Abstract
Odontogenic carcinosarcoma (OCS) is a rare malignant odontogenic tumor (OT) with only a few cases reported in the literature. Its synonyms are ameloblastic carcinosarcoma, malignant mixed OT. It is characterized by a true mixed tumor showing malignant cytology of both epithelial and mesenchymal components. The tumor invaded into adjacent tissues by destroying the bone. A 24-year-old patient visited the outpatient clinic of GITAM Dental College and Hospital, with a chief complaint of growth in the lower right back tooth region for 6 months. Based on clinical and radiographic features, it has been diagnosed as an aggressive central jaw lesion. The patient was further referred for histological examination for confirmatory diagnosis. It has been diagnosed as an adenomatoid OT. The OCS most commonly affects the posterior part of the mandible. A larger number of cases were reported recently, and prolonged follow-up is needed to further clarify the nature of OCS.
Keywords: Ameloblastoma, Odontogenic Tumors, mixed odontogenic tumor, complex disease, malignant odontogenic tumor
INTRODUCTION
Odontogenic tumors (OTs) are a heterogeneous group of lesions with different clinical behavior and histological types.[1] OT is broadly divided into two categories as benign and malignant. The majority of benign OTs seem to arise de novo, whereas malignant OTs may arise de novo but more often arise from benign precursors. According to the recent World Health Organization (WHO), in the Classification of OT 2017, odontogenic carcinosarcoma (OCS) was newly added.[2,3,4]
Heath et al. first described malignant OTs; ameloblastic fibrosarcoma (AFS) was most common in 1887.[5] Since then, about 100 cases of similar microarchitectural features were described in the literature. The WHO classification of odontogenic tumors designated AFS as a distinctive neoplasm in “blue book “edition, published in 1972. In 1991, Dr. Takuji Tanaka and co-workers first reported OT that was composed of a mixture of malignant ameloblastoma (ameloblastic carcinoma) and fibrosarcoma.[6] In 1992, WHO Classification of OTs introduced OCS. In 2005, the WHO removed OCS from the OT classification because of unknown origin and difficulty in separating from the spindle-cell ameloblastic carcinoma (SC-AMECA). Subsequently, OCS was reintroduced as a distinct disease in the newest WHO classification of OT (2017) as a result of new cases published in the literature.
The objective of the present study was based on published data, review on clinical, radiological and histopathological features, present surgical treatment options, recurrence frequency and survival of this condition.
CARE REPORT
A 24-year-old patient visited the outpatient clinic of GITAM Dental College and Hospital with a chief complaint of growth and swelling in the lower right back tooth region for 6 months. The patient gave a history of gradually increasing swelling for 6 months. The swelling initially started small and gradually enlarged to the present size, the complaining of pain for 1 week. The swelling was not associated with paresthesia, pus discharge or any other secondary change. The patient also gives the history of growth, for which the patient previously visited a private dental clinic where a biopsy was done and diagnosed as an ulcer with acute nonspecific inflammation and mild dysplasia was given. The patent visited our hospital for further treatment.
Extraoral examination
On Inspection the face was asymmetrical , swelling observed in the lower one-third of the face on the right side, as shown in [Figures 1-3]. A swelling was observed on the lower one-third of the face, measuring around 8 cm × 4 cm in its greatest diameter. Anteroposteriorly, the swelling extended from the parasymphysis region to the angle of the mandible and also extended onto the ramus of the mandible. Superoinferiorly, it extended below the ala-tragal line to 0.5 cm below the lower border of the mandible. The surface was regular, borders were ill defined and the overlying skin was normal. On palpation, tenderness was absent, hard in consistency, noncompressible, nonfluctuant and no secondary changes were present.
Figure 1.

Face asymmetrical with swelling in the lower one-third of the face on the right side
Figure 3.

Swelling extending below the lower boarder of the mandible on the right side
Figure 2.

Swelling in the lower one-third of the face on the right side
Intraoral examination
On intraoral examination, nodular erythematous ulcerated growth was observed in relation to 43, 44 and 45 tooth regions. The growth was extending mesiodistally from 43 to 46 region and free gingival in relation to 43 to 46 to the buccal vestibule with obliterating the vestibule [Figure 4]. The bicortical expansion was present mesial aspect of 43 to the distal aspect of 45.
Figure 4.

Nodular erythematous ulcerated growth in relation to 44–46 tooth region with obliteration of vestibule
Based on clinical features and examination, a provisionally diagnosed as aggressive jaw lesion/central jaw lesion. Further radiological investigations were done to come to the final diagnosis.
Radiological investigations
On panoramic radiography, the multilocular ill-defined radiolucent lesion was observed in relation to 41–46. The associated teeth near the radiolucency had resorption of roots. There was an unerupted submerged tooth associated with the radiolucent area [Figure 5]. Cone-beam computed tomography revealed an ill-defined hypodense lesion involving the symphysis and parasymphysis, i.e., from 41 to 46. There was aggressive bone destruction and bone loss in lower border mandible buccolingually with associated tooth root resorption [Figure 6]. The biopsy specimens were obtained and sent for histopathological examination.
Figure 5.

Multilocular ill-defined radiolucent lesion with root resorption and submerged tooth observed
Figure 6.

Computed tomography shows destruction of the inner and outer cortex in parasymphysis of the right mandible when viewed from the buccal and lingual aspect
Macroscopic examination
Multiple bits of soft tissue specimen were received, which was soft in consistency, multinodular, white to brown. The soft tissues were taken for processing.
Microscopic examination
The hematoxylin and eosin-stained soft tissue sections exhibit invasive tumors consisting of epithelial and mesenchymal neoplastic components. Islands and cords of ameloblastic epithelial cells and hypercellular mesenchymal cells were observed. The connective tissue shows large epithelial odontogenic islands with ameloblastic-like cells in the periphery and stellate reticulum-like cells in the center. The connective tissue exhibits budding and branching epithelial cord widely separated by hypercellular fibroblastic stroma. The cells in the sarcomatous component are markedly pleomorphism with enlarged and bizarre nuclei. The epithelial component was frankly malignant with cytological atypia, hyperchromatic nuclei, increased mitoses, enlarged hyperchromatic nuclei and increased nuclear-to-cytoplasmic ratio. The connective tissue also exhibited dense collagen fibers; few inflammatory cells infiltrate vascular spaces and red blood cells [Figures 7-11].
Figure 7.
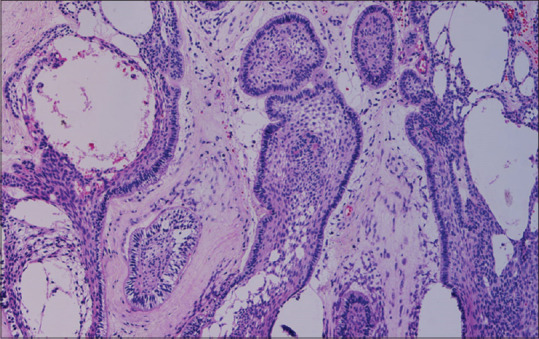
Hematoxylin and eosin-stained section exhibits plexiform arrangement of cells in connective tissue stroma with bone viewed in ×4
Figure 11.

(a and b) Hematoxylin and eosin ×40 stained section malignant epithelium cells with hyperchromatic, bizarre, vesicular nuclei and mitotic figures
Figure 8.

Hematoxylin and eosin-stained section exhibits cords of ameloblastic cells in connective tissue viewed in ×10
Figure 9.

Hematoxylin and eosin-stained section exhibits island with peripheral tall columnar cells with reversal of polarity with central stellate reticulum-like cells viewed in ×10
Figure 10.

(a) Hematoxylin and eosin ×20 stained section exhibits ameloblastic follicles, comprising of malignant, pleomorphic, hyperchromatic, bizarre, vesiculous nuclei, cuboidal or low columnar cells with inverted polarization and mitotic figures. (b) Neoangiogenesis within central stellate reticulum-like cells
Immunohistochemistry
The specimen has been processed by the horseradish peroxidase polymer method. Protein retrieval has been done by the heat-induced epitope retrieval technique. The following antibody clones have been used:
Monoclonal mouse antihuman cytokeratin clone AE1/AE3
Monoclonal mouse antihuman cytokeratin clone V9.
Cytokeratin has revealed that ameloblastic epithelium showing positive staining and stroma is negative [Figure 12]. Vimentin has shown ameloblastic epithelium negative and stroma is positive [Figure 13].
Figure 12.

Epithelial island showing intense positivity with cytokeratin AE1/AE3 immunohistochemical stain, original magnification ×10
Figure 13.

Mesenchymal component showing diffuse intense positivity with vimentin immunohistochemical stain, original magnification ×10
Based on clinical, radiographic, histopathological findings and immunohistochemical studies are suggestive of “OCS.”
DISCUSSION
In 1992, WHO defined the OCS as “a very rare neoplasm, similar in pattern to AFS, but in which both the epithelium and mesenchymal components show cytological features of malignancy.” The terms ameloblastic carcinosarcoma and malignant odontogenic mixed tumor are synonyms of OCS.[7]
The mandible is the only reported site of occurrence. The size of the lesion was approximately 6–8 cm. The tumor had resulted gradually in the bicortical expansion of the body of the mandible for several months. It was usually painless, sometimes associated with paresthesia of the lower lip.
The etiopathogenesis was de novo, arising from remnants, originated from the embryologic process of odontogenesis or can develop from a preexisting odontogenic lesion. Clinically, OCS has aggressive behavior with high rates of recurrence and frequent metastasis. The OCS was generally misdiagnosed as ameloblastic carcinoma due to failure to identify the malignant mesenchymal component.[8]
In 1999, Slater stated that “such tumor had not been reported as yet, to the best of my knowledge.” A literature search in 2001 did not reveal any case reports or mentions of this neoplasm. In his review, however, Slater presented a case of OCS from his files.[9]
A 55-year-old man living in Saudi Arabia had a tumor on the right body and ramus of mandible excised by hemimandibulectomy. Slater[10] further pointed out that a carcinosarcoma lacking the ameloblastic fibroma-like pattern could still be recognized as odontogenic if the epithelial component resembled that of ameloblastoma. He considered a tumor of this type to be a sarcomatoid carcinoma arising in an ameloblastoma and not ameloblastic carcinosarcoma. Sarcomatoid carcinomas or carcinosarcomas have been reported as mixed tumors (malignant ameloblastoma and fibrosarcomas) and as odontogenic carcinoma with sarcomatous proliferation.[10]
The conference held at Lyon in July 2003 WHO decided not to include the OCS in any WHO classification because there was no immunohistochemical origin confirmed. Another reason was the OCS had similar histopathological features as that of SC-AMECA. It was difficult to distingue both the lesions, so WHO decided to remove OCS from 2005.
Subsequently, OCS was reintroduced as a distinct disease in the newest WHO Classification of OT (2017), almost 30 years after its first description in the literature, little is known about OCS pathogenesis, epidemiology and outcomes.
Table 1: Describes the review of literature of 136 references, and ten articles are following features.[11,12,13,14,15,16,17,18,19,20]
Table 1.
Review Of Literature Of Identified Odontogenic Carcinosarcoma Cases
| Author (s) (year of publication) | Country Patient | Age/sex | Anatomical location | Clinical presentation | Symptoms | Preexisting lesion | Radiological Features | Treatment Recurrence |
|---|---|---|---|---|---|---|---|---|
| Tanaka et al. (1991) | Japan | 63 M | Posterior maxilla Gingiva | ulcer & Swelling | not informed | Ameloblastoma | Radiolucent, ill-defined, bordered area | Hemimaxillectomy + chemotherapy |
| Hosokawa et al. (1991) | Japan | 30 M | Posterior Mandible& Maxillaa | Swelling | Pain | Cementomatous lesion/benign osteoblastoma | Radiopaque image within the fairly well circumscribed Radiolucent area | not informed |
| Slater (1999) | Saudi Arabia | 55 M | Posterior mandible | Tumor | not informed | Ameloblastic fibroma | not informed | Hemimandibulectomy |
| Slama et al. (2002) | France | 26 F | Posterior mandible | Swelling and bone expansion | Pain and numbness of the lip | Ameloblastoma | Mixed, ill-defined | Hemimandibulectomy |
| Kunkel et al. (2004) | Germany | 52 M | Posterior mandible | Tumor with a central exophytic area. | Numbness of the lower lip | Ameloblastic fibrosarcoma | Radiolucent with indistinct margins & fine bony Spicules | Hemimandibulectomy including wide surgical excision of the surrounding soft tissues |
| DeLair et al. (2007) | United States | 19 F | Posterior mandible | Indurated swelling | Pain and difficulty in open mouth | Ameloblastic fibroma | Radiolucency of the mandible body extending to the condyle | Hemimandibulectomy |
| Chikosi et al. (2011) | Venezuela | 9 F | Posterior mandible | Large lobulated purplish soft tissue mass | No pain but numbness of the lip | Ameloblastoma | Radiolucent lesion without defined borders extending to the retromolar area | Hemimandibulectomy + chemotherapy + radiation therapy |
| Kim et al. (2015) | South Korea | 61 M | Posterior mandible | No abnormality | Discomfort, intermittent paresthesia and a slightly painful mass | De novo | Radiolucent lesion of a round shape and with clear margins | Hemimandibulectomy |
| da Silva et al. (2017) | Brazil | 79 M | Posterior mandible | Swelling | Painful mass | De novo | lIll-defined bilocular Radiolucency with an Irregular osteolytic aspect | Marginal resection |
| Jean nune et al. (2018) | Brazil | 42 M | Posterior maxilla | Swelling | nasal obstriction | - | - | Patient did not report for treatment |
A PUBMED d searchhad provided 136 references, and ten articles with varied geographical distribution, OCS following data was collected. The patient age ranged from 9 to 79 and the mean age was 43.8. Males were commonly affected than females. Posterior part of the mandible was the most common site of occurrence, followed by the maxilla. All the individuals exhibited swelling; few cases were associated with pain. The radiological features such as lesion ill defined radiolucency with bicortical plate expansion. Concerning the origin, almost all the cases of OCS arise from preexisting OT, mostly ameloblastic and AFS, and treatment was hemimandibulectomy. The histopathological features observed were tabulated, as shown in Table 2.
Table 2.
Histopathologic features of odontogenic carcinosarcoma cases review.
| Author (s) (year of publication) | Epithelial features | Mesenchymal features |
|---|---|---|
| Tanaka et al. (1991) | Nests and strands of epithelial neoplastic cells, mainly cuboidal; atypical mitoses | Oval or spindle-shaped cells, nuclear polymorphism, abnormal mitoses |
| Hosokawa et al. (1991) Slater (1999) | Islands of polygonal epithelial cells scattered in an osteoid matrix | Not detailed |
| Ameloblastic fibroma-like pattern with budding and branching epithelial cords widely separated by hypercellular fibrous connective tissue, hyperchromatic nuclei, mitotic figures, peripheral large cells, basaloid cells among plump cells in the central stellate reticulum area, and epithelial cords | Closely packed mitotically active polygonal cells, hyperchromatic nuclei, moderate nuclear pleomorphism | |
| Slama et al. (2002) | Follicular structures formed by ameloblastic epithelial cells with cytological criteria of malignancy: round or ovoid nucleus, high nuclear-cytoplasmic ratio and dense and irregularly distributed chromatin | The proliferation of fusiform cells of fibroblastic type with elongated nuclei, atypical with a high mitotic index allowing the diagnosis of fibrosarcoma |
| Kunkel et al. (2004) | Islands and cords of malignant epithelial cells, rows of cuboidal or low columnar cells, hyperchromatic nuclei with coarse chromatin, irregular nuclear margins, numerous mitotic figures; necrotic areas | Hypercellular mesenchymal and pleomorphic cells, typical cytological features of malignancy |
| DeLair et al. (2007) | Multiples areas showed a typical ameloblastoma-like proliferation consisting of island and cords of tall, columnar, peripheral palisading cells; pleomorphism; large and hyperchromatic nuclei, increased nuclear-to-cytoplasmic ratio, loss of the typical ameloblastic architecture, peripheral nuclear palisading | Hypercellularity, pleomorphism, enlarged nuclei, bizarre nuclei, multinucleation of cells; occasional mitoses |
| Chikosi et al. (2011) | Islands, large pleomorphic cells and nuclei, hyperchromatic nuclei, atypical mitotic figures | Islands, large pleomorphic cells and nuclei, hyperchromatic nuclei, atypical mitotic figures |
| Kim et al. (2015) | Nests and strands similar to ameloblastoma, aberrant cytological atypia, hyperchromasia, abnormal mitoses | Pleomorphism, enlarged hyperchromatic nuclei, increased nuclearto- cytoplasmic ratio |
| da Silva et al. (2017) | Island and cords of malignant epithelial cells, polygonal or ovoid cells, hyperchromatic or vesiculous nuclei, cuboidal or low columnar cells with inverted polarization, mitotic figures | Pleomorphic and hyperchromatic hypercellular mesenchymal cells |
In the present case, a 24-year-old male reported with a chief complaint of swelling in the right posterior mandible. On radiological examination, an ill-defined aggressive bone resorption with bicortical plate expansion was observed. The biopsy was obtained and histological examination was done. Based on the histopathological examination, final diagnosis of OCS was given.
Histopathological feature of OCS has close resemblance with other OTs, the main differential diagnosis is given in Table 3 and flow chart 1.
Table 3.
Summary of the differential diagnosis for odontogenic carcinosarcoma
| Diagnosis Origin | Histopathology | Treatment |
|---|---|---|
| Ameloblastic carcinosarcoma | Outer arrangement of columnar or palisaded ameloblast like cells Inner zone of triangular shaped stellate reticulam cells.ameloblast cells shows nuclear hyperchromatism and pleomorphism. | Surgical resection |
| Ameloblastic fibroma | Epithelium proliferating in a ‘cord like fashion’ Connective tissue backgroundSpindled and angular cells |
Curettage or surgical resection |
| Ameloblastic fibrosarcoma | thin branching cords or small nests of odontogenic epithelium Little cytoplasm and basophilic nucleiMesenchymal component: malignant Pleomorphic fibroblasts with hyperchromatic nuclei, atypical mitoses |
Radical surgical resection , Adjuvant treatment (controversial) |
| Odontogenic carcinosarcoma | Mesenchymal component: malignant Epithelial component: malignant |
Radical surgical resection Adjuvant treatment (controversial) |
Flow chart 1.

Various subtypes of OCS were recognized by WHO, based on the stage of dental development.[3,21,22,23]
The AFS has epithelial islands similar to those seen in ameloblastoma or ameloblastic fibroma, malignant mesenchymal fibrosarcoma-like features such as nuclear pleomorphism and high mitotic activity dispersed in the loose myxoid stroma.[10,22] When associated with dentin, the lesion is designated as ameloblastic fibrodentinosarcoma, and with enamel, it was designated as ameloblastic fibro-odontosarcoma. However, this subclassification has no prognostic relevance. It's extremely rare lesions with combinedcarcinomatous and sarcomatous elements hence the nameOCS or odontogenic carcinoma with sarcomatous proliferation was given.[24] It is important to differentiate OCS from other diseases with similar histological features.
Different immunohistochemical markerssuch as CAM 5.2, cytokeratin (5, 6, 8, 14, 17 and 19) and pancytokeratin AE1/AE3, the epithelial components demonstrated positivity. Vimentin and desmin were shown to be positive in the sarcomatous elements. Ki-67 and the p53 tumor suppressor gene were useful to determine proliferation.[14,15,16,17,18,24,25,26,27,28,29,30,31]
In the present case, cytokeratin has revealed ameloblastic epithelium showing positive staining and stroma is negative [Figure 12]. Vimentin has shown ameloblastic epithelium negative and stroma is positive [Figure 13], thus confirming the respective origins. Hence, it is the lesion with combined carcinomatous and sarcomatous proliferation.
Hence by correlating clinical, radiographic, histopathological findings and immunohistochemical studies, it was confirmed as a case of OCS.
Treatment of choice was wide surgical resection with long-term follow-up. Postoperative chemotherapy and radiotherapy have been used for the successful treatment of OCS cases. In most of the cases, recurrence was noted. Long-term follow-up was required in all the cases. Poor prognosis, death is reported in 50% of cases.
In the present case, wide surgical excision is done under anesthesia. The patient was under regular follow-up till date, no recurrence has been observed.
CONCLUSION
Due to the low prevalence of odontogenic malignancies such as OCS, dentists must be aware of histopathological differential diagnosis of malignant tumors such as ameloblastic carcinoma, AFS and SC-AMECA and to provide a suitable parameter that can aid in classifying such aggressive and myriad spectrum of lesions.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
REFERENCES
- 1.Wright J, Soluk Tekkeşin M. Odontogenic tumors. Where are we in 2017? J Istanb Univ Fac Dent. 2017 Dec 2;51:S10–30. doi: 10.17096/jiufd.52886. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Takata T, Slootweg PJ, editors. WHO classification of Head and Neck Tumours. Chapter 8: Odontogenic and maxilofacial bone tumours. 4th ed. Lyon: IARC; 2017. pp. 205–260. [Google Scholar]
- 3.Barnes L, Eveson J, Reichart P, Sidransky D, editors. WHO Head and Neck Tumours. Chapter 6: Odontogenic Tumours. 3rd ed. Lyon: IARC; 2005. pp. 283–327. [Google Scholar]
- 4.Kramer IR, Pindborg JJ, Shear M. The WHO histological typing of odontogenic tumours. A commentary on the second edition. Cancer. 1992;70:2988–94. doi: 10.1002/1097-0142(19921215)70:12<2988::aid-cncr2820701242>3.0.co;2-v. [DOI] [PubMed] [Google Scholar]
- 5.Heath C. Five cases of tumor of jaws treated by excision. BMJ. 1887;1:777–9. [Google Scholar]
- 6.Servato J, Faria P, Ribeiro C, Cardoso S, Faria P, Dias F, et al. Ameloblastic fibrosarcoma: A case report and literature review. Braz Dent JMar-Apr. 2017;28:262–72. doi: 10.1590/0103-6440201701050. [DOI] [PubMed] [Google Scholar]
- 7.El-Naggar A. WHO Classification of Head and Neck Tumours. Lyon: International Agency for Research on Cancer (IARC); 2016. [Google Scholar]
- 8.Kim I, Pae S, Cho H, Cho H, Seo J, Lee D, et al. Odontogenic carcinosarcoma of the mandible: A case report and review. J Korean Assoc Oral Maxillofac Surg. 2015;41:139–44. doi: 10.5125/jkaoms.2015.41.3.139. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Reichart P, Philipsen H. Odontogenic Tumors and Allied Lesions. London: Quintessence; 2004. [Google Scholar]
- 10.Slater LJ. Odontogenic sarcoma and carcinosarcoma. Semin Diagn Pathol. 1999;16:325–32. [PubMed] [Google Scholar]
- 11.Kim IK, Pae SP, Cho HY, Cho HW, Seo JH, Lee DH, et al. Odontogenic carcinosarcoma of the mandible: A case report and review. J Korean Assoc Oral Maxillofac Surg. 2015;41:139–44. doi: 10.5125/jkaoms.2015.41.3.139. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.da Silva KD, Flores IL, Etges A, Vasconcelos AC, Mesquita RA, Gomes AP, et al. Unusual osteolytic lesion of the jaw. Oral Surg Oral Med Oral Pathol Oral Radiol. 2017;124:443–8. doi: 10.1016/j.oooo.2017.06.123. [DOI] [PubMed] [Google Scholar]
- 13.DeLair D, Bejarano PA, Peleg M, El-Mofty SK. Ameloblastic carcinosarcoma of the mandible arising in ameloblastic fibroma: A case report and review of the literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;103:516–20. doi: 10.1016/j.tripleo.2006.02.025. [DOI] [PubMed] [Google Scholar]
- 14.Kunkel M, Ghalibafian M, Radner H, Reichert TE, Fischer B, Wagner W. Ameloblastic fibrosarcoma or odontogenic carcinosarcoma: A matter of classification? Oral Oncol. 2004;40:444–9. doi: 10.1016/j.oraloncology.2003.09.010. [DOI] [PubMed] [Google Scholar]
- 15.Chikosi R, Segall N, Augusto P, Freedman P. Odontogenic carcinosarcoma: Case report and literature review. J Oral Maxillofac Surg. 2011;69:1501–7. doi: 10.1016/j.joms.2010.05.071. [DOI] [PubMed] [Google Scholar]
- 16.Tanaka T, Ohkubo T, Fujitsuka H, Tatematsu N, Oka N, Kojima T, et al. Malignant mixed tumor (malignant ameloblastoma and fibrosarcoma) of the maxilla. Arch Pathol Lab Med. 1991;115:84–7. [PubMed] [Google Scholar]
- 17.Hosokawa Y, Minowa K, Abe S, Ohmori K, Yamasaki M, Shindoh M, et al. Invasion of the intracranial space by a malignant odontogenic mixed tumor: Report of a case. Oral Radiol. 1991;7:1–6. [Google Scholar]
- 18.Slama A, Yacoubi T, Khochtali H, Bakir A. Mandibular odontogenic carcinosarcoma: A case report. Rev Stomatol Chir Maxillofac. 2002;103:124–7. [PubMed] [Google Scholar]
- 19.Schuch LF, de Arruda JA, Silva LV, Abreu LG, Silva TA, Mesquita RA. Odontogenic carcinosarcoma: A systematic review. Oral Oncol. 2018;85:52–9. doi: 10.1016/j.oraloncology.2018.08.017. [DOI] [PubMed] [Google Scholar]
- 20.Dos Santos JN, Servato JP, Cardoso SV, de Faria PR, Pires BC, Loyola AM. Odontogenic carcinosarcoma: Morphologic and immunohistochemical description of a case. Oral Surg Oral Med Oral Pathol Oral Radiol. 2018;126:e264–70. doi: 10.1016/j.oooo.2018.05.013. [DOI] [PubMed] [Google Scholar]
- 21.Sapp JP, Eversol LR, Wysocki GP. Contemporary Oral and Maxillofacial Pathology. 2nd ed. New York: Elsevier Inc; 2004. [Google Scholar]
- 22.Slootweg PJ. Malignant odontogenic tumors: An overview. Mund Kiefer Gesichtschir. 2002;6:295–302. doi: 10.1007/s10006-002-0419-y. [DOI] [PubMed] [Google Scholar]
- 23.Richardson MS, Muller S. Malignant odontogenic tumors: An update on selected tumors. Head Neck Pathol. 2014;8:411–20. doi: 10.1007/s12105-014-0584-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Muller S, Parker DC, Kapadia SB, Budnick SD, Barnes EL. Ameloblastic fibrosarcoma of the jaws. A clinicopathologic and DNA analysis of five cases and review of the literature with discussion of its relationship to ameloblastic fibroma. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1995;79:469–77. doi: 10.1016/s1079-2104(05)80130-1. [DOI] [PubMed] [Google Scholar]
- 25.Altini M, Thompson SH, Lownie JF, Berezowski BB. Ameloblastic sarcoma of the mandible. J Oral Maxillofac Surg. 1985;43:789–94. doi: 10.1016/0278-2391(85)90336-2. [DOI] [PubMed] [Google Scholar]
- 26.Kawauchi S, Hayatsu Y, Takahashi M, Furuya T, Oga A, Niwa S, et al. Spindle-cell ameloblastic carcinoma: A case report with immunohistochemical, ultrastructural, and comparative genomic hybridization analyses. Oncol Rep. 2003;10:31–4. [PubMed] [Google Scholar]
- 27.da Silva KD, Flores IL, Etges A, Vasconcelos AC, Mesquita RA, Gomes AP, et al. Ameloblastic carcinosarcoma: A case report. In abstracts of XXIII Brazilian congress of oral medicine and oral pathology 8-11 July 2015 – Sao Paulo, Brazil. Oral Surg Oral Med Oral Pathol Oral Radiol. 2017;123:E54. [Google Scholar]
- 28.Shinoda T, Iwata H, Nakamura A, Ohkubo T, Yoshimi N, Sugie S, et al. Cytologic appearance of carcinosarcoma (malignant ameloblastoma and fibrosarcoma) of the maxilla. A case report. Acta Cytol. 1992;36:132–6. [PubMed] [Google Scholar]
- 29.Matsushita Y, Fujita S, Yanamoto S, Yamada S, Rokutanda S, Yamashita K, et al. Spindle cell variant of ameloblastic carcinoma: A case report and literature review. Oral Surg Oral Med Oral Pathol Oral Radiol. 2016;121:e54–61. doi: 10.1016/j.oooo.2015.06.034. [DOI] [PubMed] [Google Scholar]
- 30.McNaught MJ, Turella SJ, Fallah DM, Demsar WJ. Spindle cell variant of ameloblastic carcinoma: A case report and review of literature. Mil Med. 2015;180:e614–7. doi: 10.7205/MILMED-D-14-00509. [DOI] [PubMed] [Google Scholar]
- 31.Servato JP, Faria PR, Ribeiro CV, Cardoso SV, Faria PR, Dias FL, et al. Ameloblastic fibrosarcoma: A case report and literature review. Braz Dent J. 2017;28:262–72. doi: 10.1590/0103-6440201701050. [DOI] [PubMed] [Google Scholar]


