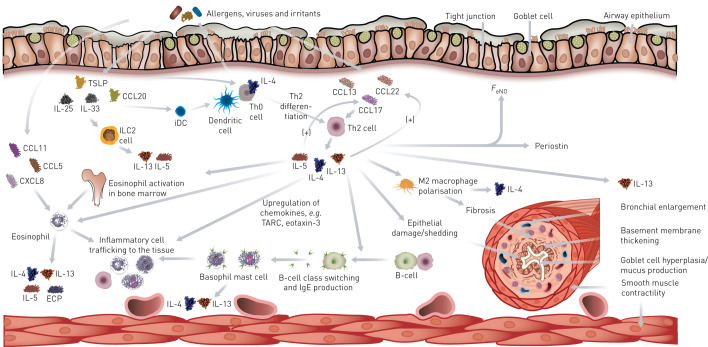
FIGURE 2.
The interplay between innate and adaptive cells and mediators in type 2 inflammation underpins asthma pathophysiology. Disruption of the epithelium allows penetration by allergens, viruses or bacteria, activating innate and adaptive immune responses. Presentation of antigens by dendritic cells activates naïve T-helper cells (T-helper cell type 0 (Th0) cells) to differentiate into T-helper cell type 2 (Th2) cells, which in turn produce interleukin (IL)-4, leading to further differentiation of Th0 cells. Cytokines released by Th2 cells lead to eosinophil activation and trafficking of inflammatory cells, B-cell class switching and changes to the airway, including basement membrane thickening, bronchial enlargement, goblet cell hyperplasia and fibrosis. CCL: chemokine (C-C motif) ligand; CXCL: chemokine (C-X-C motif) ligand; ECP: eosinophil cationic protein; FeNO: fraction of exhaled nitric oxide; iDC: interstitial dendritic cell; ILC2: type 2 innate lymphoid cell; TARC: thymus and activation-regulated chemokine; TSLP: thymic stromal lymphopoietin.