Abstract
Retained calculi in the cystic duct or gall bladder remnant can present as a post-cholecystectomy problem. Increased suspicion is necessary to diagnose this condition in a symptomatic post-cholecystectomy patient. Ultrasonography usually detects this condition, but magnetic resonance cholangiopancreatography is the test of choice for diagnosis as well as for surgical planning. Laparoscopic re-excision of the stump in most cases is feasible and safe. It is increasingly becoming the treatment of choice.
Keywords: MRCP—magnetic resonance cholangiopancreatography, ERCP—endoscopic retrograde cholangiopancreatography, USG—ultrasonography, LC—laparoscopic cholecystectomy
Introduction
Retained stone in a remnant of cystic duct or gall bladder is a well-known factor, among a number of causes which can present as post-cholecystectomy problem. Laparoscopic cholecystectomy (LC) has favored the division of cystic duct closer to the gall bladder. This is of paramount importance to avoid iatrogenic injury to the common bile duct. However, this renders the possibility of leaving a long cystic duct remnant [1]. Frequently, even gall bladder remnants remain behind either because of performance of subtotal cholecystectomy or as a result of improper identification of the gall bladder—cystic duct junction, due to inadequate skeletonization of the cystic duct [2]. This problem compounds during performance of LC for acute cholecystitis or Mirizzi’s syndrome. The large number of patients (85%) [3] derives relief of symptoms following this procedure. Five percent of patients after laparoscopic cholecystectomy still continue to have severe, persistent pre-surgical symptoms, and significant numbers among these patients have cystic duct or gall bladder remnant stone [4].
Patients and Methods
We managed 13 such patients of cystic duct stump stone and gall bladder remnant stone, between 2010 and 2015 (Table 1). Because of incomplete data, one patient was excluded from the analysis.
Table 1.
List of patients and their clinical details
| Sl no. | Age (years) | Sex | Duration of symptoms | Time since first procedure | Diagnostic test | Past surgery | Repeat procedure | Stump length (cm) | Follow-up |
|---|---|---|---|---|---|---|---|---|---|
| 01) | 64 | Female | 3 months | 8 years | USG and MRCP | OC | LCC 2010 | 3.0 | 5 years |
| 02) | 45 | Female | 7 years | 9 years | USG | OC | LCC 2010 | 3.5 | 5 years |
| 03) | 44 | Female | 2 years | 3 years | USG and MRCP | OC* | OCC+ Roux-en-Y CDJ 2010 | 3.0 | 5 years |
| 04) | 40 | Female | 6 months | 2.5 years | USG and MRCP | OC | LAP → OCC 2011 | 6 | 4 years |
| 05) | 32 | Male | 8 years | 8 years | USG and MRCP | OC | OCC 2011 | 2.5 | 4 years |
| 06) | 46 | Female | 2 months | 2 years 9 months | USG and MRCP | OC** | OCC + CDD 2011 | 2.5 | 2 years |
| 07) | 24 | Female | 2.5 months | 10 months | USG | OC# | LAP → OCC 2012 | 4.0 | 3 years |
| 08) | 72 | Male | 10 days | 4 years | MRCP | LC | LCC 2014 | 2.2 | 1 year |
| 09) | 22 | Female | 8 days | 6 years | MRCP | LC | LCC 2015 | 3.5 | 6 months |
| 10) | 22 | Female | 6 years | 6 years | MRCP | LC | LCC 2015 | 1.3 | 11 months |
| 11) | 49 | Female | 2 months | 2.5 years | USG & MRCP | LC | LCC 2015 | 4.0 | 10 months |
| 12) | 51 | Male | 1 month | 11 years | MRCP | OC | LCC 2015 | 2.0 | 9 months |
LCC laparoscopic completion cholecystectomy, OCC open completion cholecystectomy, CDJ choledochojejunostomy, CDD choledochoduodenostomy. LAP→OCC laparoscopy converted to open completion cholecystectomy
*Benign lower end biliary stricture (history of choledocholithiasis and multiple ERCP stone clearance)
**Benign lower end biliary stricture (history of choledocholithiasis, multiple ERCP stone clearance, and CBD exploration)
#Beta thalassemia, history of cholecystostomy, splenectomy followed by cholecystectomy
This is a retrospective, observational study.
Results
Upper abdominal pain was the universal complaint among our patients. However, the duration of symptoms varied widely, ranging from 8 days to 8 years (median 2.25 months). Eight patients had the history of open cholecystectomy and four patients had undergone LC in the past. The time gap between the index surgery and the development of symptoms is also quite varied in our series (range 0–10 years 11 months and median 39.33 months). There was no relief of symptoms in two patients after the index procedure. They continued to have persistent symptoms for many years. On the other hand, one patient developed symptoms, 10 years 11 months after the first procedure. One patient was diagnosed with cystic duct stump stones on post-operative day 1 by ultrasonography as the operating surgeon suspected the condition (patient no. 11), though the patient became symptomatic only after almost 2.5 years. Ultrasonography detected the condition in eight (66.67%) patients. Magnetic resonance cholangiopancreatography (MRCP) diagnosed the condition, when considered, in ten out of ten patients. One MRCP done outside was reported as normal, but the cystic duct stump was picked up on reviewing the images. Nine patients were considered for laparoscopic completion cholecystectomy. Laparoscopic completion cholecystectomy could be successfully performed in seven (77.78%) patients. In all laparoscopically completed cases, cystic duct stump could be clipped and divided except in one patient where it was ligated with suture. In one patient, the cystic artery stump was initially mistaken for the cystic duct stump during surgery, but comparing the size of the specimen with the MRCP size of the stump, we realized the mistake and proceeded to dissect out the true cystic duct stump.
In two patients, the laparoscopic procedure was converted to an open procedure, in view of dense adhesions, making dissection extremely difficult. Two of our patients had distal common bile duct stricture, which required an additional procedure in the form of a Roux-en-Y choledochojejunostomy in one and choledochoduodenostomy in another. Post-operative recovery was uneventful in all the cases. After a median follow-up of 42 months (range 6 months to 5 years), all but one patient remained asymptomatic after the performance of the completion procedure. In this patient (patient no. 9), she presented 6 days after the completion surgery with upper abdominal pain. Serum bilirubin (total and conjugated), alkaline phosphatase, and gamma-glutamyltransferase were raised. Her MRCP was normal. Endoscopic retrograde cholangiopancreatography (ERCP) did not reveal any retained stone; however, symptoms resolved after endoscopic sphincterotomy. We suspect the symptoms were due to passage of stones in the bile duct from the cystic duct stump.
Discussion
Florcken in 1912 first reported the problem of “cystic duct remnant” [5]. A cystic duct remnant is a term used when the size of the cystic duct following cholecystectomy is more than or equal to 1 cm [6] resulting in persistent symptoms.
In our series, the presentation has been persistence or recurrence of intermittent upper abdominal pain. Thus, such symptoms necessitate appropriate investigations to exclude this condition. Nihilism from the surgeon’s side and mere treatment of the symptoms following cholecystectomy should be avoided. Interestingly, recurrent symptoms may occur years after cholecystectomy with an apparently long symptom-free interval. This fact has been quite evident in our series.
Although literature regarding this entity is sparse, however, some researchers have reported the incidence of cystic duct stump syndrome to be as high as 16% [4]. With the establishment of LC as the current standard of care for gallstone disease, it is thought the incidence of cystic duct stone has increased. Laparoscopically dividing the cystic duct close to the gallbladder is advocated to prevent bile duct injury and that increases the possibility of long cystic duct stump. In a study of intravenous cholangiography in 113 post-cholecystectomy patients, Keiler et al. found that > 65% patients had > 1 cm cystic duct left in situ, and they hypothesized that these patients may develop post-cholecystectomy syndrome [7].
But even in patients with history of open cholecystectomy, the incidence is significant in our experience. Eight patients had undergone open cholecystectomy in our series among 12 patients, and 3 of them had multiple procedures in the past.
It is believed that laparoscopic subtotal cholecystectomy is a safe and definitive procedure during difficult situations [8]. Therefore, chances of retained stones in a gall bladder remnant or a cystic duct stump seem to increase in such scenarios.
In an ideal scenario, the cystic duct stump should not be more than 0.5 cm [9]. This necessitates division of the cystic duct close to the bile duct. In our series, stump length varied from 1.3 to 6 cm (Fig. 1). This clearly reiterates the need for careful dissection of cystic duct up to its junction with the common hepatic duct, before occlusion and division, in elective conditions.
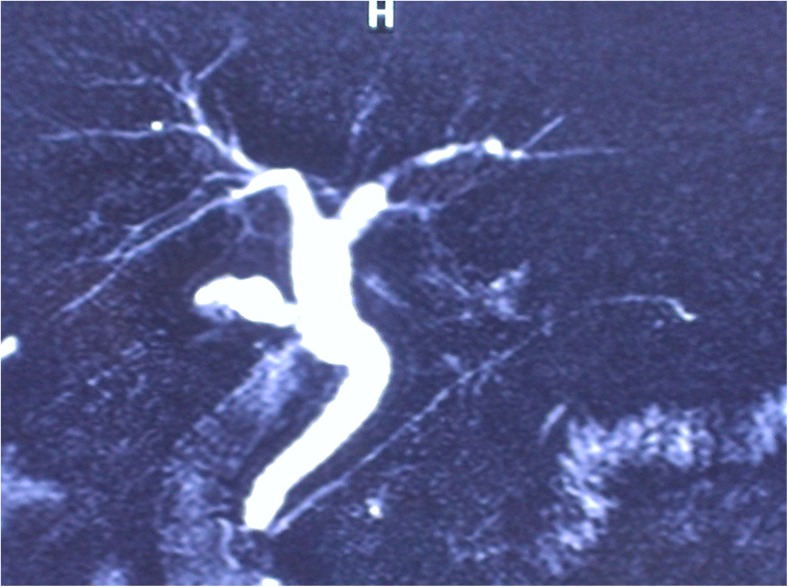
Fig. 1.
MRCP image of post-cholecystectomy gall bladder remnant
Palanivelu et al. found that MRCP was 92% accurate and ultrasound was only 60% accurate [10] in the evaluation of this entity. Ultrasonography has detected this condition in 8 out of 12 patients (66.67%) in our series. This finding was confirmed at the operation. MRCP has emerged as the optimal method for evaluating the biliary tree in these cases, especially if ultrasonography (USG) is inconclusive. It is non-invasive and helps in improved preoperative planning [11]. MRCP (when considered) has detected this condition in ten out ten patients of our series, and it was helpful during the surgery for identification of the cystic duct stump (Fig. 2).
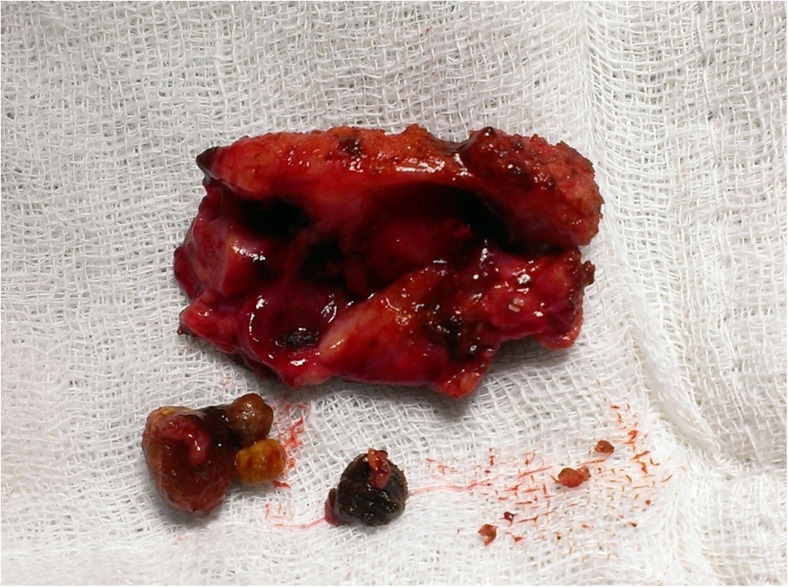
Fig. 2.
Specimen of gall bladder remnant with calculi, post-laparoscopic completion cholecystectomy
Traditionally, gall bladder or cystic duct remnant stone has been managed with open completion cholecystectomy. In view of the effects of the previous operation which results in considerable adhesions, performance of such procedures with laparoscopic approach was discouraged [12]. Now, there are increasing reports in the treatment of this problem with laparoscopic approach [13–17]. In our series, seven out of nine patients could be treated laparoscopically where it was tried. Dissection in most situations was difficult, so safety-first strategy should hold the key and conversion to open should not be considered a failure.
Alternative, strategies have been cited in the treatment of this condition, like extracorporeal shock wave lithotripsy [18] and ERCP [19]. But, these strategies are anecdotal. Such non-conventional modalities of treatment are largely confined to only a small subset of patients or those unfit for surgery.
Conclusion
Cystic duct stump and gall bladder remnant stone are not infrequent as it was believed earlier. Epigastric or right upper abdominal pain after cholecystectomy should prompt for a search for this condition if no other cause of the pain is found. MRCP should be considered in the algorithm of post-cholecystectomy upper abdominal pain if USG is inconclusive and it helps in surgical planning. Surgery is the treatment of choice. Laparoscopic approach now should be a part of the surgeon’s armamentarium in the successful treatment of this condition as this can be done safely in most of the patients.
Compliance with Ethical Standards
Conflict of Interest
The authors declare that they have no conflict of interest.
Contributor Information
Abhimanyu Kar, Phone: +917044067328, Email: mohulcar@gmail.com.
Sumit Gulati, Phone: +919903784717, Email: gulati_73@yahoo.co.uk.
Sudheer Mohammed, Phone: +919674227160, Email: drsudheermohammedm@yahoo.com.
Mithun Valiya Valappil, Phone: +919073128065, Email: mithunrv@yahoo.com.
Bhaviya Bhargavan Sarala, Phone: +919496367947, Email: bavya_bs@yahoo.com.
Supriyo Ghatak, Phone: +919874138687, Email: drsupriyo@yahoo.co.in.
Avik Bhattacharyya, Phone: +919674189179, Email: dr.avik@yahoo.com.
References
- 1.Lum YW, House MG. Hayanga AJ, et al. Postcholecystectomy syndrome in the laparoscopic era. J Laparoendosc Adv Surg Tech A. 2006;16(5):482–485. doi: 10.1089/lap.2006.16.482. [DOI] [PubMed] [Google Scholar]
- 2.Walsh RM, Chung RS, Grundfest-Broniatowski S. Incomplete excision of the gallbladder during laparoscopic cholecystectomy. Surg Endosc. 1995;9(1):67–70. doi: 10.1007/BF00187890. [DOI] [PubMed] [Google Scholar]
- 3.Shaw C, O’Hanlon DM, Fenlon HM, et al. Cystic duct remnant and the ‘post cholecystectomy syndrome’. Hepato-Gastroenterology. 2004;51(55):36–38. [PubMed] [Google Scholar]
- 4.Rozsos I, Magyarodi Z, Orban P. Cystic duct syndrome and minimally invasive surgery. Orv Hetil. 1997;138:2397–2401. [PubMed] [Google Scholar]
- 5.Florcken H. Gallenblasenregeneration mit steinrecidiv nachcholecystectomie. Deutsch Z Chir. 1912;113(5–6):604–605. doi: 10.1007/BF02800896. [DOI] [Google Scholar]
- 6.Sitenko VM, Nechai AI, Stukalov VV, et al. Large stump of the cystic duct. Vestn Khir Im I I Grek. 1976;116(2):56–59. [PubMed] [Google Scholar]
- 7.Keiler A, Pernegger C, Hornof R, et al. The cystic duct stump after laparoscopic cholecystectomy. Wien Klin Wochenschr. 1992;104:356–359. [PubMed] [Google Scholar]
- 8.Michalowski K, Bornman PC, Krige JE, Gallagher PJ, Terblanche J. Laparoscopic subtotal cholecystectomy in patients with complicated acute cholecystitis or fibrosis. Br J Surg. 1998;85(7):904–906. doi: 10.1046/j.1365-2168.1998.00749.x. [DOI] [PubMed] [Google Scholar]
- 9.Freud M, Djaldetti M, deVries A. Postcholecystectomy syndrome survey of 114 patients after biliary tract surgery. Gastroenterologia. 1960;93(5):288–293. doi: 10.1159/000202839. [DOI] [PubMed] [Google Scholar]
- 10.Palanivelu C, Rangarajan M, Jategaonkar PA, et al. Laparoscopic management of remnant cystic duct calculi: a retrospective study. Ann R Coll Surg Engl. 2009;91:25–29. doi: 10.1308/003588409X358980. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Girometti R, Brondani G, Cereser L, et al. Post-cholecystectomy syndrome: spectrum of biliary findings at magnetic resonance cholangiopancreatography. Br J Radiol. 2010;83:351–361. doi: 10.1259/bjr/99865290. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Rozsos I, Magyarodi Z, Orban P. The removal of cystic duct and gall bladder remnant by microlaparotomy. Acta Chir Hung. 1997;36:297–298. [PubMed] [Google Scholar]
- 13.Demetriades H, Pramateftakis MG, Kanellos I, Angelopoulos S, Mantzoros I, Betsis D. Retained gallbladder remnant after laparoscopic cholecystectomy. J Laparoendosc Adv Surg Tech A. 2008;18(2):276–279. doi: 10.1089/lap.2006.0210. [DOI] [PubMed] [Google Scholar]
- 14.Chowbey PK, Bandyopadhyay SK, Sharma A, Khullar R, Soni V, Baijal M. Laparoscopic reintervention for residual gallstone disease. Surg Laparosc Endosc Percutan Tech. 2003;13(1):31–35. doi: 10.1097/00129689-200302000-00007. [DOI] [PubMed] [Google Scholar]
- 15.Clemente G, Giuliante F, Cadeddu F, Nuzzo G. Laparoscopic removal of gall bladder remnant and long cystic stump. Endoscopy. 2001;33(9):814–815. [PubMed] [Google Scholar]
- 16.Li LB, Cai XJ, Mou YP, Wei Q. Reoperation of biliary tract by laparoscopy: experiences with 39 cases. World J Gastroenterol. 2008;14(19):3081–3084. doi: 10.3748/wjg.14.3081. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Tantia O, Jain M, Khanna S, et al. Post cholecystectomy syndrome: role of cystic duct stump and reintervention by laparoscopic surgery. J Minim Access Surg. 2008;4:71–75. doi: 10.4103/0972-9941.43090. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Benninger J, Rabenstein T, Farnbacher M, et al. Extracorporeal shockwave lithotripsy of gallstones in cystic duct remnants and Mirizzi syndrome. Gastrointest Endosc. 2004;60:454–459. doi: 10.1016/S0016-5107(04)01810-3. [DOI] [PubMed] [Google Scholar]
- 19.Shelton JH, Mallat DB. Endoscopic retrograde removal of gallbladder remnant calculus. Gastrointest Endosc. 2006;64(2):272–273. doi: 10.1016/j.gie.2006.01.042. [DOI] [PubMed] [Google Scholar]