Abstract
Background and Aims
Vibration-controlled transient elastography (VCTE) is a noninvasive tool that uses liver stiffness measurement (LSM) to assess fibrosis. Since real-life data during everyday clinical practice in the USA are lacking, we describe the patterns of use and diagnostic performance of VCTE in patients at an academic medical center in New York City.
Methods
Patients who received VCTE scans were included if liver biopsy was performed within 1 year. Diagnostic performance of VCTE in differentiating dichotomized fibrosis stages was assessed via area under the receiver operating characteristics (AUROC). Fibrosis stage determined from VCTE LSM was compared to liver biopsy.
Results
Of 109 patients, 49 had nonalcoholic fatty liver disease, 16 chronic hepatitis C, 15 congestive hepatopathy, and 22 at least two etiologies. AUROC was 0.90 for differentiating cirrhosis (stage 4) with a positive predictive value (PPV) range of 0.28 to 0.45 and negative predictive value range of 0.96 to 0.98. For 31 (32%) patients, VCTE fibrosis stage was at least two stages higher than liver biopsy fibrosis stage. Thirteen of thirty-five patients considered to have cirrhosis by VCTE had stage 0 to 2 and 12 stage 3 fibrosis on liver biopsy.
Conclusions
VCTE has reasonable diagnostic accuracy and is reliable at ruling out cirrhosis. However, because of its low PPV, caution must be exercised when used to diagnose cirrhosis, as misdiagnosis can lead to unnecessary health care interventions. In routine practice, VTCE is also sometimes performed for disease etiologies for which it has not been robustly validated.
Keywords: Chronic liver disease, Cirrhosis, Hepatitis, Liver histopathology, Nonalcoholic fatty liver disease
Introduction
Chronic liver disease (CLD) is a major public health burden in the USA. In 2017, more than 41,000 Americans died from CLD, making it the fifth leading cause of mortality for ages 40 to 59 years and eleventh leading cause overall.1 Regardless of etiology, it is important to obtain an accurate assessment of CLD severity for clinical management. Staging of liver fibrosis helps predict a patient’s risk of progression to cirrhosis and its complications, determine potential therapeutic and surveillance options, and evaluate eligibility for clinical trials.2,3 Diagnosis and staging of mild to moderate fibrosis allow for appropriate risk stratification and delivery of care to high-risk individuals to attempt to prevent further progression.4 A diagnosis of cirrhosis initiates biannual radiological imaging and blood tests for serum alpha-fetoprotein to screen for hepatocellular carcinoma, as well as upper endoscopy to screen for esophageal varices.
Liver biopsy is the gold standard for fibrosis staging as well as evaluation of inflammation and providing critical diagnostic information.5 However, the procedure has limitations, including invasiveness, sampling error, intra-/inter-observer variability, potential complications such as bleeding, and cost.6 Therefore, noninvasive methods of assessing liver fibrosis have been developed.7 Vibration-controlled transient elastography (VCTE) is an ultrasound-based test that potentially offers a safe and rapid point-of-care solution.7 A shear wave is generated across the liver using a transducer probe; the velocity of its propagation is measured and converted to a liver stiffness measurement (LSM), which is used as a marker of fibrosis.6,7 VCTE has been extensively studied in several CLD etiologies and evidence best supports its use in ruling out cirrhosis via validated LSM thresholds for patients with chronic viral hepatitis, as well as, to a lesser extent, alcoholic liver disease.4,8 Recent literature and guidelines also support the use of VCTE in identifying advanced liver fibrosis and cirrhosis in patients with nonalcoholic fatty liver disease (NAFLD).9–13 However, there are major limitations in its application, including lack of defined LSM thresholds for cirrhosis and increased LSM in patients with a body mass index (BMI) ≥30 kg/m2 regardless of type of probe used.14,15 Currently, there is no compelling evidence for the use of VCTE in CLD of other etiologies.9
VCTE has gained significant popularity in Europe since its introduction almost two decades ago, establishing itself as the noninvasive standard for liver fibrosis assessment.16 Clinical practice guidelines issued by the European Association for the Study of the Liver recommend cirrhosis screening via VCTE for all patients with chronic hepatitis C.8 VCTE is also approved in parts of Asia, and the China Foundation for Hepatitis Prevention and Control provided recommendations for its use in 2012.17 In comparison, adoption of VCTE has been slower in the USA, with a later regulatory approval in 2013.16 Since then, several USA-based studies have been published, with most focusing on validating the diagnostic performance of VCTE in prospective longitudinal cohorts where patients with one or two CLD etiologies were selected based on a series of inclusion and exclusion criteria.13,18–20 However, there has been limited published data describing the use of VCTE by clinicians during regular, everyday clinical operations in real-life patient populations in the USA. To bridge this gap, we conducted this retrospective study at a single academic tertiary care medical center in the USA. The aims were to characterize the center’s experience in utilizing VCTE during its early years of adoption and assess diagnostic accuracy using liver biopsy as comparison.
Methods
Study population
This was a retrospective study conducted at Columbia University Irving Medical Center in New York City. We included adult Liver Clinic and Liver Transplant Clinic patients who underwent VCTE between February 2016 and April 2018. Attending hepatologists or gastroenterology fellows, supervised by attendings, followed these patients for a wide range of conditions, including diagnostic workup of abnormal liver blood tests, longitudinal care of CLD, and pre-transplant evaluations. Patients were included if they received a liver biopsy within 1 year of a VCTE scan and before April 2018. The 1-year interval threshold was chosen due to the minimal progression of liver fibrosis for CLD etiologies, including the three most prevalent ones in this study, during that time period.21–23 In cases where multiple VCTEs and/or liver biopsies were performed during the study period, one pair of data was chosen by minimizing the duration between scan and biopsy while also taking completeness of each study into consideration. The Columbia University Institutional Review Board approved the protocol with a waiver of informed consent. For liver transplant recipients included in this study, no donor organs were obtained from executed prisoners or other institutionalized persons.
Clinical data collection
We reviewed electronic medical records to obtain the following parameters at the time of VCTE: age, sex, race, ethnicity, comorbidities (history of type II diabetes mellitus, hypertension, dyslipidemia), and history of smoking or heavy alcohol use. Smoking was defined by any current or past use of cigarettes, and heavy alcohol use by consumption greater than moderate as defined by 2015–2020 Dietary Guidelines for Americans.24 Weight, BMI, serum total bilirubin concentration, serum aspartate aminotransferase, alanine aminotransferase, and alkaline phosphatase activities, international normalized ratio, serum creatinine concentration and platelet count closest to the date of VCTE were recorded. Aspartate aminotransferase to platelet ratio index fibrosis-4 index were calculated as described.25,26 CLD etiology for each patient was determined by a review of diagnoses rendered by an attending liver pathologist in the liver biopsy report and the judgement of clinicians as documented in records. Multiple diagnoses per patient and nonspecific diagnosis are possible.
Liver histology
Liver biopsies were performed by either percutaneous or transjugular approaches for a range of indications as determined by the patient’s physician. An attending liver pathologist interpreted each liver biopsy as per regular clinical operation, providing diagnoses and fibrosis assessment in each pathology report. Some liver biopsies were performed at outside institutions and re-interpreted by a liver pathologist at Columbia University. Tissue sections from all biopsies were stained with Masson’s trichrome to assess fibrosis. Three distinct fibrosis staging systems were utilized. In patients with congestive hepatopathy, isolated perivenular fibrosis, extensive perivenular fibrosis, bridging fibrosis, and cirrhosis represent stage 1 through stage 4 fibrosis respectively.27 For NAFLD patients, perisinusoidal or periportal fibrosis signifies stage 1, perisinusoidal and periportal fibrosis represent stage 2, while bridging fibrosis and cirrhosis represent stage 3 and stage 4.28 The staging system for chronic viral hepatitis was used for all remaining etiologies, where stage 1 and stage 2 are portal fibrosis and periportal fibrosis, while stage 3 is bridging fibrosis and stage 4 is cirrhosis.29 All three staging systems are very similar with minor differences in the earlier stages. For each biopsy, stages 0 to 4 were determined using the appropriate staging system and included in most pathology reports. For reports without this type of staging, a liver pathologist (AL, JHL) re-reviewed these biopsies. If a range of fibrosis stages was provided for a biopsy (for example, stage 1–2), we used the higher stage in data analysis.
VCTE
Fourteen different operators performed VCTE using a FibroScan 502 Touch (Echosens, Paris, France) to simultaneously measure LSM and controlled attenuation parameter (CAP). All operators were experienced hepatologists or nurse practitioners at the Liver Transplant Clinic of Columbia University Irving Medical Center and were trained and had experience performing VCTE. After fasting for at least 3 hours prior to the scan, patients were placed in supine position with right arm in maximum abduction to allow optimal exposure of right lateral abdomen. Measurements were obtained using either an M or XL probe placed within an intercostal space over the right hepatic lobe. Probe selection was performed using the FibroScan automatic probe selection tool with operator discretion in select cases. LSM interquartile range (IQR) to median ratio (IQR/median) and CAP IQR were recorded as well. At least 10 sets of valid measurements were required for a successful study; results were considered unreliable if IQR/median was greater than 30% when median LSM was greater than 7.1 kPa.30 Using LSM cut-offs provided within the device software, combined with patient’s clinical history and recent liver blood tests when CLD etiology was unknown, the operator determined a fibrosis stage from F0 to F4. As with liver biopsy, if a range of fibrosis stages was documented, we used the higher stage in data analysis.
Statistical analysis
Patient characteristics are presented using descriptive statistics where continuous variables are reported as median [IQR]. Categorical variables are reported as absolute number (proportion %). Ranges for continuous variables are also provided.
We used Wilcoxon rank sum test to assess differences between two groups for continuous variables and Kruskal-Wallis test to compare LSM across all fibrosis stages (more than two groups). We used post-hoc Dunn’s test with Benjamini-Hochberg adjustment for multiple comparisons. For comparison of categorical variables between two groups, we used Fisher’s exact test. Kendall rank correlation coefficient was used to assess correlation between LSM and fibrosis stage by liver biopsy as well as between stages by VCTE and biopsy. We assessed diagnostic performance of LSM in evaluating fibrosis via area under the receiver operating characteristics (AUROC) and its 95% confidence interval (CI). To differentiate between dichotomized fibrosis stages (for example, stage 0 vs. stage 1–4) using VCTE, we calculated LSM cut-off values using three methods: Youden’s index, which maximizes both sensitivity and specificity, setting sensitivity to 0.90, and setting specificity to 0.90. We calculated sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV) for each LSM cut-off when used to identify the higher fibrosis stage.
We constructed univariate linear regression models to assess potential influences of various demographic, clinical, biopsy, and VCTE variables on LSM. Variables with p-values of <0.20 on univariate analysis were included in the initial multivariate linear regression model, and subsequently model selection was performed via a stepwise backwards selection process using Bayesian Information Criteria. LSM, the dependent variable, was transformed to normal distribution using the Box-Cox method in all regression models. We then used the final multivariate linear regression model to predict LSM as a function of CAP and biopsy fibrosis stage. For all statistical analyses, we considered p-values <0.05 to be statistically significant. All statistical analyses were conducted using RStudio software (PBC, Boston, MA, USA).
Results
Patient characteristics
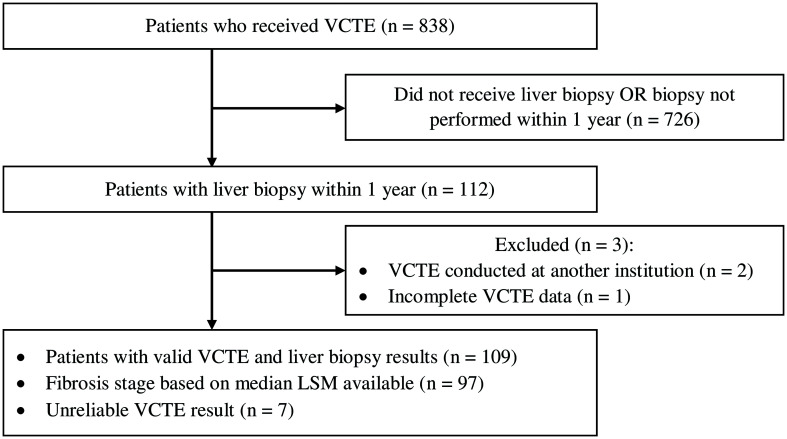
Among 838 patients who underwent VCTE between February 2016 and April 2018, 112 received liver biopsy within 1 year. Of these patients, two received VCTE at an outside institution and one additional patient’s VCTE result was not completely recorded. Therefore, 109 patients met our inclusion criteria (Fig. 1).
Fig. 1. Study entry flow chart.
The patient cohort had a median age [IQR] of 56 [27] years, more men (freq.=59, 54%) than women, and most patients being white (freq.=73, 67%) and non-Hispanic (freq.=79, 72%) (Table 1). Regarding comorbidities, 32% (freq.=35) had type II diabetes mellitus, 54% (freq.=59) had hypertension, and 50% (freq.=55) had dyslipidemia; median BMI [IQR] was 27.86 [6.68] kg/m2. Median values for liver-related blood tests were all within normal laboratory reference values. Patients had diverse initial chief complaints, ranging from elevated serum aminotransferase and alkaline phosphatase activities, abnormal liver imaging, to pre-transplant evaluation and post-transplant monitoring. The most common etiology of liver disease was NAFLD (freq.=49, 45%), followed by chronic hepatitis C (freq.=16, 15%), and congestive hepatopathy (freq.=15, 14%); only 7% (freq.=8) of patients had apparently normal liver and 9% (freq.=10) had CLD of unclear etiology. Additionally, 80% (freq.=87) had a single liver disease diagnosis, while 16% (freq.=17) had two and 5% (freq.=5) had three.
Table 1. Patient characteristics, n=109.
| Patient characteristic | Distribution† | Range |
|---|---|---|
| Age in years | 56 [27] | 23–78 |
| Sex, males | 59 (54) | – |
| Race | White: 73 (67) | – |
| African American: 13 (12) | – | |
| Asian: 5 (5) | – | |
| Other: 7 (6) | – | |
| Unknown: 11 (10) | – | |
| Ethnicity | Hispanic/Latino: 20 (18) | – |
| Not Hispanic/Latino: 79 (72) | – | |
| Unknown/Declined: 10 (9) | – | |
| Weight in kg | 78.0 [24.5] | 40.8–129.6 |
| BMI in kg/m2 | 27.86 [6.68] | 17.7–49.4 |
| Type II diabetes | 35 (32) | – |
| Hypertension | 59 (54) | – |
| Dyslipidemia | 55 (50) | – |
| Heavy alcohol use | 24 (22) | – |
| Smoking | 49 (46) | – |
| Total bilirubin in mg/dL | 0.5 [0.4] | 0.1–3.2 |
| AST in U/L | 37 [43] | 10–397 |
| ALT in U/L | 39 [48] | 7–444 |
| Alkaline Phosphatase in U/L | 95 [77] | 37–845 |
| Platelets count ×103/µL | 197 [106] | 55–412 |
| INR | 1.1 [0.2] | 0.88–2.7 |
| Albumin in g/dL | 4.4[0.5] | 1.3–5.3 |
| Creatinine in mg/dL | 0.93 [0.67] | 0.5–10.0 |
| Liver disease etiology | NAFLD: 49 (45) | – |
| Hepatitis C: 16 (15) | – | |
| Congestive: 15 (14) | – | |
| Non-specific: 10 (9) | – | |
| Autoimmune: 9 (8) | – | |
| Normal: 8 (7) | – | |
| Post-transplant: 7 (6) | – | |
| Other: 6 (6) | – | |
| PBC: 5 (5) | – | |
| Alcoholic liver disease: 4 (4) | – | |
| NRH: 4 (4) | – | |
| Hepatitis B: 3 (3) | – | |
| # of Etiologies/Subject | 1: 87 (80) | – |
| 2: 17 (16) | – | |
| 3: 5 (5) | – | |
| Biopsy fibrosis stage | Stage 0: 35 (32) | – |
| Stage 1: 23 (21) | – | |
| Stage 2: 19 (17) | – | |
| Stage 3: 20 (18) | – | |
| Stage 4: 12 (11) | – |
†For continuous variables (for example, age, AST, albumin), values are medians followed by [IQR]. For categorical variables (for example, sex, hypertension, biopsy fibrosis stage), values are number of patients in each category follow by (percentage). ALT, alanine aminotransferase; AST, aspartate aminotransferase; INR, international normalized ratio; NRH, nodular regenerative hyperplasia; PBC, primary biliary cholangitis.
VCTE characteristics and diagnostic performance in staging fibrosis
All VCTE studies were successful, with at least 10 valid LSM measurements per study and a median [IQR] of 13 [5] valid measurements (Table 2). Median LSM [IQR] for the patient cohort was 10.7 [12.9] kPa, and median CAP [IQR] was 250 [120] dB/m. M probe was used to evaluate 91 (83%) patients whereas XL probe was used for 18 patients (17%). Patients assessed with XL probe had higher median BMI (34.56 [6.46] kg/m2 vs. 26.89 [6.71] kg/m2; p<0.001), CAP (315 [98] dB/m vs. 241 [117] dB/m; p=0.003), and LSM (12.05 [14.85] kPa vs. 9.8 [11.15] kPa; p=0.025) compared to patients assessed with M probe. Additionally, a higher proportion of patients who were assessed with XL probe carried a diagnosis of NAFLD (freq.=13, 72% vs. freq.=36, 40%; p=0.018). Seven (6%) patients had unreliable studies, where the IQR/median LSM was greater than 0.30 when median LSM was greater than 7.1 kPa. For these patients, 4 studies were done using M probe and 3 using XL probe. Four operators performed 80% of the VCTE scans, evaluating 35 (32%), 23 (21%), 18 (17%), and 11 (10%) patients, respectively.
Table 2. Characteristics of VCTE scans.
| VCTE characteristic | Sample size | Distribution† | Range |
|---|---|---|---|
| Probe | 109 | M: 91 (83) | – |
| XL: 18 (17) | – | ||
| # of Valid measurements/Subject | 109 | 13 [5] | 10–38 |
| Patients with unreliable VCTE studies‡ | 109 | 7 (6) | – |
| Median LSM in kPa | 109 | 10.7 [12.9] | 2.8–75 |
| IQR/Median LSM | 109 | 0.18 [0.12] | 0.03–0.93 |
| CAP in dB/m | 106 | 250 [120] | 100–400 |
| CAP IQR | 106 | 36 [25] | 0–147 |
| VCTE operator | 109 | Operator A: 35 (32) | – |
| Operator B: 23 (21) | – | ||
| Operator C: 18 (17) | – | ||
| Operator D: 11 (10) | – | ||
| Ten others: 22 (20) | – | ||
| VCTE F-score | 97 | F0: 13 (13) | – |
| F1: 13 (13) | – | ||
| F2: 15 (15) | – | ||
| F3: 21 (22) | – | ||
| F4: 35 (36) | – |
†For continuous variables (for example, LSM, CAP), median values are reported followed by IQR in square brackets. For categorical variables (for example probe, operator, F-score), number of patients in each category followed by percentage of total in parentheses are reported. ‡Defined as studies with IQR/median LSM greater than 0.30 when median LSM is greater than 7.1 kPa. CAP, controlled attenuation parameter; IQR, interquartile range; VCTE, vibration-controlled transient elastography.
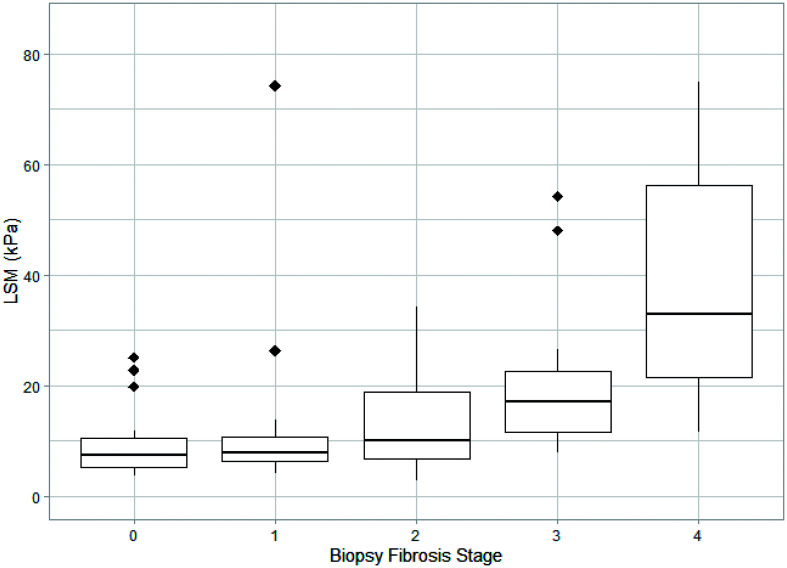
All liver biopsies were interpretable, and each had an assigned histological fibrosis stage either in the initial report (freq.=71, 65%) or on a second review (freq.=38, 35%). Thirty-five (32%) patients had no fibrosis on biopsy, twenty-three (21%) stage 1, nineteen (17%) stage 2, twenty (18%) stage 3, and twelve (11%) stage 4 (cirrhosis). Figure 2 outlines the distribution of LSM values for patients with each histological fibrosis stage. VCTE LSM and fibrosis stage on biopsy were moderately correlated with Kendall coefficient of τ=0.449 (p<0.001). Compared across all fibrosis stages, LSM values were significantly different for most pairs (Kruskal-Wallis p<0.001; Dunn’s post-hoc test, p<0.01) except for those only one stage apart: stage 0 and stage 1 (Dunn’s, p=0.571), stage 1 and stage 2 (p=0.225), stage 2 and stage 3 (p=0.053), and stage 3 and stage 4 (p=0.158), as well as between stage 0 and stage 2 (p=0.079). The median interval between VCTE and liver biopsy was 47 [89] days.
Fig. 2. LSM distribution by each liver biopsy fibrosis stage represented by boxplot.
The ends of each box visualize first and third quartile of LSM, whereas the solid line in the middle represents median LSM. Diamonds illustrate outlier LSM values for each fibrosis stage. LSM, liver stiffness measurement.
Using Youden’s index, which maximizes both sensitivity and specificity, we calculated LSM cut-off values that would best differentiate stage 0 (no fibrosis) vs. stage 1–4 (any fibrosis), stage 0–1 (no to minimal fibrosis) vs. stage 2–4 (moderate to advanced fibrosis and cirrhosis), stage 0–2 (no to moderate fibrosis) vs. stage 3–4 (advanced fibrosis and cirrhosis), and stage 0–3 (not cirrhosis) vs. stage 4 (cirrhosis) as determined via liver biopsy. We then assessed the diagnostic performance of these LSM cut-offs in differentiating dichotomized fibrosis stages (Table 3). For stage 0–3 vs. stage 4, LSM cut-off was 20.45, which had a corresponding AUROC (95% CI) of 0.90 (0.83–0.98), sensitivity of 0.83 for detecting stage 4 fibrosis and specificity of 0.85 for detecting stage 0–3 fibrosis. For stage 0–1 vs. stage 2–4, LSM cut-off was 12.3 with a lower AUROC (95% CI) of 0.80 (0.72–0.89), sensitivity of 0.67 and specificity of 0.88. For Stage 0 vs stage 1–4, LSM cut-off was 11.95 and it had the lowest AUROC (95% CI) of 0.74 (0.64–0.83) with sensitivity of 0.53 and specificity of 0.91. LSM cut-offs were also calculated for dichotomized fibrosis stages when sensitivity or specificity was set at 0.90. In both cases, as well as when using Youden’s index cut-off, PPV decreased by around 0.50 from stage 0 vs. stage 1–4 to stage 0–3 vs. stage 4. NPV increased by around 0.40 from stage 0 vs. stage 1–4 to stage 0–3 vs. stage 4. Therefore, regardless of the LSM cut-off selected, PPV was highest when LSM was used to identify any liver fibrosis (stage 1–4) and NPV was highest when LSM was used to rule out cirrhosis.
Table 3. Diagnostic performance of LSM for each histopathological fibrosis stage as determined by biopsy interpretation.
| Patient group | Liver biopsy fibrosis stages | AUROC (95% confidence interval) | LSM cut-off, kPa | Sensitivity | Specificity | PPV | NPV |
|---|---|---|---|---|---|---|---|
| All patients, Youden’s index (n=109) | Stage 0 vs. 1–4 | 0.74 (0.64–0.83) | 11.95 | 0.53 | 0.91 | 0.93 | 0.48 |
| Stage 0–1 vs. 2–4 | 0.80 (0.72–0.89) | 12.3 | 0.67 | 0.88 | 0.83 | 0.75 | |
| Stage 0–2 vs. 3–4 | 0.87 (0.80–0.93) | 10.75 | 0.94 | 0.69 | 0.56 | 0.96 | |
| Stage 0–3 vs. 4 | 0.90 (0.83–0.98) | 20.45 | 0.83 | 0.85 | 0.40 | 0.98 | |
| All patients, sensitivity=0.90 (n=109) | Stage 0 vs. 1–4 | 5.55 | 0.90 | 0.34 | 0.74 | 0.62 | |
| Stage 0–1 vs. 2–4 | 6.85 | 0.90 | 0.47 | 0.60 | 0.84 | ||
| Stage 0–2 vs. 3–4 | 11.05 | 0.90 | 0.72 | 0.57 | 0.95 | ||
| Stage 0–3 vs. 4 | 13.25 | 0.90 | 0.71 | 0.28 | 0.98 | ||
| All patients, specificity=0.90 (n=109) | Stage 0 vs. 1–4 | 11.95 | 0.53 | 0.90 | 0.92 | 0.47 | |
| Stage 0–1 vs. 2–4 | 14.05 | 0.64 | 0.90 | 0.85 | 0.74 | ||
| Stage 0–2 vs. 3–4 | 23.35 | 0.41 | 0.90 | 0.63 | 0.78 | ||
| Stage 0–3 vs. 4 | 25.40 | 0.67 | 0.90 | 0.45 | 0.96 |
AUROC, area under the receiver operating characteristics; LSM, liver stiffness measurement; NPV, negative predictive value; PPV, positive predictive value.
We performed sensitivity analyses to assess diagnostic performance using reliable VCTEs only (freq.=102), VCTEs in patients with NAFLD only (freq.=49), and VCTEs in non-NAFLD patients only (freq.=60) (Supplemental Table 1). The AUROCs of these sub-cohorts were similar when compared to the AUROCs of the complete cohort. We also compared the diagnostic performance of VCTE in the entire cohort to that of the aspartate aminotransferase to platelet ratio index and fibrosis-4 index and found no significant difference between the three methods (Supplemental Table 2).
Among 109 patients, fibrosis stage as determined by VCTE was recorded for 97. Correlations of fibrosis stages by VCTE and on biopsy were τ=0.426 (p<0.001) for all patients, τ=0.38 (p=0.004) for NAFLD patients only, and τ=0.461 (p<0.001) for non-NAFLD patients (Table 4). Therefore, a moderate correlation was found for the entire cohort as well as subpopulations. Compared to histological fibrosis stage determined by liver biopsy interpretation, VCTE fibrosis stage was at least two stages greater in 31 (32%) patients. In several instances, there were disparities of 3–4 stages. Overall, cirrhosis (stage 4) was diagnosed by VCTE in 35 cases. However, for 13 (37%) of these cases, histological fibrosis stage was between none and moderate (stage 0–2), while for 12 (34%) it was advanced (stage 3). Among 20 patients with NAFLD considered to have cirrhosis by VCTE, 7 (35%) had between none and moderate fibrosis, while 8 (40%) had advanced fibrosis on liver biopsy. On the flip side, histological fibrosis was at least 2 stages greater than determined by VCTE in only three (3%) patients.
Table 4. Correlation between VCTE fibrosis stage and biopsy fibrosis stage.
| Patient group | Sample size | Fibrosis stages | Kendall’s tau |
|---|---|---|---|
| All patients | 97 | All stages | 0.426 (p<0.001) |
| Stage 0–1 vs. 2–4 | 0.32 (p=0.002) | ||
| Stage 0–3 vs. 4 | 0.408 (p<0.001) | ||
| NAFLD only | 41 | All stages | 0.38 (p=0.004) |
| Stage 0–1 vs. 2–4 | 0.309 (p=0.053) | ||
| Stage 0–3 vs. 4 | 0.382 (p=0.017) | ||
| Non-NAFLD only | 56 | All stages | 0.461 (p<0.001) |
| Stage 0–1 vs. 2–4 | 0.31 (p=0.022) | ||
| Stage 0–3 vs. 4 | 0.442 (p=0.001) |
NAFLD, nonalcoholic fatty liver disease; VCTE, vibration-controlled transient elastography.
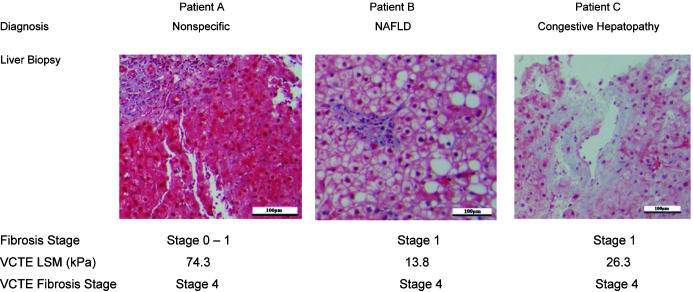
Representative cases clearly show no to minimal histological fibrosis when the VCTE diagnosis was cirrhosis (Fig. 3). Liver biopsy interpretation for patient A did not provide a specific diagnosis and showed stage 0–1 fibrosis, whereas the VCTE LSM was 74.3 kPa, which corresponded to stage 4 fibrosis. Patient B with a diagnosis of NAFLD had stage 1 histological fibrosis on biopsy and stage 4 fibrosis by VCTE (LSM=13.8 kPa). Patient C had congestive hepatopathy with stage 1 fibrosis on biopsy and stage 4 fibrosis by VCTE (LSM=26.3 kPa).
Fig. 3. Representative cases in which fibrosis stage determined by VCTE LSM significantly overstated histopathological fibrosis on liver biopsy.
Representative photomicrographs are liver sections stained with Masson’s trichrome. LSM, liver stiffness measurement; NAFLD, nonalcoholic fatty liver disease; VCTE, vibration-controlled transient elastography.
Regression models for LSM
We fit univariate linear regression models to examine the associations of various clinical, histological, and demographic variables with Box-Cox transformed LSM (λ=−0.33). Normal biopsy (β=0.104, p=0.006) and higher platelet count (β=3.48×10−4, p=0.002) were significantly associated with lower LSM (higher Box-Cox transformed LSM), whereas autoimmune hepatitis diagnosis (β=−0.080, p=0.028), use of VCTE XL probe (β=−0.061, p=0.024), increased CAP (β=−3.13×10−4, p=0.015), higher histological fibrosis stage (β=−0.045, p<0.001), and increased total bilirubin (β=−0.040, p=0.026) were associated with higher LSM (lower Box-Cox transformed LSM). No other variables, including other etiologies of CLD, were significant on univariate analysis. On multivariate linear regression analysis where independent variables were selected via backwards selection using Bayesian Information Criterion, only histological fibrosis stage on biopsy (β=−0.044, p<0.001) and CAP (β=−2.93×10−4, p=0.005) were retained in the final model (Table 5). At a CAP of 100 dB/m, predicted median LSMs (95% mean prediction CI) for liver biopsies with stage 0, stage 1, stage 2, stage 3, and stage 4 fibrosis were 4.36 (3.52–5.49), 5.45 (4.46–6.75), 6.94 (5.69–8.57), 9.02 (7.27–11.38), and 12.02 (9.28–15.96). At a CAP of 300 dB/m, predicted median LSMs for liver biopsies with stage 0, stage 1, stage 2, stage 3 and stage 4 fibrosis were 5.89 (4.92–7.15), 7.55 (6.53–8.81), 9.90 (8.77–11.23), 13.32 (11.69–15.26), and 18.52 (15.35–22.62). Therefore, greater VCTE CAP values led to higher LSM irrespective of underlying fibrosis stage.
Table 5. Prediction of LSM and its mean prediction confidence interval based on linear regression model with cap and biopsy fibrosis stage as independent variable.
| CAP in dB/m | Fibrosis stage on biopsy | LSM in kPa | CI of mean prediction |
|---|---|---|---|
| 100 | Stage 0 | 4.36 | 3.52–5.49 |
| Stage 1 | 5.45 | 4.46–6.75 | |
| Stage 2 | 6.94 | 5.69–8.57 | |
| Stage 3 | 9.02 | 7.27–11.38 | |
| Stage 4 | 12.02 | 9.28–15.96 | |
| 200 | Stage 0 | 5.05 | 4.24–6.07 |
| Stage 1 | 6.39 | 5.54–7.42 | |
| Stage 2 | 8.24 | 7.3–9.35 | |
| Stage 3 | 10.89 | 9.54–12.5 | |
| Stage 4 | 14.81 | 12.31–18.03 | |
| 300 | Stage 0 | 5.89 | 4.92–7.15 |
| Stage 1 | 7.55 | 6.53–8.81 | |
| Stage 2 | 9.90 | 8.77–11.23 | |
| Stage 3 | 13.32 | 11.69–15.26 | |
| Stage 4 | 18.52 | 15.35–22.62 | |
| 400 | Stage 0 | 6.94 | 5.44–9.05 |
| Stage 1 | 9.02 | 7.19–11.52 | |
| Stage 2 | 12.03 | 9.63–15.29 | |
| Stage 3 | 16.53 | 12.96–21.54 | |
| Stage 4 | 23.59 | 17.5–32.86 |
CAP, controlled attenuation parameter; CI, confidence interval; LSM, liver stiffness measurement.
Discussion
Since the Food and Drug Administration approved VCTE in 2013, many hepatology practices in the USA have adopted it as a screening tool to assess liver fibrosis. However, published reports on VCTE use in uncontrolled, routine clinical settings in the USA have been lacking. We conducted this retrospective study that described one academic medical center’s experience with VCTE during the first 2 years after its adoption and examined its diagnostic utility in staging fibrosis.
Current guidelines recommend the use of VCTE as a noninvasive screening modality for liver fibrosis in patients with NAFLD, alcoholic liver disease, chronic hepatitis C, and chronic hepatitis B.4,8–10 This is consistent with our finding where the majority of our VCTE studies were conducted in patients with these etiologies. While there is currently no robust evidence supporting the use of VCTE in other CLD etiologies, clinicians in our study ordered or performed it in patients with congestive hepatopathy (14%), autoimmune hepatitis (8%), liver allograft rejection (6%), and even those with nonspecific diagnostic workups (9%), or apparently normal livers (7%). In these cases, caution must be exercised when interpreting LSM and deriving fibrosis stage from it, as the applicability of VCTE in these etiologies has not been established. For example, in congestive hepatopathy, case reports have shown VCTE to be unreliable in assessing liver fibrosis, and experiments in pigs have shown a direct relationship between central venous pressure and LSM.31,32 Nonetheless, our data showed that in clinical practice at an academic medical center with experienced hepatologists, VCTE is being used to attempt to assess fibrosis in patients with liver diseases for which it is not indicated. Furthermore, many patients do not obtain a definitive diagnosis until after VCTE is performed and often the initial presumptive diagnosis is inaccurate. Therefore, staging information provided by VCTE may be incorrect as well, since LSM cut-offs for each fibrosis stage vary by CLD etiology.
Nonetheless, the diagnostic performance of VCTE LSM in differentiating dichotomized fibrosis stages was reasonably strong in this heterogenous cohort where patients had different and, at times, multiple CLD diagnoses. This is evidenced by AUROCs of 0.74, 0.80, 0.87, 0.9 for stage 0 vs. 1–4, stage 0–1 vs. 2–4, stage 0–2 vs. 3–4, and stage 0–3 vs. 4 respectively. There was also a moderate correlation of τ=0.426 between two distinct sets of fibrosis stages determined by VCTE and liver biopsy.
Current guidelines also recommend VCTE as a tool for ruling out cirrhosis in patients with certain CLD etiologies.4,8,9 This position is supported by our data showing that regardless of method used to derive LSM cut-off for stage 0–3 vs. stage 4 fibrosis (Youden’s index, sensitivity=0.90, specificity=0.90), NPV remained above 0.96. Additionally, it suggests that the use of VCTE in non-recommended etiologies did not compromise NPV. On the other hand, PPV for identifying cirrhosis remained poor. It was 0.28 when using a LSM threshold of 13.25 kPa (sensitivity=0.90), and only a modest improvement to 0.45 if the LSM threshold was nearly doubled to 25.40 kPa (specificity=0.90) with minimal decrease in NPV. This finding is supported by other single CLD etiology studies.11,18–20 A substantial number of patients in our study received LSM values that corresponded to stage 3 or 4 fibrosis but had liver biopsies that showed no or minimal fibrosis. In fact, VCTE LSM overstated fibrosis stage by at least two stages for 32% of patients in our cohort. Most concerningly, among cases where VTCE provided a diagnosis of cirrhosis, 71% did not have this histological diagnosis and 37% had no to moderate fibrosis on biopsy.
The diagnosis of cirrhosis is associated with a significantly increased healthcare burden, including more frequent physician visits, periodic imaging and blood tests for hepatocellular carcinoma surveillance, and endoscopy to screen for esophageal varices. It can also be psychologically stressful for a misdiagnosed patient. Therefore, a high VCTE LSM should not be considered definitive and only interpreted in the context of patient’s overall clinical picture. One possible strategy to reduce the false positivity rate involves utilizing a simultaneous or stepwise combination of VCTE LSM and another blood biomarker, such as the aspartate aminotransferase to platelet ratio index, fibrosis-4 index or age-platelet index, which has been shown to increase diagnostic accuracy and PPV in identifying advanced fibrosis.33,34 Alternatively, the Baveno VI consensus recommended conducting two separate VCTE measurements on different days to minimize false positive results.35 This guidance is supported by two studies in patients with NAFLD that showed an increase in PPV when VCTE was repeated, and only patients with high LSM values for both studies were considered to have advanced fibrosis or cirrhosis.36,37 Regardless of these non-invasive strategies, liver biopsy remains the gold standard for staging fibrosis and may be necessary in many cases. Furthermore, in some CLDs, only liver biopsy interpretation can provide an etiological diagnosis, particularly for nonalcoholic steatohepatitis.
On multivariate linear regression analysis, we found that after controlling for the severity of liver fibrosis on biopsy, CAP, which is a value measured by VCTE to assess hepatic steatosis, remained significantly associated with LSM. This is consistent with findings from a study of patients with NAFLD that showed greater mean LSM for higher CAP tertile in patients with stage 0–2 fibrosis.38 CAP positively influenced LSM in our cohort where patients had a wide range of CLD etiologies, not only NAFLD. Future single-etiology cohort studies are necessary to confirm the influence of CAP on LSM in other CLD diagnoses. Since hepatic steatosis influences VCTE CAP,16 CAP’s association with LSM suggests that patients with high liver fat content may have greater LSMs without advanced liver fibrosis. This may serve as a potential explanation for the phenomenon where fibrosis stage derived from VCTE LSM overstates histological fibrosis.
Our study has several limitations. First, the cohort contained patients with different and, at times, multiple etiologies of CLD, and thus the calculated LSM cut-offs may not be applicable to any single etiology. Some patients had nonspecific diagnoses and even apparently no histopathological evidence of liver disease. However, our aim was to report real-life experience with VCTE in routine clinical practice, which necessitated the inclusion of all patients, regardless of underlying etiology or clinical condition. Indeed, our data show that experienced clinical hepatologists order VCTE for indications for which its use has not been robustly validated, and without following guidelines or product specifications. Second, we did not convert liver biopsy fibrosis determined from three distinct staging systems into one common system. However, the differences in the definitions of each fibrosis stage (0–4) among the staging systems are minor, mainly influenced by location of fibrosis within the hepatic lobule and subtle differences in the number of bridging septa. Furthermore, in all these systems, bridging fibrosis is stage 3, and the presence of completely formed cirrhotic nodules is classified as stage 4. Additionally, results from this study are from the patient population of a tertiary care academic medical center with a liver transplantation program, which may not translate to patients in community practices. Finally, liver biopsies may vary in sample size and quality, which we did not account for and may introduce variability to a patient’s histological fibrosis stage.6 However, biopsy sampling variation is random, which combined with fluctuations in VCTE LSM measurements should decrease the chance and impact of any errors. Despite potential variability in liver biopsies,39–41 it remains the gold standard for assessing fibrosis.5 We also did not evaluate other emerging non-invasive diagnostics, such as two-dimensional shear wave and magnetic resonance elastography that may eventually become more available for the routine assessment of liver fibrosis.42,43
In summary, in routine clinical practice at a USA academic medical center, VCTE is highly reliable for ruling out cirrhosis. However, due to its low PPV, extreme caution must be exercised when used as the sole methodology to identify cirrhosis. This could lead to unnecessary health care interventions and psychological stress from a misdiagnosis.
Supporting information
Diagnostic performance of LSM for dichotomized fibrosis stage as determined by liver biopsy for patients with reliable VCTE scans, NAFLD patients, and non-NAFLD patients.
Diagnostic performance (AUROCs) of LSM obtained by VCTE, APRI, and Fibrosis-4 index in assessing liver fibrosis.
Acknowledgments
We thank Dr. Christopher Packey and Dr. Eugenia Uche-Anya for assistance in initial data collection, Jimmy Duong for assistance with statistical analysis, and the Scholarly Projects Program at Columbia University Vagelos College of Physicians and Surgeons for administrative support.
Abbreviations
- AUROC
area under the receiver operating characteristics
- BMI
body mass index
- CAP
controlled attenuation parameter
- CI
confidence interval
- CLD
chronic liver disease
- IQR
interquartile range
- LSM
liver stiffness measurement
- NAFLD
nonalcoholic fatty liver disease
- NPV
negative predictive value
- PPV
positive predictive value
- VCTE
vibration-controlled transient elastography
Data sharing statement
Deidentified data are available upon request.
References
- 1.Heron M. Deaths: leading causes for 2017. Natl Vital Stat Rep. 2019;68(6):1–77. [PubMed] [Google Scholar]
- 2.Bataller R, Brenner DA. Liver fibrosis. J Clin Invest. 2005;115(2):209–218. doi: 10.1172/JCI24282. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Poordad FF. Presentation and complications associated with cirrhosis of the liver. Curr Med Res Opin. 2015;31(5):925–937. doi: 10.1185/03007995.2015.1021905. [DOI] [PubMed] [Google Scholar]
- 4.Singh S, Muir AJ, Dieterich DT, Falck-Ytter YT. American Gastroenterological Association Institute technical review on the role of elastography in chronic liver diseases. Gastroenterology. 2017;152(6):1544–1577. doi: 10.1053/j.gastro.2017.03.016l. [DOI] [PubMed] [Google Scholar]
- 5.Khalifa A, Rockey DC. The utility of liver biopsy in 2020. Curr Opin Gastroenterol. 2020;36(3):184–191. doi: 10.1097/MOG.0000000000000621. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Tapper EB, Lok ASF. Use of liver imaging and biopsy in clinical practice. N Engl J Med. 2017;377(8):756–768. doi: 10.1056/NEJMra1610570. [DOI] [PubMed] [Google Scholar]
- 7.Agbim U, Asrani SK. Non-invasive assessment of liver fibrosis and prognosis: an update on serum and elastography markers. Expert Rev Gastroenterol Hepatol. 2019;13(4):361–374. doi: 10.1080/17474124.2019.1579641. [DOI] [PubMed] [Google Scholar]
- 8.European Association for Study of Liver; Asociacion Latinoamericana para el Estudio del Higado EASL-ALEH clinical practice guidelines: non-invasive tests for evaluation of liver disease severity and prognosis. J Hepatol. 2015;63(1):237–264. doi: 10.1016/j.jhep.2015.04.006. [DOI] [PubMed] [Google Scholar]
- 9.Ferraioli G, Wong VW, Castera L, Berzigotti A, Sporea I, Dietrich CF, et al. Liver ultrasound elastography: an update to the World Federation for Ultrasound in Medicine and Biology guidelines and recommendations. Ultrasound Med Biol. 2018;44(12):2419–2440. doi: 10.1016/j.ultrasmedbio.2018.07.008. [DOI] [PubMed] [Google Scholar]
- 10.Chalasani N, Younossi Z, Lavine JE, Charlton M, Cusi K, Rinella M, et al. The diagnosis and management of nonalcoholic fatty liver disease: practice guidance from the American Association for the Study of Liver Diseases. Hepatology. 2018;67(1):328–357. doi: 10.1002/hep.29367. [DOI] [PubMed] [Google Scholar]
- 11.Eddowes PJ, Sasso M, Allison M, Tsochatzis E, Anstee QM, Sheridan D, et al. Accuracy of FibroScan controlled attenuation parameter and liver stiffness measurement in assessing steatosis and fibrosis in patients with nonalcoholic fatty liver disease. Gastroenterology. 2019;156(6):1717–1730. doi: 10.1053/j.gastro.2019.01.042. [DOI] [PubMed] [Google Scholar]
- 12.Anstee QM, Lawitz EJ, Alkhouri N, Wong VW, Romero-Gomez M, Okanoue T, et al. Noninvasive tests accurately identify advanced fibrosis due to NASH: baseline data from the STELLAR trials. Hepatology. 2019;70(5):1521–1530. doi: 10.1002/hep.30842. [DOI] [PubMed] [Google Scholar]
- 13.Vuppalanchi R, Siddiqui MS, Van Natta ML, Hallinan E, Brandman D, Kowdley K, et al. Performance characteristics of vibration-controlled transient elastography for evaluation of nonalcoholic fatty liver disease. Hepatology. 2018;67(1):134–144. doi: 10.1002/hep.29489. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Patel K, Sebastiani G. Limitations of non-invasive tests for assessment of liver fibrosis. JHEP Rep. 2020;2(2):100067. doi: 10.1016/j.jhepr.2020.100067. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Wong VW, Irles M, Wong GL, Shili S, Chan AW, Merrouche W, et al. Unified interpretation of liver stiffness measurement by M and XL probes in non-alcoholic fatty liver disease. Gut. 2019;68(11):2057–2064. doi: 10.1136/gutjnl-2018-317334. [DOI] [PubMed] [Google Scholar]
- 16.Tapper EB, Castera L, Afdhal NH. FibroScan (vibration-controlled transient elastography): where does it stand in the United States practice. Clin Gastroenterol Hepatol. 2015;13(1):27–36. doi: 10.1016/j.cgh.2014.04.039. [DOI] [PubMed] [Google Scholar]
- 17.Hous JL. Clinical application of transient elastography in the diagnosis of liver fibrosis: an expert panel review and opinion. J Clin Transl Hepatol. 2014;2(2):110–116. doi: 10.14218/JCTH.2014.00008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Afdhal NH, Bacon BR, Patel K, Lawitz EJ, Gordon SC, Nelson DR, et al. Accuracy of fibroscan, compared with histology, in analysis of liver fibrosis in patients with hepatitis B or C: a United States multicenter study. Clin Gastroenterol Hepatol. 2015;13(4):772–779. doi: 10.1016/j.cgh.2014.12.014. [DOI] [PubMed] [Google Scholar]
- 19.Siddiqui MS, Idowu MO, Stromberg K, Sima A, Lee E, Patel S, et al. Diagnostic performance of vibration-controlled transient elastography in liver transplant recipients. Clin Gastroenterol Hepatol. 2021;19(2):367–374. doi: 10.1016/j.cgh.2020.03.067. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Siddiqui MS, Vuppalanchi R, Van Natta ML, Hallinan E, Kowdley KV, Abdelmalek M, et al. Vibration-controlled transient elastography to assess fibrosis and steatosis in patients with nonalcoholic fatty liver disease. Clin Gastroenterol Hepatol. 2019;17(1):156–163. doi: 10.1016/j.cgh.2018.04.043. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Thein HH, Yi Q, Dore GJ, Krahn MD. Estimation of stage-specific fibrosis progression rates in chronic hepatitis C virus infection: a meta-analysis and meta-regression. Hepatology. 2008;48(2):418–431. doi: 10.1002/hep.22375. [DOI] [PubMed] [Google Scholar]
- 22.Roskilly A, Hicks A, Taylor EJ, Jones R, Parker R, Rowe IA. Fibrosis progression rate in a systematic review of placebo-treated nonalcoholic steatohepatitis. Liver Int. 2021;41(5):982–995. doi: 10.1111/liv.14749. [DOI] [PubMed] [Google Scholar]
- 23.Myers RP, Cerini R, Sayegh R, Moreau R, Degott C, Lebrec D, et al. Cardiac hepatopathy: clinical, hemodynamic, and histologic characteristics and correlations. Hepatology. 2003;37(2):393–400. doi: 10.1053/jhep.2003.50062. [DOI] [PubMed] [Google Scholar]
- 24. U.S. Department of Health and Human Services and U.S. Department of Agriculture. 2015 – 2020 dietary guidelines for Americans. 8th edition. December 2015. Available from: https://health.gov/our-work/food-nutrition/previous-dietary-guidelines/2015.
- 25.Wai CT, Greenson JK, Fontana RJ, Kalbfleisch JD, Marrero JA, Conjeevaram HS, et al. A simple noninvasive index can predict both significant fibrosis and cirrhosis in patients with chronic hepatitis C. Hepatology. 2003;38(2):518–526. doi: 10.1053/jhep.2003.50346. [DOI] [PubMed] [Google Scholar]
- 26.Sterling RK, Lissen E, Clumeck N, Sola R, Correa MC, Montaner J, et al. Development of a simple noninvasive index to predict significant fibrosis in patients with HIV/HCV coinfection. Hepatology. 2006;43(6):1317–1325. doi: 10.1002/hep.21178. [DOI] [PubMed] [Google Scholar]
- 27.Farr M, Mitchell J, Lippel M, Kato TS, Jin Z, Ippolito P, et al. Combination of liver biopsy with MELD-XI scores for post-transplant outcome prediction in patients with advanced heart failure and suspected liver dysfunction. J Heart Lung Transplant. 2015;34(7):873–882. doi: 10.1016/j.healun.2014.12.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Kleiner DE, Brunt EM, Van Natta M, Behling C, Contos MJ, Cummings OW, et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology. 2005;41(6):1313–1321. doi: 10.1002/hep.20701. [DOI] [PubMed] [Google Scholar]
- 29.Batts KP, Ludwig J. Chronic hepatitis. An update on terminology and reporting. Am J Surg Pathol. 1995;19(12):1409–1417. doi: 10.1097/00000478-199512000-00007. [DOI] [PubMed] [Google Scholar]
- 30.Boursier J, Zarski JP, de Ledinghen V, Rousselet MC, Sturm N, Lebail B, et al. Determination of reliability criteria for liver stiffness evaluation by transient elastography. Hepatology. 2013;57(3):1182–1191. doi: 10.1002/hep.25993. [DOI] [PubMed] [Google Scholar]
- 31.Millonig G, Friedrich S, Adolf S, Fonouni H, Golriz M, Mehrabi A, et al. Liver stiffness is directly influenced by central venous pressure. J Hepatol. 2010;52(2):206–210. doi: 10.1016/j.jhep.2009.11.018. [DOI] [PubMed] [Google Scholar]
- 32.Park Y, Kim SU, Koh MJ, Lee S. Compensated heart failure does not always alleviate overestimation of liver stiffness by transient elastography. Eur J Gastroenterol Hepatol. 2013;25(3):385–387. doi: 10.1097/MEG.0b013e32835b9bc9. [DOI] [PubMed] [Google Scholar]
- 33.Liang XE, Zhong C, Huang L, Yang S, Zhu Y, Chen Y, et al. Optimization of hepatitis B cirrhosis detection by stepwise application of transient elastography and routine biomarkers. J Gastroenterol Hepatol. 2017;32(2):459–465. doi: 10.1111/jgh.13475. [DOI] [PubMed] [Google Scholar]
- 34.Petta S, Vanni E, Bugianesi E, Di Marco V, Camma C, Cabibi D, et al. The combination of liver stiffness measurement and NAFLD fibrosis score improves the noninvasive diagnostic accuracy for severe liver fibrosis in patients with nonalcoholic fatty liver disease. Liver Int. 2015;35(5):1566–1573. doi: 10.1111/liv.12584. [DOI] [PubMed] [Google Scholar]
- 35.de Franchis R, Baveno VIF. Expanding consensus in portal hypertension: report of the Baveno VI Consensus Workshop: stratifying risk and individualizing care for portal hypertension. J Hepatol. 2015;63(3):743–752. doi: 10.1016/j.jhep.2015.05.022. [DOI] [PubMed] [Google Scholar]
- 36.Chow JC, Wong GL, Chan AW, Shu SS, Chan CK, Leung JK, et al. Repeating measurements by transient elastography in non-alcoholic fatty liver disease patients with high liver stiffness. J Gastroenterol Hepatol. 2019;34(1):241–248. doi: 10.1111/jgh.14311. [DOI] [PubMed] [Google Scholar]
- 37.Chuah KH, Lai LL, Vethakkan SR, Nik Mustapha NR, Mahadeva S, Chan WK. Liver stiffness measurement in non-alcoholic fatty liver disease: two is better than one. J Gastroenterol Hepatol. 2020;35(8):1404–1411. doi: 10.1111/jgh.14978. [DOI] [PubMed] [Google Scholar]
- 38.Petta S, Wong VW, Camma C, Hiriart JB, Wong GL, Marra F, et al. Improved noninvasive prediction of liver fibrosis by liver stiffness measurement in patients with nonalcoholic fatty liver disease accounting for controlled attenuation parameter values. Hepatology. 2017;65(4):1145–1155. doi: 10.1002/hep.28843. [DOI] [PubMed] [Google Scholar]
- 39.Regev A, Berho M, Jeffers LJ, Milikowski C, Molina EG, Pyrsopoulos NT, et al. Sampling error and intraobserver variation in liver biopsy in patients with chronic HCV infection. Am J Gastroenterol. 2002;97(10):2614–2618. doi: 10.1111/j.1572-0241.2002.06038.x. [DOI] [PubMed] [Google Scholar]
- 40.Dhall D, Kim SA, Mc Phaul C, Kransdorf EP, Kobashigawa JA, Sundaram V, et al. Heterogeneity of fibrosis in liver biopsies of patients with heart failure undergoing heart transplant evaluation. Am J Surg Pathol. 2018;42(12):1617–1624. doi: 10.1097/PAS.0000000000001163. [DOI] [PubMed] [Google Scholar]
- 41.Ratziu V, Charlotte F, Heurtier A, Gombert S, Giral P, Bruckert E, et al. Sampling variability of liver biopsy in nonalcoholic fatty liver disease. Gastroenterology. 2005;128(7):1898–1906. doi: 10.1053/j.gastro.2005.03.084. [DOI] [PubMed] [Google Scholar]
- 42.Furlan A, Tublin ME, Yu L, Chopra KB, Lippello A, Behari J. Comparison of 2D shear wave elastography, transient elastography, and MR Elastography for the diagnosis of fibrosis in patients with nonalcoholic fatty liver disease. AJR Am J Roentgenol. 2020;214(1):W20–W26. doi: 10.2214/AJR.19.21267. [DOI] [PubMed] [Google Scholar]
- 43.Dong BT, Chen YP, Lyu GR, Wang HM, Lin GF, Gu JH. Diagnostic accuracy of two-dimensional shear wave elastography and magnetic resonance elastography for staging liver fibrosis in patients with chronic hepatitis B: a systematic review and meta-analysis. J Gastroenterol Hepatol. 2021 doi: 10.1111/jgh.15549. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Diagnostic performance of LSM for dichotomized fibrosis stage as determined by liver biopsy for patients with reliable VCTE scans, NAFLD patients, and non-NAFLD patients.
Diagnostic performance (AUROCs) of LSM obtained by VCTE, APRI, and Fibrosis-4 index in assessing liver fibrosis.