Abstract
The mortality of conservative treatment and the risk resulting from operation for elderly patients with femoral intertrochanteric fractures are high. Safety in the perioperative period and quicker recovery should be placed at the top priority for elderly patients with hip fractures. We reported a case of 109-year-old female patient with intertrochanteric fracture who has undergone the hemiarthroplasty in our center recently.
With sciatic nerve and lateral cutaneous nerve block anesthesia, she was offered the artificial femoral head replacement in the lumbar plexus block after sufficient preoperative preparation. The surgery went well with minimally invasive cut, and the patient's recovery was satisfactory.
Keywords: Aged, Hip fractures, Hemiarthroplasty
Introduction
Hip fracture is a disabling event, which is an important cause of the death of the elderly.1, 2, 3, 4 The patients may die of pulmonary infection, heart failure, etc, usually lie in bed for a long time. And the quality of life is poor, which is a heavy burden to the family. To restore the function and activity, a fixation of surgery is needed, of which the recovery is slow and may result in the risks of no healing because of osteoporosis, while artificial femoral head replacement allows early walk with weight bearing and provides a quick recovery. We treated a case of 109-year-old female patient with intertrochanteric fracture recently, with hemiarthroplasty in the local nerve block anesthesia. The surgery went well with a satisfactory result.
Case report
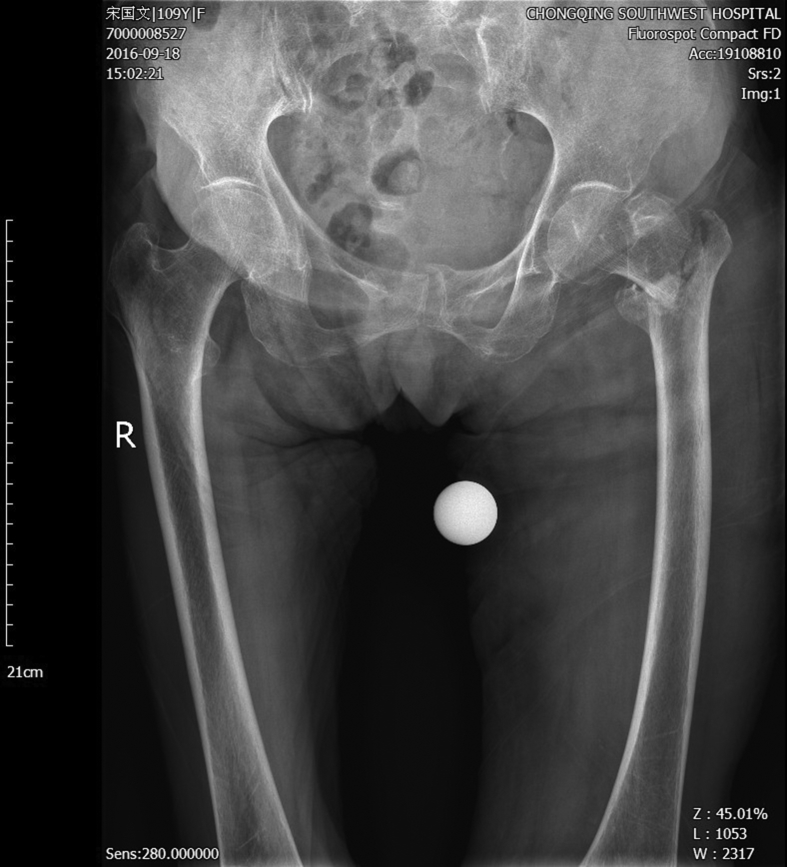
A 109-year-old female patient fell in the bathroom and could not stand up by herself with the left hip and the left palm injured. She was sent to a local hospital immediately. The X-ray examination showed left femur intertrochanteric fracture (Fig. 1). Due to the high risk of surgery of such super senior age, the operation was not performed. A week later, the patient was transferred to our department, and we found that she was in a good condition. She was able to walk indoor without crutches before the injury. Since there was no obvious surgery contraindication, the patient and his family decided to do the surgery hoping to restore the function and improve the quality of life. Physical examinations found ecchymosis in her left hip with the size of 8 cm × 20 cm, no skin damage and bedsore. With severe pain in the left hip, she prevented active activities from the left leg which resulted in shortening deformity. In April, she was hospitalized for one week for the pericardial effusion.
Fig. 1.
The preoperative X-ray shows intertrochanteric fractures without broken end shift.
Preoperative examinations showed: heart ejection fraction 57%, BNP1673.0 pg/ml, PO2 67 mmHg, HGB 61 g/L, UN 14.7 mmol/L, Cr 137.0 mmol/L, albumin 31.00 g/L left, serum iron 8 μmol/L, transferrin 123 mg/dl.
After admission, blood transfusion, intravenous iron supplement, erythropoietin subcutaneous injection and folic acid were offered to correct anemia, the HGB raised to 89 g/L, close to her basic level. We evaluated her basal metabolism by recording the intake and output volume. Hospital consultation was conducted preoperatively, and the related department collaboration and perioperative treatment plan were carefully made. Lumbar plexus, sciatic nerve and the lateral cutaneous nerve block were chosen. Perioperative intravenous infusion speed was controlled under 120 ml/h. And urine output remained at around 30 ml/h. The three dimensions visual template technology and hip fracture model printing ensured accurate measurement and evaluation (Fig. 2). After full preparation, she was offered the left artificial femoral head replacement with lateral position and posterolateral approach. We found that fracture line extended from the great trochanter to the top of the small trochanter with great trochanter avulsion fracture. The femoral neck was cut without dislocation. Then we took out the femoral head, reamed the cavity directly and inserted the implant mold. The fracture was stable, so we put the prosthesis to the fracture position apart from suturing of avulsion fracture (Fig. 3). The operation went smoothly and safely, with about 100 ml bleeding during the operation and 8 cm incision length.
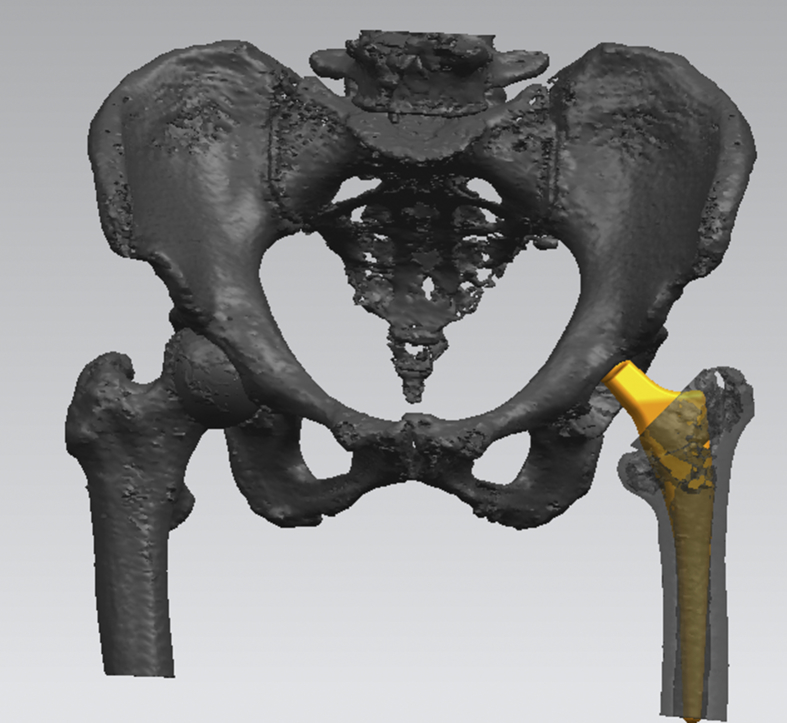
Fig. 2.
The preoperative three dimensions visual template technology measured the size accurately.
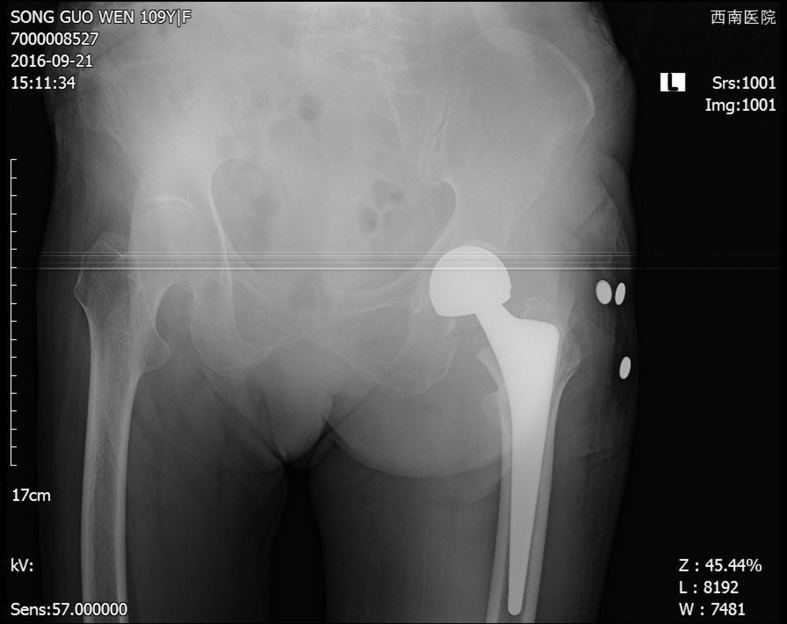
Fig. 3.
Postoperative prosthesis position was good and the fracture end was stable.
The patient was conscious after the operation without special discomfort complains, and immediately returned to normal diet. Semireclining position was maintained, and the patient had a good rest. The swelling was not obvious in the first day, and the dressing was dry. The drainage volume was about 90 ml. We controlled infusion speed in 40 drops/min, and urine volume remained at around 30 ml/h, which was consistent with preoperative level.
The patient was able to walk 22 h after the operation, and we took out the extubation 2 h later, then she could have fully weight-bearing walk herself slowly with walking aid. Rehabilitation exercise went well without complications, such as heart and lung failure. Then she was discharged four days after operation. Two weeks postoperatively, the wound healed completely, and her 110 -year - old birthday were celebrated happily with her family.
The function was good and no special discomfort half years after the operation. X-ray showed the fracture healed completely with the prosthesis in a good position (Fig. 4).
Fig. 4.
The fracture healed completely with the prosthesis in good position half years after the operation.
Discussion
Previous literature showed that the mortality at 3, 6, 12 and 24 months of the injury in the elderly patients with hip fracture was 54%, 61%, 64% and 82%, while 9%, 11%, 14%, and 21% after surgery.5 So regaining activity ability fast by surgical operation is an effective way to reduce mortality for senile fracture patients. Yet the risk is significantly increased within a month after injury for the elderly patients with hip fracture, which is higher in two days postoperatively.6 So the way to make the perioperative period fast, safe and smooth is the key.
The patient could walk without any walking aid in a good physical condition, but had poor cardiopulmonary function. If she spent a long time bedridden without surgery, her heart and lung function would decline, and even hypostatic pneumonia might happen. Then her prognosis is poor, the mortality is high, and the quality of life is poor. The patient and her family had a strong desire to do the surgery. But she would face many risks, such as perioperative cardiorespiratory failure, pulmonary infection, deep vein thrombosis, etc. As far as we know from the literature, the patient might be currently the eldest one who received artificial joint replacement because of hip fracture.
Preoperative examination showed that the patient had moderate anemia accompanying iron deficiency, so we improved the level of HB from the following several ways such as iron supplement, red blood cell mobilization and blood transfusion. In addition, we administered tranexamic acid 0.5 g intravenously before the operation and 0.5 g tranexamic acid into the joint through the drainage tube after the incision was closed. Perioperative bleeding was about 190 ml, hemoglobin maintained at her basic level, and there was no complication caused by anemia and no postoperative thromboembolism.
Regarding surgical intervention, three dimensions visual template technology and hip fracture model printing ensured accurate measurement and evaluation, and hence reduced operative time. 3D printing model is conducive to doctor-patient communication and improves the surgical program.7 We used minimally invasive small incision, thorough hemostasis and shortened operation time as far as possible. Dislocation bone cutting technology could not avoid further enlargement of fracture wound. Through a rectangular conventional short shank prosthesis could achieve local stability, thus avoiding greater trauma and blood loss by the long handle prosthesis. A rectangular conventional short shank prosthesis could achieve local stability, which could avoid greater trauma and blood loss by the long handle prosthesis.
Nerve block anesthesia with minimum side effects was chosen, of which the operation process did not use any sedative drugs, and systolic blood pressure remained at around 140 mmHg. By monitoring the postoperative intake and output volume, the transfusion speed was controlled in 40 drops/min and urine remained at around 30 ml/h. There was no fluctuation in blood pressure and heart rate in the perioperative period, which was consistent with the preoperative levels, so the internal environment of patient was interfered very slightly.
Preoperative ankle pump training was for reducing the incidence of deep vein thrombosis, and atomization treatment for reducing the incidence of pulmonary infection. The patient immediately returned to the normal diet and half supine position after the surgery, then she could get out of the bed and have a seat 22 h after the operation. After taking out the extubation 2 h later, she could have fully weight-bearing walk on her own. There were no signs of lung infection because of less time in bed, and no deep venous thrombosis by early getting out of the bed and functional exercise.
Internal fixation treatment is still the main stream for elderly patients with intertrochanteric fracture at present, which may delay the time of weight bearing, prolong postoperative bedridden time, and increase probability of fracture nonunion. And the artificial femoral head replacement allows immediate postoperative full weight-bearing and restores a normal daily life. She recovered well, and can walk without walking aid. So the artificial femoral head replacement is a choice for elderly patients with intertrochanteric fracture.
We know from the case that advanced age is not the contraindication of the hip fracture surgery. Sufficient preoperative assessments and detailed strategies, the least interference mode of anesthesia, the stability of internal environment, the minimally invasive surgery and the early functional exercise are essential to achieve a successful outcome.
Footnotes
Peer review under responsibility of Daping Hospital and the Research Institute of Surgery of the Third Military Medical University.
References
- 1.Bhattacharyya T., Iorio R., Healy W.L. Rate of and risk factors for acute inpatient mortality after orthopaedic surgery. J Bone Joint Surg Am. 2002;84:562–572. doi: 10.2106/00004623-200204000-00009. [DOI] [PubMed] [Google Scholar]
- 2.Kanis J.A., Oden A., Johnell O. The components of excess mortality after hip fracture. Bone. 2003;32 doi: 10.1016/s8756-3282(03)00061-9. 468–468. [DOI] [PubMed] [Google Scholar]
- 3.Yoon H.K., Park C., Jang S. Incidence and mortality following hip fracture in Korea. J Korean Med Sci. 2011;26:1087–1092. doi: 10.3346/jkms.2011.26.8.1087. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Kim S.R., Ha Y.C., Park Y.G. Orthopedic surgeon's awareness can improve osteoporosis treatment following hip fracture: a prospective cohort study. J Korean Med Sci. 2011;26:1501–1507. doi: 10.3346/jkms.2011.26.11.1501. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Yoon B.H.1, Baek J.H., Kim M.K. Poor prognosis in elderly patients who refused surgery because of economic burden and medical problem after hip fracture. J Korean Med Sci. 2013;28:1378–1381. doi: 10.3346/jkms.2013.28.9.1378. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Castronuovo E., Pezzotti P., Franzo A. Early and late mortality in elderly patients after hip fracture: a cohort study using administrative health databases in the Lazio region, Italy. BMC Geriatr. 2011;5:11–37. doi: 10.1186/1471-2318-11-37. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Ren X., Yang L., Duan X.J. Three-dimensional printing in the surgical treatment of osteoid osteoma of the calcaneus: a case report. J Int Med Res. 2017;45:372–380. doi: 10.1177/0300060516686514. [DOI] [PMC free article] [PubMed] [Google Scholar]