Highlights
-
•
Weight regain is a common problem within Bariatric Surgery and about 20% of patients who undergo Roux-en-Y gastric bypass patients may experience weight regain.
-
•
Among the arsenal of alternatives to treat weight regain we have endoscopic therapies and surgical modifications of the primary technique, among others.
-
•
This case represents the first report in which endoscopic therapy via transjejunal is used in conjunction with distalization of the biliopancreatic limb.
Keywords: Revisional surgery, Weight regain, Biliopancreatic limb distalization, Argon plasma coagulation, Gastric bypass
Abstract
Introduction
In recent years there has been a significant growth in the percentage of patients with weight regain after Roux-en-Y gastric bypass (RYGB). Approximately 20% RYGB patients may experience weight regain 24 months after the intervention.
Presentation of case
A 53 yr male patient who underwent RYGB in 2011 with an initial weight of 140 kg and BMI of 44.19 kg/m who consults in 2019 for a weight regain of 45.9%. Transoperative endoscopy assessment revealed a gastric pouch and gastrojejunal anastomosis with a diameter of 7 cm and 2.5 cm respectively. During the procedure we found a common channel of 725 cm, it is decided to shorten it through the distalization of the biliopancreatic limb. Afterward using the same laparoscopic ports to introduce the endoscope through jejunal cane to realize the APC therapy. He was discharged on the 2nd-day, without any complaint.
Discussion
The purpose of this case report is to expose the viability to perform a combined surgical technique such as the distalization of the biliopancreatic limb with endoscopic techniques of argon plasma coagulation (APC) via transjejunal in the same operative course. Using this combined technique we can increase hypoabsortive and restrictive components that would represent a secure and efficient weight loss in our patient.
Conclusions
This innovative technique can represent a viable alternative that is secure and reproducible in revisional surgery for weight regain context.
1. Introduction
Roux-en-Y Gastric Bypass (RGYB) is one of the most effective treatment for weight control and remission of many metabolic comorbidities associated with obesity. Approximately 20% RYGB patients may experience weight regain 24 months after the intervention [1]. This is attributed to multiple factors related to the patient such as sedentary lifestyle, metabolic factors, or inappropriate diet and others related to the surgery itself, such as inadequate surgical technique, dilatation of the gastric pouch, or dilatation of the gastro-jejunal anastomosis.
In the evaluation of patients with weight regain a therapeutic option is revisional bariatric surgery, which can be the conversion of one technique to another technique or modification of the primary surgery such as distalization of the biliopancreatic limb or gastric pouch resizing [2]. Also is possible to utilize endoscopic procedures such as Argon Plasma Coagulation (APC) to reduce the diameter gastrojejunal anastomosis [3]. This innovative technique has been reported in line with the SCARE criteria [4].
2. Presentation of case
A 53 yr male patient who underwent RYGB in 2011 with an initial weight of 140 kg and body mass index (BMI) of 44.19 kg/m2. Reaching a minimum weight of 103 kg, which is the equivalent to 53.62% of the excess weight loss. The patient consults in 2019 for weight regain, based on our medical evaluation our team determines weight of 120.7 kg and BMI of 37.87 kg/m2 and weight regain of 45.9%; with no history of drugs, allergies, or any other relevant disease.
In the multidisciplinary evaluation, we performed laboratory work-up with normal parameters and trans-operative endoscopy that reports a gastric pouch with 7 cm of diameter and a gastrojejunal anastomosis diameter of 2.5 cm.
2.1. Management/operative course
Revisional bariatric surgery is performed with the patient in the French position by a bariatric surgeon with 8 years of exprience. During the exploration of the bowel, we found an alimentary limb of 140 cm, a biliopancreatic limb of 110 cm, and a common channel of 725 cm. It is decided to perform a distalization of the biliopancreatic limb, using a blue load to resect the intestinal segment of the alimentary limb proximal to the jejunojejunal anastomosis. Posteriorly, we began to measure the common channel to create the new jejunojejunal anastomosis at 300 cm of the ileocecal valve (Fig. 1) distalizing the biliopancreatic limb to 535 cm and shortening the common channel to 300 cm.
Fig. 1.
Jejuno-jejunal anastomosis.
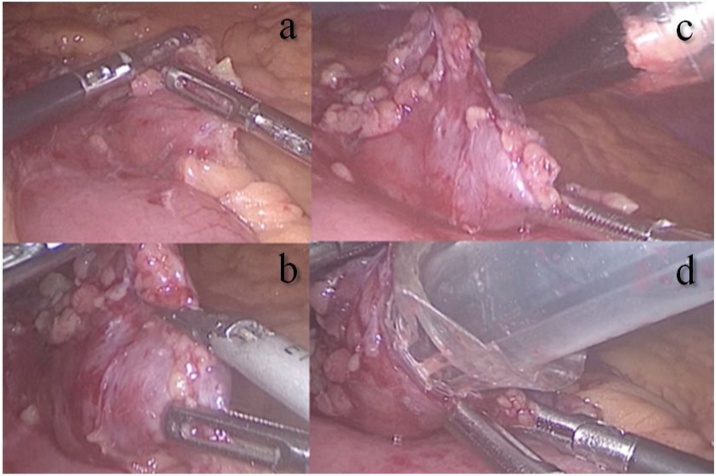
Transoperatively, assessing via endoscopy a gastric pouch of 7 cm is measured with a large non-functional limb (jejunal cane). Subsequently, it is decided to perform an enterotomy in the jejunal cane of the gastrojejunal anastomosis with a harmonic scalpel, then a laparoscopic port is used to introduce a trocar with a 12 mm balloon (Fig. 2) where the endoscope is introduced (via transjejunal) for the observation of the gastric pouch and to perform in the gastrojejunal anastomosis the argon plasma coagulation therapy to reduce the size of the anastomosis (Fig. 3).
Fig. 2.
a. Non-functional limb / b. Enterotomy of the non-functional limb. / c. Introduction of the laparoscopic guider. / d. Introduction of the trocar with a balloon.
Fig. 3.
Laparoscopic and endoscopic view of APC therapy.
At the moment we finalize the endoscopic procedure we proceed to do the resection of the jejunal cane with a blue load (Fig. 4), finalizing then the surgery with a duration of 150 min without complications.
Fig. 4.
Resection of the non-functional limb.
2.2. Postoperative course
The patient ambulates 6 h after the surgery, initiating oral tolerance after 48 h during the postoperative period, with a satisfactory recovery being discharged under medical and nutritional indications. No intraoperative or postoperative complications were reported. 10 months after surgery the patient has lost 14 kg with a BMI 33.46 kg/m2 and all laboratory parameters are within normal limits (Table 1). Normal hepatic and renal function. Adequate eating pattern, taking multivitamin supplements, and no gastroesophageal reflux disease (GERD) or dysphagia symptoms. The patient is satisfied with the results without any complaint.
Table 1.
Hematological and biochemical studies.
| Hemoglobin | 134 g/dL |
| Hematocrit | 43% |
| Iron | 6797 mcg/dl |
| Vit B12 | 941 pg/mL |
| Albumin | 4,0 g/dl |
| Total Protein | 6,9 g/dl |
| Total Cholesterol | 142 mg/dl |
| Triglycerides | 68 mg/dl |
| HDL | 440 mg/dl |
| LDL | 849 mg/dl |
| VLDL | 135 mg/dl |
| Glucose | 88 mg/dl |
| Hemoglobin A1C | 4,6% |
3. Discussion
Revisional surgery is a growing area within bariatric surgery with the advent of greater acceptance and a greater amount of bariatric procedures worldwide. There is not yet a concession of defined criteria of when to perform revisional surgery, but worldwide 20% of patients with bariatric procedures experience negative results such as inadequate weight loss or weight regain [5]. These negative results are the main criteria to approach the patient with revisional surgery.
Among the options within revisional surgery in bariatric surgery, we have procedures such as the conversion of one procedure to another, the review and modification of the primary procedure, and the reversal of the primary procedure. There are also complementary endoscopic alternatives as a solution for patients with inadequate weight loss or weight regain. The endoscopic technique of Argon Plasma Coagulation is one of the most used and accepted techniques [6].
In revisional surgery, an effective option is the distalization of the biliopancreatic limb to achieve with this procedure a shortening of the common channel giving a greater hypoabsortive component. Shah, K, et al. [7] with 187 patients where they assess the importance of the modification of the total length of the common channel, making a comparison between 3 groups with different lengths. They concluded that with a shortening of the common channel and a biliopancreatic limb distalization a sustained long-term weight loss can be achieved. In this study, the lengths of the second group were biliopancreatic limb 200 cm and common channel 150 cm, and in the third group a biliopancreatic limb of 200 cm and a common channel of 200 cm.
In this case, the biliopancreatic limb was distalized to 535 cm and the new common channel was shortened to 300 cm. We consider the nutritional complications of the initial technique described by Sugerman in 1997 [8] with a common channel of 150 cm; regarding this, we made a moderate distalization of 300 cm in this case.
This procedure is not exempt from complications. Tran D, et al. [9] reports a complication rate of 11.9% and 0.6% mortality in the distalization of biliopancreatic limb. Also Fobi, et al. [10] in its series of 65 patients determined that the weight loss is greater with the distalization of the biliopancreatic limb but with the consequence of a higher percentage of complications mainly protein malnutrition and diarrhea. This study also describes a racial difference where African-Americans and Asians do not tolerate the distal Roux-en-Y gastric bypass (DRYGBP) as well as whites.
As previously mentioned, with the endoscopic alternatives, APC is a technique that in itself increases the restrictive component in gastrojejunal anastomosis with abnormal dilation. This procedure consists of a noncontact electrocoagulation method in which radiofrequency energy is applied to the tissue using ionized gas. A study [3] with a series of 30 patients with weight regain associated with gastrojejunal dilation were subjected to argon plasma coagulation therapy in sessions with intervals of 8 weeks, achieving a 66.89% reduction in the final diameter of the anastomosis and a weight loss of 15.48 kg of the 19.6 kg of regained weight after RYGB.
In our case, it is decided to perform a combination of a laparoscopic and endoscopic technique at the same surgical time. We begin with the distalization of the biliopancreatic limb and then with the introduction of a trocar of 12 mm balloon towards the light of the jejunal limb (using a transjejunal access through pouch-jejunal anastomosis limb) assisted by laparoscopy. Afterward, to the gastrojejunal anastomosis was applied argon plasma coagulation therapy. With this, we seek to reduce the interval upon the first session of argon plasma coagulation therapy after the surgery, with the same endoscopic control of 8 weeks between one session and another session if necessary.
Here we show an innovative example of the feasibility of performing two different procedures. This technique combines two different methods that provide good results in the patient and can represent a starting point for future implementation. The combination of an endoscopy and laparoscopic procedure brings the benefits to improve restrictive and hypoabsortive components in a single surgical act.
4. Conclusion
We concluded that performing these procedures in the same surgical intervention is technically viable, reproducible, and safe for the patient under a trained and experienced surgical team. The surgical time is not significantly increased and the combination of increasing the hypoabsortive and restrictive components is achieved by maintaining the basic initial concept of gastric bypass. It is important to emphasize that according to what has been reported in the literature, a common channel shorter than 200 cm is not recommended due to the high risk of malnutrition. This technique can represent an important alternative in an area that is in wide development as it is in bariatric revisional surgery. However, it is necessary to conduct studies on a larger scale to have conclusive results to implement this new technique. This procedure may be the beginning of a new field of alternatives in revisional bariatric surgery.
Declaration of Competing Interest
The author declare they have no conflict of interest.
Funding
This study was self-funded. No funding was received for this article.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Consent
Informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal on request.
Author contribution
Borjas, Guillermo M.D: study concept, design, data collection, data analysis, data interpretation, patient management, and writing the paper.
Marrufo, Mario M.D: data collection, patient management.
Sanchez, Nestor M.D: study concept, design, data collection, data analysis, data interpretation, patient management, and writing the paper.
Urdaneta, Ali M.D: study concept, design, data collection, data analysis, data interpretation, and writing the paper.
González, María M.D: study concept, design, data collection, data analysis, data interpretation, and writing the paper.
Ramos, Eduardo M.D: study concept, design, data collection, data analysis, data interpretation, and writing the paper.
Maldonado, Andres M.D: study concept, design, data collection, data analysis, data interpretation, and writing the paper.
Registration of research studies
researchregistry6042.
Guarantor
Dr. Guillermo Borjas.
Provenance and peer review
Not commissioned, externally peer-reviewed.
Acknowledgments
We thank each person in my team for putting all their efforts into taking this intuition to the top level and all my patients without their trust we could never reach this greatness.
Footnotes
Supplementary material related to this article can be found, in the online version, at https://doi.org/10.1016/j.ijscr.2020.09.168.
Contributor Information
Guillermo Borjas, Email: drguillermoborjas@hotmail.com.
Mario Marruffo, Email: mariomarruffo@gmail.com.
Nestor Sanchez, Email: nestormsf@hotmail.com.
Ali Urdaneta, Email: ali_urdaneta@hotmail.com.
María Gonzalez, Email: angeles0807@gmail.com.
Eduardo Ramos, Email: eduandresrr@gmail.com.
Andres Maldonado, Email: maldonadoandres94@gmail.com.
Appendix A. Supplementary data
The following is Supplementary data to this article:
References
- 1.Dayan D., Kuriansky J., Abu-Abeid S. Weight regain following Roux-en-Y gastric bypass: etiology and surgical treatment. Isr. Med. Assoc. J. 2019;12(21):823–828. [PubMed] [Google Scholar]
- 2.Ferraz A.A., de Siqueira L.T., Nunes Filho E. Revision surgery for treatment of weight regain after Roux-En-Y gastric bypass. Obes. Surg. 2014;24(1):2–8. doi: 10.1007/s11695-013-1055-3. [DOI] [PubMed] [Google Scholar]
- 3.Baretta G.A., Alhinho H.C., Matias J.E. Argon plasma coagulation of gastrojejunal anastomosis for weight regain after gastric bypass. Obes. Surg. 2015;25(1):72–79. doi: 10.1007/s11695-014-1363-2. [DOI] [PubMed] [Google Scholar]
- 4.Agha R.A., Borelli M.R., Farwana R., Koshy K., Fowler A., Orgill D.P., For the SCARE Group The SCARE 2018 statement updating consensus surgical CAse REport (SCARE) guidelines. Int. J. Surg. 2018;60:132–136. doi: 10.1016/j.ijsu.2018.10.028. [DOI] [PubMed] [Google Scholar]
- 5.Patel S., Szomstein S., Rosenthal R.J. Reasons and outcomes of reoperative bariatric surgery for failed and complicated procedures (excluding adjustable gastric banding) Obes. Surg. 2011;21:1209–1219. doi: 10.1007/s11695-010-0234-8. [DOI] [PubMed] [Google Scholar]
- 6.Brunaldi V.O., Jirapinyo P., de Moura D.T.H. Endoscopic treatment of weight regain following roux en Y gastric bypass: a systematic review and meta-analysis. Obes. Surg. 2018;28(1) doi: 10.1007/s11695-017-2986-x. [DOI] [PubMed] [Google Scholar]
- 7.Shah K., Nergård B.J., Fagerland M.W., Gislason H. Distal gastric bypass: 2-m biliopancreatic limb construction with varying lengths of common channel. Surg. Obes. Relat. Dis. 2019;15(9):1520–1526. doi: 10.1016/j.soard.2019.05.003. [DOI] [PubMed] [Google Scholar]
- 8.Sugerman H.J., Kellum J.M., DeMaria E.J. Conversion of proximal to distal gastric bypass for failed gastric bypass for super obesity. J. Gastrointest. Surg. 1997;1(6):517–526. doi: 10.1016/S1091-255X(97)80067-4. [DOI] [PubMed] [Google Scholar]
- 9.Tran D.D., Nwokeabia I.D., Purnell S. Revision of roux en y gastric bypass for weight regain: a systematic review of techniques and outcomes. Obes. Surg. 2016;26(7):1627–1634. doi: 10.1007/s11695-016-2201-5. [DOI] [PubMed] [Google Scholar]
- 10.Fobi M.A., Lee H., Igwe D., Jr. Revision of failed gastric bypass to distal roux en y gastric bypass: a review of 65 cases. Obes. Surg. 2001;11(2):190–195. doi: 10.1381/096089201321577866. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.