Abstract
Background
For decades, treatment of mood disorders, psychoses, anxiety and dementia have been confounded by limited efficacy and high rates of treatment resistance. Preclinical and clinical evidence have highlighted disruption of cholinergic signalling in several neuropsychiatric conditions and examined intervention strategies including acetylcholinesterase inhibitors and nicotinic receptor-targeted intervention. However, the effectiveness of these approaches is often curtailed by on-target side effects. Post mortem studies implicate muscarinic receptor dysregulation in neuropsychiatric pathophysiology; therefore, we conducted a systematic review and meta-analysis to investigate the therapeutic efficacy and safety of muscarinic receptor-targeted interventions in adults with neuropsychiatric disorders.
Methods
PubMed, EMBASE, PsycINFO, EBSCO and Web of Science were searched using relevant keywords from database inception to 7 August 2022. Randomised, double-blind, placebo-controlled studies were included if they investigated the effect of muscarinic receptor-targeted intervention in adults with a diagnosis of a neuropsychiatric disorder and were published in English. A narrative synthesis approach was adopted to describe the findings. Wherever three or more studies with a similar intervention were available, effect sizes were calculated, and a meta-analysis was performed. Cochrane risk-of-bias-2 tool was utilised to assess the risk of bias, and sensitivity analyses were performed to identify publication bias. Certainty analysis (high, moderate, low and/or very low) was conducted using GRADE criteria.
Results
Overall, 33 studies met the inclusion criteria and 5 were included in the meta-analysis. Despite a limited pool with several different interventions, we found therapeutic efficacy of xanomeline (M1/M4 agonist) in primary psychotic disorders plus behavioural and psychological symptoms of dementia. Scopolamine showed a significant antidepressant effect in a combined cohort of major depressive and bipolar disorders in the short-term outcome measure, but no effect following cessation of treatment. Results from bias assessments suggest “very low” certainty in the antidepressant effect of scopolamine. Critical limitations of the current literature included low power, high heterogeneity in the patient population and a lack of active comparators.
Conclusion
While the results are not definitive, findings on muscarinic receptor-targeted interventions in several mental disorders are promising in terms of efficacy and safety, specifically in treating schizophrenia, mood disorders, and behavioural and psychiatric symptoms of Alzheimer’s disease. However, orthosteric muscarinic receptor-targeted interventions are associated with a range of peripheral adverse effects that are thought to be mediated via M2/M3 receptors. The orthosteric binding site of muscarinic acetylcholine receptors is remarkably conserved, posing a challenge for subtype-selective interventions; nonetheless allosteric ligands with biased signalling pathways are now in development. We conclude that adequately powered prospective studies with subtype-selective interventions are required to determine the clinical effectiveness of muscarinic-receptor targeted interventions for the treatment of neuropsychiatric disorders.
Graphical Abstract

Key Points
| Acetylcholine imbalance is apparent across various psychiatric illnesses. |
| Xanomeline improved positive and negative symptoms of schizophrenia. |
| Scopolamine shows antidepressant effects in major depressive and bipolar disorder patients. |
Introduction
In the brain, the cholinergic system forms an intricate neural network with three segregated elements based on their localisation and projection pattern [1]; (1) long-range basal forebrain projections, critical for attention, learning, memory, decision-making [2, 3]; (2) projections from the brainstem, which modulate attention, sleep, and motor control [4]; and (3) cholinergic interneurons of the striatum, which play a crucial role in reward and motivation [4, 5]. At the cellular level, acetylcholine signalling is modulated by nicotinic (nAChR; ionotropic receptors) and muscarinic acetylcholine receptors (mAChR; G-protein coupled receptors). To date, there are five cloned mAChR subtypes (M1, M2, M3, M4, and M5). M1, M3 and M5 receptors couple primarily to Gq/11, stimulating phospholipase C and inositol phosphate, mediating an excitatory effect through intracellular calcium influx. In contrast, M2 and M4 are coupled with Gi/o, resulting in an inhibition of the downstream adenyl cyclase activation [6–8].
Due to its widespread innervation and diverse central function, the acetylcholine system has attracted attention as a target for new pharmacotherapies to treat neuropsychiatric disorders with overlapping symptomatology [9, 10]. In 2019, 1 in every 8 or 970 million people in the world suffered from a mental disorder [11]. In the USA, 18.1% (43.6 million) adults experience mental health problems annually [12]. Current clinical strategies to combat dysfunctional cholinergic signalling include acetylcholinesterase inhibitors to avoid the breakdown of Ach- and nAChR-targeted interventions. However, the clinical effectiveness of these compounds is curtailed by on-target adverse effects [13–15]. As detailed below, growing evidence suggests the apparent involvement of muscarinic receptors in certain neuropsychiatric illnesses, including major depressive disorder (MDD), bipolar disorder (BP), schizophrenia, dementia, Alzheimer’s disease (AD) and anxiety disorders [16].
Mood Disorders
The term mood disorder broadly defines all types of depression and BP. In the USA, an estimated 8.4% of adults will have at least one major depressive episode during their lifetime, with the prevalence rate higher in women (10.5%) than men (6.2%) [17]. Major depressive disorder is diagnosed when an individual has persistent feelings of sadness, anhedonia, worthlessness, lack of concentration, suicidal thoughts, appetite and sleep disturbances [18]. On the other hand, people with BP move between two states, from depression to mania. Treatment options mainly include pharmacological interventions such as antidepressants, anticonvulsants, mood stabilisers, and non-pharmacological approaches such as cognitive behavioural therapy, interpersonal psychotherapy, or a combination of these approaches [19]. Despite the accessibility of multiple treatment options, approximately 20–40% of people with MDD do not respond to the primary therapy, and the proportion of non-responders increases further for people with BP [20–22].
The involvement of the acetylcholine system in mood disorders was proposed in 1950, following a study in which psychiatric patients developed depressive-like symptoms after administration of acetylcholine esterase inhibitors [23]. Subsequently, this was assisted by studies showing that depressive symptoms were exaggerated in patients with MDD after administration of physostigmine, an acetylcholinesterase inhibitor [24, 25]. A PET study using [18F]FP-TZTP, a selective M2 ligand, found reduced receptor availability in the anterior cingulate cortex of patients with BP and MDD [26]. Similarly, haplotype analysis also suggests a possible involvement of M2 receptors in patients with depression [27]. To date, only one study measured M3 receptors and found a decrease in density in the frontal but not in the parietal and prefrontal cortex. Collectively, these data provide considerable support for region-specific differences in M2 or M3 receptors in patients with mood disorders, but no apparent regulation of M1 receptor [28, 29].
Primary Psychotic Disorders
As defined by the International Classification of Diseases 11th Revision (ICD-11), primary psychotic disorders encompass schizophrenia, schizoaffective disorder, and other psychotic disorders. The prevalence of schizophrenia and related psychotic disorders range from 0.25 to 0.64% in the USA, based on a household survey, clinical diagnostic examinations, and health records [30–32]. Schizophrenia is a potentially devastating disorder with the following symptoms: positive (psychotic) symptoms such as disorganised thoughts, hallucination, delusion; negative symptoms consisting of social withdrawal, affective flattening, alogia, anhedonia; and cognitive impairments in all domains. A vital issue with conventional antipsychotics is limited efficacy for negative symptoms and cognitive impairments, with predominant focus to date on the monoamine hypothesis [33, 34]. Even second-generation neuroleptics, including clozapine and olanzapine, produce only modest improvement in people with chronic and refractory illness [35, 36].
Initial investigation for the function of muscarinic receptors in schizophrenia was conducted using human post mortem brain tissue and radioligand binding assays. These results revealed region-specific alterations in M1 and M4 muscarinic receptors in the striatum, prefrontal cortex, hippocampus, anterior cingulate and superior temporal gyrus [37–40]. Studies employing receptor-specific antibodies, in situ hybridisation, and tomographic imaging revealed a region-specific negative correlation between muscarinic receptor availability and symptoms of schizophrenia [40, 41]. Notably, scopolamine (non-selective muscarinic receptor antagonist) induces psychotic-like symptoms, referred to as "anti-muscarinic syndrome" [42, 43]. Based on available evidence from tomographic imaging and post mortem studies, it was proposed that combined agonism of M1 and M4 receptors may be more efficacious given that a subgroup of people with schizophrenia also showed M1 muscarinic receptor deficiency, known as muscarinic receptor deficit schizophrenia (MRDS) [44]. Moreover, intervention with agonist action at M4 receptors also produced cognitive enhancement and anti-psychotic-like effects in animal models of the schizophrenia [45, 46]. This is a growing area of development with several pharmaceutical companies pursuing active muscarinic programmes (Table 1) for psychiatric disorders, including Karuna therapeutics (KarXT (Xanomeline+Trospium); NCT04659161), Sosei Heptares (HTL0016878; NCT03244228, NCT04849286, NCT04935320) and Cerevel therapeutics (Emraclidine: NCT05227703, NCT05227690).
Table 1.
Characteristics of muscarinic-receptor targeted interventions
| Name of drug | Muscarinic receptor preference | Pharmacological action | References |
|---|---|---|---|
| RS-86 | M1/M2 | Agonist | [122] |
| Xanomeline | M1/M4 | Agonist |
[123] [124] |
| KarXT: A fixed combination of xanomeline and trospium chloride | Xanomeline: M1/M4 | Agonist |
[123] [124] |
| Trospium chloride: Non-selective | Peripherally acting antagonist |
[125] https://www.medicines.org.uk/emc/medicine/22236 Last accessed: 19th Sept 2022 |
|
| Biperiden | M1 | Antagonist |
[126] [127] |
| Scopolamine | Non-selective | Antagonist | [126] |
| Glycopyrrolate | Non-selective | Peripherally acting antagonist | [128] |
| Lu 25-109 | Partial M1 agonist, M2 and M3 antagonist | Agonist | [129] |
| Drugs in clinical trials | |||
| HTL9936 (NCT02291783) | M1 | Agonist |
Last accessed: 19th Sept 2022 |
| HTL0018318 (NCT03456349) | M1 | Partial agonist |
https://soseiheptares.com/news/109/129/Sosei-Provides-Update-on-HTL0018318.html Last accessed: 19th Sept 2022 |
| Talsaclidine (NCT02249403) | M1 /M2/M3 | Agonist | [130] |
| HTL0016878 (NCT03244228) | M4 | Agonist |
Last accessed: 19th Sept 2022 |
| Emraclidine (CVL-231) (NCT05227703, NCT05443724, NCT05227690) | M4 | Positive allosteric modulator |
https://www.cerevel.com/compounds/emraclidine/ Last accessed: 19th Sept 2022 |
M1-M5 muscarinic receptor subtypes 1–5
Dementia/Alzheimer’s Disease
The clinical syndrome of dementia consists of several subtypes, including AD, vascular, frontotemporal and dementia with Lewy bodies. Alzheimer’s Disease contributes to 60–70% of cases [47]. Globally, 55 million individuals have dementia, which is expected to rise to 139 million by 2050 [47]. Along with cognitive impairment, 97% of patients also experience neuropsychiatric symptoms [48], also referred to as ‘behavioural and psychological symptoms of dementia (BPSD)’, which include lack of motivation, psychotic symptoms, depression, anxiety, agitation, and impulsivity [49, 50]. Current drug therapy for BPSD consists of atypical antipsychotics, antidepressants and anticonvulsants, which may cause severe adverse effects such as excessive sedation, orthostatic hypotension and cognitive slowing [51].
The cholinergic hypothesis of AD suggests that degeneration of cholinergic innervations in the cortex and hippocampus substantially contributes to cognitive dysfunction. In fact, the role of the acetylcholine system in learning and memory was first identified 50 years ago, when the muscarinic receptor antagonist scopolamine produced cognitive impairment in rats [52]. Clinical observation found acetylcholine esterase inhibitors such as tacrine, rivastigmine, donepezil and galantamine improved both cognition and behavioural and psychiatric symptoms. Unfortunately, dose-dependent adverse effects attributed to non-selective activation of acetylcholine receptors in both the central and peripheral nervous system restrict clinical utility [53].
Preclinical and post mortem findings also implicate muscarinic receptors in BPSD [54, 55]. Out of all five subtypes, M1 receptor is most abundantly expressed in the prefrontal cortex and hippocampus [56]. Recently, M1 muscarinic receptors have been postulated to be potential therapeutic agents for both cognitive and non-cognitive symptoms of AD [57, 58]. Additionally, the M4 receptor may also represent a potential target for BPSD because of its widespread expression in the cortex, striatum, thalamus and hippocampus, key brain regulators for emotional processing and motivation [59]. Collectively, these results highlight the potential of muscarinic receptors in the regulation of cognitive and behavioural symptoms observed in AD patients [59].
Anxiety Disorders
Anxiety disorders are a group of psychiatric disorders comprised of generalised anxiety, panic disorders and various phobias (such as social phobia or claustrophobia). Data from the National Comorbidity Survey Replication suggest that 31.1% of US adults experience an anxiety disorder at least once in their lifetime [60]. A preclinical study revealed pro-depressive and anxiogenic-like effects following infusion of pilocarpine (a cholinergic agonist) in rats. In this study, pilocarpine was infused directly into ventral tegmental area (VTA), as mAChR in the midbrain are critical regulators of anxiety-like behaviour [61]. In contrast, the non-selective mAChR antagonist scopolamine attenuated chronic stress-induced anxiety-like behaviour in mice following intra-hippocampal administration [62]. Additionally, a recent study showed that direct infusion of a selective M5 negative allosteric modulator into the VTA can modulate both depressive-like and anxiety-related behaviours in rats, implying a potential role for M5 receptors in the regulation of anxiety-like behaviour [63].
Given this evidence, we therefore aimed to systematically review findings from randomised controlled trials (RCTs) assessing the therapeutic effectiveness of muscarinic-receptor targeted interventions in adults with neuropsychiatric disorders, including mood disorders, primary psychotic disorders, dementia/AD, and anxiety disorders.
Methods
Protocol and Registration
The study was registered with the International Prospective Register of Systematic Reviews (PROSPERO: CRD42021236260) and followed the Preferred Reporting Items for Systematic Reviews and Meta-Analysis guidelines (PRISMA) statement [64]. To limit the number of studies retained for screening, each step adhered to the PRISMA statement.
Detailed Search Strategy
Comprehensive systematic computer-based searches were carried out in PubMed, EMBASE, PsycINFO, EBSCO, and Web of Science, from database inception to the 31st of August 2021, with no date or publication type limitation. Different combinations of keywords along with synonyms and word variants of keywords were used to create a comprehensive search strategy. Relevant search terms included: ("Muscarinic") AND ("Mental Health" OR "Mental disorder" OR "Psychiatric disease" OR "Psychiatric illness" OR "Psychiatric disorder" OR "Psychological disorder" OR "Behaviour disorder" OR "Behavior disorder" OR "Psychosis" OR "Schizophrenics" OR "Schizophrenia" OR "Mental illness" OR "Psychotic disorder" OR "Schizoaffective disorder" OR "Depression" OR "Depressive" OR "Anxiety" OR "Neurotic disorder" OR "Habit" OR "Impulsive disorder" OR "Bipolar disorder" OR "Bipolar" OR "Mood disorder" OR "Learning" OR "Memory" OR "Attention" OR "Neuropsychiatric disorder" OR "Obsessive-compulsive disorder" OR "Personality disorder" OR “Dementia” OR “Alzheimer”) AND ("Human" OR "Participants "OR "Subjects" OR "Clinical") in the title, abstract, and keywords. We also manually searched the bibliography of eligible studies and full-text reviews for relevant papers if not incorporated in the primary search strategy. Searches were re-run before submission on 7th August 2022.
Inclusion Criteria
Articles qualified for inclusion if they: (1) investigated the effect of muscarinic receptor-targeted interventions; (2) included adults with a Diagnostic and Statistical Manual of Mental Disorders (DSM)/ICD diagnosis of neuropsychiatric disorder (schizophrenia, psychotic disorder, schizoaffective disorders, mood (affective) disorder, depression, mania, bipolar disorder, neurotic disorders, anxiety disorder, obsessive-compulsive disorder, habit and impulse behaviour, personality disorder), OR patients with dementia/AD (where the symptomatic measures are both cognitive and non-cognitive function or neuropsychological test); (3) had a comparison group (inactive placebo/active placebo); and (4) were published in English-language in a peer-reviewed journal. There were no restrictions to sample sizes, demographics, trial type (i.e., parallel or crossover) or type of intervention (agonist/antagonist). After initial title and abstract screening, only empirical articles were included in the full-text screening. For further inclusion in the meta-analysis, trials needed to be: (1) randomised controlled trials; (2) have no repeated participants; and (3) measure psychiatric symptoms on a validated disorder-specific psychometric scale.
Full-text articles were excluded if they: (1) were other systematic reviews or meta-analyses, conference proceedings published as abstract only, case reports, book chapters or animal study; and (2) lacked randomisation details (i.e., whether treatment allocation was randomised) (3) Published in other than English language. We also excluded studies where the population of interest were adolescents and children aged ≤ 17 years or adults with dementia and AD where cognition was the only outcome measure.
Study Selection
Full-text articles were screened by two independent reviewers (SV and AAG) using the web-based systematic review tool Covidence (Veritas Health Innovation, Melbourne, Australia). Any disagreement between the two reviewers was resolved via discussion to achieve consensus.
Data Extraction and Outcome Included in the Qualitative Synthesis
A custom datasheet was generated using Microsoft Excel, and all relevant data were extracted by the primary reviewer (SV). All extracted data were verified independently by a second reviewer (AAG). The following study characteristics were extracted: (1) lead author; (2) publication year; (3) country; (4) sample size; (5) sample demographics (age, sex, and ethnicity); (6) study settings; and (7) participant characteristics (any co-morbidity or treatment status). In addition, details of mAChR interventions were extracted, including (1) name of the drug and mechanism of action; (2) dose; (3) route of administration; (4) washout period; (5) frequency; (6) experimental design; (7) comparison group used; (8) adverse effects; (9) retention rates; and (10) main findings of the trial.
The primary outcome measures were the mean and standard deviation of the after-treatment symptomology measurement for active and placebo interventions. We also included studies where rapid eye movement (REM) sleep alteration was a diagnostic measure. It has been hypothesised that REM sleep alterations in depression aid in the progression of depressive symptoms, including cognitive distortions and negative self-esteem [65].
Quality and Risk of Bias Assessment
The quality of studies included for analysis was assessed using the Cochrane risk of bias assessment tool (ROB-2) for randomised controlled trials [66]. Cochrane ROB-2 assesses five individual domains for bias: (1) randomisation process; (2) deviations from intended interventions; (3) missing outcome data; (4) measurement of the outcome; and (5) selection of the reported result. Each individual category was ranked as low risk, some concern or high risk of bias. Two independent reviewers (SV and AAG) assessed the risk of bias, any disagreements were solved by discussion.
Data Synthesis and Analysis
For the systematic review, a narrative synthesis approach was utilised to describe findings from included studies. There are four significant steps included in the Cochrane guidelines [67]. The first step was to develop a hypothesis about the mechanism of intervention. Alteration in acetylcholine release has been widely observed across various neuropsychiatric disorders, and muscarinic receptors modulate the release of acetylcholine both pre- and post-synaptically. Based on these facts, the question was framed. In the next step, we performed a pilot search for relevant studies. In addition to data extraction, discrepancies and factors influencing results were also interrogated to follow step 3. A significant challenge with narrative synthesis is the lack of transparency, which increases the likelihood of bias and reduces the robustness of findings. To prevent that, methods were pre-specified in the PROSPERO protocol and strictly followed.
Meta-analyses were performed with the help of Cochrane Review Manager software (Revman Version 5.4, The Cochrane Collaboration 2020). The standardised mean difference (SMD) was used as an outcome measure. The SMD was calculated as the difference in mean outcome between placebo and active intervention, divided by the pooled standard deviation of outcome among participants. In the absence of standard deviation, it was calculated from the number of participants, p-values and standard error. We used pre-crossover data from crossover trials to mimic the parallel trials. By assuming study level variability, we used a random-effects model. A Forest plot was generated to visualise the individual contribution of the study, and I2 statistics were computed to assess heterogeneity between studies, where < 40% was considered low heterogeneity while > 40% represents moderate to substantial (< 60%) heterogeneity. Leave-one-out sensitivity analyses were performed to estimate influence and bias, whereby SMD values were calculated by discarding one different observation each time. Meta-regression and funnel plots were considered inappropriate for this study as less than ten studies were included in the quantitative analysis [68]. To assess our confidence in meta-analysis effect estimates, the certainty of the evidence was judged by using the grading of recommendation assessment, development, and evaluation (GRADE) system using the GRADEpro GDT web application (Grade Pro GDT, 2020). The assessed criteria were risk of bias, consistency, directness, precision, and publication bias (Table 2).
Table 2.
Certainty analysis using GRADE
| Certainty analysis | ||||||||
|---|---|---|---|---|---|---|---|---|
| Outcome | No. of studies | Study design | Risk of bias | Inconsistency | Indirectness | Imprecision | Publication bias | Certainty |
| Anti-depressant effect | 5 | Randomised controlled trial | Not serious | Seriousa | Not serious | Seriousb | Strongly suspectedc |
⊕⊝⊝⊝ Very Low |
| Anti-anxiety effect | 3 | Randomised controlled trial | Not serious | Seriousa | Not serious | Seriousb | Strongly suspectedc |
⊕⊝⊝⊝ Very Low |
aDown-graded one level for inconsistency: I2 value represents high heterogeneity (>50%)
bDown-graded for imprecision due to lower sample size for standardised mean difference (< 100/group)
cDown-graded one level for publication bias: Funnel plot was not created because of low study numbers (<10); however, leave one out sensitivity analysis changes the significance
Results
Selection of Studies
Initial database searches yielded 4368 potential articles, of which 2525 duplicates were removed (Fig. 1). Following title and abstract screening, full-text for the remaining 287 articles were reviewed for eligibility; of these, 254 were excluded for various reasons (e.g., inappropriate outcome measures, no information about randomisation, conference abstracts and other reviews). In total, 33 studies were included in the systematic review. Five studies were included in the meta-analysis. Table 1 represents the characteristics of each included muscarinic-receptor targeted intervention. Table 3 summarises the study characteristics of the 33 trials included. Studies were divided into groups based on disorder; 17 studies on mood disorders, 7 on primary psychotic disorders, 5 studies on dementia/AD, 2 on anxiety disorders, and the remaining 2 articles included people with both psychotic and mood disorders.
Fig. 1.
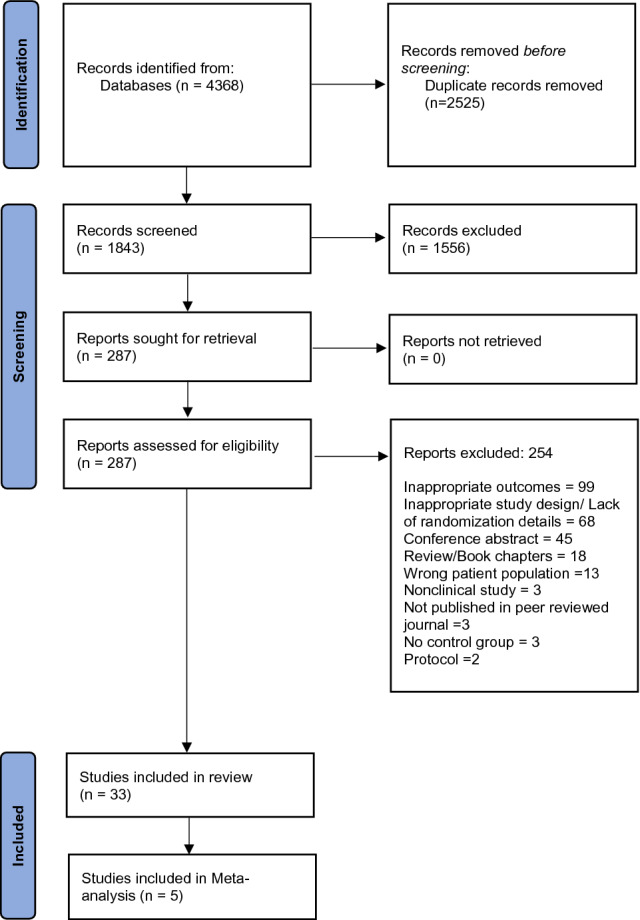
Preferred Reporting Items for Systematic Reviews and Meta-Analysis guidelines (PRISMA) flow diagram
Table 3.
Study characteristics listed alphabetically based on the first author
| Lead author and year | Sample size and characteristics | Study settings and country | Psychiatric diagnosis | Patients characteristics | ROB-2 score | ||
|---|---|---|---|---|---|---|---|
| The total number of patients enrolled | Mean age (SD) | Sex (%) | |||||
| Battaglia (2001) [70] | N = 12 | 27.35 (5.1) | M = 50, F = 50 |
San Raffaelle Hospital, Italy |
DSM-III-R and DSM-IV: panic disorder |
None of the subjects taking a benzodiazepine, one man qualified for alcohol abuse 4 years before the experiment | High risk |
| Bakker (2020) [92] | N = 26 | 27.7 (4.9) | M = 73, F = 27 | Netherlands | DSM-IV: Psychotic disorder | Medication-free and were recruited from early detection and intervention programmes | Some concerns |
| Beckmann (1982) [83] | N = 6 | 49 (7.8) | F = 100 | Germany | ICD-9: Primary affective disorder or MDD |
Mainly diagnosed as an affective disorder, consecutively admitted, severely depressed, Duration of illness >15 days. Unipolar n = 4, bipolar n = 1, neurotic depression n = 1 All patients were drug-free at least 7 days before the study |
Some concerns |
| Berger (1989) [104] | N = 16 | 38 (14) | M = 37.5, F = 62.5 | Germany |
DSM-III: MDD |
Drug-free >1 week Patients are acutely depressed |
Some concerns |
| Bodick (1997) [99] | N = 343 | 74.9 (6.6) | M = 43, F = 57 | USA |
NINCDS/ADARA: Mild to moderate AD |
Same as Veroff, 1998 | Some concern |
| Brannan (2021) [72] |
Total N = 182 Placebo (n = 90) KarXT (n = 92) |
Placebo group: 41.6 (10.1) KarXT group: 43.1 (10.1) |
Placebo M = 74, F = 26 KarXT M = 80, F = 20 |
USA |
DSM-5: SCZ |
Free from anti-psychotic medication 2 weeks before the baseline assessment | Low risk |
| Bruno (1986) [101] | N = 8 | 62 (SEM 1.5) | M = 38, F = 62 | National Institute of Health, USA |
DSM-III: AD with mild to moderately advanced dementia |
No centrally active medications received > 2 weeks before study | Some concern |
| Craske (2019) [103] | N = 66 |
Placebo group: 23.05 (8.58), 0.5 mg group: 26.53 (10.21), 0.6 mg group: 25.47 (10.56) |
M: N = 22, F: N = 35, undeclared n = 2, did not answer n = 1 (Placebo: M n = 4, F n = 17, Scopolamine 0.5 mg; M n = 8, F n = 10, undeclared = 1, Scopolamine 0.6 mg; M n = 10, F n = 8 transgender n = 1, undeclared n = 1) |
California, USA |
DSM-IV/5: Anxiety disorder Social anxiety disorder |
Patients have a fear, anxiety disorder and fear of public speaking | Low risk |
| Drevets (2010) [75] | N = 22 |
P/S group: 30 (7.0), S/P group: 33 (7.1) |
M = 45, F = 55 | National Institute of Mental Health, USA |
DSM-IV: MDD |
Chronic illness (>2 years) n = 13, comorbid anxiety n = 8, unresponsive to treatment n = 6 | Low risk |
| Ellis (2014) [78] | N = 62 | 32.4 (9.5) | M = 40, F = 60 | National Institute of Mental Health, USA |
DSM-IV: BP or MDD |
Treatment resistant n=31, treatment-naïve n=31, all the participants were medication-free at least two weeks before the study (MDD n=49, BP-I n=1, BP-II n=12) |
Some concerns |
| Furey (2015) [79] | N = 16 | 32.4 (8.9) | M = 19, F = 81 | National Institute of Mental Health, USA |
DSM-IV: MDD without psychosis |
Unmedicated depressed major depressive disorder patients, 5 patients have a comorbid anxiety disorder | Low risk |
| Furey (2013) [77] | N = 15 | 32.9 (7.8) | M = 74, F = 26 | National Institute of Mental Health, USA |
DSM-IV: Recurrent MDD |
MDD without psychotic features, 5 MDD patients have comorbid anxiety disorder | Low risk |
| Furey (2010) [76] |
N = 52 P/S group (n = 27) S/P group (n = 25) |
P/S group: F = 31.2 (7.6) M = 30 (9.1) S/P group: F = 35.7 (7.6) M = 32.8 (10.2) |
P/S group M = 44, F = 56 S/P group M = 36, F = 64 |
National Institute of Mental Health, USA |
DSM-IV: BP or MDD |
MDD: Male n=17, F n=21; BP: M n=4, F n=10, patients have severe illness >2 years n=31, patients have comorbid anxiety n=20 |
Low risk |
| Furey (2006) [74] | N = 19 |
P/S group: 35.1 (8.5) S/P group: 30.9 (9.2) |
P/S F = 70, M = 30 S/P F = 87.5, M = 12.5 |
National Institute of Mental Health, USA |
DSM-IV: BP or MDD |
Chronically ill n=12, co-morbid anxiety n=8, unresponsive to previous treatment n=5 |
Low risk |
| Gillin (1995) [84] | N = 19 | 44 (26) | M = 58, F = 42 | Mental Health Clinical Research Center in the San Diego VA Medical Center, USA |
DSM-III-R: BP or MDD |
Drug-free 14 days before the study; Major depression n = 17, bipolar disorder, depressed type n=2 (secondary diagnosis: dysthymia n = 3, alcohol abuse in remission n = 6, substance abuse in remission n = 5, social phobia = 5, panic disorder n = 3, OCD n = 1, PTSD n = 2) |
High risk |
| Hollander (1987) [100] | N = 15 |
66.1 (54–78) |
M = 47, F = 53 | Clinical Research Center of the Mount Sinai Hospital; Special Treatment Unit of the Bronx VA Medical Center of the Mount Sinai School of Medicine, USA |
Research diagnostic criteria for Alzheimer's disease/NINCDS: Probable AD |
All patients were drug free for 2 weeks prior to, and throughout the study | High risk |
| Khajavi (2012) [80] |
Total: N = 40 Scopolamine n = 20 Placebo n = 20 |
Scopolamine group: 37.8 (6.7) Placebo group: 36.6 (6.8) |
Scopolamine F = 60, M = 40 Placebo F = 65, M = 35 |
Outpatient clinics of Roozbeh Psychiatric Hospital and National Iranian Oil Company Central Hospital, Iran |
DSM-IV-TR: MDD |
Citalopram (up to 40 mg) is given in both groups along with scopolamine and placebo during all 6 weeks. As per the author's knowledge, no interaction between escitalopram and scopolamine | Low risk |
| Liang (2010) [94] | N = 13 |
Age range: 20–65 |
M = 42, F = 58 |
Tri-service general hospital, Taiwan |
DSM-IV: SCZ |
All the patients are taking routine antipsychotic treatment (includes clozapine) except any other anticholinergic drugs during a 12-week study | Low risk |
| Newhouse (1988) [69] | N = 9 | 69.7 (6.1) | M = 67, F = 33 | National Institute of Mental Health, USA |
DSM-III: Major depression |
Elderly patients, drug-free for at least 3 weeks | High risk |
| Park (2019) [81] | N = 23 | 36.83 (10.78) | M = 48, F = 52 |
National Institute of Mental Health USA |
DSM-IV: MDD |
MDD subjects with more severe and refractory forms of major depressive disorder relative to previous patients, medication-free depressive subjects, comorbid disorders: Anxiety disorder n = 7, OCD n = 3, PTSD n = 3, personal history of alcohol n = 7 | Some concerns |
| Poland (1997) [90] |
Depressed N = 14 Remitted/Recovered N = 16 |
Depressed: 42.6 (3.1) Remitted/Recovered: 39.7 (3.3) |
Depressed M = 21, F = 79 Remitted/Recovered M = 31, F = 69 |
California, USA |
DSM-III-R: Major depression |
Patients with unipolar major depressive disorder and recovered subjects | Some concerns |
| Rao (2004) [91]) | N = 10 | 33.3 (8.8) | F = 100 | USA |
DSM-IV: MDD |
Unipolar major depressive disorder/medication free from last 3 months | High risk |
| Riemann (1994a) [89] | N = 56 | 40.6 (13.6) | M = 36, F = 64 | Germany |
DSM-III: MDD |
Major depressive disorder | High risk |
| Riemann (1994b) [96] | N = 40 |
Depression: 42.7 (12.1) |
M = 35, F = 65 | Psychiatric clinic of the University of Freiburg, Germany |
DSM-III-R: Unipolar depression, BP I & II |
Patients with major depressive disorder; unipolar depression n=34, bipolar depression I or II n = 6, Drug-free 7 days prior to investigation |
Some concerns |
| N = 43 |
Schizophrenia: 29.3 (6.7) |
M = 70, F = 30 | Psychiatric clinic of the University of Freiburg, Germany |
DSM-III-R: SCZ |
Schizophrenic form subtype n = 5, paranoid schizophrenia n = 10, residual type of disorder n = 21, undifferentiated/unorganized schizophrenia n=7, Patients are drug-free for > 6 days. Patients also have first-degree depressive disorder n = 6; patients have some other psychiatric symptoms (e.g., alcoholism) n = 10 |
Some concerns | |
| Riemann (1992) [88] | N = 40 | 40.9 (12.3) | M = 42.5, F = 57.5 | Germany |
DSM-III: MDD & bipolar disorder “depressed type.” |
MDD=33, bipolar disorder "depressed type" n = 7 | Some concerns |
| Riemann (1991) [87] | N = 11 | 33.9 (3.9) | M = 36, F = 64 | Germany |
DSM-III: MDD |
No medication 7 days before treatment | Some concerns |
| N = 11 | 33.6 (8.7) | M = 73, F = 27 | Germany |
DSM-III-R: Residual SCZ |
Patients also fulfilled the MDD criteria for a secondary measure n=6, all subjects were free from psychoactive medicine 7 days before | Some concerns | |
| Segev (2019) [73]) | N = 15 | 38.7 (12) | M = 71, F = 29 | UK |
DSM-IV-TR: SCZ or schizoaffective disorder |
Receiving clozapine for <2 weeks | Low risk |
| Shekhar (2008) [71] | N = 20 |
Control: 42.1 (9.2) Xanomeline: 43.4 (9.3) |
Control M = 80, F = 20 Xanomeline M = 60, F = 40 |
Neuroscience Clinical Research Center at Indiana University, USA |
DSM-IV: SCZ or schizoaffective disorder |
Patients taking atypical antipsychotic n = 12, typical antipsychotic n = 6, Drug-free from 1 month n= 1, drug-free from 3 months n=1, medication-free before 3–7 days |
Some concerns |
| Silver (1995a) [93] | N = 26 | 36.7 (8.9) | M = 69, F = 31 | Israel |
DSM-III-R: Schizophrenia |
Chronically medicated schizophrenic patients, all anti-psychotic medication continued throughout the study | Some concerns |
| Silver (1995b) [95] | N = 26 | 36.65 (8.89) | M = 69, F = 31 | Israel |
DSM-III-R: Schizophrenia |
All antipsychotic medication continued throughout the study | Some concerns |
| Thal (2000) [102] | N = 496 | 75.5 (1) | M = 42, F = 58 | 29 centres across the USA |
National Institute of Neurologic and Communicative Disorders-Alzheimer's Disease and Related Disorders Association criteria: Probable AD |
N/A | Low risk |
| Veroff (1998) [98] | N = 343 | 74.9 (6.6) | M = 43, F = 57 | Lily research laboratories, California, USA |
NINCDS/ADRDA: Mild to moderate AD |
Use of central nervous system drugs were prohibited 1 month before study | Some concern |
| Zhou (2020) 82] | N = 66 |
Saline: 27.1 (7.0), Low dose: 25.7 (5.3), High dose: 26.5 (5.6) |
M = 35, F = 65 | Beijing Anding Hospital, Capital Medical University, China |
DSM-IV: MDD |
Permitted non-benzodiazepines for severe insomnia and benzodiazepines for significant anxiety but not 8 h before assessment) | High risk |
AD Alzheimer’s disease, ADRDA AD and associated disorders association, BP bipolar disorder, BP-I bipolar disorder type-I, BP-II bipolar disorder type-II, DSM Diagnostic and Statistical Manual of Mental Disorders, F female, ICD International Classification of Diseases, M male, MDD major depressive disorder, N total numbers of participants, n participants in subgroup, N/A not available, NINCDS National Institute of Neurological and Communicative Disorders and Stroke, OCD obsessive-compulsive disorder, PTSD posttraumatic stress disorder, P/S placebo/scopolamine group, RDS research diagnostic criteria, SCZ schizophrenia, SD standard deviation, SEM standard error of the mean, S/P scopolamine/placebo group
Quality and Risk of Bias
Table 3 and Fig. 2 show the ROB-2 quality assessment for each study. Seven studies were rated as high risk of bias, 15 had some concerns, and 11 were rated as low risk of bias. The percentage similarities between the two reviewers were 82%, and the kappa score was 0.76 indicating substantial agreement. All studies included were randomised, placebo-controlled double-blind trials, except one, where the study was pseudo-randomised [69]. The main limitation across studies was poorly described randomisation details. Only 10 trials explicitly described randomisation methods, and 13 described allocation concealment. The second prime reason for some concern was the lack of information about assessors’ blinding, which may lead to bias in study results. In seven studies, the dropout rate exceeded 20% [69–73]. In two studies, the key reason was adverse events, especially in the high-dose group. The reason for dropout was unavailable for two studies. Despite one having a significant effect on the overall visual analogue score (VAS) in people with depression, the reason for dropout was not given [69, 70]. Shekhar and colleagues (2008) reported that participants dropped out in both arms [71]. The KarXT clinical trial mentioned several reasons, including adverse events, consent withdrawal, withdrawal by an investigator, and forgetting to follow-up [72].
Fig. 2.

Risk of bias assessment using ROB-2 tool. The weighted summary plot suggests that most studies fall under the category of “some concern” due to insufficient details about the randomisation process
Mood Disorders
Among the 19 studies in people with MDD or BP (Tables 3 and 4), 11 were conducted in the USA, 6 in Germany, one in Iran and one in China. A total of 538 participants ranging in age from 18 to 72 years, and 66% were female. In all, 12 studies investigated the effect of scopolamine, 5 studies RS-86 and 2 studies investigated the impact of biperiden. Seven scopolamine studies administered the medication intravenously, of which six showed that scopolamine effectively reduced depressive symptoms [74–79]. Further, when administered orally, scopolamine also reduced depressive symptoms in one study [80]. However, a more recent study exhibited no significant difference between scopolamine and placebo treatments post-intravenous administration [81]. In agreement with a more recent study, intramuscular scopolamine injection did not produce a significant difference compared to placebo [82]. However, in all the previous studies, symptom measurement was performed after every three infusions, whereas results were obtained 28 days after scopolamine injections in the intramuscular study. Acute biperiden administration reduced depressive symptoms compared to the placebo group [83]. In contrast, participants who received biperiden for 4 weeks did not significantly differ from placebo [84].
Table 4.
Outcomes of mood disorders (mixed cohort of MDD and BP)
| Lead author, year | Study design | Interventions and comparator (Dose/route of administration) | Adverse effects | Main outcome measures | Key findings | Retention rate (%) |
|---|---|---|---|---|---|---|
| Beckmann (1982) [83] |
Acute, double- blind, randomised, placebo- controlled |
Intervention: biperiden 10 mg IV 4 days Control: placebo Washout: 24 h |
No psychiatric or somatic side effects reported |
HAM-D MADRS EWL-K |
Biperiden significantly (p < 0.01) reduced MADRS and EWL-K score compared to placebo Overall, HAM-D score did not significantly differ between two groups; only retardation, agitation factors, depressed mood, and work and interests improved (p = 0.01, p = 0.05, p = 0.01, p = 0.05, respectively). |
100 |
| Berger (1989) [104] | Randomised, double-blind, cross-over |
Intervention: RS-86 1.5 mg oral Once Control: placebo Washout: 24 h |
Increased salivation post RS-86 administration |
REM sleep (latency, duration and density) Both depressive and remissive |
RS-86 significantly reduced REM latency (p < 0.001) compared to placebo In contrast, first REM period density (p < 0.0001), total REM density (p < 0.012) and first REM period (p < 0.26) were increased post RS-86 compared to placebo in depressives No significant effect in remissive on the parameters mentioned above post-RS-86 compared to placebo |
100 |
| Drevets (2010) [75] | Double-blind, randomised, placebo-controlled, cross-over |
Intervention: scopolamine 0.004 mg/kg IV 3 sessions Control: placebo Washout: 3–5 days |
Drowsiness, dry mouth, blurred vision, light headedness, dizziness |
MADRS HAM-A, CGI-I VAS YMRS POMS |
Scopolamine significantly reduced MADRS score change from baseline (p = 0.011) and CGI-I score (p < 0.001) compared to placebo in block 1 However, no difference was found between two groups after cross-over Due to baseline variation HAM-A score, differences in each group (scopolamine and placebo) were measured separately. A significant reduction was observed in HAM-A in the 2nd block in the P/S group (p = 0.001) and 1st block the in S/P group (p < 0.023) compared to the baseline No significant difference in VAS and POMS score relative to placebo |
91.30 |
| Ellis (2014) [78] | Double-blind, randomised, placebo-controlled, cross-over |
Intervention: scopolamine 0.004 mg/kg IV 3 sessions Control: placebo Washout: 3–5 days |
N/A | MADRS |
Scopolamine significantly the reduced MADRS score (p < 0.001) compared to placebo This reduction was higher in treatment-naïve patients compared to treatment-resistant patients (p = 0.04) |
93.54 |
| Furey (2015) [79] | Double-blind, randomised, placebo-controlled, cross-over |
Intervention: scopolamine 0.004 mg/kg IV 3 sessions Control: placebo Washout: 3–5 days |
N/A |
MADRS Selective attention task |
Significant reduction (p < 0.001) in MADRS score compared to baseline at the study end. No data are given For selective attention task, scopolamine did not produce a significant effect on implicit emotional processing compared to baseline |
93.75 |
| Furey (2013) [77] | Double-blind, randomised, placebo-controlled, cross-over |
Intervention: scopolamine 0.004 mg/kg IV 3 sessions Control: placebo Washout: 3–5 days |
N/A |
MADRS Working memory tasks |
Scopolamine significantly reduced MADRS score (p < 0.001) compared to baseline In working memory tasks, scopolamine decreased reaction time in the emotional task and increased in identity tasks (p = 0.05) compared to placebo |
93.33 |
| Furey (2010) [76] | Double-blind, randomised, placebo-controlled, cross-over |
Intervention: Scopolamine 0.004 mg/kg IV 3 sessions Control: placebo Washout: 3–5 days |
Side effects after scopolamine: Dizziness, light-headed, blurred-vision, drowsy, dry mouth, fatigue, feel drugged |
MADRS HAM-A/HARS CGI-I |
Scopolamine significantly reduced MADRS, HAM-A and CGI-I scores (p < 0.001) in females compared to placebo Whereas less significant reduction was observed in MADRS (p = 0.043) and CGI-I (p = 0.046) in males and no change in HAM-A score |
Completed treatment 100 Completed follow up: 84.61 |
| Furey (2006) [74] | Randomised, double-blind, cross-over |
Intervention: scopolamine 0.004 mg/kg IV 3 sessions Control: placebo Washout: 3–5 days |
Drowsiness, dry mouth, blurred vision, light headedness, dizziness, hypotension Drowsiness and dry mouth also reported after placebo |
MADRS HARS/HAM-A CGI-I VAS YMRS POMS Selective attention task |
Scopolamine significantly reduced MADRS (p < 0.001) and CGI-I (p = 0.002) scores compared to placebo in block 1 Due to baseline variation HAM-A score, Difference in each group was measured separately. Significant reduction (p < 0.001) was observed in HAM-A score in 2nd block in P/S group and in 1st block in S/P group compared to baseline No difference was found between two groups in block 2 In selective attention task, performance accuracy was significantly reduced (p = 0.02) No significant effect of scopolamine was observed in VAS, YMRS and POMS scale |
94.73 |
| Gillin (1995) [84] | Randomised, double-blind, parallel |
Intervention: biperiden 4–12 mg/day oral For 4 consecutive weeks Control: glycopyrrolate (active placebo) |
Mild dry mouth and mild constipation (both groups) |
HDRS-17 POMS REM sleep [latency, density, total (%)] |
There was no significant difference in HDRS, POMS and REM latency between biperiden and glycopyrrolate at the end of 4th week | 94.73 |
| Khajavi (2012) [80] | Two-centre, randomised, placebo-controlled, double-blind, parallel |
Intervention: scopolamine 0.5 mg BID Oral 6 weeks Control: placebo |
Dry mouth, blurred vision, dizziness was more common in the scopolamine group compared to the placebo group | HDRS | Scopolamine significantly reduced HDRS score (p = 0.021) compared to placebo after 6 weeks | 100 |
| Newhouse (1988) [69] | Double-blind, pseudorandom, placebo-controlled |
Intervention: scopolamine 0.1 mg, 0.25 mg, 0.5 mg IV once Control: Placebo Washout: 48 h |
Pulse rate shows a decreasing trend with dose, Increase in pupillary size, dry skin and dry mucus membrane Attentional impairment, drowsiness and mild confusion, Restlessness at higher dose |
VAS BPRS Vigilance Selective-reminding words Continuous performance task POMS BPI NSRS Pfeiffer Short Portable Mental Status Questionnaire, Cognitive battery |
Scopolamine significantly increased VAS score (p < 0.01), BPRS score (p < 0.01), NSRS anxiety sub-score (p = 0.02) at 0.5 mg relative to placebo No significant changes in BPI and POMS All the cognitive parameters were impaired at 0.5 mg (p < 0.05) compared to placebo |
100 (9/9) For all other tests 66.66 (6/9) For VAS |
| Park (2019) [81] | Randomised, placebo-controlled, cross-over |
Intervention: scopolamine 0.004 mg/kg IV 3 sessions Control: placebo Washout: 3–5 days |
Dry mouth, constipation, blurred vision, drowsiness, and nervousness |
MADRS HAM-A |
There was no significant difference in antidepressant and antianxiety effects between scopolamine and placebo | 82.60 |
| Poland (1997) [90] | Double-blind, randomised, placebo-controlled |
Intervention: scopolamine 0.0045 mg/kg IM Twice Control: placebo Washout: 24 h |
N/A |
REM sleep (latency, density, duration) |
Scopolamine significantly (p < 0.05) increased 1st REM period latency and decreased overall REM duration relative to placebo | 100 |
| Rao (2004) [91] |
Randomised double-blind, cross-over |
Intervention: scopolamine, 0.0015 mg/kg, IM, twice Control: placebo Washout: 1 week |
None noted |
REM sleep (latency, density, total duration) |
Scopolamine significantly (p < 0.001) increased 1st REM period latency and decreased 1st REM period density (p < 0.005) and overall, REM duration (p < 0.001) relative to placebo | 100 |
| Riemann (1994a) [89] | Randomised, double-blind, cross-over |
Intervention: RS-86 1.5 mg Oral, once Control: placebo Washout: 24 h |
N/A | REM latency | RS-86 significantly reduced REM sleep latency (p = 0.0001) compared to placebo | 100 |
| Riemann (1994b) [96] | Randomised, double-blind cross over |
Intervention: RS-86 1.5 mg Oral, once Control: placebo Washout: 24 h |
N/A |
REM sleep (latency, duration and density) |
RS-86 significantly reduced REM sleep latency (p = 0.0001) compared to placebo | 100 |
| Riemann (1992) [88] | Randomised, double-blind, cross-over |
Intervention: RS-86 1.5 mg Oral, once Control: placebo Washout: 24 h |
N/A | REM latency | RS-86 significantly (p < 0.001) reduced REM latency compared to placebo | 100 |
| Riemann (1991) [87] | Randomised, double-blind-cross over |
Intervention: RS-86 1.5 mg Oral, once Control: placebo Washout: 24 h |
N/A | REM latency | RS-86 significantly reduced REM latency (p = 0.0072) compared to placebo | 100 |
| Zhou (2020) [82] | Double blind, randomised, three-arm, 4 week follow-up, parallel design |
Intervention: Scopolamine: 0.3 mg (OD) 0.3 mg (BID) IM 3 days Control: placebo 10 mg/day of escitalopram was administered for first 3 days as add-on and all also for remaining 25 days until the last follow-up |
Blurred vision, dizziness, somnolence, nausea, fatigue, drowsiness, dry mouth, anxiety, insomnia, and tachycardia |
HDRS-17 MADRS YMRS CGI-I QIDS-SR-16 GAD-7 |
There was no significant effect of scopolamine on any of the symptoms | 83.3 |
BID twice daily, BPI Beck Depression Inventory, BPRS Brief Psychiatric Rating Scale, CGI-I Clinical Global Impression – Improvement scale, EWL-K The Janke and Debus self-rating questionnaire, GAD-7 Generalised Anxiety disorder scale, IM intramuscular, IV intravenous, HAM-A/HARS Hamilton Anxiety Rating Scale, HAM-D Modified Hamilton Rating scale, HDRS The Hamilton Rating Scale for Depression, MADRS Montgomery and Åsberg Depression Rating Scale, N/A not available, NSRS National Institute of Mental Health Self-Rating Scale, OD once daily, POMS Profile of Mood States, QIDS-SR-16 Quick Inventory of Depressive symptomatology, REM rapid eye movement, VAS visual analogue scale, YMRS Young Mania Rating Scale
People with MDD frequently display sleep abnormalities, specifically reduced REM latency and heightened REM density [85, 86]. The remaining mood disorder studies focused on muscarinic receptor interventions in the modulation of REM sleep in people with depression. The muscarinic receptor agonist RS-86 reduced REM latency and enhanced REM density in depressed patients compared to placebo [87–89]. Conversely, REM latency was increased in response to the muscarinic receptor antagonist scopolamine compared to placebo [90, 91].
Primary Psychotic Disorders
Nine studies examined the effect of muscarinic receptor interventions in primary psychotic disorders (Tables 3 and 5). Six studies included people with schizophrenia, two with unspecified psychotic disorders, and one with schizophrenia and schizoaffective disorder. The sample sizes ranged from 11 to 182 participants, for a total of 361 participants (age range: 19–65 years; 31.2% female participants). Biperiden treatment was administered in four studies, and one for each of scopolamine, xanomeline, and KarXT. In the remaining two studies, RS-86 was used to measure disrupted sleep parameters in psychiatric patients but not for primary psychiatric symptom measurements.
Table 5.
Outcomes of primary psychotic disorders
| Lead author, year | Study design | Interventions and comparisons (dose/route of administration) | Adverse effects | Main outcome measures | Key findings | Retention rate (%) |
|---|---|---|---|---|---|---|
| Bakker (2020) [92] |
Counter-balanced, randomised- controlled trial |
Intervention: biperiden 4 mg Oral, once Control: placebo |
N/A | PAL of CANTAB | Biperiden significantly impaired all cognitive loads of learning (p < 0.001 for 4 and 6 pairs, p = 0.002 for 8 pairs) and memory (p < 0.004) phase except 6 and 8 pair association in the memory phase | 100 |
| Brannan (2021) [72] |
Phase 2, randomised, double-blind, placebo- controlled |
Intervention: KarXT 50–125 mg xanomeline + 20–30 mg trospium, with the option to reduce to 100 mg + 20 mg Oral, BID 5 weeks Control: placebo |
Constipation, nausea, dry mouth, dyspepsia, vomiting |
CGI-I PANSS Marder negative symptom sub-score |
KarXT significantly reduced (p < 0.001) PANSS total score, PANSS positive and negative symptom sub-scores and Marder negative symptom sub-score There was no significant difference in CGI-I score between the groups |
79.67 |
| Liang (2010) [94] |
Randomised, double-blind, cross-over, fixed dose |
Intervention: biperiden 2 mg BID Oral, 4 weeks Control: glycopyrrolate Washout: 4 weeks |
Constipation, inner unrest |
MMSE DRS |
No significant difference was found in DRS score across two groups Biperiden significantly reduced MMSE score at week 4 compared to baseline (p = 0.008) |
92.30 |
| Riemann (1994b) [96] |
Randomised, double-blind cross over |
Intervention: RS-86 1.5 mg Oral, once Control: placebo Washout, 24 h |
N/A |
REM sleep (density, latency, duration) |
RS-86 significantly reduced REM sleep latency (p = 0.0001) compared to placebo | 100 |
| Riemann (1991) [87] |
Randomised, double-blind cross over |
Intervention: RS-86 1.5 mg Oral, once Control: placebo Washout: 24 h |
N/A | REM Latency | RS-86 significantly reduced REM sleep latency (p = 0.0072) compared to placebo | 100 |
| Segev (2019) [73] |
Randomised, double-blind, cross-over, placebo- controlled |
Intervention: scopolamine 0.3 mg/day oral 28 days Control: placebo Cross-over: 7 days |
GIT-1, neurological-2, psychological-2, Musculoskeletal-2 |
HADS anxiety score HADS depression score Toronto nocturnal hypersalivation scale EQ5D-quality of life analogue scale |
Scopolamine significantly (p < 0.001) improved hypersalivation compared to placebo While no significant difference was found in the HADS anxiety scale, HADS depression scale and EQ5D scale across two groups |
73.33 |
| Shekhar (2008) [71] |
Randomised, double-blind, placebo- controlled |
Intervention: xanomeline up to 75 mg TID Oral, 28 days Control: placebo |
Salivation, diarrhoea, nausea, vomiting, GI distress, dizziness, increase in liver function, sweating, flatulence |
CGI-I BPRS PANSS Cognitive measure (processing speed, vigilance, working memory, verbal learning, visual learning) Simpson-Angus rating scale Abnormal involuntary movement scale Barnes rating scale for drug-induced akathisia |
Xanomeline significantly reduced total BPRS scores (p < 0.05) and total PANSS scores (p = 0.039) compared to placebo In the cognitive test battery, subjects in the xanomeline group showed improvements most robustly (p < 0.05) in measures of verbal learning and short-term memory function compared to placebo No significant difference was observed across groups in any other scales |
75 |
| Silver (1995a) [93] |
Double-blind, cross-over, randomised |
Intervention: biperiden 4 mg/day (2 mg BID) Oral, 2 weeks Control: amantadine Washout, 1 week |
N/A |
MMSE BVRT WMS |
Biperiden significantly reduced BVRT (p < 0.003) and visual subscale of WMS (p ≤ 0.02) score, with a trend to poorer scores on WMS total (p = 0.086) and the digit span (p = 0.065) and logical memory (p = 0.06) subscales. No significant difference in MMSE score between the two groups |
100 |
| Silver (1995b) [95] |
Double-blind, cross-over, randomised |
Intervention: biperiden 4 mg/day (2 mg BID) Oral, 2 weeks Control: amantadine Washout, 1 week |
N/A |
SANS BPRS SAPS SAS |
No significant difference was found between biperiden and amantadine in any of the scales | 100 |
BID twice daily, BPRS Brief Psychiatric Rating Scale, BVRT Benton Visual Retention test, CANTAB Cambridge Neuropsychological Test Automated Battery, CGI-I Clinical Global Impression – Improvement scale, DRS Drooling Rating Scale, EQ-5D EuroQol five-dimension scale, GIT Gastrointestinal tract, HADS Hospital Anxiety and Depression Scale, HAM-A Hamilton Anxiety Rating Scale, MMSE Mini-Mental State Examination, N/A not available, PAL paired associate learning, PANSS The Positive and Negative Syndrome Scale, REM rapid eye movement, SANS Scale for the Assessment of Negative Symptoms, SAPS Scale for the Assessment of Positive Symptoms, SAS Simpson-Angus scale, WMS Wechsler Memory Scale Mental Health Self-Rating Scale, POMS Profile of Mood States, QIDS-SR-16 Quick Inventory of Depressive symptomatology, REM rapid eye movement, TID three times daily, VAS visual analogue scale, YMRS Young Mania Rating Scale
Administration of biperiden (4 mg, orally) produced significant impairment in Weschler memory scale, Benton visual retention test and paired-associate learning on Cambridge Neuropsychological Test Automated Battery in people with a primary psychotic disorder compared with controls [92, 93]. In contrast, one of the four studies showed no changes in Mini-Mental State Examination [93, 94]. Additionally, no significant difference was found in positive and negative symptoms [95]. Like biperiden, scopolamine had no significant impact on anxiety and depressive symptoms in subjects with a psychotic disorder [73], suggesting the potential efficacy of scopolamine is limited to patients with mood disorders.
Shekhar et al. 2008, studied the efficaciousness of xanomeline in subjects with schizophrenia, finding a beneficial effect of xanomeline in both positive and negative symptoms compared with placebo [71]. In the cognitive domain, improvements were most robustly observed in verbal and short-term memory function. In line with xanomeline, the response to KarXT treatment in schizophrenia demonstrated a lower score on the positive and negative syndrome scale, clinical global impressions scale-improvement, and Marder negative symptoms scale [72].
Two studies also examined the effect of RS-86 on sleep parameters in schizophrenia patients compared to placebo [87, 96]. Similar to observations in individuals with depressive disorders, RS-86 significantly reduced REM latency in this population compared with placebo [87, 96].
Dementia/Alzheimer’s Disease
In total, five studies were included, investigating muscarinic-receptor-targeted interventions in cognitive and psychiatric symptoms of dementia. Among them, four studies included patients with mild to moderate AD, and one study included probable AD participants. Probable AD was diagnosed when a patient had cognitive gradual decline without a history of illness that could cause mental impairment without AD [97]. All studies were performed in the USA. The number of patients varied from 8 to 66, while two studies had 343 participants (age range 60–82 years, 57.5% females) [98, 99]. Trial durations ranged from 8 days to 24 weeks, and interventions included RS-86, Lu 25-109, and xanomeline tartrate. Data for outcome measures were analysed using intention-to-treat to prevent attrition bias. Participant characteristics and outcome interventions information are summarised in Tables 3 and 6.
Table 6.
Outcomes of dementia/Alzheimer’s disease
| Lead author, year | Study design | Interventions and comparator (dose/route of administration) | Adverse effects | Main outcome measures | Key findings | Retention rate (%) |
|---|---|---|---|---|---|---|
| Bodick (1997) [99] | 6-month, randomised, double-blind, placebo- controlled, parallel-group trial |
Intervention: Xanomeline Tartrate 25 mg (TID) 50 mg (TID) 75 mg (TID) Oral, 24 weeks Control: placebo |
Syncope, nausea, vomiting, increased salivation, increased diaphoresis, mild to moderate increase in hepatic and biliary transaminase enzyme |
ADAS-Cog CIBIC+, ADSS, NOSGER |
Xanomeline at highest dose of 75 mg significantly improved CIBIC+ (p = 0.01), NOSGER score (p = 0.03) In ADSS score, higher improvement (p < 0.002) was evident for vocal outbursts, suspiciousness, delusions, agitations and hallucinations No significant improvement was observed in ADAS-cog scale compared to placebo |
<30 |
| Bruno (1986) [101] | Double blind, placebo controlled, randomised |
Intervention: RS-86 Started at 0.5 mg/day Titrated up to 5 mg/day Maximum mean dose/day=4.6 mg (4–5 mg) 4 times a day 8 days oral Control: placebo Washout: 5 days |
Diaphoresis, hypersalivation |
Neuropsychological tests Story recall for immediate memory Word learning Dichotic listening Visual form of discrimination test Pictorial memory Recurring figures Reaction time |
No significant difference between RS-86 and placebo in any of the tasks | 100 |
| Hollander (1987) [100] | Double blind, cross-over, randomised, placebo-controlled |
Intervention: RS-86 Dose varies between patients till Maximum tolerated Dose range = 0.75–1.5 mg Oral, 2 weeks Control: placebo |
Chills, excessive sweating, flushing, depressed mood, prolongation of P-R interval on EKG, tremor, hypersalivation, and confusion | Cognitive and noncognitive symptoms using ADAS | No statistical significance difference was observed in any of the ADAS symptomatic subscales |
80 3 patients dropped out due to severe adverse events (syncope, abdominal distress, seizure) |
| Thal (2000) [102] | Multisite 6-month, randomised, double-blind, placebo-controlled, parallel group trial |
Intervention: Lu 25-109 25 mg (TID) 50 mg (TID) 100 mg (TID) oral 24 weeks Control: placebo |
Dizziness, nausea, diarrhoea, fatigue, sweating, anorexia, increased salivation, vomiting, loss of weight, and asthenia |
ADAS-Cog ADCS-ADL BEHAVE-AD |
No significant differences in any of the outcome measures compared with placebo |
61 Higher discontinuation rate in high dose group due to adverse effects |
| Veroff (1998) [98] | Multisite 6-month, randomized, double-blind, placebo- controlled, parallel-group trial |
Intervention: xanomeline tartrate 25 mg (TID) 50 mg (TID) 75 mg (TID) Oral, 24 weeks Control: placebo |
Not reported |
CNTB ADAS |
Xanomeline significantly improved CNTB summary score (p < 0.05), but not ADAS | 61 |
AD Alzheimer’s Disease, ADAS-Cog The Alzheimer's Disease Assessment Scale-Cognitive subscale, ADCS-ADL AD in basic and instrumental activities of daily living, ADSS AD symptomatology scale, BEHAVE-AD Behavioural Pathology in AD Rating Scale, CIBIC+ AD Cooperative Study-Clinical Global Impression of Change, CNTB Computerised Neuropsychological Test Battery, NOSGER Nurses' Observation Scale for Geriatric Patients
Two studies with RS-86, one assessing cognitive and psychiatric symptoms on the Alzheimer’s Disease Assessment Scale (ADAS) [100] and another one with neuropsychiatric tests including verbal memory, a visuospatial form of memory and attention [101] did not find a significant difference in any of the scales compared to placebo. One study investigated the efficacy of Lu25-109 using the activities of the daily living scale, behaviour symptom scale and cognition subscale of ADAS, and found no significant change [102]. Two large studies of medium quality assessed xanomeline tartrate. One study found a substantial difference in the neuropsychological test battery but not in the cognitive subscale of AD [98]. In another study, psychiatric symptoms were also assessed along with cognition, and the intervention group with the highest dose significantly improved BPSD compared to placebo and lower dose groups. At the same time, ADAS-cognition score was unaffected [99].
Anxiety Disorders
To date, only two clinical trials have examined the effect of muscarinic receptor-targeted interventions in anxiety disorders – one in people with panic disorder and one in people with social anxiety disorder [70, 103] (Tables 3 and 7). The sample size in the two studies was 12 and 66 participants, respectively (age range 18–55 years, 54% female). The first study found that biperiden was effective in reducing anxiety symptom severity in people with panic disorder against placebo [70]. In contrast, the second study showed that scopolamine had no effect on self-reported social anxiety disorder symptoms. However, scopolamine caused a significant reduction in skin conductance responses, which are a less subjective measure of anxiety levels. In addition, this study examined a combination of scopolamine and exposure therapy, where scopolamine augmented extinction in severely anxious participants, highlighting the importance of muscarinic receptors in anxiety-related behaviour [103]. The same study also showed that scopolamine increased the error rate in the mnemonic similarity task at the dose of 0.5 mg, suggesting impaired cognition.
Table 7.
Outcomes of anxiety disorders
| Lead author and year | Study design | Interventions and comparisons (dose/route of administration) | Adverse effects | Main outcome measures | Key findings | Retention rate (%) |
|---|---|---|---|---|---|---|
| Battaglia (2001) [70] | Randomised, double-blind, cross-over |
Intervention: biperiden hydrochloride 4 mg Oral, once Control: placebo Washout: 48 h |
Not available |
VASA Panic symptoms list-III (PSL-III-R) |
Biperiden significantly reduced CO2 exaggerated %VASA (p ≤ 0.003) and %PSL-III-R (p ≤ 0.005) compared to placebo |
75 |
| Craske (2019) [103] | Double-blind, randomised, placebo-controlled |
Intervention: scopolamine 0.5 mg, 0.6 mg Intranasal Once Control: placebo |
Drowsiness 3 patients |
Paired associate learning (cue-context learning) MST SUDS |
Not significant The difference was observed in SUDS during extinction and paired-associate learning task across groups, while errors were significantly increased in MST at 0.5 mg scopolamine (p < 0.05) |
90.90 |
MST mnemonic similarity task, SUDS subjective units of distress scale, VASA visual analogue scale of anxiety
Meta-Analysis
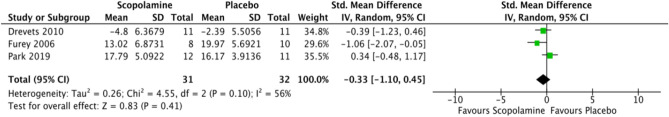
Five studies were incorporated in the meta-analysis of the antidepressant effect of scopolamine in a combined cohort of MDD and BP patients (Fig. 3). Three of the studies were crossover [74, 75, 81], and two were parallel design [80, 82]. Due to the possible carry-over effects of scopolamine, we used the last observation of pre-crossover data (following the 3rd scopolamine administration). In the parallel study, we used the 4th observation to equalise the observation parameters with crossover trials. In all four studies mentioned above, outcome measures were available after three infusion days. The results available for the fifth study were at a different time point (after 28 days), so we performed a sub-group analysis. Overall, a non-significant anti-depressant effect was observed for studies of scopolamine compared with placebo (5 studies, N = 147) (SMD = − 0.53; 95% CI = [− 1.33, 0.27]; z = 1.29, p = 0.20) with substantial heterogeneity (I2 = 80%). However, when sub-group analysis was performed, all studies with a short duration of 3 days showed a significant anti-depressant effect (4 studies, N = 103) (SMD = −0.81; 95% CI = [− 1.57, − 0.06]; z = 2.12, p = 0.03) with substantially higher heterogeneity (I2 = 67%). This became non-significant when including the study with 28 days of observation (1 study, N = 44) (SMD = 0.58; 95% CI = [− 0.02, 1.19]; z = 1.88, p = 0.06). Within the short-term duration studies (symptoms measured after 3 days), leave-one-out sensitivity analyses indicated significant changes in inferences leaving out study 1 [75] and study 3 [80], whereby removal of these studies increased the p-value (p = 0.11).
Fig. 3.
Forest plot of the scopolamine’s antidepressant effect in patients with mood disorders. There was no significant overall antidepressant effect (p = 0.20). CI confidence interval, IV inverse variance, SD standard deviation
In contrast, scopolamine had no overall effect on anxiety in individuals with mood disorders (3 studies, SMD = − 0.33; 95% CI = [− 1.10, 0.45]; z = 0.83, p = 0.41), and moderate heterogeneity (I2 = 56%) (Fig. 4). Leave-one-out sensitivity analyses showed that omitting study 3 [81] decreased the p-value significantly (from 0.41 to 0.04). Using GRADE analysis, we rated the certainty of scopolamine’s antidepressant and anxiolytic effect as “very low” in people with mood disorders.
Fig. 4.
Forest plot of the scopolamine's antianxiety effect in patients with mood disorders. There was no significant difference was found between the two treatment arms (p = 0.41) for the anxiolytic effect of scopolamine. CI confidence interval, IV inverse variance, SD standard deviation
Reported Adverse Events
Adverse events were most commonly reported with scopolamine treatment, even at a low dose (0.004 mg/kg). Common adverse events were dry mouth, dry skin, dry mucus membranes, constipation, drowsiness, blurred vision, light-headedness, dizziness, hypotension, fatigue, feeling drugged [74–76, 80, 81, 103]. At higher doses (0.5 mg/kg), scopolamine also showed a reduction in pulse and increased psychiatric symptoms such as visual hallucinations, disorganised speech, and cognitive impairments at the acute drug response phase [69]. Only two studies reported adverse events during biperiden treatment, including mild dry mouth (also reported in the placebo group) and constipation [84, 94]. In studies of primary psychotic disorders, xanomeline increased salivation, diarrhoea, nausea, vomiting, gastrointestinal distress, dizziness, liver function, sweating, and flatulence, likely through the activation of peripheral muscarinic acetylcholine receptors [71]. However, a few patients from the placebo group also showed some gastric disturbances. When xanomeline was combined with trospium (KarXT), side effects were minimal but included nausea, constipation, dry mouth, vomiting and dyspepsia [72]. No severe adverse incidents were stated in any of the studies. Increased salivation was the only adverse effect reported with oral RS-86 administration in MDD patients [104]. In contrast, side effects were higher in AD patients, including, diaphoresis, hypersalivation, depressed mood, confusion, prolonged P-R interval and tremors [100].
Discussion
This systematic review and meta-analysis examined the therapeutic efficacy of muscarinic-targeted interventions for neuropsychiatric disorders. Here, we reviewed 33 clinical trials to examine their effectiveness in treating mood, primary psychotic, dementia, or anxiety disorders. The most common medications tested for mood disorders were the non-selective muscarinic antagonist scopolamine, and biperiden, an M1 mAChR preferring antagonist. Meta-analysis revealed that scopolamine did not show significant improvement in depressive symptoms compared to placebo. For schizophrenia, most studies used biperiden, followed by the M1/M4 mAChR preferring agonist xanomeline and the antagonist scopolamine. Xanomeline significantly reduced positive and negative symptoms; however, safety was improved when combined with a peripheral mAChR antagonist trospium (KarXT). Neither scopolamine nor repeated-dose biperiden improved symptoms in people with schizophrenia. In patients with AD, treatments included RS-86, xanomeline tartrate and Lu 25-109; only xanomeline significantly improved psychiatric and behavioural symptoms of AD. No conclusive findings can be drawn for anxiety disorders as only two clinical trials were available, and neither examined the same compound.
Mood Disorders
The most substantial evidence of efficacy for muscarinic-targeted interventions was observed in mood disorders. Eight RCTs reported scopolamine's efficacy relative to placebo in patients with mood disorders regardless of diagnosis. The effect was rapid as symptom alleviation was seen 3–5 days following the first scopolamine administration [74, 105]. Compared to typical antidepressants, which can take several weeks to become effective, this time span is beneficial to individuals with depression [74]. The rapid antidepressant effect of scopolamine was observed in both sexes; however, one study showed the magnitude was higher in women than men, which may be driven by renal elimination rate. Although there are no studies examining pharmacokinetic differences of scopolamine in men versus women, results from drugs with weak anticholinergic activity such as amantadine and digoxin suggest slower clearance in females compared to males, due to sex differences in renal tubule secretion by organic cation transporters [106]. A second possibility is p-glycoprotein transporter polymorphisms may lead to variability in efficacy [76, 107]. This potential difference may also be explained by sex differences observed in the A/T 1890 SNP in CHRM2 [108].
One study documented substantial symptom improvement when scopolamine was combined with the selective serotonin reuptake inhibitor (SSRI) citalopram, rather than citalopram alone, despite no evidence of interactions between SSRI and anticholinergic agents [80]. On the other hand, scopolamine failed to alleviate depressive symptoms in treatment-resistant patients with higher severity Montgomery-Åsberg Depression Rating Scale scores [81]. Three reasons have been suggested to explain treatment-resistance [109]. First, pathophysiological adaptations are more serious, so standard doses are ineffective. Second, progressive neurobiological changes alter the diagnosis. For example, a patient initially presented with MDD, and subsequently BP or worsening symptoms emerged. A drug targeting the initial diagnosis may not generate an appropriate therapeutic response in such cases. Third, different underlying neurobiological mechanisms may exist between treatment-responsive and treatment-resistant patients. All the studies from Furey and colleagues displayed scopolamine's antidepressant effect at a low dose (0.004 mg) [74–79]. In contrast, Newhouse et al. (1988) showed no significant difference in Beck depression inventory score at a higher dose range (0.1–0.5 mg) [69]. One plausible reason for this difference is pseudo-resistance, where some treatments display a bell-shaped dose-response curve. Pseudo-resistance can be defined as a patient being non-responsive to the treatment, but the criteria for treatment resistance are not fulfilled [109].
Lastly, the antidepressant effect of scopolamine was non-significant in the meta-analysis, and this result contradicts the findings from another review. From the sub-group analysis, it was also evident that significant alleviation of depressive symptoms is observed after 3 days; however, after 28 days it is no longer significant [110]. Various reasons suggest extreme caution should be taken before scopolamine is recommended as a therapeutic agent. The latter review included different papers which had the same datasets, and they also mentioned this as the biggest limitation. We excluded those studies because the number of repeated participants is much higher than the newly enrolled participants. For example, in the study with the highest sample size (N = 62) [78], data from 52 participants were previously reported [74–76]. Second, the significant antidepressant effect from short-duration studies of scopolamine did not survive our sensitivity analyses, which were not performed by McCaffery and colleagues. Third, GRADE analysis suggested a “very low” certainty of the evidence. Fourth, most scopolamine trials were conducted by the same group of authors. Lastly, the majority of studies were either acute or short-term problems (< 6 weeks); it should be noted that chronic use of scopolamine shows abuse liability [111] and can have significant impact on memory [112]. Therefore, while these data suggest scopolamine may help reduce depressive symptoms in individuals with mood disorders, the dose and route of administration need to be optimised to obtain a clinical response that can produce beneficial results without limiting on-target side effects. More independent replication with a larger sample size would be required to confirm the findings. In the future, novel allosteric modulators, which selectively target central M2 or M3 mAChR with negligible peripheral side effects might show clinical effectiveness in patients with mood disorders [113].
In addition, two RCTs examined the effectiveness of biperiden. Acute biperiden administration showed a significant antidepressant effect. However, a 6-week trial did not demonstrate the substantial antidepressant effect of biperiden compared with placebo [84]. From a clinical perspective, however, long-term M1 receptor antagonism is likely to be problematic, as detailed below. Results from RS-86 studies showed reduction in REM-latency and increase in REM-density, suggesting a possible role of muscarinic receptors in sleep disturbances accompanied by MDD.
Primary Psychotic Disorders
Muscarinic targeted inventions showed promising results in schizophrenia and psychotic disorders, particularly alleviating positive and negative symptoms. However, there were not enough RCTs to perform a meta-analysis, highlighting the need for additional trials to ascertain the efficacy of such interventions fully. Preliminary data from studies using biperiden suggest that antagonism of the M1 receptor produces mild to moderate impairment in learning and memory processes in subjects with primary psychotic disorders [92, 93]. As mentioned, biperiden is an M1 mAChR preferring antagonist, and cognitive impairment results suggest that down-regulation of the M1 receptor could be a significant contributor to cognitive symptoms of schizophrenia. Although scopolamine has been used to generate “cognitive dysfunction”, it has been observed that, along with cognitive dysfunction, scopolamine also produces impairment in attention and motivation [114]. This effect is due to the non-selective nature of scopolamine. Based on these findings, it was proposed that scopolamine could be used to model cognition dysfunction in AD. Notably, biperiden could be a “cleaner” way to develop a “cholinergic deficit model of cognitive dysfunction” [114]. Previous literature indicates that cognitive impairment may be a vulnerability marker for psychotic disorders as it is also observed in healthy people with high genetic risk [115]. On the contrary to biperiden, xanomeline, an M1/M4 receptor orthosteric agonist, showed significant improvement in positive and negative symptoms of schizophrenia [71]. However, the therapeutic use of xanomeline is limited due to severe gastric side effects, driven by its potential to bind to peripheral muscarinic receptors. The combination of xanomeline with trospium (KarXT) shows a similar therapeutic potential of xanomeline in treating psychotic disorders, with minor side effects compared to xanomeline alone, due to the ability of trospium to block peripheral muscarinic receptors without crossing the blood-brain barrier and thereby alleviate gastrointestinal side effects [72]. Indeed, KarXT has recently shown positive results in the Phase 3 EMERGENT-2 Trial (see https://investors.karunatx.com/news-releases/news-release-details/karuna-therapeutics-announces-positive-results-phase-3-emergent). Based on the KarXT results, M1/M4 receptor-targeted treatments appear to be a novel potential therapeutic approach in primary psychotic disorder patients. In addition to KarXT, a Phase 1b clinical trial is ongoing for the positive allosteric modulator of M4 receptor, emraclidine in patients with schizophrenia and is expected to finish by 2024 (NCT05227703, NCT05227690). Notably, when targeting the orthosteric site, it is essential to consider that drug response to the orthosteric agonist of the M1 receptor was altered in the subgroup of patients with MRDS phenotype. Still, no difference was observed in response to an allosteric agonists, suggesting that positive allosteric modulators with bias signalling may provide a better approach for all types of schizophrenic patients [116]. In this regard, there are several preclinical studies that support positive allosteric modulators of M4 receptors as novel anti-psychotics [117, 118]. For RS-86 in schizophrenia, a significant decline in REM latency was observed, which is similar to the depression [87, 96], while the results for REM density are the opposite. The authors speculated that this REM latency reduction is due to subpopulations of people with schizophrenia also having secondary depression. In a subsequent study, no significant difference emerged when samples were split with and without secondary depression [87, 96], which suggests that REM latency measurement alone is not a sufficient marker to conclude any specific neuropsychiatric disorder.
Dementia/Alzheimer’s Disease
RS-86 was ineffective for cognition and psychiatric symptoms in patients with mild to moderate AD. Even the highest tolerable dose of 10 mg showed no significant improvement [119]. Similar to RS-86, Lu 25-109 failed to produce a significant difference in cognitive or behavioural symptoms of AD; rather, symptoms worsened at the highest dose of 300 mg, relative to placebo. A potential reason could be that Lu 25-109 also acts as an M2/M3 receptor antagonist, leading to a higher discontinuation rate [102]. There is evidence that xanomeline tartrate (75 mg, TID) is effective for psychiatric symptoms [99]. The results were equivocal for cognitive symptoms as improvement was observed in the neuropsychological test battery but not from the ADAS-cognition subscale [98]. Also, there was a difference in MMSE scores across treatment groups during baseline measurement, which can be a confounding factor for measuring actual treatment effect. The primary concern across most of the dementia studies is the lack of assessor’s blinding information.
In summary, except for xanomeline, no other muscarinic receptor agonist with a higher selectivity for the M1 receptor produced significant improvement in behavioural or psychiatric symptoms of dementia. These results are in line with other previous trials with oxotremorine, pilocarpine and RS-86 [102]. Favourable results from xanomeline suggest a potential role of the M4 receptor in behavioural and psychiatric disturbances associated with dementia. The hypothesis behind antipsychotic efficacy is that activating the M4 receptor reduces hyperdopaminergic activity, an effect confirmed in patients with schizophrenia [59]. Xanomeline may also attenuate the beta-amyloid plaque burden by increasing the secretion of non-amyloidogenic form of precursor protein and may thereby slow down the disease progression [99].
Anxiety Disorders
Results concerning anxiety disorders are equivocal. Scopolamine treatment did not significantly differ in self-reported distress in public speaking compared to placebo [103]. In contrast, scopolamine administration reduced anxiety rating scale scores in people with mood disorders relative to placebo [74]. While these preliminary studies show some promising results, no conclusions can be drawn, and additional studies are needed to determine the role of muscarinic receptors in anxiety disorders. Preclinical studies point out the possible involvement of the M5 receptor in anxiety [63].
Strengths and Limitations
In this systematic review, all included studies were randomised (except one pseudo-randomised study), placebo-controlled and double-blind studies. These are considered to produce highest quality of evidence for medical research. A recent review showed a role for cholinergic therapeutics in depressive/manic symptoms [110]. However, they included interventions that can also target nicotinic receptors. So, to our knowledge, this is the first systematic review with a registered protocol assessing the exclusive role of muscarinic receptor-targeted interventions in neuropsychiatric disorders. For risk of bias assessment, we used Cochrane ROB-2 software. Cochrane ROB-2 is a structured tool that helps assess bias in each domain of the study, such as trial design, conduct and reporting rather than overall RCT. To identify publication bias, we undertook sensitivity analyses. We also performed GRADE analysis for meta-analysis findings, a critical approach in assessing the certainty of evidence. A shortcoming in the available data is that only five studies were included for meta-analysis, so we cannot formally evaluate bias due to missing results (such as funnel plot generation) and meta-regression. However, sensitivity analyses allowed us to assess the robustness of the findings.
There are critical limitations in the literature reviewed in the present study. First, sample sizes were small (N < 30) in most included articles; caution is required as underpowered studies may increase error and reduce reliability. Second, numerous studies used different doses and routes of administration. While many studies focused on repeated dosing, some tested acute administration. Acute treatment with biperiden showed improvement in depressive symptoms, and opposite to that, studies lasting 6 weeks failed to see this same efficacy, highlighting the need for optimal treatment protocols. Third, most studies did not report the ethnicity of participants, which can be a limiting factor for the generalisability of findings [120]. Lastly, active comparators/controls are lacking in a number of studies. For instance, in dementia studies, higher rates of adverse events in the treatment but not the placebo condition may have unblinded both participants and assessors; thus, having no active placebo can compromise the integrity of the trial [98, 99].
Conclusion and Future Directions
While the results are not yet definitive, findings on muscarinic receptor-targeted interventions in several mental disorders are promising in efficacy and safety, specifically in treating schizophrenia, mood disorders such as MDD and BP and behavioural and psychiatric symptoms of AD. However, several methodological discrepancies question the ability to generalise findings. The most favourable evidence is the combination of M1/M4 agonist xanomeline and trospium (although inconclusive for meta-analysis) in schizophrenia because of a higher safety profile. Weak evidence also tentatively suggests a role for scopolamine in mood disorders, more specifically major depressive and bipolar disorders. For BPSD only xanomeline tartare showed significant improvement, but more evidence is required to validate the results.
In conclusion, the major challenge with orthosteric muscarinic receptor-targeted interventions is a wide range of peripheral adverse effects thought to be mediated via binding to M2/M3 receptors. The orthosteric binding site of mAChR is remarkably conserved, making it challenging to develop subtype-selective interventions. However, many allosteric ligands with biased signalling pathways are in development [16]. Positive allosteric modulators are compounds that increase the co-bound orthosteric pharmacological effect of the ligand. Allosteric modulators with biased signalling pathways can achieve subtype selectivity and be devoid of side effects (off-target or on-target), a key attribute for targeting mAChR in psychiatric disorders [121]. Comprehensive knowledge of pathways and their engagement in the disease could change the therapeutic use of muscarinic targeted interventions. Despite representing a critical target for neuropsychiatric disorders, most of the included studies in this review were less contemporary and receptor non-selective, which makes it difficult to predict clinical effectiveness. In future studies, more subtype-selective interventions are needed to establish clinical effectiveness with limited side effects.
Acknowledgements
Graphical abstract was generated using biorender.com.
Declarations
Funding
SV was supported by Melbourne International Research Scholarship. LCW is supported by an NHMRC emerging leader fellowship (GNT2008344). AAG is supported by an NCCRED Seed Funding Grant and Medical Research Future Fund (MRFF). We acknowledge the Victorian State Government Operational Infrastructure Programme. Open Access funding enabled and organized by CAUL and its Member Institutions.
Conflict of interest
None.
Ethics approval
Not Applicable.
Consent to participate
Not Applicable.
Consent for publication
Not Applicable.
Availability of data and material
Not Applicable.
Code availability
Not Applicable.
Author’s contributions
AJL and LCW conceived the study; SV and AAG performed the analysis; all authors wrote the manuscript. We confirm that all authors have read and approved the final submitted manuscript and agree to be accountable for the work.
References
- 1.Mesulam M-M. Human brain cholinergic pathways. Prog Brain Res. 1990;84:231–241. doi: 10.1016/S0079-6123(08)60908-5. [DOI] [PubMed] [Google Scholar]
- 2.Everitt BJ, Robbins TW. Central cholinergic systems and cognition. Annu Rev Psychol. 1997;48(1):649–684. doi: 10.1146/annurev.psych.48.1.649. [DOI] [PubMed] [Google Scholar]
- 3.Aitta-Aho T, Hay YA, Phillips BU, Saksida LM, Bussey TJ, Paulsen O, et al. Basal forebrain and brainstem cholinergic neurons differentially impact amygdala circuits and learning-related behavior. Curr Biol. 2018;28(16):2557–69.e4. doi: 10.1016/j.cub.2018.06.064. [DOI] [PubMed] [Google Scholar]
- 4.Martinez-Gonzalez C, Bolam JP, Mena-Segovia J. Topographical organization of the pedunculopontine nucleus. Front Neuroanat. 2011;5:22. doi: 10.3389/fnana.2011.00022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Cachope R, Mateo Y, Mathur BN, Irving J, Wang H-L, Morales M, et al. Selective activation of cholinergic interneurons enhances accumbal phasic dopamine release: setting the tone for reward processing. Cell Rep. 2012;2(1):33–41. doi: 10.1016/j.celrep.2012.05.011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Peralta EG, Ashkenazi A, Winslow JW, Ramachandran J, Capon DJ. Differential regulation of PI hydrolysis and adenylyl cyclase by muscarinic receptor subtypes. Nature. 1988;334(6181):434–437. doi: 10.1038/334434a0. [DOI] [PubMed] [Google Scholar]
- 7.Peralta EG, Ashkenazi A, Winslow J, Smith D, Ramachandran J, Capon DJ. Distinct primary structures, ligand-binding properties and tissue-specific expression of four human muscarinic acetylcholine receptors. EMBO J. 1987;6(13):3923–3929. doi: 10.1002/j.1460-2075.1987.tb02733.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Offermanns S, Wieland T, Homann D, Sandmann J, Bombien E, Spicher K, et al. Transfected muscarinic acetylcholine receptors selectively couple to Gi-type G proteins and Gq/11. Mol Pharmacol. 1994;45(5):890–898. [PubMed] [Google Scholar]
- 9.Erskine D, Taylor J-P, Bakker G, Brown AJ, Tasker T, Nathan PJ. Cholinergic muscarinic M1 and M4 receptors as therapeutic targets for cognitive, behavioural, and psychological symptoms in psychiatric and neurological disorders. Drug Discov Today. 2019;24(12):2307–2314. doi: 10.1016/j.drudis.2019.08.009. [DOI] [PubMed] [Google Scholar]
- 10.Johnson CR, Kangas BD, Jutkiewicz EM, Bergman J, Coop A. Drug design targeting the muscarinic receptors and the implications in central nervous system disorders. Biomedicines. 2022;10(2):398. doi: 10.3390/biomedicines10020398. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.WHO. Fact sheet of mental disorders. 2021. https://www.who.int/news-room/fact-sheets/detail/mental-disorders. Accessed 17 Aug 2022.
- 12.Colorafi K, Vanselow J, Nelson T. Treating anxiety and depression in primary care: reducing barriers to access. Fam Pract Manag. 2017;24(4):11–16. [PubMed] [Google Scholar]
- 13.Singh R, Sadiq N. Cholinesterase inhibitors. StatPearls. Treasure Island: StatPearls Publishing; 2021. [PubMed] [Google Scholar]
- 14.Davies NM, Taylor G, Taylor AE, Martin RM, Munafò MR, Thomas KH. Cardiovascular and neuropsychiatric risks of varenicline: too good to be true? Lancet Respir Med. 2015;3(12):e39–e40. doi: 10.1016/S2213-2600(15)00468-3. [DOI] [PubMed] [Google Scholar]
- 15.Gauthier S. Cholinergic adverse effects of cholinesterase inhibitors in Alzheimer’s disease. Drugs Aging. 2001;18(11):853–862. doi: 10.2165/00002512-200118110-00006. [DOI] [PubMed] [Google Scholar]
- 16.Van der Westhuizen ET, Choy K, Valant C, McKenzie-Nickson S, Bradley SJ, Tobin AB, et al. Fine tuning muscarinic acetylcholine receptor signaling through allostery and bias. Front pharmacol. 2021;11:2217. doi: 10.3389/fphar.2020.606656. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.NSDUH . National survey on drug use and health, Center for behavioural health and statistics quality. Rockville: NSDUH; 2020. p. 2021. [Google Scholar]
- 18.Bains N, Abdijadid S. Major depressive disorder. StatPearls [Internet] StatPearls Publishing; 2021. [PubMed] [Google Scholar]
- 19.Geddes JR, Miklowitz DJ. Treatment of bipolar disorder. Lancet. 2013;381(9878):1672–1682. doi: 10.1016/S0140-6736(13)60857-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Sackeim HA. The definition and meaning of treatment-resistant depression. J Clin Psychiatry. 2001;62:10–17. [PubMed] [Google Scholar]
- 21.Prien RF, Kupfer DJ, Mansky PA, Small JG, Tuason VB, Voss CB, et al. Drug therapy in the prevention of recurrences in unipolar and bipolar affective disorders: report of the NIMH Collaborative Study Group comparing lithium carbonate, imipramine, and a lithium carbonate-imipramine combination. Arch Gen Psychiatry. 1984;41(11):1096–1104. doi: 10.1001/archpsyc.1983.01790220086014. [DOI] [PubMed] [Google Scholar]
- 22.Zhdanava M, Pilon D, Ghelerter I, Chow W, Joshi K, Lefebvre P, et al. The prevalence and national burden of treatment-resistant depression and major depressive disorder in the United States. J Clin Psychiatry. 2021;82(2):29169. doi: 10.4088/JCP.20m13699. [DOI] [PubMed] [Google Scholar]
- 23.Rowntree DW, Nevin S, Wilson A. The effects of diisopropylfluorophosphonate in schizophrenia and manic depressive psychosis. J Neurol Neurosurg Psychiatry. 1950;13(1):47. doi: 10.1136/jnnp.13.1.47. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Janowsky D, El-Yousef MK, Davis J, Hubbard B, Sekerke HJ. Cholinergic reversal of manic symptoms. Lancet. 1972;299(7762):1236–1237. doi: 10.1016/s0140-6736(72)90956-7. [DOI] [PubMed] [Google Scholar]
- 25.Witkin JM, Smith JL, Golani LK, Brooks EA, Martin AE. Involvement of muscarinic receptor mechanisms in antidepressant drug action. Adv Pharmacol. 2020;89:311–356. doi: 10.1016/bs.apha.2020.03.003. [DOI] [PubMed] [Google Scholar]
- 26.Cannon DM, Carson RE, Nugent AC, Eckelman WC, Kiesewetter DO, Williams J, et al. Reduced muscarinic type 2 receptor binding in subjects with bipolar disorder. Arch Gen Psychiatry. 2006;63(7):741–747. doi: 10.1001/archpsyc.63.7.741. [DOI] [PubMed] [Google Scholar]
- 27.Wang JC, Hinrichs AL, Stock H, Budde J, Allen R, Bertelsen S, et al. Evidence of common and specific genetic effects: association of the muscarinic acetylcholine receptor M2 (CHRM2) gene with alcohol dependence and major depressive syndrome. Hum Mol Genet. 2004;13(17):1903–1911. doi: 10.1093/hmg/ddh194. [DOI] [PubMed] [Google Scholar]
- 28.Gibbons A, Scarr E, McLean C, Sundram S, Dean B. Decreased muscarinic receptor binding in the frontal cortex of bipolar disorder and major depressive disorder subjects. J Affect Disord. 2009;116(3):184–191. doi: 10.1016/j.jad.2008.11.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Dean B, Scarr E. Possible involvement of muscarinic receptors in psychiatric disorders: a focus on schizophrenia and mood disorders. Curr Mol Med. 2015;15(3):253–264. doi: 10.2174/1566524015666150330144821. [DOI] [PubMed] [Google Scholar]
- 30.Kessler RC, Birnbaum H, Demler O, Falloon IR, Gagnon E, Guyer M, et al. The prevalence and correlates of nonaffective psychosis in the National Comorbidity Survey Replication (NCS-R) Biol Psychiatry. 2005;58(8):668–676. doi: 10.1016/j.biopsych.2005.04.034. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Wu EQ, Shi L, Birnbaum H, Hudson T, Kessler R. Annual prevalence of diagnosed schizophrenia in the USA: a claims data analysis approach. Psychol Med. 2006;36(11):1535–1540. doi: 10.1017/S0033291706008191. [DOI] [PubMed] [Google Scholar]
- 32.Desai PR, Lawson KA, Barner JC, Rascati KL. Estimating the direct and indirect costs for community-dwelling patients with schizophrenia. J Pharm Health Serv Res. 2013;4(4):187–194. doi: 10.1111/jphs.12027. [DOI] [Google Scholar]
- 33.Clissold M, Crowe SF. Comparing the effect of the subcategories of atypical antipsychotic medications on cognition in schizophrenia using a meta-analytic approach. J Clin Exp Neuropsychol. 2019;41(1):26–42. doi: 10.1080/13803395.2018.1488952. [DOI] [PubMed] [Google Scholar]
- 34.Fusar-Poli P, Papanastasiou E, Stahl D, Rocchetti M, Carpenter W, Shergill S, et al. Treatments of negative symptoms in schizophrenia: meta-analysis of 168 randomized placebo-controlled trials. Schizophr Bull. 2015;41(4):892–899. doi: 10.1093/schbul/sbu170. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Volavka J, Czobor P, Sheitman B, Lindenmayer J-P, Citrome L, McEvoy JP, et al. Clozapine, olanzapine, risperidone, and haloperidol in the treatment of patients with chronic schizophrenia and schizoaffective disorder. Am J Psychiatry. 2002;159(2):255–262. doi: 10.1176/appi.ajp.159.2.255. [DOI] [PubMed] [Google Scholar]
- 36.Pardiñas AF, Smart SE, Willcocks IR, Holmans PA, Dennison CA, Lynham AJ, et al. Interaction testing and polygenic risk scoring to estimate the association of common genetic variants with treatment resistance in schizophrenia. JAMA Psychiat. 2022;79(3):260–269. doi: 10.1001/jamapsychiatry.2021.3799. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Crook JM, Tomaskovic-Crook E, Copolov DL, Dean B. Decreased muscarinic receptor binding in subjects with schizophrenia: a study of the human hippocampal formation. Biol Psychiatry. 2000;48(5):381–388. doi: 10.1016/s0006-3223(00)00918-5. [DOI] [PubMed] [Google Scholar]
- 38.Crook JM, Tomaskovic-Crook E, Copolov DL, Dean B. Low muscarinic receptor binding in prefrontal cortex from subjects with schizophrenia: a study of Brodmann’s areas 8, 9, 10, and 46 and the effects of neuroleptic drug treatment. Am J Psychiatry. 2001;158(6):918–925. doi: 10.1176/appi.ajp.158.6.918. [DOI] [PubMed] [Google Scholar]
- 39.Dean B, McLeod M, Keriakous D, McKenzie J, Scarr E. Decreased muscarinic1 receptors in the dorsolateral prefrontal cortex of subjects with schizophrenia. Mol Psychiatry. 2002;7(10):1083–1091. doi: 10.1038/sj.mp.4001199. [DOI] [PubMed] [Google Scholar]
- 40.Scarr E, Sundram S, Keriakous D, Dean B. Altered hippocampal muscarinic M4, but not M1, receptor expression from subjects with schizophrenia. Biol Psychiatry. 2007;61(10):1161–1170. doi: 10.1016/j.biopsych.2006.08.050. [DOI] [PubMed] [Google Scholar]
- 41.Raedler TJ, Knable MB, Jones DW, Urbina RA, Gorey JG, Lee KS, et al. In vivo determination of muscarinic acetylcholine receptor availability in schizophrenia. Am J Psychiatry. 2003;160(1):118–127. doi: 10.1176/appi.ajp.160.1.118. [DOI] [PubMed] [Google Scholar]
- 42.Marchlewski MB. Anticholinergic syndrome: avoiding misdiagnosis. Thorofare: SLACK Incorporated; 1994. pp. 22–24. [DOI] [PubMed] [Google Scholar]
- 43.Ch’ng SS, Walker AJ, McCarthy M, Le T-K, Thomas N, Gibbons A, et al. The impact of removal of ovarian hormones on cholinergic muscarinic receptors: examining prepulse inhibition and receptor binding. Brain Sci. 2020;10(2):106. doi: 10.3390/brainsci10020106. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Dean B, Hopper S, Conn PJ, Scarr E. Changes in BQCA allosteric modulation of [3H] NMS binding to human cortex within schizophrenia and by divalent cations. Neuropsychopharmacology. 2016;41(6):1620–1628. doi: 10.1038/npp.2015.330. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Bubser M, Bridges TM, Dencker D, Gould RW, Grannan M, Noetzel MJ, et al. Selective activation of M4 muscarinic acetylcholine receptors reverses MK-801-induced behavioral impairments and enhances associative learning in rodents. ACS Chem Neurosci. 2014;5(10):920–942. doi: 10.1021/cn500128b. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Gould RW, Grannan MD, Gunter BW, Ball J, Bubser M, Bridges TM, et al. Cognitive enhancement and antipsychotic-like activity following repeated dosing with the selective M4 PAM VU0467154. Neuropharmacology. 2018;128:492–502. doi: 10.1016/j.neuropharm.2017.07.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.WHO. Dementia Fact sheet. 2021. https://www.who.int/news-room/fact-sheets/detail/dementia. Accessed 15 Aug 2022.
- 48.Steinberg M, Shao H, Zandi P, Lyketsos CG, Welsh-Bohmer KA, Norton MC, et al. Point and 5-year period prevalence of neuropsychiatric symptoms in dementia: the Cache County Study. Int J Geriatr Psychiatry. 2008;23(2):170–177. doi: 10.1002/gps.1858. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Müller-Spahn F. Behavioral disturbances in dementia. Dialogues Clin Neurosci. 2022 doi: 10.31887/DCNS.2003.5.1/fmuellerspahn. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Cloak N, Al Khalili Y. Behavioral and psychological symptoms in dementia. 2019.Bookshelf ID: NBK551552. (PMID: 31855379). [PubMed]
- 51.Holt S, Schmiedl S, Thürmann PA. Potentially inappropriate medications in the elderly: the PRISCUS list. Dtsch Arztebl Int. 2010;107(31–32):543. doi: 10.3238/arztebl.2010.0543. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Deutsch JA. The cholinergic synapse and the site of memory. Science. 1971;174(4011):788–794. doi: 10.1126/science.174.4011.788. [DOI] [PubMed] [Google Scholar]
- 53.Inglis F. The tolerability and safety of cholinesterase inhibitors in the treatment of dementia. Int J Clin Pract Suppl. 2002;127:45–63. [PubMed] [Google Scholar]
- 54.Lai M, Lai OF, Keene J, Esiri M, Francis P, Hope T, et al. Psychosis of Alzheimer’s disease is associated with elevated muscarinic M2 binding in the cortex. Neurology. 2001;57(5):805–811. doi: 10.1212/wnl.57.5.805. [DOI] [PubMed] [Google Scholar]
- 55.Teaktong T, Piggott MA, Mckeith IG, Perry RH, Ballard CG, Perry EK. Muscarinic M2 and M4 receptors in anterior cingulate cortex: relation to neuropsychiatric symptoms in dementia with Lewy bodies. Behav Brain Res. 2005;161(2):299–305. doi: 10.1016/j.bbr.2005.02.019. [DOI] [PubMed] [Google Scholar]
- 56.Ma L, Seager MA, Wittmann M, Jacobson M, Bickel D, Burno M, et al. Selective activation of the M1 muscarinic acetylcholine receptor achieved by allosteric potentiation. Proc Natl Acad Sci. 2009;106(37):15950–15955. doi: 10.1073/pnas.0900903106. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Dwomoh L, Tejeda GS, Tobin AB. Targeting the M1 muscarinic acetylcholine receptor in Alzheimer’s disease. Neuronal Signal. 2022;6(1):NS20210007. doi: 10.1042/NS20210004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Scarpa M, Hesse S, Bradley SJ. M1 muscarinic acetylcholine receptors: a therapeutic strategy for symptomatic and disease-modifying effects in Alzheimer's disease? Adv Pharmacol. 2020;88:277–310. doi: 10.1016/bs.apha.2019.12.003. [DOI] [PubMed] [Google Scholar]
- 59.Moran SP, Maksymetz J, Conn PJ. Targeting muscarinic acetylcholine receptors for the treatment of psychiatric and neurological disorders. Trends Pharmacol Sci. 2019;40(12):1006–1020. doi: 10.1016/j.tips.2019.10.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.NCS-R. National Comorbidity Survey (NCS)-2017. Harvard Medical School, 2007; 2021. https://www.nimh.nih.gov/health/statistics/any-anxiety-disorder. Accessed 15 Aug 2022.
- 61.Small KM, Nunes E, Hughley S, Addy NA. Ventral tegmental area muscarinic receptors modulate depression and anxiety-related behaviors in rats. Neurosci Lett. 2016;616:80–85. doi: 10.1016/j.neulet.2016.01.057. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Mei L, Zhou Y, Sun Y, Liu H, Zhang D, Liu P, et al. Acetylcholine muscarinic receptors in ventral hippocampus modulate stress-induced anxiety-like behaviors in mice. Front Mol Neurosci. 2020;13:235. doi: 10.3389/fnmol.2020.598811. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Nunes EJ, Rupprecht LE, Foster DJ, Lindsley CW, Conn PJ, Addy NA. Examining the role of muscarinic M5 receptors in VTA cholinergic modulation of depressive-like and anxiety-related behaviors in rats. Neuropharmacology. 2020;171:108089. doi: 10.1016/j.neuropharm.2020.108089. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Int J Surg. 2021;88:105906. doi: 10.1136/bmj.n71. [DOI] [PubMed] [Google Scholar]
- 65.Palagini L, Baglioni C, Ciapparelli A, Gemignani A, Riemann D. REM sleep dysregulation in depression: state of the art. Sleep Med Rev. 2013;17(5):377–390. doi: 10.1016/j.smrv.2012.11.001. [DOI] [PubMed] [Google Scholar]
- 66.Sterne JA, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I, et al. RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ. 2019;366:l4898. doi: 10.1136/bmj.l4898. [DOI] [PubMed] [Google Scholar]
- 67.Ryan R. Cochrane Consumers and Communication Review Group: data synthesis and analysis. Cochrane Consumers and Communication Review Group. 2013.
- 68.Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, et al. Cochrane handbook for systematic reviews of interventions. Wiley; 2019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Newhouse PA, Sunderland T, Tariot PN, Weingartner H, Thompson K, Mellow AM, et al. The effects of acute scopolamine in geriatric depression. Arch Gen Psychiatry. 1988;45(10):906–912. doi: 10.1001/archpsyc.1988.01800340028004. [DOI] [PubMed] [Google Scholar]
- 70.Battaglia M, Bertella S, Ogliari A, Bellodi L, Smeraldi E. Modulation by muscarinic antagonists of the response to carbon dioxide challenge in panic disorder. Arch Gen Psychiatry. 2001;58(2):114–119. doi: 10.1001/archpsyc.58.2.114. [DOI] [PubMed] [Google Scholar]
- 71.Shekhar A, Potter WZ, Lightfoot J, Lienemann D, Pharm J, Dubé S, Mallinckrodt C, et al. Selective muscarinic receptor agonist xanomeline as a novel treatment approach for schizophrenia. Am J Psychiatry. 2008;165(8):1033–1039. doi: 10.1176/appi.ajp.2008.06091591. [DOI] [PubMed] [Google Scholar]
- 72.Brannan SK, Sawchak S, Miller AC, Lieberman JA, Paul SM, Breier A. Muscarinic cholinergic receptor agonist and peripheral antagonist for schizophrenia. N Engl J Med. 2021;384(8):717–726. doi: 10.1056/NEJMoa2017015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Segev A, Evans A, Hodsoll J, Whiskey E, Sheriff RS, Shergill S, et al. Hyoscine for clozapine-induced hypersalivation: a double-blind, randomized, placebo-controlled cross-over trial. Int Clin Psychopharmacol. 2019;34(2):101–107. doi: 10.1097/YIC.0000000000000251. [DOI] [PubMed] [Google Scholar]
- 74.Furey ML, Drevets WC. Antidepressant efficacy of the antimuscarinic drug scopolamine: a randomized, placebo-controlled clinical trial. Arch Gen Psychiatry. 2006;63(10):1121–1129. doi: 10.1001/archpsyc.63.10.1121. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Drevets WC, Furey ML. Replication of scopolamine's antidepressant efficacy in major depressive disorder: a randomized, placebo-controlled clinical trial. Biol Psychiatry. 2010;67(5):432–438. doi: 10.1016/j.biopsych.2009.11.021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Furey ML, Khanna A, Hoffman EM, Drevets WC. Scopolamine produces larger antidepressant and antianxiety effects in women than in men. Neuropsychopharmacology. 2010;35(12):2479–2488. doi: 10.1038/npp.2010.131. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Furey ML, Drevets WC, Hoffman EM, Frankel E, Speer AM, Zarate CA. Potential of pretreatment neural activity in the visual cortex during emotional processing to predict treatment response to scopolamine in major depressive disorder. JAMA Psychiat. 2013;70(3):280–290. doi: 10.1001/2013.jamapsychiatry.60. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Ellis JS, Zarate CA, Jr, Luckenbaugh DA, Furey ML. Antidepressant treatment history as a predictor of response to scopolamine: clinical implications. J Affect Disord. 2014;162:39–42. doi: 10.1016/j.jad.2014.03.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Furey ML, Drevets WC, Szczepanik J, Khanna A, Nugent A, Zarate CA. Pretreatment differences in BOLD response to emotional faces correlate with antidepressant response to scopolamine. Int J Neuropsychopharmacol. 2015 doi: 10.1093/ijnp/pyv028. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Khajavi D, Farokhnia M, Modabbernia A, Ashrafi M, Abbasi S-H, Tabrizi M, et al. Oral scopolamine augmentation in moderate to severe major depressive disorder: a randomized, double-blind, placebo-controlled study. J Clin Psychiatry. 2012;73(11):13538. doi: 10.4088/JCP.12m07706. [DOI] [PubMed] [Google Scholar]
- 81.Park L, Furey M, Nugent AC, Farmer C, Ellis J, Szczepanik J, et al. Neurophysiological changes associated with antidepressant response to ketamine not observed in a negative trial of scopolamine in major depressive disorder. Int J Neuropsychopharmacol. I. 2019;22(1):10–18. doi: 10.1093/ijnp/pyy051. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 82.Zhou J, Yang J, Zhu X, Zghoul T, Feng L, Chen R, et al. The effects of intramuscular administration of scopolamine augmentation in moderate to severe major depressive disorder: a randomized, double-blind, placebo-controlled trial. Ther Adv Psychopharmacol. 2020;10:2045125320938556. doi: 10.1177/2045125320938556. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Beckmann H, Moises H. The cholinolytic biperiden in depression. Arch Psychiatr Nervenkr. 1982;231(3):213–220. doi: 10.1007/BF00343291. [DOI] [PubMed] [Google Scholar]
- 84.Gillin JC, Lauriello J, Kelsoe JR, Rapaport M, Golshan S, Kenny WM, et al. No antidepressant effect of biperiden compared with placebo in depression: a double-blind 6-week clinical trial. Psychiatry Res. 1995;58(2):99–105. doi: 10.1016/0165-1781(95)02700-7. [DOI] [PubMed] [Google Scholar]
- 85.Kupfer D. REM latency: a psychobiologic marker for primary depressive disease. Biol Psychiatry. 1976;11(2):159–174. [PubMed] [Google Scholar]
- 86.Steiger A, Pawlowski M. Depression and sleep. Int J Mol Sci. 2019;20(3):607. doi: 10.3390/ijms20030607. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87.Riemann D, Gann H, Fleckenstein P, Hohagen F, Olbrich R, Berger M. Effect of RS 86 on REM latency in schizophrenia. Psychiatry Res. 1991;38(1):89–92. doi: 10.1016/0165-1781(91)90055-t. [DOI] [PubMed] [Google Scholar]
- 88.Riemann D, Berger M. Sleep, age, depression and the cholinergic REM induction test with RS 86. Prog Neuropsychopharmacol Biol Psychiatry. 1992;16(3):311–316. doi: 10.1016/0278-5846(92)90082-p. [DOI] [PubMed] [Google Scholar]
- 89.Riemann D, Hohagen F, Bahro M, Berger M. Sleep in depression: the influence of age, gender and diagnostic subtype on baseline sleep and the cholinergic REM induction test with RS 86. Eur Arch Psychiatry Clin Neurosci. 1994;243(5):279–290. doi: 10.1007/BF02191586. [DOI] [PubMed] [Google Scholar]
- 90.Poland RE, McCracken JT, Lutchmansingh P, Lesser IM, Tondo L, Edwards C, et al. Differential response of rapid eye movement sleep to cholinergic blockade by scopolamine in currently depressed, remitted, and normal control subjects. Biol Psychiatry. 1997;41(9):929–938. doi: 10.1016/S0006-3223(96)00183-7. [DOI] [PubMed] [Google Scholar]
- 91.Rao U, Lin K-M, Schramm P, Poland RE. REM sleep and cortisol responses to scopolamine during depression and remission in women. Int J Neuropsychopharmacol. 2004;7(3):265–274. doi: 10.1017/S1461145704004328. [DOI] [PubMed] [Google Scholar]
- 92.Bakker G, Vingerhoets C, Bloemen OJ, Sahakian BJ, Booij J, Caan MW, et al. The muscarinic M1 receptor modulates associative learning and memory in psychotic disorders. NeuroImage Clin. 2020;27:102278. doi: 10.1016/j.nicl.2020.102278. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93.Silver H, Geraisy N. Effects of biperiden and amantadine on memory in medicated chronic schizophrenic patients: a double-blind cross-over study. Br J Psychiatry. 1995;166(2):241–243. doi: 10.1192/bjp.166.2.241. [DOI] [PubMed] [Google Scholar]
- 94.Liang C-S, Ho P-S, Shen L-J, Lee W-K, Yang F-W, Chiang K-T. Comparison of the efficacy and impact on cognition of glycopyrrolate and biperiden for clozapine-induced sialorrhea in schizophrenic patients: a randomized, double-blind, crossover study. Schizophr Res. 2010;119(1–3):138–144. doi: 10.1016/j.schres.2010.02.1060. [DOI] [PubMed] [Google Scholar]
- 95.Silver H, Geraisy N. No difference in the effect of biperiden and amantadine on negative symptoms in medicated chronic schizophrenic patients. Biol Psychiatry. 1995 doi: 10.1016/0006-3223(95)00231-5. [DOI] [PubMed] [Google Scholar]
- 96.Riemann D, Hohagen F, Krieger S, Gann H, Müller WE, Olbrich R, et al. Cholinergic REM induction test: muscarinic supersensitivity underlies polysomnographic findings in both depression and schizophrenia. J Psychiatr Res. 1994;28(3):195–210. doi: 10.1016/0022-3956(94)90006-x. [DOI] [PubMed] [Google Scholar]
- 97.Lopez O, Becker J, Klunk W, Saxton J, Hamilton R, Kaufer D, et al. Research evaluation and diagnosis of probable Alzheimer’s disease over the last two decades: I. Neurology. 2000;55(12):1854–1862. doi: 10.1212/wnl.55.12.1854. [DOI] [PubMed] [Google Scholar]
- 98.Veroff AE, Bodick NC, Offen WW, Sramek JJ, Cutler NR. Efficacy of xanomeline in Alzheimer disease: cognitive improvement measured using the Computerized Neuropsychological Test Battery (CNTB) Alzheimer Dis Assoc Disord. 1998;12(4):304–312. doi: 10.1097/00002093-199812000-00010. [DOI] [PubMed] [Google Scholar]
- 99.Bodick NC, Offen WW, Levey AI, Cutler NR, Gauthier SG, Satlin A, et al. Effects of xanomeline, a selective muscarinic receptor agonist, on cognitive function and behavioral symptoms in Alzheimer disease. Arch Neurol. 1997;54(4):465–473. doi: 10.1001/archneur.1997.00550160091022. [DOI] [PubMed] [Google Scholar]
- 100.Hollander E, Davidson M, Mohs RC, Horvath TB, Davis BM, Zemishlany Z, et al. RS 86 in the treatment of Alzheimer's disease: cognitive and biological effects. Biol Psychiatry. 1987;22(9):1067–1078. doi: 10.1016/0006-3223(87)90049-7. [DOI] [PubMed] [Google Scholar]
- 101.Bruno G, Mohr E, Gillespie M, Fedio P, Chase TN. Muscarinic agonist therapy of Alzheimer's disease: a clinical trial of RS-86. Arch Neurol. 1986;43(7):659–661. doi: 10.1001/archneur.1986.00520070017009. [DOI] [PubMed] [Google Scholar]
- 102.Thal L, Forrest M, Loft H, Mengel H, Group L-S Lu 25–109, a muscarinic agonist, fails to improve cognition in Alzheimer’s disease. Neurology. 2000;54(2):421–521. doi: 10.1212/wnl.54.2.421. [DOI] [PubMed] [Google Scholar]
- 103.Craske MG, Fanselow M, Treanor M, Bystritksy A. Cholinergic modulation of exposure disrupts hippocampal processes and augments extinction: Proof-of-concept study with social anxiety disorder. Biol Psychiatry. 2019;86(9):703–711. doi: 10.1016/j.biopsych.2019.04.012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 104.Berger M, Riemann D, Höchli D, Spiegel R. The cholinergic rapid eye movement sleep induction test with RS-86: State or trait marker of depression? Arch Gen Psychiatry. 1989;46(5):421–428. doi: 10.1001/archpsyc.1989.01810050035006. [DOI] [PubMed] [Google Scholar]
- 105.Drevets WC, Bhattacharya A, Furey ML. The antidepressant efficacy of the muscarinic antagonist scopolamine: past findings and future directions. Adv Pharmacol. 2020;89:357–386. doi: 10.1016/bs.apha.2020.04.002. [DOI] [PubMed] [Google Scholar]
- 106.Trenaman SC, Bowles SK, Andrew MK, Goralski K. The role of sex, age and genetic polymorphisms of CYP enzymes on the pharmacokinetics of anticholinergic drugs. Pharmacol Res Perspect. 2021;9(3):e00775. doi: 10.1002/prp2.775. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 107.Uhr M, Grauer MT, Holsboer F. Differential enhancement of antidepressant penetration into the brain in mice with abcb1ab (mdr1ab) P-glycoprotein gene disruption. Biol Psychiatry. 2003;54(8):840–846. doi: 10.1016/s0006-3223(03)00074-x. [DOI] [PubMed] [Google Scholar]
- 108.Comings DE, Wu S, Rostamkhani M, McGue M, Iacono WG, MacMurray JP. Association of the muscarinic cholinergic 2 receptor (CHRM2) gene with major depression in women. Am J Med Genet. 2002;114(5):527–529. doi: 10.1002/ajmg.10406. [DOI] [PubMed] [Google Scholar]
- 109.Howes OD, Thase ME, Pillinger T. Treatment resistance in psychiatry: state of the art and new directions. Mol Psychiatry. 2021;27(1):1–15. doi: 10.1038/s41380-021-01200-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 110.McCaffrey U, Cannon DM, Hallahan B. The muscarinic-cholinergic system as a target in the treatment of depressive or manic episodes in bipolar disorder: A systematic review and meta-analysis. J Affect Disord. 2021;6:100235. doi: 10.1016/j.jadr.2021.100235. [DOI] [Google Scholar]
- 111.Luetje CM, Wooten J. Clinical manifestations of transdermal scopolamine addiction. Ear Nose Throat J. 1996;75(4):210–214. doi: 10.1177/014556139607500408. [DOI] [PubMed] [Google Scholar]
- 112.Lenz RA, Baker JD, Locke C, Rueter LE, Mohler EG, Wesnes K, et al. The scopolamine model as a pharmacodynamic marker in early drug development. Psychopharmacology. 2012;220(1):97–107. doi: 10.1007/s00213-011-2456-4. [DOI] [PubMed] [Google Scholar]
- 113.Scarr E. Muscarinic receptors in psychiatric disorders–can we mimic ‘health’? Neurosignals. 2009;17(4):298–310. doi: 10.1159/000231896. [DOI] [PubMed] [Google Scholar]
- 114.Blokland A. Cholinergic models of memory impairment in animals and man: scopolamine vs. biperiden. Behav Pharmacol. 2022;33(4):231–237. doi: 10.1097/FBP.0000000000000670. [DOI] [PubMed] [Google Scholar]
- 115.Reichenberg A. Cognitive impairment as a risk factor for psychosis. Dialogues Clin Neurosci. 2005;7(1):31. doi: 10.31887/DCNS.2005.7.1/areichenberg. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 116.Hopper S, Pavey GM, Gogos A, Dean B. Widespread changes in positive allosteric modulation of the muscarinic M1 receptor in some participants with schizophrenia. Int J Neuropsychopharmacol. 2019;22(10):640–650. doi: 10.1093/ijnp/pyz045. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 117.Yohn SE, Conn PJ. Positive allosteric modulation of M1 and M4 muscarinic receptors as potential therapeutic treatments for schizophrenia. Neuropharmacology. 2018;136:438–448. doi: 10.1016/j.neuropharm.2017.09.012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 118.Foster DJ, Wilson JM, Remke DH, Mahmood MS, Uddin MJ, Wess J, et al. Antipsychotic-like effects of M4 positive allosteric modulators are mediated by CB2 receptor-dependent inhibition of dopamine release. Neuron. 2016;91(6):1244–1252. doi: 10.1016/j.neuron.2016.08.017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 119.Mouradian MM, Mohr E, Williams JA, Chase TN. No response to high-dose muscarinic agonist therapy in Alzheimer's disease. Neurology. 1988;38(4):606–706. doi: 10.1212/wnl.38.4.606. [DOI] [PubMed] [Google Scholar]
- 120.Burkhard C, Cicek S, Barzilay R, Radhakrishnan R, Guloksuz S. Need for ethnic and population diversity in psychosis research. Schizophr Bull. 2021;47(4):889–895. doi: 10.1093/schbul/sbab048. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 121.Randáková A, Jakubík J. Functionally selective and biased agonists of muscarinic receptors. Pharmacol Res. 2021;169:105641. doi: 10.1016/j.phrs.2021.105641. [DOI] [PubMed] [Google Scholar]
- 122.Palacios JM, Bolliger G, Closse A, Enz A, Gmelin G, Malanowski J. The pharmacological assessment of RS 86 (2-ethyl-8-methyl-2, 8-diazaspiro-[4, 5]-decan-1, 3-dion hydrobromide). A potent, specific muscarinic acetylcholine receptor agonist. Eur J Pharmacol. 1986;125(1):45–62. doi: 10.1016/0014-2999(86)90082-8. [DOI] [PubMed] [Google Scholar]
- 123.Bymaster FP, Wong DT, Mitch CH, Ward JS, Calligaro DO, Schoepp DD, et al. Neurochemical effects of the M1 muscarinic agonist xanomeline (LY246708/NNC11-0232) J Pharmacol Exp Ther. 1994;269(1):282–289. [PubMed] [Google Scholar]
- 124.Bymaster FP, Whitesitt CA, Shannon HE, DeLapp N, Ward JS, Calligaro DO, et al. Xanomeline: a selective muscarinic agonist for the treatment of Alzheimer's disease. Drug Dev Res. 1997;40(2):158–170. doi: 10.1002/(SICI)1098-2299(199702)40:2<158::AID-DDR6>3.0.CO;2-K. [DOI] [Google Scholar]
- 125.Callegari E, Malhotra B, Bungay PJ, Webster R, Fenner KS, Kempshall S, et al. A comprehensive non-clinical evaluation of the CNS penetration potential of antimuscarinic agents for the treatment of overactive bladder. Br J Clin Pharmacol. 2011;72(2):235–246. doi: 10.1111/j.1365-2125.2011.03961.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 126.Bolden C, Cusack B, Richelson E. Antagonism by antimuscarinic and neuroleptic compounds at the five cloned human muscarinic cholinergic receptors expressed in Chinese hamster ovary cells. J Pharmacol Exp Ther. 1992;260(2):576–80. [PubMed]
- 127.Eltze M, Figala V. Affinity and selectivity of biperiden enantiomers for muscarinic receptor subtypes. Eur J Pharmacol. 1988;158(1–2):11–19. doi: 10.1016/0014-2999(88)90247-6. [DOI] [PubMed] [Google Scholar]
- 128.Chabicovsky M, Winkler S, Soeberdt M, Kilic A, Masur C, Abels C. Pharmacology, toxicology and clinical safety of glycopyrrolate. Toxicol Appl Pharmacol. 2019;370:154–169. doi: 10.1016/j.taap.2019.03.016. [DOI] [PubMed] [Google Scholar]
- 129.Sanchez C, Arnt J, Didriksen M, Dragsted N, Moltzen Lenz S, Matz J. In vivo muscarinic cholinergic mediated effects of Lu 25–109, a M1 agonist and M2/M3 antagonist in vitro. Psychopharmacology. 1998;137(3):233–240. doi: 10.1007/s002130050615. [DOI] [PubMed] [Google Scholar]
- 130.Wienrich M, Meier D, Ensinger H, Gaida W, Raschig A, Walland A, et al. Pharmacodynamic profile of the M1 agonist talsaclidine in animals and man. Life Sci. 2001;68(22–23):2593–2600. doi: 10.1016/s0024-3205(01)01057-8. [DOI] [PubMed] [Google Scholar]