Dear Editors,
Biologics such as infliximab account for a growing multibillion-dollar industry, treating a myriad of inflammatory conditions ranging from psoriasis to inflammatory bowel disease. As patents for these medications expire, a growing market is surfacing to derive highly similar but more affordable therapies, known as biosimilars (McKinnon and Ward, 2016). Because the approval process of biosimilars does not require the same extensive clinical trial phases as the originators, we highlight that informational gaps exist on the postmarking side effects of biosimilars (Yamauchi et al., 2018). The following case presents an example of a new-onset rash in the setting of initiating biosimilar infliximab-dyyb treatment.
A 34-year-old woman with a history of Crohn’s disease treated with originator infliximab for 10 years was referred for an evaluation of pruritic lesions present for 2 weeks. Prior to presentation, the patient’s gastroenterologist substituted infliximab for the biosimilar infliximab-dyyb. Five weeks later, she developed a pustular rash (Fig. 1, Fig. 2) and was treated for presumed dermatitis with a steroid injection, hydroxyzine, and doxycycline by her primary care provider, without improvement.
Fig. 1.
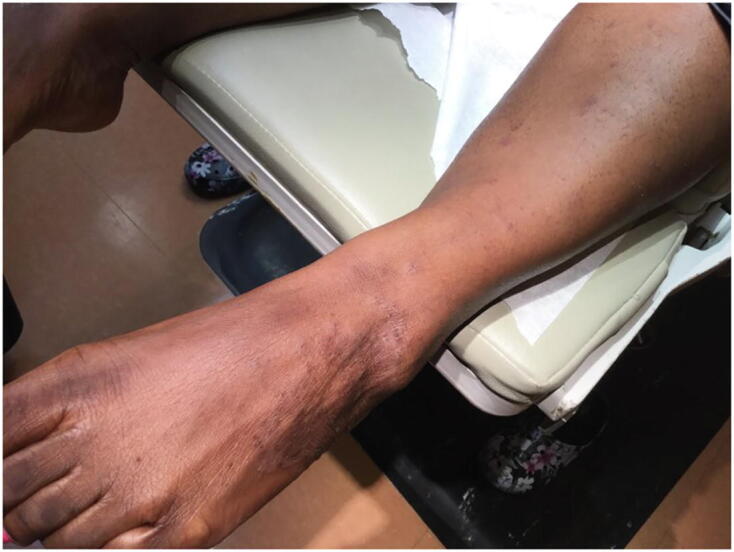
Patient's left foot and leg upon initial presentation to dermatology clinic: examination revealed diffuse scattered follicular papules on the arms, legs, and trunk.
Fig. 2.

Patient's right foot and leg upon initial presentation to dermatology clinic demonstrating blister formation on the right dorsolateral foot.
A week later, the patient was evaluated at our clinic, and examination revealed diffuse, scattered follicular papules and pustules on the arms, legs, and trunk, comprising 10% of the body surface area. Lab workup, including syphilis IgG, hepatitis panel, and antinuclear antibody, were all unremarkable. The patient was prescribed triamcinolone, topical clindamycin, and trimethoprim-sulfamethoxazole. A punch biopsy revealed subcorneal blister formation with neutrophils and was negative for fungal organisms on periodic acid–Schiff staining. The patient was started on minocycline and continued on triamcinolone. She followed up with gastroenterology 1 week later and was switched from infliximab-dyyb back to originator infliximab, which resolved her symptoms within 4 weeks. Since the initial presentation in July 2018, the patient has had no recurrence.
Biosimilars differ from generics in that biologic therapies are highly complex, and exact replication is currently impossible (Khraishi et al., 2016). To minimize costly clinical trials, biosimilars undergo an expedited regulatory process that relies more on nonclinical data and structure analysis in comparison with the originator biologic than clinical trials (Yamauchi et al., 2018). Once similarity is established, manufacturers of biosimilars may extrapolate to other indications for the reference product and be approved for other indications that the originator has been licensed for (Bui and Taylor, 2014).
Due to the nature of development, relatively little is known about biosimilar side effects. In our case, the biosimilar infliximab-dyyb was approved for the same indications as the reference product, using extrapolation of indication based on studies conducted for rheumatoid arthritis and ankylosing spondylitis (McKinnon and Ward, 2016, Yamauchi et al., 2018). Although increased competition and decreased cost of therapies overall would benefit patients, this paucity of clinical trial data creates potential uncertainty regarding the safety and efficacy of biosimilars. The Center for Biologics Evaluation and Research is an organization within the U.S. Food and Drug Administration to which biosimilar adverse events can be reported (U.S. Food and Drug Administration, 2020).
To date, no case reports have discussed similar side effects to biosimilars in the postmarketing phase. There have been few cases of infliximab treatment of subcorneal pustular dermatosis, but no publication describes the reverse (Kretschmer et al., 2017). This case represents the significance of identifying side effect profiles of biosimilars, not to dissuade but to inform prescribing clinicians, because side effect profiles of these treatments may differ from their originator.
Acknowledgments
Acknowledgments
The authors thank the patient for granting permission to publish this case.
Conflicts of interest
None.
Funding
None.
Study approval
The author(s) confirm that any aspect of the work covered in this manuscript that has involved human patients has been conducted with the ethical approval of all relevant bodies.
References
- Bui L.A., Taylor C. Developing clinical trials for biosimilars. Semin Oncol. 2014;41(Suppl. 1):S15–S25. doi: 10.1053/j.seminoncol.2013.12.002. [DOI] [PubMed] [Google Scholar]
- Khraishi M., Stead D., Lukas M., Scotte F., Schmid H. Biosimilars: a multidisciplinary perspective. Clin Ther. 2016;38(5):1238–1249. doi: 10.1016/j.clinthera.2016.02.023. [DOI] [PubMed] [Google Scholar]
- Kretschmer L., Maul J.-T., Hofer T., Navarini A. Interruption of Sneddon-Wilkinson subcorneal pustulation with infliximab. Case Rep Dermatol. 2017;9(1):140–144. doi: 10.1159/000468917. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McKinnon R., Ward M. Safety considerations of biosimilars. AustPrescr. 2016;39(6):188–189. doi: 10.18773/austprescr.2016.084. [DOI] [PMC free article] [PubMed] [Google Scholar]
- U.S. Food and Drug Administration. Report a problem to the Center for Biologics Evaluation and Research [Internet]. 2020 cited 2020 April 21]. Available from: https://www.fda.gov/vaccines-blood-biologics/safety-availability-biologics/report-problem-center-biologics-evaluation-research.
- Yamauchi P., Crowley J., Kaur P., Spelman L., Warren R. Biosimilars: what the dermatologist should know. J Eur Acad Dermatol Venereol. 2018;32(7):1066–1074. doi: 10.1111/jdv.14812. [DOI] [PubMed] [Google Scholar]


