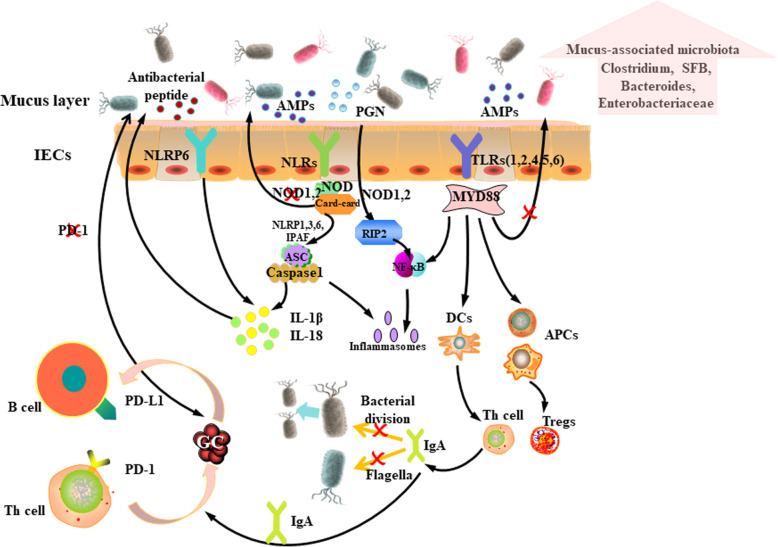
Fig. 1.
TLRs and NLRs effectively regulate intestinal immune function. The lack of the TLR adapter MYD88 will alter the composition of the microbiota, resulting in an increase in the amount of the mucus-associated microbiota. The lack of nucleoside-binding oligomeric domain protein 1 (NOD1) leads to an increase in the size of the of microbiota, including increased numbers of Clostridium, Bacteroides, segmented filamentous bacteria (SFB), and Enterobacteriaceae. Lack of NOD2 also leads to an increase in the size of the mucus-associated microbiota, which induces inflammation and colorectal cancer. The microbiota produce metabolites that activate NOD-, LRR-, and pyrin domain-containing 6 (NLRP6) and secretes interleukin (IL)-18, which maintains the stability of the mucus, and antimicrobial peptides. Activation of antigen-presenting cells (APCs) promotes the differentiation of CD4+ T cells into T helper (Th) cells and regulatory T cells (Tregs). Th cells regulate the function of the intestinal microbiota via the expression of immunoglobulin A (IgA). Furthermore, the secretion of IgA is regulated by the specific binding of PD-1 on the surface of Th cells to PD-L1 on the surface of B cells