Abstract
Objective: To investigate the correlation between short-term imaging techniques and long-term function using receiver operating characteristic (ROC) curve after tibia fracture surgery. Methods: Seventy patients with tibia fracture admitted to our hospital were selected as the study subjects, and were divided into a < 60 years old group (n = 40) and a ≥ 60 years old group (n = 30), a removed internal fixation group (n = 26) and a retained internal fixation group (n = 44). The short-term imaging results, long-term function, the degree of pain, the range of ankle joint motion, and the subjective satisfaction of patient care were scored and compared among the four groups. The influencing factors of subjective satisfaction of patients were analyzed using logistic regression analysis. Results: There were marked differences in the scores of Jakim, Garland & Werley scoring system, and Kofoed’s scale and subjective satisfaction between the < 60 years old group and the ≥ 60 years old group, and between the removed internal fixation group and the retained internal fixation group (P < 0.05), but there was no remarkable difference in visual analog scale (VAS) scores (P > 0.05). Spearman’s correlation analysis revealed a correlation between the short-term imaging manifestations and the long-term function in tibia fracture patients, and the correlation was remarkable in patients aged < 60 years without internal fixation (P < 0.05). Logistic correlation analysis showed that Kofoed’s scale scores were significantly correlated with patients’ subjective satisfaction (P < 0.05). Conclusion: There is a correlation between early imaging and long-term function in tibia fracture patients, and the correlation was remarkable in patients aged < 60 years and without internal fixation. The range of joint motion and degree of pain are the primary influencing factors for evaluation of patients’ subjective satisfaction.
Keywords: Tibial fractures, short-term imaging manifestations, long-term function, ROC curve, correlation analysis
Introduction
The tibia is a long bone located in the lower portion of the leg, which is composed of 3 parts: upper end, lower end, and interceding shaft [1]. The proximal end of tibia swells and protrudes to both sides to form the medial and lateral ankles. Tibial fractures are the most common long bone fractures, accounting for approximately 10%-15% of systemic fractures. Tibial fractures may occur because the tibia’s closeness to the ground, resulting in a greater possibility of its being subjected to adverse events (e.g., forcible hits and crushing). In addition, its minimal external muscles can lead to easy contamination, which leads to delayed healing [2,3]. Currently, surgery has been extensively implemented for the clinical treatment of tibial fractures. Physicians often select appropriate regimens in accordance with the type of fractures and the degree of soft tissue injury. The therapeutic principle focuses on the restoration of the weight-bearing function of the legs and the parallel relationship between upper and lower articular surfaces [4,5].
In recent years, with the penetrating understanding of tibial fractures, more and more scholars begin to investigate the correlation between functional restoration and imaging manifestations, and their understandings of such correlation vary greatly [6,7]. A study indicates that the joint function will be seriously affected if there is a displacement of 1 mm between the joint surfaces after fracture surgery [8]. Some scholars believe that even if early imaging manifestations occur in arthritis patients after surgery, there is no marked change in the long-term joint function [9]. Based on a retrospective analysis of patients with fractures of the tibial plateau, scholar study has suggested that there is a significant correlation between the early imaging results in patients with fractures of tibial plateau after surgery and the degrees of joint degeneration during follow-ups [10]. However, study demonstrates that early imaging results after surgery cannot fully reflect the functional status of knee joint after fracture surgery, which should be evaluated based on the actual conditions of patients. The aforementioned studies describe the long-term imaging results of patients’ joints, focusing on the relationships between arthritis and joint flatness and joint functions. However, there is a lack of study on the influence of patients’ individual factors on the functions after fracture surgery [11].
This study aimed to explore the correlation between short-term imaging manifestations and long-term function after tibial fracture surgery, with a view to identifying the optimal indicators for evaluation of the prognosis of tibial fracture patients, thereby providing a reference for the determination of the best clinical intervention protocol.
Materials and methods
General data
A total of 70 tibial fracture patients admitted to our hospital from January 2018 to October 2020 were selected as the study subjects, including 41 males and 29 females aged 18-78 years and weighing 62-83 kg, with an average age of (49.18 ± 2.33) years and an average weight of (73.98 ± 3.22) kg. The subjects were followed up for 2-30 months, with an average follow-up duration of (15.44 ± 2.10) months.
Inclusion criteria: patients (1) diagnosed with tibial fractures by imaging examination; (2) with clear consciousness and ability to cooperate with the investigation; (3) with complete medical records; (4) aged ≥18 years; (5) with unilateral tibial fractures. The present study was approved by the Ethics Committee of Jinggangshan University Affiliated Hospital. All study participants provided written informed consent before participating in the study.
Exclusion criteria: patients (1) with mental illness; (2) complicated by severe malignant tumors, hematologic diseases or connective tissue diseases; (3) complicated by severe renal and hepatic dysfunction; (4) complicated by hematological diseases; (5) with poor compliance with the investigation; (6) with pathologic fractures; (7) complicated with underlying health conditions that seriously affected the investigation.
Rejection criteria: (1) loss to follow up during the investigation; (2) voluntary withdrawal during the investigation.
Intervention methods
The short-term imaging results (30 days after surgery), long-term function (3 months after surgery), degrees of pain (3 months after surgery), range of joint motion (3 months after surgery) and subjective satisfaction (3 months after surgery) of subjects were evaluated. The short-term imaging results were evaluated using Jakim. Jakim can be used to evaluate subjects from five aspects, such as joint surface unevenness and fracture line alignment. The total score of the scale is 100 points. A higher score indicates better imaging indicators [12]. The long-term function was evaluated using the Garland & Werley scoring system. Garland & Werley scoring system consists of four major items, including patients’ evaluation of their restricted activities or loss of function and physicians’ evaluation of joint flexion and extension and rotation. The total score of the scale is 20 points. A lower score indicates a better joint function [13]. The degrees of pain were evaluated by visual analog scale (VAS). VAS, a commonly used tool for evaluation of degrees of pain clinically, comprises a straight line of 0-10 cm. Zero indicates painless, and 10 indicates severe pain. Subjects were asked to select a point on the scale to represent their degree of pain based on their conditions [14]. The joint function was evaluated by Kofoed’s scale. Kofoed’s scale is composed of three dimensions: function, range of motion and pain. The total score is 100 points, and 85-100 points indicates excellent function, 75-84 points indicates good function, 70-74 points indicates qualified function, and < 70 points indicates poor function [15]. The subjective satisfaction was evaluated using the scale prepared by the hospital. The scale was primarily adopted for evaluation of patients’ satisfaction with treatment and restoration of joint function. The total score of the scale is 100 points. A higher score indicates a higher level of satisfaction.
Observational indices and assessment criteria
The difference in the short-term imaging results, long-term function, degree of pain, joint function and satisfaction between the < 60 years old group (n = 40) and the ≥ 60 years old group (n = 30) and between the removed internal fixation group (n = 26) and the retained internal fixation group (n = 44), and the correlations between the aforementioned indicators were the observational indices. Finally, the short-term imaging manifestations and long-term function in the four groups were explored through plotting the receiver operating characteristic (ROC) curves.
Statistical analysis
The collected data were input into an EXCEL table, and SPSS 22.0 was adopted for statistical analysis. GraphPad Prism 8 was used to illustrate the figures. The collected data were detected using a normal distribution. The data conforming to a normal distribution were expressed as [n (%)]. The differences between groups were analyzed using chi-square test. The measurement data were expressed using mean ± standard deviation (mean ± SD). The differences between groups were analyzed using t test, and Spearman’s correlation analysis was performed. P < 0.05 indicated a statistically significant difference [16].
Results
Differences in imaging results, long-term function and related indicators in tibial fracture patients with different ages
The patients were divided into a < 60 years old group (n = 40) and a ≥ 60 years old group (n = 30) based on ages, and the indicators were evaluated. The results suggested that the scores of Jakim and Kofoed’s scale and subjective satisfaction of patients aged < 60 years were markedly higher than those of patients aged ≥ 60 years (P < 0.05), while Garland & Werley scores of patients aged < 60 years were significantly lower than those of patients aged ≥ 60 years (P < 0.05). There was no statistically significant difference in VAS scores between the < 60 years old group and the ≥ 60 years old group (P > 0.05) (Figure 1 and Table 1).
Figure 1.

Differences in imaging resluts, long-term function and related indicators in tibial fracture patients with different ages. The scores of Jakim, Kofoed’s scale and subjective satisfaction of patients aged < 60 years were significantly higher than those of patients aged ≥ 60 years (P < 0.05), while Garland & Werley scores of patients aged < 60 years were remarkably lower than those of patients aged ≥ 60 years (P < 0.05). There was no significant difference in VAS scores between the two groups (P > 0.05). # indicates a statistically significant difference in the same indices between the two groups before and after surgery.
Table 1.
Differences in imaging results, long-term function and related indicators in tibial fracture patients with different ages (mean ± SD)
| Group | n | Jakim | Garland & Werley | VAS | Kofoed | Subjective satisfaction |
|---|---|---|---|---|---|---|
| < 60 years old group | 40 | 15.44 ± 3.22 | 4.89 ± 1.02 | 83.29 ± 3.22 | 87.19 ± 4.33 | |
| ≥ 60 years old group | 30 | 18.29 ± 2.98 | 5.01 ± 0.98 | 78.98 ± 2.98 | 80.18 ± 3.98 | |
| X2 | - | 5.808 | 3.782 | 0.495 | 5.72 | 6.936 |
| P | - | < 0.001 | < 0.001 | 0.622 | < 0.001 | < 0.001 |
Differences in imaging results, long-term function and related indicators in tibial fracture patients treated with different internal fixation methods
The patients were divided into a removed internal fixation group (n = 26) and a retained internal fixation group (n = 44) based on internal fixation methods. The imaging results, long-term function and related indicators were compared between the two groups. The results exhibited that the scores of Jakim and Kofoed’s scale and subjective satisfaction in the removed internal fixation group were significantly higher than those in the retained internal fixation group (P < 0.05), while Garland & Werley scores were notably lower than those in the retained internal fixation group (P < 0.05). There was no statistically significant difference in VAS scores (P > 0.05) (Table 2 and Figure 2).
Table 2.
Differences in imaging results, long-term function and related indicators in tibial fracture patients treated with different internal fixation methods (mean ± SD)
| Group | n | Jakim | Garland & Werley | VAS | Kofoed | Subjective satisfaction |
|---|---|---|---|---|---|---|
| Removed internal fixation group | 26 | 16.29 ± 2.98 | 4.98 ± 1.02 | 83.88 ± 2.98 | 88.87 ± 3.98 | |
| Retained internal fixation group | 44 | 17.98 ± 3.01 | 5.01 ± 0.78 | 79.98 ± 2.88 | 83.29 ± 2.98 | |
| X2 | - | 2.271 | 2.278 | 0.138 | 5.405 | 6.67 |
| P | - | 0.026 | 0.026 | 0.891 | < 0.001 | < 0.001 |
Figure 2.

Differences in imaging results, long-term function and related indicators in tibial fracture patients treated with different internal fixation methods. The scores of Jakim and Kofoed’s scale and subjective satisfaction of patients without internal fixation were noticeably higher than those of patients with internal fixation (P < 0.05), while Garland & Werley scores of patients without internal fixation were significantly lower than those of patients with internal fixation (P < 0.05). There was no significant difference in VAS scores between the two groups (P > 0.05). # indicates a statistically significant difference in the same indices between the two groups before and after surgery.
Correlation analysis of short-term imaging results, long-term function and other indicators
Spearman’s correlation analysis of the scores of Jakim, Garland & Werley scoring system, VAS, and Kofoed’s scale and subjective satisfaction was performed. The results demonstrated that Jakim scores were significantly correlated with Garland & Werley scores (r = -0.676, P < 0.05) and the scores of VAS and Kofoed’s scale (r = -0.671, r = 0.678, P < 0.05), but Jakim scores were not remarkably correlated with subjective satisfaction (r = 0.343, P > 0.05). Garland & Werley scores were remarkably correlated with the scores of VAS and Kofoed’s scale (r = 0.559, r = -0.674, P < 0.05), but Garland & Werley scores were not remarkably correlated with subjective satisfaction (r = -0.379, P > 0.05) (Table 3).
Table 3.
Correlation analysis of short-term imaging indicators, long-term function and other indicators
| Group | Jakim | Garland & Werley | VAS | Kofoed | Subjective satisfaction |
|---|---|---|---|---|---|
| Jakim | 1 | -0.676 | -0.671 | 0.678 | 0.343 |
| Garland & Werley | -0.676 | 1 | 0.559 | -0.674 | -0.379 |
| VAS | -0.671 | 0.559 | 1 | -0.378 | -0.655 |
| Kofoed | 0.678 | -0.674 | -0.378 | 1 | 0.781 |
| Subjective satisfaction | 0.343 | -0.379 | -0.655 | 0.781 | 1 |
Analysis of influences of age and internal fixation status on the correlation between short-term imaging results and long-term function
The patients were grouped based on age and internal fixation status, and their short-term imaging results and long-term function were evaluated. Eventually, the ROC curve analysis showed that the area under curve (AUC) of ROC of patients aged < 60 years was 0.7711 (95% CI: 0.5925-0.9497, P < 0.05), while that of patients without internal fixation was 0.7488 (95% CI: 0.5690-0.9287, P < 0.05) (Figure 3).
Figure 3.
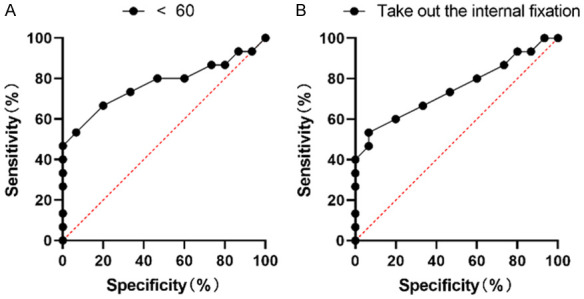
Analysis of influences of age and internal fixation status on the correlation between short-term imaging manifestations and long-term function. The AUC of ROC of patients aged < 60 years was 0.7711 (95% CI: 0.5925-0.9497, P < 0.05) (A), while that of patients without internal fixation was 0.7489 (95% CI: 0.5690-0.9287, P < 0.05) (B).
Logistic multivariate regression analysis of subjective satisfaction of tibial fracture patients
Multivariate regression analysis was conducted on the factors affecting subjective satisfaction of tibial fracture patients. The results suggested that the scores of VAS and Kofoed’s scale were the independent factors affecting patients’ subjective satisfaction, with patients’ subjective satisfaction set as a dependent variable, and short-term imaging results, long-term function, VAS scores and joint function set as independent variables (P < 0.05) (Table 4).
Table 4.
Logistic regression analysis of influencing factors of subjective satisfaction of tibial fracture patients after surgery
| Independent variable | Β | SE | Wald | P | OR |
|---|---|---|---|---|---|
| VAS | 0.53 | 0.12 | 22.44 | 0.000 | 1.71 |
| Kofoed | 0.29 | 0.10 | 10.81 | 0.001 | 1.41 |
Discussion
The tibia is the main weight-bearing bone of the lower limb [17]. With less coverage of soft tissues (e.g., anterior muscles of lower leg) this may lead to poor blood supply of the tibia, and unstable fractures commonly occur among all types of tibial fractures. Therefore, patients with tibial fracture have a high incidence of fracture infections and osteofascial compartment syndrome [18]. Clinical results show that tibial fractures account for approximately 13.7% of systemic fractures, and fracture patients often experience shortened or angular displacements at the beginning of fractures [19]. A study indicates that if the shortened displacement of patients’ fractures is 0.5-1.0 cm and even if there is only slight axial displacement, surgical intervention should be implemented as soon as possible, so as to reduce the incidence of postoperative joint dysfunction [20].
Currently, the clinical studies of tibial fractures have mainly focused on how to improve the prognosis, restricted joint motion and the quality of life of patients [21]. Various scales and imaging examinations have been widely used to evaluate the intervention effects on tibial fracture patients. However, with the promotion and implementation of the scales, some scholars indicate that there are certain errors in evaluating the status of tibial fracture patients only using scales. For example, Katz Adjustment Scale (KAS) overemphasizes patients’ subjective feelings, and Humor Styles Scale (HSS) is for people with high qualifications [22], which to a certain extent restricts the evaluation of the prognosis of tibial fracture patients, and may even affect the normal treatment. Therefore, it is necessary to seek an evaluation method that is more closely associated with the actual conditions of tibial fracture patients, thereby providing a reference for the determination of the clinical therapeutic strategies.
In this study, different groups were established, and the correlation between the short-term imaging results and the long-term function was evaluated using the ROC curve after tibial fracture surgery. The comparisons among groups after grouping based on age and internal fixation methods showed that the < 60 years old group and the removed internal fixation group were superior to the ≥ 60 years old group and the retained internal fixation group in the short-term imaging indicators and the indicators of long-term function. A comparative study of 80 patients with tibial fracture exhibited that the patients aged < 60 years had a shorter duration of postoperative rehabilitation, shorter hospital stay, lower therapeutic cost and fewer complications, and the scholars believe that this may be due to the better physical function of patients aged < 60 years and their higher tolerance to trauma [23]. In the present study, the correlation analysis using the ROC curve revealed that the short-term imaging results of patients aged < 60 years and patients without internal fixation were more significantly related to better long-term functions, which may be due to the following reasons: (1) compared with patients aged < 60 years, patients aged ≥ 60 years were more likely to be complicated by other diseases, and the progression of previous diseases may affect postoperative rehabilitation. Patients aged < 60 years were generally free from the influences of disease on their postoperative indicators. A previous study has shown that age is an important factor affecting the rehabilitation of patients with orthopedic diseases, and elderly fracture patients need more clinical care [24], these results are consistent with our study. (2) Patients aged ≥ 60 years often experience declined cognitive abilities to some extent, and tibial fracture patients require systematic rehabilitation exercises to restore their joint functions as much as possible. Patients aged ≥ 60 years have better rehabilitation effects, but they have a slow rehabilitation process as a result of their own reasons, which may be one of the reasons contributing to the weak correlation between the scores of Jakim and Garland & Werley [25]. (3) Patients aged ≥ 60 years tended to have a lower bone density. Although the rehabilitation of tibial fracture patients is less subjected to bone density compared with that of hip or spinal fracture patients, massive studies and evidence-based medicine have confirmed that the bone density affects patients’ rehabilitation. (4) Although internal fixation can play a fixing role, it can affect the joint rehabilitation exercises of tibial fracture patients. The early removal of internal fixation devices can help patients avoid the influences of implants on their joint functions. In regard to this, there is a significant correlation between the scores of Jakim and Garland & Werley in such patients [26].
Finally, the independent factors affecting the subjective satisfaction of tibial fracture patients were analyzed using logistic regression. The results suggested that the scores of VAS and Kofoed’s scale were the independent factors affecting the subjective satisfaction of the patients. The authors believe that the aforementioned two indicators directly reflect the joint function, and the patients believe in their own feelings and joint activities rather than systematically evaluating their own conditions. This indicates that physicians need to focus on improving the pain and range of joint motion of patients during clinical intervention, so as to facilitate the establishment of a harmonious doctor-patient relationship.
In summary, there is a correlation between early imaging results and long-term function in tibial fracture patients, and the correlation is remarkable in patients aged < 60 years and without internal fixation. The range of joint motion and degrees of pain are the main influencing factors for evaluation of subjective satisfaction of patients. The innovation of this study lies in the implementation of the ROC curve for the correlation analysis rather than for disease diagnosis, and the investigation of the factors affecting the correlation between short-term imaging results and long-term function of tibial fracture patients through grouping, thus providing a reference for clinical intervention. The deficiency of this study is that it did not evaluate the quality of life of tibial fracture patients, and did not consider the influences of patients’ underlying health conditions on the intervention outcomes, which are planned to be implemented in future studies.
Disclosure of conflict of interest
None.
References
- 1.Wennergren D, Bergdahl C, Ekelund J, Juto H, Sundfeldt M, Möller M. Epidemiology and incidence of tibia fractures in the Swedish Fracture Register. Injury. 2018;49:2068–2074. doi: 10.1016/j.injury.2018.09.008. [DOI] [PubMed] [Google Scholar]
- 2.Yao X, Xu Y, Yuan J, Lv B, Fu X, Wang L, Yang S, Meng S. Classification of tibia plateau fracture according to the “four-column and nine-segment”. Injury. 2018;49:2275–2283. doi: 10.1016/j.injury.2018.09.031. [DOI] [PubMed] [Google Scholar]
- 3.Onyekwelu I, Sinicrope BJ, Riehl JT, Roberts CS, Voor MJ. Biomechanics of the injured fibula following plate fixation of a concomitant tibia fracture to fix or not to fix? Bull Hosp Jt Dis (2013) 2018;76:176–182. [PubMed] [Google Scholar]
- 4.McGonagle L, Cordier T, Link BC, Rickman MS, Solomon LB. Tibia plateau fracture mapping and its influence on fracture fixation. J Orthop Traumatol. 2019;20:12. doi: 10.1186/s10195-019-0519-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Aymen F, Youcef O, Aymen S, Issam A, Abderrazek A. Triplane fracture of the proximal tibia: a case report and literature review. Pan Afr Med J. 2019;33:40. doi: 10.11604/pamj.2019.33.40.17953. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Costa ML, Achten J, Griffin J, Petrou S, Pallister I, Lamb SE, Parsons NR. Effect of locking plate fixation vs intramedullary nail fixation on 6-month disability among adults with displaced fracture of the distal tibia: the UK FixDT randomized clinical trial. JAMA. 2017;318:1767–1776. doi: 10.1001/jama.2017.16429. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Bell A, Templeman D, Weinlein JC. Nonunion of the femur and tibia: an update. Orthop Clin North Am. 2016;47:365–375. doi: 10.1016/j.ocl.2015.09.010. [DOI] [PubMed] [Google Scholar]
- 8.Liu J, Smith CD, White E, Ebraheim NA. A systematic review of the role of surgical approaches on the outcomes of the tibia pilon fracture. Foot Ankle Spec. 2016;9:163–168. doi: 10.1177/1938640015620637. [DOI] [PubMed] [Google Scholar]
- 9.Lehreitani ML, Abid H, Marcaillou F, Rachid M, Ibrahimi AE, Mrini AE, Blanc S. Triplane fracture of the proximal end of the tibia: a rare lesion (case study and literature review) Pan Afr Med J. 2019;32:46. doi: 10.11604/pamj.2019.32.46.9680. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Çiçekli Ö, Kochai A, Şükür E, Başak AM, Kurtoğlu A, Türker M. Suprapatellar approach for fractures of the tibia: does the fracture level matter? Eklem Hastalik Cerrahisi. 2019;30:10–16. doi: 10.5606/ehc.2019.63487. [DOI] [PubMed] [Google Scholar]
- 11.Mitchell PM, Harms KA, Lee AK, Collinge CA. Morphology of the posterior malleolar fracture associated with a spiral distal tibia fracture. J Orthop Trauma. 2019;33:185–188. doi: 10.1097/BOT.0000000000001398. [DOI] [PubMed] [Google Scholar]
- 12.Saade-Lemus S, Nguyen JC, Francavilla ML, Martin-Saavedra JS, Ho-Fung VM, Kaplan SL. Buckle fracture of the proximal tibia in children and frequency of association with trampoline and inflatable bouncer use. Pediatr Radiol. 2019;49:1327–1334. doi: 10.1007/s00247-019-04450-0. [DOI] [PubMed] [Google Scholar]
- 13.Kang HJ, Kim BS, Kim SM, Kim YM, Kim HN, Park JY, Cho JH, Choi Y. Can preoperative 3D printing change surgeon’s operative plan for distal tibia fracture? Biomed Res Int. 2019;2019:7059413. doi: 10.1155/2019/7059413. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Kfuri M, Schatzker J. Revisiting the Schatzker classification of tibial plateau fractures. Injury. 2018;49:2252–2263. doi: 10.1016/j.injury.2018.11.010. [DOI] [PubMed] [Google Scholar]
- 15.Parratte S, Ollivier M, Argenson JN. Primary total knee arthroplasty for acute fracture around the knee. Orthop Traumatol Surg Res. 2018;104:S71–S80. doi: 10.1016/j.otsr.2017.05.029. [DOI] [PubMed] [Google Scholar]
- 16.Chen Q, Song L, Fang J, Qin X, Lv T, Li X. Effectiveness of diagnosis and treatment of spiral fracture of the distal third of the tibia combined with posterior malleolus fracture (a series of ten cases) J Am Podiatr Med Assoc. 2018;108:106–114. doi: 10.7547/15-181. [DOI] [PubMed] [Google Scholar]
- 17.Pires J, Oliveira S, Figueiredo P, Pinheiro JP. Rehabilitation of simultaneous bilateral epiphysial fracture of proximal tibia in adolescent. BMJ Case Rep. 2018;2018:bcr2017223619. doi: 10.1136/bcr-2017-223619. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Tan L, Li YH, Li Y, Lin T, Zhu D, Sun DH. Tibial plateau fractures (AO type B3) combined with tibial tubercle fracture: case report and review of the literature. Medicine (Baltimore) 2018;97:e12015. doi: 10.1097/MD.0000000000012015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Metsemakers WJ, Smeets B, Nijs S, Hoekstra H. Infection after fracture fixation of the tibia: analysis of healthcare utilization and related costs. Injury. 2017;48:1204–1210. doi: 10.1016/j.injury.2017.03.030. [DOI] [PubMed] [Google Scholar]
- 20.Alshammari D, Alhefzi A, Bund L, Schneider L, Gicquel P. Popliteal artery dissection presented 12 hours after admission for a Salter III fracture of proximal tibia. Acta Orthop Belg. 2016;82:918–922. [PubMed] [Google Scholar]
- 21.Lowenberg DW, DeBaun MR, Sox-Harris A, Behn A. Influence of fracture obliquity and interlocking nail screw configuration on interfragmentary motion in distal metaphyseal tibia fractures. Eur J Orthop Surg Traumatol. 2020;30:343–350. doi: 10.1007/s00590-019-02553-w. [DOI] [PubMed] [Google Scholar]
- 22.Ranjan R, Sud A, Adhikary D, Sinha A, Chand S. Incidence and risk factors for iatrogenic distal tibia/fibula fracture during ponseti technique of clubfoot treatment. J Pediatr Orthop B. 2019;28:572–578. doi: 10.1097/BPB.0000000000000595. [DOI] [PubMed] [Google Scholar]
- 23.Ahmad N, Khan MS, Afridi SA, Afridi SA, Awan AS, Afridi SK, Sultan S, Saifullah K, Lodhi FS. Efficacy and safety of interlocked intramedullary nailing for open fracture shaft of tibia. J Ayub Med Coll Abbottabad. 2016;28:341–344. [PubMed] [Google Scholar]
- 24.Kothadia S, Birole U, Ranade A. Paediatric salter-harris type IV injury of distal tibia with talus fracture. BMJ Case Rep. 2017;2017:bcr2017222226. doi: 10.1136/bcr-2017-222226. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Ladurner A, Acklin YP, Mueller TS, Sommer C. Decrease surgery time by using an alternative lateral parapatellar approach for tibia shaft fracture nailing. Arch Orthop Trauma Surg. 2019;139:943–949. doi: 10.1007/s00402-019-03154-2. [DOI] [PubMed] [Google Scholar]
- 26.Hake ME, Goulet JA. Open reduction and internal fixation of the posteromedial tibial plateau via the lobenhoffer approach. J Orthop Trauma. 2016;30(Suppl 2):S35–36. doi: 10.1097/BOT.0000000000000582. [DOI] [PubMed] [Google Scholar]


