Pathological meeting
This case was presented at the on-line meeting on the ADOI platform held on October 27th 2021 by Dr Zardo.
Surgical pathologists attending the meeting: 18.
Surgical pathologists that reviewed the slides before the meeting: 12.
Clinical data
Caucasian 29 years old female; enlarging pigmented lesion on the calf with asymmetric pigmentation. Concern of the patient. Clinical pictures not available.
Histopathology
Virtual slides are available at:
https://www.dropbox.com/sh/5v4ydf0o1t5x0th/AACqtKvynw mDNL6wwYrdPSp3a?dl=0
Description
Asymmetric, not sharply circumscribed, mostly junctional melanocytic proliferation composed predominantly by nests that are different one from another, with different shape and dimension, asymmetric disposition and with uneven distribution of pigment. The nests are expansile and push the epidermis from the bottom squeezing the stratum spinosum. The epidermis shows focal pigmented parakeratosis and pigmentation of basal keratinocytes. At one edge of the lesion, atypical melanocytes in single unit are present in the stratum spinosum. Irregular nests are present also in the superficial dermis, together with melanophages, few dendritic melanocytes and a very spare lymphocytic infiltrate. Mild solar elastosis is present. Melanocytes with long dendrites are found also in the epidermis, within the nests (the whole description refers to Figures 1 to 8 and virtual slides). Few mitotic figures were seen.
Immunohistochemistry
Positivity for Melan-A, BRAF-V600E and PRAME.
Heterogenous positivity for HMB-45 (some nests are positive, others are negative)
Molecular biology
Not performed
Premeeting survey
Virtual slides were reviewed by 12 surgical pathologists before the meeting (Table 1).
Five pathologists favored a common acquired nevus, six agreed on melanoma (three nevoid melanoma), one pathologist was uncertain.
The level of confidence was judged as low by 6 pathologists, average by four and high by two of them.
The complexity of the case was reported as “high” by 8 pathologists, “average” by two and “low” by two of them.
Meeting real-time survey
This case was presented to18 Italian surgical pathologists. After collegial discussion, 16 of them agreed on the diagnosis of nested (nevoid) melanoma, one favored a combined nevus and one a congenital nevus.
Discussion
The term “nevoid melanoma” applies theoretically to all melanomas simulating on pathology a benign nevus.1,2 The first description of melanomas that are deceitfully similar to their benign counterparts occurred in the ‘80 by Levene,3 and subsequently also the definition of “minimal deviation melanoma”, “small cell melanoma“ or “spitzoid melanoma” among other have been used. However, even if there is general agreement that in some cases primary melanomas and melanoma metastasis may show overlapping histopathological features with benign nevi, precise criteria and classification are still lacking.
Some authors distinguish two types of nevoid melanomas: a papillomatous subtype, and the dome-shaped, nonpapillomatous nevoid melanoma (by some also called ‘maturing naevoid’).1,4 According to Massi and LeBoit a third category including nested melanoma shoudl be added.5 Others divide nevoid melanoma into 5 main categories according to the simulated nevus: (1) nevoid melanoma with dysplastic nevus-like pattern; (2) nevoid melanoma with congenital nevus-like pattern; (3) nevoid melanoma with Reed nevus-like pattern (4) nevoid melanoma with dermal nevus-like pattern (papillomatous or dome-shaped); and (5) nevoid melanoma with hypermelanotic nevus-like pattern.2 There is general agreement not to use the definition of nevoid melanoma for those lesions with architectural and/or cytomorphological features similar to Spitz nevus, as this last may be characterized by atypical cytomorphological features. In fact, in the new WHO classification Spitz melanoma is considered as a distinct variant of melanoma.6
Nested melanoma of the elderly is a peculiar variant of superficial melanoma characterized by predominance of large, irregular, confluent nests of melanocytes simulating nested junctional nevi and belonging to the heterogeneous spectrum of nevoid melanomas.2,5,6
Criteria favouring the diagnosis of nevoid melanoma are: advanced age of patients, large size of the lesion, architectural disarray of nests regarding size, distribution and shape, and even mild spread of single melanocytes above the dermoepidermal junction, presence of actinic elastosis. Cannonball-like irregular nests strikingly predominating over solitary melanocytes, focal pagetoid spread of melanocytes and thinning of epidermal rim surrounding the nests are peculiar features of nested melanomas. 1-6
Clinical features are aspecific; dermoscopic findings are irregular globular pattern, atypical vessels and/or irregular dots/globules.7
In the case herein presented the College of pathologists agreed on the diagnosis of invasive nested (nevoid) melanoma (T1a; Breslow thickness: 0.6mm) because of asymmetry of the lesion and pigment distribution, predominance of irregular nests with varing size and shape, presence of dentritic melanocytes in the epidermis, focal pagetoid spread and mitoses.
Figure 1.

Asymmetric, not sharply circumscribed, mostly junctional melanocytic proliferation (H&E; 20x).
Figure 2.

Left half of the lesion: nests are different one from another, with different shape and dimension, asymmetric disposition and with uneven distribution of pigment (H&E; 40x).
Figure 3.

Right half of the lesion: nests are different one from another, with different shape and dimension, asymmetric disposition and with uneven distribution of pigment (H&E; 40x).
Figure 4.

The nests are expansile and push the epidermis from the bottom squeezing the stratum spinosum. The epidermis shows focal pigmented parakeratosis and pigmentation of basal keratinocytes (H&E; 100x).
Figure 5.

At one edge of the lesion, atypical melanocytes in single unit are present in the stratum spinosum (H&E; 100x).
Figure 6.

Irregular nests and single melanocytes in the epidermis also above the dermoepidermal junction. In the superficial dermis melanophages, few dendritic melanocytes and lymphocytes are present (H&E; 100x).
Figure 7.

Irregular nests with cohesive melanocytes pushing the epidermis from the bottom (H&E; 200x).
Figure 8.
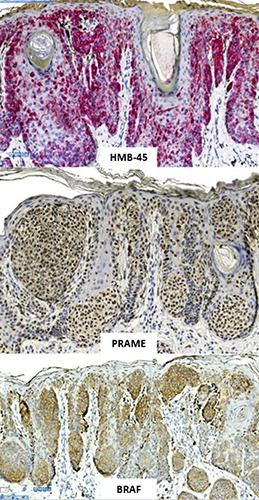
Positivity BRAF-V600E and PRAME; heterogenous positivity for HMB-45 (x100).
Table 1.
Results of the collegial discussion on the lesion – October 27, 2021.

References
- 1.Cook MG, Massi D, Blokx WAM, et al. New insights into naevoid melanomas: a clinicopathological reassessment. Histopathology 2017;71:943-50. [DOI] [PubMed] [Google Scholar]
- 2.Saggini A, Cota C, Lora V, et al. Uncommon Histopathological Variants of Malignant Melanoma. Part 2. Am J Dermatopathol 2019;41:321-42. [DOI] [PubMed] [Google Scholar]
- 3.Levene A. On the histological diagnosis and prognosis of malignant melanoma. J Clin Pathol 1980;33;101–24. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Idriss MH, Rizwan L, Sferuzza A, et al. Nevoid melanoma: a study of 43 cases with emphasis on growth pattern. J Am Acad Dermatol 2015;73:836–42. [DOI] [PubMed] [Google Scholar]
- 5.Massi G, LeBoit PE. Melanoma resembling blue nevus. In: Histological Diagnosis of Nevi and Melanoma. 2nd ed. Berlin, Heidelberg: Springer; 2014:535–546. [Google Scholar]
- 6.Elder D, Scolyer R, Massi D, et al. , eds. World Health Organization Classification of Tu-mours. Pathology and Genetics of Skin Tumors. 4th ed. Lyon, France: WHO IARC, 2018 [Google Scholar]
- 7.Longo C, Piana S, Marghoob A, et al. Morphological features of naevoid melanoma: results of a multicentre study of the International Dermoscopy Society. Br J Dermatol 2015;172:961-7. [DOI] [PubMed] [Google Scholar]


