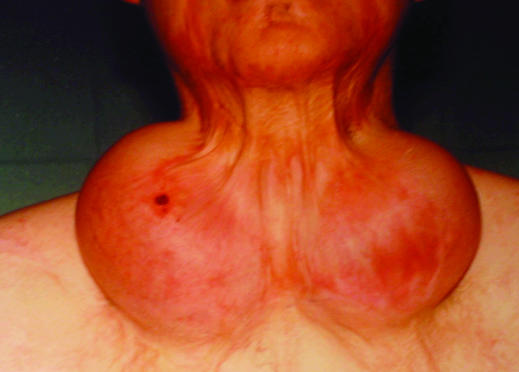
The basic concerns in burns reconstruction are for function, comfort, and appearance. Normal and hypertrophic scarring, scar contracture, loss of parts of the body, and change in colour and texture of injured skin are processes common to all seriously burnt patients and yet unique to each.
A realistic approach is necessary to harmonise patients' expectations (which are very high) with the probable outcomes of reconstructive surgery. Burn reconstruction starts when a patient is admitted with acute burns and lasts until the patient's expectations have been reached or there is nothing else to offer. However, even when this time has come, the patient-surgeon relationship may still continue and can last a lifetime.
Any surgeon undertaking burn reconstruction must have good understanding of wound healing and scar maturation to plan the time of reconstruction, and sound knowledge of all surgical techniques and all the aftercare required (usually in conjunction with a burn team). A strong patient-surgeon relationship is necessary in order to negotiate a master plan and agree on priorities.
Time of reconstruction
Definitive correction of burn scarring should generally be delayed for a year or more after scar healing. Unsightly scars mature over time, and, with the help of pressure and splints, many of them do not require surgery once the acute phase of scar maturation is over. Patience is often the best tool of a reconstructive surgeon. However, certain problems must be dealt with before scar maturation is complete. In burn reconstruction there are urgent procedures, others that are essential, and many that are desirable. It is for the last group that a good patient-surgeon relationship is necessary for negotiation on which procedures take priority.
Figure 1.
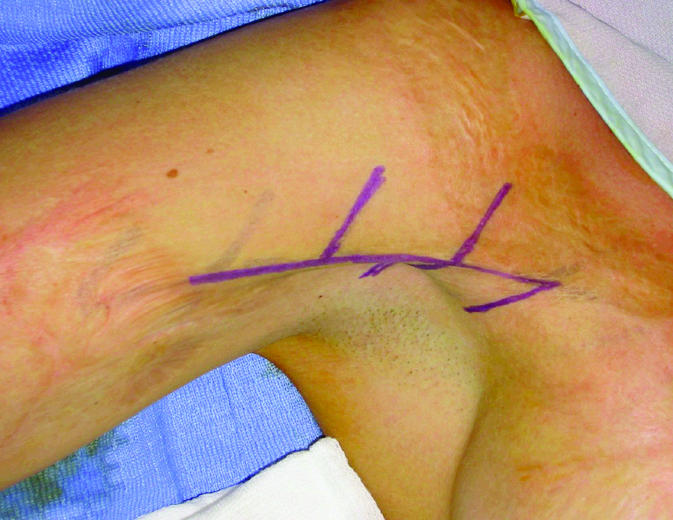
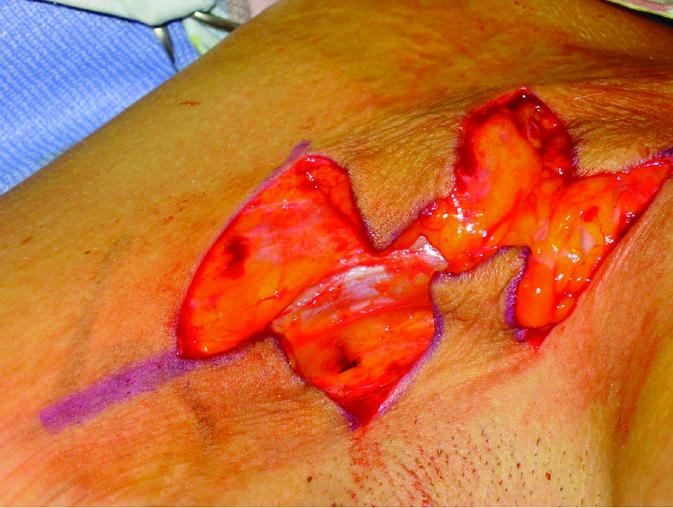
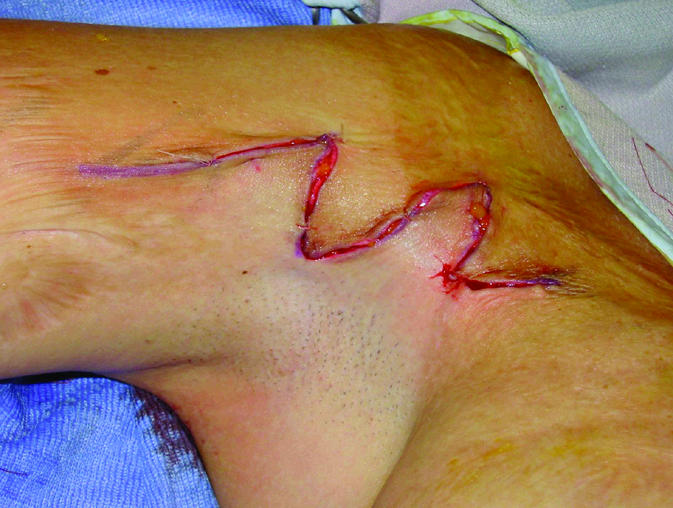
Top: Burn scar contracture on the anterior axillary line. Planned Z-plasties for contracture release are shown. Middle: The scar has been incised and all flaps raised. Bottom: Closure of the Z-plasties after rotation of all flaps. Note that the scar contracture has been released and the scar lengthened. This method increases the tissue availability in the reconstructed area and increases the range of motion
Urgent procedures—Waiting for scar maturation is inappropriate when it is certain that an operation is needed to correct a deformity or if vital structures are exposed or can be severely damaged. Urgent procedures should be restricted to those needed to correct function for injuries that are not suitable for other treatments. Examples include an eyelid release to protect an exposed cornea, correction of distracted or entrapped neurovascular bundles, severe fourth degree contractures, and severe microstomia.
Table 1.
Techniques for use in acute phase of scar maturation to diminish reconstructive needs
| • Use of darts in escharotomies when crossing joints | • Place seams following skin tension lines |
| • Use sheet grafts when possible | • Place grafts transversely over joints |
| • Use aesthetic units to face and hands with medium thickness split skin grafts | • Early pressure therapy |
| • Use of splints, face masks, and silicone inserts as soon as possible | • Early ambulation and exercise |
Essential procedures—Although they are not urgent since no important structure or the patient's overall health is challenged, essential procedures may, if performed early, improve the patient's final appearance and rehabilitation. Such procedures include operations for all burn scar contractures that do not respond to rehabilitation, and hypertrophic scarring and contractures that prevent a patient from eating, bathing, moving, or performing everyday activities.
Table 2.
Timing of burn reconstructive surgery
| Urgent procedures |
| • Exposure of vital structures (such as eyelid releases) |
| • Entrapment or compression of neurovascular bundles |
| • Fourth degree contractures |
| • Severe microstomia |
| Essential procedures |
| • Reconstruction of function (such as limited range of motion) |
| • Progressive deformities not correctable by ordinary methods |
| Desirable procedures |
| • Reconstruction of passive areas |
| • Aesthetics |
Desirable reconstructive procedures—Most of the problems that patients may present fall in this category. These are often aesthetic problems and scars contractures that, although not prominent, produce great discomfort. For all desirable procedures, it is good practice to wait until all red and immature scars have disappeared before starting any kind of surgery. An early operation is often unnecessary in these circumstances.
Patient-surgeon relationship
The relationship between a burns patients and a reconstructive burn surgeon is normally long lasting, often continuing for a lifetime. Patients not only require a surgeon's professional expertise, but also time, a good dose of optimism, and compassion.
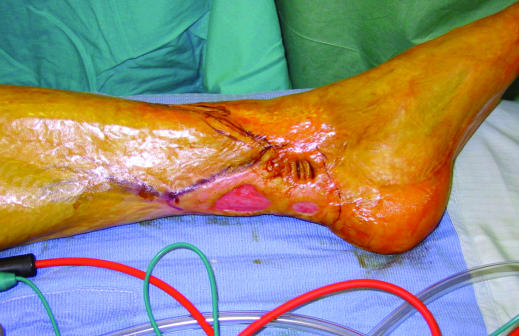
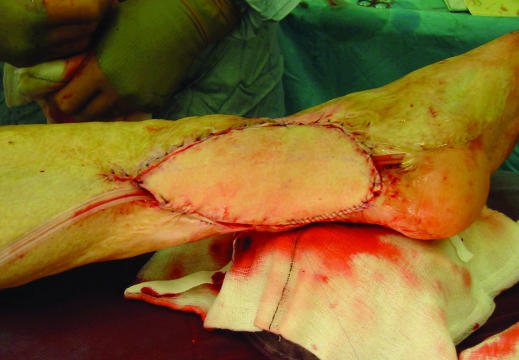
Figure 4.
Top: Unstable burn scars with chronic open wounds on medial malleolus. Bottom: The scars were excised and the defect reconstructed with a free vascularised perforator based skin flap. In this case skin from the thigh was transplanted to the ankle with microsurgical vascular anastomosis. These techniques allow the transplantation of any tissue (skin, fascia, fat, functional muscle, and bone) in the same patient
The initial meeting is one of the most important events. The patient presents a set of problems, and the reconstructive surgeon has to evaluate these and the patient's motivation for surgery and psychological status. We have to remember, though, that the patient will also evaluate the surgeon's attitude and conduct.
Although deformities or chief complaints will often be apparent and ready for surgery, it is preferable to have further visits before surgery, to allow new queries to be addressed and unhurried preparation for surgery. Photographic workup is extremely important to assist in definitive preoperative planning and for documentation.
Patients need frequent reassurance. A reconstructive surgeon needs to know a patient's fears and feelings as the reconstructive plan goes on. A burn reconstruction project commonly requires more than 10 operations and many clinic visits over a long period before a final assessment is made. In the case of a small child, this may take more than 18 years. Patients' feelings and impressions must be addressed continuously, and any trouble, minor disappointment, or depression detected early and treated as needed.
Burn reconstructive visit
One of the most important events during burn reconstruction is the burn reconstructive visit. At that time, a complete and accurate overview of the problems and possible solutions is performed in the following step wise manner:
Obtain as complete a record of the acute hospitalisation as possible
Take a thorough history and make a full physical examination
Make a complete record of all encountered problems. Note quality and colour of the skin in the affected areas—abnormal scars, hyperpigmentation or hypopigmentation, contractures, atrophy, and open wounds
Consider function. Explore all affected joints and note ranges of motion. Outline any scar contracture extending beyond joints
Consider skeletal deformities. Scar contractures may distract joints and the body maintain an abnormal position to overcome the deformity. This is particularly true in children; the effect of traction on a growing joint and bone can create long term deformities
Consider needs for physiotherapy, occupational therapy, and pressure garments. If any of these devices will be needed after surgery the patient must be referred to the rehabilitation department for consideration
Make an inventory of all possible sites for donor tissue.
Once a patient has voiced all his or her chief complaints and a thorough examination of the patient has been done, a master plan is developed. All reconstructive possibilities are discussed with the patient, and the timing and order of such procedures are outlined.
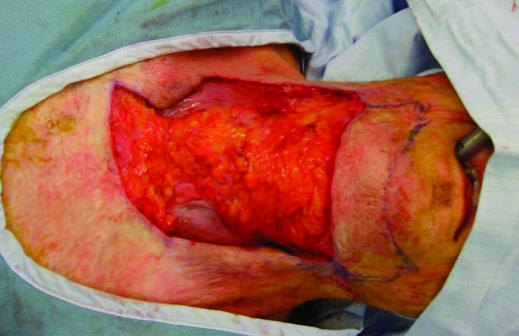
Figure 6.
Incisional release of a severe neck contracture. Scar releases leave substantial tissue losses that require extensive skin autografting. Although scar release is still the first choice for some difficult contractures, flap reconstruction and mobilisation of adjacent tissues should be attempted to decrease the size of the defect to be grafted
Surgical procedures
Burn reconstructive surgery has advanced in recent decades, though not as dramatically as in other areas of plastic surgery. For many years, burn reconstructive surgery comprised incisional or excisional releases of scars and skin autografting. Nowadays, however, the first approach that should be considered is use of local or regional flaps. These provide new and vascularised tissue to the area, they grow in children, and they give the best functional and cosmetic results. Such flaps can be raised either with normal skin or with burn scar. Even though burnt tissue generally has a high tendency to congestion, ischaemia, and necrosis, it can be used as a reliable flap if extreme care is taken while raising the flap and the injured skin is left attached to the underlying tissues.
When planning surgery for a burnt patient, a surgeon must consider what is the patient's primary complaint, what tissues are left, what parts are missing, and what sort of donor sites are available. This will help to determine the techniques available for burn reconstruction. The patient's chief complaint or complaints need to be carefully evaluated. If immature scars or an increasing deformity is present, and no urgent or essential procedure is required, pressure garments and occupational and physical therapy are indicated. If the deformity is stable and there is a need for reconstruction, an inventory of donor sites and priorities should be made.
Table 4.
Techniques for burn reconstruction
| Without deficiency of tissue |
| • Excision and primary closure |
| • Z-plasty |
| With deficiency of tissue |
| • Simple reconstruction |
| • Skin graft |
| • Dermal templates and skin grafts |
| Transposition flaps (Z-plasty and modifications) |
| • Reconstruction of skin and underlying tissues |
| Axial and random flaps |
| Myocutaneous flaps |
| Tissue expansion |
| • Free flaps |
| • Prefabricated flaps |
Dealing with deficiency of tissue
At this point, the burn injury must be assessed for deficiency in tissue. If there is no deficiency and local tissues can be easily mobilised, excision and direct closure or Z-plasties can be performed.
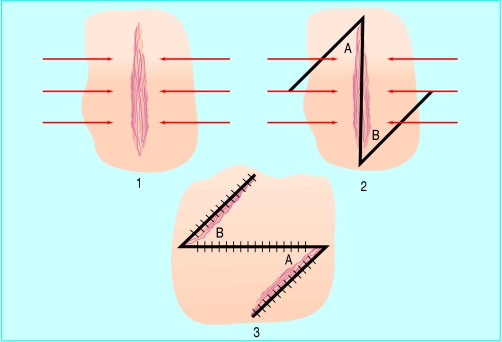
Figure 7.
Traditional Z-plasty to release a burn scar contracture. (1) The burn scar, showing the skin tension lines. (2) Z-plasty is performed by rotating two transposition flaps with an angle of 60° with the middle limb of the Z on the scar. (3) Final appearance after insetting of flaps. Note the lengthening of the tissue and the change of scar pattern. Z-plasties can be combined with other flaps (five limb Z-plasty, seven limb Z-plasty, etc)
If, however, there is a deficiency in tissue, the problem of how to reconstruct underlying structures must be addressed. If the deformity affects the skin and subcutaneous tissues, skin autografting, Z-plasties, and all the modifications of them (such as trident flaps) are advised. When reconstruction of underlying structures is necessary, flaps should be considered, including direct cutaneous, musculocutaneous, perforator based, and expanded flaps and microvascular transfer of tissues (free flaps). The precise choice is made on an individual basis.
Figure 8.
Expansion of normal skin by means of inflatable prostheses implanted in subcutaneous tissue. These are inflated with saline over several weeks until enough extra skin has been created. The expanded skin is then mobilised as full thickness skin grafts, regional advancement flaps, or free flaps. These provide large amounts of normal skin to resurface scarred areas
In addition, composite grafts and bone or cartilage grafts are often necessary in order to perform a complete reconstruction. The use of alloplastic materials in these circumstances is not advisable because of their tendency to extrusion.
Summary
Even though incisional or excisional release and skin autografting (with or without use of dermal templates) are still the main techniques used in burn reconstruction, flaps should be used when possible (remember that Z-plasty and its modifications are transposition flaps). The burn reconstruction plan needs to be tailored to the individual patient and the patient's chief complaint, since certain anatomical areas are better suited to some techniques than others.
Table 3.
Essentials of burn reconstruction
| • Strong patient-surgeon relationship |
| • Psychological support |
| • Clarify expectations |
| • Explain priorities |
| • Note all available donor sites |
| • Start with a “winner” (easy and quick operation) |
| • As many surgeries as possible in preschool years |
| • Offer multiple, simultaneous procedures |
| • Reassure and support patient |
This is the eighth in a series of 12 articles
Juan P Barret is consultant plastic and reconstructive surgeon, St Andrews Centre for Plastic Surgery and Burns, Broomfield Hospital, Chelmsford.
The ABC of burns is edited by Shehan Hettiaratchy, specialist registrar in plastic and reconstructive surgery, Pan-Thames Training Scheme, London; Remo Papini, consultant and clinical lead in burns, West Midlands Regional Burn Unit, Selly Oak University Hospital, Birmingham; and Peter Dziewulski, consultant burns and plastic surgeon, St Andrews Centre for Plastic Surgery and Burns, Broomfield Hospital, Chelmsford. The series will be published as a book in the autumn.
Competing interests: See first article for series editors' details.
Further reading and resources
- • Herndon DN, ed. Total burn care. 2nd ed. London: WB Saunders, 2002
- • Engrav LH, Donelan MB. Operative techniques in plastic and reconstructive surgery. Face burns: acute care and reconstruction. London: WB Saunders, 1997
- • Achauer BM. Burn reconstruction. New York: Thiene, 1991
- • Barret JP, Herndon DN. Color atlas of burn care. London: WB Saunders, 2001
- • Brou JA, Robson MC, McCauley RL. Inventory of potential reconstructive needs in the patient with burns. J Burn Care Rehabil 1989;10: 555-60 [DOI] [PubMed] [Google Scholar]