Abstract
Yellow nail syndrome (YNS) is a rare entity characterized by thickened yellowish nails, lymphedema and respiratory manifestations such as pleural effusion. Lymphatic dysfunction is considered as a cause of YNS. However, evidence of systemic dilatation/hyperplasia of lymphatics based on autopsy in YNS is not available. In this report, autopsy revealed dilatation and hyperplasia of lymphatic vessels in lungs, visceral and parietal pleurae, and intestines. We identified the direct opening of lymphatic vessels of the visceral pleura to the pleural cavity, which indicated the pathophysiology of uncontrollable pleural effusion in YNS. The current case was compromised with primary biliary cholangitis (PBC). The onset of PBC seemed to be related with the progression of YNS.
Keywords: Yellow nail syndrome, Primary biliary cholangitis, Autopsy
Introduction
Yellow nail syndrome (YNS) is characterized by yellowish nails, lymphatic edema and respiratory symptoms and is either idiopathic or associated with other autoimmune diseases. Lymphatic dysfunction is considered as a cause of YNS. However, evidence of systemic dilatation/hyperplasia of lymphatics based on autopsy in YNS is not available. Here, we report an autopsy report of YNS that details in the systemic pathology of the disease and describes the dilatation/hyperplasia of lymphatic vessels resulting in uncontrollable chylous pleural effusion and ascites. This is also the first case of YNS coincided with primary biliary cholangitis (PBC).
Case description
A-64-year-old woman was referred to our hospital for chronic dyspnea and bilateral pleural effusion. She reported yellowish fingernails and toenails for 10 years (Fig. 1). Chronic sinusitis, lymphedema of lower extremities, and pleural and pericardial effusions were identified, fulfilling the diagnostic criteria of YNS. Because bilateral pleural effusion, which was exudative and lymphocyte-predominant, did not respond to treatments with furosemide and erythromycin, pleurodesis with minocycline was performed. During the follow-up over 10 years, because serum levels of alkaline phosphatase (Al-p) and γ-glutamyl transpeptidase elevated up to 844 U/L (normal range: 50–350 U/L) and 680U/L (normal range: ≤ 32 U/L), respectively, and anti-mitochondrial M2 antibody turned positive, diagnosis of PBC was made at the age of 75, followed by the administration of ursodeoxycolic acid. Increased pleural effusion and ascites were identified within one year after the diagnosis of PBC (Fig. 2). At age 78, effusions turned chylous and she needed repeated drainages due to progressive dyspnea. Despite the administration of diuretics, erythromycin, tocopherol nicotinate, levothyroxine and dexamethasone, she was dead of respiratory failure.
Fig. 1.
Yellowish discoloration of the fingernails (A) and toenails (B).
Fig. 2.
Computed tomography one year after the diagnosis of primary biliary cholangitis showing severe bilateral pleural effusion and ascites.
At autopsy, hyperplasia and dilatation of lymphatic vessels, and lymphocyte infiltration were widely identified in bronchial and bronchiolar mucosa and stroma, interlobular and perivascular interstitia, and visceral and parietal pleurae. Some of the dilated lymphatic vessels in the visceral pleura were directly open to the pleural cavity (Fig. 3). The thoracic duct was intact. Moreover, lymphatic vessel dilatations were observed in the entire thickened wall of the small intestine (Fig. 4) and the para-adrenal fat tissue. Mild pericholangial fibrosis, which was consistent with PBC, was observed (Fig. 5). The absence of hypoalbuminemia and repeated confirmation of lymphocyte-predominant exudative features suggested that YNS was the cause of the effusions.
Fig. 3.
Dilated lymphatic vessels in the bronchial wall (A) and intralobular interstitium (B) (immunohistochemical staining for D2-40, ×10 objective). Visceral pleura with lymphocyte infiltration (C: elastic van Gieson staining, ×5 objective and D: hematoxylin and eosin staining, ×10 objective). Magnified images of visceral pleura with stained methothelial cells (arrows in E: immunohistochemical staining for AE1/3, ×40 objective) or lymphatic vessels (F: immunohistochemical staining for D2-40, ×40 objective). Dilated lymphatic vessels are directly open to thoracic cavity (arrowhead in F).
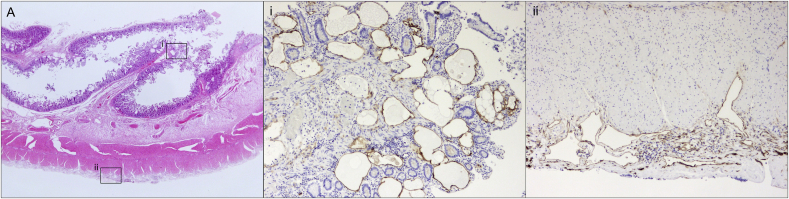
Fig. 4.
Overview image of the thickened wall of the small intestine. (A: H&E staining, ×5 objective) Magnified images of mucosal (i) and serosal (ii) regions of small intestine with dilated lymphatic vessels (immunohistochemical staining for D2-40, ×10 objective).
Fig. 5.
Pericholangial fibrosis considered to be the sequelae of cholangitis (H&E staining, ×20 objective).
Discussion
YNS is a rare entity characterized by the triad: slow-growing yellowish nails; lymphatic edema; and respiratory symptoms [[1], [2], [3]]. Pleural effusion, which is usually bilateral, exudative and lymphocyte-predominant, is present in 40% of YNS patients [4]. Pericardial effusion and ascites can be seen [5]. Impairment of lymphatic drainage has been considered to play a primary role in the pathogenesis of YNS, which was recently confirmed by a case-control study that utilized lymphoscintigraphy for patients with YNS and healthy controls [6]. Maldonado et al. reported that about one third of YNS cases with pleural fluid showed chylothorax, which also indicates that dysregulation of lymphatics is involved in the pathogenesis of YNS [4]. Although there have been several reports that showed pathological findings of lymphangiectasis in lungs [7,8], pleurae [9], and small intestines [10,11], autopsy reports detailing pathology of YNS in multiple organs are not available.
In the current case, dilated lymphatic vessels and lymphocyte infiltration were identified in multiple organs. Strikingly, lymphatic vessels in the visceral pleurae showed marked dilatation and some of them were directly open to the pleural cavity, suggesting the pathogenesis of pleural effusion in YNS. Furthermore, lymphatic dilatation was observed in small intestine and peri-adrenal fat tissues, furthering the evidence that YNS is a systemic lymphatic disorder.
YNS can be either idiopathic or associated with other diseases including autoimmune diseases such as rheumatoid arthritis (RA) [12], malignancies [13], immunodeficiency [14], titanium exposure [15] and so on. There have been cases whose onset of YNS were considered secondary to autoimmune thyroiditis [16] or Guillain-Barré syndrome [17]. In the present case, clinical deterioration of pleural effusion and ascites followed the diagnosis of PBC. PBC is an autoimmune disease characterized by diffuse inflammation, destruction, and fibrosis of intrahepatic bile ducts. Elevated serum Al-p levels and the positivity of serum anti-mitochondrial antibodies are useful for diagnosis [18]. Up to 55% of PBC patients have other autoimmune diseases such as Sjögren's syndrome, Raynaud's syndrome, Hashimoto thyroiditis and RA [19,20]. To the best of our knowledge, this is also the first report of YNS co-existing with PBC. Although it is difficult to be definitive, the clinical course of YNS showing deterioration concomitant with the onset of PBC suggested the possible association between these two diseases.
In conclusion, the current report described detailed autopsy findings of YNS including marked dilatation of pleural and intestinal lymphatic vessels that caused uncontrollable effusions.
Declaration of competing interest
The authors have no conflicts of interest to disclose.
Acknowledgements
The authors thank Dr. Wanda K. O'Neal (Marsico Lung Institute, University of North Carolina at Chapel Hill, Chapel Hill, NC) for English editing of the manuscript.
Abbreviations
- A-lp
alkaline phosphatase
- PBC
primary biliary cholangitis
- RA
rheumatoid arthritis
- YNS
yellow nail syndrome
Authors’ contributions
TK, SA, KK and MKa were the pulmonologists responsible for the patient care. NO and HM supervised the clinical management of the patient. MKi and AH were pathologists responsible for pathological diagnosis and autopsy. TK wrote the initial manuscript. TK and SA revised the manuscript. All the authors read and approved the final manuscript.
Funding
None declared.
Availability of data and materials
Not applicable.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Written informed consent for publication was obtained from the patient's spouse.
References
- 1.Samman P.D., White W.F. The "yellow nail" syndrome. Br. J. Dermatol. 1964;76:153–157. doi: 10.1111/j.1365-2133.1964.tb14499.x. [DOI] [PubMed] [Google Scholar]
- 2.Emerson P.A. Yellow nails, lymphoedema, and pleural effusions. Thorax. 1966;21(3):247–253. doi: 10.1136/thx.21.3.247. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Vignes S., Baran R. Yellow nail syndrome: a review. Orphanet J. Rare Dis. 2017;12(1):42. doi: 10.1186/s13023-017-0594-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Maldonado F., Ryu J.H. Yellow nail syndrome. Curr. Opin. Pulm. Med. 2009;15(4):371–375. doi: 10.1097/MCP.0b013e32832ad45a. [DOI] [PubMed] [Google Scholar]
- 5.Valdés L., Huggins J.T., Gude F., Ferreiro L., Alvarez-Dobaño J.M., Golpe A. Characteristics of patients with yellow nail syndrome and pleural effusion. Respirology. 2014;19(7):985–992. doi: 10.1111/resp.12357. [DOI] [PubMed] [Google Scholar]
- 6.Cousins E., Cintolesi V., Vass L., Stanton A.W.B., Irwin A., Heenan S.D. A case-control study of the lymphatic phenotype of yellow nail syndrome. Lymphatic Res. Biol. 2018;16(4):340–346. doi: 10.1089/lrb.2018.0009. [DOI] [PubMed] [Google Scholar]
- 7.Sacco O., Fregonese B., Marino C.E., Mattioli G., Gambini C., Rossi G.A. Yellow nail syndrome and bilateral cystic lung disease. Pediatr. Pulmonol. 1998;26(6):429–433. doi: 10.1002/(sici)1099-0496(199812)26:6<429::aid-ppul8>3.0.co;2-8. [DOI] [PubMed] [Google Scholar]
- 8.Liptrot S., Hulks G., Roberts F. Early pulmonary manifestations of yellow nail syndrome: a case report. Virchows Arch. 2007;451(5):985–986. doi: 10.1007/s00428-007-0503-7. [DOI] [PubMed] [Google Scholar]
- 9.Solal-Céligny P., Cormier Y., Fournier M. The yellow nail syndrome. Light and electron microscopic aspects of the pleura. Arch. Pathol. Lab Med. 1983;107(4):183–185. [PubMed] [Google Scholar]
- 10.Ocaña I., Bejarano E., Ruiz I., Ribera E., Pigrau C., Martinez-Vázquez J.M. Intestinal lymphangiectasia and the yellow nail syndrome. Gastroenterology. 1988;94(3):858. doi: 10.1016/0016-5085(88)90278-8. [DOI] [PubMed] [Google Scholar]
- 11.Duhra P.M., Quigley E.M., Marsh M.N. Chylous ascites, intestinal lymphangiectasia and the 'yellow-nail' syndrome. Gut. 1985;26(11):1266–1269. doi: 10.1136/gut.26.11.1266. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Mattingly P.C., Bossingham D.H. Yellow nail syndrome in rheumatoid arthritis: report of three cases. Ann. Rheum. Dis. 1979;38(5):475–478. doi: 10.1136/ard.38.5.475. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Thomas P.S., Sidhu B. Yellow nail syndrome and bronchial carcinoma. Chest. 1987;92(1):191. doi: 10.1378/chest.92.1.191a. [DOI] [PubMed] [Google Scholar]
- 14.Siegelman S.S., Heckman B.H., Hasson J. Lymphedema, pleural effusions and yellow nails: associated immunologic deficiency. Dis. Chest. 1969;56(2):114–117. doi: 10.1378/chest.56.2.114. [DOI] [PubMed] [Google Scholar]
- 15.Berglund F., Carlmark B. Titanium, sinusitis, and the yellow nail syndrome. Biol. Trace Elem. Res. 2011;143(1):1–7. doi: 10.1007/s12011-010-8828-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Crişan-Dabija R., Mihăescu T. A curious case of yellow nail syndrome. Pneumologia. 2015;64(1):36–38. [PubMed] [Google Scholar]
- 17.Woollons A., Darley C.R. Yellow nail syndrome following Guillain-Barré syndrome. Clin. Exp. Dermatol. 1997;22(5):253–254. doi: 10.1111/j.1365-2230.1997.tb01084.x. [DOI] [PubMed] [Google Scholar]
- 18.Carey E.J., Ali A.H., Lindor K.D. Primary biliary cirrhosis. Lancet. 2015;386(10003):1565–1575. doi: 10.1016/S0140-6736(15)00154-3. [DOI] [PubMed] [Google Scholar]
- 19.Corpechot C., Chrétien Y., Chazouillères O., Poupon R. Demographic, lifestyle, medical and familial factors associated with primary biliary cirrhosis. J. Hepatol. 2010;53(1):162–169. doi: 10.1016/j.jhep.2010.02.019. [DOI] [PubMed] [Google Scholar]
- 20.Parikh-Patel A., Gold E.B., Worman H., Krivy K.E., Gershwin M.E. Risk factors for primary biliary cirrhosis in a cohort of patients from the United States. Hepatology. 2001;33(1):16–21. doi: 10.1053/jhep.2001.21165. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
Not applicable.