Abstract
Background and aims
The relationship between severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) disease (COVID-19) and diabetes mellitus is bidirectional. On one hand, diabetes mellitus is associated with an increased risk of severe COVID-19. On the other hand, new onset diabetes and severe metabolic complications of pre-existing diabetes, including diabetic ketoacidosis (DKA) have been observed in patients with COVID-19. In this report, we describe two patient with diabetes mellitus who presented to our hospital with DKA. We also reviewed almost all published cases of DKA that had been precipitated by COVID-19.
Methods
Two patients were admitted with DKA, who were diagnosed to have COVID-19 on the basis of real time reverse transcription-polymerase chain reaction (RT-PCR) assay. Detailed history, anthropometry, laboratory investigations, imaging studies, clinical course and management outcomes were documented.
Results
First patient (30-year-male) had undiagnosed diabetes and no other comorbidities, and COVID-19 precipitated DKA. He also had COVID-19-associated pneumonia. Second patient (60-year-male) had long duration hypertension with no prior history of diabetes and developed cerebrovascular accident (CVA). He was also diagnosed with COVID-19 (RT-PCR assay) and DKA in the hospital. CVA and COVID-19 could have precipitated DKA. Both patients responded well to treatment and were discharged in a stable condition.
Conclusions
These cases show that COVID-19 can precipitate DKA in a significant number of patients. DKA can occur in patients with pre-existing diabetes or newly diagnosed diabetes. As COVID-19 and diabetes are prevalent conditions, high degree of suspicion is required to diagnose DKA timely in order to improve the prognosis of COVID-19-related diabetic ketoacidosis.
Keywords: COVID-19, Diabetic ketoacidosis, Coronavirus, Metabolic complications
Highlights
-
•
Diabetes mellitus is associated with an increased risk of severe COVID-19.
-
•
COVID-19 may precipitate diabetic ketoacidosis in patients with new onset or pre-existing diabetes.
-
•
In this report, two patients with diabetes mellitus presented with diabetic ketoacidosis precipitated by COVID-19.
1. Introduction
In December 2019, unexplained severe viral pneumonia occurred in Wuhan, Hubei province, in China [1,2]. A novel coronavirus, severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), was isolated from patients with this pneumonia [3]. Since the COVID-19 pandemic began in China, more than 1.28 million confirmed cases and around 30,645 COVID-19-related deaths have been reported in India (as of July 23, 2020). Individuals with diabetes are more likely to suffer severe consequences, including death. Recent studies have shown that advanced age or underlying medical comorbidities, such as cardiovascular disease, diabetes mellitus, hypertension, and obesity are risk factors for severe illness and mortality among patients with COVID-19 [4].
Acute hyperglycemic crises – diabetic ketoacidosis (DKA) and hyperosmolar hyperglycemic state (HHS), are the serious acute metabolic complications of diabetes, and commonly precipitated by infection. In a retrospective study from China, 42 (6.4%) patients admitted with COVID-19 had ketosis out of which 15 (35.7%) had diabetes. Three (20%) out of 15 patients with diabetes had DKA [4]. A few case reports also were published that COVID-19 may trigger acute hyperglycemic crises (DKA/HHS) in patients with inadequately controlled diabetes, as well as newly diagnosed diabetes [5,6]. Here, we describe two patients with confirmed COVID-19 who presented to our emergency department (ED) with DKA. We also reviewed almost all published cases of COVID-19-related DKA.
2. Methods
Demography, detailed medical history, physical examination, laboratory investigations including real time RT-PCR test, computed tomography (CT) imaging studies, treatment given, clinical course and management outcomes were documented prospectively. Informed consent was obtained from both patients for the study. Diabetic ketoacidosis was defined as plasma glucose >250 mg/dL, a positive test for urine or serum ketones, and arterial pH < 7.35 and/or serum HCo3 <18 mmol/L.
3. Results
3.1. Case 1
Our first patient was a 30-year-old man who presented with general weakness, fever, loss of taste and mild dyspnea of 6 days’ duration. He had a history of contact with a COVID-19 patient. He tested positive for SARS COV-2 on RT-PCR assay. He was initially managed at home. However, his condition worsened and presented to our emergency department with progressive breathlessness and unresolved fever. The patient reported no prior history of diabetes or other comorbidities. There was no family history of diabetes. At admission, his blood pressure was 152/84 mmHg, heart rate of 122 beats/min and respiratory rate of 24 breaths/min. His body temperature was 100 °F, and oxygen saturation of 90% by pulse oximetry on room air. His investigations (Table 1 ) revealed random plasma glucose of 555 mg/dL with venous blood gas analysis on room air indicating metabolic acidosis (pH-7.07 and HCO3-6.1mmol/L). Urine ketones were present. His glycosylated hemoglobin (HbA1c) was 9.6%. He was diagnosed to have moderate-severe DKA and management was initiated with initial intravenous fluid replacement followed by intravenous insulin infusion. Serum electrolytes were closely monitored. The chest imaging (X ray) revealed patchy airspace opacities in bilateral lung fields and HRCT chest showed ground-glass opacities in bilateral upper lobes and ground-glass opacities along with early consolidation in bilateral lower lobes and lingular segment of left upper lobe (Fig. 1 ). His laboratory investigations and imaging characteristics were consistent with moderately severe COVID-19 as per the criteria set by Ministry of Health and Family Welfare, Government of India. Therefore, anti-viral agent (Inj. Remdesivir), empirical antibiotics, steroids and other symptomatic respiratory treatment for COVID-19 was instituted. He was also started on Inj. Enoxaparin in view of elevated D-dimer levels. Patient was admitted in intensive care setting for close monitoring of the clinical status and inflammatory markers. He improved well with the above management (his metabolic acidosis improved, blood glucose levels stabilized, and blood parameters returned to normal). DKA resolved on the second day. Once patient stabilized, subcutaneous insulin was initiated. He was discharged in a stable condition with adequate education regarding the management of diabetes at home.
Table 1.
Laboratory investigations of the two patients at admission.
| Parameter | Case 1 | Case 2 | Reference range |
|---|---|---|---|
| pH | 7.07 | 7.30 | 7.25–7.35 |
| HCO3 (mmol/L) | 6.1 | 13 | 22–28 |
| Hemoglobin (g/dL) | 14.5 | 15.2 | 13.0–17.0 |
| Total leucocyte count (x103/μL) | 13.6 | 21.0 | 4.0–10.0 |
| ESR (mm/hr) | 16 | 10 | 0–14 |
| Sodium (mmol/L) | 131 | 134 | 135–145 |
| Potassium (mmol/L) | 3.9 | 3.7 | 3.5–5.1 |
| Chloride (mmol/L) | 110 | 96 | 95–110 |
| Creatinine (mg/dL) | 0.7 | 0.8 | 0.8–1.5 |
| Anion Gap (mmol/L) | 11.9 | 16.2 | 12–18 |
| Lactate (mmol/L) | 1.22 | 1.13 | 0.5–1.5 |
| Glycated hemoglobin (%) | 9.6 | 12.6 | ≤5.6 |
| SGPT (U/L) | 61 | 24 | 21–72 |
| CRP (mg/L) | 156.6 | 13.7 | 0–10 |
| IL-6 | 60 | 12 | <6 |
| Ferritin (ng/mL) | 817 | 135 | 17.9–464 |
| D-dimer (mg/L) | 1.86 | 0.88 | 0.00–0.50 |
ESR, erythrocyte sedimentation rate; SGPT, serum glutamyl pyruvate transaminase; CRP, C-reactive protein, IL-6, interleukin-6.
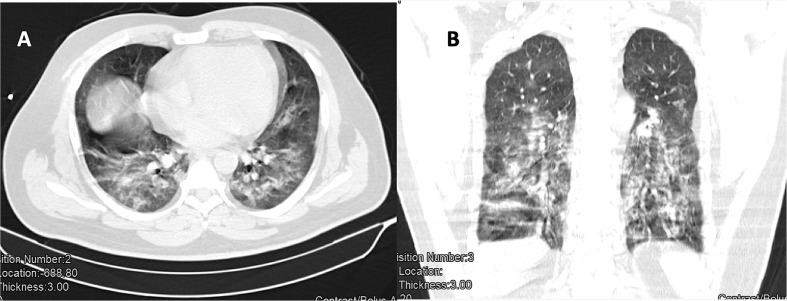
Fig. 1.
Axial (A) and coronal (B) images of HRCT chest (patient 1) showing ground glass opacities and early consolidation changes in bilateral lower lung fields.
3.2. Case 2
Our second patient was a 60-year-old man, who had a long duration hypertension. He had no personal history of diabetes. He presented to our emergency department with sudden onset uneasiness and inability to move the left upper limb associated with weakness of left lower limb. He was not able to walk. His initial blood pressure was 220/180 mm Hg, heart rate 126 beats/min, respiratory rate 26 breaths/min, and body temperature 99 °F. His oxygen saturation was 92% by pulse oximetry on room air. Upon admission, random blood glucose was 582 mg/dL and HbA1c was 12.6%. Venous blood gas analysis on room air revealed a compensated metabolic acidosis (pH-7.30 and HCO3-13 mmol/L), urine ketones were present (Table 1). He was managed with intravenous fluid, intravenous insulin infusion with monitoring of serum electrolytes. Due to the high prevalence of COVID-19 and atypical clinical presentations that are known to occur with COVID-19, throat swab was sent for testing and was confirmed to have COVID-19 on the basis of RT-PCR assay. HRCT chest did not reveal any significant lung pathology. CT head and CT angiography of brain and neck revealed hypoperfusion of right MCA territory, consistent with acute cerebrovascular accident. He was managed as per neurology guidance (thrombolysed with intravenous Alteplase). His laboratory investigations were consistent with mild-moderate COVID-19. Therefore, anti-viral agent (Inj. Remdesivir), empirical antibiotics and other symptomatic respiratory treatment for COVID-19 was instituted. He was also started on Inj. Enoxaparin in view of elevated D-dimer levels. Patient was admitted in intensive care setting for close monitoring of the clinical, and neurological status. He improved well with the above management and was discharged in stable condition with adequate education regarding the management of stroke and diabetes at home.
4. Discussion
Herein we report two patients with DKA precipitated by COVID-19 in patients with underlying undiagnosed diabetes. The impact of diabetes on the severity of COVID-19 and occurrence of new onset diabetes and severe metabolic complications of pre-existing diabetes, including DKA and HHS in patients with COVID-19 pose challenges in clinical management [6]. DKA occurs as a result of insulin deficiency and increased counterregulatory responses, which favour the production of ketones. Interleukin-6 (IL-6) levels have been shown to be elevated in both DKA and COVID-19, and may be an important prognostic factor [7]. Both of our cases had elevated IL-6 levels (Table 1). In our cases, there was no previous history of diabetes and the severe DKA episode that occurred leading to hospitalisation in an intensive care setting might be due to the triggering effect of COVID-19 on diabetes. The exact pathogenic mechanisms involved are yet to be determined. However, the role of the inflammatory cytokines released during the viral illness have been implicated.
The interactions between SARS-CoV-2 and the renin angiotensin-aldosterone system (RAAS) might provide another mechanism in the pathophysiology of DKA [8]. Angiotensin-converting enzyme 2 (ACE2) is a crucial enzyme in the RAAS system. It catalyzes the conversion of angiotensin II to angiotensin. ACE2 is highly expressed in the lungs and pancreas. It serves as the entry point for SARS-CoV-2. Expression of ACE2 is downregulated after endocytosis of the virus complex [8,9]. The possible implications of these interactions are twofold. Firstly, entry of SARS-CoV-2 into pancreatic islet cells may directly aggravate beta cell injury [10]. Secondly, downregulation of ACE2 after viral entry can lead to unopposed angiotensin II, which may impede insulin secretion [11]. These 2 factors might have contributed to the acute worsening of pancreatic beta cell function and precipitated DKA in our patients. In addition, the relationship between SARS-CoV-2 and the RAAS can complicate DKA management. Excessive fluid resuscitation may potentiate acute respiratory distress. Therefore, proper fluid management is vital in these patients. Furthermore, angiotensin II stimulates aldosterone secretion, potentiating the risk of hypokalemia, which may necessitate more potassium supplementation in order to continue intravenous insulin to suppress ketogenesis. To our knowledge few reports of DKA in COVID-19 have been published. Table 2 shows the summary of all the previous published reports [5,11,12,16].
Table 2.
Summary of the previous published cases of DKA in COVID-19.
| Case report | Age (years) | Presenting features | Initial RBS | HbA1c at admission | Comorbidities | Outcome |
|---|---|---|---|---|---|---|
| Chee et al. (2020) (11) | 37/male | Fever, vomiting, polyuria, polydipsia | 714 | 14.2 | None | Discharge |
| Kim et al. (2020) (12) | 59/male | General weakness, polyuria, polydipsia, mild dyspnoea | 655 | 11.4 | T2D, hypertension | Death |
| Goldman et al. (2020) (16) | 4 patients Age 40-82 | Fever, dyspnoea | 342–468 | 9.5–12.8 | One-none Three-T2D | Two-deaths Two-improved |
| Li et al. (2020) (5) | 3 patients Age 26-54 | General weakness, fever, dyspnoea, polyuria, polydipsia | 298–406 | 6.8–7.3 | – | One-death Two-Improved |
| Current study (2020) | 30/male | General weakness, fever, loss of taste and mild dyspnoea | 555 | 9.6 | None | Discharge |
| 60/male | Cerebrovascular accident | 582 | 12.6 | Hypertension | Discharge |
Emerging information suggests that individuals with diabetes are at increased risk for complications including death among COVID-19 patients [13]. According to a clinical report in China involving 1099 confirmed COVID-19 patients, diabetes was the second most common comorbidity (16.2%) among severe 173 cases [14]. There are not enough evidences to determine the risk of diabetes for poor outcomes in COVID-19 patients yet, a small study showed that COVID-19 patients with diabetes were not only at higher risk of severe pneumonia but also release excessive inflammatory biomarkers [15]. Our patient 1 also had severe pneumonia based on the HRCT grading. These results suggest that people with comorbidities, especially with diabetes, are susceptible to COVID-19. It is well known that acute hyperglycemic crises are significantly related to morbidity or death in people with diabetes [16].
5. Conclusions
COVID-19 may aggravate pancreatic beta cell function and precipitate DKA in patients with pre-existing or newly onset diabetes, as demonstrated by our cases. We also highlight that aggressive management with close monitoring in an ICU setting and timely intervention with the available treatment may lead to improved prognosis. As both conditions (diabetes mellitus and COVID-19) are highly prevalent in our country, high degree of suspicion is required to diagnose DKA timely in order to improve the prognosis of COVID-19-related acute hyperglycemic complications.
Author contributions
PKR was involved in patient management, revised manuscript, approved manuscript. MSK wrote manuscript, revised and approved manuscript. YM was involved in patient management, approved manuscript, SKM was involved in patient management, revised and approved the manuscript.
Declaration of competing interest
The authors declare no competing interests.
References
- 1.Wang D., Hu B., Hu C. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. J Am Med Assoc. 2020;323(11):1061–1069. doi: 10.1001/jama.2020.1585. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Huang C., Wang Y., Li X. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. 2020;395(10223):497–506. doi: 10.1016/S0140-6736(20)30183-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Guan W.J., Ni Z.Y., Hu Y. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med. 2020;382(18):1708–1720. doi: 10.1056/NEJMoa2002032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Zhou F., Yu T., Du R. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet. 2020;395(10229):1054–1062. doi: 10.1016/S0140-6736(20)30566-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Li J., Wang X., Chen J., Zuo X., Zhang H., Deng A. COVID-19 infection may cause ketosis and ketoacidosis. Diabetes Obes Metabol. 2020 doi: 10.1111/dom.14057. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Palermo N.E., Sadhu A.R., McDonnell M.E. Diabetic ketoacidosis in COVID-19: unique concerns and considerations. J Clin Endocrinol Metab. 2020;105(8) doi: 10.1210/clinem/dgaa360. dgaa360. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Vaduganathan M., Vardeny O., Michel T., McMurray J.J.V., Pfeffer M.A., Solomon S.D. Renin-angiotensin-aldosterone system inhibitors in patients with Covid-19. N Engl J Med. 2020;382(17):1653–1659. doi: 10.1056/NEJMsr2005760. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Bornstein S.R., Dalan R., Hopkins D., Mingrone G., Boehm B.O. Endocrine and metabolic link to coronavirus infection. Nat Rev Endocrinol. 2020;16(6):297–298. doi: 10.1038/s41574-020-0353-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Yang J.K., Lin S.S., Ji X.J., Guo L.M. Binding of SARS coronavirus to its receptor damages islets and causes acute diabetes. Acta Diabetol. 2010;47(3):193–199. doi: 10.1007/s00592-009-0109-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Carlsson P.O., Berne C., Jansson L. Angiotensin II and the endocrine pancreas: effects on islet blood flow and insulin secretion in rats. Diabetologia. 1998;41(2):127–133. doi: 10.1007/s001250050880. [DOI] [PubMed] [Google Scholar]
- 11.Chee Y.J., Ng S.J.H., Yeoh E. Diabetic ketoacidosis precipitated by Covid-19 in a patient with newly diagnosed diabetes mellitus. Diabetes Res Clin Pract. 2020;164:108166. doi: 10.1016/j.diabres.2020.108166. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Kim N.Y., Ha E., Moon J.S., Lee Y.H., Choi E.Y. Acute hyperglycemic crises with coronavirus disease-19: case reports. Diabetes Metab J. 2020;44(2):349–353. doi: 10.4093/dmj.2020.0091. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Yang X., Yu Y., Xu J. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study. Lancet Respir Med. 2020;8(5):475–481. doi: 10.1016/S2213-2600(20)30079-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Guo W., Li M., Dong Y. Diabetes is a risk factor for the progression and prognosis of COVID-19. Diabetes Metab Res Rev. 2020:e3319. doi: 10.1002/dmrr.3319. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Kim K.J., Kwon T.Y., Yu S. Ten-year mortality trends for adults with and without diabetes mellitus in South Korea, 2003 to 2013. Diabetes Metab J. 2018;42(5):394–401. doi: 10.4093/dmj.2017.0088. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Goldman N., Fink D., Cai J., Lee Y.N., Davies Z. High prevalence of COVID-19-associated diabetic ketoacidosis in UK secondary care. Diabetes Res Clin Pract. 2020;166:108291. doi: 10.1016/j.diabres.2020.108291. [DOI] [PMC free article] [PubMed] [Google Scholar]