Abstract
Background
Generative pre-trained transformer-4 (GPT-4) is a large language model (LLM) trained on a vast corpus of data, including the medical literature. Nutrition plays an important role in managing inflammatory bowel disease (IBD), with an unmet need for nutrition-related patient education resources. This study examines the accuracy, comprehensiveness, and reproducibility of responses by GPT-4 to patient nutrition questions related to IBD.
Methods
Questions were obtained from adult IBD clinic visits, Facebook, and Reddit. Two IBD-focused registered dieticians independently graded the accuracy and reproducibility of GPT-4’s responses while a third senior IBD-focused registered dietitian arbitrated. Each question was inputted twice into the model.
Results
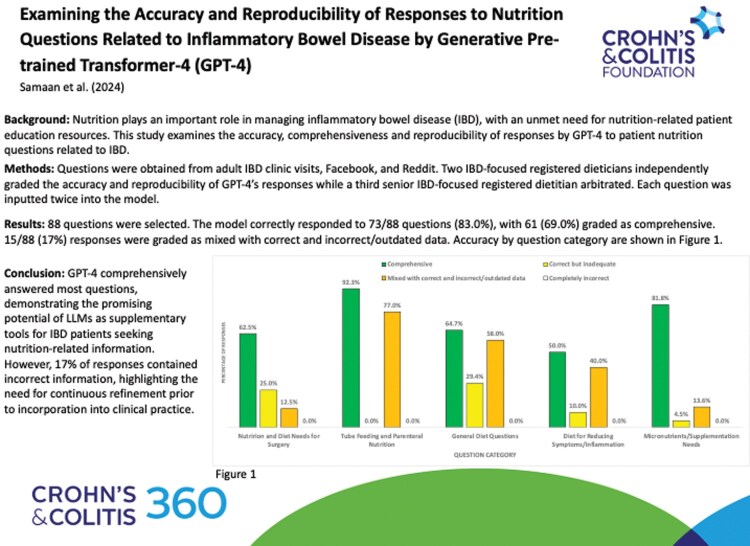
88 questions were selected. The model correctly responded to 73/88 questions (83.0%), with 61 (69.0%) graded as comprehensive. 15/88 (17%) responses were graded as mixed with correct and incorrect/outdated data. The model comprehensively responded to 10 (62.5%) questions related to “Nutrition and diet needs for surgery,” 12 (92.3%) “Tube feeding and parenteral nutrition,” 11 (64.7%) “General diet questions,” 10 (50%) “Diet for reducing symptoms/inflammation,” and 18 (81.8%) “Micronutrients/supplementation needs.” The model provided reproducible responses to 81/88 (92.0%) questions.
Conclusions
GPT-4 comprehensively answered most questions, demonstrating the promising potential of LLMs as supplementary tools for IBD patients seeking nutrition-related information. However, 17% of responses contained incorrect information, highlighting the need for continuous refinement prior to incorporation into clinical practice. Future studies should emphasize leveraging LLMs to enhance patient outcomes and promoting patient and healthcare professional proficiency in using LLMs to maximize their efficacy.
Keywords: ChatGPT, GPT-4, nutrition, dietitian, IBD
Graphical Abstract
Graphical Abstract.
Introduction
Inflammatory bowel disease (IBD), which includes Crohn’s disease (CD) and ulcerative colitis, are chronic, often debilitating conditions impacting an estimated 4.9 million cases worldwide.1 Prevalence is highest in the United States and China with studies showing a rising incidence in newly industrialized nations that have adopted more Western lifestyles1,2
Nutrition plays an important role in the management of patients with IBD, not only influencing disease activity but also impacting overall patient outcomes given the increased risk for malnutrition and micronutrient deficiencies in this patient population.3,4 Proper nutritional interventions, such as exclusive enteral nutrition (EEN) can alleviate symptoms, reduce the need for medications, and promote mucosal healing, thus improving their quality of life.4–7 Furthermore, diet and lifestyle modifications can influence the course of these diseases by modulating gut microbiota, inflammatory responses, and disease-related complications.8
The important role of nutrition in IBD underscores a pressing need for effective patient education in this domain. Patient surveys have consistently indicated a strong demand for comprehensive nutrition guidance and education, both in general and within the IBD community.9 One study of IBD patients showed 15.4% (86/559) of patients did not talk to any provider about nutrition while 15.5% (63/407) rarely entered discussion with their healthcare providers regarding this subject. When asked the reason for the lack of discussion, 31.3% (21/67) of patients felt their provider did not have enough time during clinical visits while 20.9% (14/67) reported feeling their provider lacked the requisite expertise on the subject.10 Moreover, studies show patients frequently turn to external sources of information in lieu of their healthcare providers.11,12 More and more patients are seeking information about their disease from online sources, and this trend is anticipated to grow.13 Despite this demand, there is variable access to high-quality IBD-specific dietary information available to patients.14 Furthermore, when navigating online sources patients are confronted with both high-quality information as well as misinformation that may be harmful, a dichotomy that often makes it challenging to distinguish between valid medical guidance from erroneous or misleading advice.
Large language models (LLMs), like ChatGPT, may revolutionize the way information is accessed and disseminated. These models have the potential in assisting patients with IBD by helping them navigate the complex landscape of nutrition information. Personalized dietary recommendations can play a pivotal role in managing IBD, and LLMs may offer an accessible platform for patients to receive timely and pertinent information. While not a replacement for professional medical advice, LLMs can serve as a complementary resource by providing general dietary guidelines and addressing common nutritional queries. Studies have shown the impressive ability of ChatGPT in answering clinical questions on a wide range of topics including cirrhosis, bariatric surgery, laryngology, and orthopedic surgery.15–18 Studies have also examined the performance of LLMs in gastroenterology with a recent study showing generative pre-trained transformer-4 (GPT-4) surpassed the passing grade threshold and average human test taker performance on the American College of Gastroenterology self-assessment.19 There is a growing body of evidence demonstrating the strength and limitations of LLMs across multiple topics in gastroenterology including IBD.20–24 One recent study showed ChatGPT has promise in providing appropriate answers to questions related to the dietary management of IBD although the study was limited by a small number of questions evaluated (n = 6).25
This study aims to expand on the current literature by examining the accuracy, comprehensiveness, and reproducibility of ChatGPT when answering nutrition-related questions in IBD. Examining the performance of LLMs, like ChatGPT, in the realm of nutrition will be important to understanding the future role and limitations of this technology.
Materials and Methods
Question Selection/Data Source
All questions posed during adult patient clinic visits with IBD-focused registered dietitians at a tertiary academic hospital, Facebook groups (“Crohn’s and Colitis Food, recipes, Diet, and Nutrition,” “Crohn’s Disease & Ulcerative Colitis Support Group,” “Crohn’s Disease Support Group”), and Reddit pages (“r/CrohnsDisease,” “r/IBD”) during the month of February 2023 were considered for inclusion. Questions were obtained, screened, and approved by three authors (C.F., E.F., K.I.) to evaluate their inclusion in the study. Only nutrition questions related to IBD were selected. Duplicate and similar questions from multiple sources were removed. Questions requiring subjective or personalized responses (ex.) and questions that were vague (ex.) were rephrased to a generic language format to allow for inclusion in the study. Other questions were grammatically modified to eliminate ambiguity. A total of 88 questions were selected and used to generate responses from GPT-4. To better characterize GPT-4’s performance in various topics within IBD nutrition, questions were categorized into multiple groups for statistical analysis purposes: (1) Nutrition and diet need for surgery, (2) tube feeding and parenteral nutrition, (3) general diet questions, (4) diet for reducing symptoms/inflammation, and (5) micronutrients/supplementation needs. Approval from the institutional review board was not sought given all questions are publicly available.
ChatGPT
ChatGPT is an LLM trained using an expansive dataset from various sources such as online websites, books, and articles up to the year 2021 at the time of data collection, including the medical literature.26 GPT-4, or Generative Pre-trained Transformer-4, was released in March of 2023 and is the fourth iteration of the GPT series. Based on a given input, the model generates responses that are easy-to-understand and conversational in nature.27 By leveraging billions of sentences from diverse internet sources, GPT-4 can engage in complex conversations, answer questions, write essays, and even generate creative content like stories or poems. Its developers employed Reinforcement Learning from Human Feedback to optimize the model, ensuring it effectively responds to a wide range of commands and written inquiries. This fine-tuning was driven by human preferences, which served as a reward signal, ensuring the model’s alignment with user intent and desired outcomes.28 The model has been fine-tuned to resonate with user goals and to reduce biased, or potentially harmful outputs. The exact origins of the data used to train ChatGPT remain undisclosed. As a product of extensive research and refinement, this model has found applications across various industries with growing literature highlighting its potential use in the field of healthcare.
Response Generation
Each question was prompted to the March 14, 2023 version of GPT-4 to generate responses. GPT-4 was accessed using the OpenAI website interface. Default model settings (temperature, max token size, etc.) were used. Questions were entered into the model without additional prompting in order to emulate the manner in which patients may potentially engage with the model. Every question was entered twice at different times using the “new chat” feature, yielding two responses for each question. This approach aimed to assess the reproducibility of responses to the same question.
Question Grading
Responses to the questions underwent an initial evaluation for accuracy, comprehensiveness, and reproducibility by two actively practicing IBD-focused registered dietitians in a tertiary care center (E.F. and C.F.). In instances of disagreement regarding reproducibility or accuracy grading, a third reviewer who has 10 years of experience as a clinical dietitian working with IBD patients at a tertiary care center arbitrated (K.I.). Given GPT-4’s training data were limited to information prior to September 2021, the reviewers used this date as a benchmark for assessing accuracy and comprehensiveness. This meant, the model was not critiqued on any guidelines (American, European, etc.) or scientific literature published after this date.
Accuracy and comprehensiveness were graded using a grading scale used in previous studies15,16,29–31:
Comprehensive: Defined as a response meeting two criteria: (1) contains only accurate information without any inaccurate information, (2) contains comprehensive information, nothing more a registered dietitian would add if asked this question by a patient in the clinic.
Correct but inadequate: Defined as a response meeting two criteria: (1) contains only accurate information without any inaccurate information, (2) does not contain comprehensive information, a registered dietitian would have more important information to add if asked this question by a patient in clinic.
Mixed with correct and incorrect/outdated data
Completely incorrect: No correct information was provided.
Reproducibility was assessed by examining the similarity in accuracy between the two responses provided for each question. To assess reproducibility, both responses for each question were categorized into two categories based on the presence of incorrect information: grades comprehensive and correct but inadequate formed the first category, while grades of mixed with correct and incorrect/outdated data and completely incorrect made up the second. A pair of responses to a question were deemed non-reproducible if their respective grades belonged to separate categories.
Statistical Analysis
The proportions of responses earning each grade were calculated and shown as counts and percentages. All analyses were conducted using Microsoft Excel. (version 16.69.1).
Results
In total, 88 nutrition questions related to IBD were inputted into GPT-4. The model performed well overall in terms of accuracy and provided correct responses to 73/88 questions (83.0%), with 61 (69.0%) of responses graded as comprehensive. For example, the model provided a comprehensive summary of EEN that is clear, concise, comprehensive, and accurate. This included a summary of the route of administration, avoidance of consumption of solids, nutritional content of EEN, its impact on mucosal healing, length of administration, reintroduction of solids, and its efficacy in inducing remission, particularly in children and adolescents. Another example of a comprehensive response is an important and common questions asked by patients regarding taking vitamins and minerals despite normal laboratory values. The model first stressed the importance of monitoring nutrient deficiencies in patients with IBD and the temptation by patients to discontinue these supplements when laboratory tests reveal normal values. The model then advised the user to consult with their healthcare professional who will consider the patient’s medical history, medications, and IBD disease status prior to making such a decision.
A total of 15/88 (17.0%) responses were graded as mixed with correct and incorrect/outdated data while no responses were graded as completely incorrect. For example, the model was asked about diet recommendations for IBD patients, which is one of the most common questions encountered in the IBD clinic. The model offered various suggestions that are not necessarily applicable to all patients with IBD. For example, a low-fat and lactose-free diet may only be suitable for a limited subset of these patients. Furthermore, the model recommended a low residue diet, often conflated with “low fiber” diet, which is not recognized as a diet by the Academy of Nutrition and Dietetics due to the lack of definition and therefore inability to accurately measure from available data.32 This also contradicts the current International Organization for the Study of IBD Diet Guidelines, which recommend patients with IBD consume more fiber. These recommendations may lead to confusion or unnecessary nutritional restrictions for patients and ultimately to worse outcomes. Another example is the model stating “a plant-based diet is not a guaranteed cure” when asked if a plant-based diet is a cure for IBD. This is inaccurate as it suggests that a plant-based diet may sometimes cure IBD.
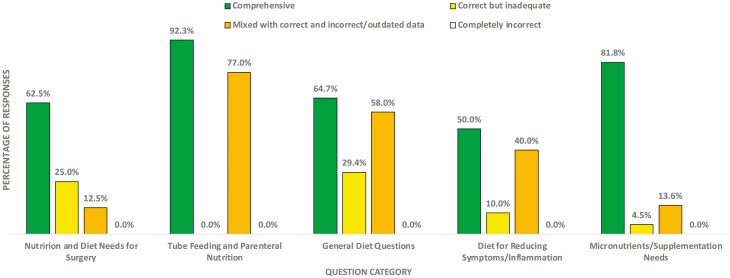
When examined by question category, the model provided comprehensive responses to 10 (62.5%) questions related to “Nutrition and diet needs for surgery,” 12 (92.3%) “Tube feeding and parenteral nutrition,” 11 (64.7%) “General diet questions,” (50%) “Diet for reducing symptoms/inflammation,” and 18 (81.8%) to “Micronutrients/Supplementation needs” (Table 1, Figure 1). The percentage of comprehensive responses was lowest among questions regarding “Diet for reducing symptoms/inflammation” at 50% and highest among questions regarding “Tube feeding and parenteral nutrition” at 92.3%.
Table 1.
Grading of responses generated by GPT-4 to nutrition questions related to IBD stratified by question category.
| Question Category and Grading Scale | Number of responses (%) |
|---|---|
| Nutrition and diet needs for surgery (N = 16) | |
| 1. Comprehensive | 10 (62.5) |
| 2. Correct but inadequate | 4 (25.0) |
| 3. Mixed with correct and incorrect/outdated data | 2 (12.5) |
| 4. Completely incorrect | 0 |
| Tube feeding and parenteral nutrition (N = 13) | |
| 1. Comprehensive | 12 (92.3) |
| 2. Correct but inadequate | 0 |
| 3. Mixed with correct and incorrect/outdated data | 1 (7.7) |
| 4. Completely incorrect | 0 |
| General diet questions (N = 17) | |
| 1. Comprehensive | 11 (64.7) |
| 2. Correct but inadequate | 5 (29.4) |
| 3. Mixed with correct and incorrect/outdated data | 1 (5.8) |
| 4. Completely incorrect | 0 |
| Diet for reducing symptoms/inflammation (N = 20) | |
| 1. Comprehensive | 10 (50.0) |
| 2. Correct but inadequate | 2 (10.0) |
| 3. Mixed with correct and incorrect/outdated data | 8 (40.0) |
| 4. Completely incorrect | 0 |
| Micronutrients/supplementation needs (N = 22) | |
| 1. Comprehensive | 18 (81.8) |
| 2. Correct but inadequate | 1 (4.5) |
| 3. Mixed with correct and incorrect/outdated data | 3 (13.6) |
| 4. Completely incorrect | 0 |
Figure 1.
Graphical illustration of grading of responses generated by GPT-4 to nutrition questions related to IBD stratified by question category.
The model provided overall high reproducibility in accuracy with 81/88 (92.0%) of questions generating reproducible responses. When examined by question category, the model provided reproducible responses to 100% of questions related to “Tube feeding and parenteral nutrition” (100%), 94.1% “General diet questions,” 90.0% “Diet for reducing symptoms/inflammation,” 95.4% “Micronutrients/Supplementation needs,” and 81.3% “Nutrition and diet needs for surgery” (Table 2).
Table 2.
Proportion of nutrition questions related to IBD with reproducible grading of responses generated by GPT-4 stratified by question category.
| Question categories | Number of responses (%) |
|---|---|
| Nutrition and diet needs for surgery (N = 16) | 13 (81.3%) |
| Tube feeding and parenteral nutrition (N = 13) | 13 (100.0%) |
| General diet questions (N = 17) | 16 (94.1%) |
| Diet for reducing symptoms/inflammation (N = 20) | 18 (90.0%) |
| Micronutrients/supplementation needs (N = 22) | 21 (95.4%) |
Reproducibility was defined as no difference in grading categories (comprehensive and correct but inadequate vs mixed with correct and incorrect/outdated data and completely incorrect) between the two responses for each question.
Discussion
The increasing global prevalence of IBD, coupled with the important role of nutrition in its management, underscores the importance of reliable and accessible nutrition-related patient educational resources. Our study evaluated the accuracy, comprehensiveness, and reproducibility of GPT-4’s responses to patient nutrition questions related to IBD. The model provided accurate and reproducible responses to the majority of questions prompted, highlighting the future potential of LLMs as a complementary source of information related to nutrition for IBD patients. However, the model provided inaccurate information in 17% of responses, underscoring the need for further improvement in performance prior to its introduction into clinical practice. With future iterations and improvements in performance, we see this technology as a supplementary tool rather than a substitute for advice from licensed healthcare professionals.
Individuals with IBD place significant emphasis on their diet, frequently implementing self-imposed dietary limitations.33–35 Subsequently, patients frequently seek nutritional guidance and turn to external sources in lieu of their healthcare providers with one study revealing that IBD patients were most confident in advice from online sources when experiencing active disease.11,12,33 The quality and reliability of information available online are either limited or frequently inconsistent. Using conventional online search engines provides patients with an abundance of information from a variety of sources, making distinguishing reliable information both difficult and time consuming. As the disease predominantly affects young adults with high computer literacy, the potential impact of online resources, like LLMs, becomes increasingly significant. This provides urgency in examining the role of LLMs in nutrition-related patient education in order to understand the strengths and limitations of this technology. A recent study evaluated the accuracy of three LLMs, including ChatGPT, in answering 6 IBD dietary management questions with promising results. Two physician reviewers found ChatGPT answered most questions appropriately.25 Our study builds on these findings with a larger sample of questions as well as utilizing actively practicing academic dietitian reviewers. GPT-4 provided accurate and comprehensive responses to the majority of questions in our study, highlighting a promising potential for LLMs in the realm of patient education. The reproducibility of GPT-4’s responses in our study, which exceeded 80% across all categories, is also noteworthy and crucial for building trust among users and ensuring consistently accurate information. If validated, LLMs like ChatGPT may serve as an easy-to-understand and efficient tool for patients to obtain reliable supplemental information based on the medical literature.
Its also important to highlight the limitations of GPT-4, as seen in our study. The model provided incorrect or outdated information in 17% of responses which demonstrates its lack of readiness for clinical use in its current form. There are multiple possible reasons for this. ChatGPT’s training includes data from a wide range of sources, some of which may not be accurate, leading to potential inaccuracies in its outputs. Moreover, the data sources used to train the model have not been publicly disclosed making critical appraisal of its knowledge base regarding a particular topic not possible. Even when accessing information from the medical literature in its training data, the model may emphasize or utilize conflicting or outdated information resulting in inaccurate or inconsistent outputs. Prompting strategies may also play a role in the quality of responses. For our investigation, we pursued a pragmatic study design where real-world patient questions were obtained from our IBD clinic and online sources and subsequently inputted into GPT-4 without additional prompting. This is likely not the optimal prompting method to produce the highest quality outputs from LLMs. We hypothesize that more advanced prompt engineering would likely produce higher quality responses, both in accuracy and comprehensiveness. In light of this, the design of intuitive, precise prompts for both patients and healthcare providers may be an effective strategy in harnessing the full potential of LLMs, as it ensures these tools deliver relevant, accurate information to specific medical contexts. By educating both groups on effective prompt crafting, we can greatly enhance the quality of interactions with LLMs, potentially leading to improved patient outcomes, more efficient healthcare delivery, and a deeper integration of AI in healthcare.
If future iterations of this technology are validated for clinical use, they may have a significant impact on the patient experience and healthcare outcomes. The timely accessibility of healthcare providers, particularly dietitians and IBD specialists, remains a consistent hurdle for many IBD patients.36–38 This can not only exacerbate delays in care and result in potentially detrimental outcomes, but also augment the challenges of patients navigating through the sea of inaccurate or insufficient online information. These barriers may also disrupt the proactive efforts of informed patients, leading to misguided actions based on flawed knowledge. In the future, patients equipped with accurate and holistic knowledge from LLMs may be able to streamline in-person appointments with more focused questions, allowing healthcare providers to focus on patient-specific concerns.39 Moreover, empowering patients with more information can potentially foster a greater sense of autonomy among patients, encouraging them to initiate discussions regarding nutrition with their healthcare providers. This, in turn, may help promote the focus on nutrition during clinic visits, and potentially increase the rate of referrals to dietitians.
LLMs may also help bridge healthcare disparities by democratizing access to health information. Barriers to care, such as lengthy wait times and inaccessibility to a dietician or IBD specialist, are even more pronounced in patients of minority backgrounds, which can further exaggerate disparities and lead to delays in diagnosis and treatment.40 LLMs may empower these patients with knowledge regarding their disease, giving them a tool that helps them proactively engage with their healthcare providers. LLMs may also prove beneficial to patients who have language discordance with their healthcare providers, given disparities in healthcare outcomes based on language preference have been previously shown.41,42 ChatGPT’s ability to provide patient education in languages other than English is an active area of research with some studies demonstrating its ability to respond to inquiries related to cirrhosis in Arabic, Korean, Mandarin, and Spanish.31,43,44 LLMs can provide a valuable resource for these patients, and potentially serve to mitigate disparities in outcomes.
Limitations and Future Directions
This study had several limitations. First, the selection of 88 questions, though reflective of common patient inquiries, was not exhaustive and did not encompass all possible topics that patients may ask. Modifications to the grammar or context of certain questions were made to improve the clarity for GPT-4, which does not reflect the variability and ambiguity often present in patient inquiries in real-world settings. In practice, LLMs have the ability to request clarification from users, a feature that was not incorporated into the study design, potentially affecting the model’s performance under real-world conditions. Duplicate questions were removed during screening which introduced the potential for selection bias. LLMs may respond differently to different wording of the same question. Another limitation is the subjective nature of the grading scale and reviewers used in our study. Although experienced registered dietitians independently graded the responses, future research should prioritize the development of more objective and standardized methods to evaluate accuracy, comprehensiveness, and reproducibility. Moreover, only registered dietitians were involved in the review process, which may limit the scope of the evaluation. Future studies would benefit from a multidisciplinary panel of healthcare provider reviewers in addition to patients, to provide a more holistic assessment of the quality and relevance of GPT-4’s responses.
Looking ahead, further avenues of research should aim towards ameliorating the inaccuracies and limitations of this technology as revealed by our study. While ChatGPT can provide answers to general IBD nutrition-related questions, it lacks the ability to comprehensively assess individual health status, address behavioral needs, or monitor progress over time. IBD can vary significantly from person to person in terms of symptoms, triggers, and nutritional needs. Registered dietitians can assess individual cases, considering medical history, current medications, symptom severity, and tailor nutrition advice to the individuals’ specific needs and goals. While the model’s linguistic prowess is commendable, it can sometimes produce responses that sound convincing but may be incorrect or nonsensical, a phenomenon termed “hallucinations.” Continuous feedback and iterative improvements are essential to minimize these limitations. Considering the growing popularity of LLMs and their potential in delivering patient education, it’s imperative to further study and validate their utility. The role of dieticians and physicians in managing patients with IBD remains critical to positive outcomes, and further research should investigate ways in which collaborations between AI-models and the healthcare team can benefit our patients.
Conclusion
Generative pre-trained transformer-4 provided accurate and comprehensive responses to the majority of nutrition questions related to IBD, demonstrating the promising potential of LLMs as supplementary tools for IBD patients seeking nutrition-related information. It is important to note that 17% of responses contained incorrect information, highlighting the need for continuous refinement and validation of LLMs prior to their incorporation into clinical practice. Going forward, it’s essential to approach the use of LLMs as an adjunct to professional medical advice. Future studies should focus on leveraging LLMs to enhance patient outcomes in the realm of IBD nutrition. Furthermore, efforts towards promoting patient and healthcare professional proficiency in using LLMs are essential to maximizing their impact and personalization.
Contributor Information
Jamil S Samaan, Department of Medicine, Karsh Division of Digestive and Liver Diseases, Cedars-Sinai Medical Center, Los Angeles, CA, USA.
Kelly Issokson, Department of Medicine, Karsh Division of Digestive and Liver Diseases, Cedars-Sinai Medical Center, Los Angeles, CA, USA.
Erin Feldman, Department of Medicine, Karsh Division of Digestive and Liver Diseases, Cedars-Sinai Medical Center, Los Angeles, CA, USA.
Christina Fasulo, Department of Medicine, Karsh Division of Digestive and Liver Diseases, Cedars-Sinai Medical Center, Los Angeles, CA, USA.
Nithya Rajeev, Keck School of Medicine of USC, Los Angeles, CA, USA.
Wee Han Ng, Bristol Medical School, University of Bristol, Bristol, UK.
Barbara Hollander, Department of Medicine, Karsh Division of Digestive and Liver Diseases, Cedars-Sinai Medical Center, Los Angeles, CA, USA.
Yee Hui Yeo, Department of Medicine, Karsh Division of Digestive and Liver Diseases, Cedars-Sinai Medical Center, Los Angeles, CA, USA.
Eric Vasiliauskas, Department of Medicine, Karsh Division of Digestive and Liver Diseases, Inflammatory Bowel and Immunobiology Research Institute, Cedars-Sinai Medical Center, Los Angeles, CA, USA.
Author Contributions
J.S.S.: Conceived and designed the study, manuscript preparation. K.I.: Question curation, response grading, edited the paper for important intellectual content. E.F.: Question curation, response grading, edited the paper for important intellectual content. C.F.: Question curation, response grading, edited the paper for important intellectual content. W.N.: Data management, statistical analysis, edited the paper for important intellectual content. N.R.: Assisted with manuscript preparation, edited the paper for important intellectual content. B.H.: Edited the paper for important intellectual content. Y.Y.: Edited the paper for important intellectual content. E.V.: Edited the paper for important intellectual content.
Funding
None declared.
Conflicts of Interest
The authors J.S.S., E.F., C.F., W.N., N.R., B.H., Y.Y., and E.V. declare that they have no conflict of interest. K.I. holds the position of associate Editor of Diet and Nutrition for Crohn’s & Colitis 360 and has been recused from reviewing or making decisions for the manuscript. K.I. is also a consultant for Takeda.
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed Consent Statement
Informed Consent does not apply.
Declaration of AI and AI-Assisted Technologies in the Writing Process
During the preparation of this work, the authors used GPT-4 in order to improve readability and language. After using this tool/service, the authors reviewed and edited the content as needed and took full responsibility for the content of the publication.
Data Availability
Data not publicly available.
References
- 1. Wang R, Li Z, Liu S, Zhang D.. Global, regional and national burden of inflammatory bowel disease in 204 countries and territories from 1990 to 2019: a systematic analysis based on the Global Burden of Disease Study 2019. BMJ Open. 2023;13(3):e065186. doi: https://doi.org/ 10.1136/bmjopen-2022-065186 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Ng SC, Shi HY, Hamidi N, et al. Worldwide incidence and prevalence of inflammatory bowel disease in the 21st century: a systematic review of population-based studies. Lancet (London, England). 2017;390(10114):2769-2778. doi: https://doi.org/ 10.1016/S0140-6736(17)32448-0 [DOI] [PubMed] [Google Scholar]
- 3. Hashash JG, Elkins J, Lewis JD, Binion DG.. AGA clinical practice update on diet and nutritional therapies in patients with inflammatory bowel disease: expert review. Gastroenterology. 2024;166(3):521-532. doi: https://doi.org/ 10.1053/j.gastro.2023.11.303 [DOI] [PubMed] [Google Scholar]
- 4. Bischoff SC, Escher J, Hébuterne X, et al. ESPEN practical guideline: clinical nutrition in inflammatory bowel disease. Clin Nutr (Edinburgh, Scotland). 2020;39(3):632-653. doi: https://doi.org/ 10.1016/j.clnu.2019.11.002 [DOI] [PubMed] [Google Scholar]
- 5. Richman E, Rhodes JM.. Review article: evidence-based dietary advice for patients with inflammatory bowel disease. Aliment Pharmacol Ther. 2013;38(10):1156-1171. doi: https://doi.org/ 10.1111/apt.12500 [DOI] [PubMed] [Google Scholar]
- 6. Lee D, Albenberg L, Compher C, et al. Diet in the pathogenesis and treatment of inflammatory bowel diseases. Gastroenterology. 2015;148(6):1087-1106. doi: https://doi.org/ 10.1053/j.gastro.2015.01.007 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Whelan K, Murrells T, Morgan M, et al. Food-related quality of life is impaired in inflammatory bowel disease and associated with reduced intake of key nutrients. Am J Clin Nutr. 2021;113(4):832-844. doi: https://doi.org/ 10.1093/ajcn/nqaa395 [DOI] [PubMed] [Google Scholar]
- 8. Lewis JD, Abreu MT.. Diet as a trigger or therapy for inflammatory bowel diseases. Gastroenterology. 2017;152(2):398-414.e6. doi: https://doi.org/ 10.1053/j.gastro.2016.10.019 [DOI] [PubMed] [Google Scholar]
- 9. Limdi JK, Aggarwal D, McLaughlin JT.. Dietary practices and beliefs in patients with inflammatory bowel disease. Inflamm Bowel Dis. 2016;22(1):164-170. doi: https://doi.org/ 10.1097/MIB.0000000000000585 [DOI] [PubMed] [Google Scholar]
- 10. Tinsley A, Ehrlich OG, Hwang C, et al. Knowledge, attitudes, and beliefs regarding the role of nutrition in IBD among patients and providers. Inflamm Bowel Dis. 2016;22(10):2474-2481. doi: https://doi.org/ 10.1097/MIB.0000000000000901 [DOI] [PubMed] [Google Scholar]
- 11. Bernstein KI, Promislow S, Carr R, Rawsthorne P, Walker JR, Bernstein CN.. Information needs and preferences of recently diagnosed patients with inflammatory bowel disease. Inflamm Bowel Dis. 2011;17(2):590-598. doi: https://doi.org/ 10.1002/ibd.21363 [DOI] [PubMed] [Google Scholar]
- 12. Limdi JK, Butcher RO.. Information resources and inflammatory bowel disease. Inflamm Bowel Dis. 2011;17(8):E89-E90. doi: https://doi.org/ 10.1002/ibd.21749 [DOI] [PubMed] [Google Scholar]
- 13. Cima RR, Anderson KJ, Larson DW, et al. Internet use by patients in an inflammatory bowel disease specialty clinic. Inflamm Bowel Dis. 2007;13(10):1266-1270. doi: https://doi.org/ 10.1002/ibd.20198 [DOI] [PubMed] [Google Scholar]
- 14. Prince AC, Moosa A, Lomer MCE, Reidlinger DP, Whelan K.. Variable access to quality nutrition information regarding inflammatory bowel disease: a survey of patients and health professionals and objective examination of written information. Health Expect. 2015;18(6):2501-2512. doi: https://doi.org/ 10.1111/hex.12219 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. Yeo YH, Samaan JS, Ng WH, et al. Assessing the performance of ChatGPT in answering questions regarding cirrhosis and hepatocellular carcinoma. Clin Mol Hepatol. 2023;29(3):721-732. doi: https://doi.org/ 10.3350/cmh.2023.0089. Epub 2023 Mar 22. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16. Samaan JS, Yeo YH, Rajeev N, et al. Assessing the accuracy of responses by the language model ChatGPT to questions regarding bariatric surgery [Internet]. Obes Surg. 2023;33(6):1790-1796. doi: https://doi.org/ 10.1007/s11695-023-06603-5. Cited May 29, 2023. Available from: https://link.springer.com/10.1007/s11695-023-06603-5 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Lechien JR, Georgescu BM, Hans S, Chiesa-Estomba CM.. ChatGPT performance in laryngology and head and neck surgery: a clinical case-series [Internet]. Eur Arch Otorhinolaryngol. 2024Jan;281(1):319-333. doi: https://doi.org/ 10.1007/s00405-023-08282-5. Epub 2023 Oct 24. PMID: 37874336. [DOI] [PubMed] [Google Scholar]
- 18. Kaarre J, Feldt R, Keeling LE, et al. Exploring the potential of ChatGPT as a supplementary tool for providing orthopaedic information. Knee Surg Sports Traumatol Arthrosc. 2023;31(11):5190-5198. doi: https://doi.org/ 10.1007/s00167-023-07529-2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19. Samaan JS, Margolis S, Srinivasan N, et al. Multimodal large language model passes specialty board examination and surpasses human test-taker scores: a comparative analysis examining the stepwise impact of model prompting strategies on performance [Internet]. 2024. Cited September 21, 2024. Available from: http://medrxiv.org/lookup/doi/10.1101/2024.07.27.24310809 [Google Scholar]
- 20. Klang E, Sourosh A, Nadkarni GN, Sharif K, Lahat A.. Evaluating the role of ChatGPT in gastroenterology: a comprehensive systematic review of applications, benefits, and limitations. Therap Adv Gastroenterol. 2023;16. doi: https://doi.org/ 10.1177/17562848231218618 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Gravina AG, Pellegrino R, Cipullo M, et al. May ChatGPT be a tool producing medical information for common inflammatory bowel disease patients’ questions? An evidence-controlled analysis. World J Gastroenterol. 2024;30(1):17-33. doi: https://doi.org/ 10.3748/wjg.v30.i1.17 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22. Sciberras M, Farrugia Y, Gordon H, et al. Accuracy of Information given by ChatGPT for patients with inflammatory bowel disease in relation to ECCO guidelines. J Crohns Colitis. 2024;18(8):1215-1221. doi: https://doi.org/ 10.1093/ecco-jcc/jjae040 [DOI] [PubMed] [Google Scholar]
- 23. Ghersin I, Weisshof R, Koifman E, et al. Comparative evaluation of a language model and human specialists in the application of European guidelines for the management of inflammatory bowel diseases and malignancies. Endoscopy. 2024;56(09):706-709. doi: https://doi.org/ 10.1055/a-2289-5732 [DOI] [PubMed] [Google Scholar]
- 24. Gong EJ, Bang CS.. Evaluating the role of large language models in inflammatory bowel disease patient information. World J Gastroenterol. 2024;30(29):3538-3540. doi: https://doi.org/ 10.3748/wjg.v30.i29.3538 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25. Naqvi HA, Delungahawatta T, Atarere JO, Bandaru SK, Barrow JB, Mattar MC.. Evaluation of online chat-based artificial intelligence responses about inflammatory bowel disease and diet. Euro J Gastroenterol Hepatol. 2024;36(9):1109-1112. doi: https://doi.org/ 10.1097/MEG.0000000000002815 [DOI] [PubMed] [Google Scholar]
- 26. Openai. ChatGPT: Optimizing language models for dialogue. 2023. Accessed January 1, 2023. https://openai.com/index/chatgpt/ [Google Scholar]
- 27. OpenAI. GPT-4 Technical report. 2023. Cited August 11, 2023. Available from: https://arxiv.org/abs/2303.08774 [Google Scholar]
- 28. Ouyang L, Wu J, Jiang X, et al. Training language models to follow instructions with human feedback. 2022. Cited February 10, 2023. Available from: https://arxiv.org/abs/2203.02155 [Google Scholar]
- 29. King RC, Samaan JS, Yeo YH, et al. A Multidisciplinary assessment of ChatGPT’s knowledge of amyloidosis: observational study. JMIR Cardio. 2024;8:e53421. doi: https://doi.org/ 10.2196/53421 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30. King RC, Samaan JS, Yeo YH, Mody B, Lombardo DM, Ghashghaei R.. Appropriateness of ChatGPT in answering heart failure related questions. Heart Lung Circ. 2024;33(9):1314-1318. doi: https://doi.org/ 10.1016/j.hlc.2024.03.005 [DOI] [PubMed] [Google Scholar]
- 31. Samaan JS, Yeo YH, Ng WH, et al. ChatGPT’s ability to comprehend and answer cirrhosis related questions in Arabic. Arab J Gastroenterol. 2023;24(3):S1687197923000588. doi: 10.1016/j.ajg.2023.08.001 [DOI] [PubMed] [Google Scholar]
- 32. Cunningham E. Are low-residue diets still applicable? J Acad Nutr Diet. 2012;112(6):960. doi: https://doi.org/ 10.1016/j.jand.2012.04.005 [DOI] [PubMed] [Google Scholar]
- 33. Larussa T, Suraci E, Marasco R, Imeneo M, Abenavoli L, Luzza F.. Self-prescribed dietary restrictions are common in inflammatory bowel disease patients and are associated with low bone mineralization. Medicina (Kaunas, Lithuania). 2019;55(8):507. doi: https://doi.org/ 10.3390/medicina55080507 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34. Marsh A, Kinneally J, Robertson T, Lord A, Young A, Radford –Smith G.. Food avoidance in outpatients with inflammatory bowel disease – Who, what and why. Clin Nutr ESPEN. 2019;31:10-16. doi: https://doi.org/ 10.1016/j.clnesp.2019.03.018 [DOI] [PubMed] [Google Scholar]
- 35. Godala M, Gaszyńska E, Durko L, Małecka-Wojciesko E.. Dietary behaviors and beliefs in patients with inflammatory bowel disease. J Clin Med. 2023;12(10):3455. doi: https://doi.org/ 10.3390/jcm12103455 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36. Habashi P, Bouchard S, Nguyen GC.. Transforming access to specialist care for inflammatory bowel disease: the PACE telemedicine program. J. Can. Assoc. Gastroenterol.. 2019;2(4):186-194. doi: https://doi.org/ 10.1093/jcag/gwy046 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37. Borren NZ, Conway G, Tan W, et al. Distance to specialist care and disease outcomes in inflammatory bowel disease. Inflamm Bowel Dis. 2017;23(7):1234-1239. doi: https://doi.org/ 10.1097/MIB.0000000000001133 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38. Malter L, Jain A, Cohen BL, et al. Identifying IBD providers’ knowledge gaps using a prospective web-based survey. Inflamm Bowel Dis. 2020;26(9):1445-1450. doi: https://doi.org/ 10.1093/ibd/izaa032 [DOI] [PubMed] [Google Scholar]
- 39. Bickmore TW, Pfeifer LM, Paasche-Orlow MK.. Using computer agents to explain medical documents to patients with low health literacy. Patient Educ Couns. 2009;75(3):315-320. doi: https://doi.org/ 10.1016/j.pec.2009.02.007 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40. Liu JJ, Abraham BP, Adamson P, et al. The Current state of care for black and hispanic inflammatory bowel disease patients. Inflamm Bowel Dis. 2023;29(2):297-307. doi: https://doi.org/ 10.1093/ibd/izac124 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41. Al Shamsi H, Almutairi AG, Al Mashrafi S, Al Kalbani T.. Implications of language barriers for healthcare: a systematic review. Oman Med J. 2020;35(2):e122. doi: https://doi.org/ 10.5001/omj.2020.40 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42. Divi C, Koss RG, Schmaltz SP, Loeb JM.. Language proficiency and adverse events in US hospitals: a pilot study. Int J Qual Health Care. 2007;19(2):60-67. doi: https://doi.org/ 10.1093/intqhc/mzl069 [DOI] [PubMed] [Google Scholar]
- 43. Yeo YH, Samaan JS, Ng WH, et al. GPT-4 outperforms ChatGPT in answering non-english questions related to cirrhosis [Internet]. Cited July 29, 2023.Gastroenterology. 2023. Available from: http://medrxiv.org/lookup/doi/10.1101/2023.05.04.23289482 [Google Scholar]
- 44. Zhu Z, Ying Y, Zhu J, Wu H.. ChatGPT’s potential role in non-English-speaking outpatient clinic settings. Digital Health. 2023;9:20552076231184091. doi: https://doi.org/ 10.1177/20552076231184091 [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
Data not publicly available.