Abstract
Background
Complex abdominal wall reconstruction following multiple surgical interventions remains challenging in resource-limited settings. We report the first successful case of combined post-caesarean and post-laparotomy total abdominal wall reconstruction with mesh reinforcement in a low-to-middle-income country setting
Case presentation
A 27-year-old multipara Nigerian woman presented with severe abdominal wall laxity and aesthetic deformity following caesarean delivery complicated by cryptogenic ascites requiring exploratory laparotomy. Clinical examination revealed extensive abdominal wall weakness with positive diastasis recti (Diver’s test). She underwent comprehensive abdominal wall reconstruction, including total abdominoplasty with polypropylene mesh reinforcement. Intraoperative findings demonstrated diffuse muscle attenuation without discrete hernial defects. The procedure was completed without complications, with 0.8kg of excess tissue excised. The patient achieved complete wound healing by postoperative day 15 with excellent functional and aesthetic outcomes maintained at 15-month follow-up. No postoperative complications, mesh-related adverse events, or recurrence of abdominal wall laxity were observed.
Conclusion
This case demonstrates the feasibility and safety of complex abdominal wall reconstruction in resource-constrained environments when appropriate patient selection, surgical technique, and perioperative management are employed. The successful outcome challenges conventional assumptions about the technical requirements for such procedures and supports the expansion of reconstructive surgical services in low-resource settings
Keywords: Abdominoplasty, Exploratory Laparotomy, Mesh Repair, Sagging Abdomen, Satisfactory Healing
1. Introduction
Abdominal wall reconstruction, commonly referred to as abdominoplasty or a tummy tuck, is a surgical procedure designed to restore the functional and aesthetic integrity of the abdominal region. This procedure is often sought by patients following significant changes in abdominal morphology due to factors such as pregnancy, weight fluctuations, or, as in the case presented here, the resolution of ascites. Ascites, the abnormal accumulation of fluid in the peritoneal cavity, can lead to substantial distension of the abdominal wall, resulting in residual laxity and skin redundancy once the ascites resolves [1-4].
In low-income settings, the management of such conditions poses unique challenges due to limited resources, access to specialized care, and potential delays in intervention. These constraints can exacerbate the psychological and physical burden on patients who seek to restore their abdominal contour and function after conditions like ascites. The case of a 27-year-old Nigerian woman highlights the complexities involved in managing post-ascites abdominal wall reconstruction, particularly in a resource-limited environment. This report aims to discuss the surgical approach, challenges, and outcomes associated with the successful management of her case, while also considering the broader implications for similar interventions in low-income settings [5,6].
2. Case Presentation
2.1. Patient History and Clinical Presentation
A 27-year-old Nigerian woman presented with progressive abdominal wall laxity and aesthetic deformity, leading to considerable psychological distress and functional impairment. Her obstetric history was significant for three term deliveries, the most recent of which was via caesarean section. Following her last delivery, she developed marked ascites, prompting further investigation and eventual exploratory laparotomy through a sub-umbilical midline incision. The intraoperative findings were unremarkable, with no identifiable pathology to account for the ascites. The ascites resolved after about seven months, leaving her with a loose, sagging abdomen that affected her body shape and how her clothes fit. She has no history of diabetes, hypertension, smoking, or alcohol use, and there were no notable cardiovascular events or in her family history. She has completed her family and does not wish to have more children. With her husband’s support, she requested for abdominal wall repair and a tummy tuck.
2.2. Clinical Assessment
Upon admission, the patient was stable with vital signs: body temperature 36.1 °C, blood pressure 135/70 mmHg, pulse rate 78 beats per minute and regular, and peripheral oxygen saturation (SpO2) of 98%. Abdominal examination revealed significant skin redundancy and laxity, with visible surgical scars from both a Pfannenstiel incision and a sub-umbilical midline laparotomy. Palpation demonstrated marked diastasis recti, confirmed by a positive Diver’s test, indicating severe separation of the rectus abdominis muscles. There was generalised weakness of the abdominal wall, with loss of normal muscular tone and support. Laboratory investigations showed a haemoglobin level of 11.9 g/dL. Renal and liver function tests were within normal limits. Following comprehensive preoperative counselling and informed consent, the patient underwent total abdominoplasty with mesh reinforcement of the abdominal wall on February 10, 2024.
2.3. Intraoperative Findings and Surgical Technique
The patient was placed in a supine position under general anaesthesia. After aseptic preparation and draping, a standard low transverse incision was made, incorporating and excising the previous Pfannenstiel scar. Dissection proceeded through the subcutaneous tissue to the anterior rectus sheath. A meticulous dissection of the abdominal flap was carried out in the supraumbilical and infraumbilical regions, elevating the flap up to the costal margins and xiphoid process while preserving perforating vessels where possible. Particular care was taken during dissection around the umbilical stalk. The umbilicus was isolated on a generous cuff of subcutaneous tissue to maintain adequate vascularity and minimise the risk of necrosis. The abdominal wall was inspected and found to be uniformly thinned, with no evidence of herniation, fascial defects, or abnormal openings. However, there was a marked diastasis of the rectus abdominis muscles. Rectus sheath plication was performed using a non-absorbable interrupted suture technique to approximate the rectus muscles and reinforce the midline. A lightweight polypropylene mesh was placed in an onlay fashion to further strengthen the abdominal wall and reduce the risk of recurrence. Haemostasis was meticulously achieved throughout the procedure. Excess redundant skin and subcutaneous tissue were excised, with a total resection weight of 0.8 kg. No intraoperative complications occurred, and no blood transfusion was required. Closed-suction drains were not placed (Figure 1 to Figure 10). Instead, a crepe bandage was applied circumferentially to the abdominal wound site to support haemostasis, maintain the newly contoured abdominal profile, and reduce seroma formation. The umbilicus was repositioned and sutured in place after flap redraping. The procedure was completed successfully, and the patient was extubated in the operating room and transferred to the recovery unit in stable condition.
Figure 1:

The Abdominal Wall Before the Surgical Procedure
Figure 10:

15th Day Post-Operation Side View with Protective Dressing
2.4. Postoperative Management and Outcomes
After surgery, the patient was cared for in the jack-knife position (hips and knees flexed) for five days to minimize tension on the sutures, after which she was placed flat. Clexane was initiated 24 hours postoperatively and continued for nine days. Additionally, she underwent chest physiotherapy using a balloon technique. The patient also received intravenous ceftriaxone and metronidazole for 15 days as prophylactic antibiotic therapy. Her recovery was uneventful, with no signs of surgical site infection, wound dehiscence, or other complications. By postoperative day 15, she demonstrated satisfactory wound healing and was discharged home in stable condition with an aesthetically pleasing abdominal contour. Upon discharge, she was advised to avoid strenuous physical activities or exercises for at least four weeks to facilitate optimal healing and prevent disruption of the abdominal wall repair. At her most recent follow-up, fifteen months after the procedure, the patient remains well, with no recurrence of abdominal wall laxity or functional complaints. She reports significant improvement in her psychological well-being and body image.
3. Discussion
This case represents the first documented successful complex abdominal wall reconstruction addressing combined post-caesarean and post-laparotomy deformities in a resource-limited setting. The favourable outcome, achieved despite significant infrastructural limitations, challenges prevailing assumptions about the necessity of high-resource environments for performing such technically demanding procedures. It reinforces the feasibility and potential for expanding access to reconstructive surgical services in low- and middle-income countries (LMICs), thereby improving quality of life and functional outcomes for affected patients. The case of abdominal wall reconstruction presented here reveals several important considerations in the management of post-ascites abdominal deformities, particularly within the context of low-income settings. The patient, having undergone multiple pregnancies and a caesarean section, experienced significant abdominal wall distension secondary to ascites, which ultimately resolved but left her with an aesthetically displeasing and functionally compromised abdomen. The decision to pursue total abdominoplasty and mesh repair was made in response to these concerns, with an emphasis on restoring both form and function. Abdominoplasty in the context of post-ascites management is not without its challenges. The presence of prior surgical scars, as in this patient’s case, can complicate the procedure, increasing the risk of wound complications and affecting the aesthetic outcome. Additionally, the uniformly thinned abdominal wall muscles observed intraoperatively highlight the potential for compromised structural integrity, necessitating the use of mesh reinforcement to achieve a durable repair. The absence of any noticeable hernia or abnormal opening, despite the significant muscle thinning, is noteworthy and suggests that the ascites primarily contributed to diffuse weakness rather than focal defects [7,8].
Resource limitations in low-income settings can further complicate the management of such cases. The availability of appropriate surgical materials, such as polypropylene mesh, and postoperative care resources is often constrained, which can impact the overall success and safety of the procedure. Despite these challenges, the patient's outcome was favourable, with satisfactory healing and an aesthetically pleasing result reported six months postoperatively. This success underlines the importance of careful patient selection, meticulous surgical technique, and the provision of appropriate postoperative care, even in resource-limited environments. This case also highlights the psychosocial aspects of post-ascites abdominal wall reconstruction. The patient’s concerns about her appearance and the impact on her quality of life were significant motivators for seeking surgical intervention. The successful restoration of her abdominal contour not only addressed these concerns but also contributed positively to her overall well-being, reflecting the broader benefits of such procedures beyond mere physical repair. Patients with poor health including advanced cardiopulmonary disease, cirrhosis, and uncontrolled diabetes, are poor candidates for this procedure. Smoking is severely detrimental to the abdominoplasty, as the procedure requires an adequate blood supply. Many plastic surgeons consider current smoking a contraindication to the surgery. Unlike in our case, our patient had no history of diabetes mellitus, hypertension, smoking, or alcohol use, and there were no notable cardiovascular events in her family history. A crepe bandage was applied circumferentially on the abdominal wound sites to maintain the haemostasis and contour of the abdomen. There was no placement of closed-suction drainage systems. Placement of closed-suction drainage systems can help decrease the incidence of accumulation of these fluids anecdotally, though high-quality data are not available to demonstrate efficacy. As in our case, careful dissection of the umbilical stalk was done to maintain enough fat around the umbilicus to preserve adequate blood supply. Furthermore, effective haemostasis was ensured during surgery using diathermy prior to draping the abdominal flap. This, along with the tamponade effect created by the pre-trimmed abdominal flap, helps to reduce the risk of postoperative bleeding and eliminates the need for a drain, which often results in an additional puncture scar following removal and healing [9, 10].
3.1. Strengths and Limitations
This case report has several strengths. This case report is unique in addressing a dual post-caesarean and post-ascites abdominal deformity, managed successfully with total abdominoplasty and mesh repair in a low-income setting. It contributes valuable insights into feasible surgical options in under-resourced environments. The report highlights both the functional and psychological/aesthetic concerns of the patient, which are often neglected in resource-limited settings. This adds to its relevance for patient-centered care in global surgery. The case provides a clear and comprehensive description of the patient’s history, physical examination, intraoperative findings, and postoperative care. This level of detail is useful for practitioners in similar contexts seeking practical guidance. A follow-up of fifteen months demonstrating sustained improvement strengthens the credibility of the outcome and suggests durability of the surgical intervention. Finally, the report reveals that complex procedures like abdominoplasty can be done safely without sophisticated surgical tools or intensive postoperative care, which is critical information for surgeons in similar settings. Despite its strengths, this case report is subject to several important limitations. As a single-patient case, it inherently lacks generalisability. The findings cannot be extrapolated to the broader population of patients with similar conditions, particularly given the heterogeneity of clinical presentations, healthcare infrastructure, and socioeconomic contexts across low- and middle-income countries (LMICs). Outcomes achieved in this specific setting may not be reproducible elsewhere without similar resources, surgical expertise, and institutional support. Additionally, while the aesthetic and functional outcomes were described as satisfactory, no objectivetools, such as validated quality-of-life questionnaires or functional performance assessments, were used to quantify improvements. This limits the ability to rigorously evaluate the impact of the intervention on patient well-being. The follow-up period of fifteen months, though promising, remains relatively short to assess long-term complications associated with mesh implantation and complex abdominal wall reconstruction. Mesh-related complications, such as infection, erosion, chronic pain, and recurrence of abdominal wall laxity, can emerge years after surgery, reinforcing the need for prolonged surveillance. Furthermore, economic considerations were not systematically evaluated in this report. The cost-effectiveness of undertaking complex abdominal wall reconstruction in resource-constrained settings remains unclear. Comprehensive analyses incorporating direct medical costs, indirect costs (e.g., time off work), and metrics such as quality-adjusted life years (QALYs) would be essential for informing healthcare policy and prioritising resource allocation. Finally, the case report does not explore systemic enablers or barriers that influenced the patient's access to surgical care, such as affordability, healthcare infrastructure, insurance coverage, or policy-level facilitators. Understanding these contextual factors is crucial for scaling similar interventions in LMICs.
3.2. Future Directions
Future research should focus on expanding the evidence base for complex abdominal wall reconstruction in resource-limited environments. Key priorities include: First: collaborative research involving multiple institutions across diverse LMIC settings can help assess the reproducibility, safety, and outcomes of these surgical techniques. Standardised surgical protocols, outcome measures, and extended follow-up periods will be essential for generating robust data to inform clinical practice and policy. Second, there is a critical need to design and validate simplified, cost-effective surgical protocols tailored to LMICs. This includes exploring the use of alternative mesh materials, minimal or no-drain techniques, and streamlined perioperative pathways that maintain safety and effectiveness while reducing costs and logistical burdens. Third, investment in training programmes for surgeons and perioperative teams in LMICs is vital. Evaluating such capacity-building initiatives will ensure the sustainable expansion and maintenance of reconstructive surgical services in resource-poor settings. Fourth, establishing national or regional registries to track outcomes, complications, and patient satisfaction over time would enable better understanding of long-term durability, identify predictors of success or failure, and refine patient selection criteria. Fifth, implementation research should explore how to best integrate complex reconstructive surgery into existing health systems. This includes examining models of care delivery, cost-effectiveness, equitable access, and barriers and facilitators at the policy and community levels. Collectively, these directions will help ensure that life-enhancing reconstructive surgery becomes more accessible, sustainable, and evidence-driven in low-resource settings.
4. Conclusion
This case report documents the first successful case of combined post-caesarean and post-laparotomy total abdominal wall reconstruction and mesh repair reported in a low and middle-resource setting. The functional and aesthetic outcomes illustrate its feasibility and potential benefits, even within the constraints of a low-income setting. The successful outcome achieved in this patient demonstrates that with appropriate planning and execution, the challenges associated with these procedures can be effectively managed, leading to both functional and aesthetic restoration.
Figure 2:

The Flattening of Abdominal Wall Before the Procedure
Figure 3:

Abdominal Flap Raised
Figure 4:

On-Lay Mesh Done
Figure 5:

Tailoring and Excision
Figure 6:
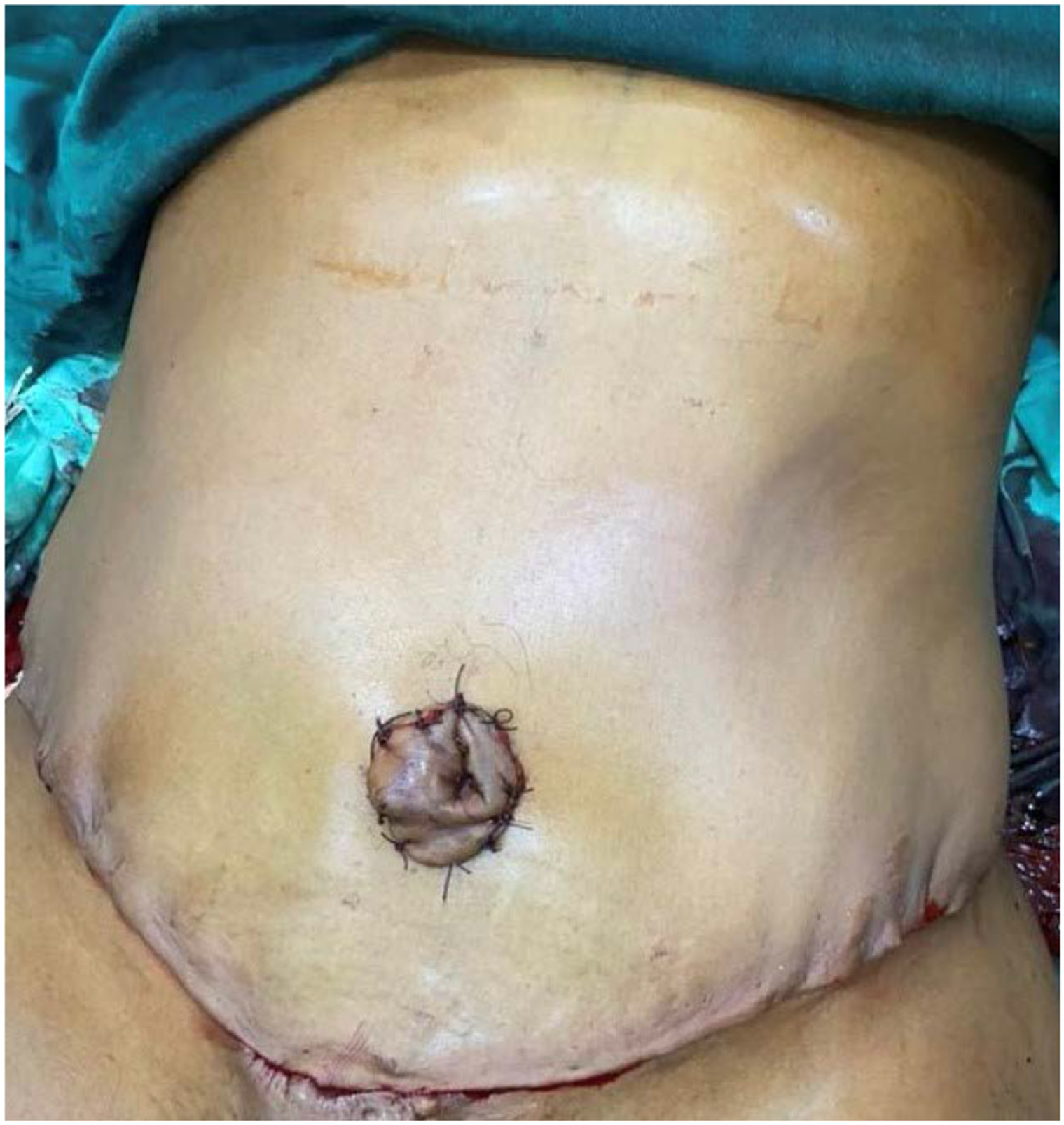
Immediate Post-Op
Figure 7:

5th Day Post-Operation
Figure 8:

10th Day Post-Operation
Figure 9:

15th Day Post-Operation with Neo Umbilicus Healed
Acknowledgements
The authors express their gratitude to the index patient for her informed consent to participate in this presentation (signed consent was obtained from her). We also appreciate Miracle Omeokachie for assisting in the nursing care of the patient.
Funding
No specific funding was received from funding agencies in the public, commercial or not-for-profit sectors.
Footnotes
Disclosure
The authors declare that there is no conflict of interest in this work.
Ethical Consideration
Our institution does not require ethical approval for reporting individual cases or case series.
Consent for Publication
Written informed consent was obtained from the patient for publication of her de-identified data and images.
Availability of Data and Materials
Data sharing is not applicable to this article as no datasets were generated or analysed during this study.
References
- 1.Huang Q, Li J, & Lau WY (2016). Techniques for abdominal wall closure after damage control laparotomy: from temporary abdominal closure to early/delayed fascial closure—a review. Gastroenterology research and practice, 2016(1), 2073260. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Swift RW, Matarasso A, & Rankin M. (2007). Abdominoplasty and abdominal contour surgery: A national plastic surgery survey. Plastic and reconstructive surgery, 119(1), 426–427. [DOI] [PubMed] [Google Scholar]
- 3.Rodriguez ED, Bluebond-Langner R, Silverman RP, Bochicchio G, Yao A, Manson PN, & Scalea T. (2007). Abdominal wall reconstruction following severe loss of domain: the R Adams Cowley Shock Trauma Center algorithm. Plastic and reconstructive surgery, 120(3), 669–680. [DOI] [PubMed] [Google Scholar]
- 4.Peralta R, & Latifi R. (2012). Long-term outcomes of abdominal wall reconstruction. What are the real numbers?. World journal of surgery, 36(3), 534–538. [DOI] [PubMed] [Google Scholar]
- 5.Runyon BA (2009). Management of adult patients with ascites due to cirrhosis: An update†‡ §. Hepatology, 49(6), 2087–2107. [DOI] [PubMed] [Google Scholar]
- 6.De Franchis R, & Faculty BV (2015). Expanding consensus in portal hypertension: Report of the Baveno VI Consensus Workshop: Stratifying risk and individualizing care for portal hypertension. Journal of hepatology, 63(3), 743–752. [DOI] [PubMed] [Google Scholar]
- 7.Jensen SAMS, Lauridsen SV, Fonnes S, Rosenberg J, & Tønnesen H. (2025). Effect of tailored, intensive prehabilitation for risky lifestyles before ventral hernia repair on postoperative outcomes, health, and costs–study protocol for a randomised controlled trial (STRONG-Hernia). PLoS One, 20(5), e0324002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Anusitviwat Y, Cheewatanakornkul S, Yolsuriyanwong K, Mahattanobon S, Laohawiriyakamol S, & Wangkulangkul P. (2025). Comparison of Laparoscopic eTEP-RS/TAR and IPOM Techniques for Ventral Hernia Repair. Journal of Abdominal Wall Surgery, 4, 14176. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Diener MK, Voss S, Jensen K, Büchler MW. (2020). Elective abdominal wall closure: the efficacy of onlay mesh versus no mesh—a multicenter randomized controlled trial. Lancet. 395(10225):913–21. [Google Scholar]
- 10.Zammit D, Safran T, Ponnudurai N, Jaberi M, Chen L, Noel G, & Gilardino MS (2020). Step-specific simulation: the utility of 3D printing for the fabrication of a low-cost, learning needs-based rhinoplasty simulator. Aesthetic Surgery Journal, 40(6), NP340–NP345. [DOI] [PubMed] [Google Scholar]


