Abstract
Objective
Quality of life (QoL) has so far seldom been taken into account by default in decision‐making for surgical indication in thyroid surgery. Therefore, we compared pre‐ and postoperative QoL of patients using the EuroQoL‐5D (EQ‐5D) questionnaire. The influence of certain socio‐economic factors on QoL as a second end‐point was considered.
Design
Prospective cohort study.
Patients
About 153 patients with euthyroid symptomatic benign goitre after hemi‐ and total thyroidectomy (follow‐up 83.6%) have been included.
Measurements
The EQ‐5D questionnaire was used prior to and 1 year after surgery. In addition, a questionnaire for assessment of socio‐economic status was collected.
Results
For n = 90 (n = 67 female, n = 23 male), total thyroidectomy (TT) and, for n = 63 (n = 45 female, n = 18 male), hemithyroidectomy (HT) were performed. None permanent dysfunction of the vocal cord was recorded. Transient symptomatic hypocalcaemia was detected in 9% of the thyroidectomy group (8/90 patients). At follow‐up, 86% of patients showed either no change or improved QoL. About 14% of patients complained of deteriorated QoL, regardless of the extent of surgery. Socio‐economic factors did not influence postoperative QoL.
Conclusions
Results indicate that in pre‐operative consultation of patients with benign goitre, the improvement of QoL should be taken into account for decision‐making in cases of ambiguous surgical indication. Contrary to current discussions that too much thyroid surgery is performed in Germany, we can recommend presenting surgery as an equivalent option to watchful waiting as QoL is at least preserved or improved. The extension of the resection should, however, be decided individually.
Keywords: EQ‐5D, health‐related quality of life, hemithyroidectomy, patient‐reported outcome, PRO, QoL, total thyroidectomy
We compared pre‐ and postoperative quality of life (QoL) of patients using the EuroQoL‐5D questionnaire and the influence of certain socio‐economic factors on QoL. Results indicate that in preoperative consultation of patients with benign goiter, the improvement of QoL should be taken into account for decision‐making in cases of ambiguous surgical indication. We can recommend presenting surgery as an equivalent option to watchful waiting as QoL is at least preserved or improved.

1. INTRODUCTION
The high amount of thyroid operations in Germany compared with other nations has heated up an ongoing debate about the indications for operation especially for benign nontoxic thyroid diseases. Although the amount of thyroid operations has decreased in the last years to about 80.000 per year,1 Germany still shows three to six times more thyroid operations compared with the US, England or Scandinavian countries.2, 3, 4
If a goitre therapy is necessary due to, that is local compression symptoms such as dysphagia or respiratory impairment,5, 6 numerous therapeutic options are available. These include surgery, radioiodine and ultrasound‐guided interventional ablation.7, 8, 9, 10 The best therapeutic method(s) should be selected individually, and according to patient's wishes, but for large goitres compromising and displacing trachea or oesophagus, surgery should be the first and radioiodine the second choice.11, 12
The options for thyroid surgery range from enucleation of nodules, hemithyroidectomy, subtotal resection to total thyroidectomy.13 In recent years, even in large goitres, extensive surgery can be performed, without an accompanying increased risk of permanent hypoparathyroidism or recurrent laryngeal nerve (RLN) injury due to new technical devices and growing operative experience.14 However, with regard to the above‐mentioned risks, which could be underestimated, there is also a common agreement for individualizing the extent of resection instead of performing a routine total thyroidectomy.15 In summary, the indication and the extent of surgery remain an individual decision balancing patients' symptoms, operative morbidity and possibility of re‐operation for recurrent goitre, but the change in quality of life (QoL) does not find significant consideration in the decision‐making for or against an operation or alternative therapeutic methods.
There is a consensus that QoL is negatively influenced by thyroid dysfunction, both in hyperthyroidism and hypothyroidism, and one of the main aims in the therapy of thyroid dysfunction should be at least preserving or, ideally, improving QoL.16, 17, 18, 19, 20 The measurement of QoL is an important tool for assessment of the therapy and patients' overall outcome. It can be measured by two types of questionnaires: disease‐specific and generic questionnaires. Both are important in clinical trails as they often provide complimentary information.21
Surgery seems to improve postoperative QoL in patients with benign goitres using generic and disease‐specific questionnaires.22, 23, 24, 25 For instance, the Thyroid Patient‐Reported Outcome (ThyPRO), a disease‐specific questionnaire, has been recommended for use in patients with benign thyroid diseases,26 but a German version of this questionnaire has not been validated yet. To our knowledge, a disease‐specific questionnaire for nontoxic benign thyroid diseases in German language has not been developed until now. For this reason, generic QoL questionnaires are used for determining QoL in nontoxic goitres in German‐speaking countries.
It is well known that socio‐economic factors influence individual QoL. Persons belonging to a lower social class show a minor life satisfaction, higher subjective complaints and a poor state of health in general.27 In thyroid cancer, female sex, young age at diagnosis and lower educational attainment were predictive of decreased QoL.28 In children with well‐differentiated thyroid cancer, lower family income and lack of insurance caused a delay in diagnosis and therapy. These patients also presented with higher stage diseases.29
Therefore, we aimed to investigate the impact of thyroid surgery (hemi‐ and total thyroidectomy) for benign nontoxic goitre on quality of life by a generic questionnaire (EuroQoL‐5D), while taking into account various socio‐economic factors.
2. MATERIALS AND METHODS
Between January 2010 and February 2011, n = 190 consecutive patients with euthyroid goitre were included in our prospective longitudinal study. Therefore, inclusion criteria were normal TSH, fT3 and fT4 levels in the absence of autoimmune antibodies, such as TPO antibodies. The study was approved by the ethics commission of the University of Oldenburg (004/2016). The patients were informed in detail and gave their written consent for participation in the study.
2.1. General treatment/Surgical procedure
Either hemi‐ or total thyroidectomy was performed because of symptomatic goitre or/and malignant suspect nodules by pre‐operative sonomorphological parameters or Bethesda III‐V results of the fine‐needle aspiration cytologie. The operations were performed by four experienced surgeons, each with at least 50 thyroid operations per year in our surgical department.
In all patients, the recurrent laryngeal nerve (RLN) was monitored intraoperatively and the parathyroid gland vascularization was obtained.10 Postoperatively, a routine monitoring on the intermediate care unit was performed for 24 hours. All patients were discharged between 3 and 5 days after receiving the final histological examination of the thyroid. Routinely, all patients after total thyroidectomy received 1.5 µg levothyroxine/kg bodyweight followed by control of the hormonal status by their general practitioner after approximately 6 weeks.
2.2. Study design
At least 24 hours prior to operation, each patient completed the EuroQoL‐5D (EQ‐5D) questionnaire. The EQ‐5D‐3L essentially consists of two parts: the EQ‐5D descriptive system and the EQ visual analogue scale (EQ VAS).
The EQ VAS records the patient's self‐rated health on a vertical VAS where the end‐points are labelled ‘Best imaginable health state (100)’ and ‘Worst imaginable health state (0)’.
The EQ‐5D system comprises five dimensions: mobility, self‐care, usual activities, pain/discomfort and anxiety/depression. Each dimension has three levels: no problems, some problems and extreme problems. The patients' statement was converted into a 1‐digit number that expressed the level selected for that dimension. The digits for the five dimensions have been combined into a 5‐digit number that described the patient's health state and were converted by the time trade‐off (TTO) valuation technique for inter‐ and intra‐individual comparison. The EQ‐5D index was thus calculated in accordance with the appropriate instructions and calculated pre‐operatively and 1 year postoperatively for each patient.30, 31
A positive difference indicates a positive change in QoL 1 year after surgery in comparison with QoL before surgery; a negative difference is indicative for a deterioration of QoL. In this way, the change in QoL for each patient was detected.
In addition, a second self‐developed questionnaire for assessment of the socio‐economic status was collected. It included annual salary income, family status, school education and employment status. One year after the operation, the patients were asked to answer the same questionnaires in writing again.
2.3. Statistical analysis
Data collection was performed using Microsoft Excel, Version 2007 Professional. For statistical analyses, the statistical program ‘r’ in version R1.5.1. was used. Continuous data were described by calculating mean, standard deviation, median, minimum and maximum. A Wilcoxon one sample signed‐rank test with reference zero was performed to evaluate improvement in overall QoL. To evaluate pre‐ and postoperative differences in the five dimensions of the EQ‐5D, Wilcoxon's signed‐rank tests for paired comparison were used. Univariate ANCOVA was performed to test the influence of socio‐economic factors on QoL. Since we could not use empirical values for an a priori power calculation, a post hoc power analysis was carried out with G*Power for all statistical tests. A P value ≤.05 was considered as significant. Bonferroni‐Holm correction for multiple testing was implemented where necessary.
3. RESULTS
3.1. Distribution of patients
A total of 190 patients were included in the study. N = 7 patients were excluded because malignant disease was detected at histological examination. N = 30 patients were lost of follow‐up due to incorrectly filled‐out questionnaires or due to inaccessibility. The 1‐year follow‐up was 83.6% (153/183 patients). The sex ratio was 26.8% male (n = 41) and 73.2% female (n = 112). For n = 90 (n = 67 female, n = 23 male), a total thyroidectomy (TT) and, for n = 63 (n = 45 female, n = 18 male), a hemithyroidectomy (HT) were performed. A subgroup analysis with respect to gender and type of surgery was performed.
3.2. Surgical complications
Postoperative transient symptomatic hypocalcaemia was seen only in the TT group (n = 6 female and n = 2 male). A permanent hypocalcaemia with need for substitution of calcium and vitamin D for at least 6 months occurred in n = 3 females and n = 2 males in the TT group. A transient vocal cord paralysis was seen in n = 2 females with TT and n = 0 males with TT. n = 2 females with HT and n = 1 male with HT. None of the patients suffered from a persistent vocal cord palsy at a 3‐month follow‐up (Table 1).
Table 1.
Patient characteristics and perioperative morbidity
|
Hemithyroidectomy n = 63 |
Thyroidectomy n = 90 |
|||
|---|---|---|---|---|
|
Female n = 45 |
Male n = 18 |
Female n = 67 |
Male n = 23 |
|
| Age mean (y) | 46.9 | 50.5 | 55.3 | 56.4 |
| BMI (kg/m2), pre‐operative | 27.5 | 27.4 | 27.5 | 28.9 |
| BMI (kg/m2), 1 y postoperative | 27.5 | 27.7 | 27.8 | 29.3 |
| Presence of compressive symptoms (n/%) | 16/35.6 | 5/27.8 | 28/41.8 | 8/34.8 |
| Surgery duration | 45.2 | 60.1 | 63.5 | 91.6 |
| Thyroid weight (g) | 31.8 | 40.1 | 63.3 | 102.3 |
| Thyroid volume (mL) | 36.9 | 55.1 | 55.7 | 89.6 |
| TSH (μIE/mL) | 1.1 | 1.3 | 0.7 | 0.8 |
| T3 (pg/mL) | 3.5 | 4.0 | 3.4 | 3.4 |
| T4 (ng/dL) | 1.3 | 1.5 | 1.3 | 1.3 |
| Transient postoperative symptomatic hypocalcaemia (n/%) | 0/0 | 0/0 | 6/9.0 | 2/8.7 |
| Transient vocal cord paralysis (n/%) | 2/4.4 | 1/5.6 | 2/3.0 | 0/0 |
3.3. EQ‐5D‐questionnaire
The change in the TTO score indicates an influence of the surgery on QoL. In most patients (56% after TT, 65% after HT), the TTO score did not change. In 30% after TT and 21% after HT, a positive change in the EQ‐5D QoL was determined. In each group, deterioration was noticed in 14% of all patients, respectively (Figure 1, Table 2).
Figure 1.

Overall change in time trade‐off (TTO) score calculated by the five dimensions of the EuroQoL‐5D (EQ‐5D) questionnaire is shown 1 y postoperatively
Table 2.
Change in the time trade‐off score 1 y after surgery; given are amounts and percentages of patients showing either deterioration, no change or improvement
| Hemithyroidectomy | Thyroidectomy | |||
|---|---|---|---|---|
| n | % | n | % | |
| Deterioration | 9 | 14 | 13 | 14 |
| No change | 41 | 65 | 50 | 56 |
| Improvement | 13 | 21 | 27 | 30 |
| Total | 63 | 100 | 90 | 100 |
The subjective EQ‐5D VAS scores pre‐operatively and 1 year postoperatively demonstrate an improvement of QoL in general (Figure 2), which is in accordance with the results of the TTO score of the five domains.
Figure 2.

Box plot for the EuroQoL‐5D (EQ‐5D) visual analogue scale (VAS) with the y‐axis ranging from 0 (worst imaginable health) to 100 (best imaginable health); depicted are the mean (filled squares), the median, and upper and lower quartile (boxes), and the 5 and 95 percentiles (whiskers). The grey represents the 95% confidence interval for the mean VAS score in a representative, population based German study of healthy people according to44 in the age group 45‐54 y
In addition, with regard to the postoperative change, a clinically relevant, positive difference was observed (Figure 3). Indeed, for both types of surgery, there is a statistically significant difference between the median of the group and zero, indicating a significant postoperative improvement in QoL for both types of surgery (Wilcoxon's one sample signed‐rank test; thyroidectomy: W = 1528, P < .001, post hoc power = 0.99; hemithyroidectomy: W = 442, P = .028, post hoc power = 0.45).
Figure 3.
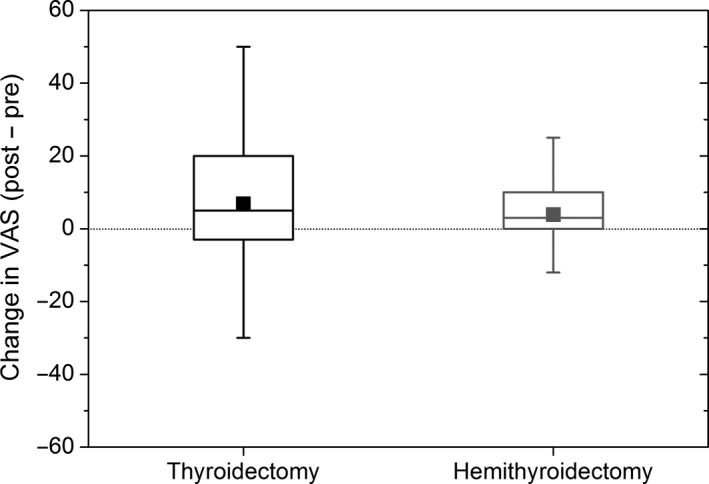
Box plot for the change in VAS (VAS postoperative − VAS pre‐operative) of the EuroQoL‐5D (EQ‐5D) visual analogue scale (VAS) with the y‐axis ranging from 0 (worst imaginable health) to 100 (best imaginable health); depicted are the mean (filled squares), the median, and upper and lower quartile (boxes), and the 5 and 95 percentiles (whiskers). Values above zero indicate better quality of life (QoL) after surgery
When examining the postoperative data in all patients in the individual domains of the EQ‐5D questionnaire, a statistically significant improvement could only be detected in the domain ‘anxiety/ depression’ (Wilcoxon's signed‐rank test: Z = −4438; P < .001, post hoc power = 0.99). N = 40 patients report a postoperative improvement, nine patients a worsening and 104 patients no change in this domain. In the other four dimensions, ‘mobility’, ‘self‐care’, ‘general activities’ and ‘pain’, no statistically significant difference could be observed.
3.4. Influence of socio‐economic factors on QoL
A univariate ANCOVA was performed to investigate the influence of socio‐economic factors on postoperative VAS change (see Table 3 for an overview of descriptive statistics with regard to the socio‐economic factors). The dependent variable was the difference between post‐ and pre‐operative VAS, the fixed factors were type of surgery, sex, familial status, length of school education, employment status and yearly income, and the covariates were age and BMI. Out of these factors, only the yearly income had a significant influence on the way the VAS score changed 1 year postoperatively as compared with pre‐operatively (F(1, 151) = 3.686, P = .045, post hoc power = 0.76). The mean difference in VAS Score for patients with an annual household income up to €33 700 was 6.1 ± 17.9 and 4.4 ± 19.2 for patients with an annual household income above €33 700, indicating a more positive change in QoL for patients with a lower income. No significant interactions were found.
Table 3.
Socio‐economic characteristics given as amount of patients
|
Hemithyroidectomy n = 63 |
Thyroidectomy n = 90 |
|||
|---|---|---|---|---|
|
Female n = 45 |
Male n = 18 |
Female n = 67 |
Male n = 23 |
|
| School education <9 y | 4 | 5 | 16 | 9 |
| School education >9 y | 41 | 13 | 51 | 14 |
| Single | 10 | 3 | 17 | 2 |
| Living in partnership | 35 | 15 | 50 | 21 |
| Employed | 25 | 13 | 38 | 17 |
| Unemployed | 20 | 5 | 29 | 6 |
| Yearly household income (<33 700€) | 21 | 10 | 36 | 14 |
| Yearly household income (>33 700€) | 16 | 8 | 17 | 9 |
4. DISCUSSION
From the beginnings of thyroid surgery by Theodore Billroth in 1877 to date, a consensus regarding the optimum therapy for benign thyroid goitre is missing.13 The indication for surgery on benign nontoxic nodular goitre is met in patients with local symptoms or/and potential abnormal nodes. It is well known that patients suffering from thyroid dysfunction report an impairment of QoL. In hypothyroidism or hyperthyroidism, the postoperative QoL is improved.16, 17, 18, 32, 33, 34 Therefore, the hormonal status should be considered in comparison of groups. As in euthyroid patients the influence of hormonal status on QoL is irrelevant, it can be assumed that surgical therapy itself influences the postoperative QoL. In this context, it has been shown that thyroidectomy improves sleep apnoea symptoms, as well as swallowing‐related QoL, and can positively influence psychiatric symptoms.23, 35, 36 For the evaluation of QoL in nontoxic benign goitre, a disease‐specific questionnaire has been established in Denmark and is now used in further countries, except for German‐speaking countries,37, 38 as it is not validated currently.
For this reason, we used the established generic EQ‐5D‐3L questionnaire to determine potential changes in QoL after HT and TT for benign nontoxic diseases. Few published studies have evaluated QoL after thyroid surgery using disease‐specific and generic questionnaires.19, 22, 24, 25, 34, 36, 39, 40 To our knowledge, there is only one German publication concerning the effect of different thyroid resections on QoL.24, 25
In our study, complete data of 153 patients were evaluated (83.6% follow‐up) according to surgical procedure (HT vs TT). The gender ratio in the HT group was 71.4% female and 74.4% female in the TT group, which is consistent with the higher prevalence of thyroid disease in women. The age ratio in each group was similar with a trend to younger female patients at time of operation. Women are more likely to report problems in QoL than men, which is consistent with our results of the pre‐operative VAS score.40 To check the influence of surgery on QoL, the TTO score for each patient was calculated by comparing the five domains of the EQ‐5D questionnaire. In general, regarding the postoperative change in the TTO score, a clear tendency to improvement of QoL, which was larger in the TT group, could be detected. A statistical significance could only be seen in the domain ‘anxiety/ depression’ which can be understood as the emotional domain of the questionnaire. This is consistent with the results of Watt et al,5 who have shown in preparation for the development of the ThyPRO questionnaire that for thyroid patients, psychosocial factors such as emotional susceptibility are most relevant. Compared with the general population, patients with nontoxic goitre have the greatest QoL impairment on goitre associated local symptoms as well as anxiety scales prior to treatment. For both aspects, it has been shown that they improve after the respective treatment, including operation, radioiodine therapy or cyst aspiration with ethanol sclerotherapy as potential treatment strategy.38 Our results are in line with the literature where a positive impact of thyroidectomy on QoL is seen.23, 34, 35, 41
Schmitz‐Winnenthal et al,25 who used the same generic instrument for assessing QoL, could not see a significant influence of extent of surgery, that is hemithyroidectomy vs Dunhill operation vs thyroidectomy, on QoL postoperatively. Although this study only compared the postoperative influence of surgery retrospectively, our data are consistent with their study regarding that 50% of the patients in all groups show no change in QoL.
Only few studies have examined pre‐ and postoperative QoL in nontoxic goitres. Mishra et al compared in a prospective study presurgical and 6 months postsurgical assessment of QoL in a relatively homogenous group of patients with benign thyroid goitre. They showed a significant improvement of QoL using the ThyPRO questionnaire.24 However, in this study, the biochemical status was not similar and patients with thyroid dysfunction were also included. Therefore, the improvement of QoL could either be linked to a postoperative improvement of the metabolic situation or the influence of the operation.
Bukvic et al22 used the same questionnaire in patients with mostly nontoxic goitres and could present a significant improvement of QoL independently of type of surgery (hemithyroidectomy and thyroidectomy). They assessed the pre‐operative status 1 day before operation in their surgical department, which is similar to the setting of our study, and they noted critically that the immediate pre‐operative status survey could possibly have led to worse results in the domain of anxiety. This could also be an explanation for the fact that in our study, we only found a significant improvement in the domain anxiety. On the other hand, thyroid patients often have a longer history of their disease and it is likely that they also inquired about an operation, so that perhaps not only the immediate direct temporal connection with the operation influences this domain. On the other hand, suspected malignancy might have a strong influence on the ‘anxiety’ domain as well, which might explain the difference between the pre‐ and postoperative QoL in this domain. It has also been reported that goitre recurrence might influence QoL.42 However, we did not include patients with recurrent goitre and no recurrence was recorded during follow‐up. Therefore, this aspect should not influence our data set.
In a representative survey with over 3552 participants measuring the health status of the German population using the EQ‐5D questionnaire, the influence of socio‐economic factors was examined, and a positive influence of marital status, duration of education and gender on QoL was detected.40 Therefore, we examined the impact of gender, school education, employment status, family status and household income on postoperative change in QoL. Only the annual household income had a significant effect on VAS change 1 year postoperatively compared with pre‐operative status. In the US, a delayed diagnosis and therapy of thyroid cancer have been shown in black and uninsured patients as well as in families with low income.29, 43 Although the German cannot be compared with the American health system, it seems that the household income affects health‐related QoL in thyroid disease transnationally.
Bukvic et al could see a correlation of patients' education level with improvement of QoL in various domains of the ThyPRO questionnaire. They assumed that lower educated patients benefit more than higher educated patients due to the lowered pre‐operative baseline in the questionnaire.22 How far this statement corresponds to reality can only be analysed by larger collectives, and different study designs, since a correlation between household income and education level cannot be made in general.
Our results indicate that there is a tendency for improved QoL after thyroid surgery measured by EQ‐5D questionnaire (HT or TT). Regarding the VAS part of this questionnaire, more than 70%‐75% of all patients had a better postoperative QoL. Also, when compared with the results of a representative German study, the majority of our patients have the same or better QoL after surgery than a group of healthy adults of the same age (Figure 2). In other studies, it has been shown that women have statistically more benefit from surgery than men in terms of QoL.24 However, in our study, a gender‐specific difference in QoL could not be detected. Probably, for a gender‐specific subgroup analysis, more patients are required.
5. CONCLUSION
The indication for thyroid surgery in benign nontoxic diseases can be made due to local compressive symptoms or to malignant suspicious thyroid nodules. We could show that the expansion of thyroid resection does not significantly affect the long‐term postoperative QoL and there is a tendency for improved QoL in a 1‐year follow‐up. As socio‐economic status influence QoL in general, we could prove a correlation of household income on postoperative QoL. Therefore, the postoperative improvement of QoL is mostly independent of socio‐economic status in nontoxic thyroid diseases.
Thus, in the counselling of patients with symptomatic goitres and/or relative surgical indications, we recommend presenting the operation as a possible equivalent option as quality of life is at least preserved or improved. The extension of the resection should, however, be decided individually. For further studies, we would recommend to avoid an immediate pre‐operative measurement of quality of life as this seems to influence the anxiety domain of quality of life questionnaires.
CONFLICT OF INTEREST
The authors declare no commercial interest or conflict of interest in the subject of this study.
AUTHORS' CONTRIBUTIONS
NT was responsible for study design and data analysis and wrote the first draft of the manuscript. VNU was responsible for data analysis and graphics and wrote the results part of the manuscript. IT was responsible for study design and data acquisition and contributed to the manuscript in its current form. DW conceived and designed the study and contributed to the manuscript in its current form.
Tabriz N, Uslar VN, Tabriz I, Weyhe D. Quality of life is not affected by thyroid surgery in nontoxic benign goitre in long‐term surveillance—A prospective observational study. Endocrinol Diab Metab. 2020;3:e00115 10.1002/edm2.115
DATA AVAILABILITY STATEMENT
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
REFERENCES
- 1. Statistisches Bundesamt . Fallpauschalenbezogene Krankenhausstatistik (DRG‐Statistik). Operationen und Prozeduren der vollstationären Patientinnen und Patienten in Krankenhäusern‐ausführliche Darstellung. http://www.destatis.de/DE/ZahlenFakten/GesellschaftStaat/Gesundheit. Accessed December 12, 2018.
- 2. Ahn HS, Kim HJ, Welch HG. Korea's thyroid‐cancer “epidemic”–screening and overdiagnosis. N Engl J Med. 2014;371:1765‐1767. [DOI] [PubMed] [Google Scholar]
- 3. Enewold L, Harlan LC, Stevens JL, Sharon E. Thyroid cancer presentation and treatment in the United States. Ann Surg Oncol. 2015;22:1789‐1797. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Wienhold R, Scholz M, Adler J‐B, Günster C, Paschke R. The management of thyroid nodules: a retrospective analysis of health insurance data. Dtsch Arztebl Int. 2013;110:827‐834. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Watt T, Hegedüs L, Rasmussen ÅK, et al. Which domains of thyroid‐related quality of life are most relevant? Patients and clinicians provide complementary perspectives. Thyroid. 2007;17:647‐654. [DOI] [PubMed] [Google Scholar]
- 6. Stang MT, Armstrong MJ, Ogilvie JB, et al. Positional dyspnea and tracheal compression as indications for goiter resection. Arch Surg. 2012;147:621‐626. [DOI] [PubMed] [Google Scholar]
- 7. Bonnema SJ, Hegedüs L. Radioiodine therapy in benign thyroid diseases: effects, side effects, and factors affecting therapeutic outcome. Endocr Rev. 2012;33:920‐980. [DOI] [PubMed] [Google Scholar]
- 8. Gharib H, Hegedüs L, Pacella CM, Baek JH, Papini E. Nonsurgical, image‐guided, minimally invasive therapy for thyroid nodules. J Clin Endocrinol Metab. 2013;98:3949‐3957. [DOI] [PubMed] [Google Scholar]
- 9. Papini E, Pacella CM, Laszlo H. Thyroid ultrasound and ultrasound‐assisted procedures. From the shadows into an array of applications. Eur J Endocrinol. 2014;170:R133‐R146. [DOI] [PubMed] [Google Scholar]
- 10. Randolph GW, Dralle H, Abdullah H, et al. Electrophysiologic recurrent laryngeal nerve monitoring during thyroid and parathyroid surgery: international standards guideline statement. Laryngoscope. 2011;121:S1‐S16. [DOI] [PubMed] [Google Scholar]
- 11. Bonnema SJ, Bertelsen H, Mortensen J, et al. The feasibility of high dose iodine 131 treatment as an alternative to surgery in patients with a very large goiter: effect on thyroid function and size and pulmonary function. J Clin Endocrinol Metab. 1999;84:3636‐3641. [DOI] [PubMed] [Google Scholar]
- 12. Shaha A, Alfonso A, Jaffe BM. Acute airway distress due to thyroid pathology. Surgery. 1987;102:1068‐1074. [PubMed] [Google Scholar]
- 13. Delbridge L. Total thyroidectomy: the evolution of surgical technique. ANZ J Surg. 2003;73:761‐768. [DOI] [PubMed] [Google Scholar]
- 14. Moalem J, Suh I, Duh Q‐Y. Treatment and prevention of recurrence of multinodular goiter: an evidence‐based review of the literature. World J Surg. 2008;32:1301‐1312. [DOI] [PubMed] [Google Scholar]
- 15. Dralle H, Lorenz K, Machens A. State of the art: surgery for endemic goiter—a plea for individualizing the extent of resection instead of heading for routine total thyroidectomy. Langenbecks Arch Surg. 2011;396:1137‐1143. [DOI] [PubMed] [Google Scholar]
- 16. Bianchi G, Zaccheroni V, Solaroli E, et al. Health‐related quality of life in patients with thyroid disorders. Qual Life Res. 2004;13:45‐54. [DOI] [PubMed] [Google Scholar]
- 17. McMillan C, Bradley C, Razvi S, Weaver J. Evaluation of new measures of the impact of hypothyroidism on quality of life and symptoms: the ThyDQoL and ThySRQ. Value Health. 2008;11:285‐294. [DOI] [PubMed] [Google Scholar]
- 18. Scerrino G, Morfino G, Paladino NC, et al. Does thyroid surgery for Graves' disease improve health‐related quality of life? Surg Today. 2013;43:1398‐1405. [DOI] [PubMed] [Google Scholar]
- 19. Watt T, Groenvold M, Rasmussen ÅK, et al. Quality of life in patients with benign thyroid disorders. A review. Eur J Endocrinol. 2006;154:501‐510. [DOI] [PubMed] [Google Scholar]
- 20. Wojewoda B, Juzwiszyn J, Rosińczuk‐Tonderys J. Quality of life after surgical treatment of thyroid gland diseases. Rocz Akad Med Bialymst. 2005;50:133‐136. [PubMed] [Google Scholar]
- 21. Hays RD. Generic versus disease‐targeted instruments In: Fayers P, Hays R, eds. Assessing Quality of Life in Clinical Trials: Methods and Practice, Vol 2 New York, NY: Oxford University Press; 2005:3–8. [Google Scholar]
- 22. Bukvic BR, Zivaljevic VR, Sipetic SB, Diklic AD, Tausanovic KM, Paunovic IR. Improvement of quality of life in patients with benign goiter after surgical treatment. Langenbecks Arch Surg. 2014;399:755‐764. [DOI] [PubMed] [Google Scholar]
- 23. Miccoli P, Minuto M, Paggini R, et al. The impact of thyroidectomy on psychiatric symptoms and quality of life. J Endocrinol Invest. 2007;30(10):853‐859. [DOI] [PubMed] [Google Scholar]
- 24. Mishra A, Sabaretnam M, Chand G, Agarwal G, Agarwal A, Verma AK. Mishra SK 2013 quality of life (QoL) in patients with benign thyroid goiters (pre‐and post‐thyroidectomy): a prospective study. World J Surg. 2007;37:2322‐2329. [DOI] [PubMed] [Google Scholar]
- 25. Schmitz‐Winnenthal FH, Schimmack S, Lawrence B, et al. Quality of life is not influenced by the extent of surgery in patients with benign goiter. Langenbecks Arch Surg. 2011;396:1157‐1163. [DOI] [PubMed] [Google Scholar]
- 26. Wong CK, Lang BH, Lam CL. A systematic review of quality of thyroid‐specific health‐related quality‐of‐life instruments recommends ThyPRO for patients with benign thyroid diseases. J Clin Epidemiol. 2016;78:63‐72. [DOI] [PubMed] [Google Scholar]
- 27. Laubach W, Schumacher J, Mundt A, Brähler E. Social class, life satisfaction and health assessment. Results of a representative study of the German population. Soz Praventivmed. 2000;45:2‐12. [DOI] [PubMed] [Google Scholar]
- 28. Aschebrook‐Kilfoy B, James B, Nagar S, et al. Risk factors for decreased quality of life in thyroid cancer survivors: initial findings from the North American Thyroid Cancer Survivorship Study. Thyroid. 2015;25:1313‐1321. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29. Garner EF, Maizlin II, Dellinger MB, et al. Effects of socioeconomic status on children with well‐differentiated thyroid cancer. Surgery. 2017;162:662‐669. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30. Bernert S, Fernández A, Haro JM, et al. Comparison of different valuation methods for population health status measured by the EQ‐5D in three European countries. Value Health. 2009;12:750‐758. [DOI] [PubMed] [Google Scholar]
- 31. Krabbe PF, Stouthard ME, Essink‐Bot M‐L, Bonsel GJ. The effect of adding a cognitive dimension to the EuroQol multiattribute health‐status classification system. J Clin Epidemiol. 1999;52:293‐301. [DOI] [PubMed] [Google Scholar]
- 32. Cashman E, Bresnihan M, Timon C. Patients' quality of life post thyroidectomy. B‐ENT. 2011;7:261‐265. [PubMed] [Google Scholar]
- 33. Promberger R, Hermann M, Pallikunnel SJ, Seemann R, Meusel M, Ott J. Quality of life after thyroid surgery in women with benign euthyroid goiter: influencing factors including Hashimoto's thyroiditis. Am J Surg. 2014;207:974‐979. [DOI] [PubMed] [Google Scholar]
- 34. Reiher AE, Mazeh H, Schaefer S, Chen H, Sippel RS. Thyroidectomy decreases snoring and sleep apnea symptoms. Thyroid. 2012;22:1160‐1164. [DOI] [PubMed] [Google Scholar]
- 35. Sabaretnam M, Mishra A, Chand G, et al. Assessment of swallowing function impairment in patients with benign goiters and impact of thyroidectomy: a case control study. World J Surg. 2012;36:1293‐1299. [DOI] [PubMed] [Google Scholar]
- 36. Watt T, Barbesino G, Bjorner JB, et al. Cross‐cultural validity of the thyroid‐specific quality‐of‐life patient‐reported outcome measure, ThyPRO. Qual Life Res. 2015;24:769‐780. [DOI] [PubMed] [Google Scholar]
- 37. Watt T, Hegedüs L, Groenvold M, et al. Validity and reliability of the novel thyroid‐specific quality of life questionnaire, ThyPRO. Eur J Endocrinol. 2010;162:161‐167. [DOI] [PubMed] [Google Scholar]
- 38. Cramon P, Bonnema SJ, Bjorner JB, et al. Quality of life in patients with benign nontoxic goiter: impact of disease and treatment response, and comparison with the general population. Thyroid. 2015;25:284‐291. [DOI] [PubMed] [Google Scholar]
- 39. Sorensen JR, Watt T, Cramon P, et al. Quality of life after thyroidectomy in patients with nontoxic nodular goiter: a prospective cohort study. Head Neck. 2017;39:2232‐2240. [DOI] [PubMed] [Google Scholar]
- 40. König HH, Bernert S, Angermeyer MC. Gesundheitszustand der deutschen Bevölkerung: Ergebnisse einer repräsentativen Befragung mit dem EuroQol‐Instrument. Gesundheitswesen. 2005;67:173‐182. [DOI] [PubMed] [Google Scholar]
- 41. Greenblatt DY, Sippel R, Leverson G, Frydman J, Schaefer S, Chen H. Thyroid resection improves perception of swallowing function in patients with thyroid disease. World J Surg. 2008;33:255‐260. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42. Sawicka‐Gutaj N, Ziółkowska P, Sowiński J, et al. Recurrent goiter: risk factors, patient quality of life, and efficacy of radioiodine therapy. Pol Arch Intern Med. 2019;129:818‐823. [DOI] [PubMed] [Google Scholar]
- 43. Jaap K, Campbell R, Dove J, et al. Disparities in the care of differentiated thyroid cancer in the United States: exploring the national cancer database. Am Surg. 2017;83:739‐746. [PubMed] [Google Scholar]
- 44. Biondi B, Palmieri EA, Fazio S, et al. Endogenous subclinical hyperthyroidism affects quality of life and cardiac morphology and function in young and middle‐aged patients. J Clin Endocrinol Metab. 2000;85:4701‐4705. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.


