | |
|
| ||
| Employment Status | ||
|
| ||
| Unemployed | 2.150(1.279,3.612) | 0.004 |
| Employed | Ref | |
|
| ||
| Type of Partner | ||
|
| ||
| Spouse | 0.498(0124,1.993) | 0.233 |
| Steady | 0.102(0.022,0.485) | 0.067 |
| Causal | 0.338(0.035,3.300) | 0.062 |
| None | Ref | |
|
| ||
| Get Contraceptives outside the ART Center | ||
|
| ||
| Yes | 21.483(7.279,63.402) | 0.00 |
| No | Ref | |
|
| ||
| Distance to the health facilities | ||
|
| ||
| ½ to 1 kilometer | 2.669(0.949,0.949) | 0.639 |
| 2 to 3 kilometres | 4.021(1.343,12.036) | 0.304 |
| 4 to 5 kilometres | Ref | |
|
| ||
| Payment for Services | ||
|
| ||
| Yes | 14.343(2.705,76.051) | 0.020 |
| No | Ref | |
|
| ||
| Adverse Reaction while using Contraceptive | ||
|
| ||
| Yes | Ref | |
| No | 0.006(0.002,0.20) | 0.000 |
DISCUSSION
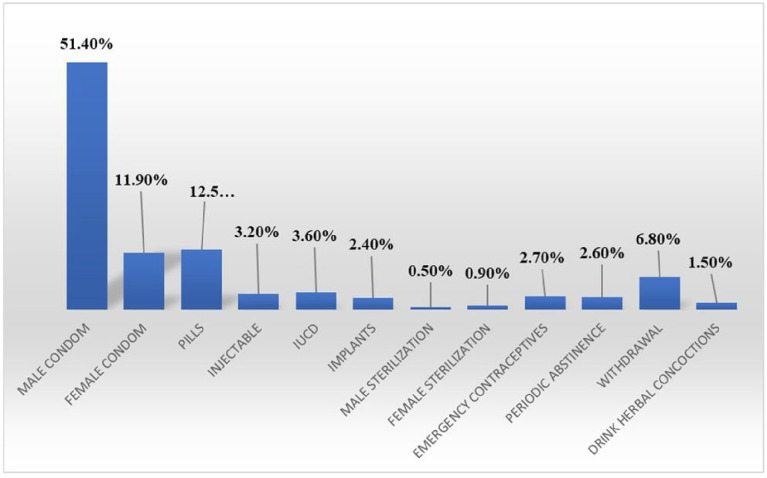
The study underscored the significant use of contraceptives among sexually active WLHIV in Ibadan, Nigeria, mirroring the contraceptive adoption rates seen in Ethiopia, where 75% of sexually active WLHIV used contraceptives while the remaining 25% faced unmet contraceptive requirements. [17, 22, 23] This utilization of contraceptives plays a fundamental role in advancing family planning goals and reinforcing the Prevention of Mother-To-Child Transmission programs.[24] Yet, the contrasting findings from Oyo State, Nigeria, remind us that awareness does not always lead to action. Even with high contraceptive knowledge levels among WLHIV, usage rates remained disappointingly low [10]; male condoms were most popular, trailed by pills and female condoms.
Conversely, less conventional methods like male and female sterilization and herbal mixtures were minimally favored. Compared to data from Togo, these rates were marginally lower.[25] Although dual contraceptive methods could effectively prevent unwanted pregnancies and sexually transmitted infections (STIs), their adoption was overshadowed by the preference for single methods.[26] Several factors are pivotal in determining contraceptive choices.[27–29] Employment status stood out, corroborated by Banten Province, Indonesia’s findings, which identified employment as a critical influencer.[30] Similarly, the absence of side effects encouraged continuity in contraceptive use, emphasizing the value of a smooth experience.
Contrastingly, the necessity of payments acted as a deterrent, with a study from Uganda linking payment barriers to reduced contraceptive use.[28] Nevertheless, the challenges faced by WLHIV are multi-layered. Sociocultural dynamics heavily influence contraceptive choices.[31] In many African settings, reproductive choices are often determined more by a woman’s partner than by herself. Moreover, the stigma attached to HIV often discourages WLHIV from availing contraceptive services, particularly if healthcare professionals hold biased views.[31–34]
The types of available contraceptives also matter. The dominant use of male condoms, while indicative of their dual protective nature against STIs and pregnancies, also shows a limitation in contraceptive choices. There is an evident need for long-acting methods like IUDs and implants, offering women greater autonomy, but their accessibility is often constrained by availability or cost.[35–37] The role of healthcare infrastructure is undeniable. The inconsistency in contraceptive stock can discourage WLHIV from relying on specific methods, prompting them to settle for less preferred options. Integrating HIV care with contraceptive services might present a more consistent and comprehensive solution.[10]
Comprehensive counseling provides essential information about contraceptive options, side effects, and effectiveness and can significantly guide WLHIV in making informed choices. This approach can demystify misconceptions and align contraceptive choices with individual reproductive and health goals. [38, 39] Lastly, policy frameworks are pivotal. For effective contraceptive adoption among WLHIV, governments, and health bodies must craft policies prioritizing their unique challenges, encompassing contraceptive procurement, training of healthcare professionals, and robust monitoring mechanisms. In essence, while global data paints an overarching picture, addressing the contraceptive needs of WLHIV requires a deeper understanding of the intricate blend of personal, sociocultural, and structural factors. Only a holistic approach, cognizant of these intricacies, can genuinely champion the reproductive rights of every woman.
Self-reported data were used, which may be affected by social desirability and recall bias. The study only focused on women living with HIV and did not include men living with HIV, which limits the understanding of the contraceptive needs of male partners of women living with HIV. The study did not explore the impact of cultural and religious beliefs on contraceptive use, which could significantly influence contraceptive use among this population. The study’s strengths include a large representative sample of the three facilities and participants, including WLHIV, which was possible due to the nature of the facilities that participated in the study.
In evaluating the reproductive health choices of WLHIV, our study traverses a landscape underscored by the United Nations’ Sustainable Development Goals (SDGs).[40] The significance we attribute to contraceptives for enhancing overall health and the crucial PMTCT resonates deeply with the ethos of SDG 3: Good Health and Well-being.[41] Delving into the sociocultural dynamics impacting WLHIV’s reproductive decisions and their multifaceted challenges, our findings mirror SDG 5: Gender Equality [42], which brings to the forefront the pressing narratives of SDG 10, highlighting the stark inequalities faced by WLHIV compared to the broader population.[41, 43] Furthermore, our proposition for integrated and cooperative policy frameworks, tailored by governments and health bodies alike, echoes the collaborative spirit of SDG 17: Partnerships for the Goals.[43, 44] Through the lens of these SDGs, our study amplifies the need for an all-encompassing approach to uphold and advocate for the reproductive rights of WLHIV genuinely
CONCLUSION
This study provides evidence that shows high levels of contraceptive use among sexually active WLHIV. However, the study identified the need for greater uptake of dual contraceptive methods to reduce the risk of unwanted pregnancy and HIV re-infection among WLHIV. The study also highlighted various factors, such as employment status, access to contraceptive methods, payment for service, and previous experience with contraceptive use, that influence the use of contraceptives among this population. These findings have important implications for policymakers and healthcare providers seeking to improve reproductive health outcomes and reduce the burden of HIV among WL HIV in Nigeria.
Figure 1.
Flow Chart Illustrating the Eligibility Process to Obtain The Final Sample For Analysis of Sexually Active WLHIV
Figure 2.
Legend not included with this version.
Acknowledgments:
This work was supported by grants from Fogarty International Center (FIC) and the National Institute of Health (Funding provided by Fogarty Training Grant: D43TW010934-03). The content is solely the author’s responsibility and does not necessarily represent the official views of the National Institutes of Health.
Footnotes
Conflicts of Interest: “The authors declare no conflict of interest.”
Institutional Review Board Statement: The study was conducted following the Declaration of Helsinki and approved by the Oyo State Ministry of Health Research Ethics Committee (Protocol code: AD 13/479/44542A and approval date: August 15, 2022).
Informed Consent Statement: “Informed consent was obtained from all subjects involved in the study.”
Consent to Publish: Not applicable.
Contributor Information
Folahanmi Tomiwa. Akinsolu, Lead City University
Zainab Oyindamola Adegbite, Lead City University.
Samuel A. Bankole, Lead City University
Abisola Lawale, Lead City University.
Ifeoluwa Eunice Adewole, Lead City University.
Olunike Rebecca Abodunrin, Lead City University.
Mobolaji Timothy Olagunju, Nanjing Medical University.
Oluwabukola Mary Ola, Lead City University.
Abel Nnamdi Chukwuemeka, Lead City University.
Aisha Oluwaseun Gambari, Lead City University.
Jacinta N. Nwogu-Attah, Lead City University
Hiliary Nosa Okunbor, Babcock University Teaching Hospital.
Akim Tafadzwa Lukwa, University of Cape Town.
Ebiere Herbertson, Nigerian Institute of Medical Research.
George Uchenna Eleje, Nnamdi Azikiwe University Teaching Hospital.
Olatunji Akanni, Lead City University.
Oliver Chukwujekwu Ezechi, Lead City University.
Data Availability Statement:
The data used to support the findings of this study are available from the corresponding author upon request.
References
- 1.Mahy MI, Sabin KM, Feizzadeh A, Wanyeki I. Progress towards 2020 global HIV impact and treatment targets. Journal of the International AIDS Society. 2021;24:e25779. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Ekholuenetale M, Onuoha H, Ekholuenetale CE, Barrow A, Nzoputam CI. Socioeconomic inequalities in human immunodeficiency virus (HIV) sero-prevalence among women in Namibia: Further analysis of population-based data. International journal of environmental research and public health. 2021;18(17):9397. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.AIDS NAftCo. National strategic framework on HIV and AIDS. 2021. [Google Scholar]
- 4.Abera L, Mengistu B. Fertility Desire and Associated Factors among Reproductive Age Women Attending Antiretroviral Therapy at Public Hospitals in Eastern Ethiopia. 2023. [Google Scholar]
- 5.Damian DJ, George JM, Martin E, Temba B, Msuya SE. Prevalence and factors influencing modern contraceptive use among HIV-positive women in Kilimanjaro region, northern Tanzania. Contraception and reproductive medicine. 2018;3:1–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Ruhil R. Millennium development goals to sustainable development goals: challenges in the health sector. International Studies. 2015;52(1–4):118–35. [Google Scholar]
- 7.Gómez-Suárez M. Prevention of HIV Perinatal Transmission: The Role of Sexual and Reproductive Health Services for Women Living with HIV. AIDS Updates-Recent Advances and New Perspectives: IntechOpen; 2021. [Google Scholar]
- 8.Ope BW. Reducing maternal mortality in Nigeria: addressing maternal health services’ perception and experience. Journal of Global Health Reports. 2020;4:e2020028. [Google Scholar]
- 9.Olufadewa I, Adesina M, Oladele R, Ayorinde T. Knowledge of HIV and other sexually transmitted infections and place of delivery among urban women in South-West Nigeria. 2022. [Google Scholar]
- 10.Adeleye KK, Akinwaare MO, Adejumo PO. Reproductive plans and utilization of contraceptives among women living with HIV. International Journal of Maternal and Child Health and AIDS. 2019;8(2):120. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Mosisa G, Tsegaye R, Wakuma B, Mulisa D, Etefa W, Abadiga M, et al. Fertility desire and associated factors among people living with HIV in Ethiopia: a systematic review and meta-analysis. Archives of Public Health. 2020;78(1):1–16. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Fite RO, Mohammedamin A, Abebe TW. Unintended pregnancy and associated factors among pregnant women in Arsi Negele Woreda, West Arsi Zone, Ethiopia. BMC research notes. 2018;11:1–7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Tsafack M. Dual contraception use and associated factors among HIV positive women follow-up at Treatment Center Unit of Yaounde Central Hospital, Cameroon. Open Access Library Journal. 2020;7(05):1. [Google Scholar]
- 14.Akinsoji AA, Olufunmilola AA, Idowu AA, Pius AO. Sexual and Contraceptive Practices among Female Undergraduates in a Nigerian Tertiary Institution. Ethiopian journal of health sciences. 2015;25(3):209–16. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Munakampe MN, Zulu JM, Michelo C. Contraception and abortion knowledge, attitudes and practices among adolescents from low and middle-income countries: a systematic review. BMC health services research. 2018;18(1):1–13. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Tshilonda JCB, Tshibanda AK, Katambue JK, Kabemba GK, Kabemba RK, Ngoyi CK, et al. Rate of Use of Female Condoms in Sex Professionals in the City of Mbuji-Mayi, Democratic Republic of Congo. Open Access Library Journal. 2020;7(9):1–9. [Google Scholar]
- 17.Feyissa TR, Harris ML, Forder PM, Loxton D. Contraceptive use among sexually active women living with HIV in western Ethiopia. PloS one. 2020;15(8):e0237212. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Capili B. Overview: Cross-Sectional Studies. The American journal of nursing. 2021;121(10):59. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Campbell S, Greenwood M, Prior S, Shearer T, Walkem K, Young S, et al. Purposive sampling: complex or simple? Research case examples. Journal of research in Nursing. 2020;25(8):652–61. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Garg R. Methodology for research I. Indian journal of anaesthesia. 2016;60(9):640. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Bujang MA, Omar ED, Baharum NA. A Review on Sample Size Determination for Cronbach’s Alpha Test: A Simple Guide for Researchers. The Malaysian journal of medical sciences : MJMS. 2018;25(6):85–99. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Blackstone SR, Iwelunmor J. Determinants of contraceptive use among Nigerian couples: evidence from the 2013 Demographic and Health Survey. Contraception and reproductive medicine. 2017;2(1):1–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Crawford EE, Atchison CJ, Ajayi YP, Doyle AM. Modern contraceptive use among unmarried girls aged 15–19 years in South Western Nigeria: results from a cross-sectional baseline survey for the Adolescent 360 (A360) impact evaluation. Reproductive Health. 2021;18:1–13. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Sherwood J, Lankiewicz E, Roose-Snyder B, Cooper B, Jones A, Honermann B. The role of contraception in preventing HIV-positive births: global estimates and projections. BMC Public Health. 2021;21(1):1–10. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Yaya I, Patassi AA, Landoh DE, Bignandi EM, Kolani K, Namoro A-DD, et al. Modern contraceptive use among HIV-infected women attending HIV care centres in Togo: a cross-sectional study. BMJ open. 2018;8(4):e019006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Mesfin Y, Argaw M, Geze S, Tefera B. Dual contraceptive use and factor associated with people living with HIV/AIDS: a systematic review and meta-analysis. Infectious Diseases in Obstetrics and Gynecology. 2021;2021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.D’Souza P, Bailey JV, Stephenson J, Oliver S. Factors influencing contraception choice and use globally: a synthesis of systematic reviews. The European Journal of Contraception & Reproductive Health Care. 2022;27(5):364–72. [DOI] [PubMed] [Google Scholar]
- 28.Robinet L, Jeffredo A, Clesse C. Factors Influencing Contraceptive Choice During the Postpartum Period: A Qualitative Systematic Review. Journal of Midwifery & Women’s Health. 2023;68(2):265–86. [DOI] [PubMed] [Google Scholar]
- 29.Hlongwa M, Mashamba-Thompson T, Makhunga S, Hlongwana K. Evidence on factors influencing contraceptive use and sexual behavior among women in South Africa: a scoping review. Medicine. 2020;99(12). [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Haile D, Lagebo B. Magnitude of dual contraceptive method utilization and the associated factors among women on antiretroviral treatment in Wolaita zone, Southern Ethiopia. Heliyon. 2022;8(6). [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Saleem HT, Rosen JG, Quinn C, Duggaraju A, Kennedy CE. Contraception values and preferences of people living with HIV: A systematic review. Contraception. 2022;111:48–60. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Willan S, Gibbs A, Petersen I, Jewkes R. Exploring young women’s reproductive decision-making, agency and social norms in South African informal settlements. PloS one. 2020;15(4):e0231181. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Kibira SPS, Karp C, Wood SN, Desta S, Galadanci H, Makumbi FE, et al. Covert use of contraception in three sub-Saharan African countries: a qualitative exploration of motivations and challenges. BMC Public Health. 2020;20:1–10. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Kriel Y, Milford C, Cordero J, Suleman F, Beksinska M, Steyn P, et al. Male partner influence on family planning and contraceptive use: perspectives from community members and healthcare providers in KwaZulu-Natal, South Africa. Reproductive health. 2019;16(1):1–15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Teal S, Edelman A. Contraception selection, effectiveness, and adverse effects: a review. Jama. 2021;326(24):2507–18. [DOI] [PubMed] [Google Scholar]
- 36.Jain R, Muralidhar S. Contraceptive methods: needs, options and utilization. The journal of obstetrics and gynecology of India. 2011;61:626–34. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Steiner RJ, Liddon N, Swartzendruber AL, Rasberry CN, Sales JM. Long-acting reversible contraception and condom use among female US high school students: implications for sexually transmitted infection prevention. JAMA pediatrics. 2016;170(5):428–34. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Patel RC, Bukusi EA, Baeten JM. Current and future contraceptive options for women living with HIV. Expert opinion on pharmacotherapy. 2018;19(1):1–12. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Dehlendorf C, Krajewski C, Borrero S. Contraceptive counseling: best practices to ensure quality communication and enable effective contraceptive use. Clinical obstetrics and gynecology. 2014;57(4):659. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Starbird E, Norton M, Marcus R. Investing in Family Planning: Key to Achieving the Sustainable Development Goals. Global health, science and practice. 2016;4(2):191–210. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Fang J, Tang S, Tan X, Tolhurst R. Achieving SDG related sexual and reproductive health targets in China: what are appropriate indicators and how we interpret them? Reproductive Health. 2020;17(1):1–11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Anugwom E, Anugwom K. Sociocultural Factors in the Access of Women to HIV/AIDS Prevention and Treatment Services in South-southern Nigeria. Iranian journal of public health. 2016;45(6):754–60. [PMC free article] [PubMed] [Google Scholar]
- 43.Nunes AR, Lee K, O’Riordan T. The importance of an integrating framework for achieving the Sustainable Development Goals: the example of health and well-being. BMJ global health. 2016;1(3):e000068. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Cruz SA. SDG 17 and global partnership for sustainable development: unraveling the rhetoric of collaboration. Frontiers in Environmental Science. 2023. [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The data used to support the findings of this study are available from the corresponding author upon request.