Abstract
Objectives
Predicting the outcome of trauma helps clinician to prioritize patients and provide timely and effective treatment. Several scoring systems are implemented to predict prognosis and mortality among these patients. Our study aims to use four scoring systems to predict mortality among multiple trauma patients.
Methods
In retrospective descriptive study, the data was collected from records of (XXX) of multiple trauma patients referred to the hospital from June 2019–January 2020. The patients were scored using four scoring systems: MGAP (mechanism, Glasgow coma scale, age, and arterial pressure), GAP (Glasgow coma scale, age, and arterial pressure), ISS (injury severity score) and RTS (revised trauma score).
Results
The mean age of the patients was 37.4 ± 4.2 years and of 112 patients, 92 patients (82.1%) were males. Sensitivity of GAP, RTS and ISS was 100% in predicting mortality where MGAP had highest specificity, 97.2%. All four scoring systems significantly predicted mortality, p < 0.001, respectively and the highest area under the curve was for RTS criteria, 0.969.
Conclusion
MGAP, GAP, RTS and ISS were all effective in predicting mortality among multiple trauma patients whereas MGAP had both, highest sensitivity and specificity. Scoring trauma for mortality can be achieved by using any of the systems, provided the information required for score can be obtained.
Keywords: Trauma, MGAP, GAP, RTS, ISS, Mortality
Abbreviations: TS, Trauma Score; ISS, Injury Severity Scale; YLL, year of life lost; SBP, systolic blood pressure; RTS, Revised Trauma Score; RR, rate of respiration; GAP, Glasgow coma scale, age, and arterial pressure
Highlights
-
•
Predicting the outcome of trauma helps clinician to prioritize patients and provide timely and effective treatment.
-
•
Several scoring systems are implemented to predict prognosis and mortality among these patients.
-
•
MGAP, GAP, RTS and ISS were all effective in predicting mortality among multiple trauma patients.
-
•
Scoring trauma for mortality can be achieved by using any of the systems.
-
•
We recommend further studies including other modern scoring system and larger sample size.
1. Introduction
Trauma is one of the four leading causes of death in developing countries and the second leading cause of death of young people in the country and the leading cause of year of life lost (YLL) [1]. Trauma is any type of wound, penetrating or non-penetrating injury, which is intentionally or unintentionally caused by external factors in the body. Trauma is a time-sensitive condition, especially during the first hours after trauma, management, examination, resuscitation, and care are very important and, if done well, can play a significant role in reducing mortality [2,3]. Studies have shown that 25–50% of deaths due to trauma are preventable. The mortality rate is the most accurate outcome to measure the prognosis of trauma. This death index can be presented in two forms: short-term (24 h) and long-term (4 weeks later). An easy scoring system for trauma patients can help the physician to judge as quickly and accurately as possible the severity of the injury and how to manage the patient [4].
The MGAP (mechanism, Glasgow coma scale, age and arterial pressure) standard is a scoring system for trauma patients that provides physicians with useful information in determining prognosis [5]. MGAP was modified to GAP (Glasgow coma scale, age and arterial pressure) for easy implementation in clinical settings by Kondo et al. [6]. In 1981, Champion et al. introduced a triage measure called the Trauma Score (TS), in which the author hypothesized that the most common cause of premature death due to secondary trauma was damage to one of the three systems: central nervous system, cardiovascular system, and respiratory systems. Thus, the TS criterion includes five variables: GCS, rate of respiration (RR), respiratory expansion, systolic blood pressure (SBP) and capillary refill [1]. In 1989, criterion called the Revised Trauma Score (RTS) was introduced, which is a modified form of the TS criterion. The RTS criterion included three variables: GCS, SBP and RR [7]. In 1974, Baker and colleagues at Johns Hopkins University developed the first scoring system based on anatomical injury to the body. The Injury Severity Scale (ISS) is mostly used for research purposes in determining the severity of injury in a trauma patient and is not a triage criterion. Before defining the ISS system, it was difficult for surgeons to predict the effectiveness of treating a traumatized person [8].
Studies have been performed to evaluate the accuracy of these criteria in determining prognosis and mortality in these patients [9,10]. However, definite conclusion regarding which scores should be used for evaluating multiple trauma patients remains a question. Number of studies have favored the use of new criteria (GAP and MGAP) for scoring whereas some studies have reported no significant difference in the performance of these system [11]. This study aims to evaluate the diagnostic accuracy of GAP, MGAP, RTS and ISS criteria in predicting mortality among multiple trauma patients.
2. Methods
In retrospective descriptive study patients with multiple traumas referred to (XXX) province from June 2019 to January 2020 were enrolled. Inclusion criteria included trauma patients over 18 years of age who have penetrating and closed trauma, including road traffic accidents, fights, and falls, knives, and bullets. Patients with mild trauma such as soft tissue damage and isolated limb fractures were not included in the study. Pregnant women, patients under 18 years of age, incomplete records or failure of follow-up led to exclusion from the study too.
According to the sample volume formula for ROC analysis and considering the probability of error of the first type equal to 0.01, power 80%, area under the curve equal to 0.7, and hypothesis zero equal to 0.5, the minimum number of samples required is equal to 100.
The files of these patients were obtained from health care information system of the hospital. After approving the plan and obtaining the code of ethics from the ethics committee of (XXX) and coordination with the hospital department and the hospital medical records department, all basic information of patients referred to the emergency department with multiple trauma complaints such as demographic characteristics (age and sex), method of arrival at the hospital, mechanism of injury (closed or penetrating), accident site, anatomical site of injury, Glasgow coma score, systolic blood pressure, heart rate, respiration rate, arterial blood oxygen saturation were extracted from patients' records. Patients were then evaluated using 4 scoring systems, GAP, MGAP, RTS and ISS. Mortality was obtained 24 h a day for 4 weeks based on the electronic file and for patients who were discharged earlier than 4 weeks, the occurrence of death was followed up by telephone using the telephone number in the file.
In GAP criteria, the lowest score is 3 and the highest score is 24. The lowest score has the worst prognosis, and the highest score has the best prognosis.
In the MGAP criterion, the lowest score is 3, which has the worst prognosis, and the highest score in this criterion is 29, which has the best prognosis.
To calculate the score in the RTS criterion, each of the three items Glasgow coma score, systolic blood pressure and respiration rate are coded based on the given numbers, and finally the codes are added, and the minimum score is 0 and the maximum score is 12.
In the ISS scoring system, which is mostly a research criterion for determining the prognosis in patients with multiple traumas, according to the AIS table, the injuries are first calculated based on the anatomical area and then entered into the ISS system. The lowest score is 0 and has the best prognosis and the highest score is 75, which has the most damage to the person and the lowest prognosis.
Descriptive statistics and graphs were used to describe the collected information according to the type of variable. To examine the relationship between GAP, MGAP, RTS and ISS and multiple trauma by modulating the effect of independent variables, the logistic regression model was used.
The patients were not directly involved in the study and identification of an individual patient was not used in the study. The hospital records was accessed from the data upon approval.
This study was approved by the Research Ethics Board of (XXX).
Unique identifying number is: researchregistry7615.
The methods are stated in accordance with STROCSS 2021 guidelines [12].
3. Results
94 patients (83.9%) were in the age range of 18–60 years and the other 18 patients (16.1%) were aged over 60 years. 92 patients (82.1%) were males, and 20 patients (17.9%) were females. 106 trauma patients were transported to Shahid Beheshti Hospital by EMS from the scene of the accident, and only 6 patients were referred to the emergency department by personal vehicle. 93.8% patients were presented with blunt trauma whereas 6.3% patients had penetrating trauma.
The most common reasons of trauma were inside and outside vehicle (28.6%), respectively followed by motorcycle accident (27.7%). The reported sites of injury were head and neck (30.4%), limbs (18.8%), abdomen (15.2%) and face (14.2%).
In the evaluation of vital signs, the mean pulse rate was 87.6 ± 11.6. The mean systolic blood pressure was 115.6 ± 15.6 mmHg and mean rate of respiration was 16.3 ± 2.2. The mean oxygen saturation was 95.9 ± 4.2 and mean Glasgow coma score 13.7 ± 2.7.
The GAP criterion, which includes Glasgow coma score, age and systolic blood pressure, the mean score was 20.7 ± 3.2, (range: 7–24). In the MGAP criterion, which includes the mechanism of trauma (blunt or penetrating), Glasgow coma score, age and systolic blood pressure, the mean was 25.3 ± 3.2 (range: 10–29). In RTS criteria that includes Glasgow coma score, systolic blood pressure and respiration rate, the mean was 7.7 ± 0.8 (range: 3–8). In the ISS criterion, the mean was 11.1 ± 9.6 (range: 3–75).
Based of GAP criteria, 3 patients were categorized into severe trauma group, of which only 1 person in the MGAP and RTS criteria was in the severe category and the other two were in the moderate group. 2 of these patients in ISS group was categorized in severe trauma group and one was categorized in mild trauma category. 14 patients were moderately traumatized based of GAP and RTS category where 11 of these were categorized in moderate trauma category as per MGAP criteria and 3 were in the mild category. Out of 14 people, according to the ISS, 4 people were in the severe category, 2 people were in the moderate category and 8 people were in the mild category. 95 of the patients in the study were mildly traumatized as per GAP criteria where 5 of these were categorized moderately traumatized based on MGAP and RTS, and 90 had mild trauma. According to the ISS, 75 people were in mild trauma group, 15 people were moderate in and 5 people were in the severe category.
Within 24 h of the patients entering the emergency department, 89 people were admitted to the hospital wards and monitored, 22 people were admitted to the ICU due to deteriorating physical condition and 1 patient was discharged taking into account the condition and normalcy of all tests, graphs and examinations. No deaths occurred within 24 h of hospitalization.
After one month, the mean age of 108 living patients was 37.45 years and the mean age of the deceased was 38.50 years, which was not statistically significant. Among the survivors, there were 88 males and 20 females, while all those who died were male, but there was no significant correlation between the gender and survival. The mean Glasgow coma score in survivors was 13.95 but the mean score in deceased0 was 5.75, which was significantly different, p < 0.001.
The systolic blood pressure, pulse rate and respiration rate were not significantly different among survivors and deceased. The mean percentage of oxygen saturation in the survivors was 96.0% but in the deceased was 90.75, which was significantly different, p = 0.013(Table 1, Table 2).
Table 1.
Demographic characteristics and clinical baseline of living patients vs. deceased after one month.
| Characteristics (Mean) |
Alive patients |
Dead patients |
p-value |
|
|---|---|---|---|---|
| Age | 37.4 | 38.50 | NS | |
| Gender | Male | 88 | 4 | NS |
| Female | 20 | 0 | ||
| GCS | 13.95 | 5.75 | S | |
| Systolic blood pressure | 115.78 | 112.50 | NS | |
| Pulse | 87.37 | 93.00 | NS | |
| Respiratory rate | 16.34 | 16.00 | NS | |
| SpO2 | 96.0 | 90.75 | S | |
Table 2.
Trauma triage score at presentation in living patients and deceased after one month.
| Criteria(mean) | Alive patients | Dead patients | p-value |
|---|---|---|---|
| GAP | 20.99 | 12.50 | <0.000 |
| MGAP | 25.62 | 17.50 | |
| RTS | 7.76 | 4.75 | |
| ISS | 10.06 | 38.75 |
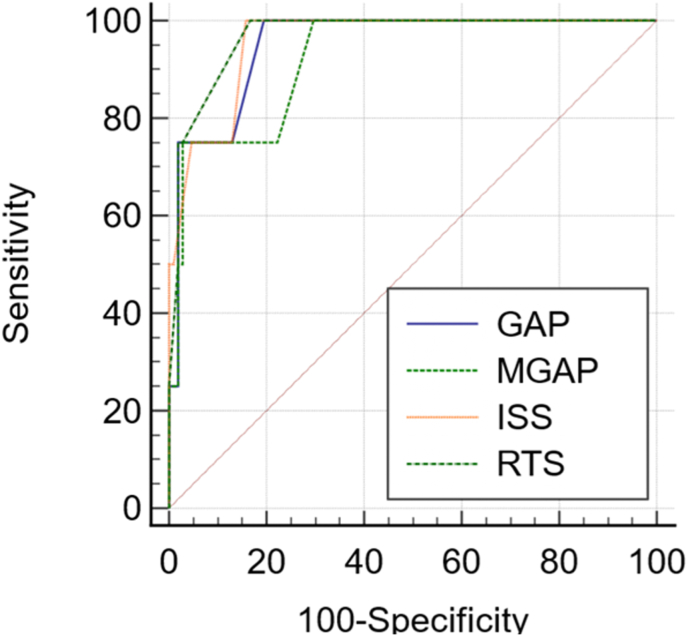
In predicting the mortality, GAP score had 100% sensitivity and 80.56% specificity. The score was significantly different among survivors and deceased, p < 0.001. MGAP had 75% sensitivity and 97.2% specificity in predicting mortality and the score was significantly different among survivors and deceased, p < 0.001. Similarly, sensitivity of RTS and ISS was 100% and their specificity was 83.33% and 84.26% respectively. Both the scores were significantly different among survivor and deceased patients, p < 0.001, respectively. The highest area under the curve was for RTS criteria, 0.969 (Table 3, Fig. 1).
Table 3.
Predicted mortality at one month from trauma criteria at presentation according to ROC chart.
| Criteria | Sensivity | Specify | AUC | p-value |
|---|---|---|---|---|
| GAP | 100.00 | 80.56 | 0.950 | 0.0001> |
| MGAP | 75.00 | 97.22 | 0.924 | 0.0001> |
| RTS | 100.00 | 83.33 | 0.969 | 0.0001> |
| ISS | 100.00 | 84.26 | 0.957 | 0.0001> |
Fig. 1.
Comparison of the predictive power of mortality of trauma criteria during a month according to the ROC chart.
4. Discussion
Trauma scoring systems are commonly used to determine the prognosis in the early stages of trauma and severity. The findings of our study showed that all four systems performed well in predicting the outcome of trauma patients, such that the three criteria, GAP, RTS and ISS were 100% sensitive in predicting one-month mortality and the MGAP criterion had the highest specificity (97.22%) in predicting death due to trauma. Comparing the area under the ROC curve between the criteria, the RTS (including Glasgow coma score, systolic blood pressure and respiration rate) performed slightly better than the other criteria, AUC = 0.996, while in the study by Erhan Ahun et al. [13] MGAP (Glasgow coma score age and systolic blood pressure) in multiple trauma patients, performed better than the RTS score while there was no difference between GAP and MGAP. A study by Hung et al. [14] comparing various trauma severity score reported that GAP and MGAP had the highest AUC whereas RTS and estimated ISS had the least, respectively. ISS is dependent of imaging modalities and associated anatomical information, which adds challenge to is usage and gives low performance [14]. A study conducted in the United States on 18,746 patients showed that GAP score had the highest power to predict mortality and Kampala trauma score (KTS), MGAP and GAP are feasible for calculating mortality in hospitals with fewer resources. Despite, RTS and ISS scores also significantly predicted in-hospital mortality, ISS requires anatomical details and cannot differentiate between severe injuries and poor care. TRISS (trauma injury severity score) and KTS had the greatest AUC in this study, respectively [15,16]. Our study does not include KTS and TRISS system which limits the implementation of our findings.
Based on the correlation between the variables of these trauma scoring systems, the results of the present study showed that most of the victims were under 60 years of the age (83.9%), indicating significance of age in multiple trauma patients, which is the component of both, GAP and MGAP scoring systems. Wui et al. showed that rate of trauma is high in men and young people, since young men engage in high-risk activities and greater frequency of male drivers in their region [17]. Decrease in oxygen saturation and consciousness were negatively associated with the incidence of mortality in our study population. Increase in the levels of consciousness was significantly associated with the decrease in mortality rate. The present study was in line with the study conducted by Amrit Saika et al. [18]. In a study conducted by Arhan Ahon et al. to determine the predictive power of GAP in extensive trauma patients, one of the two patients categorized as high risk by MGAP was categorized as moderate risk by GAP, two patients categorized as low risk by MGAP were categorized as moderate risk by GAP, and 5 patients categorized as moderate by GAP, were categorized as low risk by MGAP as [13]. In this study, similar to other studies, the highest frequency of patients was in the low-risk, moderate and high-risk groups, respectively [8,13,19].
Our study is a single-center retrospective study with small sample size, which limits the findings of the study. Furthermore, a number of biochemical factors and history of previous diseases might affect patient prognosis, which could not be evaluated in our study, due to its retrospective nature.
5. Conclusion
The choice of scoring system is likely to be based on available data and resources and preference of the performers. The results of our study showed that all 4 scoring systems significantly predicted mortality whereas, RTS system had greatest area under the curve. We recommend further studies including other modern scoring system and larger sample size.
Provenance and peer review
Not commissioned, externally peer-reviewed.
Registration of research studies
Name of the registry: This study was approved by the Research Ethics Board of Qom University of Medical Sciences.
-
1.
Unique Identifying number or registration ID: IR.MUQ.REC.1400.075
-
2.
Hyperlink to the registration (must be publicly accessible):N/A
Guarantor
Dr. Nina Farzan.
Ethical approval and consent to participate
All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Consent to participate
From the under 16 years old was given by a parent or legal guardian.
Consent for publication
Not applicable.
Availability of data and material
Data sharing is not applicable to this article as no datasets were generated or analyzed during the current study.
Funding source
No funding was secured for this study.
Contributors’ statement page
Dr. Nina Farzan: conceptualized and designed the study, drafted the initial manuscript, and reviewed and revised the manuscript. Dr. Seyed Yaser Foroghi Ghomi: Designed the data collection instruments, collected data, carried out the initial analyses, and reviewed and revised the manuscript. Dr. Atefeh Raeisi Mohammadi: Coordinated and supervised data collection, and critically reviewed the manuscript for important intellectual content.
Declaration of competing interest
The authors deny any conflict of interest in any terms or by any means during the study.
Footnotes
This study was approved by the Research Ethics Board of Qom University of Medical Sciences (IR.MUQ.REC.1400.075). https://ethics.research.ac.ir/ProposalCertificateEn.php?id=211214&Print=true&NoPrintHeader=true&NoPrintFooter=true&NoPrintPageBorder=true&LetterPrint=true.
Supplementary data to this article can be found online at https://doi.org/10.1016/j.amsu.2022.103536.
Appendix A. Supplementary data
The following is the Supplementary data to this article:
References
- 1.Champion H.R., Sacco W.J., Carnazzo A.J., Copes W., Fouty W.J. Trauma score. Crit. Care Med. 1981;9(9):672–676. doi: 10.1097/00003246-198109000-00015. [DOI] [PubMed] [Google Scholar]
- 2.Raux M., Sartorius D., Le Manach Y., David J.-S., Riou B., Vivien B. What do prehospital trauma scores predict besides mortality? J. Trauma Acute Care Surg. 2011;71(3):754–759. doi: 10.1097/TA.0b013e3181fd0dae. [DOI] [PubMed] [Google Scholar]
- 3.Ahmadinejad M., Ahmadinejad I., Maghsoudi L.H., Soltanian A., Safari M. Complications in patients with cardiac penetrating trauma. Cardiovas. Haematol. Disorders - Drug Targetsrug Targets - Cardiovas. Hematol. Disorders) 2021;21(4):212–216. doi: 10.2174/1871529X21666211214155349. [DOI] [PubMed] [Google Scholar]
- 4.Shoko T., Shiraishi A., Kaji M., Otomo Y. Effect of pre-existing medical conditions on in-hospital mortality: analysis of 20,257 trauma patients in Japan. J. Am. Coll. Surg. 2010;211(3):338–346. doi: 10.1016/j.jamcollsurg.2010.04.010. [DOI] [PubMed] [Google Scholar]
- 5.Sartorius D., Le Manach Y., David J.-S., Rancurel E., Smail N., Thicoïpé M., et al. Mechanism, glasgow coma scale, age, and arterial pressure (MGAP): a new simple prehospital triage score to predict mortality in trauma patients. Crit. Care Med. 2010;38(3):831–837. doi: 10.1097/CCM.0b013e3181cc4a67. [DOI] [PubMed] [Google Scholar]
- 6.Kondo Y., Abe T., Kohshi K., Tokuda Y., Cook E.F., Kukita I. Revised trauma scoring system to predict in-hospital mortality in the emergency department: glasgow Coma Scale, Age, and Systolic Blood Pressure score. Crit. Care. 2011;15(4):R191. doi: 10.1186/cc10348. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Alvarez B.D., Razente D., Lacerda D.A., Lother N.S., Von-Bahten L.C., Stahlschmidt C., et al. Vol. 43. 2016. Analysis of the Revised Trauma Score (RTS) in 200 victims of different trauma mechanisms; pp. 334–340. [DOI] [PubMed] [Google Scholar]
- 8.Baker S.P., O'neill B. The injury severity score: an update. Journal of Trauma and Acute Care Surgery. 1976;16(11):882–885. doi: 10.1097/00005373-197611000-00006. [DOI] [PubMed] [Google Scholar]
- 9.Ahmadinejad M., Mohammadzadeh S., Shirzadi A., Soltanian A., Ahmadinejad I., Pouryaghobi S.M. Trauma factors among adult and geriatric blunt trauma patients. Int. J. Surg. Open. 2021;28:17–21. [Google Scholar]
- 10.Ahmadinejad M., Shirzadi A., Soltanian A., Ahmadinejad I., Sootodeh S. The impact of intercostal nerve block on the necessity of a second chest x-ray in patients with penetrating trauma: a randomised controlled trial. Int. J. Surg. Open. 2021;29:24–28. [Google Scholar]
- 11.Pande M.W.T., Benny P. Prediction of mortality rate of trauma patients in emergency room at Cipto Mangunkusumo Hospital by several scoring systems. Med. J. Indonesia. 2013;22(4) [Google Scholar]
- 12.Mathew G., Agha R., Albrecht J., Goel P., Mukherjee I., Pai P., et al. Strocss 2021: strengthening the reporting of cohort, cross-sectional and case-control studies in surgery. Ann. Med. Surg. 2021;72 doi: 10.1016/j.amsu.2021.103026. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Ahun E., Köksal Ö., Sığırlı D., Torun G., Dönmez S.S., Armağan E. Value of the Glasgow Coma Scale, age, and arterial blood pressure (GAP) score for predicting the mortality of major trauma patients presenting to the emergency department. Turkish J. Trauma Emerg. Surg. 2014;20(4):241–247. doi: 10.5505/tjtes.2014.76399. [DOI] [PubMed] [Google Scholar]
- 14.Hung Y.W., He H., Mehmood A., Botchey I., Saidi H., Hyder A.A., et al. Exploring injury severity measures and in-hospital mortality: a multi-hospital study in Kenya. Injury. 2017;48(10):2112–2118. doi: 10.1016/j.injury.2017.07.001. [DOI] [PubMed] [Google Scholar]
- 15.Rutledge R. The Injury Severity Score is unable to differentiate between poor care and severe injury. J. Trauma. 1996;40(6):944–950. doi: 10.1097/00005373-199606000-00013. [DOI] [PubMed] [Google Scholar]
- 16.Laytin A.D., Dicker R.A., Gerdin M., Roy N., Sarang B., Kumar V., et al. Comparing traditional and novel injury scoring systems in a US level-I trauma center: an opportunity for improved injury surveillance in low- and middle-income countries. J. Surg. Res. 2017;215:60–66. doi: 10.1016/j.jss.2017.03.032. [DOI] [PubMed] [Google Scholar]
- 17.Wui L.W., Shaun G.E., Ramalingam G., Wai K.M.S. Epidemiology of trauma in an acute care hospital in Singapore. J. Emergencies, Trauma, Shock. 2014;7(3):174. doi: 10.4103/0974-2700.136860. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Saika A., Bansal S., Philip M., Devi B.I., Shukla D.P. Prognostic value of FOUR and GCS scores in determining mortality in patients with traumatic brain injury. Acta Neurochir. 2015;157(8):1323–1328. doi: 10.1007/s00701-015-2469-6. [DOI] [PubMed] [Google Scholar]
- 19.Kondo Y., Abe T., Kohshi K., Tokuda Y., Cook E.F., Kukita I. Revised trauma scoring system to predict in-hospital mortality in the emergency department: glasgow Coma Scale, Age, and Systolic Blood Pressure score. Crit. Care. 2011;15(4):1–8. doi: 10.1186/cc10348. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
Data sharing is not applicable to this article as no datasets were generated or analyzed during the current study.