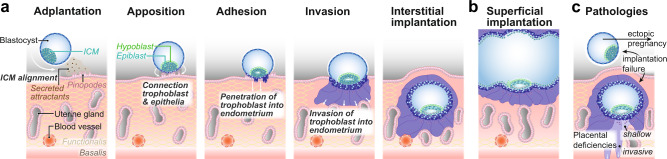
Fig. 3. Embryo development within the uterus and uterine pathologies.
a The stages leading to human interstitial embryo implantation and marmoset superficial implantation (b) are shown from left to right. The blastocyst arrives in the uterine cavity and hatches from the surrounding zone pellucida by day 5 post-fertilisation. It then moves along the uterine epithelium until it reaches a receptive environment provided by pinopodes before the inner cell mass (ICM) aligns towards the uterine epithelium (adplantation). The outer extraembryonal trophoblast cells of the blastocyst connect to the uterine cells (apposition) and penetrate through the luminal epithelium (adhesion). Concomitantly, the ICM differentiates into extraembryonal hypoblast and embryonal epiblast, which induce lumenogenesis. Trophoblast comprises of several layers of proliferative cytotrophblast (dark blue) and terminally differentiated, multinucleated syncytiotrophoblast (purple) which continue invasion into the endometrium towards nutrition-providing uterine glands and blood vessels, by degrading the extracellular matrix of the decidualised stroma. The human embryo is fully embedded in maternal endometrium following implantation. In contrast, the embryo is not fully engulfed by endometrium in superficial implantation (b) but stays within the uterine cavity. Common pathologies (c) associated with early stages of pregnancy are the failure of an embryo to implant into the uterine cavity wall, or ectopic pregnancy, when the embryo does not reach the uterine cavity for implantation, and instead implants mostly within the uterine tube. d Abnormal invasiveness causes placental deficiencies leading to placenta accreta spectrum disorders, caused by excessive trophoblast invasion, or pre-eclampsia, as a result of insufficient trophoblast invasion.