Abstract
Studies of EMG power spectra have established associations between low-back pain (LBP) and median frequency (MF). This 2-year prospective study investigates the association of LBP with EMG variables over time. 120 health care workers underwent paraspinal EMG measurements and assessment of back pain disability. The EMG recordings were performed under isometric trunk extension at 2/3 maximum voluntary contraction and acquired from erector spinae muscles at the level of L4/L5. 108 (90%) subjects were reviewed at a minimum 2-year follow up. 16 out of 93 subjects with no history of chronic low-back pain became worse as measured by time off work, disability, reported pain and self-assessment rating. The value of the EMG variable half-width at inception demonstrated significant association with changes in subject’s outcome measure and their own assessment of their LBP at follow up (p < 0.05). Based on self-assessment data, subjects with no history of chronic LBP with half-width of greater than 56 Hz were at threefold greater risk of developing back pain compared with the remainder of the population (p = 0.045). The value of the initial median frequency (IMF) and MF slope at inception were also associated with the subjects’ own assessment of LBP at follow up. Subjects with an IMF greater than 49 Hz were at 5.8-fold greater risk of developing back pain compared with the remainder of the population (p = 0.014). EMG variables recorded from lumbar paraspinal muscles can identify a sub group of subjects at increased risk of developing low-back pain in the future.
Keywords: EMG, Low back pain, Paraspinal muscles, Prediction, Cohort study
Introduction
The aetiology of LBP and the design of strategies for its prevention have been the subject of numerous scientific investigations. Despite these efforts there remains a considerable amount of uncertainty and disagreement about which risk factors are the most important.
In studies of individual factors, the most consistent associations have been with previous LBP and age [1, 13] with some association between genetic factors and LBP [30, 48, 53, 54] and less well established associations for obesity, smoking and gender [3, 10, 18, 22, 28, 29, 45, 49].
In studies of biomedical factors there has been some association between prolonged bending and twisting and LBP [19, 22, 43] and a weak association between LPB, fitness and muscular strength level [2, 3, 7, 8, 12, 29, 44, 53]. Further studies of biomedical factors have strengthened the link between muscular structure and back pain [20, 52], and today there is general consensus that muscles play an important role in low back pain [11, 20, 25, 41].
Studies of electromyography (EMG) recordings from low back muscles have demonstrated changes in activation pattern [20], fatigability [9, 36] and asymmetrical of activation [39] in back pain subjects compared with controls. These studies have also suggested a number of reliable and reproducible variables that can be extracted from routine EMG [5, 32, 33, 46, 51]. Our own studies have confirmed these findings, examining 39 subjects on three separate occasions [38]. Initial median frequency (IMF), half-width (HW) and root mean square (RMS) demonstrated satisfactory reliability, although RMS was too load-dependent to be a potentially valuable comparator between subjects.
Other studies have also shown that EMG is able to distinguish chronic pain sufferers from healthy volunteers [4, 24, 46, 47]. We have previously reported differences in many EMG variables between back pain sufferers and healthy volunteers. In a study of 350 subjects, the HW was able to distinguish between the two with a sensitivity of 64% and a specificity of 87% [21]. This study demonstrated that back pain sufferers had wider HW compared with healthy volunteers, and values >48 Hz were significantly associated with back pain.
A number of more recent studies have also investigated the change in EMG over time for prognosis purposes. Adams et al. [1] studied 430 heath care workers over a 3-year period and found no predictive value for median frequency slope (MF-slope). Stevenson et al. [49] studied 149 industrial workers and reported predictive value for IMF. However, because of variation in test conditions between these studies it is not possible to draw conclusions over these apparently contradictory results. The present study attempts to evaluate the value of IMF, MF slope and HW, under unified test conditions, as objective prognostic indicators in development of LBP. Changes in EMG variables within individuals over time have also been examined.
Methods
Subject details
The study was a prospective cohort study of 120 volunteers. Participants were recruited from staff of a large general hospital by visiting wards, hospital departments and advertising in a hospital newsletter. Those with clinical suspicion of disc prolapse, nerve root compression, inflammatory arthritis, peripheral neuropathy, severe alcohol abuse and acute back pain were excluded from the study, as were subjects who had exercised vigorously prior to the test on the day of testing (e.g. those who had cycled to work). At enrolment (time 1) subjects were assessed clinically for low back symptoms using a structured interview, a disability measure (Low Back Outcome Score; LBOS) [15] and measures of distress (Zung Depression Score [14, 55] and Modified Somatic Perception Questionnaire; MSPQ [31]). Participants were classified as follows, according to their history at presentation:
| No-history (N) | No episode of back pain sufficient to cause time off work or to prevent activities of daily living in past 5 years |
| Chronic (CH) | Continuous or intermittent pain sufficient to cause time off work or to prevent activities of daily living over last 12 months. At least one episode in the last 3 months |
| Past history (PH) | At least one episode in the last 5 years severe enough to cause time off work or to prevent activities of daily living, but no such attack in the last 2 years |
Two years later at follow up (time 2), 108 of these 120 workers were re-evaluated (90%). Twelve subjects failed to complete the study; six had left the area, one was chronically ill, two declined retest and three untraceable. Work loss records during the 2-year period were examined and the clinical assessment, disability and distress measures and EMG were repeated. At follow up, subjects were asked to classify themselves as worse, better or the same compared with 2 years before by responding to the question ‘over the last 2 years, do you feel your back is better, same or worse than it was?’ Volunteers reviewed their previously recorded symptoms, prior to their subjective decision of any change and before the EMGs were performed. No volunteer had back pain at the time of testing.
Acquisition and processing of EMG signal
Testing was performed according to the technique of Oliver et al. [40]. Briefly, the pelvic rest height was set 6 cm below the anterior superior iliac spines, and the lumbar spine was positioned in 30° flexion using a body contour formulator or goniometer. EMG recording sites were prepared to reduce skin impedance, and surface electrodes were placed over the greatest convexity of the erector spinae muscles at the L4/L5 level with a distance between the electrodes of each pair of 40 mm. Loading was performed by the subject pulling on a bar attached to a load cell fixed to the base of the frame. Maximum voluntary contraction (MVC) was determined, and after a 4-min rest the EMG was recorded while the subject maintained a load of 2/3 MVC for 30 s. The same load was used at time 1 and time 2.
A Medelec Sapphire-2ME EMG system was used to amplify and filter the EMG signal (band pass 3–300 Hz). Signals were digitised through National Instrument DAQCard-700 PCMCIA device and sampled at 1,024 Hz using continuous double-buffer process. The output from the load cell was converted to digital using the same process, while the acquisition software maintained a real-time bar graph display of load centred at the target load of 2/3 MVC. By using this clear target display, subjects were able to hold a steady load for 30 s.
Both channels of the 30-s EMG recording were divided into 1-s epochs of 1,024 voltage samples. The root mean square voltage (RMS) was calculated for the whole test period by rectifying each of the 30,720 voltage samples scaled to EMG amplifier gain, and taking the mean of these values. A fast Fourier transformation was applied to each epoch to obtain a power spectrum. The median frequency, defined as the frequency that divided the spectrum into two equal areas, was calculated for each epoch. The initial median frequency (IMF) and median frequency slope (MF slope) were obtained, respectively, from the intercept (t = 0) and the slope of a linear regression fit to the 30 median frequencies calculated for each channel.
The thirty power spectra were averaged and the composite spectrum was smoothed by applying a three-point moving average in nine passes. From this the peak power was taken as the greatest amplitude of the spectrum, and the modal frequency was taken as the frequency at which the amplitude was greatest. The HW was taken as the width of the spectrum at half the maximum power. If the HW was not unique due to spikes in the spectrum, then the narrowest value was taken for analysis based on the previous theoretical work [50].
Statistical methods
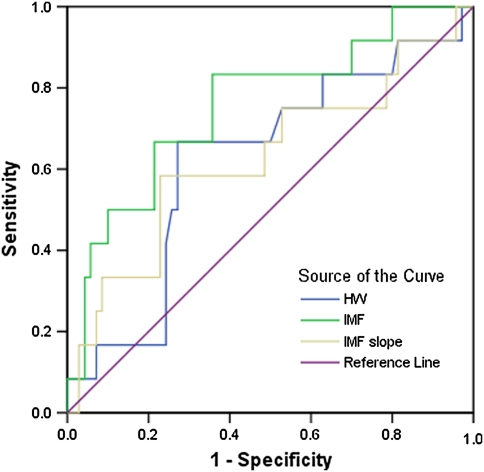
Paired sampled t tests were performed to evaluate changes in EMG variables from time 1 to time 2 (Table 4). Independent sample t tests were performed to compare differences between the worse group and the remainder of the population. The significance of the specificity and sensitivity at various cut-off values was tested using the chi-square test. Cut-off points for chi-square tests were points on the ROC curve related to that variable, yielding the highest sensitivity and specificity (Figs. 3, 4). Statistical significance was accepted at the 5% level. Values reported for each variable are the combined left and right values for that variable. Commercial statistical package SPSS (SPSS Inc. Chicago, IL, USA; V12.0) was used for all statistical analyses reported.
Table 4.
Mean and standard deviation of half-width at time 1 and time 2
| Over 2 years | Time | N | Mean HW | SD | Sig. (two-tailed) |
|---|---|---|---|---|---|
| Better | Time 1 | 13 | 61.3 | 17.5 | 0.014 |
| Time 2 | 13 | 46.6 | 19.3 | ||
| Same | Time 1 | 76 | 48.9 | 16.5 | 0.023 |
| Time 2 | 76 | 45.2 | 14.3 | ||
| Worse | Time 1 | 16 | 55.9 | 19.2 | 0.446 |
| Time 2 | 16 | 60.8 | 12.6 |
Classification of change over 2 years based on self-rating scores. The change in HW was significant for the ‘better’ and the ‘same’ group but not the ‘worse’ group
Fig. 3.
The ROC curves for IMF, IMF slope and HW based on self-rating data
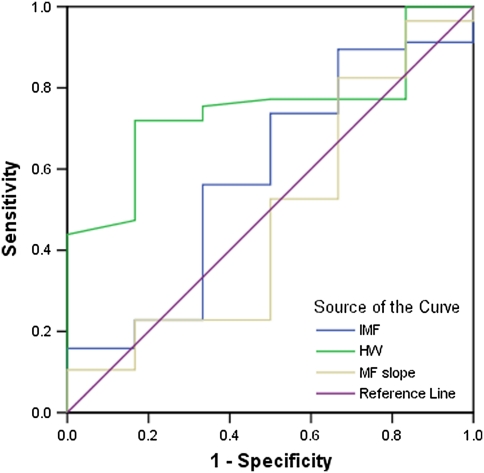
Fig. 4.
The ROC curves for IMF, IMF slope and HW based on LBOS scores
Results
Three out of the 108 results were unusable; two had corrupted file recordings and one had error in recording at time 1. Data were analysed for the remaining 105 cases.
At follow up (time 2) there were 26 males and 79 females. 76 subjects classed themselves as “unchanged (same)”, 13 “better” and 16 “worse”. Descriptive data are in Table 1. There was a significant association between the subjects’ self-rating of their condition and that demonstrated by time off work (p = 0.02), low-back disability (p < 0.01) and pain (p < 0.001). The volunteers’ subjective feeling of being the same, worse or better appeared to be a good reflection of their clinical change. The Zung and MSPQ scores were little changed over the 2 years and are not reported for this reason.
Table 1.
Specification of subjects in three groups of ‘better’, ‘same’ and ‘worse’
| Over 2 years | Classification | Gender | Mean (SD) | ||||||
|---|---|---|---|---|---|---|---|---|---|
| N | PH | CH | Female | Male | Age (t1) | Height | Weight | LBM | |
| Better | 0 | 3 | 10 | 11 | 2 | 37.2 (6.9) | 168.7 (5.3) | 65.8 (8.5) | 46.1 (5.5) |
| Same | 70 | 4 | 2 | 58 | 18 | 34.6 (9.3) | 165.8 (8.3) | 64.5 (12.5) | 46.6 (9.4) |
| Worse | 12 | 4 | 0 | 11 | 5 | 39.1 (8.6) | 169.6 (10.2) | 72.2 (13.6) | 51.4 (11.3) |
Volunteers were classified into three groups of no-history (N), past history (PH) and chronic history (CH) at inception—time 1
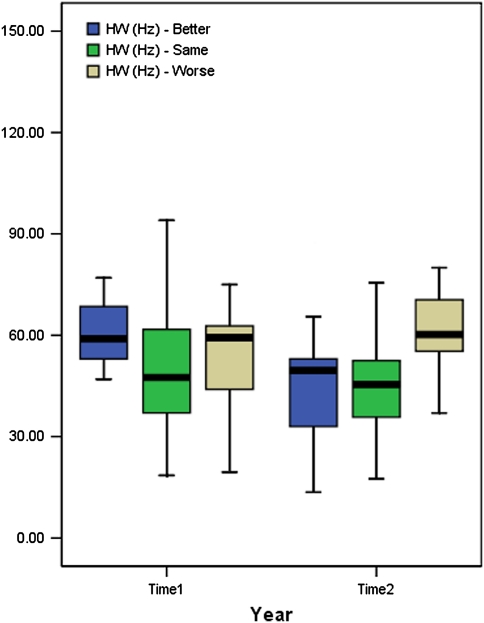
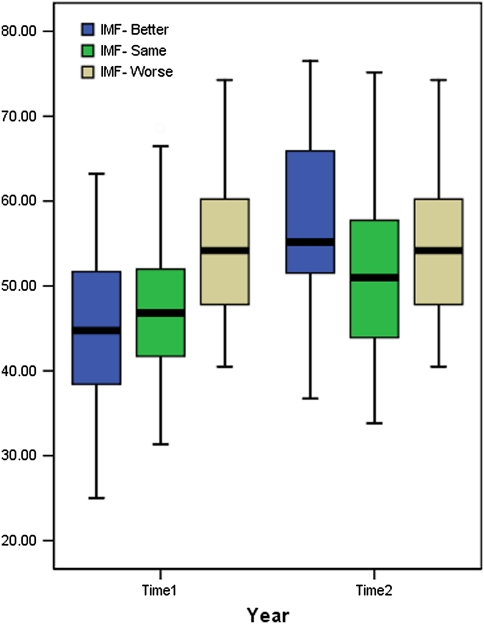
When comparing the groups as a whole, changes in the HW appeared to mirror the clinical changes over time. Plotting the HW against the time in the cohort study for three groups of worse, same, and better showed that the mean HW reduced for the better group and increased for the worse group (Fig. 1; Table 4). However, this change was only slightly over the expected 95% confidence interval (CI) of within-subject variability for the ‘better’ group and less than this value for the ‘worse’ group [40]. Plotting the mean IMF for the three groups against the time also did not show any relationship between values recorded at time 1 and time 2 for this variable (Fig. 2).
Fig. 1.
Boxplots showing half-width at time 1 and time 2 for better, same and worse group based on self-rating scores
Fig. 2.
Boxplots showing IMF at time 1 and time 2 for better, same and worse group based on self-rating scores
Analysis of the EMG variables at inception compared with individual’s own subjective assessment at follow up revealed that the HW was able to identify a group of subjects at greater risk of developing low-back pain within the next 2 years. Back pain at follow up was defined as low-back pain sufficient enough to be off work or require medical attention. Thirty out of 93 past history and no-history subjects had an initial HW of greater than 56 Hz. The relative risk for back pain in this group was 2.7 (95% CI 1.11–6.53; p = 0.05). Twenty-six out of 82 subjects with no history of back pain had an initial HW of greater than 56 Hz. The relative risk for back pain in this group was 3.01 (95% CI 1.06–8.62; p = 0.045) (Fig. 3; Table 2).
Table 2.
Comparison of all EMG variables in predicting back pain in no-history (N) subjects based on self-rating
| Parameters | Cut-off | AUC | 95% CI for AUC | Sensitivity (%) | Specificity (%) | χ2 sig. (p) |
|---|---|---|---|---|---|---|
| IMF (Hz) | 49 | 0.76 | 0.60–0.91 | 83 | 60 | 0.01 |
| MF slope | −0.203 | 0.63 | 0.44–0.82 | 58 | 77 | 0.03 |
| HW (Hz) | 56 | 0.62 | 0.45–0.80 | 58 | 73 | 0.04 |
| RMS (Hz) | 87 | 0.62 | 0.47–0.78 | 66 | 67 | 0.53 |
| RMS slope | 0.309 | 0.54 | 0.39–0.69 | 58 | 55 | 0.56 |
| IRMS (Hz) | 88 | 0.64 | 0.48–0.80 | 75 | 59 | 0.66 |
The initial median frequency and median frequency slope were also able to predict an increased incidence of low-back pain in the no-history group. The relative risk for subjects with IMF values of greater than 49 Hz was 5.8 (95% CI 1.35–25.0; p = 0.014) and for subjects with MF slope of less than −0.2077 was 3.6 (95% CI 1.27–10.18, p = 0.03) (Fig. 3; Table 2).
Data were also examined for the predictive power of these variables based on LBOS scores; ‘worse’ being the reduction in LBOS score greater than 7.5, ‘better’ being an increase in LBOS score greater than 7.5 and ‘same’ being any other value [23]. Nineteen subjects with no-history of back pain (23.2%) and 22 subjects with no history of back pain or past history (23.4%) did not have LBOS scores. In view of small numbers, the ‘better’ and ‘same’ groups were analysed together. Data were analysed for the remaining 63 subjects with no-history of back pain. Twenty out of 63 subjects in this group had an initial HW of greater than 56 Hz. The relative risk for back pain in this group was 4.3 (95% CI 0.86–22.2; p = 0.075). Twenty-seven out of 72 subjects with no-history of back pain or past history had an initial HW of greater than 56 Hz. The relative risk for back pain in this group was 5.0 (95% CI 1.1–23.2; p = 0.04). This suggests that HW is a better predictor based on the LBOS scores compared to self-rating data. However, this was not the case for IMF and MF-slope. The relative risk for IMF was reduced to 1.74 (95% CI 0.38–7.9; p = 0.66) and for IMF-slope to 2.7 (95% CI 0.60–12.13; p = 0.33), indicating no predictive value for these two variables when outcome measure was used (Table 3; Fig. 4).
Table 3.
Comparison of three EMG variables in predicting back pain in no-history (N) subjects based on LBOS scores
| Parameters | Cut-off | AUC | 95% CI for AUC | Sensitivity (%) | Specificity (%) | χ2 sig. (p) |
|---|---|---|---|---|---|---|
| IMF (Hz) | 49 | 0.58 | 0.33–0.83 | 50 | 64 | 0.66 |
| MF slope | −0.20 | 0.52 | 0.25–0.79 | 50 | 75 | 0.33 |
| HW (Hz) | 56 | 0.75 | 0.59–0.90 | 66 | 71 | 0.075 |
None of the EMG variables iRMS, RMS, or RMS Slope showed any significant predictive value for future episodes of low-back pain.
The mean HW at time 2 was found to be significantly different from time 1 for the ‘better’ (t(12) = 2.875, p = 0.014) and the ‘same’ (t(75) = 2.313, p = 0.023) group but not the ‘worse’ group (t(15) = −0.783, p = 0.45). The mean IMF at time 2 was also significantly different from time 1 for the ‘better’ (t(12) = −3.60, p = 0.004) and the ‘same’ (t(75) = −4.52, p < 0.001) group but not the ‘worse’ group (t(15) = 0.15, p = 0.88) (Table 4).
Discussion
The cause of low-back pain remains incompletely understood. The use of techniques such as strength tests, radiological and medical examinations in prognosis has been unsuccessful [6, 10, 12]. A previous history of low-back pain has been shown to be of prognostic significance, but relies on reporting by the subject and of course cannot be used to predict the first episode. For many years, the role of the spinal musculature has been little investigated, but more recently strong correlations between muscle function as evidenced by EMG measurements and chronic low-back pain have been reported [4, 24, 46, 47]. A correlation, however, implies only an association and does not necessarily imply a causal relationship.
The current study strengthens the possibility of the spinal musculature having a more fundamental role by demonstrating that EMG changes can identify a group within a population at increased risk of a significant episode of low-back pain.
Based on subject’s own assessment data, there is a consistent increase in risk of LBP with increase in HW. At the start of the study, a HW of >56 Hz was able to identify a subgroup of about one-third of the ‘past history’ and ‘no-history’ population in whom the risk of an episode of back pain severe enough to cause loss of time from work was three times greater than the remainder of the population (p = 0.05). This remained the case even when the ‘past history’ subjects were excluded (p = 0.045). IMF and IMF-slope also had potential as a predictor of back pain. All three EMG variables had relatively similar specificity and sensitivities although IMF was slightly superior in predicting those at risk of backache (Table 3).
The predictive power of these EMG variables based on the LBOS scores was also examined. About 23% of LBOS score data were missing because of administrative error. Analysis of the remaining data from no-history group (n = 63) yield to the improved predictive power for HW but IMF and IMF-slope were non-discriminating.
Our results on predictive value of IMF based on self-rating data at follow up agrees with those reported by Stevenson et al. [49] who studied 149 industrial workers, using the same method for evaluation of the outcome and reported predictive value for IMF. Our result on predictive value of MF-slope based on change in LBOS scores from time 1 to time 2 also appears to agree with those reported by Adams et al. [1] who found no predictive value for MF-slope. However, we postulate that our study is weakened by smaller number in LBOS analysis.
IMF and HW were significantly different at time 2 compared with time 1, for the same and the better group, but not the worse group. Mean HW for the same group was reduced by 3.7 Hz (SD = 13.91, p = 0.023) and mean IMF was increased by 4.43 (SD = 8.54, p < 0.001) over the 2-year period. We would note that at a concurrent period there was an ongoing campaign to promote health among the staff, which may have contributed to the shift of HW in the same and better group towards the lower value.
It is unclear how these EMG variables relate to the underlying muscle physiology. Previous research has shown that there are differences of muscle fibre types between back-pain suffers and controls [34, 35, 37]. Type I muscles have the characteristics of firing in a more orderly manner and are able to discharge at longer inter-spike-intervals (ISI) while type II muscle fibres fire at shorter intervals [16]. Changes in ISI statistics have been related to significant change in the low frequency of the spectrum [27] and to increases in IMF [26]. One explanation of the observed differences between the EMG variables of these two groups may be simply differences in their muscle fibre type.
Another factor to be considered is muscle fibre recruitment with load. It is possible that the subjects at risk group failed to employ their maximum force, possibly for a factor that predisposed them to BP. In such a scenario their motor neuron firing patterns would be less synchronised [27, 42], shifting IMF to a higher value and changing the distribution of energy along the spectra which could effect HW. It may also be argued that because these subjects failed to employ their maximum effort, they are less likely to be fatigued over the testing period causing their average IMF [27] and HW to stay high. Similar explanations can be given in terms of orderly muscle recruitment patterns [16, 17] and conduction velocity; however, such explanations would be highly speculative as none of the factors of fibre type, conduction velocity, synchronisation of impulses, dropping out of motor neurons, percentage of polyphasic AP and thickness of adipose tissue between the electrode and muscle have been monitored in this study.
Whatever the underlying reason, within the limitation of this study and providing the result of this study could be reproduced, the finding that three EMG variables are capable of predicting first time back pain is interesting and suggests that the spinal musculature has an important role in the appearance and management of back pain. We have previously shown, in study of 350 subjects, that EMG variables have also discrimination value in back pain [21]. The present study further supports our earlier findings and strengthens the possibility of link between spinal muscular and back pain.
If the current EMG techniques can be refined and further validated, there is a potential for significant clinical impact. In preventative programmes, individuals may respond much better to targeted advice given to the one-third of the population shown to be at risk than to general advice directed at whole populations. The technique may allow a useful screening role where workers might be directed away from potentially unsuitable employment, or may allow remedial treatment to be undertaken with a view to reducing the risk to potential employees. The use of EMG variables may allow objective measurement of the results of therapy in clinical trials.
Furthermore, additional evidence for the importance of the spinal musculature allows the tentative formulation of a hypothesis for low-back pain which may explain the mechanism of action of some of the observed important prognostic factors such as distress, genetic and biomedical factors.
Caution is still required as it should be noted that although EMG variables were found to be a significant prognostic indicator, the changes over time corresponding with changes in the subject’s clinical condition demonstrated considerable individual variation. Low-back pain is a complex, multi-factorial problem and it cannot be claimed on the results of this study that a causal relationship has been established.
Conclusion
EMG variables appear to undergo changes over time, which correlate with clinical changes in the subject. EMG variables are able to identify a sub group of subjects in whom the risk of subsequent back pain is increased. This prediction holds true even when a past history of back pain is excluded. If confirmed, these findings may lead to changes in both treatment and screening programmes.
Acknowledgments
The authors are grateful to two anonymous reviewers who provided many suggestions that have greatly improved this manuscript. S.-W. Yeh, S.-K. Kang, C.-H. Kim and M.-H Kwon is supported by KORDI (PE98512, PG47380, PE98511).
Contributor Information
Abbas Heydari, Email: abbas_0@yahoo.co.uk.
Charles G. Greenough, Phone: +44-1642-854311, Email: cgreenough@hotmail.com
References
- 1.Adams MA, Mannion AF, Dolan P. Personal risk factors for first-time low back pain. Spine. 1999;24:2497–2505. doi: 10.1097/00007632-199912010-00012. [DOI] [PubMed] [Google Scholar]
- 2.Batti’e MC, Bigos SJ, Fisher LD, Hansson TH, Jones ME, Wortley MD. Isometric lifting strength as a predictor of industrial back pain reports. Spine. 1989;14:851–856. doi: 10.1097/00007632-198908000-00014. [DOI] [PubMed] [Google Scholar]
- 3.Battie MC, Bigos SJ, Fisher LD, Hansson TH, Nachemson AL, Spengler DM, Wortley MD, Zeh J. A prospective study of the role of cardiovascular risk factors and fitness in industrial back pain complaints. Spine. 1989;14:141–147. doi: 10.1097/00007632-198902000-00001. [DOI] [PubMed] [Google Scholar]
- 4.Biedermann HJ, Shanks GL, Forrest WJ, Inglis J. Power spectrum analyses of electromyographic activity. Discriminators in the differential assessment of patients with chronic low-back pain. Spine. 1991;16:1179–1184. doi: 10.1097/00007632-199110000-00009. [DOI] [PubMed] [Google Scholar]
- 5.Biedermann HJ, Shanks GL, Inglis J. Median frequency estimates of paraspinal muscles: reliability analysis. Electromyogr Clin Neurophysiol. 1990;30:83–88. [PubMed] [Google Scholar]
- 6.Bigos SJ, Battie MC, Fisher LD, Hansson TH, Spengler DM, Nachemson AL. A prospective evaluation of preemployment screening methods for acute industrial back pain. Spine. 1992;17:922–926. doi: 10.1097/00007632-199208000-00009. [DOI] [PubMed] [Google Scholar]
- 7.Bigos SJ, Battie MC, Spengler DM, Fisher LD, Fordyce WE, Hansson TH, Nachemson AL, Wortley MD. A prospective study of work perceptions and psychosocial factors affecting the report of back injury. Spine. 1991;16:1–6. doi: 10.1097/00007632-199101000-00001. [DOI] [PubMed] [Google Scholar]
- 8.Cady LD, Bischoff DP, O’Connell ER, Thomas PC, Allan JH. Strength and fitness and subsequent back injuries in firefighters. J Occup Med. 1979;21:269–272. doi: 10.1097/00043764-197911000-00003. [DOI] [PubMed] [Google Scholar]
- 9.Cooper RG, Stokes MJ, Sweet C, Taylor RJ, Jayson MI. Increased central drive during fatiguing contractions of the paraspinal muscles in patients with chronic low back pain. Spine. 1993;18:610–616. doi: 10.1097/00007632-199304000-00014. [DOI] [PubMed] [Google Scholar]
- 10.Garg A, Moore JS. Prevention strategies and the low back in industry. Occup Med. 1992;7:629–640. [PubMed] [Google Scholar]
- 11.Geisser ME, Ranavaya M, Haig AJ, Roth RS, Zucker R, Ambroz C, Caruso M. A meta-analytic review of surface electromyography among persons with low back pain and normal, healthy controls. J Pain. 2005;6:711–726. doi: 10.1016/j.jpain.2005.06.008. [DOI] [PubMed] [Google Scholar]
- 12.Gibson E. The value of preplacement screening radiography of the low back. Occup Med. 1988;3:91–107. [PubMed] [Google Scholar]
- 13.Gilgil E, Kacar C, Butun B, Tuncer T, Urhan S, Yildirim C, Sunbuloglu G, Arikan V, Tekeoglu I, Oksuz MC, Dundar U. Prevalence of low back pain in a developing urban setting. Spine. 2005;30:1093–1098. doi: 10.1097/01.brs.0000161007.46849.4c. [DOI] [PubMed] [Google Scholar]
- 14.Greenough CG, Fraser RD. Comparison of eight psychometric instruments in unselected patients with back pain. Spine. 1991;16:1068–1074. doi: 10.1097/00007632-199109000-00010. [DOI] [PubMed] [Google Scholar]
- 15.Greenough CG, Fraser RD. Assessment of outcome in patients with low-back pain. Spine. 1992;17:36–41. doi: 10.1097/00007632-199201000-00006. [DOI] [PubMed] [Google Scholar]
- 16.Grimby L, Hannerz J. Firing rate and recruitment order of toe extensor motor units in different modes of voluntary conraction. J Physiol. 1977;264:865–879. doi: 10.1113/jphysiol.1977.sp011699. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Henneman E, Somjen G, Carpenter DO. Functional significance of cell size in spinal motoneurons. J Neurophysiol. 1965;28:560–580. doi: 10.1152/jn.1965.28.3.560. [DOI] [PubMed] [Google Scholar]
- 18.Hildebrandt VH (1987) A review of epidemiological research on risk factors of low back pain. In: Muskuloskeletal disorders at work. University of Surrey, Guildford. Taylor and Francis
- 19.Hoogendoorn WE, Bongers PM, Vet HC, Ariens GA, Mechelen W, Bouter LM. High physical work load and low job satisfaction increase the risk of sickness absence due to low back pain: results of a prospective cohort study. Occup Environ Med. 2002;59:323–328. doi: 10.1136/oem.59.5.323. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Hubley-Kozey CL, Vezina MJ. Differentiating temporal electromyographic waveforms between those with chronic low back pain and healthy controls. Clin Biomech (Bristol, Avon) 2002;17:621–629. doi: 10.1016/S0268-0033(02)00103-1. [DOI] [PubMed] [Google Scholar]
- 21.Humphrey AR, Nargol AV, Jones AP, Ratcliffe AA, Greenough CG. The value of electromyography of the lumbar paraspinal muscles in discriminating between chronic-low-back-pain sufferers and normal subjects. Eur Spine J. 2005;14:175–184. doi: 10.1007/s00586-004-0792-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Kelsey JL, Githens PB, White AA, 3rd, Holford TR, Walter SD, O’Connor T, Ostfeld AM, Weil U, Southwick WO, Calogero JA. An epidemiologic study of lifting and twisting on the job and risk for acute prolapsed lumbar intervertebral disc. J Orthop Res. 1984;2:61–66. doi: 10.1002/jor.1100020110. [DOI] [PubMed] [Google Scholar]
- 23.Khatri M, Murray M, Greenough CG. Minimum clinically important difference in low back outcome score in individuals with low back pain. J Bone Joint Surg Br. 2003;85-B:236. [Google Scholar]
- 24.Klein AB, Snyder-Mackler L, Roy SH, DeLuca CJ. Comparison of spinal mobility and isometric trunk extensor forces with electromyographic spectral analysis in identifying low back pain. Phys Ther. 1991;71:445–454. doi: 10.1093/ptj/71.6.445. [DOI] [PubMed] [Google Scholar]
- 25.Krismer M, Tulder M. Strategies for prevention and management of musculoskeletal conditions. Low back pain (non-specific) Best Pract Res Clin Rheumatol. 2007;21:77–91. doi: 10.1016/j.berh.2006.08.004. [DOI] [PubMed] [Google Scholar]
- 26.Kupa EJ, Roy SH, Kandarian SC, Luca CJ. Effects of muscle fiber type and size on EMG median frequency and conduction velocity. J Appl Physiol. 1995;79:23–32. doi: 10.1152/jappl.1995.79.1.23. [DOI] [PubMed] [Google Scholar]
- 27.Lago P, Jones NB. Effect of motor-unit firing time statistics on e.m.g. spectra. Med Biol Eng Comput. 1977;15:648–655. doi: 10.1007/BF02457923. [DOI] [PubMed] [Google Scholar]
- 28.Leboeuf-Yde C, Yashin A, Lauritzen T. Does smoking cause low back pain? Results from a population-based study. J Manipulative Physiol Ther. 1996;19:99–108. [PubMed] [Google Scholar]
- 29.Leino PI. Does leisure time physical activity prevent low back disorders? A prospective study of metal industry employees. Spine. 1993;18:863–871. doi: 10.1097/00007632-199306000-00009. [DOI] [PubMed] [Google Scholar]
- 30.MacGregor AJ, Andrew T, Sambrook PN, Spector TD. Structural, psychological, and genetic influences on low back and neck pain: a study of adult female twins. Arthritis Rheum. 2004;51:160–167. doi: 10.1002/art.20236. [DOI] [PubMed] [Google Scholar]
- 31.Main CJ. The modified somatic perception questionnaire (MSPQ) J Psychosom Res. 1983;27:503–514. doi: 10.1016/0022-3999(83)90040-5. [DOI] [PubMed] [Google Scholar]
- 32.Mannion AF, Connolly B, Wood K, Dolan P. The use of surface EMG power spectral analysis in the evaluation of back muscle function. J Rehabil Res Dev. 1997;34:427–439. [PubMed] [Google Scholar]
- 33.Mannion AF, Dolan P. Electromyographic median frequency changes during isometric contraction of the back extensors to fatigue. Spine. 1994;19:1223–1229. doi: 10.1097/00007632-199405310-00006. [DOI] [PubMed] [Google Scholar]
- 34.Mannion AF, Dumas GA, Stevenson JM, Cooper RG. The influence of muscle fiber size and type distribution on electromyographic measures of back muscle fatigability. Spine. 1998;23:576–584. doi: 10.1097/00007632-199803010-00010. [DOI] [PubMed] [Google Scholar]
- 35.Mannion AF, Kaser L, Weber E, Rhyner A, Dvorak J, Muntener M. Influence of age and duration of symptoms on fibre type distribution and size of the back muscles in chronic low back pain patients. Eur Spine J. 2000;9:273–281. doi: 10.1007/s005860000189. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Mannion AF, Taimela S, Muntener M, Dvorak J. Active therapy for chronic low back pain part 1. Effects on back muscle activation, fatigability, and strength. Spine. 2001;26:897–908. doi: 10.1097/00007632-200104150-00013. [DOI] [PubMed] [Google Scholar]
- 37.Mannion AF, Weber BR, Dvorak J, Grob D, Muntener M. Fibre type characteristics of the lumbar paraspinal muscles in normal healthy subjects and in patients with low back pain. J Orthop Res. 1997;15:881–887. doi: 10.1002/jor.1100150614. [DOI] [PubMed] [Google Scholar]
- 38.Nargol AV, Jones AP, Kelly PJ, Greenough CG. Factors in the reproducibility of electromyographic power spectrum analysis of lumbar paraspinal muscle fatigue. Spine. 1999;24:883–888. doi: 10.1097/00007632-199905010-00009. [DOI] [PubMed] [Google Scholar]
- 39.Oddsson LI, Luca CJ. Activation imbalances in lumbar spine muscles in the presence of chronic low back pain. J Appl Physiol. 2003;94:1410–1420. doi: 10.1152/japplphysiol.01183.2001. [DOI] [PubMed] [Google Scholar]
- 40.Oliver CW, Tillotson KM, Jones AP, Royal RA, Greenough CG. Reproducibility of lumbar paraspinal surface electromyogram power spectra. Clin Biomech (Bristol, Avon) 1996;11:317–321. doi: 10.1016/0268-0033(96)00020-4. [DOI] [PubMed] [Google Scholar]
- 41.Panjabi MM. A hypothesis of chronic back pain: ligament subfailure injuries lead to muscle control dysfunction. Eur Spine J. 2005;27:27. doi: 10.1007/s00586-005-0925-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Person RS, Mishin LN. Auto- and cross-correlation analysis of the electrical activity of muscles. Med Electron Biol Eng. 1964;42:155–159. doi: 10.1007/BF02484214. [DOI] [PubMed] [Google Scholar]
- 43.Punnett L, Fine LJ, Keyserling WM, Herrin GD, Chaffin DB. Back disorders and nonneutral trunk postures of automobile assembly workers. Scand J Work Environ Health. 1991;17:337–346. doi: 10.5271/sjweh.1700. [DOI] [PubMed] [Google Scholar]
- 44.Ready AE, Boreskie SL, Law SA, Russell R. Fitness and lifestyle parameters fail to predict back injuries in nurses. Can J Appl Physiol. 1993;18:80–90. doi: 10.1139/h93-008. [DOI] [PubMed] [Google Scholar]
- 45.Riihimaki H. Low-back pain, its origin and risk indicators. Scand J Work Environ Health. 1991;17:81–90. [PubMed] [Google Scholar]
- 46.Roy SH, Luca CJ, Casavant DA. Lumbar muscle fatigue and chronic lower back pain. Spine. 1989;14:992–1001. doi: 10.1097/00007632-198909000-00014. [DOI] [PubMed] [Google Scholar]
- 47.Roy SH, Luca CJ, Emley M, Buijs RJ. Spectral electromyographic assessment of back muscles in patients with low back pain undergoing rehabilitation. Spine. 1995;20:38–48. doi: 10.1097/00007632-199501000-00008. [DOI] [PubMed] [Google Scholar]
- 48.Seki S, Kawaguchi Y, Chiba K, Mikami Y, Kizawa H, Oya T, Mio F, Mori M, Miyamoto Y, Masuda I, Tsunoda T, Kamata M, Kubo T, Toyama Y, Kimura T, Nakamura Y, Ikegawa S. A functional SNP in CILP, encoding cartilage intermediate layer protein, is associated with susceptibility to lumbar disc disease. Nat Genet. 2005;37:607–612. doi: 10.1038/ng1557. [DOI] [PubMed] [Google Scholar]
- 49.Stevenson JM, Weber CL, Smith JT, Dumas GA, Albert WJ. A longitudinal study of the development of low back pain in an industrial population. Spine. 2001;26:1370–1377. doi: 10.1097/00007632-200106150-00022. [DOI] [PubMed] [Google Scholar]
- 50.Stulen FB, DeLuca CJ. Frequency parameters of the myoelectric signal as a measure of muscle conduction velocity. IEEE Trans Biomed Eng. 1981;28:515–523. doi: 10.1109/TBME.1981.324738. [DOI] [PubMed] [Google Scholar]
- 51.Thompson DA, Biedermann HJ. Electromyographic power spectrum analysis of the paraspinal muscles. Long-term reliability. Spine. 1993;18:2310–2313. doi: 10.1097/00007632-199311000-00029. [DOI] [PubMed] [Google Scholar]
- 52.Dieen JH, Cholewicki J, Radebold A. Trunk muscle recruitment patterns in patients with low back pain enhance the stability of the lumbar spine. Spine. 2003;28:834–841. doi: 10.1097/00007632-200304150-00018. [DOI] [PubMed] [Google Scholar]
- 53.Videman T, Battie MC, Gibbons LE, Manninen H, Gill K, Fisher LD, Koskenvuo M. Lifetime exercise and disk degeneration: an MRI study of monozygotic twins. Med Sci Sports Exerc. 1997;29:1350–1356. doi: 10.1097/00005768-199710000-00012. [DOI] [PubMed] [Google Scholar]
- 54.Waddell G. The back pain revolution. London: Churchill Livingstone; 1998. [Google Scholar]
- 55.Zung WW. A Self-Rating Depression Scale. Arch Gen Psychiatry. 1965;12:63–70. doi: 10.1001/archpsyc.1965.01720310065008. [DOI] [PubMed] [Google Scholar]