Abstract
Participating centres:
Hospital Universitario San Juan, Alicante: Maria Jesús Olaso, Javier Agulló, Clara Faura.
Hospital Torrecárdenas, Almería: Carmen Fernández Sánchez, Miguel Lorenzo Campos, Juan Manuel Rodríguez Alonso.
Hospital Quirúrgic Adriano, Barcelona: Carmen Alerany Pardo, Paquita Alvarez González, Teresa Martín Benito.
Hospital Universitari del Mar-IMIM, Barcelona: Magí Farré, Maite Terán.
Corporació Sanitària Parc Taulí, Sabadell: Montserrat Cañellas, Sergio Zavala, Josep Planell.
Hospital Universitari de la Santa Creu i Sant Pau: Gonzalo Calvo, Rosa Morros, Silvia Mateo.
Hospital General Vall d’Hebron, Barcelona: Carmen Bosch, María José Martínez.
Hospital Universitario Virgen de la Victoria, Málaga: Maribel Lucena, José Antonio González, Gabriel Carranque.
Hospital Clínico Universitario San Carlos, Madrid: Emilio Vargas, Amparo Gil López-Oliva, Míriam García Mateos.
Hospital Universitario Marqués de Valdecilla, Santander: Mario González, Antonio Cuadrado.
Hospital Universitario Virgen de la Macarena, Sevilla: Juan Antonio Durán, Pilar Máyquez, María Isabel Serrano.
Hospital Universitario Virgen del Rocío, Sevilla: Jaume Torelló, Juan Ramón Castillo, María de las Nieves Merino.
Aims
Postoperative pain is common in hospital-admitted patients. Its management is determined by different therapeutic traditions and by the attitudes of health professionals in each hospital. The aim of this study was to describe the patterns of prescription and administration of analgesic drugs used for postoperative pain after abdominal surgery in Spanish hospitals, to know the prevalence and the severity of postoperative pain, and to determine the extent of variability in the management of postoperative pain among the participating centres.
Methods
The study was a multicentre descriptive cross-sectional drug utilization study in 12 Spanish hospitals. The subjects were an unselected sample of consecutive patients undergoing abdominal surgery, admitted between October 1994 and January 1995. For each patient, information about the surgical procedure and the use of analgesics was prospectively collected. The severity of postoperative pain was assessed during the first day after surgery by means of a six-category (none, mild, moderate, severe, very severe, and unbearable) rating scale and a visual analogue scale (VAS).
Results
Nine hundred and ninety-three patients (547 men) were included. The most common surgical procedures were inguinal hernia repair (315, 32%), cholecystectomy (268, 27%), appendectomy (140, 14%), bowel resection (137, 14%), and gastric surgery (58, 6%). Fifty-nine percent of patients (587) received nonopioid analgesics only, 9% (89) received opioid analgesics only, and 27% (263) received both opioid and nonopioid analgesics. The most frequently administered drugs were metamizole (667 patients) and pethidine (213 patients). Although in the majority of medical orders the administration of analgesics was scheduled at regular time intervals, the majority of actual doses were given ‘as-needed’. The average administered daily doses of all analgesics were lower than those prescribed. Thirty-eight percent (371/967) of patients rated their maximum pain on the first day as severe to unbearable. Wide interhospital variability was recorded in the surgical procedures which had been performed, in the analgesics used, and also in the pain scores referred by patients. The percentage of patients in each centre who suffered severe to unbearable pain varied from 22 to 67%.
Conclusions
In Spain many patients still suffer severe pain after abdominal surgery, and this seems to be due to an inadequate use of analgesics. Wide interhospital variability in the management of postoperative pain and in its prevalence was also recorded.
Keywords: analgesics, drug use evalutation, drug utilization studies, hospital, postoperative pain
Introduction
Postoperative pain is one of the most common therapeutic problems in hospitals [1–8]. It can increase morbidity, leading to reduced breathing and cough suppression, facilitating retained pulmonary secretions and pneumonia [9], and delaying normal gastric and bowel function [10], thus contributing to a longer recovery period [11]. Strategies aimed at reducing postoperative pain increase patients’ comfort and can shorten hospital stay, although this has not been shown by compelling evidence.
Pain is not an unavoidable consequence of surgery. In the majority of patients postoperative pain is preventable with adequate analgesics and by the appropriate use of newer techniques [2, 8, 11, 12]. Despite this, a number of surveys have shown a high prevalence of significant pain after surgery [13–19]. The recognition of the inadequacy of postoperative pain management has prompted the development of corrective efforts by surgeons, anaesthesiologists [5, 20–23], and pain management groups [2, 3, 24, 25].
Studies where the pattern of use of analgesics has been examined in relation to their actual impact on the prevalence and severity of postoperative pain have generally included few patients and have been carried out in one single hospital. The Spanish Society of Clinical Pharmacology set up a Study Group on Postoperative Analgesia, with the following objectives: (1) to identify the most commonly used analgesic drugs in the treatment of postoperative pain after abdominal surgery; (2) to estimate the prevalence and the severity of postoperative pain, and (3) to investigate the extent of interhospital variability in the patterns of use of analgesic drugs and in the severity of postoperative pain.
Methods
Twelve Spanish hospitals participated in this cross-sectional multicentre drug utilization study: Hospital Universitario San Juan (Alicante), Hospital Torrecárdenas (Almería), Hospital Quirúrgic Adriano (Barcelona), Hospital Universitari del Mar (Barcelona), Corporació Sanitària Parc Taulí (Sabadell), Hospital Universitari de la Santa Creu i de Sant Pau (Barcelona), Hospital General Vall d’Hebron (Barcelona), Hospital Universitario Virgen de la Victoria (Málaga), Hospital Clínico Universitario San Carlos (Madrid), Hospital Universitario Marqués de Valdecilla (Santander), Hospital Universitario Virgen de la Macarena (Sevilla), and Hospital Universitario Virgen del Rocío (Sevilla). The study was approved by the Executive Committee of the General Assembly of the Spanish Society of Clinical Pharmacology.
A sample of 50–100 consecutive patients, admitted between October 1994 and January 1995 who had undergone abdominal surgery and gave informed consent were included in the study. Patients admitted to Intensive Care Units after the operation were excluded. Information on age, sex, previous or associated diseases and surgical procedure was obtained from the clinical records and by interviewing patients with a structured questionnaire, by trained physicians (mostly residents in Clinical Pharmacology). Surgical procedures were classified in three categories, according to their duration and complexity: category I included inguinal hernia repair and appendectomy, category II included cholecystectomy and laparotomy, and category III included bowel resection, gastric surgery, gynaecological surgery, and hepatopancreatic and splenic surgery. For each patient, information on the analgesic drugs used, their dose, route of administration, dosage schedule, and prescribed and administered doses in the first 24 h after abdominal surgery was prospectively recorded, by using a standard data collection form. All medical orders and nursing records regarding analgesics were considered.
Information on postoperative pain was assessed 24 h after the operation. Patients were asked to rate pain severity with a six-adjective categorical rating scale and a visual analogue scale (VAS). The categorical rating scale included the following categories: none, mild, moderate, severe, very severe and unbearable. The VAS scale was a 100-mm line labelled at the beginning with ‘no pain’ (score = 0) and at the end with ‘the worst possible pain I can imagine’ (score = 100). Both the maximal pain severity during the first 24 h after the surgical procedure and the pain at the time of the interview were recorded. Data were analysed by means of Statistical Package for Social Sciences (SPSS) software.
Results
Nine hundred and ninety-three patients (547 men, 55%) were included in the study. Their median age was 58 years (range 14–91); 13% were older than 70 years. Five hundred and seventy-one (57%) did not have any associated condition. Hypertension and/or heart failure (224 patients), chronic respiratory diseases (114 patients), and dyspepsia and/or peptic ulcer (98 patients) were the most commonly associated conditions.
The most common surgical procedures were inguinal hernia repair (315 patients, 32%), cholecystectomy (268, 27%), appendectomy (140, 14%), bowel resection (137, 14%), and gastric surgery (58, 6%). Other surgical procedures were nonspecific laparotomy (25 patients), hepatopancreatic and splenic surgery (25 patients), and gynaecological surgery (6 patients).
Only 54 patients (5%) did not receive any analgesic during the study period. In this group, the distribution of the different categories of surgical procedures did not differ from that in the whole population. Five hundred and eighty-seven patients (59%) only received a nonopioid analgesic, and 89 (9%) only received an opioid analgesic. Two hundred and sixty-three patients (27%) were administered both kinds of drugs (metamizole+opiate in 62% of these). The administered drugs were metamizole (677 patients, 68%), pethidine (213, 21%), morphine (108 patients, 11%), diclofenac (105, 10.5%), ketorolac (74, 7%), clonixin (63, 6%), tramadol (55, 5%), pentazocine (21, 2%), buprenorphine (5, 0.5%), paracetamol (4, 0.4%), methadone (2, 0.2%), lysine acetylsalicylate (2, 0.2%), and piroxicam (1, 0.1%). The proportions of patients in each surgical procedure category who received at least one dose of an opioid analgesic were 44% in category one, 48% in category two, and 61% in category three (χ2 Pearson = 15.1; P < 0.001), and the proportions receiving both opioid and nonopioid analgesics were, respectively, 12%, 20%, and 32% (χ2 Pearson = 37; P < 0.001).
In patients with contraindications to the use of analgesics (e.g. chronic respiratory disease for opiates, or peptic ulcer, dyspepsia, hypertension or heart failure for NSAIDs), the patterns of use did not differ from those in other patients.
On the first day, 1773 medical orders of analgesics were written. The route of administration was intravenous in 1242 (70%), intramuscular in 364 (20.6%), subcutaneous in 103 (6%), other (oral, rectal) in 57 (3%), and unknown in 7 (0.4%).
Analgesics were scheduled at regular predetermined intervals of time (around the clock) in 941 medical orders (54.5%), on an ‘as needed’ basis in 524 (30.3%), at predetermined intervals with a rescue analgesic in 57 (3.3%), and as patient-controlled analgesia in 42 (2.4%). In 209 medical orders (11.8%) the dosage schedule was not written.
Of the 1773 medical orders examined, 1025 gave clear instructions on the dose and dosage schedule. Only 651 (63.5%) led to actual administration of the prescribed drug. This compliance rate was higher when only one dose had been prescribed (248 of 273, 88%), and decreased to 64% (165/258), 59% (178/301), and 35% (68/193) with the prescription of two, three, or four or more doses of the analgesic, respectively (χ2 Pearson = 1017; P < 0.00001). In general, actual administered daily doses were lower than those prescribed and than those recommended in the literature (see Table 1).
Table 1.
Prescribed and administered daily doses (mean±s.d.) of analgesicsa.

The percentages of patients who received three or more doses of analgesics during the first 24 h of the postoperative procedure were 52% in category I, 65% in category II, and 69% in category III (χ2 Pearson = 23.5; P < 0.001).
Table 2 shows the proportion of patients with each of the categories of worst pain suffered during the first day, and the severity of pain 24 h after the surgical procedure, as assessed with the six-adjective categorical rating scale and with a VAS. On the categorical scale 69% of patients had suffered moderate to unbearable pain at any time during this period, and 38% had suffered severe to unbearable pain. On the VAS, 69% showed a severity of >30 mm, and 47% rated >50 mm.
Table 2.
Postoperative pain severity scored by means of an adjective categorical rating scale and by means of a visual analogue scale.

There was no apparent relation between the pain severity during the first day and the analgesics which were actually administered: the mean (s.d.) VAS score was 47.6 mm (28.9) in those given only opiates, 49.2 mm (30.6) in those given nonopioid analgesics, and 48.5 (30) in those given both kinds of drugs.
Fifty-eight patients (6%) had some adverse drug effect attributable to any of the administered analgesics: 26 had received nonopioid and opioid drugs, 23 a nonopioid analgesic, and 9 an opioid. Adverse effects were mild and the majority were gastrointestinal (abdominal pain, nausea, vomiting, and constipation). Only three patients developed respiratory depression.
Wide interhospital variability in the populations under study (see Table 3) and in the most commonly used analgesic drugs (see Table 4) was recorded. The proportion of patients who received only opioids varied greatly (from 0 to 23%), as did the proportions of those receiving only nonopioid analgesics (16–90%) and of those receiving both types of drugs (4–57%). In some hospitals (e.g. numbers 2 and 5), combinations of opioid and nonopioid analgesics were frequently administered. In the majority of hospitals, metamizole (which was given overall to 68% of patients) was the most commonly administered nonopioid analgesic, although in some centres other analgesics (diclofenac, ketorolac, clonixin) were used most frequently. Pethidine was the most commonly administered opioid analgesic in the majority of hospitals; it was given to 21% of the whole study population. Other opioids were given as well—morphine (11% of patients), tramadol (5%), and pentazocine (2%) were also used. Wide interhospital variability was also recorded in the percentage of patients receiving at least three doses of analgesics (from 31 to 88%; χ2 Pearson = 81.96; P < 0.0001), and in the mean number of doses of analgesics administered during the first day of the postoperative period, which ranged from 1.96 (s.d. = 1.3) to 6.46 (s.d. = 12) (F = 6.82; P < 0.0001).
Table 3.
Interhospital variability in patients’ characteristics.

Table 4.
Use of analgesic drugs, by hospital.

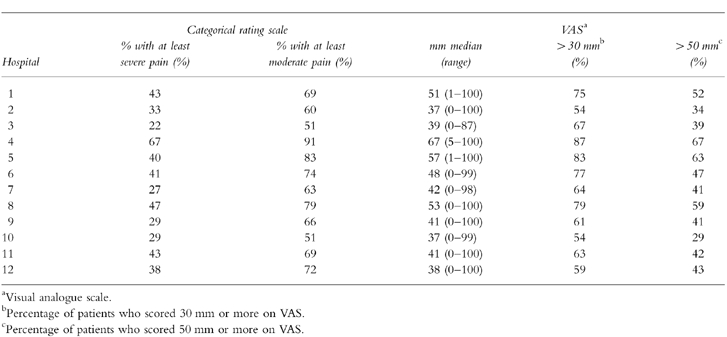
Table 5 shows the severity of postoperative pain, by hospitals. Wide interhospital variability was also recorded in pain scores during the first day after the operation. So, for example the proportion of patients with severe, very severe or unbearable pain varied from 22% in hospital 3 to 67% in hospital 4. The proportions of patients with at least moderate pain varied from 51% in hospital 3 to 95% in hospital 4. The VAS scores also varied from 37 mm in hospital 10 to 67 mm in hospital 4. No correlation was found between the maximum worst pain severity during the first 24 h (Table 5), and the prevalence of use, in each hospital, of opioid analgesics alone (Spearman rank correlation test, r = −0.12; P = 0.7), of both opioid and nonopioid analgesics (r = 0.23; P = 0.5), neither of use of opioid analgesics (r = -0.04; P = 0.9).
Table 5.
Severity of postoperative pain, by hospital.
Discussion
The present study shows that a significant proportion of patients suffer severe pain during the immediate postoperative period after abdominal surgery, despite the fact that effective analgesic drugs are available. Parenteral nonopioid analgesics were the most commonly used drugs, generally by intravenous route. The use of analgesics was inadequate in a substantial proportion of patients, because even if they had been prescribed on a predetermined regular interval schedule, they were often actually given to treat established pain rather than to prevent its appearence, and their doses were frequently inadequate. Wide interhospital differences in qualitative and quantitative aspects of analgesic use were found, but these did not seem to correlate with the mean severity of pain in each hospital.
Our study confirms previous smaller studies carried out in Spain [7–19], suggesting that, in contrast with other settings [14–16, 18], nonopioid analgesics, including nonsteroidal anti-inflammatory drugs, are the preferred drugs for the treatment of postoperative pain. The predominant use of nonopioid analgesics does not seem to be related to concerns regarding the adverse effects of opioids, because contraindications to the use of all classes of analgesics were apparently not taken into account.
Thirty-eight percent of patients rated their worst pain on the first day as severe, very severe or unbearable, and 44% rated more than 50 mm on the VAS. This high prevalence of severe pain should be considered as a therapeutic failure, because it is preventable. Special techniques for the treatment of pain were rarely prescribed (e.g. patient controlled analgesia was used in 2% of patients) or not at all (e.g. epidural analgesia).
Wide interhospital variability was found in the patterns of the use of analgesics. In four hospitals, at least 9% of patients did not receive any analgesic. Non-random selection of the study population may have contributed to this variability. Differences in the prevalence of severe pain were also seen, but no correlation could be found between this and neither the rate of use of opioid analgesics, the rate of use of nonopioid analgesics, nor the use of any analgesic at full doses and on a regular prescheduled basis. However, in a cross-sectional study like the present one this lack of correlation cannot be interpreted as a proof of ineffectiveness, because interhospital variability in the populations under study (in terms of demographic characteristics, surgical procedures, or other) can confound a causal association, if any.
Unfortunately, these results are in agreement with those of other studies [13–19, 26] showing that inappropriate prevention of postoperative pain is common. Reasons for this undertreatment which have been suggested include poor routine evaluation of pain severity, discrepancies in its assessment between patients and physicians or between patients and nurses [16, 27–29], and the prescription and administration of doses lower than those recommended. Our results confirm these suggestions. Continued education of medical and nursing staff is essential in order to improve the management of such a common problem. The participation of nursing staff is also crucial in the routine assessment of pain severity, by using simple tools, such as pain scales [8, 21]. Use of pain charts as part of the general routine clinical assessment of patients (together with fever, heart rate and blood pressure records) may also improve pain control. These charts can also be used for auditing the quality of care.
The intervention which has been most frequently proposed in order to improve the management of postoperative pain is continued education of health care professionals. However, education alone is not enough [25, 30]. In one study education was not followed by any change in the patients’ outcomes [30]. An improvement of postoperative pain relief has been reported after the introduction of a multidisciplinary team into a general hospital using simple techniques and simple instructions [21]. Routine audit of the quality of patient care has also been proposed [21].
Determining the prevalence and severity of postoperative pain is a contribution to the evaluation of health care in the hospital setting. The present study constitutes a reference for the future evaluation of intervention measures aimed at improving the management of postoperative pain.
Acknowledgments
Europharma SA provided financial support for meetings of investigators.
References
- 1.Donovan M, Dillon P, McGuire L. Incidence and characteristics of pain in a sample of medical-surgical inpatients. Pain. 1987;30:69–78. doi: 10.1016/0304-3959(87)90084-4. [DOI] [PubMed] [Google Scholar]
- 2.Agency for Health Care Policy and Research. Acute pain management: operative or medical procedures and trauma, part 1. Clin Pharm. 1992;11:309–331. [PubMed] [Google Scholar]
- 3.Agency for Health Care Policy and Research. Acute pain management: operative or medical procedures and trauma, part 2. Clin Pharm. 1992;11:391–414. [PubMed] [Google Scholar]
- 4.Cañellas M, Bosch F, Bassols A, Rué M, Baños JE. Prevalencia del dolor en pacientes hospitalizados. Med Clín (Barc) 1993;101:51–54. [PubMed] [Google Scholar]
- 5.Royal College of Surgeons of England and College of Anaesthetists’ Commission on the Provision of Surgical Services. Report of the Working Party on Pain After Surgery. London: Royal College of Surgeons; 1990. [Google Scholar]
- 6.Bruster S, Jarman B, Bosanquet N, Weston D, Erens R, Delbanco TL. National survey of hospital patients. Br Med J. 1994;309:1542–1546. doi: 10.1136/bmj.309.6968.1542. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Baños JE, Bosch F. Problemas específicos de la terapia antiálgica en el medio hospitalario. Med Clín (Barc) 1996;106:222–226. [PubMed] [Google Scholar]
- 8.McQuay H, Moore A, Justins D. Treating acute pain in hospital. Br Med J. 1997;314:1531–1535. doi: 10.1136/bmj.314.7093.1531. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Sydow FW. The influence of anesthesia and postoperative analgesic management on lung function. Acta Chir Scand. 1989;550(Suppl.):159–165. [PubMed] [Google Scholar]
- 10.Wattwil M. Postoperative pain relief and gastrointestinal motility. Acta Chir Scand. 1989;550(Suppl.):140–145. [PubMed] [Google Scholar]
- 11.Rowbotham D. Postoperative pain. Prescribers’ J. 1993;33:237–243. [Google Scholar]
- 12.Torda T. Postoperative analgesia. Aust Prescriber. 1995;18:88–91. [Google Scholar]
- 13.Papper EM, Brodie BB, Rovenstine EA. Postoperative pain: its use in the comparative evaluation of analgesics. Surg. 1952;32:107–109. [PubMed] [Google Scholar]
- 14.Marks RM, Sachar EJ. Undertreatment of medical inpatients with narcotic analgesics. Ann Intern Med. 1973;78:173–181. doi: 10.7326/0003-4819-78-2-173. [DOI] [PubMed] [Google Scholar]
- 15.Cohen FL. Postsurgical pain relief: patients’ status and nurses’ medication choices. Pain. 1980;9:265–274. doi: 10.1016/0304-3959(80)90013-5. [DOI] [PubMed] [Google Scholar]
- 16.Sriwatanakul K, Weiss OF, Alloza JL, Kelvie W, Weintraub M, Lasagna L. Analysis of narcotic analgesic usage in the treatment of postoperative pain. JAMA. 1983;250:926–929. [PubMed] [Google Scholar]
- 17.Baños JE, Bosch F, Ortega F, Bassols A, Cañellas M. Análisis del tratamiento del dolor en tres hospitales. Rev Clín Esp. 1989;184:177–181. [PubMed] [Google Scholar]
- 18.Kuhn S, Cooke K, Collins M, Mucklow JC. Perceptions of pain relief after surgery. Br Med J. 1990;300:1687–1690. doi: 10.1136/bmj.300.6741.1687. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Aguilera C, Arnau JM, Bosch C, et al. Grupo de Estudio sobre la Analgesia Postoperatoria de la Sociedad Española de Farmacología Clínica. Med Clin (Barc) 1997;108:136–140. [PubMed] [Google Scholar]
- 20.Ready LB, Oden R, Chadwick HS, et al. Development of an anesthesiology-based postoperative pain service. Anesthesiol. 1988;68:100–106. doi: 10.1097/00000542-198801000-00016. [DOI] [PubMed] [Google Scholar]
- 21.Gould TH, Crosby DL, Harmer M, et al. Policy for controlling pain after surgery: effect of sequential changes in management. Br Med J. 1992;305:1187–1193. doi: 10.1136/bmj.305.6863.1187. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Rawal N, Berggren L. Organization of acute pain services: a low-cost model. Pain. 1994;57:117–123. doi: 10.1016/0304-3959(94)90115-5. [DOI] [PubMed] [Google Scholar]
- 23.American Society of Anaesthesiologists Task Force on Pain Management, Acute Pain Section. Practice guidelines for acute pain management in the perioperative setting. Anesthesiol. 1995;82:1071–1081. [PubMed] [Google Scholar]
- 24.Réunion de la Société Française de Pharmacologie Clinique et de Thérapeutique. Table ronde: Du bon usage des antalgiques. Thérapie. 1992;47:471–479. [Google Scholar]
- 25.American Pain Society Quality of Care Committee. Quality improvement guidelines for the treatment of acute pain and cancer pain. JAMA. 1995;274:1874–1880. doi: 10.1001/jama.1995.03530230060032. [DOI] [PubMed] [Google Scholar]
- 26.Warfield CA, Kahn CH. Acute pain management. Program in US hospitals and experiences and attitudes among US adults. Anesthesiol. 1995;83:1090–1094. doi: 10.1097/00000542-199511000-00023. [DOI] [PubMed] [Google Scholar]
- 27.Teske K, Daut RL, Cleeland CS. Relationship between nurses’ observations and patients’ self-reports of pain. Pain. 1983;16:289–296. doi: 10.1016/0304-3959(83)90117-3. [DOI] [PubMed] [Google Scholar]
- 28.Weiss OF, Sriwatanakul K, Alloza JL, Weintraub M, Lasagna L. Attitudes of patients, housestaff and nurses toward postoperative analgesic care. Anesth Analg. 1983;62:70–74. [PubMed] [Google Scholar]
- 29.Zalon ML. Nurses’ assessment of postoperative patients’ pain. Pain. 1993;54:329–334. doi: 10.1016/0304-3959(93)90033-L. [DOI] [PubMed] [Google Scholar]
- 30.Rose DK, Cohen MM, Yee DA. Changing the practice of pain management. Anesth Analg. 1997;84:764–772. doi: 10.1097/00000539-199704000-00012. [DOI] [PubMed] [Google Scholar]


