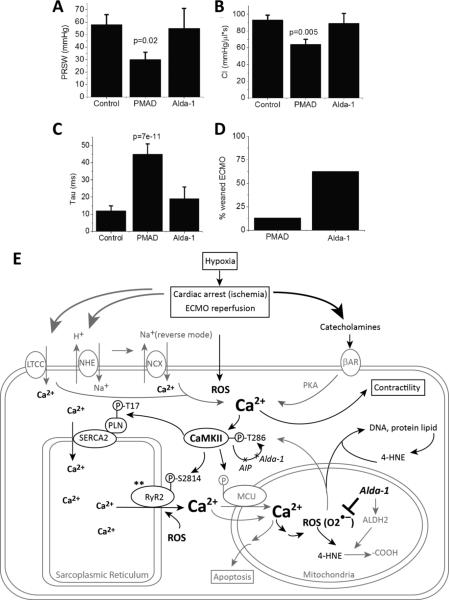
FIGURE 8.
Alda-1 improved in vivo contractility and recovery rate to spontaneous circulation after cardiac arrest. A. Summary data for ESPVR for control, PMAD, PMAD-Alda (Alda-1) p=0.006. B. Summary data for PRWV for control, PMAD, PMAD-Alda (Alda-1), p=0.04. C. Summary data for CI for control, PMAD, PMAD-Alda (Alda-1)D. Summary data for tau for control, PMAD, PMAD-Alda (Alda-1). P-values in graphs are with respect to control using post-hoc analysis. Comparisons between groups performed using Kruskall-Wallis nonparamateric test. E. Proposed mechanism for post-arrest myocardial dysfunction, mediated by calcium overload, CaMKII, and oxidative stress (ROS). Catecholamines released during cardiac arrest and the ischemic/reperfusion process triggered cytosolic Ca2+ influx and SR Ca2+ release/uptake. The activation of RyR2 (by oxidative stress or other unknown mechanism**) also increased CICR. Elevated cytosolic Ca2+ -activated CaMKII further enhanced CICR and lead to mitochondrial Ca2+ overload. This Ca2+ overload contributed to excess ROS (O2•–) and reactive aldehyde (4-HNE) generation, more CaMKII activation, and other cellular damages. AIP inhibited CaMKII autophosphorylation but did not improve cardiac function after arrest. Alda-1 reduced oxidative stress, inhibited CaMKII auto-phosphorylation and improved cardiac function.