Dear Editor,
We read with interest the article by Michael Beshara et al. [1] entitled “Nuts and bolts of lung ultrasound: utility, scanning techniques, protocols, and findings in common pathologies”. In this review, the author provides a complete and accurate description of the latest applications of pulmonary ultrasound. For the part of pneumothorax, only the diagnostic methods and ultrasound signs were described. However, the application of pneumothorax in pulmonary imaging tools should include qualitative diagnosis, quantification, and localization.
Numerous studies have demonstrated the value of lung ultrasound in diagnosing pneumothorax. Lung ultrasound can preliminarily diagnose pneumothorax by identifying four key signs: absence of pleural sliding, lung pulse, B-lines, and lung consolidation [2, 3]. Additionally, scanning for the “lung point” and/or “stratosphere sign” aids in diagnosing and localizing pneumothorax [4]. However, for intensivists, quantitative assessment is crucial for making informed decisions regarding treatment strategies for pneumothorax. This assessment helps determine whether to adopt conservative management, such as watchful waiting, or to proceed with interventional options like chest tube placement. In this context, the diagnostic accuracy of lung ultrasound is superior to that of supine chest X-ray (CXR); however, this evaluation may have significant limitations [5].
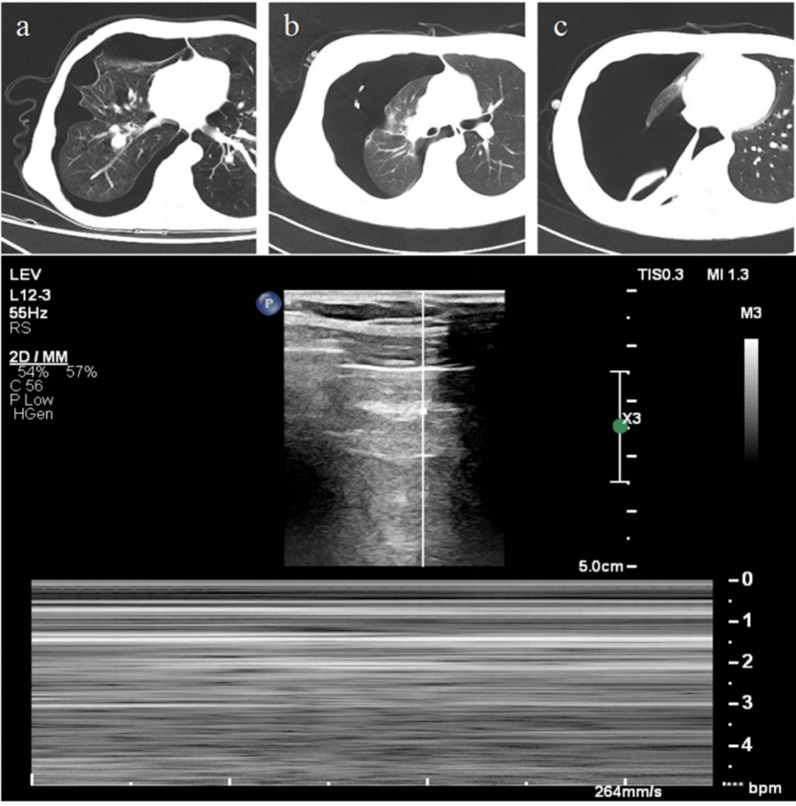
It is suggested that when lung ultrasound shows a complete "stratosphere sign" (absence of the lung point sign) on one side, it indicates that the lung lobe has been fully compressed by intrapleural gas, resulting in a complete loss of pleural apposition, potentially indicating a large pneumothorax. However, the actual volume of pneumothorax in patients with a complete stratosphere sign can vary widely. In three patients with a complete stratosphere sign on one side, chest CT scans revealed varying degrees of lung compression by pneumothorax, resulting in significant differences in pneumothorax volume and subsequent treatment choices (Fig. 1A–C). Thus, the complete stratosphere sign only indicates a large surface area of pneumothorax but cannot quantify its volume.
Fig. 1.
Three patients with pneumothorax all showed the stratosphere sign on lung ultrasound, but the pneumothorax volume could not be quantified: a Lung compression was approximately 20%. b Lung compression was approximately 50%. c Lung compression was more than 90%
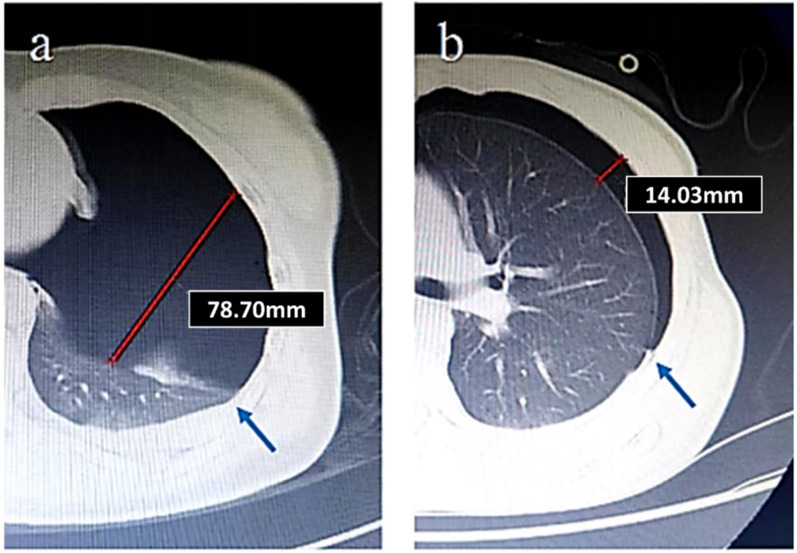
The lung point sign marks the boundary between the normal lung, where the pleural layers are apposed, and pneumothorax, where the layers have separated. It has been suggested that when the lung point sign is closer to the upper lung, it may indicate a smaller pneumothorax [6]. However, this assumption is not entirely accurate. The lung point sign reflects only the surface area of pneumothorax and may not correlate with its actual volume. For example, in two patients with the lung point sign at the same anatomical location, chest CT scans showed significant differences in intrapleural gas depth, leading to considerable variation in pneumothorax volume and different treatment choices (Fig. 2A, B). Therefore, the lung point sign indicates only the surface extent of pneumothorax and cannot be used for quantitative volume assessment.
Fig. 2.
Two patients with pneumothorax both exhibited the lung point sign on lung ultrasound, with the lung point located in almost the same position (at the junction of the left lateral chest wall, posterior axillary line, and the 7th rib). a Lung compression was approximately 70%. b Lung compression was approximately 10%
In summary, because lung ultrasound cannot assess the depth of pneumothorax, both the complete stratosphere sign (absence of the lung point sign) and the lung point sign can only qualitatively diagnose pneumothorax and indicate its surface location on the affected side. However, they cannot directly evaluate pneumothorax volume. It is crucial to recognize the limitations of lung ultrasound in quantitatively assessing pneumothorax, considering that CT would be the gold standard.
Acknowledgements
None.
Author contributions
Resources: Haotian Zhao Supervision: Heling Zhao, Li Li. Visualization: Haotian Zhao, Kai Liu. Writing—original draft: Haotian Zhao, Kai Liu. Writing—review & editing: Heling Zhao, Li Li. All authors reviewed the manuscript.
Funding
Not applicable.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request. The datasets supporting the conclusions of this article are included within the article.
Declarations
Ethics approval and consent to participate
Informed written consent was obtained from the patient’s next of kin before the examination.
Competing interests
The authors declare that they have no competing interests.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Haotian Zhao and Kai Liu have contributed equally to this work.
Contributor Information
Li Li, Email: shrmgnk@126.com.
Heling Zhao, Email: epson7777777@163.com.
References
- 1.Beshara M, Bittner EA, Goffi A, Berra L, Chang MG. Nuts and bolts of lung ultrasound: utility, scanning techniques, protocols, and findings in common pathologies. Crit Care. 2024;28(1):328. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Volpicelli G. Sonographic diagnosis of pneumothorax. Intensive Care Med. 2011;37(2):224–32. [DOI] [PubMed] [Google Scholar]
- 3.Lichtenstein DA. BLUE-protocol and FALLS-protocol: two applications of lung ultrasound in the critically ill. Chest. 2015;147(6):1659–70. [DOI] [PubMed] [Google Scholar]
- 4.Volpicelli G, Elbarbary M, Blaivas M, Lichtenstein DA, Mathis G, Kirkpatrick AW, Melniker L, Gargani L, Noble VE, Via G, Dean A, Tsung JW, Soldati G, Copetti R, Bouhemad B, Reissig A, Agricola E, Rouby JJ, Arbelot C, Liteplo A, Sargsyan A, Silva F, Hoppmann R, Breitkreutz R, Seibel A, Neri L, Storti E, Petrovic T. International Liaison Committee on lung ultrasound (ILC-LUS) for international consensus conference on lung ultrasound (ICC-LUS). International evidence-based recommendations for point-of-care lung ultrasound. Intensive Care Med. 2012;38(4):577–91. [DOI] [PubMed] [Google Scholar]
- 5.Chan KK, Joo DA, McRae AD, Takwoingi Y, Premji ZA, Lang E, Wakai A. Chest ultrasonography versus supine chest radiography for diagnosis of pneumothorax in trauma patients in the emergency department. Cochrane Database Syst Rev. 2020;7(7):CD013031. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Husain LF, Hagopian L, Wayman D, Baker WE, Carmody KA. Sonographic diagnosis of pneumothorax. J Emerg Trauma Shock. 2012;5(1):76–81. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request. The datasets supporting the conclusions of this article are included within the article.