Abstract
Importance
The newly emerged coronavirus disease 19 (COVID-19), is threatening the world. Olfactory or gustatory dysfunction is reported as one of the symptoms worldwide. As reported so far, different clinical features have been reported according to outbreak sites and gender; most of the patients, who complained of anosmia or hyposmia, were Europeans. We had a fast review for novel articles about COVID-19 infection and olfactory function.
Observations
Rapid reviews for COVID-19 or other viral infection and olfactory and/or gustatory dysfunctions were done in this review. Up to date, a lot of reports have shown that olfactory dysfunction is related to viral infections but no exact mechanism, clinical course, and definite treatment have been discovered, which is also same in COVID-19. In general, intranasal steroid (INS) and oral steroid for short time help improve the recovery of the olfactory function in case of olfactory dysfunction after virus infection. Considering severe respiratory complications and immunocompromised state of COVID-19, the use of steroid should be limited and cautious because we do not have enough data to support the usage of steroid to treat olfactory dysfunction in the clinical course of COVID-19.
Conclusions and relevance
In the days of pandemic COVID-19, we should keep in mind that olfactory dysfunctions, even without other upper respiratory infection or otolaryngologic symptoms, might be the early signs of COVID-19.
Keywords: SARS-CoV-2, COVID-19, Anosmia, Hyposmia, Olfactory dysfunction, Gustatory dysfunction
1. Introduction
All over the world, severe Acute Respiratory Syndrome coronavirus-2 (SARS-CoV-2) has been the most important public health issue this year; recently this was re-named as coronavirus disease 2019 (COVID-19) by the World Health Organization (WHO). SARS-CoV-2 is also included in the coronavirus family along with SARS-CoV and Middle East Respiratory Syndrome (MERS)-CoV [1]. COVID-19 was first reported in Wuhan, China [2,3] in December 2019. Since then, COVID-19 has spread rapidly all over the world [4] and has killed more than 226,000 people worldwide so far. This rapid spread is suspected via not only human-to-human but also interspecies transmissions [5]. The WHO declared “a pandemic” on March 11.
According to the early studies, the most common symptoms are known as fever, cough, difficulty in breathing, sputum and sore throat [6,7]. In fact, however, many patients are asymptomatic or have mild symptoms in early stages, and so they do not realize being infected. Since COVID-19 is highly contagious in early stages, such lack of recognition can cause serious problems for the prevention of the spread of COVID-19. Therefore, detection of COVID-19 in early, even asymptomatic, stages will help us reduce transmission.
Recently, olfactory or gustatory dysfunction is often reported as a symptom [8,9]. We need to pay more attention because the symptom might be easily overlooked in clinical field and so the diagnosis could be delayed. In this review, we reviewed recent findings of the viral infection-related olfactory or gustatory dysfunctions to identify a correlation between the olfactory or gustatory symptoms and corona virus, and the values of olfactory dysfunction as an early sign of COVID-19, even in asymptomatic patients.
2. Methods
We searched the articles using PubMed and Embase. The first keyword was viral infection, coronavirus, rhinovirus, influenza, COVID, SARS or MERS. The second keyword was anosmia, smell, or olfactory. The full search strategy has been reported in table (Table 1 ).
Table 1.
Full search strategy.
| #1 | Coronavirus[Title/Abstract] |
| #2 | Viral infection [Title/Abstract] |
| #3 | Rhinovirus [Title/Abstract] |
| #4 | Influenza [Title/Abstract] |
| #5 | COVID-19 [Title/Abstract] |
| #6 | SARS [Title/Abstract] |
| #7 | MERS [Title/Abstract] |
| #8 | Search #1 OR #2 OR #3 OR #4 OR #5 OR #6 OR #7 |
| #9 | Anosmia [Title/Abstract] |
| #10 | Smell [Title/Abstract] |
| #11 | Olfactory [Title/Abstract] |
| #12 | Search #9 OR #10 OR #11 |
| #13 | Search #8 AND #12 |
The articles that could not be obtained in the full text, did not mention relationship between viral infection and olfactory function directly, were not written in English, and were the duplicated papers by the same author were excluded using endnote X9 software. To date (23th, April 2020), we could find 85 papers which mentioned viral infection and olfactory function. Among them, 26 papers described relationship between olfactory symptoms and coronavirus infection including SARS. 40 papers described a relationship between olfactory symptoms and other viral infection including cytomegalovirus, herpes virus, influenza and others.
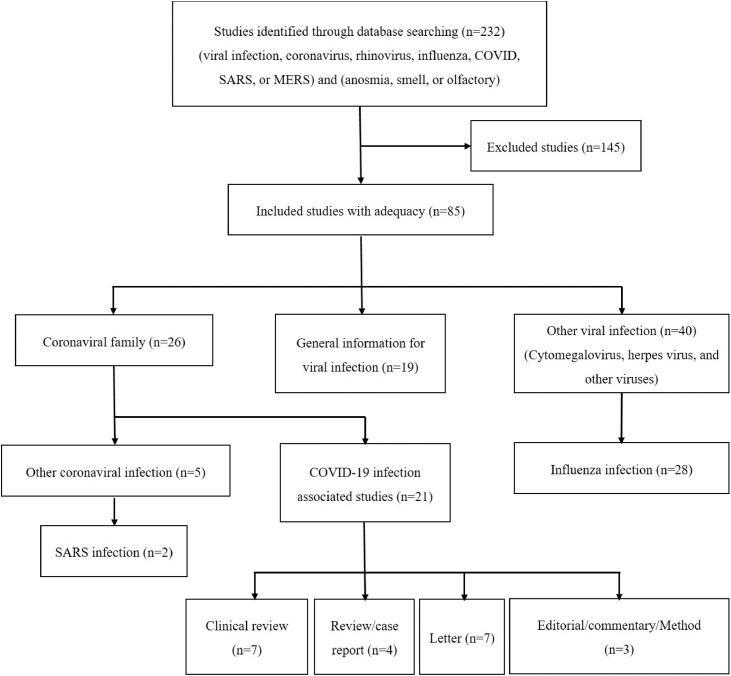
Finally, we could find 21 papers that directly described COVID-19 and olfactory symptoms; some of them also mentioned gustatory dysfunction or ageusia. From these 21 papers, 7 papers were clinical studies and others were commentary, letters, and editorial review (Fig. 1 ). The details of these 7 articles were demonstrated in table (Table 2 ). A study reported patients who initially complained of acute onset anosmia (not COVID-19 infection) but finally diagnosed with COVID-19 infection [10].
Fig. 1.
Flowchart of studies inclusion and exclusion criteria.
Table 2.
Overview the results of review the articles about relationship among COVID-19 infection, olfactory and gustatory dysfunction.
| General information (author, title, journal) | Patients (country ; age ; gender ; severity of disease ; comorbidity) | Sample size (patients with laboratory comfi rmed COVID-19) | Outcomes | |||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Diagnostic tool | The ratio patient with olfactory dysfunction ; Association with olfactor y dysfunction and COVID-19 infection | The ratio patient with gustatory dysf unction ; Association with gustatory d ysfunction and COVID-19 infection | Early onset of olfactory dysfunction (before other symptoms or hospitalization) | Gender association | Isolated symptom | Treatments | Prognosis (Early recovery rate) | |||
| Yan CH, et al.; Association of Chemosensory Dysfunction and Covid-19 in Patients Present ing with Influenza-like Symptoms ; Int Forum Allergy Rhinolology [14] | USA; 18–79 ; 35% men and 65% female ; mild ; not mentioned | 59 (among 1480 patients with influenza like symptoms) | Survey | 68% ; adjusted odds ratio with anosmia 10.9 (95%CI:5.08–23.5) | 71% ; adjusted odds ratio with ageusia 10.2 (95%CI:4.74–22.1) | 22% (anosmia as initial symptom) | Not mentioned | Not mentioned | Not mentioned | 74% (with clinical resolution) |
| Lechien JR. et al.; Olfactory and gustatory dysfunctions as a clinical presentation of mild-to-moderate forms of the coronavirus disease (COVID-19): a multicenter European study ; Eur Arch Otorhinolaryngology [9] | European (93.3%); mean age 36.9 ± 11.4(19–77); 37% men and 63% female ; mild to moderate ; allergy rhinitis (20%), asthma, high blood pressure, hypothyroidism | 417 | Survey | 85.6% | &0% 88.8% | 11.8% olfactory dysfunction | Female > Male | 18.2% (without nasal stuffiness and rhinorrhea) | 70% nothing 11% saline irrigation 8% nasal corticosteroid | 44% (within 2 weeks) |
| Hopkins C, et al.; Presentation of new onset anosmia during the COVID-19 pandemic ; Rliinology [10] * | United Kingdom ; 64% were under 40 ; 73% female ; mild ; not mentioned | 2428 of acute anosmia (However, only 80 patient got COVID-19 test and 74% were positive) | Survey | Not mentioned | Not mentioned | 13% (early anosmia among 2428 patients with acute anosmia) | Male > Female (among 2428 patients with acute anosmia) | 17% (among 2428 patients with acute anosmia) | Not mentioned | Not mentioned |
| Giacomelli A, et al.; Self-reported olfactory and taste disorders in SARS-CoV-2 patients: a cross-sectional study ; Clin. Infect Dis. [11] | Italy ; median age 60 ; 67.8% male ; not mentioned ; not mentioned | 59 | Survey | 11.9% anosmia 11.9% hyposmia | 13.6% ageusia 15.3% dysgeusia | 20.3% olfactory dysfunction 91% gustatoiy dysfunction | Female > Male (p = 0.036) | Not mentioned | Not mentioned | None |
| Moein ST, et al.; Smell Dysfunction: A biomarker for COVID-19 ; Int Forum Allergy Rliinology [15] | Iran ; mean age 46.55 ± 12.17 ; 66.7% men and 33.3% women ; mild to severe ; diabetes, hypertension, hypothyroidism (p>0.005) | 60 | University of Pennsylvania Smell Identification Test (UPSIT) | 98% (58% anosmia, 33% severe microsmia, 27% moderate microsmia, 8% mild microsmia) | 23% (not checked by UPSIT) | None (among 21 patients complained smell loss - not checked by UPSIT) | Male = Female | None (among 21 patients complained smell loss - not checked by UPSIT) | Not mentioned | Not mentioned |
| Klopfenstein T, et al.; Features of anosmia in COVID-19 ; Med Mai Infect. [12] | France ; mean age 47 ± 16 ; 33% men and 67% women ; not mentioned; hypertension, cardiovascular disease, asthma | 114 | Medical files review | 47% | 85% dysgeusia (among COVID-19 patients with anosmia) | None (The third symptom in 38% (22/52)cases) | Female > Male | None | Not mentioned | 55% (24/44, after 1 week) 20% (9/44, after 2 weeks) |
| Beltran-Corbellini A, et al.; Acute-onset smell and taste disorders in the context of Covid-19: a pilot multicenter PCR-based case-control study ; Eur J Neurol. [13] | Spain ; mean age 61.6 ± 17.4 ; 60.8% men and 39.2% women ; not mentioned ; not mentioned | 79 | Questionnaire | 31.65% (45.7% anosmia, 29% hyposmia, 6.5% dysosmia among 31 COVID-19 patients with smell and/or taste disorders) | 35.44% (45.2% ageusia, 22.6% hypogeusia, 25.8% dysgeusia among 31 COVID-19 patients with smell and/or taste disorders) | 35.5% (smell and/or taste disorders among 31 COVID- 19 patients) | No significant differences | Not mentioned | Not mentioned | 40% (complete recovery after 7.4 ± 2.3 days) 16.7% (partial recovery after 9.1 ± 3.6 days) |
Total sample size was 2428 patients with new onset anosmia including laboratory confirmed, not confirmed COVID-19 infected patients and not tested.
There were no restrictions for gender, age and nationality. The studies with inclusion criteria were checked independently by 2 reviewers. Reviewers apply inclusion criteria based on the title and abstracts. If the title and abstract were adequate, the full text was checked by the same reviewers.
3. Clinical presentation
The common symptoms in COVID-19 patients were cough, fever, myalgia, dyspnea, headache and loss of appetite. The most common ENT symptoms were facial pain and nasal congestion [9].
However, it has been recently reported that 33.9% of 59 COVID-19 patients in Italy complained of olfactory and/or gustatory dysfunction and 11% complained of both dysfunctions [11]. 47% of 114 COVID-19 patients in France complained anosmia [12]. 31.65% and 35.44% of 79 COVID-19 patients in Spain complained olfactory and gustatory dysfunctions. These proportions were more prominent in COVID-19 patients than influenza patients [13]. According to the paper from USA reported that 68% and 71% of 59 patients had olfactory and gustatory dysfunction, respectively [14]. 98% of 60 patients from Iran were confirmed smell dysfunction by University of Pennsylvania smell identification test (UPSIT) [15]. And few articles said that COVID-19 patients without severe symptoms complained these olfactory and/or gustatory dysfunctions. According to the larger-scale research from Europe, 85.6% of the 417 mild-to-moderate COVID-19 patients had olfactory dysfunctions and 88.8% gustatory dysfunctions. Phantosmia and parosmia were 12.6% and 32.4%, respectively. Among the patients who did not complain of nasal stuffiness and rhinorrhea, the rates of anosmia and hyposmia were 66.2% and 13.5% [9]. From the other Italian article, 64.4% of 202 mild symptomatic COVID-19 patients were reported alternations in smell or taste. About 37% of them complained severe alternations. 68.3% of COVID-19 patients with smell or taste alternations reported fatigue and 34.6% reported nasal stuffiness [16].
Contrary to the above papers, only 5.1% of 214 patients complained of hyposmia and 5.6% hypogeusia in China [8]. Considering the papers, the rate of olfactory or gustatory dysfunction is supposed to be different between Europe/USA and China (or Asia).
Another issue is the onset of olfactory dysfunction, which varied among many papers. The onset of olfactory or gustatory dysfunction in the clinical course of COVID-19 might be important. A multicenter study in Europe showed that 85.6% and 88% of total patients (n = 417) reported olfactory and gustatory dysfunctions, respectively, and 11.8% of COVID-19 patients with olfactory dysfunction appeared before other general symptoms, 65.4% after the general symptoms, and 22.8% at the same time [9]. In Italy, 20.3% of COVID-19 patients reported olfactory dysfunction before other general symptoms and 13.5% during hospitalization [11]. From the other study of Italy, 11.9% of COVID-19 patients (n = 130) complained of smell or taste alternations prior to other symptoms and 26.7% after other symptoms [16]. In Iran, 83% of 23 COVID-19 patients with anosmia complained of anosmia as their primary symptom [17]. In Spain, 35.5% among 31 COVID-19 patients complained early and 67.7% showed acute onset of olfactory dysfunction [13].
However, according to another study from Iran, all of 21 COVID-19 patients reported olfactory dysfunction with or immediately after the other general symptoms [15]. In case of SARS-CoV infection, complete anosmia was usually reported 3 weeks after the first symptom [18].
The other issue is the correlation of olfactory dysfunctions with otolaryngologic symptoms. The olfactory dysfunction is not closely correlated with nasal stuffiness and rhinorrhea, but it is supposed to be related to fever [9]. In China, only 4% of patients with olfactory dysfunction complained of rhinorrhea [19] and only 5% nasal stuffiness [20]. From the recent survey study of 2428 patients with new onset anosmia in United Kingdom, 17% of anosmia patients had only anosmia without any other otolaryngologic symptoms. However, this survey has limited value because only 80 patients had been tested for COVID-19 infection; only 74% of the tested patients were positive and most of the responders were young [10].
From a case report, olfactory dysfunction was described as ‘isolated sudden onset anosmia’ because a patient with confirmed COVID-19 complained of sudden onset anosmia without any other symptoms [21]. According to the other study from Italy, 3% of COVID-19 patients (n = 130) reported smell or taste alternations as the sole symptom [16]. However, there is also an article reporting that ENT symptoms can be accompanied by anosmia [12].
In Korea, Korean center for disease control (KCDC) recently (on 6 April 2020) announced in a press release that proportion of asymptomatic case was 33.3% based on the presence or absence of symptoms at the time of confirmation of COVID-19 (10,284 confirmed as positive among 466,804 tested, in republic of Korea until 6, April 2020) [22].
There is a study showing that most of gustatory dysfunction appeared as an early symptom before hospitalization [11]. Besides, there might be close correlation between olfactory and gustatory dysfunction (p<0.001) [9]. Considering above, around 20–30% COVID-19 patients may present olfactory dysfunction (and/or gustatory dysfunction) as early or sometimes isolated symptom of COVID-19.
Curiously, many studies showed that women had olfactory dysfunction more frequently than men [9,11,12,17], though the reason is hard to be explained at this time. According to a recent study, Toll-like receptor (TLR) activation with cytokine production and protein phosphorylation is related to X chromosomes. This might explain different inflammatory conditions and clinical courses after infection between men and women [23]. However, from another study, the results of UPSIT checked olfactory function were same between men and women [15]. Further investigations of gender difference are needed.
4. Pathophysiology
Globally, particularly in Europe, the olfactory and/or gustatory dysfunctions of COVID-19 patients were reported as new symptoms. However, to date, many papers have reported that the olfactory dysfunction has also occurred by other viral infections, over 200 different viruses [24], [25]–26]. Furthermore, coronavirus family, including SARS, is also related to post-viral anosmia [18]. Although the exact mechanism is not yet known, 2 basic mechanisms have been suggested.
First, conductive olfactory dysfunction can be induced if there are some problems on olfactory cleft mucosa, such as mucosa inflammation or rhinorrhea [27]. Olfactory dysfunction in viral infection with rhinovirus, Parainfluenza Epstein-Barr viruses and some other coronavirus can be explained. However, in some cases, even if the acoustic rhinometry result was normal, the olfactory function did not recover [28]. Olfactory dysfunction of COVID-19 patients is also thought to be less related to rhinorrhea or nasal congestion.
Second, if there are direct effects by virus on olfactory cleft mucosa, sensorineural olfactory dysfunction can be considered [29]. Direct mucosal infection by virus can cause severe injury of peripheral olfactory neuron, which might have fetal effects on olfactory receptors [30]. Also, both SARS-CoV and SARS-CoV-2 might have the potential of microinvasion to the target receptor, human angiotensin converting enzyme 2 (ACE2) receptor, which is expressed on the olfactory bulb and the epithelial cell of oral mucosa [31]. However the effects of virus on sensorineural olfactory dysfunction are controversial. From one study, it claims that SARS-CoV might affect neurons in the olfactory bulb of mice and spread to the cortex, basal ganglia and midbrain [32]. On the other hand, there is another case report of the SARS-CoV patients presenting with anosmia showed normal on brain magnetic resonance imaging (MRI) scan [18]. There is also a case of COVID-19 patient who showed the bilateral inflammatory mucosal obstruction of the olfactory cleft without other abnormalities in nasal cavity and olfactory bulb on computed tomographic scan (CT) and MRI scan [33].
As mentioned earlier, there are differences in the olfactory and otolaryngologic symptoms of Chinese and European patients [19] and it might be due to the diversity and mutation of ACE2 phenotypes [34,35].
5. Diagnosis
The validated tests which could quickly and accurately diagnose the olfactory dysfunction in the highly suspicious COVID-19 patients are needed. The short version of the Questionnaire of Olfactory Disorders Negative Statements (sQOD-NS) can be used to assess the quality of life of the COVID-19 patients with anosmia or hyposmia [9]. The score was significantly lower in patients with anosmia than hyposmia or normosmia.
Besides subjective questionnaires, commonly used olfactory tests are as follows: UPSIT, Cross-cultural Smell Identification Test (CC-SIT; Sensonic, Inc, Haddon Heights, NJ), T&T Olfactometry test (Daiichi Yakuhin Sangyo, Tokyo, Japan), and other olfactory threshold tests [36]. Recently, few cases of COVID-19 patients with olfactory dysfunction were confirmed by UPSIT. There was no correlation between UPSIT result and awareness of olfactory dysfunction in COVID-19 patients [15].
Also, acoustic rhinometry, rhinomanometry, CT, or MRI could identify the mechanism of olfactory dysfunction mainly due to conductive problems and identify other causes. However, the usage of nasal endoscopy is not recommended in the highly suspicious COVID-19 patients because it may provide other people unnecessary virus exposure [37].
6. Treatments
In general, spontaneous recovery rates have been reported higher in post-viral patients than post-traumatic patients, and there are no definite treatment guidelines in the post-viral patients presenting with olfactory or gustatory dysfunction, including COVID-19. There are 2 issues on anosmia treatment in COVID-19 patients.
The first issue is that early anomia treatment in COVID-19 patients can change clinical course of COVID-19. But due to lack of information, this issue is hard to be answered but early detection appears more likely to be meaningful rather than early treatment for COVID-19. The second one is whether empirical oral steroid treatment for acute anosmia can do harm to COVID-19 patients without any other symptom or with mild symptoms
Up to date, several studies have shown that oral steroid treatment for anosmia by viral infection may be effective through reducing mucosal inflammation and edema [38]. There is a controversy over the effectiveness of the use of empirical systemic corticosteroids because oral steroids may aggravate immunosuppressive state in the COVID-19 patients with severe symptoms and there are studies showing that use of corticosteroids in MERS patients may have affected the delay of RNA reduction in MERS coronavirus [39].
Moreover, in cases of the COVID-19 patients with severe lung complications, the use of corticosteroids is not recommended by WHO guideline [40]. In China, however, limited use of low dose corticosteroid during short-term can be permitted when absolutely necessary [41].
According to the recently released ARIA EAACI statement, it is recommended to keep using intranasal steroid (INS) in the COVID-19 patients with allergic rhinitis [40]. Although it may be revised later with new studies, it is also recommended to maintain the use of local intranasal corticosteroids because sneezing could get worse and the virus could spread easily if the patients stop using INS.
INS is supposed to have relatively less risky than systemic steroids because the rate of systemic bioavailability of INS is less than 1% [42]. But further studies are needed to confirm if INS may be effective for the treatment of olfactory dysfunction and for the change of clinical course in the COVID-19 patients.
It was reported that the treatments used for olfactory dysfunction were nasal saline irrigations (16.7%), nasal corticosteroids (8.1%), oral corticosteroids (2.5%), and others (2.5%). However, in actual clinical field, most of the patients with olfactory dysfunction did not receive any treatment [9].
Olfactory training, simple and easy, can bring positive results on the recovery for anosmia by viral infection, but there is no definite guideline for olfactory training in the COVID-19 patients. But a few papers recommend that early olfactory training before 12 months from the onset of anosmia could have positive results in the patients with anosmia and viral infection, including COVID-19 [37,43].
Besides steroid and olfactory training, Zinc sulfate, theophylline, Ginkgo biloba, vitamins, nasal decongestants, or other medicine could also be considered to treat olfactory dysfunction. Saline washing/ nasal saline irrigation should be considered carefully, because it could make virus more contagious [9]. However, except for the corticosteroid, the effects of other medicine have not been proven [37].
Most of the patients with gustatory dysfunction did not have any special treatment, either using l-carnitine or vitamins [9].
7. Prognosis
The recovery of olfactory function is relatively slower in sensorineural dysfunction than conductive olfactory dysfunction, and permanent functional loss might be caused [21].
There are a few studies for the recovery of olfactory function in COVID-19 infected patients yet. In USA, 74% of 38 cured patients from COVID-19 were reported to show the recovery of anosmia [14]. In France, mean duration of anosmia was within 2 weeks and 55% of 44 patients recovered more after 1week and 20% recovered more after 2 weeks. In Spain, mean duration of anosmia was also within 2 weeks and 40% of 30 patients recovered completely around 1 week later (7.4 ± 2.3 days) [13]. According to the study from Europe, a total of 357 patients (85.6%) had olfactory dysfunction from a total of 417 COVID-19 infected patients. But among 59 clinically cured patients, only 44% is reported to show the recovery of olfactory function in short term period (within 14 days), most of whom (72.6% of patients with recovered olfactory dysfunction) showed a recovery within 8 days; only a small number of patients (3.4%) showed a recovery more than 15 days after the COVID-19 resolution. Among the clinically cured patients who had residual olfactory and/or gustatory dysfunction, 53.9% complained of only olfactory dysfunction, 22.5% only gustatory dysfunction and 23.6% both remaining olfactory and gustatory dysfunctions [9].
The time to decide the recovery of olfactory function was suggested to be 2 weeks, because the viral loading significantly reduces in about 14 days [9,44]. But the further study requires to decide the time to recovery and follow up long term later.
Considering from the other viral infections, the partial or complete recovery of olfactory function could take several months [45]. And in case of anosmia after SARS, the patient was reported to suffer from anosmia continuously more than 2 years [18].
8. Discussion
The ongoing COVID-19 epidemic is still rapidly spreading all over the world. So it is very important to notice the early sign of COVID-19 and get the information about progression as soon as possible. Most of COVID-19 patients complain of no symptoms or mild symptoms in early stages though coughing, fever and difficulty breathing are main symptoms.
Up to date, the number of the COVID-19 patients with olfactory and/or gustatory symptoms is rapidly increasing and, though the onset of olfactory and/or gustatory symptoms in the COVID-19 patients was reported varied, in general, most of these 2 symptoms might precede or be accompanied by other main mild general symptoms or no other symptoms [16]. Moreover, many cases (18.2%) have been reported for the COVID-19 patients to complain of these 2 symptoms suddenly without any other otolaryngologic symptoms, like rhinorrhea or nasal obstructions [9].
Based on the previous paper, the rates of asymptomatic cases out of all SARS-CoV positive cases were reported 13% among Singaporean health care workers [46]. Furthermore, according to WHO report for MERS-CoV, 21% of the 2228 cases from all over the world were reported to have no or mild symptoms [47].
Asymptomatic case proportion of COVID-19 was 33.3% based on the presence or absence of symptoms at the time of confirmation, which was higher than SARS-CoV and MERS-CoV, according to KCDC report (on 6 April 2020) [22].
Therefore, we should pay more attention to olfactory and/or gustatory symptoms in the suspicious COVID-19 patients with or without the main COVID-19 symptoms because asymptomatic COVID-19 infection (and/or transmission) is a major public health issue at present. However, the exact rate of asymptomatic COVID-19 all over the world has not known and further analysis should be done.
Even though the pathophysiologic mechanism of olfactory or gustatory dysfunctions in COVID-19 patients has not been clearly identified yet, it is also very interesting that the clinical manifestations of olfactory or gustatory dysfunctions were different according to gender or races.
Moreover, it is necessary to follow the clinical course and the long-term results of olfactory and/or gustatory dysfunctions in the cured COVID-19 patients.
9. Conclusion
Although there is still a lack of our understanding of COVID-19, the number of COVID-19 patients is rapidly increasing all over the world. Based on the recent reports and studies, sudden olfactory and/or gustatory dysfunctions may be the early signs of COVID-19, though all olfactory and/or gustatory dysfunctions are not caused only by COVID-19, even at present. Therefore, if there are any persons complaining of olfactory and/or gustatory dysfunctions in COVID −19 pandemic areas, it is suggested that accurate and urgent diagnostic test for COVID-19 should be applied; by doing so health providers can get an opportunity to prepare personal protective equipment in advance, and isolate the suspected asymptomatic patients (or with mild symptom) to prevent the further spread of COVID-19.
Declaration of Competing Interest
The authors have no financial conflicts of interest.
Acknowledgments
None
Reference
- 1.Lai C.C., Shih T.P., Ko W.C., Tang H.J., Hsueh P.R. Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and coronavirus disease-2019 (COVID-19): the epidemic and the challenges. Int J Antimicrob Agents. 2020;55(3) doi: 10.1016/j.ijantimicag.2020.105924. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Zhu N., Zhang D., Wang W., Li X., Yang B., Song J. A novel coronavirus from patients with pneumonia in China, 2019. N Engl J Med. 2020;382(8):727–733. doi: 10.1056/NEJMoa2001017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Li Q., Guan X., Wu P., Wang X., Zhou L., Tong Y. Early transmission dynamics in Wuhan, China, of Novel coronavirus-infected pneumonia. N Engl J Med. 2020;382(13):1199–1207. doi: 10.1056/NEJMoa2001316. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Wu Y.C., Chen C.S., Chan Y.J. Overview of The 2019 Novel Coronavirus (2019-nCoV): the Pathogen of Severe Specific Contagious Pneumonia (SSCP) J Chin Med Assoc. 2020 [Google Scholar]
- 5.Ye Z.W., Yuan S., Yuen K.S., Fung S.Y., Chan C.P., Jin D.Y. Zoonotic origins of human coronaviruses. Int J Biol Sci. 2020;16(10):1686–1697. doi: 10.7150/ijbs.45472. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Young B.E., Ong S.W.X., Kalimuddin S., Low J.G., Tan S.Y., Loh J. Epidemiologic features and clinical course of patients infected with SARS-CoV-2 in Singapore. JAMA. 2020 doi: 10.1001/jama.2020.3204. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Wan S., Xiang Y., Fang W., Zheng Y., Li B., Hu Y. Clinical features and treatment of COVID-19 patients in northeast Chongqing. J Med Virol. 2020 doi: 10.1002/jmv.25783. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Mao L., Jin H., Wang M., Hu Y., Chen S., He Q. Neurologic manifestations of hospitalized patients with coronavirus disease 2019 in Wuhan, China. JAMA Neurol. 2020 doi: 10.1001/jamaneurol.2020.1127. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Lechien J.R., Chiesa-Estomba C.M., De Siati D.R., Horoi M., Le Bon S.D., Rodriguez A. Olfactory and gustatory dysfunctions as a clinical presentation of mild-to-moderate forms of the coronavirus disease (COVID-19): a multicenter European study. Eur Arch Otorhinolaryngol. 2020 doi: 10.1007/s00405-020-05965-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Hopkins C., Surda P., Kumar N. Presentation of new onset anosmia during the COVID-19 pandemic. Rhinology. 2020 doi: 10.4193/Rhin20.116. [DOI] [PubMed] [Google Scholar]
- 11.Giacomelli A., Pezzati L., Conti F., Bernacchia D., Siano M., Oreni L. Self-reported olfactory and taste disorders in SARS-CoV-2 patients: a cross-sectional study. Clin Infect Dis. 2020 doi: 10.1093/cid/ciaa330. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Klopfenstein T., Kadiane-Oussou N.J., Toko L., Royer P.Y., Lepiller Q., Gendrin V. Features of anosmia in COVID-19. Med Mal Infect. 2020 doi: 10.1016/j.medmal.2020.04.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Beltrán-Corbellini Á., Chico-García J.L., Martínez-Poles J., Rodríguez-Jorge F., Natera-Villalba E., Gómez-Corral J. Acute-onset smell and taste disorders in the context of Covid-19: a pilot multicenter PCR-based case-control study. Eur J Neurol. 2020 doi: 10.1111/ene.14273. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Yan C.H., Faraji F., Prajapati D.P., Boone C.E., DeConde A.S. Association of chemosensory dysfunction and Covid-19 in patients presenting with influenza-like symptoms. Int Forum Allergy Rhinol. 2020 doi: 10.1002/alr.22579. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Moein S.T., Hashemian S.M.R., Mansourafshar B., Khorram-Tousi A., Tabarsi P., Doty R.L. Smell dysfunction: a biomarker for COVID-19. Int Forum Allergy Rhinol. 2020 doi: 10.1002/alr.22587. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Spinato G., Fabbris C., Polesel J., Cazzador D., Borsetto D., Hopkins C. Alterations in smell or taste in mildly symptomatic outpatients with SARS-CoV-2 Infection. JAMA. 2020 doi: 10.1001/jama.2020.6771. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Heidari F., Karimi E., Firouzifar M., Khamushian P., Ansari R., Mohammadi Ardehali M. Anosmia as a prominent symptom of COVID-19 infection. Rhinology. 2020 doi: 10.4193/Rhin20.140. [DOI] [PubMed] [Google Scholar]
- 18.Hwang C.S. Olfactory neuropathy in severe acute respiratory syndrome: report of A case. Acta Neurol Taiwan. 2006;15(1):26–28. [PubMed] [Google Scholar]
- 19.Chen N., Zhou M., Dong X., Qu J., Gong F., Han Y. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet. 2020;395(10223):507–513. doi: 10.1016/S0140-6736(20)30211-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Guan W.J., Ni Z.Y., Hu Y., Liang W.H., Ou C.Q., He J.X. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med. 2020 doi: 10.1056/NEJMoa2002032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Gane S.B., Kelly C., Hopkins C. Isolated sudden onset anosmia in COVID-19 infection. A novel syndrome? Rhinology. 2020 doi: 10.4193/Rhin20.114. [DOI] [PubMed] [Google Scholar]
- 22.KCDC. The updates on COVID-19 in Korea as of 6 April. 2020. http://ncov.mohw.go.kr/en.
- 23.Lefèvre N., Corazza F., Valsamis J., Delbaere A., De Maertelaer V., Duchateau J. The Number of X chromosomes influences inflammatory cytokine production following toll-like receptor stimulation. Front Immunol. 2019;10:1052. doi: 10.3389/fimmu.2019.01052. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Hummel T., Landis B.N., Hüttenbrink K.B. Smell and taste disorders. GMS Curr Top Otorhinolaryngol Head Neck Surg. 2011;10 doi: 10.3205/cto000077. Doc04. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.van Riel D., Verdijk R., Kuiken T. The olfactory nerve: a shortcut for influenza and other viral diseases into the central nervous system. J Pathol. 2015;235(2):277–287. doi: 10.1002/path.4461. [DOI] [PubMed] [Google Scholar]
- 26.de Haro-Licer J., Roura-Moreno J., Vizitiu A., González-Fernández A., González-Ares J.A. Long term serious olfactory loss in colds and/or flu. Acta Otorrinolaringol Esp. 2013;64(5):331–338. doi: 10.1016/j.otorri.2013.04.003. [DOI] [PubMed] [Google Scholar]
- 27.Trotier D., Bensimon J.L., Herman P., Tran Ba Huy P., Døving K.B., Eloit C. Inflammatory obstruction of the olfactory clefts and olfactory loss in humans: a new syndrome? Chem Senses. 2007;32(3):285–292. doi: 10.1093/chemse/bjl057. [DOI] [PubMed] [Google Scholar]
- 28.Suzuki M., Saito K., Min W.P., Vladau C., Toida K., Itoh H. Identification of viruses in patients with postviral olfactory dysfunction. Laryngoscope. 2007;117(2):272–277. doi: 10.1097/01.mlg.0000249922.37381.1e. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Finsterer J., Stollberger C. Causes of hypogeusia/hyposmia in SARS-CoV2 infected patients. J Med Virol. 2020 doi: 10.1002/jmv.25903. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Yamagishi M., Fujiwara M., Nakamura H. Olfactory mucosal findings and clinical course in patients with olfactory disorders following upper respiratory viral infection. Rhinology. 1994;32(3):113–118. [PubMed] [Google Scholar]
- 31.Xu H., Zhong L., Deng J., Peng J., Dan H., Zeng X. High expression of ACE2 receptor of 2019-nCoV on the epithelial cells of oral mucosa. Int J Oral Sci. 2020;12(1):8. doi: 10.1038/s41368-020-0074-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Netland J., Meyerholz D.K., Moore S., Cassell M., Perlman S. Severe acute respiratory syndrome coronavirus infection causes neuronal death in the absence of encephalitis in mice transgenic for human ACE2. J Virol. 2008;82(15):7264–7275. doi: 10.1128/JVI.00737-08. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Eliezer M., Hautefort C., Hamel A.L., Verillaud B., Herman P., Houdart E. Sudden and complete olfactory loss function as a possible symptom of COVID-19. JAMA Otolaryngol Head Neck Surg. 2020 doi: 10.1001/jamaoto.2020.0832. [DOI] [PubMed] [Google Scholar]
- 34.Li W., Zhang C., Sui J., Kuhn J.H., Moore M.J., Luo S. Receptor and viral determinants of SARS-coronavirus adaptation to human ACE2. Embo. J. 2005;24(8):1634–1643. doi: 10.1038/sj.emboj.7600640. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Cao Y., Li L., Feng Z., Wan S., Huang P., Sun X. Comparative genetic analysis of the novel coronavirus (2019-nCoV/SARS-CoV-2) receptor ACE2 in different populations. Cell Discov. 2020;6:11. doi: 10.1038/s41421-020-0147-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Doty R.L., Shaman P., Dann M. Development of the University of Pennsylvania Smell Identification Test: a standardized microencapsulated test of olfactory function. Physiol Behav. 1984;32(3):489–502. doi: 10.1016/0031-9384(84)90269-5. [DOI] [PubMed] [Google Scholar]
- 37.Soler Z.M., Patel Z.M., Turner J.H., Holbrook E.H. A primer on viral-associated olfactory loss in the era of COVID-19. Int Forum Allergy Rhinol. 2020 doi: 10.1002/alr.22578. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Stenner M., Vent J., Hüttenbrink K.B., Hummel T., Damm M. Topical therapy in anosmia: relevance of steroid-responsiveness. Laryngoscope. 2008;118(9):1681–1686. doi: 10.1097/MLG.0b013e31817c1368. [DOI] [PubMed] [Google Scholar]
- 39.Arabi Y.M., Mandourah Y., Al-Hameed F., Sindi A.A., Almekhlafi G.A., Hussein M.A. Corticosteroid therapy for critically ill patients with middle east respiratory syndrome. Am J Respir Crit Care Med. 2018;197(6):757–767. doi: 10.1164/rccm.201706-1172OC. [DOI] [PubMed] [Google Scholar]
- 40.Bousquet J., Akdis C., Jutel M., Bachert C., Klimek L., Agache I. Intranasal corticosteroids in allergic rhinitis in COVID-19 infected patients: an ARIA-EAACI statement. Allergy. 2020 doi: 10.1111/all.14302. [DOI] [PubMed] [Google Scholar]
- 41.Shang L., Zhao J., Hu Y., Du R., Cao B. On the use of corticosteroids for 2019-nCoV pneumonia. Lancet. 2020;395(10225):683–684. doi: 10.1016/S0140-6736(20)30361-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Sastre J., Mosges R. Local and systemic safety of intranasal corticosteroids. J Investig Allergol Clin Immunol. 2012;22(1):1–12. [PubMed] [Google Scholar]
- 43.Damm M., Pikart L.K., Reimann H., Burkert S., Göktas Ö., Haxel B. Olfactory training is helpful in postinfectious olfactory loss: a randomized, controlled, multicenter study. Laryngoscope. 2014;124(4):826–831. doi: 10.1002/lary.24340. [DOI] [PubMed] [Google Scholar]
- 44.Zou L., Ruan F., Huang M., Liang L., Huang H., Hong Z. SARS-CoV-2 Viral Load in Upper Respiratory Specimens of Infected Patients. N Engl J Med. 2020;382(12):1177–1179. doi: 10.1056/NEJMc2001737. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Hummel T., Whitcroft K.L., Andrews P., Altundag A., Cinghi C., Costanzo R.M. Position paper on olfactory dysfunction. Rhinol Suppl. 2017;54(26):1–30. doi: 10.4193/Rhino16.248. [DOI] [PubMed] [Google Scholar]
- 46.Wilder-Smith A., Teleman M.D., Heng B.H., Earnest A., Ling A.E., Leo Y.S. Asymptomatic SARS coronavirus infection among healthcare workers. Singapore Emerg Infect Dis. 2005;11(7):1142–1145. doi: 10.3201/eid1107.041165. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Organization WHO, WHO Middle East repiratory syndrome coronavirus (MERS-CoV) Global summary and assessment of Risk, August 18 2018. https://www.who.int/csr/disease/coronavirus_infections/risk-assessment-august-2018.pdf?ua=1.