Abstract
The treatment of patients with diffuse large B cell lymphoma (DLBCL) would be greatly facilitated with a rapid method for determining prognosis that can be performed more easily and earlier than cytological or specific pathological examinations. It has been suggested that newly diagnosed patients with DLBCL who have low maximum standard uptake value (SUVmax) on 18F-fluorodeoxyglucose positron emission tomography (FDG-PET) are more likely to be successfully treated and remain in remission compared with patients with high SUVmax, but this concept has been poorly studied. We retrospectively analyzed 50 patients with de novo DLBCL to evaluate the relationship between the SUVmax and disease progression. For patients with low SUVmax (n = 10) and high SUVmax (n = 40) (P = 0.255), respectively, the 3-year overall survival rates were 90 and 72 %, and the progression-free survival (PFS) rates were 90 and 39 % (P = 0.012). By multivariate analysis, the revised International Prognostics Index (R-IPI) and SUVmax at diagnosis were shown to predict longer PFS. The 3-year PFS for patients with low SUVmax classified into the good prognosis group by R-IPI was 100 vs. 62 % for those with high SUVmax (P = 0.161), and patients with low SUVmax classified into the poor prognosis group by R-IPI was 80 vs. 18 % for those with high SUVmax (P = 0.050). We conclude that the SUVmax on FDG-PET for newly diagnosed patients with DLBCL is an important predictor of disease progression, especially for patients with poor prognosis by R-IPI.
Keywords: SUVmax, FDG-PET, Diffuse large B cell lymphoma, Progression, Revised IPI
Introduction
Diffuse large B cell lymphoma (DLBCL) is the most common aggressive form of non-Hodgkin’s lymphoma. Combination chemotherapy with rituximab is initially administered to most newly diagnosed patients with DLBCL [1–4]. However, if the patients relapse after the initial chemotherapy, their lymphoma can be poorly managed because most DLBCL cases ultimately become chemotherapy-resistant unless treated with high-dose chemotherapy with autologous stem cell transplantation (ASCT) [5, 6]. Instead of combination chemotherapy with rituximab, other treatments including more intensive chemotherapy, up-front ASCT after the first remission, or other newly developed drugs are required to improve survival of the patients who are at high risk of relapse [7, 8]. Therefore, defining prognostic factors that can easily and accurately classify patients with untreated DLBCL into appropriate risk groups for relapse is highly important for disease management.
Although 18F-fluorodeoxyglucose positron emission tomography (FDG-PET) imaging for DLBCL have been widely utilized to evaluate the staging and residual lesions after treatment with high sensitivity [9–12], the relevance of the maximum standard uptake value (SUVmax) in this technique to disease outcome has been poorly studied. The SUVmax at the biopsy site of non-Hodgkin’s lymphoma patients has been reported to correlate with the proliferation potential [13]. Anecdotal cases from our hospital (unpublished) also suggest that patients with low SUVmax DLBCL before treatment are more likely to remain in remission, while those with high SUVmax DLBCL are more likely to relapse. However, this idea has not been confirmed by a systematic analysis of clinical cases. Therefore, in this study, we retrospectively analyzed 50 patients with DLBCL in order to examine the relationship between the initial SUVmax of FDG-PET and disease progression.
Patients and methods
Eligibility criteria
In this study, patients with de novo DLBCL, excluding those with transformation from indolent lymphoma, diagnosed between April 2006 and December 2009 at Ehime Prefectural Central Hospital (Matsuyama, Japan) were retrospectively analyzed. FDG-PET imaging was performed in all patients before the treatment, and the SUVmax at the primary lesion was measured. The patients subsequently received combination chemotherapy with rituximab. Patients whose primary lesions were excised surgically before FDG-PET imaging or who were treated palliatively, including only radiotherapy or only rituximab, were excluded from this study. The observation period was from April 2006 to March 2011.
PET/CT acquisition and processing
FDG-PET/CT imaging was performed using a multi-slice PET/CT camera (Discovery STE with 16-slice CT; GE Healthcare). All patients had fasted for a minimum of 6 h, with a blood glucose level of 80–120 mg/dL before intravenous administration of 18F-FDG. A whole-body image was obtained exactly 60 min after the intravenous administration of 222–370 MBq (6–10 mCi) of 18F-FDG. The PET emission images were corrected for measured attenuation and reconstructed using an ordered-subset expectation maximization iterative algorithm per the manufacturer’s instructions. Integrated PET and CT images were reviewed on Advantage Workstations (GE Healthcare). Display field of view was 60 × 60 cm, which consisted of 192 × 192 matrixes, on the display. Voxel size was 3.125 × 3.125 × 3.27 mm3. For each PET data set, in patients with multiple lesions, the tumor with the most intense FDG uptake among all foci was identified by the maximal counts. A volumetric region of interest was approximately 8 cm3 (250 voxels) or more and set on the axial fusion images of PET and CT to calculate SUVmax. A volumetric region of interest encompassing the entire tumor was drawn to ensure correct identification of the maximal counts, and the SUVmax was calculated.
Treatment
All patients received rituximab-containing combination chemotherapy as an initial treatment. The cyclophosphamide, doxorubicin, vincristine, and prednisolone with rituximab (R-CHOP) regimen was administered to younger patients (<70 years old) with DLBCL, and the pirarubicin, cyclophosphamide, vincristine, and prednisolone with rituximab (R-THPCOP) regimen was administered to elderly patients (≥70 years old). Most patients with advanced-stage disease, defined as Ann Arbor stages III or IV, or stage I and II with bulky disease (≥10 cm), received six to eight cycles of R-CHOP or R-THPCOP every 21 days. Only the patients who had Ann Arbor stages I and II without bulky disease received three cycles of R-CHOP or R-THPCOP and field radiation therapy. Complete remission (CR) was defined by FDG-PET scan according to the recently published criteria [9]. All relapsed patients received salvage chemotherapy, and ASCT was performed in eligible cases.
Statistical analysis
Overall survival (OS) was defined as the time from the start of chemotherapy to death from any cause. Progression-free survival (PFS) was defined as the time from the start of chemotherapy to relapse or death. The Mann–Whitney U test was used to calculate the differences between two groups. The probabilities of OS and PFS were estimated by the Kaplan–Meier method. The association of various factors with the hazards of failure for the time-to-endpoint PFS was estimated using the Cox proportional hazard regression model. A P value of <0.05 was considered statistically significant. SPSS version 17.0 was used for all analyses.
Results
Patients and characteristics
Fifty patients who met the eligibility criteria were analyzed. Clinical characteristics including International Prognostic Index (IPI) factors [14], revised IPI (R-IPI) [15], and the individual treatments are listed in Table 1. Most patients (90 %) received six to eight cycles of R-CHOP or R-THPCOP. Other patients (10 %) received three cycles of R-CHOP or R-THPCOP and field radiation therapy. No patients underwent up-front ASCT after R-CHOP or R-THPCOP. All patients experiencing refractory and relapsed DLBCL (n = 26) were treated with salvage chemotherapy, and seven patients (27 %) who achieved complete or partial response and were 70 years old or younger underwent ASCT with high-dose chemotherapy.
Table 1.
Patients characteristics
| All (n = 50) | Low SUVmax (n = 10) | High SUVmax (n = 40) | P value | |
|---|---|---|---|---|
| Median SUVmax (range) | 21.0 (8.2–47.1) | 11.4 (8.2–14.7) | 22.1 (15.0–47.1) | <0.001 |
| Median age (range) | 66 (41–85) | 63 (49–82) | 67 (41–85) | 0.280 |
| Male/female | 32/18 | 4/6 | 28/12 | 0.080 |
| IPI factors | ||||
| Age >60 years | 37 | 8 | 29 | 0.632 |
| PS >1 | 16 | 1 | 15 | 0.099 |
| LDH >normal | 32 | 5 | 27 | 0.307 |
| Extranodal site >1 | 16 | 4 | 12 | 0.548 |
| Stage III/IV | 31 | 6 | 25 | 0.885 |
| DLBCL subgroup/subtype | ||||
| NOS | 42 | 10 | 32 | |
| THRLBCL | 2 | 0 | 2 | |
| PCDLBCL | 4 | 0 | 4 | |
| PMBL | 2 | 0 | 2 | |
| IPI H/I, H | 30 | 5 | 25 | 0.475 |
| Revised IPI | 0.431 | |||
| Very good | 5 | 2 | 3 | |
| Good | 16 | 3 | 13 | |
| Poor | 29 | 5 | 24 | |
| Bulky mass | 5 | 0 | 5 | 0.243 |
| sIL-2R >normal | 39 | 7 | 32 | 0.499 |
| Primary lesion | 0.401 | |||
| LNs | 24 | 6 | 18 | |
| Others | 26 | 4 | 22 | |
| Treatment | 0.161 | |||
| R-CHOP | 36 | 9 | 27 | |
| R-THPCOP | 14 | 1 | 13 | |
| Complete remission | 39 | 9 | 30 | 0.311 |
| Recurrence | 26 | 1 | 25 | 0.003 |
| Alive/death | 38/12 | 9/1 | 29/11 | 0.251 |
SUV max maximum standardized uptake value, IPI International Prognostic Index, PS Eastern Cooperative Oncology Group Performance Status, LDH lactate dehydrogenase, DLBCL diffuse large B cell lymphoma, NOS not otherwise specified, THRLBCL T cell/histiocyte-rich large B cell lymphoma, PCDLBCL primary cutaneous diffuse large B cell lymphoma, PMBL primary mediastinal large B cell lymphoma, sIL-2R soluble interleukin-2 receptor, LNs lymph nodes, R-CHOP cyclophosphamide, doxorubicin, vincristine, and prednisolone with rituximab, R-THPCOP pirarubicin, cyclophosphamide, vincristine, and prednisolone with rituximab
The patients were first divided into two prognostic factor groups at various (10, 15, 20, 25, 30, or 35) in order to determine the appropriate cutoff point, and then OS and PFS were analyzed. Although OS curves were not significantly different between each pair of groups for all cutoff values, PFS curves were significantly higher in patients with the SUVmax <15 than in those with the SUVmax ≥15. Other cutoff values for PFS curves were not statistically significant. Thus, we determined that the SUVmax cutoff value should be 15 in this study.
Univariate and multivariate analysis of OS and PFS for patients with low- and high SUVmax
The median follow-up time was 32.7 months (range, 4.8–58.3 months). Patients with SUVmax <15 (low SUVmax) (n = 10) and those with SUVmax ≥15 (high SUVmax) (n = 40) had similar backgrounds regarding age, sex, IPI factors, IPI classification, R-IPI classification, and individual treatment (Table 1). The CR rate of all patients was 78 %. CR rates of patients with low SUVmax and those with high SUVmax were 90 and 75 %, respectively (P = 0.311). However, patients with low SUVmax had a significantly lower recurrence rate than that of those with high SUVmax values (P = 0.003).
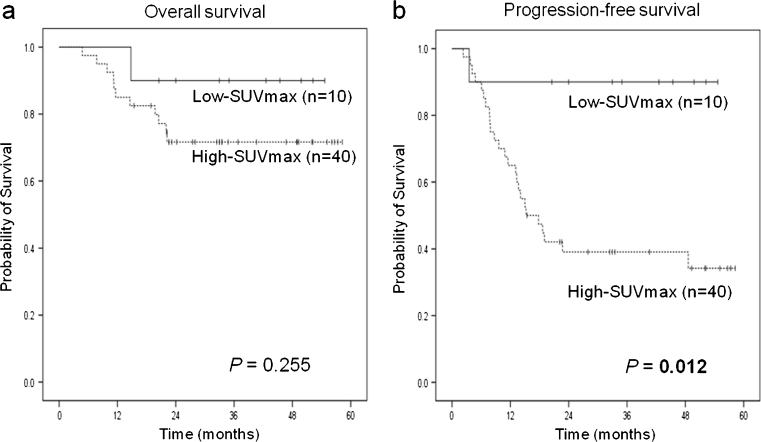
The 3-year OS rates for patients with low SUVmax and for those with high SUVmax were 90 and 72 %, respectively (P = 0.255) (Fig. 1a). The 3-year PFS rate in each group was 90 and 39 %, respectively (P = 0.012) (Fig. 1b). While no factors could predict OS, multivariate analysis of PFS showed that the R-IPI [hazard ratio (HR) 3.37 (1.35–8.39), P = 0.009] and low SUVmax [HR 7.49 (1.00–55.95), P = 0.049] were good independent prognostic factors (Table 2).
Fig. 1.
OS (a) and PFS (b) based on SUVmax
Table 2.
Multivariate analysis of risk factors for OS and PFS
| OS | PFS | |||||
|---|---|---|---|---|---|---|
| HR | (95 % CI) | P | HR | (95 % CI) | P | |
| Revised IPI | 1.92 | (0.58–6.36) | 0.287 | 3.37 | (1.35–8.39) | 0.009 |
| Low SUVmax | 2.51 | (0.31–20.03) | 0.385 | 7.49 | (1.00–55.95) | 0.049 |
| Bulky mass | 1.02 | (0.21–4.99) | 0.979 | 1.29 | (0.37–4.51) | 0.693 |
| sIL-2R >normal | 2.31 | (0.27–19.42) | 0.441 | 0.85 | (0.27–2.67) | 0.775 |
| Primary lesions except LNs | 1.49 | (0.42–5.23) | 0.533 | 1.01 | (0.44–2.29) | 0.988 |
OS overall survival, PFS progression-free survival, HR hazard ratio, 95 % CI 95 % confidence interval, IPI International Prognostic Index, SUV max maximum standardized uptake value, sIL-2R soluble interleukin-2 receptor, LNs lymph nodes
Analysis of R-IPI combined with SUVmax
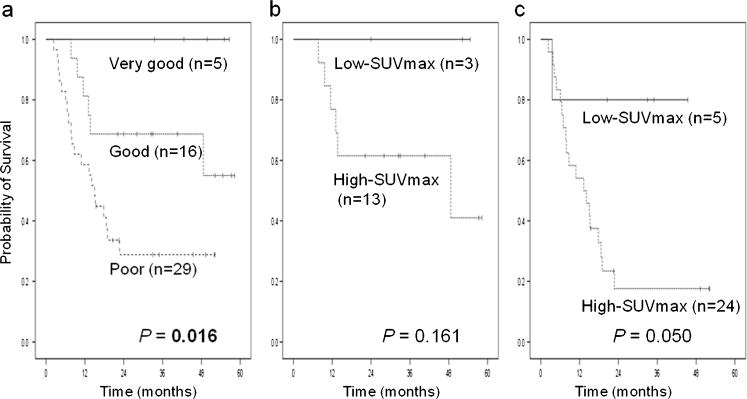
According to the R-IPI categories, all patients in this study were divided into prognosis groups of “very good” (n = 5), “good” (n = 16), and “poor” (n = 29), and the 3-year OS and PFS for each group were 100, 81, and 68 % (P = 0.167) and 100, 69, and 29 % (P = 0.016) (Fig. 2a), respectively. In the very good prognosis group, no patients had a recurrence of DLBCL. In the good prognosis group, the 3-year OS and PFS for patients with low SUVmax and those with high SUVmax were 100 and 77 % (P = 0.386) and 100 and 62 % (P = 0.161), respectively (Fig. 2b). In the poor prognosis group, the 3-year OS and PFS for patients with low SUVmax and those with high SUVmax were 80 and 68 % (P = 0.549) and 80 and 18 % (P = 0.050), respectively (Fig. 2c).
Fig. 2.
PFS of all patients divided into “very good,” “good,” and “poor” prognosis groups by R-IPI (a), of patients in the “good” prognosis group according to SUVmax (b), and of patients in the “poor” prognosis group according to SUVmax (c)
Discussion
A relatively higher proportion of patients administered initial chemotherapy including rituximab have been shown to be successfully treated and remain in remission from newly diagnosed DLBCL, compared with those receiving no rituximab [1–4], but a large number of patients still undergo relapses. Treatment strategies other than R-CHOP are either initially more intensive chemotherapy or high-dose chemotherapy followed by up-front ASCT or newly developed drug. More useful prognostic factors are clearly required to identify patients with poorly managed DLBCL. However, most cytological or pathological prognostic factors for patients with DLBCL, such as bcl-2, bcl-6, CD5, CD10, and MUM-1 [16–18], are relatively expensive or time-consuming to implement for general clinical practice, since those measurements can be performed only at specific hospitals or external laboratories.
Our results indicate that the SUVmax of FDG-PET in the primary diagnosis of DLBCL is an important predictor of progression after the initial treatment, especially for patients categorized into the poor prognostic group by R-IPI. Furthermore, most patients with low SUVmax or categorized into the very good prognostic group by R-IPI sustained CR only with R-CHOP or R-THPCOP therapy. The SUVmax has been reported to correlate with the MIB-1 labeling index (i.e., proliferation potential), a known prognostic factor in DLBCL patients treated with R-CHOP [13, 19]. Therefore, DLBCL patients with low SUVmax appear to progress more slowly and had better prognosis than those with high SUVmax. FDG-PET imaging for DLBCL can be used not only for staging but also for predicting the progression after treatment, and the SUVmax is highly useful, since it can be measured much more easily and quickly than cytological or specific pathological examinations.
Chihara et al. reported an association between high SUVmax on FDG-PET with shorter overall survival in patients with DLBCL [20]. Their conclusions were remarkably similar to ours, while the SUVmax cutoff value of 30 in their study differed greatly from that of 15 in our study. The PET/CT camera, incorporation time, and treatment were the same between the two studies. However, more good prognostic patients and fewer poor prognostic patients classified by the IPI score (probably due to patients with SUVmax values of 15–30) were included in their report than in our study. Determination of the SUVmax cutoff value was likely affected by individual patient characteristics or the number of cases at the different institutes. Therefore, a multicenter analysis may be required in order to define the appropriate SUVmax cutoff value.
Collectively, our results suggest that the SUVmax on FDG-PET for newly diagnosed patients with DLBCL is an important predictor of PFS. A future prospective study to confirm our results would be of interest.
Acknowledgments
Conflict of interest
The authors declare that they have no conflict of interest.
Open Access
This article is distributed under the terms of the Creative Commons Attribution License which permits any use, distribution, and reproduction in any medium, provided the original author(s) and the source are credited.
References
- 1.Coiffier B, Thieblemont C, Van Den Neste E, et al. Long-term outcome of patients in the LNH-98.5 trial, the first randomized study comparing rituximab-CHOP to standard CHOP chemotherapy in DLBCL patients: a study by the Group d’Etudes des Lymphomes de l’Adulte. Blood. 2010;116:2040–2045. doi: 10.1182/blood-2010-03-276246. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Pfreundschuh M, Kuhnt E, Trumper L, et al. CHOP-like chemotherapy with or without rituximab in young patients with good-prognosis diffuse large-B-cell lymphoma: 6-year results of an open-label randomised study of the MabThera International Trial (MInT) Group. Lancet Oncol. 2011;11:1013–1022. doi: 10.1016/S1470-2045(11)70235-2. [DOI] [PubMed] [Google Scholar]
- 3.Pfreundschuh M, Trumper L, Kloess M, et al. Two-weekly or 3-weekly CHOP chemotherapy with or without etoposide for the treatment of elderly patients with aggressive lymphomas: results of the NHL-B2 trial of the DSHNHL. Blood. 2004;104:634–641. doi: 10.1182/blood-2003-06-2095. [DOI] [PubMed] [Google Scholar]
- 4.Pfreundschuh M, Schubert J, Ziepert M, et al. Six versus eight cycles of bi-weekly CHOP-14 with or without rituximab in elderly patients with aggressive CD20+ B-cell lymphomas: a randomised controlled trial (RICOVER-60) Lancet Oncol. 2008;9:105–116. doi: 10.1016/S1470-2045(08)70002-0. [DOI] [PubMed] [Google Scholar]
- 5.Gisselbrecht C, Glass B, Mounier N, et al. Salvage regimens with autologous transplantation for relapsed large B-cell lymphoma in the rituximab era. J Clin Oncol. 2010;28:4148–4190. doi: 10.1200/JCO.2010.28.1618. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Philip T, Guglielmi C, Hagenbeek A, et al. Autologous bone marrow transplantation as compared with salvage chemotherapy in relapses of chemotherapy-sensitive non-Hodgkin’s lymphoma. N Engl J Med. 1995;333:1540–1545. doi: 10.1056/NEJM199512073332305. [DOI] [PubMed] [Google Scholar]
- 7.Haioun C, Lepaqe E, Gisselbrecht C, et al. Survival benefit of high-dose therapy in poor-risk aggressive non-Hodgkin’s lymphoma: final analysis of the prospective LNH87–2 protocol—a groupe d’Etude des lymphomes de l’Adulte study. J Clin Oncol. 2000;18:3025–3030. doi: 10.1200/JCO.2000.18.16.3025. [DOI] [PubMed] [Google Scholar]
- 8.Greb A, Bohlius J, Trelle S, et al. High-dose chemotherapy with autologous stem cell support in first-line treatment of aggressive non-Hodgkin lymphoma—results of a comprehensive meta-analysis. Cancer Treat Rev. 2007;33:338–346. doi: 10.1016/j.ctrv.2007.02.002. [DOI] [PubMed] [Google Scholar]
- 9.Cheson BD, Pfistner B, Juweid ME, et al. Revised response criteria for malignant lymphoma. J Clin Oncol. 2007;25:579–586. doi: 10.1200/JCO.2006.09.2403. [DOI] [PubMed] [Google Scholar]
- 10.Seam P, Juweid ME, Cheson BD. The role of FDG-PET scans in patients with lymphoma. Blood. 2007;110:3507–3516. doi: 10.1182/blood-2007-06-097238. [DOI] [PubMed] [Google Scholar]
- 11.Juweid ME, Stroobants S, Hoekstra OS, et al. Use of positron emission tomography for response assessment of lymphoma: consensus of the Imaging Subcommittee of International Harmonization Project in Lymphoma. J Clin Oncol. 2007;25:571–578. doi: 10.1200/JCO.2006.08.2305. [DOI] [PubMed] [Google Scholar]
- 12.Kobe C, Dietlein M, Franklin J, et al. Positron emission tomography has a high negative predictive value for progression or early relapse for patients with residual disease after first-line chemotherapy in advanced-stage Hodgkin lymphoma. Blood. 2008;112:3989–3994. doi: 10.1182/blood-2008-06-155820. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Watanabe R, Tomita N, Takeuchi K, et al. SUVmax in FDG-PET at the biopsy site correlates with the proliferation potential of tumor cells in non-Hodgkin lymphoma. Leuk Lymphoma. 2010;51:279–283. doi: 10.3109/10428190903440953. [DOI] [PubMed] [Google Scholar]
- 14.Anonymous (1993) A predictive model for aggressive non-Hodgkin’s lymphoma. The International Non-Hodgkin’s Lymphoma Prognostic Factors Project. N Engl J Med 329: 987–994 [DOI] [PubMed]
- 15.Sehn LH, Berry B, Chhanabhai M, et al. The revised International Prognostic Index (R-IPI) is a better predictor of outcome than the standard IPI for patients with diffuse large B-cell lymphoma treated with R-CHOP. Blood. 2007;109:1857–1861. doi: 10.1182/blood-2006-08-038257. [DOI] [PubMed] [Google Scholar]
- 16.Yamaguchi M, Seto M, Okamoto M, et al. De novo CD5+ diffuse large B-cell lymphoma: a clinicopathologic study of 109 patients. Blood. 2002;99:815–821. doi: 10.1182/blood.V99.3.815. [DOI] [PubMed] [Google Scholar]
- 17.Ennishi D, Takeuchi K, Yokoyama M, et al. CD5 expression is potentially predictive of poor outcome among biomarkers in patients with diffuse large B-cell lymphoma receiving rituximab plus CHOP therapy. Ann Oncol. 2008;19:1921–1926. doi: 10.1093/annonc/mdn392. [DOI] [PubMed] [Google Scholar]
- 18.Hans CP, Weisenburger DD, Greiner TC, et al. Confirmation of the molecular classification of diffuse large B-cell lymphoma by immunohistochemistry using a tissue microarray. Blood. 2004;103:275–282. doi: 10.1182/blood-2003-05-1545. [DOI] [PubMed] [Google Scholar]
- 19.Yoon DH, Choi DR, Ahn HJ, et al. Ki-67 expression as a prognostic factor in diffuse large B-cell lymphoma patients treated with rituximab plus CHOP. Eur J Haematol. 2010;85:149–157. doi: 10.1111/j.1600-0609.2010.01467.x. [DOI] [PubMed] [Google Scholar]
- 20.Chihara D, Oki Y, Onoda H, et al. High maximum standard uptake value (SUVmax) on PET scan is associated with shorter survival in patients with diffuse large B cell lymphoma. Int J Hematol. 2011;93:502–508. doi: 10.1007/s12185-011-0822-y. [DOI] [PubMed] [Google Scholar]