Abstract
Background
Whether the effect of the unfixed mesh during laparoscopic total extraperitoneal (TEP) inguinal hernia repair can lead to hernia recurrence remains controversial.
Methods
The PubMed, Cochrane Library, and EMBASE databases were searched to retrieve clinical randomized controlled trials (RCTs) comparing nonfixation of mesh and fixation of mesh in TEP inguinal hernia repair, and we performed a metaanalysis with RevMan 5.3 software.
Results
Fifteen RCTs were included in the metaanalysis, which showed that the operation time (P = 0.001) of the unfixed mesh group was shorter than that of the fixed mesh group; additionally, the postoperative 24-h pain score (P = 0.04) and incidence of urinary retention (P = 0.001) were lower in the unfixed mesh group. There was no significant difference between the unfixed mesh group and the fixed mesh group in terms of hospital stay (P = 0.47), time to resume normal activities (P = 0.51), incidence of haematoma (P = 0.96), incidence of chronic pain (P = 0.20), and recurrence rate (P = 0.09).
Conclusion
Unfixed mesh in TEP inguinal hernia repair shows no elevated recurrence rates compared to fixed mesh and is clinically safe.
Keywords: Inguinal hernia, Laparoscopic, Mesh fixation, Meta-analysis
Highlights
-
•
Laparoscopic TEP inguinal hernia repair offers rapid recovery and low recurrence.
-
•
Controversy exists over the need for mesh fixation in TEP repair.
-
•
Meta-analysis of 15 trials shows unfixed mesh shortens operation time and reduces 24-hour pain and urinary retention.
-
•
No significant difference in hospital stay, activity resumption, chronic pain, or recurrence between fixed and unfixed mesh.
-
•
Findings suggest unfixed mesh is a viable option in TEP inguinal hernia repair.
Introduction
After >100 years of development, herniorrhaphy has undergone several changes. With the continuous improvement of surgeons' understanding of the inguinal region anatomy and the causative mechanisms of hernias, as well as the application of artificial meshes and the popularity of tension-free inguinal hernia repair, minimally invasive techniques and concepts have become increasingly popular in recent years, which has increased the popularity of laparoscopic inguinal hernia repair [[1], [2], [3]]. At present, laparoscopic total extraperitoneal (TEP) inguinal hernia repair and laparoscopic transabdominal preperitoneal (TAPP) inguinal hernia repair are the main clinical laparoscopic inguinal hernia repair methods [4]. TEP inguinal hernia repair does not enter the abdominal cavity and repairs the abdominal wall defect in the preperitoneal space, which has the advantages of rapid postoperative recovery, mild pain, low recurrence rate and low complications [5,6]. However, whether the mesh should be fixed during TEP inguinal hernia repair has always been controversial [7,8].
Some studies believe that displacement of the mesh is the main cause of postoperative hernia recurrence; therefore, fixing the mesh has been recommended to prevent hernia recurrence [3,9]. However, other studies believe that the fixation of mesh is related to nerve injury, foreign body sensation in the operation area and chronic pain. The authors of these studies advocated that the mesh should not be fixed during TEP inguinal hernia repair [10,11]. The aim of this study is systematically analyzed published controlled clinical trials (RCTs) to compare the treatment outcomes of unfixed mesh versus fixed mesh in TEP inguinal hernia repair. We employed the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) system to evaluate outcome indicators, aiming to investigate the safety and effectiveness of unfixed mesh in TEP inguinal hernia repair and provide valuable insights for clinical decision-making.
Material and methods
This study was conducted in accordance with PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) [12] and AMSTAR (Assessing the methodological quality of systematic reviews) Guidelines [13]. The protocol was registered on INPLASY prospectively (Registry number is INPLASY2022120044).
Criteria for inclusion and exclusion of literature
Inclusion criteria
(1) Subjects: Adult patients with inguinal hernia; (2) Intervention: The mesh was not fixed or fixed, with no limitation on the type of mesh; (3) Type of study: RCTs; and (4) Outcome indicators: Operation time, postoperative 24-hour pain score, hospital stay, time to resume normal activities after operation, incidence of haematoma, incidence of urinary retention, incidence of chronic pain, and recurrence rate. Chronic pain following inguinal hernia surgery is defined as pain that persists for more than three months after the inguinal hernia repair surgery [14].
Exclusion criteria
(1) Nonrandomized controlled trial; (2) Repeated publication of literature; (3) Literature for which outcome indicators cannot be extracted; (4) Full text literature cannot be obtained; (5) Subjects were <18 years old; and (6) The operation method was TAPP inguinal hernia repair.
Retrieval strategy
A computer search of the Cochrane Library, Embase database, and PubMed databases was completed. The database search terms were inguinal hernia, groin hernia, TEP, total extraperitoneal repair, hernioplasty, mesh fixation, no-fixation, nonfixation, staple, and tack. Additionally, references of the included articles were manually searched to determine whether they met the inclusion criteria.
Literature screening and data extraction
According to the set inclusion and exclusion criteria, two authors independently read the retrieved literature, and a third author participated in the discussion to achieve resolution when there was a disagreement. When possible, missing data was obtained by contacting the original author. During literature screening, the title and abstract were first read, and after excluding obviously irrelevant literature, the full text was further read to determine whether the text could be included.
Quality evaluation
The two authors independently evaluated the risk of bias included in the study, cross-checked the results and negotiated when they disagreed. The bias risk assessment tool recommended in 5.3 of the Cochrane System Evaluator's Manual was used to evaluate the quality of the included RCTs, including random sequence generation, allocation concealment, blinding of study subjects and performers, blinding of outcome assessors, and incomplete outcomes data, selective reporting, and other biases [15].
Statistical analysis
RevMan 5.3 software provided by the Cochrane Collaboration was used for meta-analysis. The risk ratio (RR) was used as the effect size for dichotomous variables, and the weighted mean difference (WMD) was used as the effect size for continuous variables. All effects were expressed as the 95 % confidence interval (CI). The χ2 test was used to analyse the heterogeneity among the included studies, and I2 was used to quantitatively determine the magnitude of heterogeneity. If there was no statistical heterogeneity among the studies (P > 0.10, I2 ≤ 50 %), the fixed effect model was used for meta-analysis. In contrast, after excluding obvious clinical heterogeneity, a random effect model was used for meta-analysis [16]. Subgroup analysis, sensitivity analysis, or only descriptive analysis was conducted for studies with obvious heterogeneity. When the number of included studies of relevant research indicators was ≥10, the publication bias test was conducted by inverted funnel plot and Egger's test [17].
Quality assessment of evidence
GRADEprofiler 3.6 was used to assess the quality of evidence for each outcome indicator. Based on five aspects, including risk of bias, inconsistency, indirectness, imprecision, and publication bias, the outcome indicators were categorized into four levels: high, moderate, low, and very low [18].
Results
Literature search results
Initially, a total of 1391 studies were retrieved through various databases, and 2 studies were manually retrieved. After reading the titles and abstracts, 219 duplicates were excluded, 1073 studies were determined to be irrelevant to the research purpose, and 76 studies were experience summaries, case reports or reviews. The remaining 25 studies were read and rescreened; 4 studies without a control group, 2 studies without outcome indicators, and 4 nonrandomized controlled studies were excluded. After the above layer-by-layer screening, 15 [[19], [20], [21], [22], [23], [24], [25], [26], [27], [28], [29], [30], [31], [32], [33]] studies were finally included. The screening process is shown in Fig. 1. The basic information of the literature is shown in Table 1.
Fig. 1.
Study selection.
Table 1.
Characteristics of the studies included in this meta-analysis.
| Study | Country | Group | Sample size (M/F) | Age (years) | Fixing method | Type of mesh | Follow-up time | Outcome indicators |
|---|---|---|---|---|---|---|---|---|
| Abd-Raboh 2018 | Egypt | Non-fixation | 27 (27/0) | 36.70 ± 11.35 | None | Polypropylene mesh 12*15 cm | 10.15 ± 3.31 m | ①②③⑤⑧ |
| [19] | Fixation | 31 (30/1) | 35.84 ± 12.67 | Non absorbable tacks or absorbable tacks | Polypropylene mesh 12*15 cm | 9.68 ± 2.81 m | ||
| Acar 2020 [20] | Turkey | Non-fixation | 106 (101/5) | 48 (18–83) y | None | Bard 3D Max | 45 (30–67) m | ①⑤⑦⑧ |
| Fixation | 72 (70/2) | 48 (18–83) y | Absorbable tucker | Bard 3D Max | 45 (30–67) m | |||
| Buyukasik 2017 [21] | Turkey | Non-fixation | 50 (50/0) | 31.1 ± 12.8 | None | Polypropylene mesh 10*15 cm | 12 m | ①⑥⑧ |
| Fixation | 50 (50/0) | 27.3 ± 7.0 | Spiral tacks | Polypropylene mesh 10*15 cm | 12 m | |||
| Claus 2016 [22] | Brazil | Non-fixation | 50 (44/6) | 51.1 ± 15.7 | None | Polypropylene mesh 12*15 cm | at least 3 m | ①⑧ |
| Fixation | 10 (10/0) | 49.0 ± 14.0 | Absorbable mechanical stapler | Polypropylene mesh 12*15 cm | at least 3 m | |||
| Ferzli 1999 [23] | USA | Non-fixation | 49 (49/0) | Na | None | polypropylene mesh 6*6-in2 | 1y | ④⑧ |
| Fixation | 43 (43/0) | Na | Endoscopic Hernia Stapler | polypropylene mesh 6*6-in2 | 1y | |||
| Garg 2011 [24] | India | Non-fixation | 52 (49/3) | 51.9 ± 16.8 | None | Polypropylene mesh 10*15 cm | 2y | ①②③④⑤⑥⑧ |
| Fixation | 52 (51/1) | 47.2 ± 12.9 | Stapler | Polypropylene mesh 10*15 cm | 2y | |||
| Koch 2006 [25] | USA | Non-fixation | 20 (20/0) | 54.6 ± 16.1 | None | 15*10 cm mesh (3DMAX,) | 9(6–30) m | ①③⑥⑧ |
| Fixation | 20 (20/0) | 56.3 ± 11.5 | Spiral tacks | Polypropylene mesh was trimmed to the appropriate size | 9(6–30) m | |||
| Li 2007 [26] | China | Non-fixation | 30 (26/4) | 58 ± 15 | None | Polypropylene mesh 10*15 cm | 12–24 | ①②③④⑤⑧ |
| Fixation | 30 (28/2) | 61 ± 15 | Spiral tacks | Polypropylene mesh 10*15 cm | 12–24 | |||
| Moreno-Egea 2004 [27] | Spain | Non-fixation | 85 (79/6) | 56.9 ± 16.3 | None | 3-dimensional, anatomical mesh | 36 ± 12 m | ②⑦⑧ |
| Fixation | 85 (78/7) | 53.8 ± 15.6 | Stapling | 3-dimensional, anatomical mesh | 36 ± 12 m | |||
| Parshad 2005 [28] | India | Non-fixation | 25 (Na/Na) | 47.16 ± 16.40 | None | Polypropylene mesh 15*11 cm to 15*13 cm | 23.98 ± 9.9 m | ②④⑤⑦⑧ |
| Fixation | 25 (Na/Na) | 46.40 ± 15.19 | Stapler | Polypropylene mesh 15 *11 cm to 15*13 cm | 27.47 ± 8.64 m | |||
| Pielaciński 2020 [29] | Poland | Non-fixation | 18 (18/0) | 47.3 ± 10.4 | None | Ultrapro mesh (15 *10 cm) | 12 m | ①③④⑤⑦⑧ |
| Fixation | 49 (49/0) | 50.1 ± 13.6 | AbsorbaTack Fixation Device | Ultrapro mesh (15 *10 cm) | 12 m | |||
| Reddy 2017 [30] | India | Non-fixation | 15 (Na/Na) | Na | Na | Na | 18 m | ②⑧ |
| Fixation | 15 (Na/Na) | Na | Na | Na | 18 m | |||
| Shen 2017 [31] | China | Non-fixation | 80 (65/15) | 60.0 ± 13.5 | None | Polypropylene mesh 10*15 cm | 12 m | |
| Fixation | 80 (56/24) | 55.9 ± 14.6 | NBCA medical adhesive | Polypropylene mesh 10*15 cm | 12 m | |||
| Taylor 2008 [32] | Australia | Non-fixation | 180 (Na/Na) | 59.5 (18–91) | None | Polypropylene mesh 10*15 cm | 8.2(6–13) m | ①⑧ |
| Fixation | 180 (Na/Na) | 59.5 (18–91) | Titanium spiral tacks | Polypropylene mesh 10*15 cm | 8.2(6–13) m | |||
| Yıldırım 2022 [33] | Turkey | Non-fixation | 50 (45/5) | 50.58 ± 17.3 | None | Polypropylene mesh 12*15 cm | 6 m | ①③④⑤⑧ |
| Fixation | 50 (47/3) | 52.28 ± 16.64 | Non-absorbable staples | Polypropylene mesh 12*15 cm | 6 m |
F, Female; M, Male; m, month; Na, not available; NBCA, n-butyl-2-cyanoacrylate; y, year. ① Operation time; ② Postoperative 24-hour pain score; ③ Hospital stay; ④ Time to resume normal activities after operation; ⑤ Incidence of haematoma; ⑥ Incidence of urinary retention; ⑦ Incidence of chronic pain; ⑧ Recurrence rate.
Literature quality evaluation results
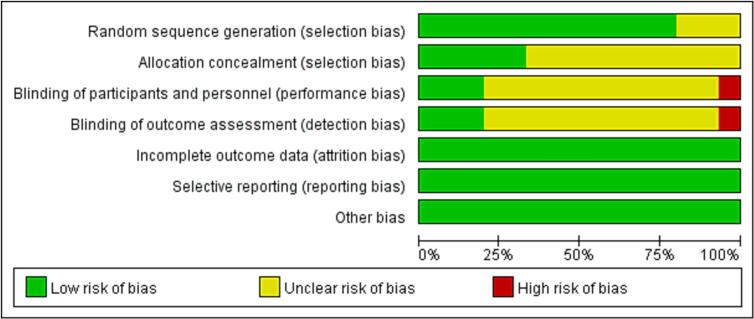
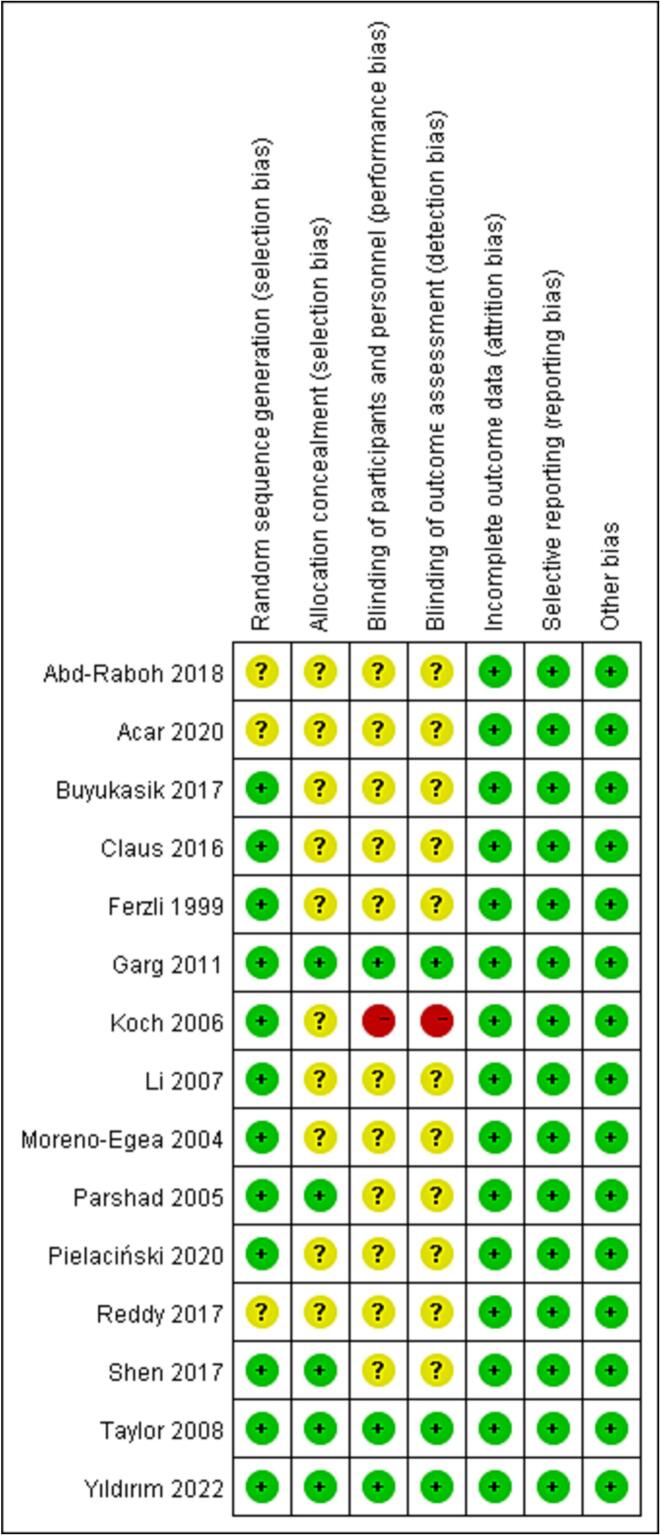
All 15 studies were RCTs [[19], [20], [21], [22], [23], [24], [25], [26], [27], [28], [29], [30], [31], [32], [33]]. Among them, 12 studies [[21], [22], [23], [24], [25], [26], [27], [28], [29],[31], [32], [33]] used a correct randomization method, and 3 studies [19,20,30] did not describe the randomization method. Five studies [24,28,[31], [32], [33]] used allocation concealment, and 10 studies [[19], [20], [21], [22], [23],[25], [26], [27],29,30] did not describe whether allocation concealment was used. Three studies [24,32,33] blinded subjects and practitioners, 11 studies [[19], [20], [21], [22], [23],[26], [27], [28], [29], [30], [31]] did not describe whether subjects and practitioners were blinded, and 1 study [25] clearly described that the subjects and practitioners were not blinded. Three studies [24,32,33] had blinded outcome assessors, 11 studies [[19], [20], [21], [22], [23],[26], [27], [28], [29], [30], [31]] did not describe whether the outcome assessors were blinded, and one study [25] explicitly indicated that the outcome assessors were not blinded. None of the studies [[19], [20], [21], [22], [23], [24], [25], [26], [27], [28], [29], [30], [31], [32], [33]] had incomplete outcome data, selective outcome reports, or other biases. See Fig. 2, Fig. 3 for details.
Fig. 2.
Risk of bias graph for randomized controlled trials included in this study.
Fig. 3.
Summary of the risk of bias analysis for the randomized controlled trials included in this study.
Meta-analysis results
Operation time
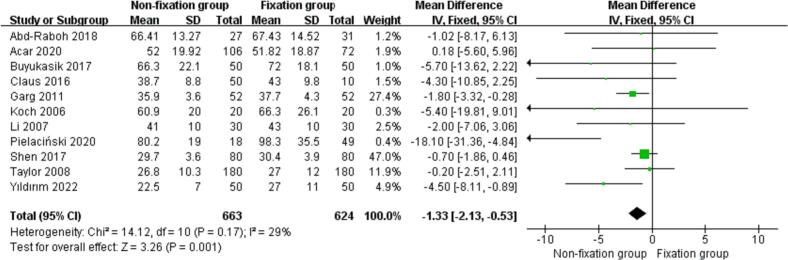
Eleven studies [[19], [20], [21], [22],[24], [25], [26],29,[31], [32], [33]] reported the operation time of the nonfixation group compared with that of the fixation group for TEP inguinal hernia repair. There was no statistical heterogeneity among the studies (P = 0.17, I2 = 29 %). The results showed that the operation time of the nonfixation group was shorter than that of the fixation group [MD = -1.33 min, 95 % CI (−2.13, −0.53), P = 0.001], and the difference was statistically significant. See Fig. 4 for details.
Fig. 4.
Comparison of operation time between the two groups.
Pain score 24 h after surgery
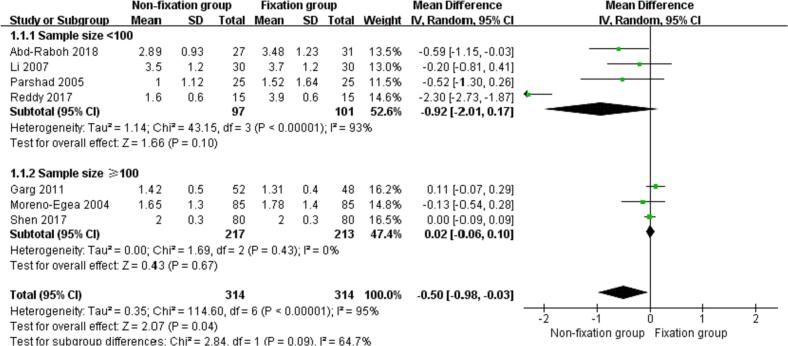
Seven studies [19,24,[26], [27], [28],30,31] reported the pain score 24 h after surgery of the nonfixation group compared with that of the fixation group for TEP inguinal hernia repair, and there was statistical heterogeneity among the studies (P < 0.00001, I2 = 95 %). Meta-analysis was performed using a random effect model combined with effect size. The results showed that the pain score 24 h after surgery of the nonfixation group was lower than that of the fixation group [MD = -0.50, 95 % CI (−0.98, 0.03), P = 0.04], and the difference was statistically significant. According to their sample size, the studies were divided into groups with a sample size of <100 cases and groups with a sample size of >100 cases. Four studies [19,26,28,30] with a sample size of <100 patients reported pain scores 24 h after surgery between the nonfixation group and the fixation group for TEP inguinal hernia repair, and there was statistical heterogeneity among the studies (P < 0.00001, I2 = 93 %). Using a random-effects model combined with effect size for meta-analysis, the results showed that there was no significant difference in the pain score 24 h after surgery between the nonfixation group and the fixation group for TEP inguinal hernia repair [MD = -0.92, 95 % CI (−2.01, 0.17), P = 0.10]. After the sensitivity analysis test, the deletion of the study of Reddy et al. [30] changed the test results, suggesting that the stability of the results in this subgroup was poor; therefore, additional research on this aspect is recommended. Three studies [24,27,31] with a sample size of >100 patients reported pain scores for the nonfixation group and the fixation group 24 h after TEP inguinal hernia repair, and there was no statistical heterogeneity among the studies (P = 0.43, I2 = 0 %). A fixed-effect model combined with effect size was used for meta-analysis, and the results showed that there was no significant difference between the pain score 24 h after surgery between the nonfixation group and the fixation group for TEP inguinal hernia repair [MD = 0.02, 95 % CI] (−0.06, 0.10), P = 0.67]. See Fig. 5 for details.
Fig. 5.
Comparison of pain score 24 h after surgery between the two groups.
Hospital stay
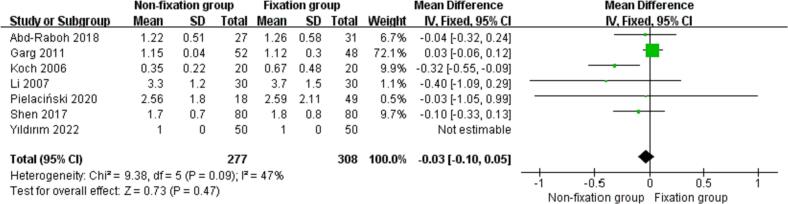
Seven studies [19,[24], [25], [26],29,31,33] reported the length of hospital stay in the nonfixation group compared with that in the fixation group for TEP inguinal hernia repair, and there was no statistical heterogeneity among the studies (P = 0.09, I2 = 47 %). Meta-analysis was conducted using the fixed-effect model combined with effect size. The results indicated that there was no significant difference in the length of hospital stay between the nonfixation group and the fixation group [MD = -0.03 days, 95 % CI (−0.10, 0.05), P = 0.47]. See Fig. 6 for details.
Fig. 6.
Comparison of hospital stay between the two groups.
Days to normal activity
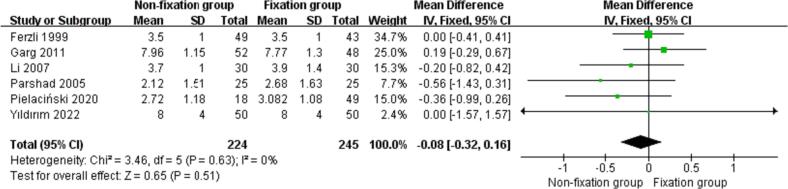
Six studies [23,24,26,28,29,33] reported the days to normal activities in the nonfixation group compared with that in the fixation group for TEP inguinal hernia repair, and there was no statistical heterogeneity among the studies (P = 0.63, I2 = 0 %). The fixed effect model combined with the effect size was used for meta-analysis, and the results showed that there was no significant difference in the days to normal activities between the nonfixation group and the fixation group [MD = -0.08 days, 95 % CI (−0.32, 0.16), P = 0.51]. See Fig. 7 for details.
Fig. 7.
Comparison of days to normal activities between the two groups.
Incidence of haematoma
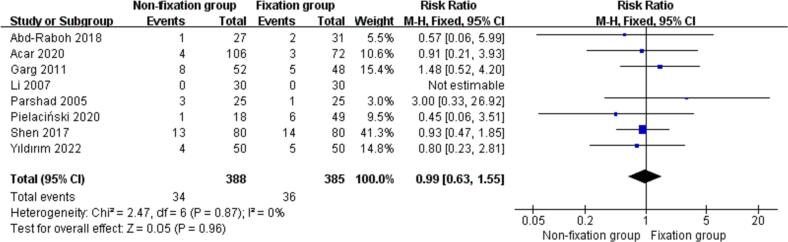
Eight studies [19,20,24,26,28,29,31,33] reported the incidence of haematoma in the nonfixation group compared with that in the fixation group for TEP inguinal hernia repair. The incidence of haematoma in the nonfixation group was 34/388 (8.7 %), and the incidence of haematoma in the fixation group was 36/385 (9.4 %). There was no statistical heterogeneity between the studies (P = 0.87, I2 = 0 %). Meta-analysis was performed using a fixed effect model combined with effect size. The results showed that there was no statistically significant difference in the incidence of haematoma between the nonfixation group and the fixation group [RR = 0.99, 95 % CI (0.63, 1.55), P = 0.96]. See Fig. 8 for details.
Fig. 8.
Comparison of incidence of haematoma between two groups.
Incidence of urinary retention
Three studies [21,24,25] reported the incidence of urinary retention in the nonfixation group compared with that in the fixation group for TEP inguinal hernia repair. The incidence of urinary retention in the nonfixation group was 6/122 (4.9 %), and the incidence of urinary retention in the fixation group was 24/118 (20.3 %). There was no statistical heterogeneity between the studies (P = 0.52, I2 = 0 %). Meta-analysis was conducted using the fixed effect model combined with the effect size. The results showed that the incidence of urinary retention in the nonfixation group was lower than that in the fixation group [RR = 0.25, 95 % CI (0.11, 0.57), P = 0.001]. The difference was statistically significant. See Fig. 9 for details.
Fig. 9.
Comparison of the incidence of urinary retention between the two groups.
Incidence of chronic pain
Five studies [20,[27], [28], [29],31] reported the incidence of chronic pain in the nonfixation group compared with that in the fixation group for TEP inguinal hernia repair. The incidence of chronic pain in the nonfixation group was 11/314 (3.5 %) and that in the fixation group was 33/311 (10.6 %). There was no statistical heterogeneity among the studies (P = 0.32, I2 = 13 %). Meta-analysis was performed using a fixed effect model combined with effect size. The results showed that there was no significant difference in the incidence of chronic pain between the nonfixation group and the fixation group [RR = 0.72, 95 % CI (0.43, 1.19), P = 0.20]. See Fig. 10 for details.
Fig. 10.
Comparison of the incidence of chronic pain between the two groups.
Recurrence rate
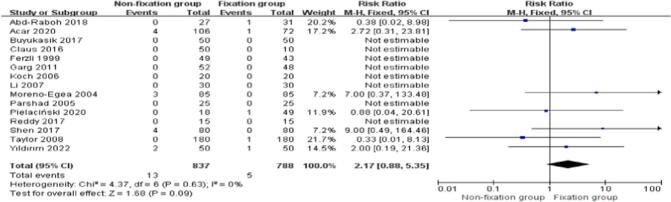
Fifteen studies [[19], [20], [21], [22], [23], [24], [25], [26], [27], [28], [29], [30], [31], [32], [33]] reported the recurrence rate in the nonfixation group compared with that in the fixation group for TEP inguinal hernia repair. The recurrence rate of the nonfixation group was 13/837 (1.5 %), and the recurrence rate of the fixation group was 5/788 (0.63 %). There was no statistical heterogeneity between the studies (P = 0.63, I2 = 0 %). Meta-analysis was performed using a fixed effect model combined with effect size. The results showed that there was no statistically significant difference in the recurrence rate between the nonfixation group and the fixation group [RR = 2.17, 95 % CI (0.88, 5.35), P = 0.09]. See Fig. 11 for details.
Fig. 11.
Comparison of recurrence rates between the two groups.
Publication bias
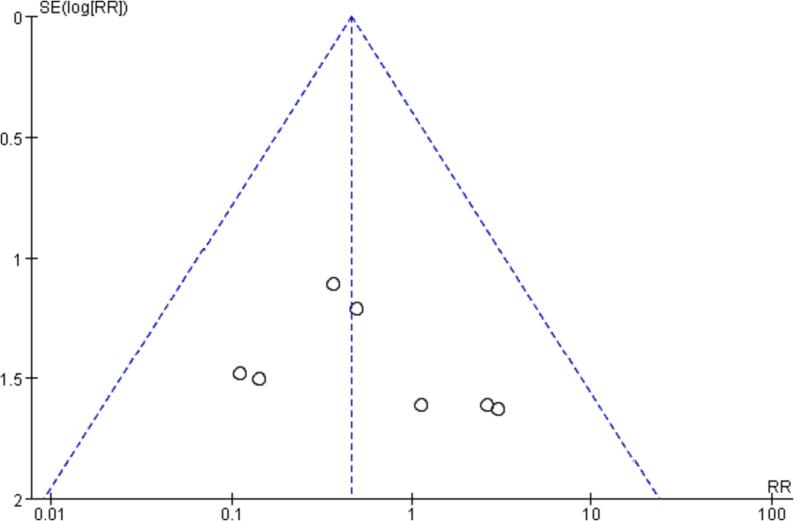
The publication bias was analyzed based on the recurrence rate. The inverted funnel plot was well symmetrical, with an Egger's test result of P = 0.392, suggesting that there was only a small possibility of publication bias in this study. The results are shown in Fig. 12.
Fig. 12.
Inverted funnel plot.
GRADE system evaluation results
The evidence for the postoperative 24-hour pain score is classified as very low. The evidence for operation time, time to resume normal activities, incidence of hematoma, incidence of chronic pain, and recurrence rate is classified as low. The evidence for hospital stay and the incidence of urinary retention is classified as moderate, as shown in Table 2.
Table 2.
GRADE assessment of outcome indicators.
| Outcome indicators | Risk of bias | Inconsistency | Indirectness | Imprecision | Publication bias | GRADE quality |
|---|---|---|---|---|---|---|
| Operation time | Serious | Not serious | Not serious | Serious | Undetected | ⊕⊕⃝⃝/Low |
| Postoperative 24-hour pain score | Serious | Serious | Not serious | Serious | Undetected | ⊕⃝⃝⃝/Very low |
| Hospital stay | Serious | Not serious | Not serious | Not serious | Undetected | ⊕⊕⊕⃝/Moderate |
| Time to resume normal activities after operation | Serious | Not serious | Not serious | Serious | Undetected | ⊕⊕⃝⃝/Low |
| Incidence of haematoma | Serious | Not serious | Not serious | Serious | Undetected | ⊕⊕⃝⃝/Low |
| Incidence of urinary retention | Serious | Not serious | Not serious | Not serious | Undetected | ⊕⊕⊕⃝/Moderate |
| Incidence of chronic pain | Serious | Not serious | Not serious | Serious | Undetected | ⊕⊕⃝⃝/Low |
| Recurrence rate | Serious | Not serious | Not serious | Serious | Undetected | ⊕⊕⃝⃝/Low |
GRADE: Grading of Recommendations Assessment, Development, and Evaluation.
Discussion
Scientific and technological innovation has brought about endless new methods, new approaches, and new thinking, enabling doctors to have more suitable choices and enabling patients to suffer the least possible trauma while obtaining the same or better curative effects. With the in-depth understanding of precise anatomy and membrane anatomy and the development of new mesh materials, laparoscopic inguinal hernia repair surgery has developed rapidly [34,35]. TEP inguinal hernia repair has the advantages of less pain and faster recovery, and the operation does not require entering the abdominal cavity, which reduces the impact of carbon dioxide pneumoperitoneum on the abdominal cavity and the occurrence of intestinal adhesions. In theory, it is an ideal method for inguinal hernia repair [[36], [37], [38]]. To reduce the possibility of hernia recurrence caused by the displacement of the mesh, the mesh is fixed during the operation, such as staple fixation or medical glue fixation; however, this may lead to postoperative pain, bleeding and other complications [39,40]. With the aim of improving the quality of life of patients after surgery, some studies began to not fix the mesh during inguinal hernia repair with TEP. However, due to the small sample size and low evidence strength of a single study, whether the effect of the unfixed mesh during TEP inguinal hernia repair is safe and whether it can lead to hernia recurrence remains controversial. Therefore, this study evaluated the efficacy and safety of the unfixed mesh in TEP inguinal hernia repair by means of meta-analysis.
In different studies, there are significant differences in operation time, which may be related to factors such as the skills of the surgeon and the method of mesh fixation. The operation procedure time of the nonfixation group was less than that of the fixation group; in other words, the operation time was shorter than that of the fixation group. The 1.33-minute time difference is statistically significant; however, it may not be clinically significant. The 24-hour postoperative pain score of the nonfixation group was lower than that of the fixation group. Postoperative pain was mainly caused by tissue damage caused by anatomy or by the use of penetrating mesh fixators to clamp nerves or muscles [[41], [42], [43]]. Some studies showed that age factors were related to postoperative acute pain, which might be related to the higher sensitivity of young people to pain [44]; this suggests that appropriate pain relief treatment could be given to young people after surgery and then improve the overall comfort of patients after surgery. However, this kind of pain did not affect the hospital stay or the time to return to normal activities and did not lead to an increase in the incidence of chronic pain. Due to the obvious heterogeneity of the pain score at 24 h after surgery and the poor stability of the subgroup, high-quality randomized controlled trials should be conducted in the future for further verification. In this meta-analysis, we are surprised to find that the incidence of urinary retention in the nonfixation group was lower than that in the fixation group. The high incidence of urinary retention in the fixation group was mainly due to two factors: one was that the sympathetic nerve excitation caused by pain stimulation increased the incidence of urinary retention; the other was that the increased pain in the early postoperative period led to the increased use of analgesia, which led to the occurrence of urinary retention [25,45,46]. Local haematoma formation is a relatively common complication after inguinal hernia surgery, usually due to poor haemostasis or vascular injury. This complication is particularly important in laparoscopic surgery because a large retroperitoneal haematoma may be formed. If patients show unstable haemodynamics, they need to undergo a second operation [47,48]. The incidence of haematoma in the nonfixation group was 8.7 %, and the incidence of haematoma in the fixation group was 9.4 %. There was no significant difference between the two groups. The success of inguinal hernia repair depends on the recurrence rate. The biggest controversy of unfixed mesh is whether it will cause postoperative recurrence [49]. In this meta-analysis, the recurrence rate of the nonfixation group was 1.5 %, while that of the fixation group was 0.63 %. There was no statistically significant difference between the two groups, indicating that the unfixed mesh in TEP inguinal hernia repair would not increase the hernia recurrence rate. However, some studies had a short follow-up time, so the follow-up time should be increased when evaluating the recurrence rate.
The strength of this study may be affected by the following factors: (1) The lack of a detailed description of randomization methods, allocation concealment and blinding methods in some studies, and the small sample size in some studies, was bound to cause certain selection, implementation and measurement bias, which affected the strength of evidence in this study to a certain extent; (2) Different surgical techniques, surgical procedures, mesh materials and fixation materials included in the study inevitably affected the results; and (3) The follow-up times of the various studies were inconsistent, and some studies had short follow-up times. Therefore, there were defects in evaluating the risk of medium- and long-term hernia recurrence. (4) The GRADE system evaluation results for some outcome indicators are rated as low or very low.
In sum, TEP with unfixed mesh shortens the operation time and reduces the 24-hour pain score and the incidence of urinary retention. The length of hospital stays, the time to resume normal activities after operation, the incidence of haematoma, the incidence of chronic pain, and the recurrence rates of procedures with unfixed mesh are similar to those utilizing mesh fixation. Furthermore, the use of unfixed mesh was safe and effective, but with a cautionary note that further follow-up is required. However, due to limitations, this conclusion still needs to be verified by a large sample, multi centre, strictly designed, high-quality clinical randomized controlled trial.
Research registration Unique Identifying number (UIN)
Name of the registry: INPLASY Registry.
Unique Identifying number or registration ID: INPLASY2022120044.
Hyperlink to your specific registration (must be publicly accessible and will be checked): https://inplasy.com/inplasy-2022-12-0044/.
Funding
No funding was received for this study.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
CRediT authorship contribution statement
Hui Dong and Li Li designed this study; Hui Dong ran the search strategy; Hui Dong and Hui-He Feng collected data; Deng-Chao Wang and Li Li rechecked the data; Deng-Chao Wang and Hui Dong performed the analysis; Hui-He Feng rechecked the data; Hui Dong and Li Li assessed the quality of the studies; Deng-Chao Wang and Hui-He Feng rechecked the data; Hui Dong wrote the manuscript; and Li Li edited the manuscript. All listed authors reviewed and revised the manuscript.
Declaration of competing interest
None.
Acknowledgements
Not applicable.
Data availability
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
References
- 1.Serra R., Bracale U.M., Conforto R., Roncone A., Nicola I., Michael A., et al. Association between inguinal hernia and arterial disease: a preliminary report. Biology. 2021;10:736. doi: 10.3390/biology10080736. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Muschalla F., Schwarz J., Bittner R. Effectivity of laparoscopic inguinal hernia repair (TAPP) in daily clinical practice: early and long-term result. Surg Endosc. 2016;30:4985–4994. doi: 10.1007/s00464-016-4843-8. [DOI] [PubMed] [Google Scholar]
- 3.Siddaiah-Subramanya M., Ashrafi D., Memon B., Memon M.A. Causes of recurrence in laparoscopic inguinal hernia repair. Hernia. 2018;22:975–986. doi: 10.1007/s10029-018-1817-x. [DOI] [PubMed] [Google Scholar]
- 4.Köckerling F., Simons M.P. Current concepts of inguinal hernia repair. Visc Med. 2018;34:145–150. doi: 10.1159/000487278. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Köckerling F., Stechemesser B., Hukauf M., Kuthe A., Schug-Pass C. TEP versus Lichtenstein: which technique is better for the repair of primary unilateral inguinal hernias in men? Surg Endosc. 2016;630:3304–3313. doi: 10.1007/s00464-015-4603-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Gutlic N., Gutlic A., Petersson U., Rogmark P., Montgomery A. Randomized clinical trial comparing total extraperitoneal with Lichtenstein inguinal hernia repair (TEPLICH trial) Br J Surg. 2019;106:845–855. doi: 10.1002/bjs.11230. [DOI] [PubMed] [Google Scholar]
- 7.Teng Y.J., Pan S.M., Liu Y.L., Yang K.H., Zhang Y.C., Tian J.H., et al. A meta-analysis of randomized controlled trials of fixation versus nonfixation of mesh in laparoscopic total extraperitoneal inguinal hernia repair. Surg Endosc. 2011;25:2849–2858. doi: 10.1007/s00464-011-1668-3. [DOI] [PubMed] [Google Scholar]
- 8.Gupta A., Ashish V.B., Bhandari V., Singh T., Subramaniyan V., Malhotra P. Comparing the clinical outcome of non fixation of mesh with mesh fixation in laparoscopic inguinal hernioplasty (TEP): a study and review of literature. Sch J Appl Med Sci. 2016;4:3442–3448. doi: 10.21276/sjams.2016.4.9.56. [DOI] [Google Scholar]
- 9.Kukleta J.F. Causes of recurrence in laparoscopic inguinal hernia repair[J] J Minim Access Surg. 2006;2(3):187. doi: 10.4103/0972-9941.27736. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Nahid A.K., Rahman S., Veerapatherar K., Fernandes R. Outcomes on mesh fixation vs non-fixation in laparoscopic totally extra peritoneal inguinal hernia repair: a comparative study. Turk J Surg. 2021;37:1–5. doi: 10.47717/turkjsurg.2021.4962. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Fortelny R.H. Is mesh fixation in TAPP and TEP still necessary? Mini-Invasive Surg. 2021;5:16. doi: 10.20517/2574-1225.2021.21. [DOI] [Google Scholar]
- 12.Moher D., Liberati A., Tetzlaff J., Altman D.G. PRISMA Group 2009 preferred reporting items for systematic reviews and meta-analyses: the Prisma statement. BMJ. 2009;339 doi: 10.7326/0003-4819-151-4-200908180-00135. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Shea B.J., Reeves B.C., Wells G., Micere Thuku, Hamel C., Moran J., et al. AMSTAR 2: a critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. BMJ. 2017;358 doi: 10.1136/bmj.j4008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Nienhuijs S., Staal E., Strobbe L., Rosman C., Groenewoud H., Bleichrodt R. Chronic pain after mesh repair of inguinal hernia: a systematic review. Am J Surg. 2007;194(3):394–400. doi: 10.1016/j.amjsurg.2007.02.012. [DOI] [PubMed] [Google Scholar]
- 15.Higgins J.P.T., Altman D.G., Gøtzsche P.C., Jüni P., Moher D., Oxman A.D., et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ. 2011;343 doi: 10.1136/bmj.d5928. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Higgins J.P.T., Thompson S.G., Deeks J.J., Altman D.G. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557–560. doi: 10.1136/bmj.327.7414.557. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Sedgwick P., Marston L. How to read a funnel plot in a meta-analysis. BMJ. 2015;351 doi: 10.1136/bmj.h4718. [DOI] [PubMed] [Google Scholar]
- 18.Zhang Y., Akl E.A., Schünemann H.J. Using systematic reviews in guideline development: the GRADE approach. Res Synth Methods. 2019;10(3):312–329. doi: 10.1002/jrsm. [DOI] [PubMed] [Google Scholar]
- 19.Abd-Raboh O.H., Hablus M.A., Elshora A.A., Saber S.A. Comparative study between mesh fixation vs. non-fixation in totally extraperitoneal hernioplasty for inguinal hernia. J Surg. 2018;6:23–28. doi: 10.11648/j.js.20180601.15. [DOI] [Google Scholar]
- 20.Acar A., Kabak I., Tolan H.K., Canbak T. Comparison between mesh fixation and non-fixation in patients undergoing total extraperitoneal inguinal hernia repair. Niger J Clin Pract. 2020;23:897–899. doi: 10.4103/njcp.njcp_398_19. [DOI] [PubMed] [Google Scholar]
- 21.Buyukasik K., Ari A., Akce B., Tatar C., Segmen O., Bektas H. Comparison of mesh fixation and non-fixation in laparoscopic totally extraperitoneal inguinal hernia repair. Hernia. 2017;21:543–548. doi: 10.1007/s10029-017-1590-2. [DOI] [PubMed] [Google Scholar]
- 22.Claus C.M.P., Rocha G.M., Campos A.C.L., Bonin E.A., Dimbarre D., Loureiro M.P., et al. Prospective, randomized and controlled study of mesh displacement after laparoscopic inguinal repair: fixation versus no fixation of mesh. Surg Endosc. 2016;30:1134–1140. doi: 10.1007/s00464-015-4314-7. [DOI] [PubMed] [Google Scholar]
- 23.Ferzli G.S., Frezza E.E., Pecoraro A.M., Jr., Ahern K.D. Prospective randomized study of stapled versus unstapled mesh in a laparoscopic preperitoneal inguinal hernia repair. J Am Coll Surg. 1999;188:461–465. doi: 10.1016/s1072-7515(99)00039-3. [DOI] [PubMed] [Google Scholar]
- 24.Garg P., Nair S., Shereef M., Thakur J.D., Nain N., Menon G.R., et al. Mesh fixation compared to nonfixation in total extraperitoneal inguinal hernia repair: a randomized controlled trial in a rural center in India. Surg Endosc. 2011;25:3300–3306. doi: 10.1007/s00464-011-1708-z. [DOI] [PubMed] [Google Scholar]
- 25.Koch C.A., Greenlee S.M., Larson D.R., Harrington J.R., Farley D.R. Randomized prospective study of totally extraperitoneal inguinal hernia repair: fixation versus no fixation of mesh. JSLS. 2006;10:457–460. [PMC free article] [PubMed] [Google Scholar]
- 26.Li J.W., Zheng M.H., Li H.Q., Zhang H., Hu W.G., Lu A.G. A randomized controlled clinical trial comparing stapling with non-stapling of mesh in laparoscopic total extraperitoneal inguinal hernioplasty. Chin J Gen Surg. 2007;22:440–442. [Google Scholar]
- 27.Moreno-Egea A., Martínez J.A.T., Cuenca G.M., Albasini J.L.A. Randomized clinical trial of fixation vs nonfixation of mesh in total extraperitoneal inguinal hernioplasty. Arch Surg. 2004;139:1376–1379. doi: 10.1001/archsurg.139.12.1376. [DOI] [PubMed] [Google Scholar]
- 28.Parshad R., Kumar R., Hazrah P., Bal S. A randomized comparison of the early outcome of stapled and unstapled techniques of laparoscopic total extraperitoneal inguinal hernia repair. JSLS. 2005;9:403–407. [PMC free article] [PubMed] [Google Scholar]
- 29.Pielaciński K., Puła B., Wróblewski T., Kuryłowicz M., Szczepanik A.B. Totally extraperitoneal inguinal hernia repair with or without fixation leads to similar results. Outcome of randomized prospective trial. Videosurg Other Miniinvasive Tech. 2020;15:1–10. doi: 10.5114/wiitm.2019.83611. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Girish T.U., BJ SC. A prospective comparative study of total extraperitoneal inguinal hernia repair: fixation versus without fixation of the mesh. Int J Surg. 2017;4:166–169. doi: 10.18203/2349-2902.isj20164380. [DOI] [Google Scholar]
- 31.Shen Y.M., Liu Y.T., Chen J., Sun L. Efficacy and safety of NBCA (n-butyl-2-cyanoacrylate) medical adhesive for patch fixation in totally extraperitoneal prosthesis (TEP): a prospective, randomized, controlled trial. Eur Rev Med Pharmacol Sci. 2017;21:680–686. [PubMed] [Google Scholar]
- 32.Taylor C., Layani L., Liew V., Ghusn M., Crampton N., White S. Laparoscopic inguinal hernia repair without mesh fixation, early results of a large randomised clinical trial. Surg Endosc. 2008;22:757–762. doi: 10.1007/s00464-007-9510-7. [DOI] [PubMed] [Google Scholar]
- 33.Yıldırım M.B., Sahiner I.T. The effect of mesh fixation on migration and postoperative pain in laparoscopic TEP repair: prospective randomized double-blinded controlled study. Hernia. 2022:1–8. doi: 10.1007/s10029-022-02587-w. [DOI] [PubMed] [Google Scholar]
- 34.Horne C.M., Prabhu A.S. Minimally invasive approaches to inguinal hernias. Surg Clin. 2018;98:637–649. doi: 10.1016/j.suc.2018.02.008. [DOI] [PubMed] [Google Scholar]
- 35.Pokala B., Armijo P.R., Flores L., Hennings D., Oleynikov D. Minimally invasive inguinal hernia repair is superior to open: a national database review. Hernia. 2019;23:593–599. doi: 10.1007/s10029-019-01934-8. [DOI] [PubMed] [Google Scholar]
- 36.Putnis S., Berney C.R. Totally extraperitoneal repair of inguinal hernia: techniques and pitfalls of a challenging procedure. Langenbeck’s Arch Surg. 2012;397:1343–1351. doi: 10.1007/s00423-012-0999-4. [DOI] [PubMed] [Google Scholar]
- 37.Bracale U., Melillo P., Pignata G., Salvo E.D., Rovani M., Merola G., et al. Which is the best laparoscopic approach for inguinal hernia repair: TEP or TAPP? A systematic review of the literature with a network meta-analysis. Surg Endosc. 2012;26:3355–3366. doi: 10.1007/s00464-012-2382-5. [DOI] [PubMed] [Google Scholar]
- 38.Shah M.Y., Raut P., Wilkinson T.R.V., Agrawal V. Surgical outcomes of laparoscopic total extraperitoneal (TEP) inguinal hernia repair compared with Lichtenstein tension-free open mesh inguinal hernia repair: a prospective randomized study. Medicine. 2022;101 doi: 10.1097/md.0000000000029746. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Golani S., Middleton P. Long-term follow-up of laparoscopic total extraperitoneal (TEP) repair in inguinal hernia without mesh fixation. Hernia. 2017;21:37–43. doi: 10.1007/s10029-016-1558-7. [DOI] [PubMed] [Google Scholar]
- 40.Tam K.W., Liang H.H., Chai C.Y. Outcomes of staple fixation of mesh versus nonfixation in laparoscopic total extraperitoneal inguinal repair: a meta-analysis of randomized controlled trials. World J Surg. 2010;34:3065–3074. doi: 10.1007/s00268-010-0760-5. [DOI] [PubMed] [Google Scholar]
- 41.Hedberg H.M., Hall T., Gitelis M., Lapin B., Butt Z., Linn J.G., et al. Quality of life after laparoscopic totally extraperitoneal repair of an asymptomatic inguinal hernia. Surg Endosc. 2018;32:813–819. doi: 10.1007/s00464-017-5748-x. [DOI] [PubMed] [Google Scholar]
- 42.Liew W., Wai Y.Y., Kosai N.R., Gendeh H.S. Tackers versus glue mesh fixation: an objective assessment of postoperative acute and chronic pain using inflammatory markers. Hernia. 2017;21:549–554. doi: 10.1007/s10029-017-1611-1. [DOI] [PubMed] [Google Scholar]
- 43.Shazi B., Koto M.Z. Comparing outcomes after laparoscopic totally extraperitoneal repair versus open (Lichtenstein) repair of inguinoscrotal hernia at dr George mukhari academic hospital. S Afr J Surg. 2017;55:77–79. [Google Scholar]
- 44.Lau H., Patil N.G. Acute pain after endoscopic totally extraperitoneal (TEP) inguinal hernioplasty: multivariate analysis of predictive factors. Surg Endosc. 2004;18:92–96. doi: 10.1007/s00464-003-9068-y. [DOI] [PubMed] [Google Scholar]
- 45.Patel J.A., Kaufman A.S., Howard R.S., Rodriguez C.J., Jessie E.M. Risk factors for urinary retention after laparoscopic inguinal hernia repairs. Surg Endosc. 2015;29:3140–3145. doi: 10.1007/s00464-014-4039-z. [DOI] [PubMed] [Google Scholar]
- 46.Mulroy M.F. Hernia surgery, anesthetic technique, and urinary retention--apples, oranges, and kumquats? Reg Anesth Pain Med. 2002;27:587–589. doi: 10.1053/rapm.2002.37326. [DOI] [PubMed] [Google Scholar]
- 47.Zeb M.H., Pandian T.K., El Khatib M.M., Naik N.D., Chandra A., Morris D.S., et al. Risk factors for postoperative hematoma after inguinal hernia repair: an update. J Surg Res. 2016;205:33–37. doi: 10.1016/j.jss.2016.06.002. [DOI] [PubMed] [Google Scholar]
- 48.Yang C., Deng S. Laparoscopic versus open mesh repair for the treatment of recurrent inguinal hernia: a systematic review and meta-analysis. Ann Palliat Med. 2020;9:1164–1173. doi: 10.21037/apm-20-968. [DOI] [PubMed] [Google Scholar]
- 49.Ersoz F., Culcu S., Duzkoylu Y., Bektas H., Sari S., Arikan S., et al. The comparison of Lichtenstein procedure with and without mesh-fixation for inguinal hernia repair. Surg Res Pract. 2016:8041515. doi: 10.1155/2016/8041515. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.