Abstract
Introduction:
Obstructed hemivagina ipsilateral renal agenesis (OHVIRA) is a rare syndrome with limited data on both treatment and postoperative sequelae, specifically of ectopic ureters to the vagina.
Case Description:
This case study describes a 22-year-old patient with OHVIRA syndrome presenting with pelvic pain and drainage from a chronic vaginal abscess secondary to a remnant distal ectopic ureter after nephrectomy and proximal ureterectomy. Imaging was significant for a right paravaginal abscess. Previously, the patient was treated with conservative therapy and on presentation her evaluation confirmed a right paravaginal abscess. She subsequently underwent a robot-assisted incision and drainage of the paravaginal abscess and excision of the remnant distal ectopic ureter. She did well postoperatively without recurrence.
Discussion:
We discuss the successful surgical technique used to identify and excise a paravaginal abscess. We also highlight the unique anatomy of a patient with OHVIRA syndrome. Lastly, we underline the importance of a complete resection of an ectopic ureter to the vagina at the time of nephrectomy, given the potential risk of ascending chronic infection and recurrent abscess formation.
Keywords: Ascending infection, OHVIRA syndrome, Ureteral stump
INTRODUCTION
Herlyn-Wurner-Wunderlich or obstructed hemivagina ipsilateral renal agenesis (OHVIRA), is a rare syndrome first described in 1922.1 It has an estimated incidence of 00.1 – 3.8%.1,2 The overall incidence of Mullerian anomalies is 2 – 3%, with 0.16 – 10% associated with OHVIRA syndrome.2 The diagnosis is made in peripubescent females with abdominopelvic pain, pelvic mass, or vaginal drainage due to an obstructed hemihematocolpos.3–6 The syndrome is characterized by uterus didelphys, unilateral blind hemivagina, and ipsilateral renal agenesis; however, other urologic anomalies can be seen, such as a dysplastic or pelvic kidney and/or an ectopic ureter.7,8 The overall incidence of an ectopic ureter is unknown but is estimated to be approximately 1:1900 to 1:4000 in the general population.9 When an ectopic ureter is present in the setting of a dysplastic kidney, the kidney and ureter are typically removed due to the risk of significant drainage into the ipsilateral hemivagina after a vaginal septoplasty.1 OHVIRA syndrome with an ectopic ureter is an uncommon anomaly limiting the understanding of post-treatment sequelae. Our goal is to bring attention to a complication which may follow a ureterectomy and remnant ectopic ureter, and our surgical approach to treatment.
CASE DESCRIPTION
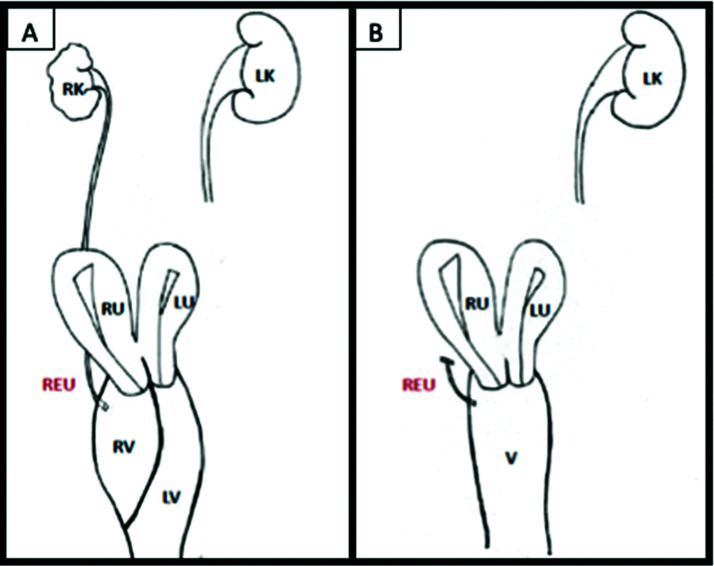
At the age of 12, a previously healthy female first presented with severe abdominopelvic pain four months after menarche. Multiple imaging modalities at differing times were significant for a uterus didelphys with obstructed hemivagina and dysplastic right kidney. Follow up imaging would show an ectopic ureter inserting into the right hemivagina. Over 10 years, she underwent a laparoscopic right nephrectomy with proximal ureterectomy (Figure 1), a transverse vaginal septoplasty, hysteroscopic polypectomy of her right uterus, cystoscopy, in addition to antibiotic and drain placement for recurrent vaginal drainage.
Figure 1.
(A) Pre-operative anatomy, (B) Post-operative anatomy. Left kidney (LK), Right dysplastic kidney (RK), Right ectopic ureter (REU), Right uterine horn (RU), Left uterine horn (LU), Right hemivagina (RV), Left hemivagina (LV), Vagina (V).
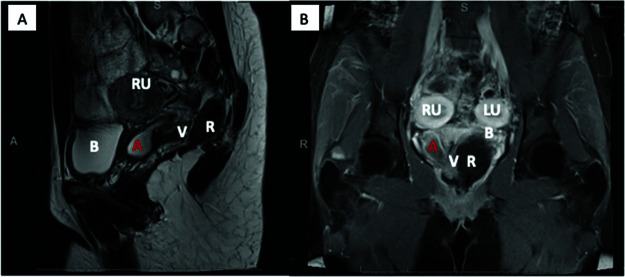
At the age of 22, she presented with chronic malodorous vaginal drainage. The patient underwent an in-office speculum examination and vaginoscopy revealing a duplicated cervix with purulent drainage originating from a small right vaginal ostium just distal to the right cervix. Cultures were obtained for pathogenic organisms and results were notable for heavy vaginal flora. An abdominal and pelvic magnetic resonance imaging was obtained, and the results suggested recurrent right paravaginal abscess arising from a remnant distal ectopic ureter (Figure 2). After consultation, the patient elected to proceed with surgical management. A minimally invasive robot-assisted laparoscopic excision and drainage of this paravaginal fluid collection with distal ureterectomy was then planned.
Figure 2.
Pre-operative magnetic resonance imaging: (A) Sagittal, (B) Coronal. Vagina (V), Right uterus (RU), Left uterus (LU), Rectum (R), Bladder (B), Right paravaginal abscess (A).
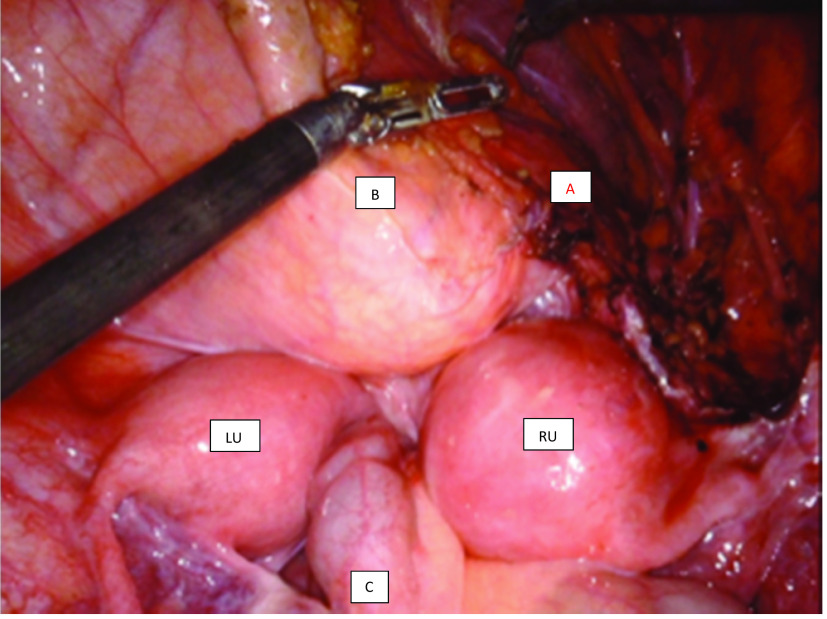
Cystoscopy was first performed, identifying a single left ureteral orifice. Two cervices and no remaining vaginal septum were confirmed by vaginoscopy. A vaginal ostium was identified just distal to the right cervix along the right vaginal sidewall. After entry into the abdomen, the bladder was mobilized and the right paravaginal and vesicovaginal spaces were developed, allowing identification of the paravaginal abscess and distal ureter. Simultaneous cystoscopic transillumination of the bladder was performed to provide robotic endoscopic visualization and delineation of the bladder, vagina, and paravaginal abscessed distal ureter (Figure 3). The abscessed ureter was then opened and drained, followed by the excision of the dilated ureteral stump. The ostium was then oversewn with a single figure-of-eight 3-0 poliglecaprone 25 suture. The peritoneum was closed with 2-0 delayed absorbable glycolide, dioxanone, trimethylene barbed suture. The patient was discharged home on postoperative day one.
Figure 3.
Intraoperative view of pelvis. Right uterus (RU), Left uterus (LU), Colon (C), Bladder (B), Right paravaginal abscess (A).
On postoperative day 15 the patient endorsed light vaginal drainage. An interval computed tomography (CT) scan demonstrated a 43 × 132 mm peritoneal fluid collection which was drained by the Interventional Radiology department. Cultures were positive for S. anginosus with treatment by a course of antibiotics. Two weeks later, follow-up CT and sinogram showed resolution of the fluid collection with subsequent drain removal. One year later she remains asymptomatic with no further pelvic pain or vaginal drainage.
DISCUSSION
OHVIRA is a rare syndrome of the genitourinary tract. One of the renal anomalies associated with this syndrome is an ectopic ureter, which typically arises from a dysplastic or atrophic kidney. The standard treatment is a nephrectomy with proximal ureterectomy. Laparoscopic dysplastic kidney resection and ureteral ligation has been found to be a successful treatment for urinary incontinence in this variant of OHVIRA syndrome, which was the childhood treatment course in our patient.7,10
We identified the symptomatic remnant distal ectopic ureter approximately one decade after initial treatment. The typical presentation of distal ureteral stump syndrome - draining into the bladder - is the constellation of symptoms that include febrile urinary tract infections, lower quadrant pain, and/or hematuria. This syndrome occurs in the setting of a prior nephrectomy with proximal ureterectomy and is very rare with an incidence of 00.8 – 1%.11 Few case reports have described empyema of a ureteral stump; however, no cases describe abscessed or empyema of an ectopic ureter to the vagina.11,12 The typical treatment of a symptomatic ureteral stump is surgical, either by excision or electrofulguration, which is the treatment course pursued for this patient.13,14
The final pathology for our patient did not identify ureteral tissue; however, it did identify atretic tissue with chronic inflammatory change encapsulating the infected structure. At the time of prior proximal ureterectomy, the distal portion was noted to be atretic and the ectopic path to the vagina could not be delineated and was left in situ. At the time of our surgery, a surgical clip was identified demarcating the most distal end of the ligated ureter abutting the abscess. Although final pathology does not demonstrate ureteric tissue, this is the most plausible etiology as the original tissue may have been replaced by chronic inflammatory changes from recurrent abscess formation ascending from the ectopic ureteral remnant from the vaginal ostia. Alternatives might include not capturing the ureteric tissue in our sample, or sinus tract from a recurrent abscess draining into the vagina. A fistula or sinus tract seems less likely given her history and location of the abscess. Our suspicion is that, albeit atretic, the distal ectopic ureteral stump was able to serve as a nidus for an ascending infection from the vagina. We suspect that this connection ultimately led to her recurrent paravaginal abscess and subsequent symptomatic vaginal drainage.
It is important to note that culture aspirates demonstrated growth of Streptococcus anginosus, a subgroup of Streptococcus viridans. S. anginosus is considered part of the typical human flora, typically found in the mouth, stool, and vagina. It can be a microbial source of aerobic vaginitis and has been found to be a pathogenic source in abscesses as well as systemic infections.15,16 The identification of this microbial pathogen supports our theory of an ascending vaginal infection.
CONCLUSIONS
We present the case of a recurrent paravaginal abscess, a very rare and underreported complication of a distal ectopic ureteral stump. In a patient with a paravaginal abscess or fluid collection, and a history of Mullerian anomaly, the differential should consider the vaginal ostium as a nidus for an ascending infection.
The concomitant use of minimally invasive techniques, both vaginal and robotic, can be useful to identify and excise fluid collections in the vesicovaginal space. Excision of an ectopic ureter to the vagina and distal ureteral stumps have been described using vaginal, laparoscopic and robotic techniques in case reports and videos, but the body of evidence remains limited, overall.17,18 This unique case, as far as we know, has yet to be described in the literature. We describe our perioperative work-up and successful surgical technique used to identify and excise the paravaginal abscess in the setting of a remnant ectopic ureter to the vagina. We highlight the importance of complete resection of an ectopic ureter to the vagina at the time of nephrectomy due to potential risk of ascending chronic infection and recurrent abscess formation.
Footnotes
Disclosure: none.
Funding sources: none.
Conflict of interests: none.
Informed consent: Dr. Daniel Y. Lovell declares that written informed consent was obtained from the patient/s for publication of this study/report and any accompanying images.
Contributor Information
Daniel Y. Lovell, Department of Obstetrics and Gynecology, Atrium Health, Carolinas Medical Center, Charlotte, North Carolina. (Dr. Lovell).
Amanda L. Merriman, Division of Urogynecology and Pelvic Surgery, Atrium Health, Carolinas Medical Center, Charlotte, North Carolina. (Drs. Merriman and Taylor, Ms. Benjamin).
Kristi C. Benjamin, Division of Urogynecology and Pelvic Surgery, Atrium Health, Carolinas Medical Center, Charlotte, North Carolina. (Drs. Merriman and Taylor, Ms. Benjamin).
Gerald B. Taylor, Division of Urogynecology and Pelvic Surgery, Atrium Health, Carolinas Medical Center, Charlotte, North Carolina. (Drs. Merriman and Taylor, Ms. Benjamin).
References:
- 1.Schlomer B, Rodriguez E, Baskin L. Obstructed hemivagina and ipsilateral renal agenesis (OHVIRA) syndrome should be redefined as ipsilateral renal anomalies: cases of symptomatic atrophic and dysplastic kidney with ectopic ureter to obstructed hemivagina. J Pediatr Urol. 2015;11(2):77.e1–77.e6. [DOI] [PubMed] [Google Scholar]
- 2.Cox D, Ching BH. Herlyn-Werner-Wunderlich syndrome: a rare presentation with pyocolpos. J Radiol Case Rep. 2012;6(3):9–15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Kim YN, Han JH, Lee YS, et al. Comparison between prepubertal and postpubertal patients with obstructed hemivagina and ipsilateral renal anomaly syndrome. J Pediatr Urol. 2021;17(5):652.e1–652.e7. [DOI] [PubMed] [Google Scholar]
- 4.Kriplani A, Dalal V, Kachhawa G, Mahey R, Yadav V, Kriplani I. Minimally invasive endoscopic approach for management of OHVIRA syndrome. J Obstet Gynaecol India. 2019;69(4):350–355. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Girardi Fachin C, Aleixes Sampaio Rocha JL, Atuati Maltoni A, et al. Herlyn-Werner-Wunderlich syndrome: diagnosis and treatment of an atypical case and review of literature. Int J Surg Case Rep. 2019;63:129–134. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Malarazhagan V, Veerasingham M, Sivanesan K. Right-sided obstructed hemivagina ipsilateral renal agenesis (OHVIRA): a case report. Case Rep Womens Health. 2020;26:e00185. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Nakahara Y, Nakada S, Hitomi K, et al. Urological anomalies associated with obstructed hemivagina and ipsilateral renal anomaly (OHVIRA) syndrome, a case series. J Pediatr Surg Case Rep. 2020;33(3):307–313.
- 8.Zhang J, Wang L. Dysplastic kidney and ectopic ureter in association with obstructed hemivagina and ipsilateral renal anomaly. Int Urogynecol J. 2020;31(8):1707–1709. [DOI] [PubMed] [Google Scholar]
- 9.Albers P, Foster RS, Bihrle R, Adams MC, Keating MA. Ectopic ureters and ureteroceles in adults. Urology. 1995;45(5):870–874. [DOI] [PubMed] [Google Scholar]
- 10.Duong DT, Shortliffe LM. A case of ectopic dysplastic kidney and ectopic ureter diagnosed by MRI. Nat Clin Pract Urol. 2008;5(11):632–636. [DOI] [PubMed] [Google Scholar]
- 11.Labanaris AP, Zugor V, Smiszek R, Nützel R, Kühn R. Empyema of the ureteral stump. An unusual complication following nephrectomy. ScientificWorldJournal. 2010;10:380–383. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Smeoui W, Samet A, Touaiti T, Rebai N, Bouzouita A, Hadjslimène M. Ureteral stump empyema with calculi. Urol Case Rep. 2020;28:101049. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Ehrlich RM, Koyle MA, Shanberg AM. A technique for ureteral stump ablation. J Urol. 1988;140:1240–1241. [DOI] [PubMed] [Google Scholar]
- 14.Ikeda D, Matsutani R, Fukuda M, Fuse H, Hirano S. Transurethral fulguration for empyema of ectopic ureteral stump. Int J Urol. 2003;10(12):664–666. [DOI] [PubMed] [Google Scholar]
- 15.Tao Z, Zhang L, Zhang Q, et al. The pathogenesis of streptococcus anginosus in aerobic vaginitis. Infect Drug Resist. 2019;12:3745–3754. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Ruoff KL. Streptococcus anginosus (“Streptococcus milleri”): the unrecognized pathogen. Clin Microbiol Rev. 1988;1(1):102–108. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Alenezi H, Eltiraifi AE, Alomar M. Minimally invasive surgery for the treatment of ureteral stump syndrome. Urol Ann. 2015;7(4):454–458. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Chang ES, Hidalgo RJ, Wiegand LR, Wyman A. Concomitant laparoscopic and vaginal excision of duplicated collecting system. Int Urogynecol J. 2021;32(10):2871–2872. [DOI] [PubMed] [Google Scholar]