Abstract
Objective
To determine whether rapid administration of a crystalloid bolus of 30 mL/kg within 3 hours of presentation harms or benefits hypotensive patients with sepsis with a history of congestive heart failure (CHF).
Patients and Methods
A retrospective cohort study using Medicare claims data enhanced by medical record data from members of the High Value Healthcare Collaborative from July 1, 2013, to June 30, 2015, examining patients with a history of CHF who did (fluid bundle compliant [FBC]) or did not (NFBC) receive a volume bolus of 30 mL/kg within 3 hours of presentation to the emergency department. A proportional Cox hazard model was used to evaluate the association of FBC with 1-year survival.
Results
Of the 211 patients examined, 190 were FBC and 21 were NFBC. The FBC patients had higher average hierarchical condition category scores but were otherwise similar to NFBC patients. The NFBC patients had higher adjusted in-hospital and postdischarge mortality rates. The risk-adjusted 1-year mortality rate was higher for NFBC patients (hazard ratio, 2.18; 95% CI, 1.2 to 4.0; P=.01) than for FBC patients.
Conclusion
In a retrospective claim data-based study of elderly patients with a history of CHF presenting with severe sepsis or septic shock, there is an association of improved mortality with adherence to the initial fluid resuscitation guidelines as part of the 3-hour sepsis bundle.
Abbreviations and Acronyms: CHF, congestive heart failure; CMS, Centers for Medicare & Medicaid Services; ED, emergency department; FBC, fluid bundle compliant; HCC, hierarchical condition category; HR, hazard ratio; HVHC, High Value Healthcare Collaborative; NFBC, not fluid bundle compliant; SEP-1, Sepsis CMS Core Measure
The Surviving Sepsis guideline1 recommends early interventions in an attempt to normalize adequate perfusion and source control. Subsequently, Centers for Medicare & Medicaid (CMS) has mandated specific measures by requiring early antibiotic administration after blood cultures and lactate measurement (and repeat if lactate >2 mmol/L) in all patients with sepsis and a 30-mL/kg crystalloid infusion within the first 3 hours of sepsis recognition if there was sepsis-induced hypotension. Recognizing the dangers of volume overload due to aggressive resuscitation,2,3 clinicians are hesitant in complying with the fluid administration mandate in patients with a history of congestive heart failure (CHF).3,4 This barrier was highlighted during member site visits and in member group discussions regarding sepsis resuscitation bundle elements.
Within the High Value Healthcare Collaborative (HVHC),5 a consortium of health care systems that seeks to enhance health care value, we sought to determine whether complying with the CMS fluid mandate in Medicare patients 65 years or older with CHF (ejection fraction <35% and admission for CHF exacerbation or principal diagnosis of CHF within 12 months) was associated with in-hospital or after-discharge mortality for patients with sepsis.
Patients and Methods
Members of the HVHC voluntarily submitted data on our respective institution’s sepsis bundle compliance metrics. From the database of 5860-patient data, we examined CMS fee-for-service patients 65 years and older with a preexisting diagnosis of CHF who were admitted through the emergency department (ED) in 4 of the participating HVHC health care systems between July 1, 2013, and June 30, 2015, with an index episode diagnosis of severe sepsis or septic shock (based on sepsis-2 definition6), survived for at least 3 hours after ED triage, and for whom we had compliance data with the CMS sepsis bundle elements. Participating institutions included Dartmouth-Hitchcock, Intermountain Healthcare, Hawaii Pacific Health, and Mayo Clinic in Rochester, Minnesota. We used CMS claims to calculate the hierarchical condition category (HCC)7 scores, which is a risk-adjustment model that reflects the patient's clinical complexity.
The HVHC health care systems reported whether patients received a crystalloid fluid bolus of 30 mL/kg as 1 of the 4 elements of the 3-hour sepsis bundle (the other 3 being antibiotics, blood culture before antibiotic administration, and lactate measurement) if they had sepsis-related hypotension. We compared patients who received all elements of the bundle (fluid bundle compliant [FBC]) with those who received all elements except the fluid component (not fluid bundle compliant [NFBC]) among patients with a history of CHF.
Participating HVHC members provided information on preexisting CHF based on chart abstraction of a larger sepsis cohort. Patients qualified if they met all of the following criteria: (1) ejection fraction less than 35% at any time but more than 7 days preceding the sepsis event (to ensure that CHF was not a result of sepsis cardiomyopathy), (2) at least 1 inpatient admission with the principal diagnosis of CHF or at least 2 primary or specialty clinic encounters within 12 months before the sepsis presentation with a diagnosis of CHF in any diagnosis code position, and (3) 1 of the following International Classification of Diseases, Ninth Revision codes: hypertensive heart disease with heart failure (I402.01, 402.11, and 402.91) or heart failure (428.xx).
Data were analyzed using a Cox proportional hazards model with age, sex, type of sepsis, and HCC score as covariates and compliance with fluid bolus as an independent variable. The reported hazard ratios (HRs) are adjusted for all other covariates in the model. The primary outcome is the impact of compliance with the fluid bolus on survival 1 year from initial presentation to the ED, which is reported as HR with 95% CI. Statistical analysis was performed using SAS analytic software (SAS Institute Inc).
Results
A total of 481 patients with CHF matching criteria and a discharge diagnosis of severe sepsis or septic shock (based on sepsis-2 definition6) were submitted by members, of whom 468 patients had sepsis as the index diagnosis. Clearly documented intravenous fluid administration data were found for 433 patients. Forty-seven patients did not initially present to the ED, 19 had missing sex data, and another 12 patients were excluded because they did not receive broad-spectrum antibiotics within 3 hours of presentation. Of the remaining 355 patients, 211 (59%) could be linked to CMS records (Figure 1)
Figure 1.
Consolidated Standards of Reporting Trials diagram of study sample. CHF = congestive heart failure; CMS = Centers for Medicare & Medicaid Services; ED = emergency department.
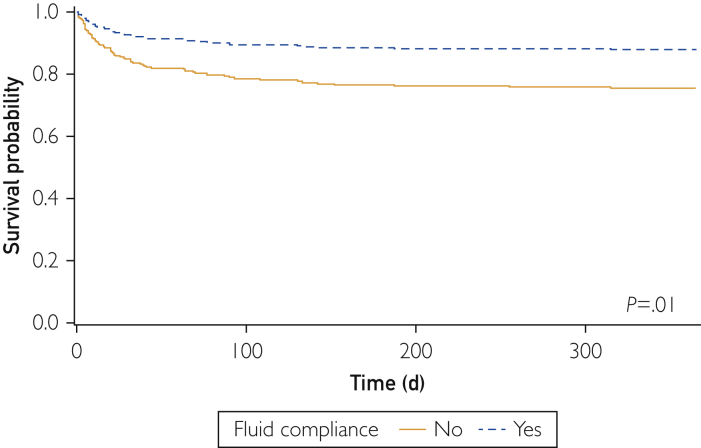
Of the 211 patients examined, 190 were FBC and 21 were NFBC. The FBC patients had a higher average HCC score (4.4±2.31 vs 3.4±2.46; not significant; P=.079) but were otherwise similar to NFBC patients in regard to age and frequency of septic shock (Table 1). The NFBC patients had higher in-hospital (57% [12 of 21] vs 31% [59 of 190]; P=.01) mortality rates. The increased risk for mortality was evident as early as 7 days after admission from the ED and persisted up to a year (Table 1). In the Cox proportional hazard model, higher HCC scores and not receiving the 30-mL/kg fluid bolus were associated with increased risk for mortality, but not age or sex (Table 2). The risk-adjusted 1-year mortality rate was higher for NFBC patients (HR, 2.18; 95% CI, 1.2 to 4.0; P=.01) than for FBC patients (Figure 2).
Table 1.
Demographic Data for the Medicare Cohort of Patients With Congestive Heart Failure Presenting to the Emergency Department With Severe Sepsis or Septic Shock
| Fluid Compliance |
P | ||
|---|---|---|---|
| Yes (n=190) | No (n=21) | ||
| Age (y), mean ± SD | 83.0±10.0 | 82.0±10.56 | .696 |
| Male sex, no. (%) | 93 (49) | 12 (57) | .50 |
| Septic shock, no (%) | 101 (53) | 11 (52) | .95 |
| Hierarchical condition category score, mean ± SD | 4.4±2.31 | 3.4±2.46 | .079 |
| In-hospital mortality, no (%) | 59 (31) | 12 (57) | .01 |
| Hazard ratio (95% CI) for mortality from admission if not fluid bundle compliant | |||
| 7 d | 1.93 (1.0-3.5) | .03 | |
| 14 d | 2.13 (1.2-3.9) | .01 | |
| 30 d | 2.17 (1.2-4.0) | .01 | |
| 90 d | 2.17 (1.2-4.0) | .01 | |
| 180 d | 2.18 (1.2-4.0) | .01 | |
| 1 y | 2.18 (1.2-4.0) | .01 | |
Table 2.
HRs for Mortality for Included Variables in the Cox Risk-Adjusted Hazard Modela
| Survival From Discharge | 7 d |
1 y |
||
|---|---|---|---|---|
| HRb (95% CI) | P | HR (95% CI) | P | |
| Agec | NS | |||
| Male sex | 0.8 (0.6-1.2) | 0.13 | 0.8 (0.5-1.2) | 0.13 |
| Severe sepsis | 1.7 (0.8-3.7) | 0.17 | 2.0 (0.9-4.3) | 0.08 |
| Septic shock | 1.8 (0.9-3.9) | 0.12 | 2.0 (0.9-4.3) | 0.07 |
| HCC score 2-4 | 2.6 (1.3-5.2) | 0.01d | 2.7 (1.4-5.4) | <0.01d |
| HCC score 4-6 | 2.6 (1.3-5.2) | 0.01d | 2.9 (1.5-5.7) | <0.01d |
| HCC score >6 | 2.4 (1.1-4.9) | 0.02d | 2.4 (1.2-5.0) | 0.02d |
| Not fluid bundle compliant | 1.9 (1.2-4.0) | 0.03d | 2.2 (1.2-4.0) | 0.01d |
HCC = hierarchical condition category; HR = hazard ratio; NS = not significant.
References for the HR are as follows: age younger than 65 years for age groups, female for male sex, sepsis for severe sepsis and septic shock, HCC score of 0 to 2 for the higher scores, and fluid bundle compliant for not fluid bundle compliant.
Age was analyzed in categories, data are suppressed in accordance with Centers for Medicare & Medicaid Services rules, but were nonsignificant for all categories.
Statistically significant.
Figure 2.
Risk-adjusted mortality for initial fluid compliance among patients with heart failure with sepsis-induced hypotension. Risk-adjusted for age, sex, type of sepsis, and hierarchical condition category scores.
Discussion
Elderly patients with preexisting CHF (as defined by ejection fraction <35% and recent admission for CHF exacerbation or CHF as principal diagnosis) who presented to HVHC EDs with severe sepsis and septic shock had higher in-hospital and 1-year mortality if the recommended 30-mL/kg fluid bolus was not given (57% [12 of 21] vs 31% [59 of 190]; P=.01; HR, 2.18; 95% CI, 1.2 to 4.0, respectively) during the initial resuscitation.
The National Sepsis CMS Core (SEP-1) measure rewards compliance with process measures that may not be related to outcomes. Rhee et al8 reported no difference in adjusted in-hospital mortality rates for SEP-1–compliant vs –noncompliant patients and recommended detailed risk adjustment to assess the association of SEP-1 compliance and mortality. However, several groups contradict this finding by reporting improved outcomes with improved compliance with SEP-1 metrics.9,10 For example, in one of the largest studies to date, data from New York City hospitals suggest improved outcomes with adherence to blood cultures, initiation of antibiotic treatment, and lactate measurement within the first 3 hours, but this benefit was not seen with the early completion of the 30-mL/kg fluid bolus compliance.9 The HVHC has improved bundle compliance rates among member institutions to more than 90%, mostly due to an increase in fluid bundle compliance to 94%. Patients with preexisting CHF presented a particular problem in treatment due to clinicians’ concern regarding volume overload and a lack of data to support the practice.
Our findings are consistent with the small subgroup analysis in a recent retrospective study that showed that a lack of fluid compliance within the first 3 hours among patients with a history of CHF was associated with increased mortality.11 Similarly, a recent study by Khan et al12 showed that in patients at risk for volume overload (including patients with heart failure), being compliant with fluid resuscitation recommendations was not at increased risk for needing invasive mechanical ventilatory support. Other studies have shown the benefit of an adequately higher volume of crystalloid early in the course of resuscitation in improving outcomes.13
A potential mechanism whereby adequate fluid resuscitation still benefits patients with a CHF history is that sepsis induces distributive shock superimposed on their cardiogenic insufficiency. Their long-term use of diuretics may exacerbate the impact of distributive shock. This combination may result in worsening perfusion pressure, leading to worse outcomes. Although we need to be very mindful of avoiding excessive volume resuscitation, initial resuscitation with 30 mL/kg of crystalloid may not be unreasonable even in patients with reduced cardiac reserve if they present with sepsis-induced hypotension.
The presented data are limited to the retrospective nature of the study and by the number of patients analyzed, along with the small cohort of patients who were NFBC. The latter group of 10% (21 of 211) of NFBC patients is consistent with the average HVHC fluid compliance. Patients who have existing CHF based on our criteria who present with sepsis to the ED are a challenging cohort to establish and are easier to analyze using a collaborative retrospective analysis as presented. Additionally, we used HCC score as a measure of risk adjustment (rather than other scores such as Acute Physiology and Chronic Health Evaluation) to reflect the patient’s clinical complexity.7 The HCC is a validated risk-adjustment model incorporating 70 condition categories used by CMS to assess clinical complexity and is updated regularly. Although the total fluid administered by 24 hours and beyond can influence outcomes, we were interested in adherence to the initial resuscitation bundle and outcomes. Therefore, we only focused on adherence to the initial fluid resuscitation guideline as it relates to their outcome, as long as they also received broad-spectrum antibiotics within the first 3 hours of presentation.
Conclusion
Elderly patients with preexisting CHF who present with sepsis-induced hypotension may benefit from receiving the recommended 30-vmL/kg fluid resuscitation as part of their early resuscitation bundle.
Acknowledgments
The data referenced in this publication were obtained from members of the High Value Healthcare Collaborative, including Dartmouth-Hitchcock, Intermountain Healthcare, Hawaii Pacific Health, and Mayo Clinic in Rochester, Minnesota. Centers for Medicare & Medicaid Services claims data were obtained through an approved Data Use Agreement for Research Identifiable Files (DUA #51958).
Footnotes
Grant Support: This work was funded by Members of the High Value Healthcare Collaborative, a consortium of health care delivery systems sharing data and experiences to improve quality, outcomes, and cost of care. The views expressed are those of the authors and not necessarily those of all participating High Value Healthcare Collaborative Members.
Potential Competing Interests: The authors declare no competing interests.
References
- 1.Rhodes A., Evans L.E., Alhazzani W., et al. Surviving Sepsis Campaign: international guidelines for management of sepsis and septic shock: 2016. Crit Care Med. 2017;45(3):486–552. doi: 10.1097/CCM.0000000000002255. [DOI] [PubMed] [Google Scholar]
- 2.Kelm D.J., Perrin J.T., Cartin-Ceba R., Gajic O., Schenck L., Kennedy C.C. Fluid overload in patients with severe sepsis and septic shock treated with early goal-directed therapy is associated with increased acute need for fluid-related medical interventions and hospital death. Shock. 2015;43(1):68–73. doi: 10.1097/SHK.0000000000000268. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Marik P.E., Linde-Zwirble W.T., Bittner E.A., Sahatjian J., Hansell D. Fluid administration in severe sepsis and septic shock, patterns and outcomes: an analysis of a large national database. Intensive Care Med. 2017;43(5):625–632. doi: 10.1007/s00134-016-4675-y. [DOI] [PubMed] [Google Scholar]
- 4.Leisman D.E., Goldman C., Doerfler M.E., et al. Patterns and outcomes associated with timeliness of initial crystalloid resuscitation in a prospective sepsis and septic shock cohort. Crit Care Med. 2017;45(10):1596–1606. doi: 10.1097/CCM.0000000000002574. [DOI] [PubMed] [Google Scholar]
- 5.Taenzer A., Kinslow A., Gorman C., et al. Dissemination and implementation of evidence based best practice across the High Value Healthcare Collaborative (HVHC) using sepsis as a prototype - rapidly learning from others. EGEMS (Wash DC) 2017;5(3):5. doi: 10.5334/egems.192. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Levy M.M., Fink M.P., Marshall J.C., et al. SCCM/ESICM/ACCP/ATS/SIS 2001 SCCM/ESICM/ACCP/ATS/SIS International Sepsis Definitions Conference. Crit Care Med. 2003;31(4):1250–1256. doi: 10.1097/01.CCM.0000050454.01978.3B. [DOI] [PubMed] [Google Scholar]
- 7.Evans M.A., Pope G.C., Kautter J., et al. Evaluation of the CMS-HCC risk adjustment model. 2011. https://www.cms.gov/Medicare/Health-Plans/MedicareAdvtgSpecRateStats/downloads/Evaluation_Risk_Adj_Model_2011.pdf Accessed October 15, 2019.
- 8.Rhee C., Filbin M.R., Massaro A.F., et al. Centers for Disease Control and Prevention (CDC) Prevention Epicenters Program Compliance with the national SEP-1 quality measure and association with sepsis outcomes: a multicenter retrospective cohort study. Crit Care Med. 2018;46(10):1585–1591. doi: 10.1097/CCM.0000000000003261. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Seymour C.W., Gesten F., Prescott H.C., et al. Time to treatment and mortality during mandated emergency care for sepsis. N Engl J Med. 2017;376(23):2235–2244. doi: 10.1056/NEJMoa1703058. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Prasad P.A., Shea E.R., Shiboski S., Sullivan M.C., Gonzales R., Shimabukuro D. Relationship between a sepsis intervention bundle and in-hospital mortality among hospitalized patients: a retrospective analysis of real-world data. Anesth Analg. 2017;125(2):507–513. doi: 10.1213/ANE.0000000000002085. [DOI] [PubMed] [Google Scholar]
- 11.Kuttab H.I., Lykins J.D., Hughes M.D., et al. Evaluation and predictors of fluid resuscitation in patients with severe sepsis and septic shock. Crit Care Med. 2019;47(11):1582–1590. doi: 10.1097/CCM.0000000000003960. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Kahn R.A., Kahn N.A., Bauer S.R., et al. Association between volume of fluid resuscitation and intubation in high-risk patients with sepsis, heart failure, end-stage renal disease, and cirrhosis. Chest. 2020;157(2):286–292. doi: 10.1016/j.chest.2019.09.029. [DOI] [PubMed] [Google Scholar]
- 13.Lee S.J., Ramar K., Park J.G., Gajic O., Li G., Kashyap R. Increased fluid administration in the first three hours of sepsis resuscitation is associated with reduced mortality: a retrospective cohort study. Chest. 2014;146(4):908–915. doi: 10.1378/chest.13-2702. [DOI] [PMC free article] [PubMed] [Google Scholar]