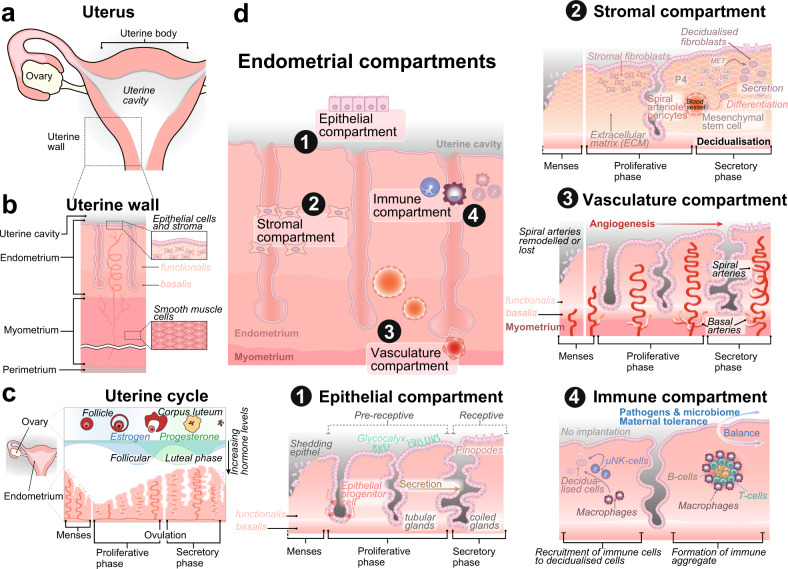
Fig. 2. Anatomical structure of the uterus.
a The cavity of the human uterine body connects to the ovaries by the fallopian tubes. b The uterine wall consists of the endometrium, the smooth muscular myometrial layer, and the outermost perimetrium. The endometrial epithelium forms the border to the cavity (luminal epithelium) and deep-reaching endometrial glands (glandular epithelium) which are embedded in the stroma. Only the endometrial functionalis layer is shed during menstruation at the beginning of the human uterine cycle (c), while the non-hormone-responsive basalis layer remains intact. Oestrogen produced by the developing follicle in the ovaries induces the growth and proliferation of endometrial tissue during the proliferative (follicular) phase. Ovulation and release of the egg from the ovaries occur mid-cycle, which leads to increased progesterone levels during the secretory (luteal) phase. Degradation of the corpus luteum and decreasing hormone levels induce menses and re-start the uterine cycle if no embryo implants into the uterine wall. d The endometrium can be functionally distinguished into four compartments, which change throughout the uterine cycle. The luminal epithelium of the epithelial compartment (1) is shed during menses and rebuilt by differentiating epithelial progenitor cells migrating from uterine glands. The luminal epithelium becomes pre-receptive but avoids pre-mature attachment of an embryo by the formation of a highly charged glycocalyx layer. Uterine glands grow in size and increase secretion towards the secretory phase while changing shape to become coiled. The luminal epithelium grows apical cellular protrusions (pinopodes), which increases receptivity and allows embryo attachment and implantation. Decidualisation occurs during the secretory phase in the stromal compartment (2) and assists in the preparation of the endometrium for implantation. Mesenchymal stem cells surrounding spiral arteriole (specialised uterine blood vessels) pericytes differentiate to become secretory. Concomitantly, stromal fibroblasts undergo mesenchymal-to-epithelial transition (MET) under the influence of progesterone (P4) and convert to decidualised, secretory fibroblasts. Spiral arteries in the vascular compartment (3) branch from basal arteries, which supply the endometrial basalis layer during menses, when arteries of the functionalis layer are extensively remodelled or lost. Angiogenesis drives the formation of spiral arteries towards the secretory phase to increase the blood supply of the upper endometrium in preparation for embryo implantation. The uterine immune compartment (4) is a highly flexible system. Immune aggregates consisting of B-cells, T-cells and macrophages form and reside in the upper parts of the functional layer, maintaining the balance between defence against pathogens and external threats and sustaining the protective microbiome barrier necessary for uterine health. During pregnancy, the immune compartment provides maternal tolerance to an embryo which induces attachment to the uterine wall. If no successful implantation occurs, immune cells such as uterine natural killer (uNK) cells and macrophages are recruited to remove decidualised cells.