Abstract
Introduction
Primary chylopericardium is an extremely rare disease with no previous reported case in Indonesia. It may be caused by an abnormality of lymphatic drainage in the thoracic region.
Case presentation
We report the case of a 19-year-old female who presented with a chief complaint of shortness of breath and fluid accumulation in her pericardial sac. Screening for autoimmune disease, tuberculosis, and malignancy all came back negative. Lymphoscintigraphy showed suspected leakage or obstruction of lymph at the supradiaphragmatic level. The patient was diagnosed with primary chylopericardium. In a span of 1 year, she had undergone 3 pericardiocentesis procedures and declined surgical treatment. On her fourth pericardiocentesis, the cardiologists were unable to remove fluid from the pericardial sac. Thoracic duct ligation and pericardial window were eventually performed and a total of 850 ml of chylous fluid was removed. At 6 months postoperation patient showed no signs and symptoms of pericardial effusion and was in good condition.
Discussion
Constrictive pericarditis can occur as a complication of chronic inflammation in the pericardium due to the presence of chylopericardium and a history of multiple pericardiocenteses. However, there are no reports regarding the exact duration of chylopericardium that will lead to constrictive pericarditis. Difficulty in pericardiocentesis might be an early sign of scarring in the pericardium.
Conclusion
Delayed surgical treatment of chylopericardium increases the risk of constrictive pericarditis and significantly reduces the patient's quality of life due to recurrent symptoms and hospitalizations.
Keywords: Primary chylopericardium, Thoracic duct ligation, Pericardial window, Constrictive pericarditis
Highlights
-
•
This is the first case of isolated primary chylopericardium reported in Indonesia.
-
•
Surgery should be performed in patients with recurrent effusion.
-
•
Delayed surgical treatment increases the risk of constrictive pericarditis.
-
•
It also reduces the patient's QoL due to recurrent symptoms and hospitalizations.
1. Introduction
Chylopericardium is an accumulation of chyle in the pericardial sac surrounding the heart. It is a rare disorder that may be primary/idiopathic or secondary due to injury to the thoracic duct. Chronic accumulation of chyle in the pericardial sac can cause inflammation that eventually leads to constrictive pericarditis [1]. Treatment of chylopericardium consists of dietary modification, fluid removal, and surgery. Surgery is usually considered when the patient does not respond to conservative therapy [2]. Currently, there is no widely accepted indication for surgical treatment. Constrictive pericarditis is one of the complications of chylopericardium [1]. However, it's still not clear when chylopericardium will eventually lead to constrictive pericarditis. We aim to review the occurrence of constrictive pericarditis in primary chylopericardium. This case is reported in line with the SCARE 2020 criteria [3].
2. Presentation of case
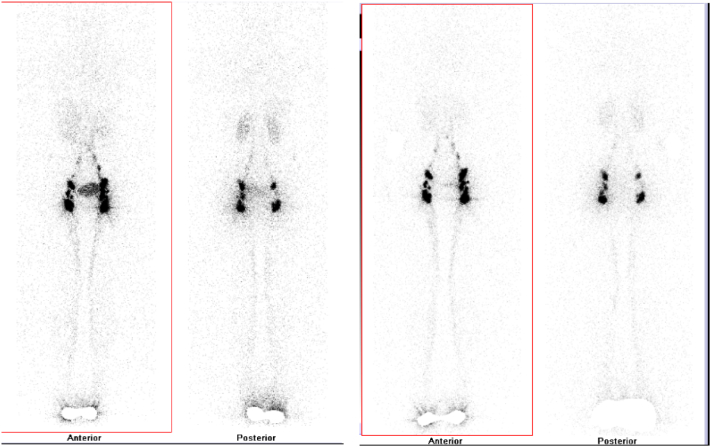
A 19-years-old female was presented to our polyclinic with a chief complaint of shortness of breath 1 year before admission. History of cough, fever, and chest pain were all denied. Her physical examinations were unremarkable. Further examination revealed an accumulation of fluid in the pericardial sac. Evaluation for autoimmune disease, tuberculosis, and malignancy all came back negative. The patient had undergone 3 pericardiocentesis procedures in the span of 1 year. Fluid with a milky white appearance was removed from the pericardial sac, a total of 1255 ml, 1180 ml, and 1000 ml at each tapping respectively. Pericardial fluid analysis revealed an increased level of triglyceride (1261 mg/dL), cholesterol (124.7 mg/dL), predominance of lymphocytes (97.2 %), and positive Sudan III staining. There were no bacteria found in the cytology and culture of the pericardial fluid. Lymphoscintigraphy showed the flow of radioactivity is stopped at the supradiaphragmatic level. There was no pathological activity in thoracic region and pericardium region. There is suspicion of lymphatic leakage or obstruction at the supradiaphragmatic level with no pericardial activity in the location of pericardial effusion (Fig. 1). The patient was diagnosed with recurrent primary chylopericardium. We highly encourage the patient to undergo surgery following recurrent accumulation of chyle in the pericardial sac however, the patient was hesitant to follow through.
Fig. 1.
Lymphoscintigraphy showed suspected leakage or obstruction of lymph at the supradiaphragmatic level.
The patient reported improved symptoms immediately following her third pericardiocentesis, but slowly worsen in the following weeks. Echocardiography showed large pericardial effusion with the collapse of the right atrium and right ventricle. On her fourth scheduled pericardial tapping, the cardiologist failed to remove fluid from the pericardial sac. It was probably due to the high viscosity of the fluid and the possibility of a septation or scarred pericardial sac due to chronic inflammation and frequent pericardial tapping. The patient finally agreed to undergo surgery. A thoracic duct ligation with a pericardial window through the right posterolateral thoracotomy was performed by experienced cardiothoracic surgeon in our hospital. A total of 850 ml of chylous fluid was drained from the pericardial sac. A 28 fr drain was put in the right hemithorax. The skin was closed using absorbable 4.0 sutures.
Following the operation, the patient was in good condition. There were no signs and symptoms of chylopericardium at 6 months follow-up postoperation.
3. Discussion
Chylopericardium is an accumulation of chyle (normal content of lacteals and thoracic duct) in the pericardial sac. Primary chylopericardium is a rare disease with only around 100 cases reported since 1954 [4]. It may be caused by obstruction of the thoracic duct, reflux of chyle that drains the pericardium and heart from normal lymphatic vessels, failure to establish collateral drainage to the right thoracic duct, and abnormal connections between the pericardial and thoracic lymphatics [5]. The characteristics of chyle are milky white in color, triglyceride level greater than 500 mg/dL, cholesterol to triglyceride ratio of less than 1, negative culture and cytology, a predominance of lymphocyte on cytologic examination, and fat globules on Sudan 111 staining [6]. All characteristics mentioned above were present in pericardial fluid analysis in our patient, establishing the diagnosis of chylopericardium. The differential diagnosis of chylopericardium includes cholesterol pericarditis and purulent pericardial effusion due to infection like tuberculosis. Fluid analysis in cholesterol pericarditis will show cholesterol crystals and a lower concentration of triglyceride. Meanwhile, pericardial effusion due to infection will show higher neutrophils than lymphocytes in cellular content, positive culture for organism, and lower triglyceride level [7]. The patient was also tested for ANA-IF to exclude pericarditis due to autoimmune disease.
Patients without cardiac tamponade can initially be treated with dietary modification while patients with cardiac tamponade require urgent fluid removal [8]. Fluid removal can be performed through pericardiocentesis or tube pericardiostomy [2]. Surgery is considered in patients with recurrent effusion or when patients do not respond to conservative therapy. There is no clear indication for surgical treatment. In general, surgery is performed in patients with hemodynamically significant effusions, recurrent effusion following pericardiocentesis, and chyle production of more than 500 ml/day over 5 day period [6], [9]. Thoracic duct ligation with pericardiotomy or pericardiectomy is the modality of choice for surgical treatment [10]. Dib et al. [6] presented a systematic review of 33 cases of chylopericardium and reported that 57.1 % of cases did not respond to conservative therapy, while surgical treatment was curative in all cases. The median duration from initiation of conservative therapy to surgical intervention was 12 days [6].
Constrictive pericarditis can occur as a complication of chronic inflammation in the pericardium due to the presence of chylopericardium and a history of multiple pericardiocenteses [1]. There are no reports regarding the duration of chylopericardium and the time of occurrence of constrictive pericarditis. Androulakis et al. [11] suggested constrictive pericarditis should actively be sought with additional imaging modalities like MRI and CT scan in patients with chylopericardium and should be considered as a differential diagnosis of chylopericardium [11]. One of a few findings suggestive of constrictive pericarditis is pericardial thickening. Echocardiography and CT scan showed there was no pericardial thickening in our patient. Chronic recurrent chylopericardium up to 1 year as reported in this case showed that constrictive pericarditis does not occur immediately. This was supported by Morishita et al. [12] who reported a case of constrictive pericarditis secondary to primary chylopericardium that was diagnosed 8 years previously. However, difficulty in performing the last pericardiocentesis in our patient raises suspicion of possible septation or scarring in the pericardium that will eventually lead to constrictive pericarditis.
4. Conclusion
We present a case of chronic recurrent primary chylopericardium treated with thoracic duct ligation and pericardial window following the failure of pericardiocentesis. Delayed surgical treatment increases the risk of constrictive pericarditis and significantly reduces the patient's quality of life due to recurrent symptoms and hospitalizations.
Consent
Written informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal on request.
Provenance and peer review
Not commissioned, externally peer-reviewed.
Ethical approval
No approval required.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Guarantor
Muhammad Arza Putra.
Research registration number
Not applicable.
CRediT authorship contribution statement
Muhammad Arza Putra performed the surgery and supervised the writing of manuscript. Stefanie Melisa and Jonathan Grantomo wrote the manuscript.
Declaration of competing interest
The authors declare there is no conflict of interest with the content of this case report.
References
- 1.Uchikawa T., Ohtani K., Muramatsu K., Sonoda H., Shiose A., Tsutsui H. Constrictive pericarditis and worsening mitral annular disjunction after long-term chylopericardium. Circ Heart Fail. 2018;11(8) doi: 10.1161/CIRCHEARTFAILURE.117.004698. [DOI] [PubMed] [Google Scholar]
- 2.Mehrotra S., Peeran N.A., Bandyopadhyay A. Idiopathic chylopericardium. Tex. Heart Inst. J. 2006;33(2):249–252. [PMC free article] [PubMed] [Google Scholar]
- 3.Agha R.A., Franchi T., Sohrabi C., et al. The SCARE 2020 guideline: updating consensus surgical CAse REport (SCARE) guidelines. Int. J. Surg. 2020;84:226–230. doi: 10.1016/j.ijsu.2020.10.034. [DOI] [PubMed] [Google Scholar]
- 4.Yu X., Jia N., Ye S., Zhou M., Liu D. Primary chylopericardium: a case report and literature review. Exp Ther Med. 2018;15(1):419–425. doi: 10.3892/etm.2017.5383. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Kawano H. Primary chylopericardium. J. Cardiol. Cases. 2012;5(3):e173–e174. doi: 10.1016/j.jccase.2012.03.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Dib C., Tajik A.J., Park S., Kheir M.E.L., Khandieria B., Mookadam F. Chylopericardium in adults: a literature review over the past decade (1996–2006) J. Thorac. Cardiovasc. Surg. 2008;136(3):650–656. doi: 10.1016/j.jtcvs.2008.03.033. [DOI] [PubMed] [Google Scholar]
- 7.Hoit B.D. 2022. Chylopericardium and cholesterol pericarditis. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Jensen G.L., Mascioli E.A., Meyer L.P., et al. Dietary modification of chyle composition in chylothorax. Gastroenterology. 1989;97(3):761–765. doi: 10.1016/0016-5085(89)90650-1. [DOI] [PubMed] [Google Scholar]
- 9.Wurnig P.N., Hollaus P.H., Ohtsuka T., Flege J.B., Wolf R.K. Thoracoscopic direct clipping of the thoracic duct for chylopericardium and chylothorax. Ann. Thorac. Surg. 2000;70(5):1662–1665. doi: 10.1016/s0003-4975(00)01921-4. [DOI] [PubMed] [Google Scholar]
- 10.Rochefort M.M. Review of chylopericardium. Mediastinum. 2022;6:3. doi: 10.21037/med-20-64. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Androulakis E., Bratis K., Chua T., Chandrasekaran V. Chylopericardium associated with constrictive pericarditis assessed by multimodality imaging. Clin Case Rep. 2021;9(6) doi: 10.1002/ccr3.4354. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Morishita Y., Taira A., Furoi A., Arima S., Tanaka H. Constrictive pericarditis secondary to primary chylopericardium. Am. Heart J. 1985;109(2):373–375. doi: 10.1016/0002-8703(85)90614-3. [DOI] [PubMed] [Google Scholar]