Abstract
Background
The optimal medical regimen for managing hypertension during acute phase of lacunar infarcts has not yet been clarified in real world setting. The aim of this study was to evaluate blood pressure lowering regimens on neurological progression and clinical outcomes during the acute phase of lacunar infarcts.
Material/Methods
For this study, 411 patients with first-episode lacunar infarcts and hypertension within 24 hours of symptom onset were included. All patients received antihypertension therapies, with different regimens, as well as routine medication during first 7 days after onset. There were 6 proposed antihypertensive treatments: calcium channel blockers (CCB), angiotensin-converting enzyme inhibitors (ACEI), angiotensin receptor blockers (ARB), β-blocker (β-B), and diuretic drug (DD) alone or in combination. Neurological progression was defined as worsening by ≥1 point in the National Institute of Health Stroke Scale (NIHSS) for motor function. The outcome was assessed using the modified Rankin Scale (mRS): favorable outcome (mRS of 0–1) or unfavorable outcome (mRS 2–5).
Results
Logistic regression analysis showed that combination therapy with CCB, ACEI/ARB, and β-B exhibited the lowest risk of deterioration (OR=0.48, P=0.019) and unfavorable outcomes (OR=0.50, P=0.022). Similarly, combination therapy with CCB, ACEI/ARB, and DD exhibited lower risk of deterioration (OR=0.63, P=0.033) and unfavorable outcome (OR=0.77, P=0.042) at 3 months.
Conclusions
Rational blood pressure lowering was beneficial to the functional outcomes of patients during acute phase of lacunar infarcts, and combination therapy was better than mono-drug therapy.
MeSH Keywords: Blood Pressure; Outcome Assessment (Health Care); Stroke, Lacunar
Background
It is estimated that 1.5–2 million new diagnosed strokes occur each year in China and a third of patients with global mortality and morbidity due to stroke are from China [1]. Previous studies have shown that 65% to 70% of acute-phase strokes were accompanied with a sudden rise in blood pressure [1,2], and high blood pressure after stroke was considered to be closely related to poor outcomes [1,2]. Therefore, rational blood pressure management is very important to achieve better prognosis in patients with stroke.
Geeganage et al. [1] analyzed the association between baseline blood pressure and 10-day mortality and neurological deterioration in 1479 patients with cerebral infarction. They found that higher baseline blood pressure indicated poorer outcome. Several large-scale clinical trials have shown that early lowering of blood pressure in patients with ischemic stroke could reduce the harmful effects of high blood pressure. The CHHIPS (Controlling Hypertension and Hypotension Immediately Post-Stroke) study [1] found that antihypertensive treatment after acute stroke did not increase the incidence of serious adverse events, but mortality was halved at 3 months. The ACCESS (Acute Candesartan Cilexetil Therapy in Stroke Survivors) trial also demonstrated that antihypertensive treatment decreased 1-year mortality and incidences of severe cardiovascular and cerebrovascular events [1]. Altmann et al. reported that lacunar infarcts may be associated with higher blood pressure compared to non-lacunar infarcts [1]. Moreover, lacunar strokes are usually caused by hypertensive small-artery disease. Accordingly, antihypertensive treatment in acute lacunar infarcts might be feasible, and improve the prognosis of patients. The 2013 practice guideline for the management of arterial hypertension of the European Society of Hypertension (ESH) and the European Society of Cardiology (ESC) [1] pointed out that it was difficult to achieve satisfactory blood pressure lowering effects with mono-therapy, and thus, combination drugs might be better. However, the guideline did not clarify how to manage the various hypertension conditions and how to apply combination drug regimens. The present study evaluates the effectiveness of 6 blood pressure lowering regimens on neurological prognosis and clinical outcomes of patients with acute lacunar infarcts.
Material and Methods
Study design
This study was a real-world, single-center registered study about hospitalized stroke patients. Its protocol was carried out based on the content of Stroke Screening and Intervention Programmer launched by Ministry of Health of the People’s Republic of China [1] and was approved by the Institutional Review Board as well as the Ethics Committee of the First People’s Hospital of Lianyungang City (Approval No. LYLL 2012-06). All clinical investigations were conducted according to the principles expressed in the Declaration of Helsinki.
Participants
Patients presenting with an acute clinical lacunar syndrome who were admitted to the First People’s Hospital of Lianyungang City from January 2012 to December 2015 were consecutively included. The diagnosis of a lacunar syndrome was based upon the patients’ history and neurological examination. The inclusion criteria were: admission within 24 hours of stroke onset; clinical evidence of lacunar stroke such as pure motor hemiparesis, pure sensory stroke, sensorimotor stroke, ataxic hemiparesis, or dysarthria-clumsy hand syndrome [1]; and correlative lacunar lesion in the brain computed tomography (CT) or magnetic resonance imaging (MRI) scan.
Exclusion criteria were: severe mental disorders or dementia; severe systematic disease with estimated survival period <90 days; alanine aminotransferase (ALT) or aspartate aminotransferase (AST) >2.0 times that of the upper limit of normal or with history of severe liver disease; and creatinine clearance rate <30 mL/min or with history of severe kidney disease. Written informed consents were provided by the patients or legally authorized surrogates.
Data collection
The time of onset was defined as the final time when a patient remembered no loss of neurological function; if the stroke symptom was found just after waking, the onset of the stroke was set at the time of falling asleep. The mean blood pressure obtained from repeated measurements within 7 days after stroke was defined as systolic blood pressure (SBP) or diastolic blood pressure (DBP) of the acute phase of lacunar infarction. Dyslipidemia was defined when the low-density lipoprotein cholesterol (LDL-C) ≥4.14 mmol/L, and/or high-density lipoprotein cholesterol (HDL-C) <1.04 mmol/L, and/or triglyceride (TG) ≥2.26 mmol/L, or current treatment with lipid lowering drugs according to the Stroke Screening and Intervention Programmer launched in 2012. Atrial fibrillation was diagnosed according to the electrocardiogram (ECG) results on admission or during the hospitalization. Body mass index (BMI) was defined as weight in kilograms (kg) divided by height in meters squared. The diagnosis of diabetes was in accordance with 2010 guideline of Prevention and Management of Diabetes Mellitus in China [1]. Thrombolytic therapy was performed through intravenous route within 4.5 hours after symptom onset or intra-arterial route within 6 hours after stroke onset by infusion of recombinant tissue type plasminogen (rt-PA) or catheter-touch thrombolysis. Blood pressure was recorded in the supine position using the non-paralyzed arm every 4 hours, within 24 hours after onset, and twice a day (morning and evening) from days 2–7 or until discharge or death with Philips SureSigns VM6 monitors; mercury sphygmomanometer was homogeneous by pre-calibrated.
Treatment
Patients received standard level baseline treatment according to the Chinese guidelines for the diagnosis and therapy of patients with acute ischemic stroke [2]. Mono-drug therapy or combination drug therapy was applied according to the guideline of the Prevention and Management of Hypertension in Chinese Third Edition [3] and the medication history of the patients.
Follow-up and functional outcomes assessment
The National Institute of Health Stroke Scale (NIHSS) and modified Rankin Scale (mRS) were used to evaluate the neurological deficit and function, and were performed by experienced neurologists who were blinded to the clinical details. Neurological deterioration was defined as worsening by ≥1 point in the NIHSS for motor function [4]. The outcome was assessed using the mRS, divided into the criteria: favorable outcome (mRS of 0–1) or unfavorable outcome (mRS 2–5) [5].
Statistical analysis
One-way ANOVA assay or rank sum test was employed for continuous variables while chi-square test was employed for categorical variables to compare differences between important covariates for the study population for each outcome among treatment regimens. The odds ratios (ORs) and 95% confidence intervals (CIs) of Model I (adjustment of age, sex, past history of coronary heart diseases, hypertension, and diabetes), Model II (adjustment of mRS, NIHSS, location of infarction lesion, cerebral infarction volume, and thrombolytic therapy on the basis of Model I), and Model III (adjustment of baseline SBP, DBP, pulse, homocysteine, fasting blood glucose, and estimated glomerular filtration rate on the basis of Model I and Model II) for neurological deterioration and unfavorable outcome with different blood lowering regimen were estimated by logistic regression analysis. All statistical analyses were performed using SPSS (version 16.0.1-ISO 1CD) software program. P<0.05 was considered as statistically significance.
Results
Characteristic of the included patients
We recruited 574 patients who presented with lacunar syndrome; 163 of these patients were excluded according to the study exclusion criteria (Figure 1). Of the 411 patients who met the inclusion criteria, the NIHSS and mRS scores at 3 months after stroke were obtained for 399 patients. Table 1 shows the baseline characteristics of all the patients included in the 6 different treatment groups. There were no significant differences in baseline demographic and clinical features between the 6 groups.
Figure 1.
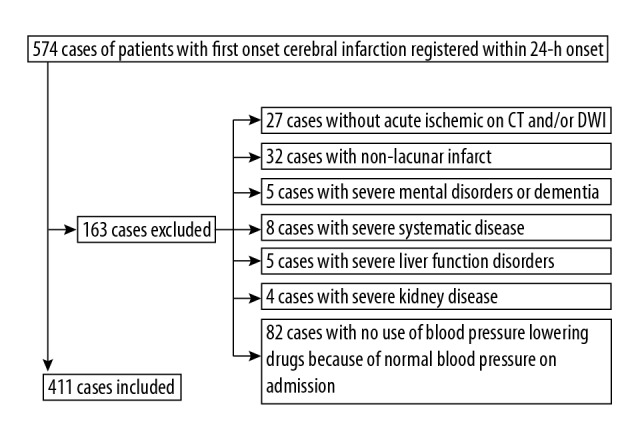
Flow diagram of patients.
Table 1.
Characteristics of the patients.
| Indexes N (%) |
R1 68 (19.03) |
R2 61 (14.88) |
R3 72 (16.26) |
R4 65 (18.69) |
R5 69 (16.61) |
R6 64 (14.52) |
P value |
|---|---|---|---|---|---|---|---|
| Age, M ±SD years | 57.6±9.3 | 58.5±10.1 | 63.8±12.4 | 61.7±9.9 | 65.2±12.4 | 62.6±11.6 | 0.413 |
| Male, n (%) | 38 (55.88) | 37 (60.66) | 37 (51.39) | 33 (50.78) | 41 (59.42) | 35 (54.69) | 0.823 |
| BMI, Kg/M2 | 23.9±4.2 | 25.7±4.6 | 26.8±5.6 | 23.7±4.3 | 26.1±5.1 | 23.8±4.4 | 0.516 |
| hypertension, n (%) | 45 (66.18) | 43 (70.49) | 53 (73.61) | 48 (73.85) | 46 (66.67) | 48 (75.00) | 0.793 |
| diabetes, n (%) | 16 (23.53) | 13 (21.31) | 20 (27.78) | 18 (27.69) | 13 (18.84) | 16 (0.25) | 0.801 |
| dyslipidemia, n (%) | 27 (39.71) | 22 (36.07) | 29 (40.28) | 28 (43.08) | 31 (44.93) | 23 (36.94) | 0.877 |
| CAD, n (%) | 15 (22.06) | 11 (18.03) | 16 (22.22) | 12 (18.46) | 17 (24.64) | 16 (25.00) | 0.895 |
| mRS, M ±SD scores | 1.8±1.1 | 2.0±1.3 | 1.7±1.1 | 1.8±1.2 | 1.9±1.2 | 1.7±1.1 | 0.685 |
| NIHSS, M ±SD scores | 3.6±2.2 | 3.8±2.3 | 3.4±2.2 | 3.8±2.4 | 3.3±1.9 | 3.5±2.1 | 0.447 |
| SBP, M ±SD mmHg | 156.7±26.3 | 151.8±23.2 | 158.0±27.7 | 154.8±25.1 | 153.9±23.6 | 155.8±25.9 | 0.351 |
| DBP, M ±SD mmHg | 108.5±19.5 | 103.8±16.2 | 110.7±21.9 | 106.2±18.1 | 109.6±19.4 | 113.5±22.6 | 0.496 |
| Pulse, M ±SD/Min | 76.6±11.3 | 80.5±11.9 | 73.6±9.7 | 75.9±9.7 | 74.2±9.3 | 71.2±8.8 | 0.383 |
| TG, M ±SD mmol/L | 1.96±1.57 | 1.74±1.51 | 2.15±1.66 | 2.17±1.69 | 1.88±1.58 | 1.65±1.47 | 0.261 |
| HDL-C, M ±SD mmol/L | 1.35±0.32 | 1.56±0.37 | 1.36±0.31 | 1.22±0.28 | 1.48±1.35 | 1.73±1.46 | 0.182 |
| LDL-C, M ±SD mmol/L | 3.25±1.14 | 3.06±1.04 | 2.96±1.01 | 3.38±1.22 | 3.37±1.23 | 3.19±1.13 | 0.545 |
| Hcy, M ±SD umol/l | 11.43±2.86 | 11.68±2.95 | 14.11±3.16 | 10.02±2.85 | 9.76±2.78 | 10.33±2.86 | 0.262 |
| FBG, M ±SD mmol/L | 5.83±2.24 | 5.55±2.08 | 5.31±1.92 | 5.48±1.97 | 5.85±2.21 | 5.66±2.14 | 0.513 |
| eGFR, M ±SD ml/min/1.73 m2 | 96.30±21.6 | 92.91±18.3 | 88.12±18.0 | 96.09±21.25 | 98.04±22.38 | 91.47±18.0 | 0.411 |
mRS – modified Rankin Scale; NIHSS – National Institutes of Health Stroke Scale; SBP – systolic blood pressure; DBP – diastolic blood pressure; TG – triglycerides; HDL-C – high density lipoprotein cholesterol; LDL-C – low density lipoprotein cholesterol; Hcy – homocysteine; FBG – fasting blood glucose; eGFR – estimated glomerular filtration rate; R1 – calcium channel blocker (CCB); R2 – angiotensin-converting enzyme inhibitors(ACEI)/angiotensin receptor blockers(ARB); R3 – CCB+ACEI/ARB; R4 – CCB+ACEI/ARB+β-blocker(β-B); R5 – CCB+ACEI/ARB+ diuretic drug (DD); R6 – other anti-hypertension drug regimens.
Blood pressure lowering regimens within 7 days after onset
Within 7 days after symptom onset, oral medication of blood pressure lowering regimens were divided into 6 groups: R1 group received calcium channel blocker (CCB); R2 group received angiotensin-converting enzyme inhibitors (ACEI)/angiotensin receptor blockers (ARB); R3 group received CCB+ACEI/ARB; R4 group received CCB+ACEI/ARB+β-blocker (β-B); R5 group received CCB+ACEI/ARB+diuretic drug (DD); R6 group received other antihypertension drug regimens. As necessary, the regimens of antihypertension therapy of each group were changed after 7 days.
The relationship between blood pressure lowering regimen and neurological outcome
Table 2 shows NIHSS and mRS scores at 24 hours and 3 months for the 6 different blood pressure lowering regimen groups. The scores for NIHSS and mRS at 3 months were significantly lower than at 24 hours. As shown in Table 3, the CCB regimen was used as reference (OR was identified as 1.00). Among all the 6 groups, combination therapy with CCB, ACEI/ARB, and β-B (R4 group) exhibited the lowest probability of neurological deterioration (OR=0.48, P=0.019) and unfavorable outcome at 3 months (OR=0.50, P=0.022). Similarly, combination therapy with CCB, ACEI/ARB, and DD (group R5) exhibited lower probability of neurological deterioration (OR=0.63, P=0.033) and unfavorable outcome at 3 months (OR=0.77, P=0.042). However, there were no significant differences in neurological deterioration and unfavorable outcome between the R4 group and the R5 group (P>0.05).
Table 2.
NIHSS and mRS scores in the 6 blood pressure lowering regimens.
| Regimens | Indexes | 24 h | 3 M |
|---|---|---|---|
| R1 (n=137) |
NIHSS, M±SD scores | 3.6±2.1 | 1.3±1.1* |
| mRS, M±SD scores | 1.8±1.2 | 1.4±0.7* | |
| R2 (n=102) |
NIHSS, M±SD scores | 3.8±1.9 | 1.3±1.2# |
| mRS, M±SD scores | 1.8±1.1 | 1.3±0.7* | |
| R3 (n=91) |
NIHSS, M±SD scores | 3.8±2.0 | 1.4±1.2* |
| mRS, M±SD scores | 1.6±0.9 | 1.2±0.6* | |
| R4 (n=104) |
NIHSS, M±SD scores | 3.7±2.2 | 1.1±0.9# |
| mRS, M±SD scores | 1.7±1.1 | 0.8±0.6* | |
| R5 (n=82) |
NIHSS, M±SD scores | 3.6±2.1 | 1.1±1.0# |
| mRS, M±SD scores | 1.9±1.2 | 0.9±0.8* | |
| R6 (n=137) |
NIHSS, M±SD scores | 3.5±1.7 | 1.5±1.2* |
| mRS, M±SD scores | 1.7±1.2 | 1.3±0.9* |
mRS – modified Rankin Scale; NIHSS – National Institutes of Health Stroke Scale; R1 – calcium channel blocker (CCB); R2 – angiotensin-converting enzyme inhibitors(ACEI)/angiotensin receptor blockers(ARB); R3 – CCB+ACEI/ARB; R4 – CCB+ACEI/ARB+β-blocker(β-B); R5 – CCB+ACEI/ARB+diuretic drug (DD); R6 – other anti-hypertension drug regimens.
Compared with 24 h, P<0.05;
compared with 24 h, P<0.01.
Table 3.
The relationship between blood pressure lowering regimen and neurological prognosis at 3 month of the onset.
| Models | Indexes | R1 | R2 | R3 | R4 | R5 | R6 |
|---|---|---|---|---|---|---|---|
| Neurological deterioration | |||||||
| Model I | Risk, n(%) | 18 (26.45) | 13 (21.31) | 15(20.83) | 7(10.78) | 9(13.04) | 18 (28.13) |
| OR (95%CI) | 1.00 | 1.08 (0.92~1.33) | 0.83 (0.71~1.28) | 0.53 (0.44~0.65) | 0.64 (0.57~0.78) | 1.03 (0.65~1.22) | |
| P value | Reference | 0.878 | 0.651 | 0.016 | 0.024 | 0.764 | |
| Model II | OR (95%CI) | 1.00 | 0.91 (0.86~1.18) | 0.80 (0.74~1.06) | 0.57 (0.42~0.66) | 0.69 (0.45~0.81) | 1.08 (0.70~1.12) |
| P value | Reference | 0.902 | 0.585 | 0.021 | 0.036 | 0.799 | |
| Model III | OR (95%CI) | 1.00 | 0.95 (0.82~1.18) | 0.76 (0.60~1.15) | 0.48 (0.32~0.57) | 0.63 (0.55~0.79) | 1.05 (0.69~1.22) |
| P value | Reference | 0.907 | 0.613 | 0.019 | 0.033 | 0.748 | |
| Poor outcome | |||||||
| Model I | Risk n, (%) | 23 (33.82) | 21 (34.43) | 21/72 (29.17) | 11 (16.92) | 13 (18.84) | 24 (37.50) |
| OR (95%CI) | 1.00 | 1.12 (0.93~1.43) | 0.85 (0.73~1.09) | 0.58 (0.48~0.70) | 0.68 (0.51~0.79) | 1.52 (1.37~1.77) | |
| P value | Reference | 0..807 | 0.919 | 0.026 | 0.041 | 0.837 | |
| Model II | OR (95%CI) | 1.00 | 0.88 (0.70~1.26) | 0.81 (0.63~1.15) | 0.67 (0.48~0.83) | 0.79 (0.63~0.94) | 1.49 (1.27~1.82) |
| P value | Reference | 0.908 | 0.558 | 0.026 | 0.087 | 0.832 | |
| Model III | OR (95%CI) | 1.00 | 0.82 (0.76~1.21) | 0.75 (0.60~0.88) | 0.50 (0.36~0.75) | 0.77 (0.53~0.92) | 1.57 (1.26~1.79) |
| P value | Reference | 0.840 | 0.353 | 0.022 | 0.042 | 0.794 | |
R1 – calcium channel blocker (CCB); R2 – angiotensin-converting enzyme inhibitors (ACEI)/angiotensin receptor blockers(ARB); R3 – CCB+ACEI/ARB; R4 – CCB+ACEI/ARB+β-blocker(β-B); R5 – CCB+ACEI/ARB+diuretic drug (DD); R6 – other anti-hypertension drugs regimens. Model I – sex-old-adjusted; Model II – plus the adjustment of mRS, NIHSS – location of infarction lesion (anterior or posterior circulation), cerebral infarction volume and thrombolytic therapy (yes or no) on the basis of Model I; Model III – plus the adjustment of baseline SBP, DBP, pulse, Hcy, FBG and eGFR on the basis of Model I and Model II. OR – odds ratios; 95% CI – 95% confidence intervals.
Discussion
This study was designed as a real-world study. The blood pressure lowering regimens were dependent on the patients’ conditions and choices. It was a non-randomized and open trial study which more closely represented a real medical situation, and thus the results were considered more reliable.
It has been reported that antihypertension treatment in acute stroke may be beneficial. Geeganage et al. [6] performed a meta-analysis on the association between blood pressure lowering treatment and prognosis in stroke patients. They found a decreased trend in mortality and morbidity after appropriate blood pressure lowering. After analysis of the QUEST data, Heeley et al. [7] found that CCB, ACEI/ARB, β-B, and DD could decrease the mortality rate at 12-month after stroke, indicating that early application of blood pressure lowering drug was associated with improved stroke outcomes.
However, there are some controversies about blood pressure lowering treatment in acute stroke. One of the main concerns is that antihypertension therapy might cause hypoperfusion in cerebral tissue and exacerbate ischemia, especially in patients with severe cerebral artery stenosis. The SCAST (Scandinavian Candesartan Acute Stroke Trial) suggested that blood pressure lowering treatment with candesartan was not beneficial in patients with acute stroke and raised blood pressure, and that antihypertension therapy could even result in harmful effects [8]. The COSSACS (Continue or Stop post-Stroke Antihypertensives Collaborative Study) demonstrated that continuation of antihypertensive drugs did not decrease mortality or dependency, and also that lower blood pressure levels in those who continued blood pressure lowering treatment were not related to an increase in adverse events [9]. However, there are few studies on the effects of antihypertension on lacunar stroke. Therefore, we chose patients with lacunar infarcts to be the study focus of antihypertension treatment, which was a different approach than previous research. Lacunar stroke is usually caused by hypertensive small-artery disease, and blood pressure lowering treatment has smaller effects on perfusion of ischemic tissue. Therefore, antihypertensive treatment in those patients may be safer than other types of stroke, especially stroke associated with large-artery atherosclerosis, and thus would more likely to get optimistic results.
In our present study, we evaluated the effects of different blood pressure lowering regimens on acute stroke; we used the CCB regimen as reference when analyzing the relationship between combination therapy and functional outcomes. Our results showed that combination therapy with CCB, ACEI/ARB and β-B (R4 group) exhibited the lowest risk of neurological functional deterioration and unfavorable outcomes. A secondary advantage was seen in CCB, ACEI/ARB, and DD regimen (R5 group), but there were no significant differences between the 2 regimens. Corrao et al. [10] also demonstrated that combination therapy exerted better blood pressure lowering effect than mono-drug therapy. Schuchert et al. [11] suggested that combination drug therapy with blood pressure lowering drugs exhibited advantages of rapid blood pressure lowering and good tolerance. Studies conducted by Pall et al. [12] and Toth et al. [13] showed that the advantages of combination therapy were based on the complementary mechanism of different drugs, which could result in decreased adverse reaction and increased blood pressure lowering effect.
There are several reasons for the good functional outcomes achieved in combination therapy with CCB, ACEI/ARB, and β-B. ACEI/ARB decreases vasoconstrictor effect and reduces volume load by blocking renal artery stenosis. β-B undermines the elevating blood pressure effect of sympathetic nervous system, drops heart rate, and decreases cardiac output. CCB directly expands blood vessels by inhibiting calcium channels on vascular smooth muscle cells. Therefore, when CCB, ACEI/ARB, and β-B were used in combination, there may have been synergistic antihypertension actions, and adverse feedback effects caused by different medicines may have been attenuated. Moreover, calcium antagonist is also effective for cerebral protection [14] and for blood pressure variability reduction during acute phase of ischemic stroke [15], and thus may have been beneficial for neurological function recovery. Accordingly, combination therapy is recommended as a priority.
There were some limitations in our study. First, this study was a real-world study, and blood pressure lowering regimens were dependent on the patients’ conditions and choices. Therefore, selection bias was inevitable in this study design. Second, the blood pressure measurement was performed using a manual method and not continuous blood pressure monitoring during hospitalization. Measurement error could result in overestimation or underestimation of the association between blood pressure and functional outcomes. Moreover, although most of the lacunar strokes were caused by small-artery disease, there were still a fraction of lacunar strokes that were related to cerebral large-artery stenosis, which may result in worse outcomes and increase the proportion of functional deterioration, and we did not exclude those strokes. Additionally, patient number was very limited in this study.
Conclusions
This study showed that rational blood pressure lowering was beneficial to the outcomes of patients during acute phases of lacunar strokes, and combination therapy was better than mono-drug therapy.
Acknowledgement
This study was supported by the Health Bureau of Lianyungang City, the Health Bureau of Ganyu County, the People’s Hospital of Xinpu District of Lianyungang, the Health Service Center of Tashan Town of Ganyu County, the Health Service Center of Banzhuang Town of Ganyu County, the Health Service Center of Haitou Town of Ganyu County during research implementation, researcher training, and coordination between researchers and patients.
Footnotes
Conflict of interest
None.
Source of support: This study was funded by China Postdoctoral Science Foundation funded project (2016M601759), Medical Scientific Specific Fund of Bureau of Science and Technology (BL2014062)
References
- 1.Zhao D, Liu J, Wang W, et al. Epidemiological transition of stroke in China: Twenty-one-year observational study from the Sino-Monica-Beijing project. Stroke. 2008;39:1668–74. doi: 10.1161/STROKEAHA.107.502807. [DOI] [PubMed] [Google Scholar]
- 2.Sandset EC, Murray GD, Bath PM, et al. Relation between change in blood pressure in acute stroke and risk of early adverse events and poor outcome. Stroke. 2012;43:2108–14. doi: 10.1161/STROKEAHA.111.647362. [DOI] [PubMed] [Google Scholar]
- 3.Hankey GJ. Lowering blood pressure in acute stroke: The SCAST trial. Lancet. 2011;377:696–98. doi: 10.1016/S0140-6736(11)60163-3. [DOI] [PubMed] [Google Scholar]
- 4.Sandset EC. Blood pressure in acute stroke. Lancet Neurol. 2014;13:342–43. doi: 10.1016/S1474-4422(14)70042-0. [DOI] [PubMed] [Google Scholar]
- 5.Kang J, Ko Y, Park JH, et al. Effect of blood pressure on 3-month functional outcome in the subacute stage of ischemic stroke. Neurology. 2012;20:2018–24. doi: 10.1212/WNL.0b013e3182749eb8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Geeganage C, Tracy M, England T, et al. Relationship between baseline blood pressure parameters (including mean pressure, pulse pressure,and variability) and early outcome after stroke: Data from the Tinzaparin in Acute Ischemic Trial (TAIST) Stroke. 2011;42:491–93. doi: 10.1161/STROKEAHA.110.596163. [DOI] [PubMed] [Google Scholar]
- 7.Potter JF, Robinson TG, Ford GA, et al. Controlling hypertension and hypotension immediately post-stroke (CHHIPS): A randomised, placebo-controlled, double-blind pilot trial. Lancet Neurol. 2009;8:48–56. doi: 10.1016/S1474-4422(08)70263-1. [DOI] [PubMed] [Google Scholar]
- 8.Schrader J, Lüders S, Kulschewski A, et al. Acute Candesartan Cilexetil Therapy in Stroke Survivors Study Group. The ACCESS Study: Evaluation of acute candesartan cilexetil therapy in stroke survivors. Stroke. 2003;34:1699–703. doi: 10.1161/01.STR.0000075777.18006.89. [DOI] [PubMed] [Google Scholar]
- 9.Altmann M, Thommessen B, Rønning OM, et al. Blood pressure differences between patients with lacunar and nonlacunar infarcts. Brain Behav. 2015;5(8):e00353. doi: 10.1002/brb3.353. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.ESH/ESC Task Force for the Management of Arterial Hypertension. 2013 Practice guidelines for the management of arterial hypertension of the European Society of Hypertension (ESH) and the European Society of Cardiology (ESC). ESH/ESC Task Force for the Management of Arterial Hypertension. J Hypertens. 2013;31:1925–38. doi: 10.1097/HJH.0b013e328364ca4c. [DOI] [PubMed] [Google Scholar]
- 11.National Health and Family Planning Commission of China. [Technical specification of stroke screening, prevention and treatment]. Chinese Journal of Neurology. 2014;47(3):199–203. [in Chinese] [Google Scholar]
- 12.Fisher M, Minematsu K. Lacunar stroke: Diagnosis, evaluation, and management. Heart Dis Stroke. 1992;1:353–56. [PubMed] [Google Scholar]
- 13.Chinese Diabetes Society. [Guideline of prevention and management for type 2 diabetes in China]. Chinese Journal of Diabetes. 2012;20:S1–36. [in Chinese] [Google Scholar]
- 14.Liu M, Zhang S, Aao M, et al. 2010 Chinese guidelines for the diagnosis and treatment of patients with acute ischemic stroke. Chin J Front Med Sci. 2010;2:50–59. [Google Scholar]
- 15.Writing Group of 2010 Chinese Guidelines for the Management of Hypertension. [2010 Chinese guidelines for the management of hypertension]. Chinese Journal of Cardiology. 2011;39:579–616. [in Chinese] [PubMed] [Google Scholar]
- 16.Audebert HJ, Pellkofer TS, Wimmer ML, Haberl RL. Progression in lacunar stroke is related to elevated acute phase parameters. Eur Neurol. 2004;51(3):125–31. doi: 10.1159/000077012. [DOI] [PubMed] [Google Scholar]
- 17.Kim JG, Choi H, Sohn SY, et al. Transient ischemic attacks preceding acute lacunar infarction. Eur Neurol. 2016;76(5–6):278–83. doi: 10.1159/000452487. [DOI] [PubMed] [Google Scholar]
- 18.Geeganage CM, Bath PM. Relationship between therapeutic changes in blood pressure and outcomes in acute stroke: A metaregression. Hypertension. 2009;54(4):775–81. doi: 10.1161/HYPERTENSIONAHA.109.133538. [DOI] [PubMed] [Google Scholar]
- 19.Heeley EL, Wei JW, Wang JG, et al. China QUEST Investigators. Comparative effects of antihypertensive drugs on stroke outcome in China. Int J Stroke. 2014;9(Suppl A100):113–18. doi: 10.1111/ijs.12330. [DOI] [PubMed] [Google Scholar]
- 20.Sandset EC, Bath PM, Boysen G, et al. SCAST Study Group. The angiotensin-receptor blocker candesartan for treatment of acute stroke (SCAST): A randomised, placebo-controlled, double-blind trial. Lancet. 2011;377(9767):741–50. doi: 10.1016/S0140-6736(11)60104-9. [DOI] [PubMed] [Google Scholar]
- 21.Robinson TG, Potter JF, Ford GA, et al. COSSACS Investigators. Effects of antihypertensive treatment after acute stroke in the Continue or Stop Post-Stroke Antihypertensives Collaborative Study (COSSACS): A prospective, randomised, open, blinded-endpoint trial. Lancet Neurol. 2010;9(8):767–75. doi: 10.1016/S1474-4422(10)70163-0. [DOI] [PubMed] [Google Scholar]
- 22.Corrao G, Parodi A, Zambon A, et al. Reduced discontinuation of antihypertensive treatment by two-drug combination as first step. Evidence from daily life practice. J Hypertens. 2010;28:134–45. doi: 10.1097/HJH.0b013e328339f9fa. [DOI] [PubMed] [Google Scholar]
- 23.Schuchert A. Present-day treatment of arterial hypertension. Med Monatsschr Pharm. 2010;33:469–70. [PubMed] [Google Scholar]
- 24.Páll D, Szántó I, Szabó Z. Triple combination therapy in hypertension: The antihypertensive efficacy of treatment with perindopril, amlodipine, and indapamide SR. Clin Drug Investig. 2014;34:701–8. doi: 10.1007/s40261-014-0223-0. [DOI] [PubMed] [Google Scholar]
- 25.Tóth K PIANIST Investigators. Antihypertensive efficacy of triple combination perindopril/indapamide plus amlodipine in high-risk hypertensives: results of the PIANIST study (Perindopril-Indapamide plus AmlodipiNe in high rISk hyperTensive patients) Am J Cardiovasc Drugs. 2014;14:137–45. doi: 10.1007/s40256-014-0067-2. [DOI] [PubMed] [Google Scholar]
- 26.Tocci G, Battistoni A, Passerini J, et al. Calcium channel blockers and hypertension. J Cardiovasc Pharmacol Ther. 2015;20:121–30. doi: 10.1177/1074248414555403. [DOI] [PubMed] [Google Scholar]
- 27.Hansen TW, Thijs L, Li Y, et al. International Database on Ambulatory Blood Pressure in Relation to Cardiovascular Outcomes Investigators. Prognostic value of reading-to-reading blood pressure variability over 24 hours in 8938 subjects from 11 populations. Hypertension. 2010;55:1049–57. doi: 10.1161/HYPERTENSIONAHA.109.140798. [DOI] [PubMed] [Google Scholar]


