Figure 1. Mechanism of CAR T-cell therapy and Cytokine Release Syndrome.
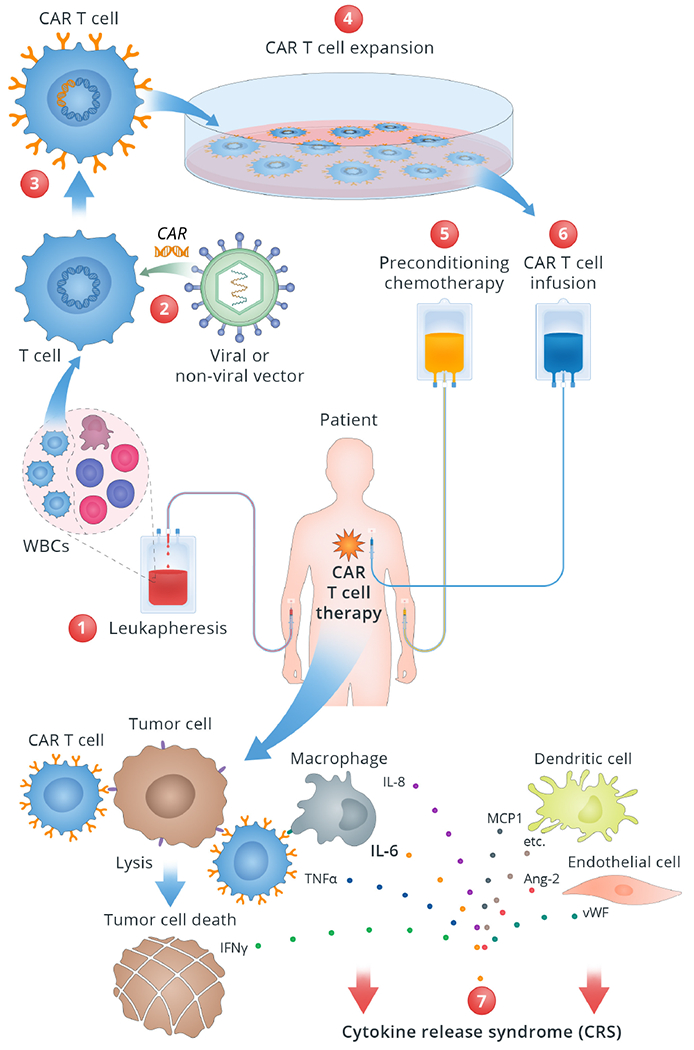
This figure illustrates stepwise mechanism of CAR T-cell therapy and related CRS.
1. White blood cells are drawn from the patient via leukapheresis. T cells are then separated in the Lab. 2. T cells are genetically modified or “engineered” with viral or nonviral vector inserting a gene encoding a chimeric antigen receptor into the T cells. 3. Engineered T cells, now known as CAR T cells, can recognize and attach to the specific antigen on the cancer cells. 4. CAR T cells are grown and multiplied in the bioreactor to create millions of copies. 5. Before the CAR T cells are administered, the patient receives preconditioning chemotherapy to lower the cell count to allow space for the incoming CAR T cells. 6. CAR T cells are infused back into the patient’s blood where they proliferate, detect and destroy the tumor cells. 7. CRS occurs as a result of the supraphysiologic levels of inflammatory cytokines released by the activated CAR T-cells and other immune cells such as macrophages.
Abbreviations: Ang-2: Angiopoetin 2; CAR: chimeric antigen receptor; IL: interleukin; IFN-γ: interferon gamma; MCP1: Monocyte chemoattractant protein 1; TNF-α: tumor necrosis factor alpha; vWF: von Willebrand factor.
