Abstract
Cirrhosis due to any etiology disrupts the homeostatic role of liver in the body. Cirrhosis-associated immune dysfunction leads to alterations in both innate and acquired immunity, due to defects in the local immunity of liver as well as in systemic immunity. Cirrhosis-associated immune dysfunction is a dynamic phenomenon, comprised of both increased systemic inflammation and immunodeficiency, and is responsible for 30% mortality. It also plays an important role in acute as well as chronic decompensation. Immune paralysis can accompany it, which is characterized by increase in anti-inflammatory cytokines and suppression of proinflammatory cytokines. There is also presence of increased gut permeability, reduced gut motility and altered gut flora, all of which leads to increased bacterial translocation. This increased bacterial translocation and consequent endotoxemia leads to increased blood stream bacterial infections that cause systemic inflammatory response syndrome, sepsis, multiorgan failure and death. The gut microbiota of cirrhotic patients has more pathogenic microbes than that of non-cirrhotic individuals, and this disturbs the homeostasis and favors gut translocation. Prompt diagnosis and treatment of such infections are necessary for better survival. We have reviewed the various mechanisms of immune dysfunction and its consequences in cirrhosis. Recognizing the exact pathophysiology of immune dysfunction will help treating clinicians in avoiding its complications in their patients and can lead to newer therapeutic interventions and reducing the morbidity and mortality rates.
Keywords: Cirrhosis, Immune dysfunction, Inflammation, Liver disease
Introduction
Cirrhosis and its complications are a major cause of morbidity and mortality at the community level. Liver has a homeostatic role in the body’s immunity and cirrhosis due to any etiology disrupts this homeostasis. Cirrhosis-associated immune dysfunction (CAID) is the acquired alteration of both innate and acquired immunity1 and leads to immunodeficiency as well as systemic inflammation,2 ultimately leading to around 30% mortality.3 Immunodeficiency in cirrhosis is due to derangement of local immunity of liver and of systemic immune cells. The systemic inflammation results from persistent immune cell stimulation, leading to production of various proinflammatory cytokines.2
In the CAID condition, there is enhanced gut translocation of bacteria that can lead to endotoxemia and increased cytokines, thereby resulting in an exaggerated inflammatory host response and increased occurrence of systemic bacterial infection that can progress to septic shock, multiorgan dysfunction and even death.4–8 Initially, in CAID, there is increased systemic inflammation in stable decompensated cirrhosis, changing to a predominantly immunodeficient state in severe decompensated cirrhosis and acute on chronic liver failure (ACLF).2 The extent of immune dysfunction is directly related to severity of liver injury,3 and the maximum dysfunction is seen in alcoholic cirrhosis.9 Therefore, gaining a comprehensive and precise understanding of this immune dysfunction is necessary for prevention, early diagnosis and proper treatment of infections in cirrhosis to improve chances of patient survival.
Immunity and liver
The innate immune system is made of cellular and humoral components, and it contains pattern recognition receptors (PRRs), antimicrobial peptides, immune cells (i.e. macrophages, dendritic cells, natural killer (NK) cells, NK–T cells), the complement system and various cytokines. Human innate immunity has surface and intracellular PRRs that recognize the microbial danger signals by recognizing pathogen-associated molecular patterns (PAMPs),10 microbial-associated molecular patterns (MAMPs)11 or danger-associated molecular patterns (DAMPs),12 after which they initiate an immune response. PAMPs are conserved structures vital to pathogens, but which cannot be mutated by the pathogen in order to escape innate immunity.13,14 They are present in microbes and absent in eukaryotes.13,14 DAMPs, on the other hand, represent damaged cells of the host (i.e. human system) which are a threat to self.12
PRRs are present in immune cells, as well as in liver parenchymal cells. The recognition of any pathogen molecules by PRRs leads to activation of the complement cascade, cytokines, antimicrobial peptides and dendritic cells, resulting in a complex interplay of pro- and anti-inflammatory responses and immunogenic and suppressive responses in the host.10 Macrophages and dendritic cells are mononuclear phagocytes derived from monocytes and are efficient antigen presenting cells involving the major histocompatibility complex-II (MHC-II) of T cells in the adaptive immune system.15 Macrophages are cells of diverse shape and location. In the liver, they are known as Kupffer cells—flattened cells present in the hepatic sinusoids.15 Adaptive immunity is dependent on innate immunity for its antigen presentation and cytokine production, as without these it will be ineffective.15 Also, monocytes are central mediators of the immune response and secrete interleukin-1 (IL-1) and tumor necrosis factor-α (TNF-α) which are responsible for recruitment of inflammatory cells.16
Liver is the major source of PRRs in the body, like C-reactive protein (CRP), lipopolysaccharide (LPS)-binding protein, peptidoglycan recognition protein and soluble CD14,17–19 and it expresses various PRRs, like Toll-like receptors (TLRs), nucleotide binding oligomerization (NOD)-like receptors and RNA helicases.2 TLRs recognize microbes on the cell surface. To date, 10 TLRs have been discovered in humans, and they harbor a common intracellular domain but a unique extracellular domain.20 Liver is the source of mRNA for all TLRs.21,22 Various parenchymal and non-parenchymal cells of liver express various TLRs.23–25 Also, immune cells of liver express various TLRs. T lymphocytes and NK cells expresses TLR 1, 2, 4, 5 and 9 and B lymphocytes expresses TLR 1, 6, 7, 9 and 10.26 Stellate cells of liver also express TLR4 and 2 as well as CD14 and respond to activation by production of proinflammatory cytokines.27–30 Kupffer cells (the liver macrophage) are scavenger cells that are exposed to gut-derived bacteria, endotoxins and various microbes and their products. Once activated, they release various cytokines, prostaglandins, nitric oxide and reactive oxygen species, making them actively involved in liver innate immunity.31 Kupffer cells and endothelium of space of Disse express TLR2 following LPS stimulation.32 TLR2 is also accumulated near the hepatocyte plasma membrane after LPS challenge. Liver is also the main source of the complement system, which is responsible for regulation of the immune system and opsonic and cytotoxic activities.
Adaptive immunity is the lymphocyte-mediated immune response against specific microbial agents and is essential for complete and effective immunity in the body. Adaptive immunity is a highly specialized immunity that provides long-lasting protection, and it is the basis for vaccination. The adaptive immunity is acquired during the lifetime of an organism and prepares the body for future challenges. It is mediated by B and T lymphocytes and its profile is specific, diverse and has a memory. The B cells are responsible for humoral immunity, and the T cells are responsible for cell-mediated immunity. Liver contains lymphocytes throughout its parenchyma and portal tracts. In the liver, CD8+ T cells are more frequent than CD4+ T cells, and memory cells are more frequent than blood cells.10
Immunological dysfunction in cirrhosis
Innate immune dysfunction
Cirrhosis affects innate immunity by impairing the synthesis and function of PRRs and various proteins, thus reducing the bactericidal capacity of that body.10 Different PRRs recognize different PAMPs. Among the PRRs, TLRs are most extensively studied and have a major influence in CAID.23,33,34 TLRs have an important role to play in the pathogenesis of various hepatic disorders, such as non-alcoholic fatty liver disease, alcoholic liver disease, viral hepatitis, autoimmune liver disease, hepatic fibrosis and liver cancer.35
Acquired alteration of TLRs and their signaling pathways are a major mechanism of innate immunity dysfunction in cirrhosis.34 This phenomenon may be due to prolonged exposure of bacteria, its products and PAMPs, as a result of the loss of barrier function related to loss of tight junctions, widening of intercellular spaces (which increases the gut translocation), presence of toxic agents (i.e. ethanol) and by their production by damaged hepatocytes.36 Gut flora can promote alcoholic liver disease by activating TLRs but this process can be reduced by altering the gut microbiota by administration of antibiotics and probiotics.37
Recent studies have shown that hepatitis B e antigen (HBeAg)-positive chronic hepatitis B (CHB) patients show down-regulation of TLR2 and that HBeAg-negative CHB patients show up-regulation of TLR2, suggesting its expression may be responsible for rapid progression of disease in the HBeAg-positive CHB patients.38 Functional impairment of TLR2 and TLR4 is one of the major reasons for immune dysfunction and risk of infection in cirrhotic patients.39 Both of these TLRs activate nuclear factor kappa β (NFKβ) in liver cells.40 Studies have shown decreased TLR2 function in early cirrhosis41,42 but decreased TLR4 function in advanced cirrhosis only.41,43–46 A study performed by Nischelke et al.47 has shown that TLR2 polymorphisms and NOD2 variants increase the susceptibility for spontaneous bacterial peritonitis (SBP) in patients with cirrhosis with ascites. Both of these defects were also found to be associated with reduced levels of NFKβ activation, which would lead to decreased activation of proinflammatory cytokines. Further studies by Bruns et al.48 have shown an increased risk of SBP in cirrhotics carrying the TLR2 R753Q polymorphism, in particular. Guarner-Argente et al. also showed that patients with the TLR4 D299G polymorphism had more infections and bacteremia.49
Impaired monocyte function is also a contributor to CAID, leading to defects in chemotaxis, phagocytosis, superoxide degeneration and production of lysosomal enzymes.50–53 Immune paralysis, which is defined as decreased human leukocyte antigen-D related (HLA-DR) expression of monocytes, is a well-known feature in ACLF and septic shock but it was recently found also in patients with liver cirrhosis.16 Immune paralysis is characterized by increase in anti-inflammatory cytokines, like IL-6 and IL-10, and suppression of proinflammatory cytokines, like IL-1 and TNF-α.17,44,45,54 Immunomodulator agents such as the granulocyte macrophage colony-stimulating factor (GM-CSF) and interferon-gamma (IFN-γ) can improve monocyte functions and should be investigated further.17 Endotoxemia, possibly through an IL-10-mediated mechanism, contributes to down-regulation of HLA-DR in cirrhotic patients.45 These low HLA-DR expressing monocytes have decreased production of proinflammatory cytokines, such as TNF-α, and nitric oxide synthetase as well as allostimulatory activity.45 Avi et al.53 has shown decreased monocyte function in liver cirrhosis as measured by phagocytosis and killing of Candida albicans and Candida pseudotropicalis. Monocytes consist of the classical CD14+CD16− types and the non-classical CD14+CD16+ types. In chronic liver disease patients, there is marked increase in non-classical CD14+CD16+ subsets, and this occurrence correlates with collagen-producing hepatic stellate cell activation, proinflammatory cytokines expression and clinical progression.55 Low lymphocyte-to-monocyte ratio has been postulated as an independent prognostic marker in liver cirrhosis.56
CD163 is a specific marker for macrophage activation and is shed into the circulation in a soluble form (sCD163).57 In cirrhosis, it increases in conjunction with increasing Child-Pugh score and shows a strong correlation with the hepatic venous pressure gradient and thus with portal hypertension.58 Waismann et al.59 has demonstrated sCD163 as an independent risk factor for death and variceal bleeding in cirrhotic patients, raising the possibility of its development as a new pharmacological target in the future. Studies have shown that peritoneal macrophages of cirrhotic patients are associated with SBP by producing nitric oxide and angiogenic peptides.60
Monocyte chemoattractant protein-1 (MCP-1) plays an important role in CAID. Its level is increased in ascites of cirrhotic patients as compared to controls, and it plays a major role in development and course of SBP. Erwin et al.60 demonstrated that in patients with alcoholic liver cirrhosis the 2518 MCP-1 genotype AA is a risk factor for development of SBP. Moreover, Muhlbauer et al.61 has shown that inheritance of the 2518 MCP-1 G allele predisposes patients infected with the hepatitis C virus to more severe hepatic inflammation and fibrosis. Finally, Tonan et al.62 reported that Kupffer cell dysfunction contributes to the pathogenesis of non-alcoholic steatohepatitis, as CD14-positive Kupffer cells increase along with increase in necroinflammation grade and fibrosis stage.
Neutrophils, which are the first-line of defense against bacterial infection, are also impaired in cirrhotics. On the one hand, this creates an impaired ability to deliver neutrophils to the infective focus, while, on other hand, this generates a reduced phagocytic activity of the neutrophils as compared to those in the healthy population. Liver is the main site of clearance of various cytokines, like IL-1, IL-3, IL-6, TNF-α, transforming growth factor-β (TGF-β), IFN-γ etc. In cirrhosis, however, liver is unable to clear the cytokines, which can lead to persistent activation of peripheral blood neutrophils63 and subsequently impair the neutrophilc functions like migration and phagocytosis.64 Also, increased endotoxin absorption and bacterial translocation (BT) leads to persistent elevation of cytokines. Removing endotoxins in vitro65 and reducing endotoxemia in vivo with probiotics46 improves polymorphonuclear leukocyte function in cirrhosis. Fiuza et al.66 demonstrated that cirrhotic patients exhibit deficient transendothelial migration and G-CSF enhances neutrophil transendothelial migration.
Recent studies have demonstrated that G-CSF therapy mobilizes CD34+ cells and improves the survival of ACLF patients.67,68 G-CSF therapy also significantly improved the rate of 2-month survival, reduced the Child-Turcotte-Pugh, model for end-stage liver disease, and sequential organ failure assessment scores, and prevented the occurrence of sepsis, hepatorenal syndrome and hepatic encephalopathy.67
Adaptive immune dysfunction
Adaptive immune dysfunction is also common in cirrhotic patients. The various defects in B and T cell functions in alcoholic liver disease have been known for a long time. Nourieta et al.69 demonstrated a broad defect of T cells and hyperactivity of B cells in patients with alcoholic liver disease. Specifically, these patients have circulating IgG and T lymphocytes that recognize epitopes against lipid peroxidation-derived antigens and are associated with an increase in hepatic production of proinflammatory cytokines and chemokines. Doi et al.70 reported that memory CD27+ B cells were reduced in the peripheral blood of patients with cirrhosis, independent of etiology, and that this reduction led to impaired TNF-β and IgG production, vaccine hyporesponsiveness and susceptibility to bacterial infection.
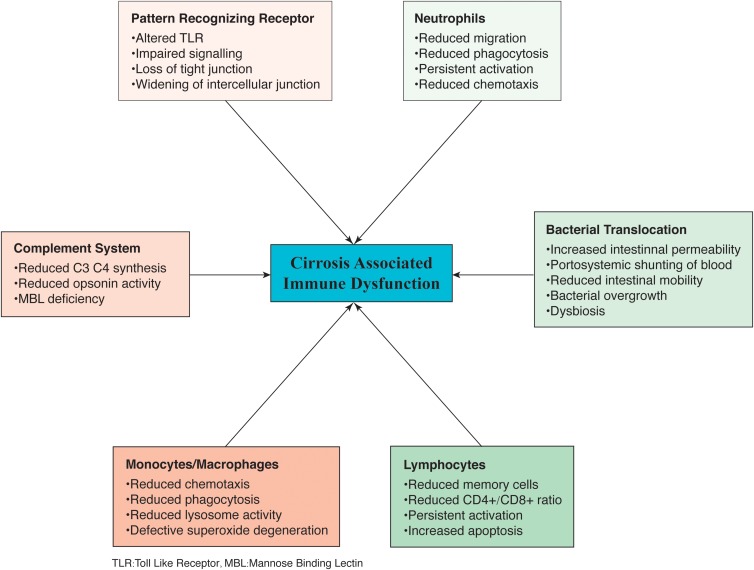
The Th1/Th2 lymphocyte ratio is important, as Th1 expresses antifibrotic cytokines and Th2 expresses profibrotic cytokines. In cirrhosis, CD8+ cells are elevated, thereby decreasing the CD4+/CD8+ cell ratio and favoring the fibrogenic process.10 A study performed by Marquez et al.71 showed intense derangement of monocytes and T cells of the immune system in patients with liver cirrhosis. Importantly, there is prolonged activation of T lymphocytes as a result of the prolonged antigenic stimulus in cirrhosis. Activated CD4+ and CD8+ lymphocytes show increase in apoptosis markers and activation-induced cell death (AICD), presumably made in order to maintain lymphocyte homeostasis. Compared with healthy controls, cirrhotic patients show higher expression of the apoptosis marker CD95+ in their memory cell population.10 These T cells are unable to proliferate after new antigenic load, which leads to immunosuppression secondary to exhaustion of the adaptive immune response. The various mechanisms of immune dysfunction described herein for cirrhosis are presented in Fig. 1.
Fig. 1. Mechanisms of immune dysfunction in cirrhosis.
It is long known that serum IgA level is enhanced in alcoholic liver disease, but the exact mechanism causing it remains to be fully elucidated.72 Silvain et al.73 demonstrated that altered Fc alpha R expression in monocytes leads to receptor saturation and increases the absolute level of IgA and IgA immune complex, due to defective clearance in alcoholic cirrhosis. Massonnet et al.74 demonstrated that enhanced IgA production by CpG led to activation of B cells in alcoholic liver cirrhosis, compared to the mechanism observed in healthy donors, and this was due to the intrinsic ability of these cells to produce more IgA.
Complement system and cirrhosis
The complement system plays an important role in both innate and adaptive immunity, and protects the body from microbial infections. Hepatocytes are the major source of synthesis of complement factors. Low opsonin activity and reduced C3 complement level increases susceptibility to infection in cirrhotic patients.75,76 Reduced C3 and C4 complement levels are observed in cirrhotics, and this phenomenon is due to decreased synthesis as a result of liver dysfunction and increased consumption of the factors due to persistent complement activation.
Hillebrand et al.77 has demonstrated a critical role of C5 and C5aR in the pathogenesis of liver fibrosis. Immunocytochemistry studies have shown that expression of C5aR1 significantly increased on hepatic stellate cells during transformation to myofibroblast. Also, Strey et al.78 has found C3a and C5a to be essential for liver regeneration. In C3 and C5 knock-out mice, liver regeneration was severely impaired and was restored after reconstitution with the factors.78 Increased susceptibility of Pneumococcus pneumonia in cirrhosis has also been demonstrated due to insufficient deposition of complement C3 on the surface of lungs.79 Altotjay et al.80 has found mannose-binding lectin (MBL) deficiency to be associated with higher infection rate in liver cirrhosis. Moreover, significant reduction in MBL levels were observed in advanced cirrhosis, and levels <100 ng/mL were associated with more bacterial infection in cirrhosis.80
Bacterial translocation
BT is migration of bacteria or their products (i.e. lipopolysaccharides, peptioglycans, muramyl dipeptides, bacterial DNA) from intestinal lumen to mesenteric lymph nodes (MLNs).81 BT is increased in cirrhotics.5,6 It has also been associated with the occurrence of SBP.5,6 Pathological BT has been characterized as the ‘Achilles heel’ of cirrhosis.
Factors leading to increased BT in cirrhotics are impaired humoral and cellular immunity,82 portosystemic shunting of blood,83 decrease intestinal mobility,82 increased intestinal permeability84 and bacterial overgrowth.85 Studies have shown that after administration of radiolabeled Escherichia coli to cirrhotic rats, the bacteria are found not only in the gut lumen but also in the MLNs and ascites.86 Also, same bacterial species have been grown in ascites and MLNs from rats with cirrhosis.87
Due to portosystemic shunting, there is reduced liver clearance of gut-derived bacteria and their products from the portal circulation. There is also reduced intestinal mobility in cirrhosis due to prolonged orocecal time, which is mainly due to increased pylorocecal transit time.88 Chang et al.89 have shown that cirrhotics with a history of SBP have more severe small intestinal motility dysfunction. Motor abnormalities have been observed in the small intestine, including changes in contraction pattern and increase in mean duration of the migratory motor complex.90
TLR248 and NOD-291 mutations have been linked with BT and SBP in cirrhosis. NOD-2 protein recognizes bacterial products and stimulates an immune reaction to limit the entry of bacteria across the gut by activation of NFKβ signaling.91 NOD-2 gene polymorphism has been described an important genetic risk factor for BT and SBP and also for reduced survival in western populations.91 Permeability of the intestinal wall is increased in cirrhosis and is one of the contributory factors for the development of SBP and hepatic encephalopathy. Permeability of the gut wall may be affected by edema of splanchnic tissue, due to congestion of the venous and lymphatic systems.92
Keshavarzian et al.93 has shown that chronic liver injury in heavy drinkers is associated with leaky gut, as evidenced by increased urinary sucrose excretion after oral administration. A similar result has been reported by Toh et al.94 after oral phenolsufonphthalein absorption test in patients with liver cirrhosis. Campillo et al.95 has shown that impairment of the intestinal function barrier is related to severe septic complications in cirrhosis. Paramo et al.96 studied the role of propranolol in cirrhotic rats with ascites and found that it increases intestinal motility and decreases the bacterial overgrowth and translocation; thus, it may serve to prevent SBP in cirrhosis. Finally, a meta-analysis performed by Senzolo et al.97 has also concluded that beta-blockers have a role in preventing SBP in cirrhosis; although, randomized controlled trials in humans are still needed to confirm this finding.
Gut microbiota in cirrhosis
The gut and liver are in constant touch with each other, through the portal vein. The fecal microbiota in cirrhosis differs from that of the healthy population. In cirrhosis, there is change in the bacteroides/fermicutes ratio and more prevalence of pathogenic microbes like the Enterobacteriaceae and Streptococcaceae, as well as less prevalence of beneficial microbes like the Lachnospiraceae, and it may affect the prognosis.98 The change in the microbiota in cirrhosis disturbs the intestinal immune homeostasis, favors BT and impairs the host defense against them, and contributes to the development of hepatic encephalopathy (HE), SBP and variceal bleeding.99 These disturbances in gut microbiota lead to various bacterial complications in cirrhosis. Though antibiotics are the main therapeutic strategy, experimental studies are ongoing to investigate the use of pre-, pro-, symbiotic and fecal microbiota transplantation in patients with decompensated cirrhosis.99 Reshaping the microbiota in a beneficial manner may help to prevent complications of cirrhosis in the future.
Bacterial infections in cirrhosis
There have been drastic improvements in the management and prognosis of cirrhotic patients in the last few decades, but the rate of mortality due to infectious complications has not changed much. Bacterial infections are common in cirrhotics and are responsible for death in 30–50% of these patients.3 The most susceptible subset are those with alcoholic cirrhosis.82 Gram-negative enteric bacteria like E. coli, Klebsiella, Enterobacter species etc. are the most common causes and responsible for 75% of cases. Gram-positive bacteria like Staphyloccocus is responsible for around 20%, and anaerobes for around 3% of cases.100 Infection rates in hospitalized patients with cirrhosis are 4- to 5-fold higher than those among the general patient population.101 The most common infections that occur in these patients are represented by SBP (25–31%).100 Other common infections are urinary tract infections (20–25%), pneumonia (15–21%), bacteremia (12%) and soft tissue infections (11%).100
For SBP, intravenous antibiotics for 5 days, intravenous albumin (to reduce the incidence of renal impairment) and long-term oral antibiotic prophylaxis (to prevent further episodes of SBP) is the standard of care. Multidrug-resistant organisms are also a concern now. In one of the large prospective trials, carried out by Fernandez et al.,101 multidrug-resistant bacteria (18%) represented 4%, 14% and 35% of the community-acquired, healthcare-associated and nosocomial infections, respectively. Extended spectrum beta lactamase was the most common multidrug-resistant organism, followed by Pseudomonas aeruginosa, and methicillin-resistant Staphylococcus aureus and Enterococcus faecium. Septic shock and mortality is high in multidrug-resistant infection patients, and it is currently recommended that empirical antibiotic prophylaxis is not effective for nosocomial infections.
Tuberculosis
The incidence of tuberculosis is increased in cirrhotic patients as compared to the general population, due to the immune dysfunction in the former. In a cohort study carried out in Denmark, the incidence rate of tuberculosis was 168.6 per 1 lakh population and was highest in men over 65 years of age.102 Another study carried out in western India showed the prevalence to be 15 times higher than in the general population; moreover, the authors showed extrapulmonary involvement (e.g. tubercular peritonitis) to be more frequent than in the general population.103
Fungal infections
Cirrhosis also increases the susceptibility to infection with the Cryptococcus neoformans fungus, which usually affects patients with acquired immune deficiency syndrome.104 It causes spontaneous peritonitis but with an elevation in lymphocyte count, and is associated with very high mortality due to late diagnosis.105 The probable pathogenetic mechanisms include percutaneous inoculation during paracentesis, gastrointestinal bleeding and BT.106
Iron overload status and immunity
End-stage cirrhosis can be associated with hepatic iron overload. Excess iron impairs the host immune system. It specifically impairs the cell-mediated immunity by impairing the Th1 response and also the functions of macrophages and neutrophils.107 Furthermore, it increases the CD8+ T cell count and reduces the CD4+ T cell count and response to common antigens. Ultimately, it increases susceptibility to organisms like E. coli, Vibrio and Listeria monocytogenes.107 Ashraflen et al.108 have shown that hepcidin is a link between liver disease and infections in hemochromatosis. Also, these patients are at increased risk of acquiring Vibrio vulnificus, with mortality of 50–60% being reported.109 Non-HFE iron overload has been shown to significantly associate with disease severity and reduced survival in patients with decompensated cirrhosis.110
Systemic inflammatory response syndrome (SIRS), sepsis and cirrhosis
Sepsis is defined as SIRS in the presence of a pathogenic infection or other injury (such as a crush injury) that can trigger the inflammatory immune response. Conventional SIRS criteria has a low sensitivity and specificity in cirrhotic patients, as it can be present in 10–30% without bacterial infections; moreover, these patients present low pulse rate and leucocyte count due to beta blocker therapy and hypersplenism, respectively, which can lead to underestimation of its prevalence.111 In SIRS, there is a cytokine storm with predominance of proinflammatory cytokines like TNF-α, IL-6 and IL-1, which leads to various changes in the coagulation cascade and circulatory system.
Cirrhotic patients are at increased risk for developing SIRS, as they have increased levels of endotoxins, TNF-α, IL-6 and nitric oxide and reduced levels of protein C and coagulation factors.8 SIRS is the cause of around 10% of hospital admissions among this patient population. In addition, SIRS occurs in patients with advanced cirrhosis and is correlated with death and portal hypertension-related complications such as HE, variceal bleeding and renal failure. Bacterial-derived toxins (i.e. lipopolysaccharides from Gram-negative bacteria and peptidoglycans/lipopeptides from Gram-positive bacteria initiate a cascade of events that lead to a surge of proinflammatory cytokines which are not balanced by anti-inflammatory cytokines, leading to a state of excessive inflammation.
There is also increased production of superoxide from nitric oxide synthase during SIRS, leading to oxidative stress and increased vasodilatation.112 This leads to widespread inflammation and consequently to impaired oxygenation, cell necrosis, apoptosis and finally organ failure and death. It has been shown that cirrhotic patients develop a higher level of proinflammatory cytokines following a lipopolysaccharide challenge as compared to the healthy population.107,108 Prophylactic antibiotics in variceal bleeding, albumin in SBP and early diagnosis and treatment of bacterial infection are needed to improve outcome for sepsis and SIRS in cirrhosis.
The roles of biomarkers, CRP and procalcitonin have been studied in cirrhotic patients and found to be beneficial for detecting sepsis. Procalcitonin is an emerging biomarker of bacterial infection in these patients, and randomized controlled trials have found benefit in its use for detecting infection in these patients.113 Li et al.114 studied the role of procalcitonin involving bacterial infection in cirrhotics and has found its sensitivity and specificity to be 81.5% and 87.3%, respectively. Procalcitonin appears to be a better diagnostic marker than SIRS for detecting bacterial infection in the cirrhotic population. Elevated levels of procalcitonin and CRP have been shown to correlate with the outcome of sepsis in cirrhotics.111 CRP levels remain persistently elevated in the majority of patients, despite resolution of the bacterial infections.111 The role of newer markers of acute phase reactants, such as lipopolysaccharide-binding proteins, sCD14, mid-region proadrenomedullin etc., still need to be studied in the cirrhotic population.
ACLF is a distinctive entity involving both acute and chronic insults to the liver and has a high short-term mortality. Host immune dysregulation is probably the leading factor in determining the severity of ACLF and its outcome.10 Host immune dysregulation is usually precipitated by bacterial infection, superimposed with other hepatotropic viruses, alcohol or drugs. In ACLF there is an imbalance between the exaggerated pro- and anti-inflammatory responses (i.e. between the systemic inflammatory response and the compensatory anti-inflammatory response). Prolonged immune paralysis predisposes an individual to sepsis, which increases the pro-inflammatory responses and results in a vicious cycle.115
To conclude, CAID is a complex phenomenon involving multiple mechanisms and leading to various complications. Gradually, researchers have been able to explore the underlying pathophysiology behind it by understanding the exact defect in each immune cell type and in systemic immunity. Cirrhosis is an immunocompromised state accompanied by a higher predisposition to various infections, most common of which are the Gram-negative bacteria. Increased BT due to reduced intestinal motility and increased intestinal permeability is an important etiological factor for CAID.
Knowing the various defects in host immune system afflicted by CAID is of utmost importance for our attempts towards gaining a precise understanding and developing new diagnostic and therapeutic tools that will reduce the morbidity and mortality. There remain an unmet need for making a scoring system that includes the various clinical and biochemical markers and/or a specific biomarker which can identify that subset of cirrhotic patients which is most at risk of immune dysfunction and infection at an early stage. Despite there being an overall better understanding of various mechanisms of immune dysfunction in recent years, further research is needed to develop an effective preventive strategy to prevent its complications.
Abbreviations
- ACLF
acute on chronic liver failure
- AICD
activation-induced cell death
- BT
bacterial translocation
- CAID
cirrhosis-associated immune dysfunction
- CHB
chronic hepatitis B
- CRP
c-reactive protein
- DAMP
danger-associated molecular pattern
- GM-CSF
granulocyte macrophage colony-stimulating factor
- HBeAg
hepatitis B e antigen
- HE
hepatic encephalopathy
- HLA-DR
human leukocyte antigen-D related
- IFN
interferon
- IL
interleukin
- LPS
lipopolysaccharide
- MAMP
microbial-associated molecular pattern
- MBL
mannose-binding lectin
- MCP
monocyte chemoattractant protein
- MHC
major histocompatibility complex
- MLN
mesenteric lymphadenopathy
- NFKβ
nuclear factor kappa β
- NK
natural killer
- NOD
nucleotide binding oligomerization
- PAMP
pathogen-associated molecular pattern
- PRR
pattern recognition receptor
- SBP
spontaneous bacterial peritonitis
- SIRS
systemic inflammatory response syndrome
- TGF
transforming growth factor
- TLR
toll-like receptors
- TNF
tumor necrosis factor
References
- 1.Christou L, Pappas G, Falagas ME. Bacterial infection-related morbidity and mortality in cirrhosis. Am J Gastroenterol. 2007;102:1510–1517. doi: 10.1111/j.1572-0241.2007.01286.x. doi: 10.1111/j.1572-0241.2007.01286.x. [DOI] [PubMed] [Google Scholar]
- 2.Albillos A, Lario M, Álvarez-Mon M. Cirrhosis-associated immune dysfunction: distinctive features and clinical relevance. J Hepatol. 2014;61:1385–1396. doi: 10.1016/j.jhep.2014.08.010. doi: 10.1016/j.jhep.2014.08.010. [DOI] [PubMed] [Google Scholar]
- 3.Tandon P, Garcia-Tsao G. Bacterial infections, sepsis, and multiorgan failure in cirrhosis. Semin Liver Dis. 2008;28:26–42. doi: 10.1055/s-2008-1040319. doi: 10.1055/s-2008-1040319. [DOI] [PubMed] [Google Scholar]
- 4.Wiest R, Lawson M, Geuking M. Pathological bacterial translocation in liver cirrhosis. J Hepatol. 2014;60:197–209. doi: 10.1016/j.jhep.2013.07.044. doi: 10.1016/j.jhep.2013.07.044. [DOI] [PubMed] [Google Scholar]
- 5.Runyon BA, Squier S, Borzio M. Translocation of gut bacteria in rats with cirrhosis to mesenteric lymph nodes partially explains the pathogenesis of spontaneous bacterial peritonitis. J Hepatol. 1994;21:792–796. doi: 10.1016/s0168-8278(94)80241-6. doi: doi.org/10.1016/S0168-8278(94)80241-6. [DOI] [PubMed] [Google Scholar]
- 6.Garcia-Tsao G, Wiest R. Gut microflora in the pathogenesis of the complications of cirrhosis. Best Pract Res Clin Gastroenterol. 2004;18:353–372. doi: 10.1016/j.bpg.2003.10.005. doi: 10.1016/j.bpg.2003.10.005. [DOI] [PubMed] [Google Scholar]
- 7.Thalheimer U, Triantos CK, Samonakis DN, Patch D, Burroughs AK. Infection, coagulation, and variceal bleeding in cirrhosis. Gut. 2005;54:556–563. doi: 10.1136/gut.2004.048181. doi: 10.1136/gut.2004.048181. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Bonnel AR, Bunchorntavakul C, Reddy KR. Immune dysfunction and infections in patients with cirrhosis. Clin Gastroenterol Hepatol. 2011;9:727–738. doi: 10.1016/j.cgh.2011.02.031. doi: 10.1016/j.cgh.2011.02.031. [DOI] [PubMed] [Google Scholar]
- 9.Duddempudi AT. Immunology in alcoholic liver disease. Clin Liver Dis. 2012;16:687–698. doi: 10.1016/j.cld.2012.08.003. doi: 10.1016/j.cld.2012.08.003. [DOI] [PubMed] [Google Scholar]
- 10.Sipeki N, Antal-Szalmas P, Lakatos PL, Papp M. Immune dysfunction in cirrhosis. World J Gastroenterol. 2014;20:2564–2577. doi: 10.3748/wjg.v20.i10.2564. doi: 10.3748/wjg.v20.i10.2564. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Neish AS. Microbes in gastrointestinal health and disease. Gastroenterology. 2009;136:65–80. doi: 10.1053/j.gastro.2008.10.080. doi: 10.1053/j.gastro.2008.10.080. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Newton K, Dixit VM. Signaling in innate immunity and inflammation. Cold Spring Harb Perspect Biol. 2012;4:pii: a006049. doi: 10.1101/cshperspect.a006049. doi: 10.1101/cshperspect.a006049. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Kawai T, Akira S. Innate immune recognition of viral infection. Nat Immunol. 2006;7:131–137. doi: 10.1038/ni1303. doi: 10.1038/ni1303. [DOI] [PubMed] [Google Scholar]
- 14.Wagner H, Bauer S. All is not Toll: new pathways in DNA recognition. J Exp Med. 2006;203:265–268. doi: 10.1084/jem.20052191. doi: 10.1084/jem.20052191. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Beutler B. Innate immunity: an overview. Mol Immunol. 2004;40:845–859. doi: 10.1016/j.molimm.2003.10.005. [DOI] [PubMed] [Google Scholar]
- 16.Antoniades CG, Wendon J, Vergani D. Paralysed monocytes in acute on chronic liver disease. J Hepatol. 2005;42:163–165. doi: 10.1016/j.jhep.2004.12.005. doi: 10.1016/j.jhep.2004.12.005. [DOI] [PubMed] [Google Scholar]
- 17.Gao B, Jeong WI, Tian Z. Liver: An organ with predominant innate immunity. Hepatology. 2008;47:729–736. doi: 10.1002/hep.22034. doi: 10.1002/hep.22034. [DOI] [PubMed] [Google Scholar]
- 18.Ramadori G, Christ B. Cytokines and the hepatic acute-phase response. Semin Liver Dis. 1999;19:141–155. doi: 10.1055/s-2007-1007106. doi: 10.1055/s-2007-1007106. [DOI] [PubMed] [Google Scholar]
- 19.Liu C, Xu Z, Gupta D, Dziarski R. Peptidoglycan recognition proteins: a novel family of four human innate immunity pattern recognition molecules. J Biol Chem. 2001;276:34686–34694. doi: 10.1074/jbc.M105566200. doi: 10.1074/jbc.M105566200. [DOI] [PubMed] [Google Scholar]
- 20.Bell JK, Mullen GE, Leifer CA, Mazzoni A, Davies DR, Segal DM. Leucine-rich repeats and pathogen recognition in Toll-like receptors. Trends Immunol. 2003;24:528–533. doi: 10.1016/s1471-4906(03)00242-4. [DOI] [PubMed] [Google Scholar]
- 21.Liu S, Gallo DJ, Green AM, Williams DL, Gong X, Shapiro RA, et al. Role of toll-like receptors in changes in gene expression and NF-kappa B activation in mouse hepatocytes stimulated with lipopolysaccharide. Infect Immun. 2002;70:3433–3442. doi: 10.1128/IAI.70.7.3433-3442.2002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Nishimura M, Naito S. Tissue-specific mRNA expression profiles of human toll-like receptors and related genes. Biol Pharm Bull. 2005;28:886–892. doi: 10.1248/bpb.28.886. [DOI] [PubMed] [Google Scholar]
- 23.Yang L, Seki E. Toll-like receptors in liver fibrosis: cellular crosstalk and mechanisms. Front Physiol. 2012;3:138. doi: 10.3389/fphys.2012.00138. doi: 10.3389/fphys.2012.00138. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Seki E, Brenner DA. Toll-like receptors and adaptor molecules in liver disease: update. Hepatology. 2008;48:322–335. doi: 10.1002/hep.22306. doi: 10.1002/hep.22306. [DOI] [PubMed] [Google Scholar]
- 25.Roh YS, Seki E. Toll-like receptors in alcoholic liver disease, non-alcoholic steatohepatitis and carcinogenesis. J Gastroenterol Hepatol. 2013;28(Suppl 1):38–42. doi: 10.1111/jgh.12019. doi: 10.1111/jgh.12019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Hornung V, Rothenfusser S, Britsch S, Krug A, Jahrsdörfer B, Giese T, et al. Quantitative expression of toll-like receptor 1-10 mRNA in cellular subsets of human peripheral blood mononuclear cells and sensitivity to CpG oligodeoxynucleotides. J Immunol. 2002;168:4531–4537. doi: 10.4049/jimmunol.168.9.4531. [DOI] [PubMed] [Google Scholar]
- 27.Paik YH, Schwabe RF, Bataller R, Russo MP, Jobin C, Brenner DA. Toll-like receptor 4 mediates inflammatory signaling by bacterial lipopolysaccharide in human hepatic stellate cells. Hepatology. 2003;37:1043–1055. doi: 10.1053/jhep.2003.50182. doi: 10.1053/jhep.2003.50182. [DOI] [PubMed] [Google Scholar]
- 28.Brun P, Castagliuolo I, Pinzani M, Palù G, Martines D. Exposure to bacterial cell wall products triggers an inflammatory phenotype in hepatic stellate cells. Am J Physiol Gastrointest Liver Physiol. 2005;289:G571–G578. doi: 10.1152/ajpgi.00537.2004. doi: 10.1152/ajpgi.00537.2004. [DOI] [PubMed] [Google Scholar]
- 29.Thirunavukkarasu C, Uemura T, Wang LF, Watkins SC, Gandhi CR. Normal rat hepatic stellate cells respond to endotoxin in LBP-independent manner to produce inhibitor(s) of DNA synthesis in hepatocytes. J Cell Physiol. 2005;204:654–665. doi: 10.1002/jcp.20366. doi: 10.1002/jcp.20366. [DOI] [PubMed] [Google Scholar]
- 30.Zhang X, Yu WP, Gao L, Wei KB, Ju JL, Xu JZ. Effects of lipopolysaccharides stimulated Kupffer cells on activation of rat hepatic stellate cells. World J Gastroenterol. 2004;10:610–613. doi: 10.3748/wjg.v10.i4.610. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Bilzer M, Roggel F, Gerbes AL. Role of Kupffer cells in host defense and liver disease. Liver Int. 2006;26:1175–1186. doi: 10.1111/j.1478-3231.2006.01342.x. doi: 10.1111/j.1478-3231.2006.01342.x. [DOI] [PubMed] [Google Scholar]
- 32.Vodovotz Y, Liu S, McCloskey C, Shapiro R, Green A, Billiar TR. The hepatocyte as a microbial product-responsive cell. J Endotoxin Res. 2001;7:365–373. [PubMed] [Google Scholar]
- 33.Broering R, Lu M, Schlaak JF. Role of Toll-like receptors in liver health and disease. Clin Sci (Lond) 2011;121:415–426. doi: 10.1042/CS20110065. doi: 10.1042/CS20110065. [DOI] [PubMed] [Google Scholar]
- 34.Aoyama T, Paik YH, Seki E. Toll-like receptor signaling and liver fibrosis. Gastroenterol Res Pract. 2010;2010:pii: 192543. doi: 10.1155/2010/192543. doi: 10.1155/2010/192543. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Szabo G, Dolganiuc A, Mandrekar P. Pattern recognition receptors: a contemporary view on liver diseases. Hepatology. 2006;44:287–298. doi: 10.1002/hep.21308. doi: 10.1002/hep.21308. [DOI] [PubMed] [Google Scholar]
- 36.Li L, Chen L, Hu L, Liu Y, Sun HY, Tang J, et al. Nuclear factor high-mobility group box1 mediating the activation of Toll-like receptor 4 signaling in hepatocytes in the early stage of nonalcoholic fatty liver disease in mice. Hepatology. 2011;54:1620–1630. doi: 10.1002/hep.24552. doi: 10.1002/hep.24552. [DOI] [PubMed] [Google Scholar]
- 37.Llorente C, Schnabl B. The gut microbiota and liver disease. Cell Mol Gastroenterol Hepatol. 2015;1:275–284. doi: 10.1016/j.jcmgh.2015.04.003. doi: 10.1016/j.jcmgh.2015.04.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Thompson AJ, Locarnini SA, Lau GK, Naoumov NV, Desmond PV, Mommeja-Marin H, et al. Quantitative HBeAg levels and patterns of TLR2 and TLR4 expression on CD14+ monocytes during potent antiviral therapy for chronic hepatitis B. J Gastroenterol Hepatol. 2005;20:A83. [Google Scholar]
- 39.Pimentel-Nunes P, Roncon-Albuquerque R, Jr, Dinis-Ribeiro M, Leite-Moreira AF. Role of Toll-like receptor impairment in cirrhosis infection risk: are we making progress? Liver Int. 2011;31:140–141. doi: 10.1111/j.1478-3231.2010.02334.x. doi: 10.1111/j.1478-3231.2010.02334.x. [DOI] [PubMed] [Google Scholar]
- 40.Matsumura T, Degawa T, Takii T, Hayashi H, Okamoto T, Inoue J, et al. TRAF6-NF-kappaB pathway is essential for interleukin-1-induced TLR2 expression and its functional response to TLR2 ligand in murine hepatocytes. Immunology. 2003;109:127–136. doi: 10.1046/j.1365-2567.2003.01627.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Pimentel-Nunes P, Roncon-Albuquerque R, Jr, Gonçalves N, Fernandes-Cerqueira C, Cardoso H, Bastos RP, et al. Attenuation of toll-like receptor 2-mediated innate immune response in patients with alcoholic chronic liver disease. Liver Int. 2010;30:1003–1011. doi: 10.1111/j.1478-3231.2010.02251.x. doi: 10.1111/j.1478-3231.2010.02251.x. [DOI] [PubMed] [Google Scholar]
- 42.Riordan SM, Skinner N, Nagree A, McCallum H, McIver CJ, Kurtovic J, et al. Peripheral blood mononuclear cell expression of toll-like receptors and relation to cytokine levels in cirrhosis. Hepatology. 2003;37:1154–1164. doi: 10.1053/jhep.2003.50180. doi: 10.1053/jhep.2003.50180. [DOI] [PubMed] [Google Scholar]
- 43.Testro AG, Gow PJ, Angus PW, Wongseelashote S, Skinner N, Markovska V, et al. Effects of antibiotics on expression and function of Toll-like receptors 2 and 4 on mononuclear cells in patients with advanced cirrhosis. J Hepatol. 2010;52:199–205. doi: 10.1016/j.jhep.2009.11.006. doi: 10.1016/j.jhep.2009.11.006. [DOI] [PubMed] [Google Scholar]
- 44.Wasmuth HE, Kunz D, Yagmur E, Timmer-Stranghöner A, Vidacek D, Siewert E, et al. Patients with acute on chronic liver failure display “sepsis-like” immune paralysis. J Hepatol. 2005;42:195–201. doi: 10.1016/j.jhep.2004.10.019. doi: 10.1016/j.jhep.2004.10.019. [DOI] [PubMed] [Google Scholar]
- 45.Lin CY, Tsai IF, Ho YP, Huang CT, Lin YC, Lin CJ, et al. Endotoxemia contributes to the immune paralysis in patients with cirrhosis. J Hepatol. 2007;46:816–826. doi: 10.1016/j.jhep.2006.12.018. doi: 10.1016/j.jhep.2006.12.018. [DOI] [PubMed] [Google Scholar]
- 46.Stadlbauer V, Mookerjee RP, Hodges S, Wright GA, Davies NA, Jalan R. Effect of probiotic treatment on deranged neutrophil function and cytokine responses in patients with compensated alcoholic cirrhosis. J Hepatol. 2008;48:945–951. doi: 10.1016/j.jhep.2008.02.015. doi: 10.1016/j.jhep.2008.02.015. [DOI] [PubMed] [Google Scholar]
- 47.Nischalke HD, Berger C, Aldenhoff K, Thyssen L, Gentemann M, Grünhage F, et al. Toll-like receptor (TLR) 2 promoter and intron 2 polymorphisms are associated with increased risk for spontaneous bacterial peritonitis in liver cirrhosis. J Hepatol. 2011;55:1010–1016. doi: 10.1016/j.jhep.2011.02.022. doi: 10.1016/j.jhep.2011.02.022. [DOI] [PubMed] [Google Scholar]
- 48.Bruns T, Reuken PA, Fischer J, Berg T, Stallmach A. Further evidence for the relevance of TLR2 gene variants in spontaneous bacterial peritonitis. J Hepatol. 2012;56:1207–1208. doi: 10.1016/j.jhep.2011.09.010. author reply 1208-1209. doi: 10.1016/j.jhep.2011.09.010. [DOI] [PubMed] [Google Scholar]
- 49.Guarner-Argente C, Sánchez E, Vidal S, Román E, Concepción M, Poca M, et al. Toll-like receptor 4 D299G polymorphism and the incidence of infections in cirrhotic patients. Aliment Pharmacol Ther. 2010;31:1192–1199. doi: 10.1111/j.1365-2036.2010.04291.x. doi: 10.1111/j.1365-2036.2010.04291.x. [DOI] [PubMed] [Google Scholar]
- 50.Nakagawara A, Inokuchi K, Ikeda K, Kumashiro R, Tamada R. Decreased superoxide (O2-)-generating activity of blood monocytes from patients with hepatic cirrhosis. Hepatogastroenterology. 1984;31:201–203. [PubMed] [Google Scholar]
- 51.Hassner A, Kletter Y, Jedvab M, Aronson M, Shibolet S. Impaired monocyte function in liver cirrhosis. Lancet. 1979;1:329–330. doi: 10.1016/s0140-6736(79)90745-1. [DOI] [PubMed] [Google Scholar]
- 52.Hassner A, Kletter Y, Shlag D, Yedvab M, Aronson M, Shibolet S. Impaired monocyte function in liver cirrhosis. Br Med J (Clin Res Ed) 1981;282:1262–1263. doi: 10.1136/bmj.282.6272.1262. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Holdstock G, Leslie B, Hill S, Tanner A, Wright R. Monocyte function in cirrhosis. J Clin Pathol. 1982;35:972–979. doi: 10.1136/jcp.35.9.972. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Xing T, Li L, Cao H, Huang J. Altered immune function of monocytes in different stages of patients with acute on chronic liver failure. Clin Exp Immunol. 2007;147:184–188. doi: 10.1111/j.1365-2249.2006.03259.x. doi: 10.1111/j.1365-2249.2006.03259.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Zimmermann HW, Seidler S, Nattermann J, Gassler N, Hellerbrand C, Zernecke A, et al. Functional contribution of elevated circulating and hepatic non-classical CD14CD16 monocytes to inflammation and human liver fibrosis. PLoS One. 2010;5:e11049. doi: 10.1371/journal.pone.0011049. doi: 10.1371/journal.pone.0011049. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Zhang J, Feng G, Zhao Y, Zhang J, Feng L, Yang J. Association between lymphocyte-to-monocyte ratio (LMR) and the mortality of HBV-related liver cirrhosis: a retrospective cohort study. BMJ Open. 2015;5:e008033. doi: 10.1136/bmjopen-2015-008033. doi: 10.1136/bmjopen-2015-008033. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Møller HJ. Soluble CD163. Scand J Clin Lab Invest. 2012;72:1–13. doi: 10.3109/00365513.2011.626868. doi: 10.3109/00365513.2011.626868. [DOI] [PubMed] [Google Scholar]
- 58.Grønbaek H, Sandahl TD, Mortensen C, Vilstrup H, Møller HJ, Møller S. Soluble CD163, a marker of Kupffer cell activation, is related to portal hypertension in patients with liver cirrhosis. Aliment Pharmacol Ther. 2012;36:173–180. doi: 10.1111/j.1365-2036.2012.05134.x. doi: 10.1111/j.1365-2036.2012.05134.x. [DOI] [PubMed] [Google Scholar]
- 59.Waidmann O, Brunner F, Herrmann E, Zeuzem S, Piiper A, Kronenberger B. Macrophage activation is a prognostic parameter for variceal bleeding and overall survival in patients with liver cirrhosis. J Hepatol. 2013;58:956–961. doi: 10.1016/j.jhep.2013.01.005. doi: 10.1016/j.jhep.2013.01.005. [DOI] [PubMed] [Google Scholar]
- 60.Gäbele E, Mühlbauer M, Paulo H, Johann M, Meltzer C, Leidl F, et al. Analysis of monocyte chemotactic protein-1 gene polymorphism in patients with spontaneous bacterial peritonitis. World J Gastroenterol. 2009;15:5558–5562. doi: 10.3748/wjg.15.5558. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Mühlbauer M, Bosserhoff AK, Hartmann A, Thasler WE, Weiss TS, Herfarth H, et al. A novel MCP-1 gene polymorphism is associated with hepatic MCP-1 expression and severity of HCV-related liver disease. Gastroenterology. 2003;125:1085–1093. doi: 10.1016/s0016-5085(03)01213-7. [DOI] [PubMed] [Google Scholar]
- 62.Tonan T, Fujimoto K, Qayyum A, Morita Y, Nakashima O, Ono N, et al. CD14 expression and Kupffer cell dysfunction in non-alcoholic steatohepatitis: superparamagnetic iron oxide-magnetic resonance image and pathologic correlation. J Gastroenterol Hepatol. 2012;27:789–796. doi: 10.1111/j.1440-1746.2011.07057.x. doi: 10.1111/j.1440-1746.2011.07057.x. [DOI] [PubMed] [Google Scholar]
- 63.Stadlbauer V, Mookerjee RP, Wright GA, Davies NA, Jürgens G, Hallström S, et al. Role of Toll-like receptors 2, 4, and 9 in mediating neutrophil dysfunction in alcoholic hepatitis. Am J Physiol Gastrointest Liver Physiol. 2009;296:G15–G22. doi: 10.1152/ajpgi.90512.2008. doi: 10.1152/ajpgi.90512.2008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Fiuza C, Salcedo M, Clemente G, Tellado JM. In vivo neutrophil dysfunction in cirrhotic patients with advanced liver disease. J Infect Dis. 2000;182:526–533. doi: 10.1086/315742. doi: 10.1086/315742. [DOI] [PubMed] [Google Scholar]
- 65.Mookerjee RP, Stadlbauer V, Lidder S, Wright GA, Hodges SJ, Davies NA, et al. Neutrophil dysfunction in alcoholic hepatitis superimposed on cirrhosis is reversible and predicts the outcome. Hepatology. 2007;46:831–840. doi: 10.1002/hep.21737. doi: 10.1002/hep.21737. [DOI] [PubMed] [Google Scholar]
- 66.Fiuza C, Salcedo M, Clemente G, Tellado JM. Granulocyte colony-stimulating factor improves deficient in vitro neutrophil transendothelial migration in patients with advanced liver disease. Clin Diagn Lab Immunol. 2002;9:433–439. doi: 10.1128/CDLI.9.2.433-439.2002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Garg V, Garg H, Khan A, Trehanpati N, Kumar A, Sharma BC, et al. Granulocyte colony-stimulating factor mobilizes CD34(+) cells and improves survival of patients with acute-on-chronic liver failure. Gastroenterology. 2012;142:505–512.e1. doi: 10.1053/j.gastro.2011.11.027. doi: 10.1053/j.gastro.2011.11.027. [DOI] [PubMed] [Google Scholar]
- 68.Singh V, Sharma AK, Narasimhan RL, Bhalla A, Sharma N, Sharma R. Granulocyte colony-stimulating factor in severe alcoholic hepatitis: a randomized pilot study. Am J Gastroenterol. 2014;109:1417–1423. doi: 10.1038/ajg.2014.154. doi: 10.1038/ajg.2014.154. [DOI] [PubMed] [Google Scholar]
- 69.Nouri-Aria KT, Alexander GJ, Portmann BC, Hegarty JE, Eddleston AL, Williams R. T and B cell function in alcoholic liver disease. J Hepatol. 1986;2:195–207. doi: 10.1016/s0168-8278(86)80078-2. [DOI] [PubMed] [Google Scholar]
- 70.Doi H, Iyer TK, Carpenter E, Li H, Chang KM, Vonderheide RH, et al. Dysfunctional B-cell activation in cirrhosis resulting from hepatitis C infection associated with disappearance of CD27-positive B-cell population. Hepatology. 2012;55:709–719. doi: 10.1002/hep.24689. doi: 10.1002/hep.24689. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Márquez M, Fernández-Gutiérrez C, Montes-de-Oca M, Blanco MJ, Brun F, Rodríguez-Ramos C, et al. Chronic antigenic stimuli as a possible explanation for the immunodepression caused by liver cirrhosis. Clin Exp Immunol. 2009;158:219–229. doi: 10.1111/j.1365-2249.2009.04005.x. doi: 10.1111/j.1365-2249.2009.04005.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.van de Wiel A, Schuurman HJ, Kater L. Alcoholic liver disease: an IgA-associated disorder. Scand J Gastroenterol. 1987;22:1025–1030. doi: 10.3109/00365528708991951. [DOI] [PubMed] [Google Scholar]
- 73.Silvain C, Patry C, Launay P, Lehuen A, Monteiro RC. Altered expression of monocyte IgA Fc receptors is associated with defective endocytosis in patients with alcoholic cirrhosis. Potential role for IFN-gamma. J Immunol. 1995;155:1606–1618. [PubMed] [Google Scholar]
- 74.Massonnet B, Delwail A, Ayrault JM, Chagneau-Derrode C, Lecron JC, Silvain C. Increased immunoglobulin A in alcoholic liver cirrhosis: exploring the response of B cells to Toll-like receptor 9 activation. Clin Exp Immunol. 2009;158:115–124. doi: 10.1111/j.1365-2249.2009.04004.x. doi: 10.1111/j.1365-2249.2009.04004.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Homann C, Varming K, Høgåsen K, Mollnes TE, Graudal N, Thomsen AC, et al. Acquired C3 deficiency in patients with alcoholic cirrhosis predisposes to infection and increased mortality. Gut. 1997;40:544–549. doi: 10.1136/gut.40.4.544. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Akalin HE, Laleli Y, Telatar H. Serum bactericidal and opsonic activities in patients with non-alcoholic cirrhosis. Q J Med. 1985;56:431–437. [PubMed] [Google Scholar]
- 77.Hillebrandt S, Wasmuth HE, Weiskirchen R, Hellerbrand C, Keppeler H, Werth A, et al. Complement factor 5 is a quantitative trait gene that modifies liver fibrogenesis in mice and humans. Nat Genet. 2005;37:835–843. doi: 10.1038/ng1599. doi: 10.1038/ng1599. [DOI] [PubMed] [Google Scholar]
- 78.Strey CW, Markiewski M, Mastellos D, Tudoran R, Spruce LA, Greenbaum LE, et al. The proinflammatory mediators C3a and C5a are essential for liver regeneration. J Exp Med. 2003;198:913–923. doi: 10.1084/jem.20030374. doi: 10.1084/jem.20030374. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Propst-Graham KL, Preheim LC, Vander Top EA, Snitily MU, Gentry-Nielsen MJ. Cirrhosis-induced defects in innate pulmonary defenses against Streptococcus pneumoniae. BMC Microbiol. 2007;7:94. doi: 10.1186/1471-2180-7-94. doi: 10.1186/1471-2180-7-94. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Altorjay I, Vitalis Z, Tornai I, Palatka K, Kacska S, Farkas G, et al. Mannose-binding lectin deficiency confers risk for bacterial infections in a large Hungarian cohort of patients with liver cirrhosis. J Hepatol. 2010;53:484–491. doi: 10.1016/j.jhep.2010.03.028. doi: 10.1016/j.jhep.2010.03.028. [DOI] [PubMed] [Google Scholar]
- 81.Wiest R, Garcia-Tsao G. Bacterial translocation (BT) in cirrhosis. Hepatology. 2005;41:422–433. doi: 10.1002/hep.20632. doi: 10.1002/hep.20632. [DOI] [PubMed] [Google Scholar]
- 82.Wyke RJ. Problems of bacterial infection in patients with liver disease. Gut. 1987;28:623–641. doi: 10.1136/gut.28.5.623. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Hoefs JC, Canawati HN, Sapico FL, Hopkins RR, Weiner J, Montgomerie JZ. Spontaneous bacterial peritonitis. Hepatology. 1982;2:399–407. doi: 10.1002/hep.1840020402. [DOI] [PubMed] [Google Scholar]
- 84.Aldersley MA, Howdle PD. Intestinal permeability and liver disease. Eur J Gastroenterol Hepatol. 1999;11:401–403. doi: 10.1097/00042737-199904000-00007. [DOI] [PubMed] [Google Scholar]
- 85.Martini GA, Phear EA, Ruebner B, Sherlock S. The bacterial content of the small intestine in normal and cirrhotic subjects: relation to methionine toxicity. Clin Sci. 1957;16:35–51. [PubMed] [Google Scholar]
- 86.Teltschik Z, Wiest R, Beisner J, Nuding S, Hofmann C, Schoelmerich J, et al. Intestinal bacterial translocation in rats with cirrhosis is related to compromised Paneth cell antimicrobial host defense. Hepatology. 2012;55:1154–1163. doi: 10.1002/hep.24789. doi: 10.1002/hep.24789. [DOI] [PubMed] [Google Scholar]
- 87.Llovet JM, Bartolí R, Planas R, Cabré E, Jimenez M, Urban A, et al. Bacterial translocation in cirrhotic rats. Its role in the development of spontaneous bacterial peritonitis. Gut. 1994;35:1648–1652. doi: 10.1136/gut.35.11.1648. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88.Chesta J, Lillo R, Defilippi C, Jouanee E, Massone MA, Maulén M, et al. Patients with liver cirrhosis: mouth-cecum transit time and gastric emptying of solid foods. Rev Med Chil. 1991;119:1248–1253. [PubMed] [Google Scholar]
- 89.Chang CS, Chen GH, Lien HC, Yeh HZ. Small intestine dysmotility and bacterial overgrowth in cirrhotic patients with spontaneous bacterial peritonitis. Hepatology. 1998;28:1187–1190. doi: 10.1002/hep.510280504. doi: 10.1002/hep.510280504. [DOI] [PubMed] [Google Scholar]
- 90.Chesta J, Defilippi C, Defilippi C. Abnormalities in proximal small bowel motility in patients with cirrhosis. Hepatology. 1993;17:828–832. [PubMed] [Google Scholar]
- 91.Appenrodt B, Grünhage F, Gentemann MG, Thyssen L, Sauerbruch T, Lammert F. Nucleotide-binding oligomerization domain containing 2 (NOD2) variants are genetic risk factors for death and spontaneous bacterial peritonitis in liver cirrhosis. Hepatology. 2010;51:1327–1333. doi: 10.1002/hep.23440. doi: 10.1002/hep.23440. [DOI] [PubMed] [Google Scholar]
- 92.Crossley IR, Williams R. Spontaneous bacterial peritonitis. Gut. 1985;26:325–331. doi: 10.1136/gut.26.4.325. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93.Keshavarzian A, Holmes EW, Patel M, Iber F, Fields JZ, Pethkar S. Leaky gut in alcoholic cirrhosis: a possible mechanism for alcohol-induced liver damage. Am J Gastroenterol. 1999;94:200–207. doi: 10.1111/j.1572-0241.1999.00797.x. doi: 10.1111/j.1572-0241.1999.00797.x. [DOI] [PubMed] [Google Scholar]
- 94.Toh Y, Korenaga D, Maekawa S, Matsumata T, Muto Y, Ikeda T, et al. Assessing the permeability of the gastrointestinal mucosa after oral administration of phenolsulfonphthalein. Hepatogastroenterology. 1997;44:1147–1151. [PubMed] [Google Scholar]
- 95.Campillo B, Pernet P, Bories PN, Richardet JP, Devanlay M, Aussel C. Intestinal permeability in liver cirrhosis: relationship with severe septic complications. Eur J Gastroenterol Hepatol. 1999;11:755–759. doi: 10.1097/00042737-199907000-00013. [DOI] [PubMed] [Google Scholar]
- 96.Pérez-Paramo M, Muñoz J, Albillos A, Freile I, Portero F, Santos M, et al. Effect of propranolol on the factors promoting bacterial translocation in cirrhotic rats with ascites. Hepatology. 2000;31:43–48. doi: 10.1002/hep.510310109. doi: 10.1002/hep.510310109. [DOI] [PubMed] [Google Scholar]
- 97.Senzolo M, Cholongitas E, Burra P, Leandro G, Thalheimer U, Patch D, et al. beta-Blockers protect against spontaneous bacterial peritonitis in cirrhotic patients: a meta-analysis. Liver Int. 2009;29:1189–1193. doi: 10.1111/j.1478-3231.2009.02038.x. doi: 10.1111/j.1478-3231.2009.02038.x. [DOI] [PubMed] [Google Scholar]
- 98.Bajaj JS, Ridlon JM, Hylemon PB, Thacker LR, Heuman DM, Smith S, et al. Linkage of gut microbiome with cognition in hepatic encephalopathy. Am J Physiol Gastrointest Liver Physiol. 2012;302:G168–G175. doi: 10.1152/ajpgi.00190.2011. doi: 10.1152/ajpgi.00190.2011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 99.Gómez-Hurtado I, Such J, Sanz Y, Francés R. Gut microbiota-related complications in cirrhosis. World J Gastroenterol. 2014;20:15624–15631. doi: 10.3748/wjg.v20.i42.15624. doi: 10.3748/wjg.v20.i42.15624. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 100.Bunchorntavakul C, Chavalitdhamrong D. Bacterial infections other than spontaneous bacterial peritonitis in cirrhosis. World J Hepatol. 2012;4:158–168. doi: 10.4254/wjh.v4.i5.158. doi: 10.4254/wjh.v4.i5.158. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 101.Fernández J, Acevedo J, Castro M, Garcia O, de Lope CR, Roca D, et al. Prevalence and risk factors of infections by multiresistant bacteria in cirrhosis: a prospective study. Hepatology. 2012;55:1551–1561. doi: 10.1002/hep.25532. doi: 10.1002/hep.25532. [DOI] [PubMed] [Google Scholar]
- 102.Thulstrup AM, Mølle I, Svendsen N, Sørensen HT. Incidence and prognosis of tuberculosis in patients with cirrhosis of the liver. A Danish nationwide population based study. Epidemiol Infect. 2000;124:221–225. doi: 10.1017/s0950268899003593. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 103.Baijal R, Praveenkumar HR, Amarapurkar DN, Nagaraj K, Jain M. Prevalence of tuberculosis in patients with cirrhosis of liver in western India. Trop Doct. 2010;40:163–164. doi: 10.1258/td.2010.090463. doi: 10.1258/td.2010.090463. [DOI] [PubMed] [Google Scholar]
- 104.Mabee CL, Mabee SW, Kirkpatrick RB, Koletar SL. Cirrhosis: a risk factor for cryptococcal peritonitis. Am J Gastroenterol. 1995;90:2042–2045. [PubMed] [Google Scholar]
- 105.Park WB, Choe YJ, Lee KD, Lee CS, Kim HB, Kim NJ, et al. Spontaneous cryptococcal peritonitis in patients with liver cirrhosis. Am J Med. 2006;119:169–171. doi: 10.1016/j.amjmed.2005.06.070. doi: 10.1016/j.amjmed.2005.06.070. [DOI] [PubMed] [Google Scholar]
- 106.Saif MW, Raj M. Cryptococcal peritonitis complicating hepatic failure: case report and review of the literature. J Appl Res. 2006;6:43–50. [PMC free article] [PubMed] [Google Scholar]
- 107.Khan FA, Fisher MA, Khakoo RA. Association of hemochromatosis with infectious diseases: expanding spectrum. Int J Infect Dis. 2007;11:482–487. doi: 10.1016/j.ijid.2007.04.007. doi: 10.1016/j.ijid.2007.04.007. [DOI] [PubMed] [Google Scholar]
- 108.Ashrafian H. Hepcidin: the missing link between hemochromatosis and infections. Infect Immun. 2003;71:6693–6700. doi: 10.1128/IAI.71.12.6693-6700.2003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 109.Kizer KW. Vibrio vulnificus hazard in patients with liver disease. West J Med. 1994;161:64–65. [PMC free article] [PubMed] [Google Scholar]
- 110.Noor MT, Tiwari M, Kumar R. Non-HFE iron overload as a surrogate marker of disease severity in patients of liver cirrhosis. Indian J Gastroenterol. 2016;35:33–39. doi: 10.1007/s12664-016-0623-6. doi: 10.1007/s12664-016-0623-6. [DOI] [PubMed] [Google Scholar]
- 111.Jalan R, Fernandez J, Wiest R, Schnabl B, Moreau R, Angeli P, et al. Bacterial infections in cirrhosis: a position statement based on the EASL Special Conference 2013. J Hepatol. 2014;60:1310–1324. doi: 10.1016/j.jhep.2014.01.024. doi: 10.1016/j.jhep.2014.01.024. [DOI] [PubMed] [Google Scholar]
- 112.Guarner C, Soriano G, Tomas A, Bulbena O, Novella MT, Balanzo J, et al. Increased serum nitrite and nitrate levels in patients with cirrhosis: relationship to endotoxemia. Hepatology. 1993;18:1139–1143. [PubMed] [Google Scholar]
- 113.Schuetz P, Albrich W, Mueller B. Procalcitonin for diagnosis of infection and guide to antibiotic decisions: past, present and future. BMC Med. 2011;9:107. doi: 10.1186/1741-7015-9-107. doi: 10.1186/1741-7015-9-107. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 114.Li CH, Yang RB, Pang JH, Chang SS, Lin CC, Chen CH, et al. Procalcitonin as a biomarker for bacterial infections in patients with liver cirrhosis in the emergency department. Acad Emerg Med. 2011;18:121–126. doi: 10.1111/j.1553-2712.2010.00991.x. doi: 10.1111/j.1553-2712.2010.00991.x. [DOI] [PubMed] [Google Scholar]
- 115.Sarin SK, Choudhury A. Acute-on-chronic liver failure: terminology, mechanisms and management. Nat Rev Gastroenterol Hepatol. 2016;13:131–149. doi: 10.1038/nrgastro.2015.219. doi: 10.1038/nrgastro.2015.219. [DOI] [PubMed] [Google Scholar]