Abstract
Musculoskeletal injury is a leading cause of pain and disability worldwide; 35-75% of people experience persistent pain for months and years after injury. Psychological treatments can reduce pain, functional impairment and psychological distress, but are not widely utilized following injury. This systematic review and meta-analysis (PROSPERO ID: CRD42021236807) aimed to synthesize the literature testing psychological treatments for pain following musculoskeletal injury. We searched EMBASE, MEDLINE, PubMed, PsycINFO, and CENTRAL from inception to May 2022. We extracted participant, treatment, and injury characteristics, and primary (e.g., pain intensity, functional impairment, depression, anxiety, PTSD symptoms) and secondary (treatment feasibility and acceptability) outcomes. 24 RCTs (N = 1,966) were included. Immediately post-treatment, people who received psychological treatments (versus any control) reported lower pain intensity (SMD = −0.25, 95% CI [−0.49, −0.02]), functional impairment (SMD = −0.32 [−0.55, −0.09]), and symptoms of depression (SMD = −0.46 [−0.64, −0.29]), anxiety (SMD = −0.34 [−0.65, −0.04]) and PTSD (SMD = −0.43 [−0.70, −0.15]); at 6-month follow-up, only depression symptoms were significantly lower. Included trials varied widely in treatment and injury characteristics. The certainty of evidence was low or very low for most effects, and heterogeneity moderate to substantial. Most studies had risk of bias domains judged to be high or unclear. Due to very low certainty of results, we are unsure whether psychological therapies reduce pain and functional impairment following musculoskeletal injury; they may result in improved depression immediately post-treatment and at follow-up. More research is needed to identify treatments that result in enduring effects.
Keywords: musculoskeletal injury, orthopedic injury, psychological intervention, cognitive behavioral therapy, systematic review, meta-analysis
Introduction
Musculoskeletal injury occurs in three million people per year in the United States and is a leading cause of pain and disability worldwide. [48] Musculoskeletal injuries involve damage to the muscular or skeletal systems, including fractures, sprains, and dislocations. [48] Acute pain following a musculoskeletal injury is expected, however for many, pain will persist for months or years following injury. [56] Among adults, 54% reported persistent pain 6-months following musculoskeletal injury, and 77% report persistent pain 7 years following severe musculoskeletal trauma. [14; 16] Among children, 35% report persistent pain 4 months post-musculoskeletal injury. [39] Musculoskeletal injury can result in psychological distress; for example, half of people who sustain orthopedic trauma will experience depression and anxiety two years post injury, [67] and about a third will experience PTSD one year post injury. [82] Pain and distress relate to and exacerbate one another [15] and contribute to long-term functional impairment. [13; 42; 44; 68] A portion of people who sustain musculoskeletal injury will rely on prescription opioid medication to manage pain past the point of physical healing. [37; 40] More so than the severity of the injury itself, psychological factors such as depression, anxiety, and pain coping predict the persistence of pain over time. [17; 42] Clinical practice guidelines for musculoskeletal injury emphasize the importance of psychological treatment for recovery; however, psychological treatments have not been widely utilized following musculoskeletal injury. [41; 69] Given the prevalence, impact, and risk for long-term prescription opioid use following musculoskeletal injury, there is a need to identify the efficacy of psychological treatments targeting pain and related symptoms in this population.
Dozens of randomized controlled trials (RCTs) have concluded that psychological treatments for chronic pain, particularly cognitive behavioral therapy (CBT), are effective in reducing pain, functional impairment, and psychological distress. [78] One review found that exposure-based and CBT interventions delivered in the first three months following any traumatic injury type resulted in improvements in PTSD and depression;33 however, limited research is available to determine the efficacy of psychological treatments for pain following musculoskeletal injury. This population requires special attention for several reasons. Sustaining an injury poses risk for persistent pain. [59] Medical procedures, such as surgery, performed to treat injuries further increase the risk of experiencing persistent pain. [58] Musculoskeletal injuries are unexpected and can have multifaceted impact including functional impairment, [7] vocational challenges, [45] financial hardship, [28] and disruption to interpersonal relationships. [36] The stress and uncertainty associated with injury can add to the burden of coping with pain and pose additional risk for poor pain-related outcomes. There are known barriers to implementing psychosocial treatments following musculoskeletal injury, including limited integration of psychosocial healthcare into orthopedic practice, stigma associated with behavioral pain management and mental healthcare, and limited available resources to screen those who may benefit most from services. [46; 69; 71]
The current review aimed to systematically review the efficacy of psychological treatments targeting pain to improve primary (pain intensity, functional impairment, depression, anxiety, PTSD symptoms, opioid consumption; patient ratings of global improvement; and adverse events) and secondary (treatment feasibility and acceptability) outcomes following musculoskeletal injury and to synthesize the characteristics of available clinical trials. These outcomes reflect core outcomes domains for chronic pain clinical trials as recommended by the Initiatives on Methods, Measurement, and Pain Assessment in Clinical Trials (IMMPACT). [65] PTSD was also included given the elevated prevalence of PTSD after injury.82 We summarize gaps in this literature to inform the next iteration of trials testing psychological treatment for pain following musculoskeletal injury and ultimately to improve clinical practice.
2.0. Methods
2.1. Protocol Registration
This systematic review was informed by PRISMA [49] and Cochrane [38] guidelines. It was pre-registered on PROSPERO (ID = CRD42021236807).
2.2. Types of studies
We included RCTs and non-randomized trials in this review. RCTs were included as the preferred source of evidence as they are the highest quality trial design that attempt to limit bias. We anticipated limited number of RCTs and thus utilized a broad search strategy that also identified non-randomized trials (e.g., single arm trials, non-randomized comparative trials). Because we expected a limited literature base and prioritized a comprehensive review of the available intervention literature, we included trials that assessed efficacy, effectiveness, or feasibility. We excluded conference abstracts, dissertations, and papers that were not peer reviewed.
2.3. Types of treatments
We included studies that delivered psychological treatment that aimed to prevent or treat pain and/or functional impairment in individuals who sustained a musculoskeletal injury, versus any control. Psychological treatment was defined as an intervention that contained specific content grounded in psychological theory of cognitive or behavioral change, or that otherwise contained recognizable psychotherapeutic content; this criteria for psychological treatment was adapted from a similar review published in the Cochrane Library, and inclusion required review and agreement by two clinical psychologists. [78] We excluded treatments that delivered skills sometimes incorporated in psychological treatments (e.g., biofeedback, relaxation) if there was no evidence that the treatment applied psychological principles in its delivery (e.g., application of skills to reduce stress, tension or pain). We did not limit our search to treatments delivered by a mental health provider, as recovery from musculoskeletal injury often requires an interdisciplinary approach and the literature suggests interdisciplinary providers can successfully deliver components of psychological treatment. [26] We included trials delivered in person or remotely, and which were delivered by an individual or were automated (e.g., text message, workbook). We included studies that employed a waitlist, treatment as usual, or active comparator. We excluded equivalence studies, that delivered the same psychological content in both arms as we were unable to determine the beneficial effect of psychological therapies in these trials.
2.4. Types of participants
We included studies in which participants sustained an identifiable musculoskeletal injury, defined as damage to the muscular or skeletal system (e.g., fracture, sprain, dislocation) which occurred in response to an identifiable event (e.g., motor vehicle crash, fall, sports injury). Musculoskeletal disorders that were not associated with an identifiable injury or trauma were excluded (e.g., idiopathic chronic low back pain, disorders of overuse [e.g., carpal tunnel]). Consistent with other systematic reviews, [17; 47] we excluded trials with a mixed populations (e.g., musculoskeletal injury and traumatic brain injury) that were comprised of less than 90% musculoskeletal injury. We conducted a comprehensive review in order to describe the state of this literature and point to relevant gaps. Thus, we included participants at any timepoint following musculoskeletal injury (e.g., acute or historical injury). We included treatments delivered to participants of all ages.
2.5. Outcomes
Primary outcomes were pain intensity; functional impairment; depression symptoms; anxiety symptoms; and PTSD symptoms; opioid consumption; patient ratings of global improvement; and adverse events. Secondary outcomes were treatment feasibility and treatment acceptability.
2.5.1. Outcome Timepoints.
We collected outcome data immediately post treatment (baseline), up to and including 6-month follow-up (6 months), and between 6- and 12-month follow-up (12 months). When multiple follow-ups were collected within a given window, preference was given to the later follow-up data point.
2.6. Search strategy and selection of studies
Detailed search strategies were developed in collaboration with university librarians. We searched EMBASE (OVID), MEDLINE, PubMed (not including MEDLINE records), PsycINFO, and The Cochrane Central Registry of Controlled Trials (CENTRAL) from inception to May 4, 2022 for studies that contained reference to pain, musculoskeletal injury, and psychological treatment. The full search strategy is provided in Appendix A. Using COVIDENCE (Veritas Health Innovation, Melbourne, Australia), two authors independently sifted records for eligibility by reading the title and abstract for each study identified in the search. Two authors (RA, FR) independently reviewed the texts of full reports and independently determined eligibility. Disagreements were resolved through discussion and consensus with a third author (EF).
2.7. Data extraction
We extracted details related to study design, participant characteristics, injury characteristics, pain characteristics, treatment details, outcome measurement tools and outcome measures. Outcomes were extracted at baseline, post-treatment, 6-month follow-up, and 12-month follow-up. Among eligible full reports, one author (RA) extracted data using a standardized form developed for this review. A second author (FN or EF) reviewed all extracted data for accuracy. Disagreements were resolved through discussion and consensus with a third author.
2.8. Risk of bias (ROB)
We judged ROB for randomized controlled trials, using the Cochrane Risk of Bias tool, [38] as high, low, or unclear in the following domains. Random sequence generation: we judged studies as low ROB when a method of truly random sequence generation was provided (e.g., random numbers generator) and high ROB for studies that provided a method that was not truly random (e.g., odd or even date of birth). Allocation concealment: we judged studies to be low ROB if they provided a method of allocation concealment where the allocation of participants could not be determined ahead of time (e.g., consecutively numbered opaque sealed envelopes). We judged studies that provided a method likely to introduce bias or that did not conceal allocation (e.g., open list) as high ROB. Blinding of participants and personnel: we judged studies as low ROB that described a sufficient method for blinding of participants and personnel. We judged studies as high ROB as no blinding, incomplete blinding, or outcomes likely influenced by lack of blinding. Incomplete outcome data: we rated studies where there was <10% attrition or if they applied appropriate methods for imputation as low ROB. Studies that did not account for missing data in analysis or used an inappropriate approach (e.g., last observation carried forward) were rated as high ROB. Selective reporting: we rated studies that prospectively registered and reported all outcomes registered in the same order (primary vs. secondary) as low ROB. Studies that registered a protocol but missed or reported outcomes in a different order were rated as high ROB. For all domains, ROB was judged as unclear when the relevant information was not reported or could not be discerned.
2.9. Certainty of evidence
We rated all outcomes for certainty of evidence using the GRADE framework. [38] Randomized controlled trials started at high-certainty evidence and were then downgraded for five considerations: limitations in the design and implementation of available studies, suggesting high likelihood of bias; indirectness (i.e., indirect population, intervention, control, outcomes); unexplained heterogeneity or inconsistency of results; imprecision (i.e., includes studies with small sample size, wide confidence intervals); and, reporting bias (e.g., publication bias). Each category could be downgraded twice. GRADE certainty of evidence judgements include: high quality (i.e., further research is very unlikely to change our confidence in the estimate of effect), moderate quality (i.e., further research is likely to have an important impact on our confidence in the estimate of effect and may change the estimate), low quality (i.e., further research is very likely to have an important impact on our confidence in the estimate of effect and is likely to change the estimate) and very low quality (i.e., we are very uncertain about the estimate).
2.10. Data analysis
For RCTs, we conducted comparisons of outcomes between psychological treatment and control groups at post-treatment, 6-month follow-up, and 12-month follow-up. Meta-analyses were conducted in Review Manager Version number 5.4 (RevMan; The Cochrane Collaboration, 2020) when there were ≥ 3 trials in a given comparison. When there were multiple assessments of the same outcome, we prioritized the assessment that was stated as the primary outcome; otherwise, we prioritized the assessment that was reported first and/or most consistently with other studies. For some trials, data was not available or suitable (e.g., SDs not reported) for meta-analysis. In these cases, we contacted the corresponding author at least twice to obtain the necessary data. When standard errors were reported, they were converted to SDs using guidance in the Cochrane Handbook. [38]
All meta-analyses were conducted with random-effects models, because of heterogeneity in study design and variability in the measures used across trials, and we reported standardized mean differences (SMD) with 95% confidence intervals for continuous outcomes. We interpreted SMD as small (0.2), medium (0.5) and large (0.8). [18] We assessed heterogeneity using I2, following conventions outlined in the Cochrane Handbook (0%–40% low heterogeneity; 30%–60% moderate heterogeneity; 50%–90% substantial heterogeneity; and 75%–100% considerable heterogeneity). [38]
There was variability in the characteristics of included trials including injury type, time since injury, session length and duration of treatment, delivery of treatment, and type of treatment. Our protocol stated we would conduct subgroup analysis only if there were K ≥ 10 in any relevant comparison (based on guidelines in the Cochrane Handbook); however, given the variability within included studies and heterogeneity of included meta-analyses, we explored select subgroup (i.e., when there were distinct two subgroups to compare) and/or sensitivity (i.e., when there was reason to isolate a particular condition) analyses based on those stated a priori in our protocol and with priority to the comparisons with the largest available number of studies. Specifically, we conducted subgroup analyses based on interventions delivered in the acute vs. chronic stage of recovery and those that were compared to an active versus passive control condition. Based on the predominance of whiplash in included studies, we conducted a sensitivity analysis isolating whiplash. To explore the effect of treatment dose, we conducted a sensitivity analysis isolating sessions greater than one session in duration only; the cutoff of a single session was based on the observation that several trials included were comprised of a single, short, session ranging from 60 seconds to 30 minutes. We did not identify any study conducted in youth, and thus did not conduct any subgroup analysis based on age.
3.0. Results
3.1. Results of the search
We identified 11,479 records across five databases and by screening reference lists, and removed 2,175 duplicate records. This yielded a total of 9,304 unique records which underwent title and abstract screening. Through this process, we identified 133 papers which were assessed for eligibility by full text review. A total of 39 papers reflecting 37 separate studies were included in the final synthesis. A PRISMA table is reported in Figure 1.
Figure 1.

PRISMA Flow Diagram
We found 24 RCTs (1,966 participants) and 13 non-randomized comparative or single arm trials (661 participants). Due to the relatively large number of RCTs, which was not anticipated, we only report findings from the RCTs in this report. A summary of findings from non-RCT studies are reported in Appendix B for the interested reader.
3.2. Characteristics of included RCTs.
Overall, treatment characteristics varied with respect to type of psychological treatment delivered, session length and treatment duration, delivery (e.g., provider type, modality), and timing of the treatment in respect to initial injury. Outcome measures varied between trials. Individual study characteristics are reported in Table 1. [1–3; 5; 6; 8; 9; 11; 12; 19; 23; 25; 29; 31; 32; 34; 35; 43; 50–54; 57; 61–64; 66; 70; 72; 74–76; 79–81] Of included RCTs, four explicitly identified trial type as a preliminary, [70] feasibility, [75] and/or pilot trial. [31; 64] Sample sizes of included trials ranged from 12-152.
Table 1.
Study Characteristics of Included Studies
| Study ID | Injury Type | N | Demographics A: Age Mean(SD); G: Gender or Sex (% Female); R: Race, Ethnicity, or Nationality; C: Country |
Intervention Type I = Intervention; C = Control |
Session Length and Treatment Duration | Delivered By | Time Since Injury | Patient Reported Outcome Measures PI: Pain Intensity; F: Functional Impact; D: Depression; A: Anxiety; P: PTSD |
|---|---|---|---|---|---|---|---|---|
| Randomized Controlled Trials | ||||||||
|
| ||||||||
| Andersen 20212 | Whiplash | 104 | A: 42.0 (12.5) G: 73% R: NR C: Australia, Denmark |
I: TF-CBT C: Supportive Psychotherapy |
10 x 60-90 minute | Psychologist | Chronic |
*PI: VAS *F: NDI *D: DASS-D *A: DASS-A *P: PCL-5 |
| Andersen 20223 | Whiplash | 92 | A: 39.3 (12.1) G: 76% R: NR C: Denmark |
I: Value-Based CBT C: Waitlist |
10 x 1-hour | Psychologist | Chronic |
*PI: NRS *F: PDI *D: HADS-D *A: HADS-A *P: Harvard Trauma Questionnaire |
| Anthony 20206 | Traumatic fracture (upper or lower extremity) | 82 | A: 47.1 (15.3) G: 50% R: 82% White; 9% African American; 1% Asian; 1% Hispanic C: United States |
I: ACT C: TAU |
2 weeks | Text Message | Acute |
*PI: PROMIS Pain Intensity (1a) *F: PROMIS Pain Interference (8a) *A: PROMIS Anxiety (8a) |
| Bérubé 20198 | Major Trauma (lower extremity) | A: 47 (19) G: 40% R: 79% Caucasian; 11% Haitian; 5% Arabic; 2% Asian; 2% African C: Canada |
I: Self-Management Intervention (iPACT-E-Trauma) C: Education Pamphlet |
7 x 15-30 minute | Nurse and Web-Based | Acute |
*PI: NRS *F: NRS *D: HADS-D *A: HADS-A |
|
| Bring 201611 | Whiplash | 55 | A: 35.7 (10.5) G: 67% R: 97% Swedish C: Sweden |
I: Behavioral Medicine Intervention C: Information Workbook |
7 x 1-hour | PT | Acute | PI: NRS F: PDI |
| Burns 200712 | Fracture (hip) | 121 | A: 81.1 (8.4) G: 77% R: NR C: United Kingdom |
I: Problem Solving Therapy or CBT C: TAU |
6-7 weeks | PT | Acute | PI: FACES D: HADS A: HADS |
| Dunne 201223 | Whiplash | 26 | A: 80.8 (6.5) G: 50% R: 73% non-indigenous Australian C: Australia |
I: TF-CBT C: Waitlist |
10 x 1-hour | Psychologist | Chronic |
*PI: NRS *F: NDI *D: DASS-D *A: DASS-A *P: PDS |
| Gambatesa 201329 | Fracture (hip) | 40 | A: 80.8 (6.5) G: 93% R: 100% White C: Italy |
I: Rogerian Counseling C: TAU |
2 x 45-minutes weekly during hospitalization | Mental Health Counselor | Acute | PI: VAS F: SF-36 *D: HDRS A: STAI |
| Ginandes 199931 | Fracture (malleolar) | 12 | A: NR G: 75% R: 100% White C: United States |
I: Hypnosis C: TAU |
6 sessions | Psychologist | Acute | *PI: VAS |
| Goudie 201834 | Fracture (distal radius) | 139 | A: NR G: 71% R: NR C: Scotland |
I: Education Workbook C: Information Workbook |
Self-paced | Workbook | Acute | PI: NRS F: DASH |
| Ludvigsson 201543 | Whiplash | 147 | A: 39.0 G: 71% R: NR C: Sweden |
I: Neck Specific Exercise with Behavioral Approach C: Physical Therapy |
12 sessions | PT | Chronic |
*PI: VAS *F: PDI *D: HADS *A: HADS |
| Ottosson 200751 | Minor Injuries | 141 | A: 42.5 (14.5) G: 48% R: NR C: Sweden |
I: Pain Neuroscience Education C: TAU |
4 x 90 minute | Interdisc. Team | Acute | PI: VAS F: Short MSK Function Assessment |
| Pato 201052 | Whiplash | 87 | A: 40.5 (12.1) G: 62% R: NR C: Switzerland |
I: CBT C: No CBT |
16 x 60-minute | Psychologist | Chronic |
*PI: VAS *F: Health Assessment Questionnaire |
| Robinson 201354 | Whiplash | 127 | A: 35.8 (12.1) G: 71% R: 75% White; 25% non-White |
I: Exposure Therapy C: Information Workbook |
3 sessions | Interdisc. Team | Acute |
*PI: Multidimensional Pain Inventory *F: NDI *D: CES-D *P: PTSD Checklist |
| Ross 199657 | Miniscus Tear | 60 | A: 28.9 (NR) G: 0% R: NR C: United States |
I: Stress Inoculation Training C: Physical Therapy |
2 x 1-hour | Psychologist | Acute |
*PI: VAS *A: STAI-State |
| Söderlund 200161 | Whiplash | 33 | A: 40.7 (NR) G: 58% R: NR C: Sweden |
I: Coping Skills Training C: Physical Therapy |
Up to 12 sessions | PT | Chronic |
*PI: NRS *F: PDI |
| Sterling 201982 | Whiplash | 108 | A: 41.3 G: 62% R: NR C: Australia |
I: Stress Inoculation Training + Guideline Based Exercise C: Physical Therapy |
10 sessions over 6 weeks | PT | Acute |
*PI: VAS *F: NDI *D: DASS-D *A: DASS-A *P: PDS |
| Tobbackx 201364 | Whiplash | 39 | A: 41 (10) G: 72% R: NR C: Belgium |
I: Relaxation C: Acupuncture |
1 x 20-minute | Audiotape | Chronic | PI: VAS F: NDI |
| Vranceanu 201570 | MSK trauma | 44 | A: 51.8 (18.6) G: 63% R: NR C: United States |
I: Mind-Body Based Intervention C: TAU |
4-6 x 60-minute | NR | Acute |
*PI: NRS *F: Short Musculoskeletal Function Assessment Questionnaire *D: CES-D *P: PCL |
| Westenberg 201874 | Upper Extremity Injury | 126 | A: 54.5 (15.0) G: 50% C: United States R: 90% White; 4% Black; 3% Latino; 1% Asian; 2% Other |
I: Mindfulness C: Education Pamphlet |
1 x 60-second | Video | NR |
*PI: NRS *D: Emotion Thermometer *A: STAI-State |
| Wiangkham 201975 | Whiplash | 28 | A: 38.7 (NR) G: 68% R: 54% White; 29% Asian; 11% Chinese or Other; 4% Black; 4% Mixed C: United Kingdom |
I: Active Behavioral PT C: Standard PT |
6-8 x 30-minute | PT | Acute | PI: VAS F: NDI P: IES |
| Wicksell 200876 | Whiplash | 22 | A: 51.5 (9.4) G: 76% R: NR C: Sweden |
I: Exposure and Acceptance C: Waitlist |
10 x 60-minute | Interdisc. Team | Chronic |
*PI: NRS *F: PDI *D: HADS-D *A: HADS-A *P: IES |
| Wong 201079 | Fracture (single limb) | 125 | A: 54.4 (18) G: 45.6% R: NR C: China |
I: Education and Relaxation C: TAU |
1 x 30-minute | Researcher | Acute |
*PI: VAS *A: STAI-State |
| Wong 201480 | Fracture (single limb) | 152 | A: 55.0 (17.7) G: 45% R: NR C: China |
I: Education and Relaxation C: TAU |
1 x 20-minute | Researcher | Acute |
*PI: VAS *A: STAI-State |
|
| ||||||||
| Non-Randomized Trials | ||||||||
|
| ||||||||
| Achterberg 19891 | Multiple Fractures | 64 | A: 29.3 (NR) G: 23% R: 70% White; 24% Black; 5% Mexican C: United States |
I: Biofeedback | 6 x 28-minute | Audiotape | Acute | PI: SUDS A: STAI |
| Angst 20105 | Whiplash | 185 | A: 37.9 (11.9) G: 80% R: NR C: Switzerland |
I: Interdisc. inpatient rehabilitation | 4-7 hours/week, four weeks | Interdisc. Team | Chronic | F: NASS D: HADS A: HADS |
| Bérubé 20189 | Major Trauma (lower extremity) | 28 | A: > 18 G: 46% R: NR C: Canada |
I: Self-Management Intervention (iPACT-E-Trauma) | 7 x 15-30 minute | Nurse and Web-Based | Acute | n/a |
| Coronado 202019 | ACL tear | 8 | A: 20.1 (2.6) G: 75% R: NR C: United States |
I: Cognitive Behavioral Physical Therapy | 7 x 30-minute | PT | NR (<12 months) | F: IKDC |
| Dunstan 200725 | Soft Tissue Injury | 30 | A: 41 (NR) G: 40% R: NR C: Australia |
I: Work-Related Activity Program | 1/2 day/week, six weeks | Interdisc. Team | Chronic | PI: NRS F: Roland-Morris Disability Questionnaire D: DASS A: DASS |
| Giordano 202232 | Orthopedic Trauma | 121 | A: 37.3 (13.3) G: 43% R: 78% Black; 10% White; 2% Asian; 11% Other C: United States |
I: Pain Coaching | ≥ 1 hour daily during hospitalization and 1 x 30-minute booster | Life Care Specialists | Acute | PI: NRS |
| Hall 201135 | MSK Injury | 96 | A: 40.9 (13.4) G: 49% R: White: 60.4%, Aboriginal/Metis: 32.3%, Other: 7.2% C: Canada |
I: Interdisc. outpatient rehabilitation | Daily, 12 weeks | Interdisc. Team | Chronic | PI: SF-36 F: SF-36 |
| New 199750 | Spinal Cord Injury | 22 | A: 41.2 (NR) G: 8% R: NR C: Australia |
I: Interdisc. inpatient rehabilitation | Daily during hospitalization | Interdisc. Team | Acute | PI: VAS |
| Ritchie 202153 | Whiplash | 6 | A: 45.3 (NR) G: 67% R: NR C: Australia |
I: Adapted Physical Activity Program | 12 x 1-hour | Exercise Physiologist | Chronic | PI: NRS F: NDI D: DASS A: DASS P: IES |
| Sullivan 200663 | Whiplash | 70 | A: 40.8 (8.3) G: 49% R: NR C: Canada |
I: Progressive Goal Attainment | 10 x 1-hour | PT and OT | NR | F: PDI |
| VanOosterwijck 201166 | Whiplash | 6 | A: 35.7 (7.3) G: 83% R: 100% White C: Belgium |
I: Pain Neurophysiology Education | 2 x 20-minute | PT | Chronic | F: NDI |
| Wald 201072 | MSK Injury | 5 | A: 42.4 (11) G: 100% R: Caucasian: 80%, South Asian: 20% C: Canada |
I: Interoceptive Exposure and Trauma-Related Exposure Therapy | 12 x 90-minute | Psychologist | Chronic | PI: BPI F: BPI A: Beck Anxiety Inventory P: CAPS |
| Wood 202181 | Spinal Cord Injury | 20 | A: > 18 G: 46% R: NR C: United States |
I: Music Assisted Relaxation | 2 x 20-minute | Board Certified Music Therapist | Acute | PI: VAS A: GAD-7 |
Note.
Outcome Measurement Included in Meta-Analysis; TAU = Treatment as Usual; MSK = musculoskeletal; CBT = Cognitive Behavioral Therapy; ACT = Acceptance and Commitment Therapy; PT = Physical Therapy; VAS = Visual Analog Scale; NRS = Numerical Rating Scale; BPI = Brief Pain Inventory; NDI = Neck Disability Index; PDI = Pain Disability Index; IKDC = International Knee Documentation Committee; NASS = North American Spine Self-assessment instrument; DASH = Disabilities of the arm, shoulder and hand Scale; DASS = Depression Anxiety Stress Scales; HADS = Hospital Anxiety and Depression Scale; CES-D = Center for Epidemiologic Studies Depression Scale; HDRS = Hamilton Depression Rating Scale; STAI = State-Trait Anxiety Inventory; GAD-7 = General Anxiety Disorder 7-item; SF-36 = 36-item Short Form Survey; PCL-5 = PTSD Checklist for DSM 5; IES = Impact of Event Scale; PDS = Posttraumatic Stress Diagnostic Scale; CAPS (Clinician Administered PTSD Scale)
3.2.1. Demographics of included participants.
The mean age of included participants was 46.8 years (SD = 12.9); of studies that reported age range, the ages of included participants ranged from 18-88. All identified trials were conducted in adult samples. Across all RCTs, 60.9% of participants identified as female (n = 1,180) and 39.1% identified as male (n = 790). Across trials, there were no reports of other gender identities. Nine RCTs reported race, ethnicity, and/or nationality; among these participants, the majority identified as White. The next most prominent racial groups represented were Asian and Black. A specific breakdown of race, ethnicity, and/or nationality is reported in Table 1. Of studies that reported education levels (K = 11), 51.3% of participants completed less than or equal to secondary education. Of studies that reported employment status (K = 14), 62.1% of participants were employed or a student. One study reported income, with 64% of participants reporting more, and 36% reporting less, than an annual income of $50K Canadian Dollars.
3.2.2. Injury Type.
Over half of included RCTs included participants who sustained whiplash (K = 12). Other injury types included fracture (distal radius, hip, malleolar, limb; K = 7), meniscus tear (K = 1), major lower extremity trauma (K = 1), or general categories of injuries (e.g., “upper extremity injuries;” K = 3).
3.2.3. Time Since Injury.
Included studies administered treatment at a variety of timepoints ranging from immediately post injury to 5 years post injury. Time since injury was not always reported, but based on available data and study eligibility criteria, we were able to classify trials as those delivered in the acute (< 3 months post injury; K = 15) or chronic phase (≥ 3 months post injury; K = 8) of post-injury pain. [59] The timing of delivery was unclear in one study.
3.2.4. Session Length and Treatment Duration.
There was variability in session length and treatment duration of included studies, ranging from one [74] to 16 sessions. [52] Four treatments were one session in duration, 11 treatments were between 2-8 sessions, and 8 treatments were between 10-16 sessions. One treatment was a workbook and therefore self-paced. Session length was not consistently specified but of those that were reported length varied from a 60-second to 90-minute sessions.
3.2.5. Delivery of Treatment.
Of the 18 trials that delivered treatment face-to-face, most (K = 7) were delivered by a mental health professional (6 by a psychologist; 1 by a mental health counselor), 6 were delivered by a physical therapist, 3 by an interdisciplinary team, 2 by a researcher, and 1 by a nurse. Of those that were not delivered face-to-face, one each was delivered via text message, audio recording, video, and workbook.
3.2.6. Types of Treatments.
There was variability in treatment type, and the specific theoretical grounding (e.g., CBT) of interventions was not always explicit and/or the treatments contained content from various theoretical orientations. However, in general, most trials described treatment components that included some form of cognitive behavioral therapy or a related approach (e.g., ACT, behavioral therapy, stress inoculation therapy).
3.3. Risk of Bias.
ROB summaries are presented in Figure 2 (overall summary) and Figure 3 (individual summaries). Selection Bias. With regards to random sequence generation, we judged 14 trials as low ROB, 4 trials as high ROB, and 6 trials as unclear ROB. With regards to allocation concealment, we judged 11 trials as low ROB and 13 as unclear ROB. Performance Bias. We judged 1 trial as low risk of blinding participants and personnel bias, 8 as high ROB, and 15 as unclear ROB. Detection Bias. With regards to blinding of outcome assessment, we judged 15 trials as low ROB, 4 as high ROB, and 5 as unclear ROB. Attrition Bias. We judged 13 trials as low risk of incomplete outcome data bias, 6 as high ROB, and 5 as unclear ROB. Reporting Bias. With regards to selective reporting, we judged 4 trials as low ROB, 7 as high ROB, and 13 as unclear ROB.
Figure 2.
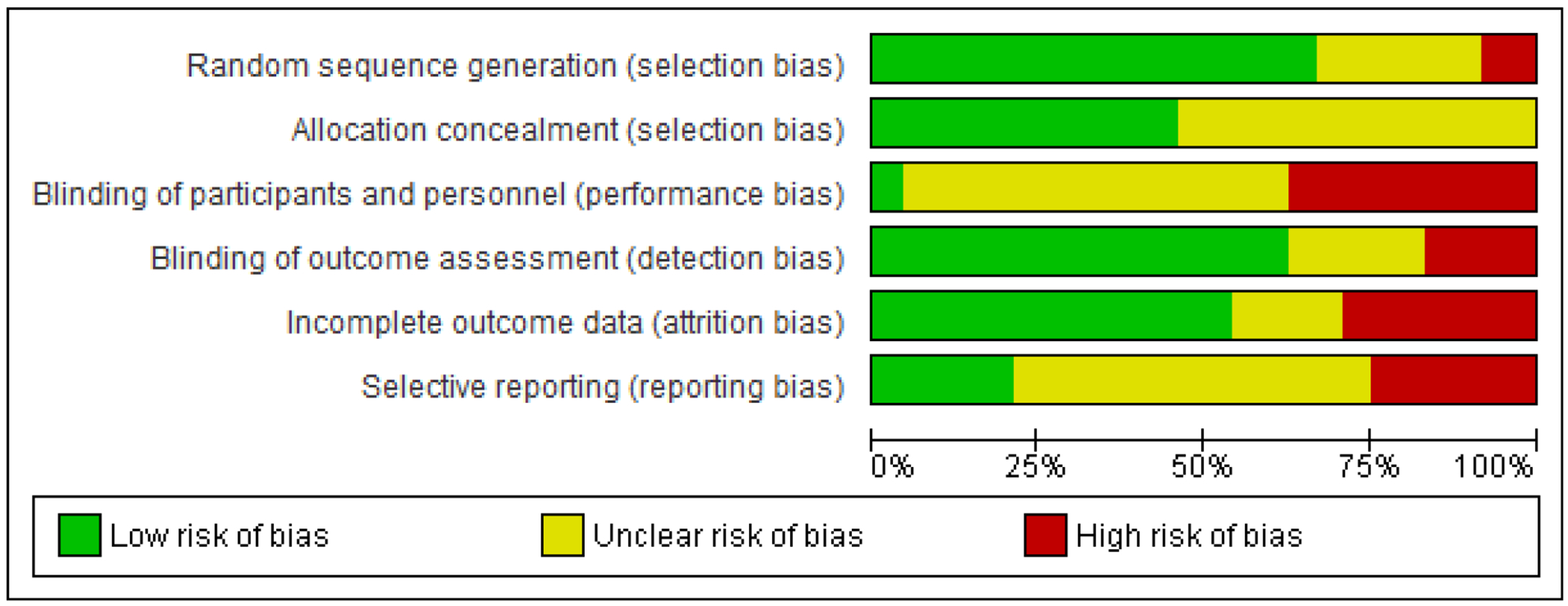
Overall Summary of Risk of Bias
Figure 3.

Individual summary of risk of bias
3.4. Effects of treatments
Sufficient data were available to meta-analyze group differences (treatment vs. control) in outcomes of pain intensity, functional impairment, depression symptoms, anxiety symptoms, and PTSD symptoms, immediately post-treatment and 6-month follow-up. At 12-month follow-up, data were available to meta-analyze the outcomes of pain intensity, functional impairment, and depression, but not anxiety and PTSD symptoms. There were insufficient data to meta-analyze our primary outcomes of opioid consumption, patient ratings of global improvement, or adverse events at any timepoint. We described secondary outcomes of feasibility and acceptance. The results of meta-analyses, including number of studies, number of participants, GRADE ratings, and reasons for downgrading are presented in Table 2. Appendix C provides a summary of findings table with additional information about GRADE ratings for meta-analyzes at post-treatment and adverse events. Six trials were not included in meta-analysis because the necessary data was not available in the article text or by author request [11; 12; 29; 34; 51; 75] or because the nature of its crossover design precluded isolating exposure to pain psychology intervention. [64] A narrative summary of findings from trials not included in meta-analysis is presented in Appendix D.
Table 2.
Summary of Meta-Analyses
| K | N | SMD | 95% CI | I2 | Grade Rating | |
|---|---|---|---|---|---|---|
| Post-Treatment | ||||||
| Pain Intensity | 17 | 1257 | −0.24 | [−0.46, −0.02] | 72% | Very Low1,2,4 |
| Functional Impairment | 12 | 790 | −0.30 | [−0.51, −0.08] | 52% | Very Low1,2,4 |
| Depression | 9 | 604 | −0.43 | [−0.60, −0.26] | 5% | Low2,4 |
| Anxiety | 11 | 837 | −0.30 | [−0.58, −0.01] | 75% | Very Low3,4 |
| PTSD | 7 | 430 | −0.43 | [−0.70, −0.15] | 43% | Low1,4 |
| 6-Month Follow-Up | ||||||
| Pain Intensity | 9 | 766 | −0.08 | [−0.23, 0.07] | 8% | Moderate4 |
| Functional Impairment | 7 | 495 | 0.01 | [−0.17, 0.19] | 0% | Moderate4 |
| Depression | 6 | 430 | −0.31 | [−0.59, −0.04] | 45% | Low2,4 |
| Anxiety | 7 | 661 | −0.19 | [−0.44, 0.06] | 59% | Low2,4 |
| PTSD | 3 | 211 | −0.23 | [−0.50, 0.05] | 0% | Low5 |
| 12-Month Follow-Up | ||||||
| Pain Intensity | 3 | 321 | 0.06 | [−0.30, 0.43] | 64% | Very Low2,5 |
| Functional Impairment | 3 | 321 | −0.08 | [−0.30, 0.14] | 2% | Low5 |
| Depression | 3 | 321 | −0.05 | [−0.28, 0.18] | 10% | Low5 |
Note. K = number of studies; N = Number of participants; SMD = Standardized mean difference; 95% CI = 95% confidence interval.
Downgraded once for limitations to study design and implementation;
Downgraded once for unexplained heterogeneity or inconsistency of results;
Downgraded twice for unexplained heterogeneity or inconsistency of results;
Downgraded once for imprecision of results;
Downgraded twice for imprecision of results
3.4.1. Primary outcomes:
For clarity, we interpret effect sizes, SMD, and 95% CI of meta-analyses in this section. However, we are uncertain about any effect with “very low” certainty of evidence. Effects with “low” certainty should be interpreted with caution as more evidence could change the estimate of effect. For pain intensity, we found a small beneficial effect of psychological therapies at reducing pain intensity post-treatment (SMD −0.24, 95% CI −0.46 to −0.02, I2 72%; Figure 4); However, certainty of evidence was judged as very low. This effect was not maintained at 6-month follow-up (SMD −0.08, 95% CI −0.23 to 0.07, I2 8%) or at 12-month follow-up (SMD 0.06, 95% CI −0.30 to 0.43, I2 64%). Certainty of evidence was judged as moderate at 6-month follow-up and very low at 12-month follow-up.
Figure 4.

Forest plot depicting effect of treatment on pain intensity at post-treatment timepoint and risk of bias of included studies
For functional impairment, we found a moderate beneficial effect of psychological therapies compared to any control at post-treatment (SMD −0.30, 95% CI −0.51 to −0.08, I2 52%); however, certainty of evidence was judged as very low. This effect was not maintained at 6-month follow-up (SMD 0.01, 95% CI −0.17 to 0.19, I2 0%) or 12-month follow-up (SMD −0.08, 95% CI −0.30 to 0.14, I2 2%). Certainty of evidence was judged as moderate at 6-month follow-up and low at 12-month follow-up.
For depression symptoms, we found a moderate beneficial effect of psychological treatments at post-treatment (SMD −0.43, 95% CI −0.60 to −0.26, I2 5%). This effect was maintained at 6-month (SMD −0.31, 95% CI −0.59 to −0.04, I2 45%) but not at 12-month (SMD −0.05, 95% CI −0.28 to 0.18, I2 10%) follow-up. Certainty of evidence was judged as low at all timepoints.
For anxiety symptoms, we found a moderate beneficial effect of psychological therapies post-treatment (SMD −0.30, 95% CI −0.58 to −0.01, I2 75%). The beneficial effect was not maintained at 6-month follow-up (SMD −0.19, 95% CI −0.44 to 0.06, I2 59%). Certainty of evidence was judged as very low at both timepoints.
For PTSD symptoms, we found a moderate beneficial effect for psychological therapies post-treatment (SMD −0.43, 95% CI −0.70 to −0.15, I2 43%). This beneficial effect was not maintained at 6-month follow-up (SMD −0.23, 95% CI −0.50 to 0.05, I2 0%). Certainty of evidence was judged as very low at both timepoints.
There were insufficient data (K = 2) to meta-analyses group differences in opioid consumption. Patients with whiplash who underwent neck-specific exercises with a behavioral approach reported less analgesic medication use at 3 and 6-month follow-up compared to those who received physical therapy alone. [43] Patients with traumatic extremity fracture who underwent a mobile ACT treatment reported less opioid use at 2-week follow-up compared to control. [6] We judged this outcome as low-certainty, downgraded twice for imprecision.
There were insufficient data to meta-analyze differences in patient ratings of global improvement (K = 4; different metrics). In three trials, patients who underwent pain psychology intervention (i.e., CBT, [52] stress inoculation training and PT, [62] neuroscience education [51]) reported greater perceived improvement after treatment. One trial reported no difference in global impression of change between Trauma Focused CBT and control. [4] We rated this outcome as low-certainty, downgraded twice for imprecision and one for indirectness.
Four studies reported adverse events. [2; 4; 62; 75] Across these four trials, one adverse event was reported by one participant in one study. The participant reported an exacerbation of neck pain, which did not result in withdrawal from the trial. No study reported any serious adverse events. We rated this outcome as low-certainty, downgraded once for imprecision and once for indirectness.
3.4.2. Secondary outcomes: Feasibility and Acceptability.
Retention statistics were available for 23 of 24 RCTs. Among those assigned to psychological treatment for pain, post-treatment retention rates ranged from 57% to 100% (21 out of 24 trials reported at least 80% retention). Among those assigned to the control condition, post-treatment retention rates ranged from 49% to 100% (20 out of 24 trials reported at least 80% retention). Reported recruitment barriers included lack of interest, [8; 70; 75] time conflicts, [70; 75] delays scheduling medical care, [75] assessment length, [70] distance to the clinic, [70; 75] and stress associated with trauma. [8] General retention barriers included loss of interest, [2; 4; 52] moving, [2; 24; 52] inability to contact participant, [4; 55] time conflicts, [4; 55] patient hospitalization, [6] patient improvement, [4] legal advice, [52] receiving additional clinical care, [2] cell phone service disconnection, [8] and treatment duration. [52] Five trials described the assessment and monitoring of treatment fidelity. Fidelity assessment included provider adherence checklists, [2; 11; 62] monitoring of audio recordings of sessions, [62] intermittent observation, [75] discussions with the clinical research team, [77] and regular supervision by a psychologist. [12] Two trials reported provider fidelity outcomes, reporting 78% [2] and 95% [62] treatment protocol adherence. One trial measured treatment acceptance, reporting moderate treatment satisfaction using the Client Satisfaction Questionnaire Scale-3. [74]
3.5. Subgroup and sensitivity Analysis.
Given variability in treatment characteristics identified and the moderate to substantial heterogeneity identified in most meta-analyses, we conducted sensitivity analyses isolating whiplash only and sessions greater than one session in duration only and subgroup analyses for treatments delivered in the acute vs. chronic stage of post-trauma recovery and active vs. passive control arm. These analyses are intended to explore heterogeneity and should be interpreted with caution as in all but one case, there were < 10 studies available for comparison. In general, patterns of statistical significance were similar, with one exception. The results of the overall meta-analysis found a small and statistically significant effect of treatment on pain intensity immediately post-treatment, with very low certainty of findings. Several sensitivity analyses (i.e., whiplash, treatments delivered in the acute stage of recovery, treatments with an active control arm) found a nonsignificant effect of treatment on pain intensity immediately post-treatment, with low certainty of findings. The results of these analyses are presented in Appendix E.
4.0. Discussion
This systematic review and meta-analysis reviewed trials that delivered psychological treatments for pain and related symptoms to people who sustained musculoskeletal injuries. We identified 24 RCTs. Trials included patients who had sustained a variety of injury types. Included trials varied in type of psychological treatment delivered (e.g., CBT, ACT), session length and treatment duration, the timing of treatment delivery with respect to initial injury, and provider type. Because the quality of evidence was very low, we are uncertain whether psychological treatment versus control results in improved pain intensity or functional impairment immediately post-treatment. Evidence did not suggest an effect of treatment on these outcomes at 6-month follow-up. Treatment may lead to immediate improvements in depression and PTSD, with moderate effects, and this effect on depression may maintain up to 6-months post-treatment; however, the quality of evidence was low. Across most meta-analyses, the quality of evidence was judged to be low or very low; and, among included studies, as all but two were judged to have at least one domain of high or unclear risk of bias. There was some evidence of reduced opioid use and improved patient ratings of global improvement post-treatment and adverse events were rare in the studies that reported them; however, the quality of evidence for each of these findings was low.
The adjacent evidence from mixed chronic pain samples, such as results from a recent Cochrane review, showed beneficial effects of psychological treatment on pain intensity, functional impairment, and psychological distress immediately post-treatment, and a lack of beneficial treatment effects at follow-up when compared to active control (of note, there was a single overlapping trial included in the current study and this recent Cochrane review [43]). [78] The effect of psychological treatment on pain intensity and functional impairment in the current study is inconclusive due to very low certainty of evidence; the results of exploratory sensitivity analysis suggested that sessions greater than a single session in duration may result in small improvements in pain intensity immediately post-treatment, but otherwise the effects of treatment on pain intensity across numerous subgroup analyses were not significant. Additional research is needed to determine effective psychological approaches for reducing pain intensity after musculoskeletal trauma, particularly given a wealth of findings that psychological interventions can lead to improved pain intensity in general chronic pain populations. Psychological treatments following musculoskeletal injury may be effective for improving psychological outcomes, particularly depression, and this finding was consistent across subgroup and sensitivity analyses. This positive effect of psychological treatments on psychological outcomes is consistent with the results of a recent review of psychological treatments targeting distress after any injury type (not limited to musculoskeletal), which reported beneficial effects of anxiety, depression, and PTSD symptoms at post-treatment and follow-up. [33]
Studies included in the current review were characterized by high or unclear risk of bias, most outcomes were low or very low quality, and there was substantial variability in the treatment characteristics of included studies. Thus, it is premature to draw conclusions about treatment efficacy or to provide specific recommendations about optimal treatment design following musculoskeletal injury. Instead, we focus our discussion on what is known, identified gaps, and areas of improvement, centering around four themes: 1) treatment characteristics, 2) participant and injury characteristics, 3) timing of delivery, and 4) provider type. For all of these themes, we identified marked variability across trials.
Treatment characteristics, including treatment type, session length and treatment duration, varied across trials. For example, studies varied in their incorporation of psychological treatment components, ranging from treatments that were more traditional (e.g., 16 sessions of CBT [52]) to more adaptive (e.g., augmenting PT with CBT with principles of psychological intervention) in design. Unfortunately, in many cases, trials did not provide a clear theoretical and/or empirical rationale for their incorporation of psychological practices. In most cases, trials did not assess or did not report provider training or treatment fidelity. These gaps prevent the generalizability and replicability of findings. Treatments varied in their length and duration, balancing competing demands of scalability and intensity. A sensitivity analysis found no difference in overall effects of treatment when single session interventions were removed; however, additional research is needed to determine the most effective treatment type and dose based on individual risk and protective factors. Ultimately, a comprehensive approach to treating post-injury pain will likely require a range of treatment options to meet the diverse needs of this population and in order to personalize treatment. [46; 73]
Participant and injury characteristics varied widely, in part due to our purposefully broad inclusion criteria. However, several gaps in recruiting and reporting hinder the generalizability of treatment findings and reduce equity in care following musculoskeletal injury. No treatments were delivered to children or adolescents after an injury. A minority of studies reported race, ethnicity, and/or relevant sociodemographic factors (e.g., income). Among studies that reported race, the majority of participants were white. Future research should recruit samples that are sociodemographically representative of the broader population, including youth, in order to promote inclusivity and generalizability of treatment effects across individual identities. Other characteristics should be considered and reported. For example, length of hospitalization, undergoing surgery, and pre-injury chronic pain may impact risk for the development of persistent pain following injury [58] but were not consistently reported in included studies.
The timing of treatment delivery varied across trials, with trials delivering treatment in the acute (<3 months) or chronic (≥ 3 months) stage of post-injury pain. [27; 30] A subgroup analysis comparing treatments in the acute and chronic stage of post-injury pain were largely consistent with findings from the overall meta-analysis, with the exception that there was no significant effect of treatment on pain intensity post-treatment among those interventions delivered in the acute stage. In general, limited research has tested treatments aimed at preventing the transition from acute to chronic pain (i.e. secondary prevention). [27; 30] The available evidence is not promising: a previous meta-analysis of the effect of secondary prevention following acute pain episodes (primarily low back pain and unrelated to injury) found no effect of secondary prevention on pain intensity and depression, and an effect on disability only at 12-month follow-up. [10] Given heightened risk for developing chronic pain, developing effective treatments delivered in the acute stage of post-injury pain is vital, particularly as trajectories of recovery can be determined as early as 4-6 weeks post injury. [13; 22] To comprehensively address the needs of this population, there is need for effective treatment options across the continuum of post-injury pain and a need for additional research to determine the ideal timing of delivery.
Provider type varied across trials. Many psychological treatments were not delivered by a mental health provider. A previous meta-analysis found that psychosocial interventions delivered by a physical therapist for general musculoskeletal pain were effective in reducing pain and disability. [60] Given a shortage of mental health providers trained in pain, the finding that psychological treatments for pain can be delivered with efficacy by non-mental healthcare providers is important. [20] In order to draw conclusions in the future, it is essential that future studies consistently describe provider training and treatment fidelity, particularly when psychological treatments are delivered by non-mental health providers.
4.1. Other Limitations
We aimed to provide a thorough summary of psychological treatments targeting pain following musculoskeletal injury to summarize the current state of the field and to inform future research and clinical practice, and in doing so utilized liberal inclusion criterion. Several indicators of low-quality trials were observed including small sample sizes and passive control conditions and are likely to inflate observed effect sizes. [21] There was variability in the baseline pain and psychological symptoms of participants included in these trials; future research should test the possible moderating effects of elevated pain or distress on treatment efficacy with the goal of individualizing psychological treatment post injury. More rigorous RCTs and diverse trial design (e.g., single case experimental studies, N-of-1 trials) are needed to determine the efficacy of psychological treatments for pain following musculoskeletal injury, moderators of treatment response, and to determine which specific treatment components are most effective.
4.2. Conclusion.
We identified 24 RCTs with variability in treatment characteristics including participant and treatment characteristics, injury characteristics, timing of delivery, and provider type. Due to very low quality evidence, it is uncertain whether psychological treatment for pain has a beneficial effect on pain intensity and functional impairment immediately post-treatment, though evidence suggested a possible positive treatment effect of depression and PTSD. With the exception of a beneficial effect of treatment on depression at 6-months, there was no effect of treatment at 6- or 12-month follow-up. Given the frequency and impact of prolonged pain, disability and distress following injury, a critical goal of future research is to develop treatments that result in lasting improvements in pain-related outcomes. Findings from the chronic literature suggest that achieving long-term improvements is possible. Much remains unknown about the ideal treatment of pain following musculoskeletal injury, including ideal treatment type, dose, and best strategies for stratifying treatment based on individual risk and protective factors. The current systematic review and meta-analysis provides an important step in synthesizing the available evidence and pointing to specific gaps to be addressed in future trials.
Supplementary Material
Acknowledgements.
This work was supported by the Johns Hopkins Clinician Scientist Award (RVA), NIH K23HD104934 (RVA), DOD W81XWH-16-2-0060 (RVA, STW, RCC) DOD JW160020 (STW), NIDILRR H133G140079 (STW), and Versus Arthritis (Career Development Fellowship; EF).
Footnotes
Conflict of Interest: The authors have no conflicts of interest to disclose.
References
- [1].Achterberg J, Kenner C, Casey D. Behavioral strategies for the reduction of pain and anxiety associated with orthopedic trauma. Biofeedback and self-regulation 1989;14(2):101–114. [DOI] [PubMed] [Google Scholar]
- [2].Andersen TE, Ravn SL, Armfield N, Maujean A, Requena SS, Sterling M. Trauma-focused cognitive behavioural therapy and exercise for chronic whiplash with comorbid posttraumatic stress disorder: a randomised controlled trial. Pain 2021;162(4):1221–1232. [DOI] [PubMed] [Google Scholar]
- [3].Andersen TE, Ravn SL, Mejldal A, Roessler KK. Values-based cognitive behavioural therapy for the prevention of chronic whiplash associated disorders: A randomized controlled trial. Eur J Pain 2022;01:01. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [4].Andersen TE, Ravn SL, Mejldal A, Roessler KK. Values‐based cognitive behavioural therapy for the prevention of chronic whiplash associated disorders: A randomized controlled trial. European Journal of Pain 2022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [5].Angst F, Francoise G, Verra M, Lehmann S, Jenni W, Aeschlimann A. Interdisciplinary rehabilitation after whiplash injury: an observational prospective outcome study. Journal of rehabilitation medicine 2010;42(4):350–356. [DOI] [PubMed] [Google Scholar]
- [6].Anthony CA, Rojas EO, Keffala V, Glass NA, Shah AS, Miller BJ, Hogue M, Willey MC, Karam M, Marsh JL. Acceptance and Commitment Therapy Delivered via a Mobile Phone Messaging Robot to Decrease Postoperative Opioid Use in Patients With Orthopedic Trauma: Randomized Controlled Trial. Journal of medical Internet research 2020;22(7):e17750. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [7].Archer KR, Castillo RC, Wegener ST, Abraham CM, Obremskey WT. Pain and satisfaction in hospitalized trauma patients: the importance of self-efficacy and psychological distress. Journal of Trauma and Acute Care Surgery 2012;72(4):1068–1077. [DOI] [PubMed] [Google Scholar]
- [8].Bérubé M, Gélinas C, Feeley N, Martorella G, Côté J, Laflamme G, Rouleau D, Choinière M. Feasibility of a Hybrid Web-Based and In-Person Self-management Intervention Aimed at Preventing Acute to Chronic Pain Transition After Major Lower Extremity Trauma (iPACT-E-Trauma): A Pilot Randomized Controlled Trial. Pain Medicine 2019;20(10):2018–2032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [9].Bérubé M, Gélinas C, Feeley N, Martorella G, Côté J, Laflamme GY, Rouleau DM, Choinière M. A hybrid web-based and in-person self-management intervention aimed at preventing acute to chronic pain transition after major lower extremity trauma: feasibility and acceptability of iPACT-E-trauma. JMIR formative research 2018;2(1):e10323. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [10].Bérubé M, Martorella G, Côté C, Gélinas C, Feeley N, Choinière M, Parent S, Streiner DL. The Effect of Psychological Interventions on the Prevention of Chronic Pain in Adults: A Systematic Review and Meta-analysis. The Clinical Journal of Pain 2021;37(5):379–395. [DOI] [PubMed] [Google Scholar]
- [11].Bring A, Asenlof P, Soderlund A. What is the comparative effectiveness of current standard treatment, against an individually tailored behavioural programme delivered either on the Internet or face-to-face for people with acute whiplash associated disorder? A randomized controlled trial. Clinical rehabilitation 2016;30(5):441–453. [DOI] [PubMed] [Google Scholar]
- [12].Burns A, Banerjee S, Morris J, Woodward Y, Baldwin R, Proctor R, Tarrier N, Pendleton N, Sutherland D, Andrew G, Horan M. Treatment and prevention of depression after surgery for hip fracture in older people: randomized, controlled trials. Journal of the American Geriatrics Society 2007;55(1):75–80. [DOI] [PubMed] [Google Scholar]
- [13].Castillo RC, Huang Y, Scharfstein D, Frey K, Bosse MJ, Pollak AN, Vallier HA, Archer KR, Hymes RA, Newcomb AB. Association Between 6-Week Postdischarge Risk Classification and 12-Month Outcomes After Orthopedic Trauma. JAMA surgery 2019;154(2):e184824–e184824. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [14].Castillo RC, MacKenzie EJ, Wegener ST, Bosse MJ, Pain LSGJ. Prevalence of chronic pain seven years following limb threatening lower extremity trauma. 2006;124(3):321–329. [DOI] [PubMed] [Google Scholar]
- [15].Castillo RC, Wegener ST, Heins SE, Haythornthwaite JA, MacKenzie EJ, Bosse MJ, Group LS. Longitudinal relationships between anxiety, depression, and pain: results from a two-year cohort study of lower extremity trauma patients. PAIN® 2013;154(12):2860–2866. [DOI] [PubMed] [Google Scholar]
- [16].Clay FJ, Newstead SV, Watson WL, Ozanne-Smith J, Guy J, McClure RJ. Bio-psychosocial determinants of persistent pain 6 months after non-life-threatening acute orthopaedic trauma. The Journal of Pain 2010;11(5):420–430. [DOI] [PubMed] [Google Scholar]
- [17].Clay FJ, Watson WL, Newstead SV, McClure RJ. A systematic review of early prognostic factors for persistent pain following acute orthopedic trauma. Pain Research and Management 2012;17(1):35–44. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [18].Cohen J Statistical power analysis Jbr the behavioral. Sciences Hillsdale (NJ): Lawrence Erlbaum Associates; 1988:18–74. [Google Scholar]
- [19].Coronado RA, Sterling EK, Fenster DE, Bird ML, Heritage AJ, Woosley VL, Burston AM, Henry AL, Huston LJ, Vanston SW, Cox CL 3rd, Sullivan JP, Wegener ST, Spindler KP, Archer KR. Cognitive-behavioral-based physical therapy to enhance return to sport after anterior cruciate ligament reconstruction: An open pilot study. Physical therapy in sport : official journal of the Association of Chartered Physiotherapists in Sports Medicine 2020;42:82–90. [DOI] [PubMed] [Google Scholar]
- [20].Darnall BD, Scheman J, Davin S, Burns JW, Murphy JL, Wilson AC, Kerns RD, Mackey SC. Pain psychology: A global needs assessment and national call to action. Pain Medicine 2016;17(2):250–263. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [21].de C Williams AC, Fisher E, Hearn L, Eccleston C. Evidence-based psychological interventions for adults with chronic pain: precision, control, quality, and equipoise. Pain 2021;162(8):2149–2153. [DOI] [PubMed] [Google Scholar]
- [22].deRoon-Cassini TA, Mancini AD, Rusch MD, Bonanno GA. Psychopathology and resilience following traumatic injury: a latent growth mixture model analysis. Rehabilitation psychology 2010;55(1):1. [DOI] [PubMed] [Google Scholar]
- [23].Dunne RL, Kenardy J, Sterling M. A randomized controlled trial of cognitive-behavioral therapy for the treatment of PTSD in the context of chronic whiplash. The Clinical journal of pain 2012;28(9):755–765. [DOI] [PubMed] [Google Scholar]
- [24].Dunne RL, Kenardy J, Sterling M. A randomized controlled trial of cognitive-behavioral therapy for the treatment of PTSD in the context of chronic whiplash. The Clinical journal of pain 2012;28(9):755–765. [DOI] [PubMed] [Google Scholar]
- [25].Dunstan DA, Covic T. Can a rural community-based work-related activity program make a difference for chronic pain-disabled injured workers? The Australian journal of rural health 2007;15(3):166–171. [DOI] [PubMed] [Google Scholar]
- [26].Ehde DM, Dillworth TM, Turner JA. Cognitive-behavioral therapy for individuals with chronic pain: efficacy, innovations, and directions for research. American Psychologist 2014;69(2):153. [DOI] [PubMed] [Google Scholar]
- [27].Fisher E, Eccleston C. Psychological aspects of pain prevention. Pain reports 2021;6(1). [DOI] [PMC free article] [PubMed] [Google Scholar]
- [28].Gabbe BJ, Sleney JS, Gosling CM, Wilson K, Sutherland A, Hart M, Watterson D, Christie N. Financial and employment impacts of serious injury: a qualitative study. Injury 2014;45(9):1445–1451. [DOI] [PubMed] [Google Scholar]
- [29].Gambatesa M, D’Ambrosio A, D’Antini D, Mirabella L, De Capraris A, Iuso S, Bellomo A, Macchiarola A, Dambrosio M, Cinnella G. Counseling, quality of life, and acute postoperative pain in elderly patients with hip fracture. J Multidiscip Healthc 2013;6:335–346. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [30].Gatchel RJ, Reuben DB, Dagenais S, Turk DC, Chou R, Hershey AD, Hicks GE, Licciardone JC, Horn SD. Research agenda for the prevention of pain and its impact: report of the work group on the prevention of acute and chronic pain of the Federal Pain Research Strategy. The journal of pain 2018;19(8):837–851. [DOI] [PubMed] [Google Scholar]
- [31].Ginandes CS, Rosenthal DI. Using hypnosis to accelerate the healing of bone fractures: a randomized controlled pilot study. Alternative therapies in health and medicine 1999;5(2):67–75. [PubMed] [Google Scholar]
- [32].Giordano NA, Seilern Und Aspang J, Baker J, Medline A, Rice CW, Barrell B, Kirk L, Ortega E, Wallace M, Steck A, Schenker ML. Integration of Life Care Specialists Into Orthopaedic Trauma Care to Improve Postoperative Outcomes: A Pilot Study. Pain Manag Nurs 2022. [DOI] [PubMed] [Google Scholar]
- [33].Giummarra MJ, Lennox A, Dali G, Costa B, Gabbe BJ. Early psychological interventions for posttraumatic stress, depression and anxiety after traumatic injury: A systematic review and meta-analysis. Clinical psychology review 2018;62:11–36. [DOI] [PubMed] [Google Scholar]
- [34].Goudie S, Dixon D, McMillan G, Ring D, McQueen M. Is Use of a Psychological Workbook Associated With Improved Disabilities of the Arm, Shoulder and Hand Scores in Patients With Distal Radius Fracture? Clinical orthopaedics and related research 2018;476(4):832–845. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [35].Hall PA, Marshall J, Mercado A, Tkachuk G. Changes in coping style and treatment outcome following motor vehicle accident. Rehabilitation psychology 2011;56(1):43–51. [DOI] [PubMed] [Google Scholar]
- [36].Harvey-Kelly KF, Kanakaris NK, Obakponovwe O, West RM, Giannoudis PV. Quality of life and sexual function after traumatic pelvic fracture. Journal of orthopaedic trauma 2014;28(1):28–35. [DOI] [PubMed] [Google Scholar]
- [37].Helmerhorst GT, Vranceanu A-M, Vrahas M, Smith M, Ring D. Risk factors for continued opioid use one to two months after surgery for musculoskeletal trauma. JBJS 2014;96(6):495–499. [DOI] [PubMed] [Google Scholar]
- [38].Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA. Cochrane handbook for systematic reviews of interventions: John Wiley & Sons, 2019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [39].Holley AL, Wilson AC, Palermo TM. Predictors of the transition from acute to persistent musculoskeletal pain in children and adolescents: a prospective study. Pain 2017;158(5):794. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [40].Holman JE, Stoddard GJ, Higgins TF. Rates of prescription opiate use before and after injury in patients with orthopaedic trauma and the risk factors for prolonged opiate use. Journal of Bone and Joint Surgery 2013;95(12):1075–1080. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [41].Hsu JR, Mir H, Wally MK, Seymour RB. Clinical practice guidelines for pain management in acute musculoskeletal injury. Journal of orthopaedic trauma 2019;33(5):e158. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [42].Jayakumar P, Overbeek CL, Lamb S, Williams M, Funes C, Gwilym S, Ring D, Vranceanu A-M. What Factors Are Associated With Disability After Upper Extremity Injuries? A Systematic Review. Clinical orthopaedics and related research 2018;476(11):2190–2215. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [43].Ludvigsson ML, Peterson G, O’Leary S, Dedering A, Peolsson A. The effect of neck-specific exercise with, or without a behavioral approach, on pain, disability, and self-efficacy in chronic whiplash-associated disorders: a randomized clinical trial. The Clinical journal of pain 2015;31(4):294–303. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [44].MacKenzie EJ, Bosse MJ, Pollak AN, Webb LX, Swiontkowski MF, Kellam JF, Smith DG, Sanders RW, Jones AL, Starr AJ. Long-term persistence of disability following severe lower-limb trauma: Results of a seven-year follow-up. JBJS 2005;87(8):1801–1809. [DOI] [PubMed] [Google Scholar]
- [45].MacKenzie EJ, Morris JA Jr, Jurkovich GJ, Yasui Y, Cushing BM, Burgess AR, DeLateur BJ, McAndrew MP, Swiontkowski MF. Return to work following injury: the role of economic, social, and job-related factors. American journal of public health 1998;88(11):1630–1637. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [46].METRC. Early Effects of the Trauma Collaborative Care Intervention: Results From a Prospective Multicenter Cluster Clinical Trial. Journal of orthopaedic trauma 2019;33(11):538–546. [DOI] [PubMed] [Google Scholar]
- [47].Middlebrook N, Rushton AB, Abichandani D, Kuithan P, Heneghan NR, Falla D. Measures of central sensitization and their measurement properties in musculoskeletal trauma: A systematic review. European Journal of Pain 2021;25(1):71–87. [DOI] [PubMed] [Google Scholar]
- [48].Mock C, Cherian MN. The global burden of musculoskeletal injuries: challenges and solutions. Clinical orthopaedics and related research 2008;466(10):2306. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [49].Moher D, Liberati A, Tetzlaff J, Altman DG, Group* P. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Annals of internal medicine 2009;151(4):264–269. [DOI] [PubMed] [Google Scholar]
- [50].New PW, Lim TC, Hill ST, Brown DJ. A survey of pain during rehabilitation after acute spinal cord injury. Spinal cord 1997;35(10):658–663. [DOI] [PubMed] [Google Scholar]
- [51].Ottosson C, Pettersson H, Johansson SE, Nyrén O, Ponzer S. Recovery after minor traffic injuries: A randomized controlled trial. PLoS Clinical Trials 2007;2(3). [DOI] [PMC free article] [PubMed] [Google Scholar]
- [52].Pato U, Di Stefano G, Fravi N, Arnold M, Curatolo M, Radanov BP, Ballinari P, Sturzenegger M. Comparison of randomized treatments for late whiplash. Neurology 2010;74(15):1223–1230. [DOI] [PubMed] [Google Scholar]
- [53].Ritchie C, Clanchy K, Sterling M, Tate R, Smits EJ, Day M, Nikles J, Liimatainen J, Tweedy SM. Evaluation of a physical activity promotion intervention for adults with whiplash associated disorders: a single-case experimental design study. Disabil Rehabil 2021:1–14. [DOI] [PubMed] [Google Scholar]
- [54].Robinson JP, Theodore BR, Dansie EJ, Wilson HD, Turk DC. The role of fear of movement in subacute whiplash-associated disorders grades I and II. Pain 2013;154(3):393–401. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [55].Robinson JP, Theodore BR, Dansie EJ, Wilson HD, Turk DC. The role of fear of movement in subacute whiplash-associated disorders grades I and II. PAIN® 2013;154(3):393–401. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [56].Rosenbloom BN, Khan S, McCartney C, Katz JJJopr. Systematic review of persistent pain and psychological outcomes following traumatic musculoskeletal injury. 2013;6:39. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [57].Ross MJ, Berger RS. Effects of stress inoculation training on athletes’ postsurgical pain and rehabilitation after orthopedic injury. Journal of consulting and clinical psychology 1996;64(2):406–410. [DOI] [PubMed] [Google Scholar]
- [58].Schug SA, Bruce J. Risk stratification for the development of chronic postsurgical pain. Pain Reports 2017;2(6). [DOI] [PMC free article] [PubMed] [Google Scholar]
- [59].Schug SA, Lavand’homme P, Barke A, Korwisi B, Rief W, Treede R-D. The IASP classification of chronic pain for ICD-11: chronic postsurgical or posttraumatic pain. Pain 2019;160(1):45–52. [DOI] [PubMed] [Google Scholar]
- [60].Silva Guerrero AV, Maujean A, Campbell L, Sterling M. A systematic review and meta-analysis of the effectiveness of psychological interventions delivered by physiotherapists on pain, disability and psychological outcomes in musculoskeletal pain conditions. The Clinical journal of pain 2018;34(9):838–857. [DOI] [PubMed] [Google Scholar]
- [61].Söderlund A, Lindberg P. Cognitive behavioural components in physiotherapy management of chronic whiplash associated disorders (WAD) - A randomised group study. Physiotherapy Theory and Practice 2001;17(4):229–238. [PubMed] [Google Scholar]
- [62].Sterling M, Smeets R, Keijzers G, Warren J, Kenardy J. Physiotherapist-delivered stress inoculation training integrated with exercise versus physiotherapy exercise alone for acute whiplash-associated disorder (StressModex): a randomised controlled trial of a combined psychological/physical intervention. British journal of sports medicine 2019;53(19):1240–1247. [DOI] [PubMed] [Google Scholar]
- [63].Sullivan MJL, Adams H, Rhodenizer T, Stanish WD. A psychosocial risk factor–targeted intervention for the prevention of chronic pain and disability following whiplash injury. Physical therapy 2006;86(1):8–18. [DOI] [PubMed] [Google Scholar]
- [64].Tobbackx Y, Meeus M, Wauters L, De Vilder P, Roose J, Verhaeghe T, Nijs J. Does acupuncture activate endogenous analgesia in chronic whiplash-associated disorders? A randomized crossover trial. European journal of pain (London, England) 2013;17(2):279–289. [DOI] [PubMed] [Google Scholar]
- [65].Turk DC, Dworkin RH, Allen RR, Bellamy N, Brandenburg N, Carr DB, Cleeland C, Dionne R, Farrar JT, Galer BS. Core outcome domains for chronic pain clinical trials: IMMPACT recommendations. Pain 2003;106(3):337–345. [DOI] [PubMed] [Google Scholar]
- [66].Van Oosterwijck J, Nijs J, Meeus M, Truijen S, Craps J, Van den Keybus N, Paul L. Pain neurophysiology education improves cognitions, pain thresholds, and movement performance in people with chronic whiplash: a pilot study. Journal of rehabilitation research and development 2011;48(1):43–58. [DOI] [PubMed] [Google Scholar]
- [67].Vincent HK, Horodyski M, Vincent KR, Brisbane ST, Sadasivan KKJP. Psychological distress after orthopedic trauma: prevalence in patients and implications for rehabilitation. 2015;7(9):978–989. [DOI] [PubMed] [Google Scholar]
- [68].Vranceanu A-M, Bachoura A, Weening A, Vrahas M, Smith RM, Ring D. Psychological factors predict disability and pain intensity after skeletal trauma. JBJS 2014;96(3):e20. [DOI] [PubMed] [Google Scholar]
- [69].Vranceanu A-M, Bakhshaie J, Reichman M, Doorley J, Mace RA, Jacobs C, Harris M, Archer KR, Ring D, Elwy AR. Understanding barriers and facilitators to implementation of psychosocial care within orthopedic trauma centers: a qualitative study with multidisciplinary stakeholders from geographically diverse settings. Implementation science communications 2021;2(1):1–17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [70].Vranceanu A-M, Hageman M, Strooker J, Ter Meulen D, Vrahas M, Ring D. A preliminary RCT of a mind body skills based intervention addressing mood and coping strategies in patients with acute orthopaedic trauma. Injury 2015;46(4):552–557. [DOI] [PubMed] [Google Scholar]
- [71].Vranceanu A-M, Jacobs C, Lin A, Greenberg J, Funes CJ, Harris MB, Heng MM, Macklin EA, Ring D. Results of a feasibility randomized controlled trial (RCT) of the Toolkit for Optimal Recovery (TOR): a live video program to prevent chronic pain in at-risk adults with orthopedic injuries. Pilot and feasibility studies 2019;5(1):30. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [72].Wald J, Taylor S, Chiri LR, Sica C. Posttraumatic stress disorder and chronic pain arising from motor vehicle accidents: efficacy of interoceptive exposure plus trauma-related exposure therapy. Cognitive behaviour therapy 2010;39(2):104–113. [DOI] [PubMed] [Google Scholar]
- [73].Wegener ST, Pollak AN, Frey KP, Hymes RA, Archer KR, Jones CB, Seymour RB, O’Toole RV, Castillo RC, Huang Y. The trauma collaborative care study (TCCS). Journal of orthopaedic trauma 2017;31:S78–S87. [DOI] [PubMed] [Google Scholar]
- [74].Westenberg RF, Zale EL, Heinhuis TJ, Ozkan S, Nazzal A, Lee S-G, Chen NC, Vranceanu A-M. Does a Brief Mindfulness Exercise Improve Outcomes in Upper Extremity Patients? A Randomized Controlled Trial. Clinical orthopaedics and related research 2018;476(4):790–798. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [75].Wiangkham T, Duda J, Haque MS, Price J, Rushton A. A cluster randomised, double-blind pilot and feasibility trial of an active behavioural physiotherapy intervention for acute whiplash-associated disorder (WAD)II. PloS one 2019;14(5):e0215803. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [76].Wicksell RK, Ahlqvist J, Bring A, Melin L, Olsson GL. Can exposure and acceptance strategies improve functioning and life satisfaction in people with chronic pain and whiplash-associated disorders (WAD)? A randomized controlled trial. Cognitive behaviour therapy 2008;37(3):169–182. [DOI] [PubMed] [Google Scholar]
- [77].Wicksell RK, Ahlqvist J, Bring A, Melin L, Olsson GL. Can exposure and acceptance strategies improve functioning and life satisfaction in people with chronic pain and Whiplash‐Associated Disorders (WAD)? A randomized controlled trial. Cognitive behaviour therapy 2008;37(3):169–182. [DOI] [PubMed] [Google Scholar]
- [78].Williams A, Fisher E, Hearn L, Eccleston C. Psychological therapies for the management of chronic pain (excluding headache) in adults. Cochrane database of systematic reviews 2020(8). [DOI] [PMC free article] [PubMed] [Google Scholar]
- [79].Wong EM- L, Chan SW- C, Chair S-Y. Effectiveness of an educational intervention on levels of pain, anxiety and self-efficacy for patients with musculoskeletal trauma. Journal of advanced nursing 2010;66(5):1120–1131. [DOI] [PubMed] [Google Scholar]
- [80].Wong EML, Chair SY, Leung DY, Chan SWC. Can a brief educational intervention improve sleep and anxiety outcomes for emergency orthopaedic surgical patients? Contemporary nurse 2014;47(1-2):132–143. [DOI] [PubMed] [Google Scholar]
- [81].Wood C, Cutshall SM, Lawson DK, Ochtrup HM, Henning NB, Larsen BE, Bauer BA, Mahapatra S, Wahner-Roedler DL. Music Therapy for Anxiety and Pain After Spinal Cord Injury: A Pilot Study. Global Advances In Health and Medicine 2021;10. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [82].Zatzick DF, Rivara FP, Nathens AB, Jurkovich GJ, Wang J, Fan M-Y, Russo J, Salkever DS, MacKenzie EJ. A nationwide US study of post-traumatic stress after hospitalization for physical injury. Psychological medicine 2007;37(10):1469–1480. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.


