Abstract
Clostridium septicum bacteremia is a rare (72 cases reported) aneurysm-inducing disease that has resulted in a 6-month mortality of 100% when treated conservatively. We report the case of a patient who was completely symptom free at 6 months of follow-up but who ultimately died at 8.9 months after aortic rupture. In compliance with the patient’s choice, a long-time antibiotic regimen was applied, instead of the surgical approach recommended by our surgical department. The use of an antibiotic regimen represents an option for patients unfit for surgery or as a bridge to surgery for damage control; however, aortic repair represents the only curative approach. Definitive antibiotic treatment is limited to a palliative approach for patients with C. septicum aortitis and has been accompanied by 100% 1-year mortality (90-day mortality, 84.2%).
Keywords: Abdominal aneurysm, Aortitis, Case report, Clostridium septicum, Occult colonic malignancy
Representing 1.3% of clostridial infections, Clostridium septicum is a gram-positive anaerobic bacillus.1,2 Additionally, C. septicum aortitis is associated with occult gastrointestinal malignancies (≤80%; 56% of colorectal cancer) and hematologic disorders.1,2 Alpha toxin production can lead to gas gangrene building up in the aortic wall and, ultimately, systemic invasion through the bowel mucosa, resulting in fast aneurysm induction accompanied by a high risk of rupture.2, 3, 4 However, few cases have been reported (n = 72). When open aortic repair (OAR) is not performed, C. septicum aortitis will result in a 100% 6-month mortality rate.2 Rupture of the abdominal aorta (77%-94% mortality for outpatients compared with 51.9% in-hospital mortality) is in contrast to a 90-day mortality of ∼30% after OAR.2,5,6
In the present study, we have reported the case of a patient with this rare disease surviving >6 months (8.9 months) after conservative treatment. The patient provided written informed consent for the report of her case details and imaging studies. Our report followed the CARE guidelines (Supplementary Fig).7
Supplementary Fig.
CARE checklist of information to include when writing a case report.
Case report
A 76-year-old woman with permanent atrial fibrillation, dilated cardiomyopathy, arterial hypertension, chronic obstructive pulmonary disease, and chronic kidney disease had presented with diffuse abdominal pain, fatigue, and a mild fever. Her white blood cell count (15,070 K/μL; normal range, 4-10.8 K/μL) and C-reactive protein (20.5 mg/dL; normal range, <0.5 mg/dL) were elevated, and contrast-enhanced computed tomography (CT) revealed a slight dilatation of the juxtarenal and infrarenal aorta with circumferential intramural gas present. Thus, empiric intravenous antibiotic treatment was applied (ampicillin/sulbactam, 1 g intravenously every 8 hours), and the patient was hospitalized. She experienced a fast decrease in symptom severity and decline of the inflammatory parameters. However, a blood culture was positive for a gram-positive bacillus that was later identified as C. septicum. A literature review revealed a dramatic prognosis for patients for whom aortic surgery was not performed. Furthermore, reevaluating the CT scan revealed a colonic mass with a diameter of 3 cm at the right flexure that was later histologically confirmed as a high-grade intraepithelial neoplasm by colonoscopy. Nevertheless, the interdisciplinary evaluation (preoperative internist statement and geriatric assessment [ie, Barthel index and Mini-Mental State Examination]) estimated the patient to be frail and at increased risk of open abdominal surgery, although echocardiography had revealed good cardiac pump function (ejection fraction, 55%). However, the interdisciplinary vascular board, including vascular surgeons and interventional radiologists, decided against endovascular aortic aneurysm repair (EVAR) accompanied by long-term antibiotic treatment because of the presence of advanced aortic calcification, stenotic visceral arteries, and the juxtarenal anatomic site of the aneurysm with placement of an endovascular stent difficult (Fig 1). OAR would also have been risky owing to the general condition of the patient and insecure suture possibility because of the advanced inflammation state of the arterial wall. Ultimately, it was the patient’s and her family’s utmost will to try a conservative approach, rejecting the offered intervention possibilities (EVAR and OAR, which were preferred by our vascular board). Thus, long-term broad-spectrum antibiotic treatment with penicillin (amoxicillin/clavulanic acid), 1 g every 12 hours, was administered. The patient recovered quickly and was discharged with an absolute absence of symptoms. Readmission with follow-up CT after 3 months (Fig 2) showed progressive aneurysmatic growth (+12 mm) of the juxtarenal aorta, with a wide penetrating ulcer and dissection of the outermost vessel layers into the calcified aortic wall, with a craniocaudal expansion of 5 cm.
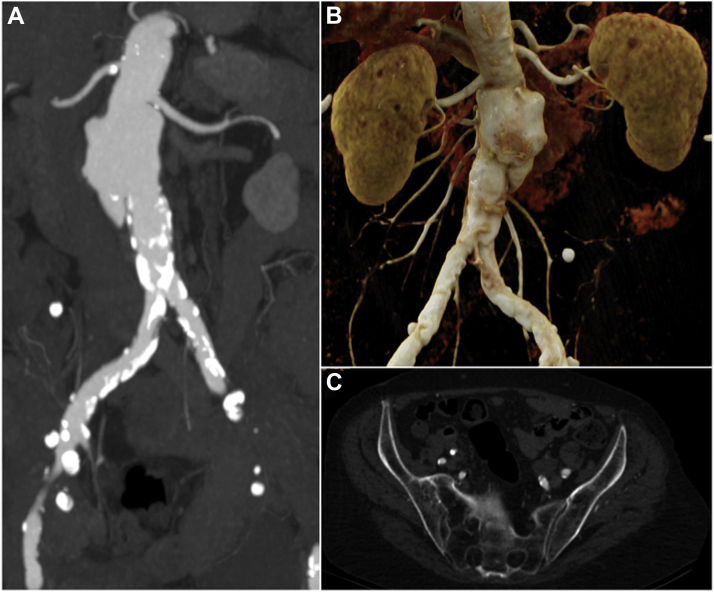
Fig 1.
Anatomic characteristics influencing treatment decisions. Maximum intensity projection (A) and cinematic volume rendering technique (B) images of the juxtarenal aneurysm in correlation with the renal arteries. C, Note the highly calcified and stenotic iliac vessels, with the largest diameter of the right and left external iliac artery being 5 mm and 6 mm, respectively.
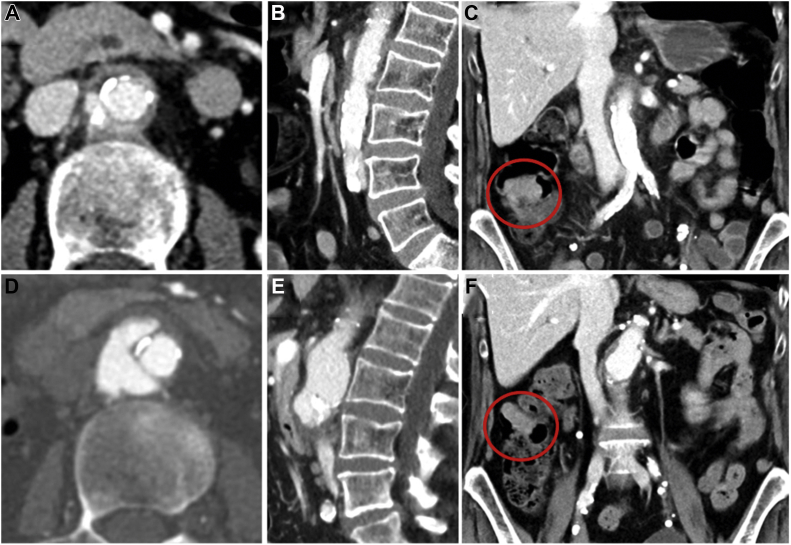
Fig 2.
Computed tomography (CT) scans at diagnosis (A-C) and at 3 months of follow-up (D-F). After 3 months of antibiotic treatment, progressive aneurysmatic growth (+12 mm) of the juxtarenal aorta was found with a wide penetrating ulcer and dissection of the outermost vessel layers at a craniocaudal expansion of 5 cm. The tumorous structure in the right colon is highlighted with red circles(C and F).
The inflammatory parameters were within the normal range, and the patient had not had any symptoms at 3 months of follow-up. The interdisciplinary and ethical board evaluation rejected an attempt of aortic repair at this stage and agreed to further antibiotic treatment in consensus with the patient and her close family, aware of the imminently fatal end due to rupture. Thus, no further diagnostic or interventional treatment was administered because such treatment was rejected by the patient. The patient did not undergo curative intended colorectal surgery, and the colonic mass was left untouched. However, the patient was in satisfactory condition at the 6-month follow-up and, ultimately, died of rupture after 8.9 months (266 days).
Discussion
Our literature search in August 2021 revealed a total of 72 cases of C. septicum–associated aortitis.1, 2, 3, 4, 5, 6, 7, 8, 9, 10, 11, 12, 13, 14, 15, 16, 17, 18, 19, 20, 21, 22, 23 Thus, the case we have presented is case number 73. Demographically, we found a predisposition for male sex (66.2%), older age (median, 76 years; interquartile range, 67-82 years), gastrointestinal malignancies (52.1%), and diabetes (22.5%). The abdominal aorta was involved in 64.8% of the cases, and 8.5% had thoracoabdominal expansion.
Antibiotic treatment as the only conservative approach was administered to 23 patients compared with 39 patients who had undergone OAR, 5 patients who had undergone EVAR, and 5 patients whose further treatment was not specified.14,18,20, 21, 22, 23 However, to date, the 6-month mortality was 100% for patients receiving conservative treatment (90-day mortality, 84.2%), in contrast to 43.2% for patients undergoing surgery (90-day mortality, 32.1%).2,13,16,17,19,21 Regarding OAR, long-term survival (>1 year) was reached for 25% to 50% of patients.2,13,16,17,19,21
Despite the dramatic benefit of surgical repair, long-term broad-spectrum antibiotic treatment can be offered as a palliative approach or to the rare patient with critical status who are believed will not survive extensive open abdominal surgery and might be not suitable for an endovascular approach (eg, anatomic situation) at admission as a bridge-to-surgery concept to improve the patient’s general status. In addition, for some patients, the feasibility of sufficient vessel anastomosis might be eased by prior antibiotic treatment by minimizing the acute aortic wall inflammation.
Regarding the technical feasibility, our case has revealed several pitfalls in the suitability of a potential curative approach. OAR was considered to have a high probability of resulting in perioperative death because of the patient’s general and cardiac condition, which was considered not sufficiently robust enough for aortic repair, with the need for infradiaphragmal clamping and a high risk of insecure suturing owing to the vulnerable inflammatory aortic wall for proximal anastomosis. However, OAR would have been the treatment of choice for our patient and, therefore, was offered, acknowledging the increased perioperative risk. However, any interventional approach was rejected by the patient. Anatomically, the process was located in the juxtarenal aorta, with expansion from the left renal artery to the inferior mesenteric artery, making sufficient infrarenal clamping difficult and causing longer ischemic times of the viscera, especially the kidney.
Given this anatomic situation (Fig 1), the potential for EVAR as a salvage regimen would have required a fourfold fenestrated stent, with the need for an additional surgical conduit to access the pelvic area because of the calcified stenosing pelvic axis of both and the chronic dissection membrane of the left common iliac artery. Alternatively, an endobronchial prosthesis with a thoracic proximal landing area could have been used. Nevertheless, EVAR carries a high risk of stent graft infection, making this technique a rather experimental approach for C. septicum aortitis. To date, long-term survival (>1 year) after EVAR was achieved for two patients.14,18 Future studies are needed to address the use of EVAR as definitive treatment or a bridge to definitive open surgery for C. septicum aortitis because no sufficient long-term data are available on this topic.
Conclusions
OAR should be offered to all patients with C. septicum aortitis fit for surgery after a careful interdisciplinary evaluation. EVAR might be a treatment option for selected patients, although only a few data are available to support this treatment approach for patients with C. septicum aortitis. However, it should be the decision of the patient and, if appropriate, the patient’s family, with consideration of the potential perioperative morbidity and mortality (90-day mortality, 30%) of high-risk OAR against the possibility of long-term survival (25%-50%). However, severe suffering from symptoms is not expected until death results from aortic rupture, which, to date, has occurred in all patients receiving conservative treatment only within the first year.
Footnotes
Author conflict of interest: none.
The editors and reviewers of this article have no relevant financial relationships to disclose per the Journal policy that requires reviewers to decline review of any manuscript for which they may have a conflict of interest.
Appendix
References
- 1.Alpern R.J., Dowell V.R. Clostridium septicum infections and malignancy. JAMA. 1969;209:385–388. [PubMed] [Google Scholar]
- 2.Lehman B., Miller R.M., Richter S.S., Keller G., Tan C., Rodriguez E.R., et al. Clostridium septicum-infected aortic aneurysm or graft is a deadly diagnosis. J Vasc Surg. 2020;71:1781–1788. doi: 10.1016/j.jvs.2019.09.029. [DOI] [PubMed] [Google Scholar]
- 3.Kennedy C.L., Krejany E.O., Young L.F., O'Connor J.R., Awad M.M., Boyd R.L., et al. The alpha-toxin of Clostridium septicum is essential for virulence. Mol Microbiol. 2005;57:1357–1366. doi: 10.1111/j.1365-2958.2005.04774.x. [DOI] [PubMed] [Google Scholar]
- 4.Srivastava I., Aldape M.J., Bryant A.E., Stevens D.L. Spontaneous C. septicum gas gangrene: a literature review. Anaerobe. 2017;48:165–171. doi: 10.1016/j.anaerobe.2017.07.008. [DOI] [PubMed] [Google Scholar]
- 5.Bengtsson H., Bergqvist D. Ruptured abdominal aortic aneurysm: a population-based study. J Vasc Surg. 1993;18:74–80. doi: 10.1067/mva.1993.42107. [DOI] [PubMed] [Google Scholar]
- 6.Durieux R., Lardinois M.J., Albert A., Defraigne J.O., Sakalihasan N. Outcomes and predictors of mortality in a Belgian population of patients admitted with ruptured abdominal aortic aneurysm and treated by open repair in the contemporary era. Ann Vasc Surg. 2022;78:197–208. doi: 10.1016/j.avsg.2021.05.015. [DOI] [PubMed] [Google Scholar]
- 7.Gagnier J.J., Kienie G., Altman D.G., Moher D., Sox H., Riley D. The CARE guidelines: consensus-based clinical case report guideline development. J Clin Epidemiol. 2014;67:46–51. doi: 10.1016/j.jclinepi.2013.08.003. [DOI] [PubMed] [Google Scholar]
- 8.Upchurch G.R., Clair D.G., Whittemore A.D., Mannick J.A. Clostridium septicum bacteremia associated with aortic graft infection. J Vasc Surg. 1995;22:493–495. doi: 10.1016/s0741-5214(95)70019-6. [DOI] [PubMed] [Google Scholar]
- 9.Sailors D.M., Eidt J.F., Cagne P.J., Barnes R.W., Barone G.W., McFarland D.R. Primary Clostridium septicum aortitis: a rare cause of necrotizing suprarenal aortic infection. A case report and review of the literature. J Vasc Surg. 1996;23:714–718. doi: 10.1016/s0741-5214(96)80055-3. [DOI] [PubMed] [Google Scholar]
- 10.Monsen T., Palmgren H., Amerlöv C., Billheden J. Aortic dissection due to Clostridium septicum infection. Eur J Vasc Endovasc Surg. 1997;13:517–518. doi: 10.1016/s1078-5884(97)80183-9. [DOI] [PubMed] [Google Scholar]
- 11.Zenati M.A., Bonanomi G., Kastov D., Lee R. Images in cardiovascular medicine: fulminant Clostridium septicum aortitis. Circulation. 2002;105:1871. doi: 10.1161/01.cir.0000016163.45584.a1. [DOI] [PubMed] [Google Scholar]
- 12.Takano H., Taniguchi K., Kuki S., Nakamura T., Miyagawa S., Masai T. Mycotic aneurysm of the infrarenal abdominal aorta infected by Clostridium septicum: a case report of surgical management and review of the literature. J Vasc Surg. 2003;38:847–851. doi: 10.1016/s0741-5214(03)00612-8. [DOI] [PubMed] [Google Scholar]
- 13.Seder C.W., Kramer M., Long G., Uzieblo M.R., Shanley C.J., Bove P. Clostridium septicum aortitis: report of two cases and review of the literature. J Vasc Surg. 2009;49:1304–1309. doi: 10.1016/j.jvs.2008.11.058. [DOI] [PubMed] [Google Scholar]
- 14.Sha S., Whitehead D., Sampath K., Toor A. A case of Clostridium septicum aortitis with concomitant adenocarcinoma of the cecum. ACG Case Rep J. 2015;2:230–232. doi: 10.14309/crj.2015.68. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Shahi N., Arosemena M., Kwon J., DiMuzio P., Abai B., Salvatore D.M. A rare case of Clostridium septicum aortitis with colon adenocarcinoma. J Vasc Surg Cases Innov Tech. 2018;4:87–90. doi: 10.1016/j.jvscit.2017.12.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Ramphal W., Raaijmakers N., van der Klift M., Wijsman J.H., Kluytmans J., Veen E.J. Mycotic aneurysm caused by Clostridium septicum in a patient with colorectal cancer. Infection. 2018;46:711–716. doi: 10.1007/s15010-018-1155-z. [DOI] [PubMed] [Google Scholar]
- 17.Curtis-Martinez C., Sanchez-Guillen L. Emphysematous aortitis by Clostridium septicum: a rare and lethal complication of right colon cancer. Eur J Vasc Endovasc Surg. 2019;57:509. doi: 10.1016/j.ejvs.2018.12.022. [DOI] [PubMed] [Google Scholar]
- 18.Cresser S., Maddock L., Smart P. Clostridium septicum: a usual suspect? Aortic rupture following right hemicolectomy: a case report. Int J Surg Case Rep. 2019;54:51–54. doi: 10.1016/j.ijscr.2018.10.083. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Urgiles S., Matos-Casano H., Win K.Z., Berardo J., Bhatt U., Shah J. Emphysematous aortitis due to Clostridium septicum in an 89-year-old female with ileus. Case Rep Infect Dis. 2019;2019:1–4. doi: 10.1155/2019/1094837. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Akita K., Takami Y., Matsuhashi K., Sakurai Y., Amano K., Ishikawa H., et al. Clostridium septicum-infected Stanford type A acute aortic dissection: a case report. Surg Case Rep. 2020;6:PMC6965561. doi: 10.1186/s40792-020-0770-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Jerrari R., Jayet J. Mycotic aneurysm rupture due to Clostridium septicum thoracic aortitis. Eur J Vasc Endovasc Surg. 2021;61:421. doi: 10.1016/j.ejvs.2020.10.014. [DOI] [PubMed] [Google Scholar]
- 22.Hashimoto T., Okamatsu Y., Hyakuna Y., Sedutsu Y., Miyata K., Origuchi H., et al. Perianeurysmal emphysema: Clostridium septicum-infected aortic aneurysm. Circulation. 2014;129:1900–1901. doi: 10.1161/CIRCULATIONAHA.114.009337. [DOI] [PubMed] [Google Scholar]
- 23.Lintin L., Wheeler R., Whiston R., Gordon A., Berry D., Torkington J. Mycotic thoracic aortic arch aneurysm from haematogenous spread of Clostridium septicum due to metastatic colorectal cancer: a survival guide. J Surg Case Rep. 2014;2014:rju117. doi: 10.1093/jscr/rju117. [DOI] [PMC free article] [PubMed] [Google Scholar]