Introduction
Colonizing opportunistic pathogens (COPs) are microbes that asymptomatically colonize the human body and, when the conditions are right, can cause infections. Their ability to persist indefinitely and to be transmitted without detection [1] gives COPs a unique epidemiology that warrants special consideration. There are examples of COPs among bacteria, fungi (e.g., Candida albicans [2]), protozoa (e.g., Blastocystis [3, 4]), and viruses (e.g., Rhinovirus [5]), but bacterial COPs are of particular relevance because of their major contribution to today’s antibiotic resistance crisis. The COPs include a long list of notorious bacteria that live double lives as passive stowaways and virulent foes. Some of the best-known COPs include Staphylococcus aureus, extraintestinal pathogenic Escherichia coli (ExPEC), Klebsiella pneumoniae, and Streptococcus pneumoniae (Table 1). Their capacity for benign coexistence with humans belies their alter egos that exact a heavy burden of human disease. For example, in the United States, ExPEC bloodstream infections kill as many as 40,000 people annually [6], but, ExPEC are also benign colonizers in the gastrointestinal tract [7]. Host factors, including age, sex, health status, anatomy, and behavior, all play profound roles in infection susceptibility and severity [8–10]. In particular, immunocompromised individuals are at excess risk for infections caused by diverse bacteria, including COPs [11, 12] and even commensals. Yet, health status is not the sole determinant of infection by COPs. For example, healthy women more frequently suffer from urinary tract infections than men because of anatomical differences, including shorter urethrae. Likewise, healthy children more commonly suffer from acute otitis media than adults due to their shorter, flatter eustachian tubes [13].
Table 1. Common bacterial colonizing opportunistic pathogens, simple opportunistic pathogens, and frank pathogens.
| COPs | Reservoir/Site of Colonization | Associated Human Diseases |
|---|---|---|
| Staphylococcus aureus | Nasal cavity, skin | Cellulitis, abscesses, osteomyelitis, endocarditis, sepsis |
| Streptococcus pneumoniae | Nasopharynx | Otitis media, pneumonia, sepsis |
| ExPEC | Oral cavity, skin, intestinal tract | Cystitis, pyelonephritis, meningitis, sepsis |
| Klebsiella pneumoniae | Oral cavity, skin, intestinal tract | Cystitis, pneumonia, sepsis |
| SOPs | ||
| Vibrio vulnificus | Raw/undercooked seafood, warm costal water | Wound infection, hemorrhagic bullae, sepsis |
| Mycobacterium marinum | Contaminated water sources (e.g., untreated pools, fish aquaria) | Granuloma, tenosynovitis, osteomyelitis |
| Legionella pneumophila | Freshwaters, contaminated human water systems (e.g., showers, faucets, cooling towers) | Legionnaires’ disease, Pontiac fever |
| Frank pathogens | ||
| Escherichia coli 0157:H7 | Food animals, food products | Bloody diarrhea, hemolytic uremic syndrome |
| Campylobacter jejuni | Food animals, food products | Watery diarrhea, Guillain-Barre syndrome |
| Salmonella enterica (including S. typhi) | Food animals, food products | Gastroenteritis, cystitis, typhoid fever, sepsis |
| Mycobacterium tuberculosis | Lungs of infected patients | Tuberculosis |
COPs, colonizing opportunistic pathogens; ExPEC, extraintestinal pathogenic Escherichia coli; SOPs, simple opportunistic pathogens.
Here, we focus on the ecological features that distinguish COPs from other bacterial pathogens. We explore the public health implications that arise from their unique biology and discuss the research needed to illuminate the dynamics of COPs among their human, animal, and environmental reservoirs. And finally, we consider the commonalities among COPs that may require active monitoring and management. Our examination complements and extends the damage-response framework of pathogenesis proposed by Casadevall and Pirofski [14] without focusing on the pathogenicity or virulence potential of COPs, exploring specifically the host immune response, or delving into mechanisms of how COPs transition from colonization to infection.
COPs are a distinct subgroup of the opportunistic pathogens
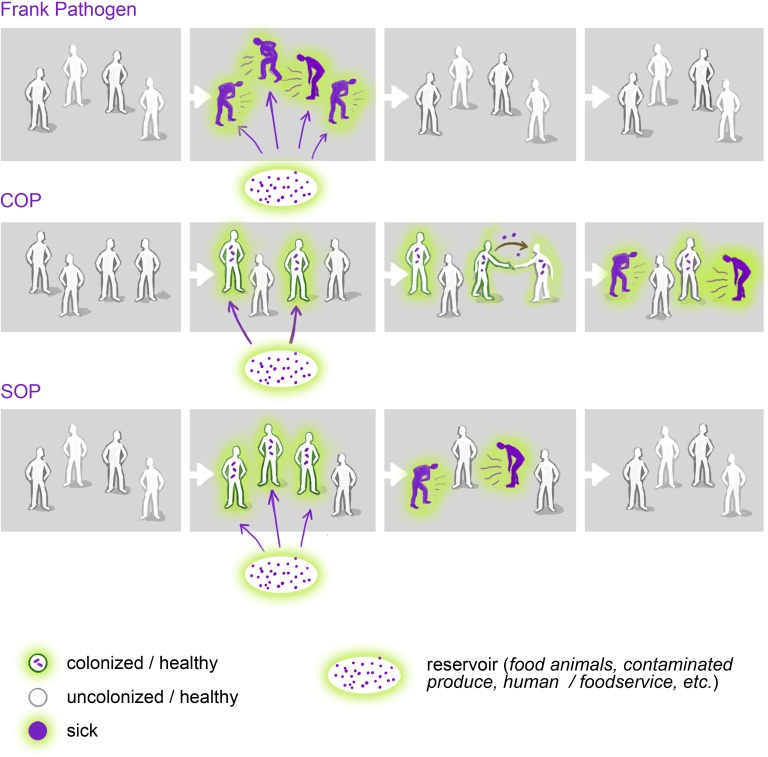
The broad category of opportunistic pathogens can be divided into 2 distinct subgroups: the COPs and the noncolonizing, simple opportunistic pathogens (SOPs; Fig 1). The defining feature of all opportunistic pathogens is their capacity to cause disease when they are introduced into a susceptible body site or when hosts are immunologically compromised. The reservoirs of opportunistic pathogens are diverse and include food, water, soil, animals, and people with active infections. Whereas SOPs, such as Vibrio vulnificus, Mycobacterium marinum, and Legionella pneumophila, are only present in environmental reservoirs, COPs can also take up long-term residence in or on the human body as part of the “normal” human microbiome. For example, S. aureus can colonize the human nose asymptomatically and transmit from person-to-person without causing disease [15, 16]. Although COP colonization itself is asymptomatic, it can be an important risk factor for subsequent disease [17]. For S. aureus, higher-abundance colonization that is detectable by culture is further linked to higher risk of subsequent infection than lower-abundance colonization that is frequently undetected by culture [18].
Fig 1. Colonizing opportunistic pathogens (COPs) can persist asymptomatically and indefinitely within a host and may spread silently within the community.
These unique features of COPs result in epidemiological patterns distinct from those of frank pathogens and simple opportunistic pathogens (SOPs)—patterns that may have substantial public health consequences—such as the spread of antibiotic resistance. A deeper understanding of COP ecology is needed to reveal the reservoirs and transmission pathways of COPs and to design surveillance programs capable of detecting the otherwise invisible epidemics caused by COPs. (Illustration by Victor Leshyk.)
COPs differ from frank pathogens (Table 1), which can cause acute, chronic, or latent infections that can be symptomatic or asymptomatic [19]. While the latent and reactivation phases of frank pathogens, such as Mycobacterium tuberculosis and Salmonella enterica serovar Typhi, may mimic the colonization and infection phases of COPs, they are distinct in that these latent infections are typically preceded by an acute infection and maintenance of the latent phase requires an active adaptive immune response [20]. This is distinct from the fully asymptomatic colonization by COPs (Fig 1). The detection of frank pathogens is often associated with a diseased state, whether active or latent, and identifying cases of active or recent infections is usually enough to trace transmission routes. The well-characterized incubation periods of frank pathogens are consistent features of their epidemiology and aid in tracking infections [21]. In contrast, COPs lack predictable periods between colonization and infection, making their epidemiology cryptic. Because of this, COPs can cause insidious epidemics, where new clones transmit widely—even globally—among healthy populations before being recognized. For example, by the time ExPEC strain ST131 was discovered in 2008, it had already made its way to at least 3 continents [22].
COPs present a special challenge with respect to antibiotic resistance
Today, some of the most important multidrug-resistant bacterial pathogens—methicillin-resistant S. aureus (MRSA) and carbapenem-resistant Enterobacteriaceae—are COPs. Administration of an antibiotic exerts selective pressure on all bacterial populations within a host. As a result, antibiotics can select for antibiotic-resistant COPs, in addition to commensals within the host microbiome, regardless of whether or not the specific COP was the intended target of the antibiotic treatment. For example, 30% to 50% of healthy adults are carriers of S. aureus [17, 23, 24], and if a carrier takes a course of cephalosporins for an unrelated infection, the antibiotic is applying collateral selective pressure on the carrier’s S. aureus population, conferring advantage to resistant subpopulations, including MRSA. Resistant strains that surge under such selective pressure may persist long after the target infection is cleared; this is consistent with the finding that previous antibiotic use significantly increases the risk for future antibiotic-resistant infections [25–29]. Vaccination can also exert selective pressure on target species population, such as in the example of pneumococcal vaccine [30], in which the resultant serotype replacement has shifted the resistance profile seen among invasive S. pneumoniae infections [31].
Characterizing the ecology of COPs is paramount to understanding their epidemiology
Characterizing the ecology of COPs will require a new research framework beyond studies of virulence, antibiotic resistance, and epidemiology of individual species. Fully capturing the ecology of COPs will require studying their distribution and dynamics which span 17 orders of spatial magnitude—from the human microbiome (1x10-5 m) to global travel and commerce (5x1011m). This will require investigating the intra- and inter-species relationships that determine the success and duration of COP colonization, and also the roles of reservoirs (e.g., humans, animals, soil, water, air, and others) in the maintenance and transmission of COPs. Vegetable crops, meat products, water resources, and air can all potentially be contaminated by antibiotic-resistant COPs from food animals and animal wastes [32, 33], in which airborne exposure likely drives the link between proximity of residence to manure application and livestock operations to increased risk of community-acquired MRSA infections [34]. Such ambitious ecological studies may require species- and even strain- or clonal-level focus, but the collective lessons learned can inform how we monitor, forecast, and respond to COPs in general.
The most urgent knowledge gaps related to COPs are the determinants of their colonization after exposure, the duration of colonization, and the transition from colonization to infection. Carefully designed observational studies could provide the samples necessary to close these knowledge gaps, given that empirical studies on human subjects may face ethical challenges, and that animal models—unless they are truly humanized in terms of immunity and resident microbiome—are likely to offer limited insight. Designing informative monitoring and observational studies will require creative and careful planning, as these knowledge gaps are well beyond the scope of typical studies conducted to date. One possible design encompassing the broad scale of COP ecology would be to monitor individuals from regions with a low prevalence of specific multidrug-resistant COPs that travel to regions where they are endemic [35]. One could then assess the microbiome and other host and microbial determinants of colonization and subsequent follow-up could provide insight into the transition from colonization to infection and human-to-human transmissions.
COPs require new active and integrative surveillance programs
Enhanced surveillance of COPs can enable public health agencies to identify and control emerging COP clones more quickly than is currently possible. Because of the insidious nature of COP epidemics, active surveillance programs that monitor both COPs circulating among asymptomatic carriers in the community and COPs causing clinical infections are crucial. This work will require the development of new molecular methods and could be integrated into existing surveillance programs, such as the National Healthcare and Safety Network, FoodNet, PulseNet, and the National Antimicrobial Resistance Monitoring System [36–39]. Active surveillance of COPs can involve sentinel communities, households, or individuals who are recruited to provide samples from body sites where COPs reside, such as nasal swabs and stool specimens for culture-based and molecular analyses. Current surveillance programs could expand their monitoring to encompass COP clones in clinical infections and in environmental reservoirs. Linking these data could allow an early warning system on emerging COP clones and provide valuable information for tracing community- versus healthcare-associated COP clones. Incorporating whole-genome DNA sequencing can further resolve subtleties ranging from shifts in COP clonal populations to the loss and gain of resistance-encoding mobile genetic elements [40–42].
Both frank pathogens and COPs can cause foodborne zoonotic infections. Infections caused by frank pathogens, such as Salmonella enterica, Campylobacter jejuni, and E. coli 0157:H7 (Table 1), can quickly be recognized and controlled by tracing clusters of infections to a common source [43–45]. Foodborne COPs, such as K. pneumoniae and multidrug-resistant ExPEC, are known to contaminate meat products and can cause infections in consumers [46]; however, because they may persist indefinitely in exposed hosts before causing an infection, disease clusters can be dispersed in time and space, obscuring the source of the pathogen. In addition to the prolonged colonization period, once a foodborne COP successfully colonizes a person, it may also be transmitted person-to-person [47], spreading through the human population to a far greater extent than frank foodborne pathogens. All of this contributes to the challenge of estimating the disease burden of foodborne COPs.
A key target in active surveillance of COPs is the environmental reservoirs (e.g., air, food, and water) and nonhuman “co-host” species such as wild animals, companion animals, and livestock. The widespread use of antimicrobials in livestock [48] makes food animals an important target in monitoring novel resistance elements in COPs and emerging antibiotic-resistant COP clones—this is supported by the recent report of a mobile colistin-resistance element, mcr-1, among livestock in China [49]. We will need to monitor COPs throughout the livestock production system—from breeder farms to slaughter—to identify the origins and potential control points for emerging COPs from livestock. Other livestock products, such as wastes and meat, should be integrated into the active surveillance of COPs. Ideally, the active surveillance of environmental reservoirs should be coordinated with the sentinel community-based sites to maximize the integration across scales.
Concluding thoughts
“Sometimes, it tries to kid me that it's just a teddy bear
or even somehow managed to vanish in the air
and that is when I must beware
of the beast in me.”
The Beast in Me by Nick Lowe
COPs are an important subgroup of the opportunistic pathogens that deserve special attention and require novel intervention strategies to curb their heavy public health burden. Understanding both the ecology and the epidemiology of COPs is necessary to identify effective interventions. Antimicrobial therapy is the current mainstay of treating COP infections, but the emergence of broadly multidrug-resistant COPs challenges this modality. The post-antibiotic era requires new ways to prevent COP infections by disrupting colonization rather than trying to treat pan-resistant infections. While much research will have to be conducted on the species or strain level, characterizing the full scope of COP ecology—from persistence in environmental reservoirs to transmission among humans—is key for taming these beasts in all of us.
Acknowledgments
The authors thank Victor Leshyk for creating the illustration.
Funding Statement
LBP's salary was supported by grants from the National Institutes of Health (4R01AI101371-04 and 5R21AI117654-02). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
References
- 1.Johnson JR, Russo TA. Extraintestinal pathogenic Escherichia coli: "the other bad E coli". The Journal of laboratory and clinical medicine. 2002;139(3):155–62. Epub 2002/04/11. . [DOI] [PubMed] [Google Scholar]
- 2.Achkar JM, Fries BC. Candida infections of the genitourinary tract. Clinical microbiology reviews. 2010;23(2):253–73. PubMed Central PMCID: PMCPMC2863365. doi: 10.1128/CMR.00076-09 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Andersen LO, Stensvold CR. Blastocystis in Health and Disease: Are We Moving from a Clinical to a Public Health Perspective? J Clin Microbiol. 2016;54(3):524–8. PubMed Central PMCID: PMCPMC4767957. doi: 10.1128/JCM.02520-15 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Scanlan PD, Stensvold CR, Rajilic-Stojanovic M, Heilig HG, De Vos WM, O'Toole PW, et al. The microbial eukaryote Blastocystis is a prevalent and diverse member of the healthy human gut microbiota. FEMS Microbiol Ecol. 2014;90(1):326–30. doi: 10.1111/1574-6941.12396 . [DOI] [PubMed] [Google Scholar]
- 5.Jansen RR, Wieringa J, Koekkoek SM, Visser CE, Pajkrt D, Molenkamp R, et al. Frequent detection of respiratory viruses without symptoms: toward defining clinically relevant cutoff values. J Clin Microbiol. 2011;49(7):2631–6. PubMed Central PMCID: PMCPMC3147826. doi: 10.1128/JCM.02094-10 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Russo TA, Johnson JR. Medical and economic impact of extraintestinal infections due to Escherichia coli: focus on an increasingly important endemic problem. Microbes and infection. 2003;5(5):449–56. Epub 2003/05/10. . [DOI] [PubMed] [Google Scholar]
- 7.Russo TA, Johnson JR. Proposal for a new inclusive designation for extraintestinal pathogenic isolates of Escherichia coli: ExPEC. The Journal of infectious diseases. 2000;181(5):1753–4. Epub 2000/05/24. doi: 10.1086/315418 . [DOI] [PubMed] [Google Scholar]
- 8.Wang MC, Tseng CC, Wu AB, Huang JJ, Sheu BS, Wu JJ. Different roles of host and bacterial factors in Escherichia coli extra-intestinal infections. Clin Microbiol Infect. 2009;15(4):372–9. . [DOI] [PubMed] [Google Scholar]
- 9.Andersen PS, Larsen LA, Fowler VG Jr., Stegger M, Skov RL, Christensen K. Risk factors for Staphylococcus aureus nasal colonization in Danish middle-aged and elderly twins. Eur J Clin Microbiol Infect Dis. 2013;32(10):1321–6. PubMed Central PMCID: PMCPMC3775156. doi: 10.1007/s10096-013-1882-0 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Graffunder EM, Venezia RA. Risk factors associated with nosocomial methicillin-resistant Staphylococcus aureus (MRSA) infection including previous use of antimicrobials. J Antimicrob Chemother. 2002;49(6):999–1005. . [DOI] [PubMed] [Google Scholar]
- 11.Karuthu S, Blumberg EA. Common infections in kidney transplant recipients. Clin J Am Soc Nephrol. 2012;7(12):2058–70. doi: 10.2215/CJN.04410512 . [DOI] [PubMed] [Google Scholar]
- 12.Kaplan JE, Hanson D, Dworkin MS, Frederick T, Bertolli J, Lindegren ML, et al. Epidemiology of human immunodeficiency virus-associated opportunistic infections in the United States in the era of highly active antiretroviral therapy. Clin Infect Dis. 2000;30 Suppl 1:S5–14. doi: 10.1086/313843 . [DOI] [PubMed] [Google Scholar]
- 13.Harmes KM, Blackwood RA, Burrows HL, Cooke JM, Harrison RV, Passamani PP. Otitis media: diagnosis and treatment. Am Fam Physician. 2013;88(7):435–40. . [PubMed] [Google Scholar]
- 14.Casadevall A, Pirofski LA. The damage-response framework of microbial pathogenesis. Nat Rev Microbiol. 2003;1(1):17–24. doi: 10.1038/nrmicro732 . [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Kluytmans JA, Wertheim HF. Nasal carriage of Staphylococcus aureus and prevention of nosocomial infections. Infection. 2005;33(1):3–8. Epub 2005/03/08. doi: 10.1007/s15010-005-4012-9 . [DOI] [PubMed] [Google Scholar]
- 16.Calfee DP, Durbin LJ, Germanson TP, Toney DM, Smith EB, Farr BM. Spread of methicillin-resistant Staphylococcus aureus (MRSA) among household contacts of individuals with nosocomially acquired MRSA. Infection control and hospital epidemiology. 2003;24(6):422–6. Epub 2003/06/28. doi: 10.1086/502225 . [DOI] [PubMed] [Google Scholar]
- 17.Kluytmans J, van Belkum A, Verbrugh H. Nasal carriage of Staphylococcus aureus: epidemiology, underlying mechanisms, and associated risks. Clinical microbiology reviews. 1997;10(3):505–20. Epub 1997/07/01. ; PubMed Central PMCID: PMCPMC172932. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Liu CM, Price LB, Hungate BA, Abraham AG, Larsen LA, Christensen K, et al. Staphylococcus aureus and the ecology of the nasal microbiome. Sci Adv. 2015;1(5):e1400216 PubMed Central PMCID: PMCPMC4640600. doi: 10.1126/sciadv.1400216 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Parrish NM, Dick JD, Bishai WR. Mechanisms of latency in Mycobacterium tuberculosis. Trends in microbiology. 1998;6(3):107–12. Epub 1998/05/16. . [DOI] [PubMed] [Google Scholar]
- 20.Monack DM, Mueller A, Falkow S. Persistent bacterial infections: the interface of the pathogen and the host immune system. Nat Rev Microbiol. 2004;2(9):747–65. doi: 10.1038/nrmicro955 . [DOI] [PubMed] [Google Scholar]
- 21.Organization WH. Foodborne disease outbreaks: Guidelines for investigation and control. France: 2008.
- 22.Nicolas-Chanoine MH, Blanco J, Leflon-Guibout V, Demarty R, Alonso MP, Canica MM, et al. Intercontinental emergence of Escherichia coli clone O25:H4-ST131 producing CTX-M-15. J Antimicrob Chemother. 2008;61(2):273–81. Epub 2007/12/14. doi: 10.1093/jac/dkm464 . [DOI] [PubMed] [Google Scholar]
- 23.van Belkum A, Verkaik NJ, de Vogel CP, Boelens HA, Verveer J, Nouwen JL, et al. Reclassification of Staphylococcus aureus nasal carriage types. The Journal of infectious diseases. 2009;199(12):1820–6. Epub 2009/05/08. doi: 10.1086/599119 . [DOI] [PubMed] [Google Scholar]
- 24.Brown AF, Leech JM, Rogers TR, McLoughlin RM. Staphylococcus aureus Colonization: Modulation of Host Immune Response and Impact on Human Vaccine Design. Frontiers in immunology. 2014;4:507 Epub 2014/01/11. PubMed Central PMCID: PMCPMC3884195. doi: 10.3389/fimmu.2013.00507 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Arnold KE, Leggiadro RJ, Breiman RF, Lipman HB, Schwartz B, Appleton MA, et al. Risk factors for carriage of drug-resistant Streptococcus pneumoniae among children in Memphis, Tennessee. The Journal of pediatrics. 1996;128(6):757–64. Epub 1996/06/01. . [DOI] [PubMed] [Google Scholar]
- 26.Baden LR, Thiemke W, Skolnik A, Chambers R, Strymish J, Gold HS, et al. Prolonged colonization with vancomycin-resistant Enterococcus faecium in long-term care patients and the significance of "clearance". Clin Infect Dis. 2001;33(10):1654–60. Epub 2001/10/12. doi: 10.1086/323762 . [DOI] [PubMed] [Google Scholar]
- 27.Radetsky MS, Istre GR, Johansen TL, Parmelee SW, Lauer BA, Wiesenthal AM, et al. Multiply resistant pneumococcus causing meningitis: its epidemiology within a day-care centre. Lancet. 1981;2(8250):771–3. Epub 1981/10/10. . [DOI] [PubMed] [Google Scholar]
- 28.Reichler MR, Allphin AA, Breiman RF, Schreiber JR, Arnold JE, McDougal LK, et al. The spread of multiply resistant Streptococcus pneumoniae at a day care center in Ohio. The Journal of infectious diseases. 1992;166(6):1346–53. Epub 1992/12/01. . [DOI] [PubMed] [Google Scholar]
- 29.Tan TQ, Mason EO Jr., Kaplan SL. Penicillin-resistant systemic pneumococcal infections in children: a retrospective case-control study. Pediatrics. 1993;92(6):761–7. Epub 1993/12/01. . [PubMed] [Google Scholar]
- 30.Miller E, Andrews NJ, Waight PA, Slack MP, George RC. Herd immunity and serotype replacement 4 years after seven-valent pneumococcal conjugate vaccination in England and Wales: an observational cohort study. The Lancet Infectious diseases. 2011;11(10):760–8. doi: 10.1016/S1473-3099(11)70090-1 . [DOI] [PubMed] [Google Scholar]
- 31.Dagan R. Impact of pneumococcal conjugate vaccine on infections caused by antibiotic-resistant Streptococcus pneumoniae. Clin Microbiol Infect. 2009;15 Suppl 3:16–20. doi: 10.1111/j.1469-0691.2009.02726.x . [DOI] [PubMed] [Google Scholar]
- 32.Schulz J, Friese A, Klees S, Tenhagen BA, Fetsch A, Rosler U, et al. Longitudinal study of the contamination of air and of soil surfaces in the vicinity of pig barns by livestock-associated methicillin-resistant Staphylococcus aureus. Appl Environ Microbiol. 2012;78(16):5666–71. PubMed Central PMCID: PMCPMC3406131. doi: 10.1128/AEM.00550-12 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Marti R, Scott A, Tien YC, Murray R, Sabourin L, Zhang Y, et al. Impact of manure fertilization on the abundance of antibiotic-resistant bacteria and frequency of detection of antibiotic resistance genes in soil and on vegetables at harvest. Appl Environ Microbiol. 2013;79(18):5701–9. PubMed Central PMCID: PMCPMC3754188. doi: 10.1128/AEM.01682-13 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Casey JA, Curriero FC, Cosgrove SE, Nachman KE, Schwartz BS. High-density livestock operations, crop field application of manure, and risk of community-associated methicillin-resistant Staphylococcus aureus infection in Pennsylvania. JAMA Intern Med. 2013;173(21):1980–90. PubMed Central PMCID: PMCPMC4372690. doi: 10.1001/jamainternmed.2013.10408 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Arcilla MS, van Hattem JM, Matamoros S, Melles DC, Penders J, de Jong MD, et al. Dissemination of the mcr-1 colistin resistance gene. The Lancet Infectious diseases. 2016;16(2):147–9. Epub 2015/12/30. doi: 10.1016/S1473-3099(15)00541-1 . [DOI] [PubMed] [Google Scholar]
- 36.Prevention CfDCa. Foodborne Disease Active Surveillance Network (FoodNet) 2015 [updated 11/28/2016; cited 2017 01/25/17]. Available from: https://www.cdc.gov/foodnet/index.html.
- 37.Prevention CfDCa. National Healthcare Safety Network 2016 [updated 10/21/2016; cited 2017 01/25/17]. Available from: https://www.cdc.gov/nhsn/.
- 38.Prevention CfDCa. PulseNet 2016 [updated 10/03/16; cited 2017 01/25/17]. Available from: https://www.cdc.gov/pulsenet/.
- 39.Prevention CfDCa. National Antimicrobial Resistance Monitoring System for Enteric Bacteria (NARMS) 2017 [updated 01/20/17; cited 2017 01/25/17]. Available from: https://www.cdc.gov/narms/.
- 40.Price LB, Johnson JR, Aziz M, Clabots C, Johnston B, Tchesnokova V, et al. The epidemic of extended-spectrum-beta-lactamase-producing Escherichia coli ST131 is driven by a single highly pathogenic subclone, H30-Rx. mBio. 2013;4(6):e00377–13. Epub 2013/12/19. PubMed Central PMCID: PMCPMC3870262. doi: 10.1128/mBio.00377-13 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Price LB, Stegger M, Hasman H, Aziz M, Larsen J, Andersen PS, et al. Staphylococcus aureus CC398: host adaptation and emergence of methicillin resistance in livestock. mBio. 2012;3(1). Epub 2012/02/23. PubMed Central PMCID: PMCPMC3280451. doi: 10.1128/mBio.00305-11 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Uhlemann AC, Dordel J, Knox JR, Raven KE, Parkhill J, Holden MT, et al. Molecular tracing of the emergence, diversification, and transmission of S. aureus sequence type 8 in a New York community. Proceedings of the National Academy of Sciences of the United States of America. 2014;111(18):6738–43. Epub 2014/04/23. PubMed Central PMCID: PMCPMC4020051. doi: 10.1073/pnas.1401006111 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Two multistate outbreaks of Shiga toxin—producing Escherichia coli infections linked to beef from a single slaughter facility—United States, 2008. MMWR Morbidity and mortality weekly report. 2010;59(18):557–60. Epub 2010/05/15. . [PubMed] [Google Scholar]
- 44.Maguire HC, Codd AA, Mackay VE, Rowe B, Mitchell E. A large outbreak of human salmonellosis traced to a local pig farm. Epidemiology and infection. 1993;110(2):239–46. Epub 1993/04/01. ; PubMed Central PMCID: PMCPMC2272258. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Spika JS, Waterman SH, Hoo GW, St Louis ME, Pacer RE, James SM, et al. Chloramphenicol-resistant Salmonella newport traced through hamburger to dairy farms. A major persisting source of human salmonellosis in California. The New England journal of medicine. 1987;316(10):565–70. Epub 1987/03/05. doi: 10.1056/NEJM198703053161001 . [DOI] [PubMed] [Google Scholar]
- 46.Overdevest I, Willemsen I, Rijnsburger M, Eustace A, Xu L, Hawkey P, et al. Extended-spectrum beta-lactamase genes of Escherichia coli in chicken meat and humans, The Netherlands. Emerg Infect Dis. 2011;17(7):1216–22. PubMed Central PMCID: PMCPMC3381403. doi: 10.3201/eid1707.110209 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Johnson JR, Clabots C. Sharing of virulent Escherichia coli clones among household members of a woman with acute cystitis. Clin Infect Dis. 2006;43(10):e101–8. Epub 2006/10/20. doi: 10.1086/508541 . [DOI] [PubMed] [Google Scholar]
- 48.Administration UFaD. FDA Annual Summary Report on Antimicrobials Sold or Distributed in 2014 for Use in Food-Producing Animals. 2015.
- 49.Liu YY, Wang Y, Walsh TR, Yi LX, Zhang R, Spencer J, et al. Emergence of plasmid-mediated colistin resistance mechanism MCR-1 in animals and human beings in China: a microbiological and molecular biological study. The Lancet Infectious diseases. 2016;16(2):161–8. Epub 2015/11/26. doi: 10.1016/S1473-3099(15)00424-7 . [DOI] [PubMed] [Google Scholar]