Abstract
Background
To describe the past, present and future burden of pancreatitis in older adults, and to explore cross-national inequalities across socio-demographic index (SDI).
Methods
Data on pancreatitis in older adults, including mortality and disability-adjusted life years (DALYs) rates, were collected from the Global Burden of Disease (GBD) 2019 study. Temporal trends were measured using joinpoint analyses and predicted using a Bayesian age-period-cohort model. Additionally, the unequal distribution of the burden of pancreatitis in older adults was quantified.
Results
From 1990 to 2019, the number of deaths and DALYs due to pancreatitis in older adults has been increasing annually. However, in most regions of the world, age-standardized death rates (ASDR) and age-standardized DALYs rates have been declining. The burden of pancreatitis in older adults was highest in low SDI region, primarily affecting the population aged 65–74, with a greater burden on males than females. Furthermore, from 1990 to 2019, absolute and relative cross-national inequalities in pancreatitis among older adults have remained largely unchanged. It is projected that in the next 11 years, the number of deaths in older adults due to pancreatitis will continue to increase, but the ASDR is expected to decline.
Conclusion
Over the past 30 years, the ASDR and age-standardized DALYs rate of pancreatitis in older adults have shown a decline globally, but the absolute burden continues to increase. Cross-national health inequalities persist. Therefore, it is necessary to develop targeted intervention measures and enhance awareness among this vulnerable population regarding the risk factors associated with pancreatitis.
Keywords: Older adult, Pancreatitis, Global burden of disease, Joinpoint analysis, Cross-national inequalities
1. Introduction
Pancreatitis, characterized by inflammation of the pancreas, is a significant global health concern with substantial morbidity and mortality rates. Acute pancreatitis is the most common gastrointestinal cause of hospital admission in the United States (Yadav and Lowenfels, 2013). Chronic pancreatitis, although less prevalent, significantly reduces patients' quality of life. Despite the proliferation of new treatments and preventive measures, pancreatitis continues to pose a serious public health problem, resulting in an enormous medical and social burden (Trikudanathan et al., 2019). The overall global incidence of acute pancreatitis was 34 cases [95 % confidence interval (CI) 23–49] per 100,000 of the general population per year, and chronic pancreatitis was 10 cases (95 % CI 8–12) per 100,000 per year (Xiao et al., 2016). The disease predominantly affects those who are middle-aged or older, with approximately one third of all patients with this condition aged ≥ 65 years (Pendharkar et al., 2017, Pendharkar et al., 2017, Gloor et al., 2002). In addition, it has been shown that older age is an important risk factor for progression and death in patients with pancreatitis (Yu et al., 2023, Liu et al., 2022).
Population aging is a global phenomenon, with the number and proportion of older adults (aged > 65 years) growing in almost every country in the world. According to the United Nations' World Population Prospects 2019, the number of older adults is projected to double to 1.5 billion by 2050, and the proportion is expected to increase from 9 % in 2019 to 16 % in 2025 (Nations U, 2019). Population ageing leads to the onset and development of many diseases, such as cardiovascular diseases, digestive diseases, neurological diseases and various types of cancer (Sadighi, 2018, Bottazzi et al., 2018). It is projected that by 2035, 14 million new cancer cases will be diagnosed in older adults, accounting for nearly 60 % of the global cancer incidence (Pilleron et al., 2019). Consequently, the health of the ageing population has become an important public health issue that affects the formulation and adjustment of national health policies.
The extent of global ageing varies geographically. Therefore, we hypothesize that the burden of pancreatitis in older adults varies geographically and is influenced by recognized risk factors for the disease. Specifically, we predict that regions with a higher proportion of older adults and a greater prevalence of risk factors such as alcohol consumption and obesity will exhibit a higher burden of pancreatitis in this population. Furthermore, we expect that the burden of pancreatitis among older adults will show significant inequalities across different countries, with implications for health policy and resource allocation. Previous studies have examined the global incidence and prevalence of pancreatitis (Jiang et al., 2023, Ouyang et al., 2020). However, there are limited research on the burden of deaths and DALYs due to pancreatitis in older adults. Therefore, we conducted an assessment of the burden of pancreatitis in older adults globally, regionally, and across 204 countries using the Global Burden of Disease (GBD) 2019 dataset, including an examination of their age and sex distribution. Additionally, we estimated the proportion of deaths attributed to recognized risk factors for pancreatitis in older adults. Furthermore, we conducted cross-national inequality analyses using the standard health equity analysis methodology recommended by the World Health Organization to determine the magnitude and trends of inequality in the burden of pancreatitis among older adults across countries in relation to their level of social development. Finally, we projected the global burden of death from pancreatitis in older adults by 2030. These findings can provide valuable insights for informing health policies and facilitating the efficient allocation of healthcare resources for the management and prevention of pancreatitis.
2. Methods
2.1. Data sources
In this study, we extracted estimates of deaths and disability-adjusted life years (DALYs) and their 95 % uncertainty intervals (UIs) for pancreatitis in older adults aged ≥ 65 years from GBD 2019 (https://ghdx.healthdata.org/gbd-2019). Using the latest epidemiological data and improved standardized methodologies, the database provides comprehensive estimates of the burden of 369 diseases and injuries, as well as the 87 risk factors attributable to them, considering factors such as sex, age, region, and country (GBD 2019 Diseases and Injuries Collaborators, 2020, GBD 2019 Risk Factors Collaborators, 2020). The 204 countries and territories worldwide can be divided into 21 regions, such as the Western Pacific, Central Asia, and Eastern Europe. Additionally, these countries and territories are further divided into five regions based on the Socio-demographic Index (SDI), which include low, low-middle, middle, high-middle, and high categories. The cases of pancreatitis included in this study were diagnosed according to the classification criteria of the International Classification of Diseases-10 (ICD-10)/ICD-9 (GBD 2019 Diseases and Injuries Collaborators, 2020) (Table S1). Our study conducting analysis on publicly available deidentified data did not involve research on human subjects and animals, and thus, it was exempt from the requirement for ethical approval.
2.2. SDI
The SDI, developed by GBD researchers, is a composite indicator of developmental status that is closely related to health outcomes (IHME, 2019). It is calculated as the geometric mean of indices ranging from 0 to 1, including total fertility rate under the age of 25, mean education for individuals aged 15 and older, and lag-distributed income per capita. As a composite measure, areas with an SDI of 0 represent the lowest theoretical level of health-related development, while areas with an SDI of 1 represent the highest theoretical level of health-related development.
2.3. Joinpoint analysis
To characterize the burden of pancreatitis in older adults at a global, regional, and national level, we conducted descriptive analyses. We compared the burden of deaths and DALYs between the sexes and each age group. Additionally, the annual percentage change (APC) and average annual percentage change (AAPC) were estimated using Joinpoint analysis to quantify the temporal trend in ASDR/age-standardized DALYs rate for pancreatitis in older adults from 1990 to 2019. APC is used to evaluate the internal trend of each independent interval of a segmented function, or the global trend where the number of connection points is 0. The AAPC refers to the average APC considering the full period. Disparities in disease burden across populations and regions were found by comparing the timing of the emergence of different joinpoints, the AAPC, and the APCs across segments. If both the AAPC value and its 95 % confidence interval (CI) were greater than 0, the trend was defined as increasing. Conversely, if both the AAPC value and its 95 % CI were less than 0, the trend was defined as decreasing. Otherwise, the trend was considered relatively stable (Zhang et al., 2024, Liu et al., 2023).
2.4. Cross-country social inequalities analysis
The unequal distribution of the burden of pancreatitis among older adults across countries is assessed using the slope index of inequality and the health inequality concentration index. These indicators are standard measures of absolute and relative gradient inequality, respectively (Howe, 2014). The slope index of inequality was calculated by regressing national DALYs rates due to pancreatitis in the older adult population on an SDI-associated relative position scale. This scale was defined by the midpoint of the cumulative range of the population ranked by SDI. Heteroskedasticity was considered by employing a weighted regression model. The health inequality concentration index was calculated by numerically integrating the area under the Lorenz concentration curve, which was fitted using the cumulative fraction of DALYs and the cumulative relative distribution of the population ranked by SDI (Mujica and Moreno, 2019). It has been suggested that an absolute value of 0.2–0.3 represents a reasonably high level of relative inequality (World HO, 2013).
2.5. Bayesian Age-Period-Cohort analysis
The Bayesian age-period-cohort (BAPC) models have the highest coverage and higher accuracy in predicting future disease burden (Yu et al., 2021, Riebler and Held, 2017, Du et al., 2020). The model is based on an age-period-cohort model that assumes an association between morbidity or mortality and age structure and population size. The BAPC, Nordpred, and integrated nested Laplacian approximation (INLA) packages were applied to conduct the forecast, to adjust for over-dispersion, assuming the inverse gamma prior distribution of age, period, and cohort effects (modeled by a second-order random walk [RW2]) (Knoll et al., 2020). Predicted values of pancreatitis deaths and ASDR were estimated by multiplying the prediction rates by the corresponding sex, age, calendar year, and country-specific population prediction. The predicted values in each stratum are then aggregated for presentation of global.
2.6. Statistics
Joinpoint regression analyses were performed using the Joinpoint regression program v5.0.2 provided by the National Cancer Institute Surveillance Research Program. All analyses and visualizations in this study were performed on R software (v.4.3.1).
3. Results
3.1. Temporal trends in the burden of pancreatitis in older adults
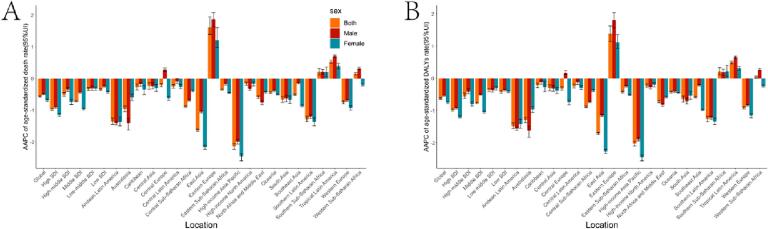
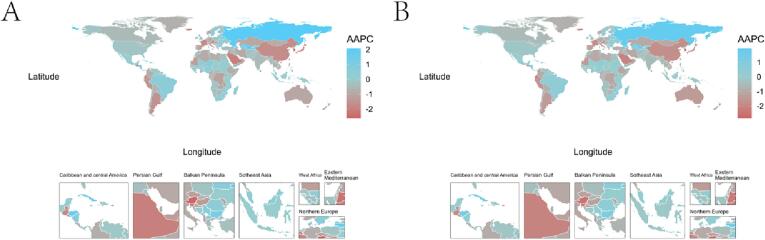
In 2019, there were 52,605.0 (95 % UI, 45,201.3 to 59,766.4) deaths from pancreatitis in older adults, accounting for 45.7 % of all pancreatitis deaths (Table 1). From 1990 to 2019, the ASDR declines annually, with an AAPC of 0.56 (95 % CI, −0.58 to −0.54). In 2019, the global number of DALYs due to pancreatitis in older adults was 856936.3 (95 % UI, 747857.3–963889.0). At the same time, age-standardized DALYs rate declined, with an AAPC of −0.62 (95 % CI, −0.64 to −0.60). In the five SDI regions, ASDR and age-standardized DALY rates for pancreatitis were highest in the low SDI region. Fortunately, the burden of pancreatitis among older adults in all SDI regions showed a significant downward trend (Fig. 1A, B). Regionally, the top three regions with the highest burden of ASDR and age-standardized DALYs rate were Andean Latin America, Eastern Europe, and Central Europe. The largest increases in ASDR and age-standardized DALYs rate for pancreatitis in older adults were in Eastern Europe and Tropical Latin America, whereas the largest decreases were in the High-income Asia Pacific and East Asia. At the same time, the countries with the greatest increase in the burden of pancreatitis in older adults were the Russian Federation and Uzbekistan (Fig. 2A,B). The ASDR and age-standardized DALYs rates for elderly pancreatitis in Bolivia (Plurinational State of), Mongolia, and Honduras were among the top three in the world (Table S2).
Table 1.
The number, age-standardized rate and temporal trend of pancreatitis in older adults from 1990 to 2019.
| Location | Death |
DALYs |
||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| 1990 |
2019 |
1990–2019 |
1990 |
2019 |
1990–2019 |
|||||
| Cases | ASDR | Cases | ASDR | AAPC (95 % CI) | Count | Age-standardized DALYs rate | Count | Age-standardized DALYs rate | AAPC (95 % CI) | |
| Global | 26791.3 | 8.24 | 52605.0 | 7.28 | −0.56*(−0.58 to −0.54) | 463113.5 | 142.48 | 856936.3 | 118.65 | −0.62*(−0.64 to −0.60) |
| Sex | ||||||||||
| Female | 14409.5 | 7.77 | 26672.2 | 6.75 | −0.68*(−0.71 to −0.64) | 238852.3 | 128.73 | 410902.0 | 103.97 | −0.75*(−0.78 to −0.72) |
| Male | 12381.7 | 8.88 | 25932.8 | 7.93 | −0.49*(−0.50 to −0.47) | 224261.1 | 160.77 | 446034.3 | 136.39 | −0.53*(−0.55 to −0.51) |
| Regions | ||||||||||
| Andean Latin America | 364.1 | 22.74 | 737.6 | 15.46 | −1.35*(−1.44 to −1.25) | 6067.9 | 378.93 | 11637.4 | 243.93 | −1.48*(−1.56 to −1.38) |
| Australasia | 144.5 | 6.48 | 264.3 | 5.54 | −0.96*(−1.05 to −0.86) | 2400.8 | 107.60 | 3707.4 | 77.78 | −1.29*(−1.37 to −1.21) |
| Caribbean | 156.2 | 6.88 | 307.3 | 6.68 | −0.27*(−0.36 to −0.18) | 2580.7 | 113.59 | 4943.0 | 107.51 | −0.22*(−0.28 to −0.15) |
| Central Asia | 385.5 | 11.12 | 473.4 | 9.43 | −0.23*(−0.33 to −0.13) | 6496.8 | 187.34 | 8372.0 | 166.69 | −0.30*(−0.39 to −0.20) |
| Central Europe | 1775.9 | 13.67 | 2861.9 | 13.47 | −0.20*(−0.25 to −0.15) | 31070.0 | 239.18 | 46268.0 | 217.77 | −0.31*(−0.36 to −0.26) |
| Central Latin America | 627.6 | 9.72 | 1903.6 | 9.58 | −0.24*(−0.30 to −0.19) | 10697.4 | 165.76 | 30891.3 | 155.53 | −0.24*(−0.29 to −0.18) |
| Central Sub-Saharan Africa | 118.6 | 7.63 | 212.8 | 6.22 | −0.88*(−0.90 to −0.86) | 2242.5 | 144.22 | 3829.3 | 111.87 | −0.88*(−0.90 to −0.86) |
| East Asia | 3709.0 | 5.45 | 6616.5 | 3.58 | −1.63*(−1.66 to −1.59) | 67270.1 | 98.91 | 112094.2 | 60.72 | −1.71*(−1.74 to −1.67) |
| Eastern Europe | 2176.4 | 9.31 | 4776.8 | 14.83 | 1.61*(1.40 to 1.95) | 40762.4 | 174.33 | 84822.4 | 263.32 | 1.39*(1.14 to 1.63) |
| Eastern Sub-Saharan Africa | 454.9 | 8.39 | 870.1 | 7.63 | −0.35*(−0.37 to −0.33) | 8324.7 | 153.44 | 15215.3 | 133.51 | −0.42*(−0.45 to −0.39) |
| High-income Asia Pacific | 954.3 | 5.49 | 1774.6 | 3.96 | −2.13*(−2.23 to −2.05) | 15256.5 | 87.76 | 24281.6 | 54.16 | −2.02*(−2.09 to −1.96) |
| High-income North America | 2006.4 | 5.81 | 3457.4 | 5.75 | −0.15*(−0.21 to −0.11) | 34717.3 | 100.61 | 57126.8 | 95.08 | −0.23*(−0.28 to −0.17) |
| North Africa and Middle East | 946.7 | 7.46 | 2089.8 | 6.53 | −0.59*(−0.63 to −0.54) | 15605.7 | 123.00 | 32079.3 | 100.22 | −0.72*(−0.76 to −0.67) |
| Oceania | 9.4 | 4.66 | 19.1 | 4.25 | −0.44*(−0.47 to −0.42) | 176.2 | 87.70 | 350.1 | 77.71 | −0.42*(−0.45 to −0.40) |
| South Asia | 3866.7 | 10.03 | 9927.6 | 8.74 | −0.66*(−0.75 to −0.56) | 71358.0 | 185.05 | 175486.2 | 154.55 | −0.64*(−0.74 to −0.54) |
| Southeast Asia | 1605.5 | 8.67 | 3483.6 | 7.56 | −0.51*(−0.53 to −0.49) | 27717.4 | 149.73 | 57654.9 | 125.19 | −0.58*(−0.60 to −0.56) |
| Southern Latin America | 650.0 | 15.87 | 863.4 | 11.19 | −1.28*(−1.36 to −1.19) | 11238.7 | 274.48 | 14271.9 | 184.92 | −1.26*(−1.34 to −1.18) |
| Southern Sub-Saharan Africa | 88.6 | 4.08 | 185.6 | 4.26 | 0.21*(0.11 to 0.32) | 1528.0 | 70.41 | 3205.5 | 73.50 | 0.22*(0.11 to 0.33) |
| Tropical Latin America | 666.3 | 9.40 | 2434.8 | 11.74 | 0.54*(0.48 to 0.59) | 11924.5 | 168.22 | 39615.4 | 191.03 | 0.49*(0.44 to 0.53) |
| Western Europe | 5250.8 | 9.41 | 7646.4 | 8.74 | −0.75*(−0.80 to −0.71) | 81338.6 | 145.80 | 103236.0 | 117.94 | −0.91*(−0.95 to −0.87) |
| Western Sub-Saharan Africa | 833.8 | 12.53 | 1698.3 | 13.04 | 0.15*(0.12 to 0.19) | 14339.2 | 215.43 | 27848.3 | 213.80 | 0.03*(0.00 to 0.07) |
| SDI | ||||||||||
| High SDI | 7137.4 | 7.23 | 11032.6 | 6.04 | −0.97*(−1.01 to −0.94) | 115653.7 | 117.12 | 164826.7 | 90.30 | −0.98*(−1.01 to −0.95) |
| High-middle SDI | 8468.1 | 9.48 | 16029.5 | 8.65 | −0.50*(−0.56 to −0.43) | 147360.3 | 165.04 | 257253.4 | 138.78 | −0.55*(−0.62 to −0.45) |
| Middle SDI | 5338.3 | 6.94 | 12116.3 | 5.89 | −0.71*(−0.73 to −0.69) | 93951.9 | 122.23 | 201609.0 | 97.99 | −0.76*(−0.78 to −0.74) |
| Low-middle SDI | 4162.7 | 9.66 | 9945.4 | 9.01 | −0.34*(−0.38 to −0.29) | 75597.8 | 175.47 | 172934.4 | 156.65 | −0.36*(−0.41 to −0.31) |
| Low SDI | 1671.6 | 9.90 | 3455.8 | 9.13 | −0.35*(−0.38 to −0.32) | 30331.4 | 179.72 | 59916.5 | 158.34 | −0.42*(−0.46 to −0.37) |
ASDR: Age-standardized death rate; DALYs: Disability-adjusted life years; AAPC: Average annual percentage change; SDI: Socio-demographic index.
Fig. 1.
The AAPC of ASR burden for pancreatitis in older adults from 1990 to 2019 in global, SDI regions, and 21 GBD regions by sex. A AAPC of ASDR in pancreatitis; B AAPC of age-standardized DALY rate in pancreatitis. AAPC average annual percentage change, ASR age-standardized rate; GBD Global Burden of Diseases, Injuries, and Risk Factors Study; SDI socio-demographic index; ASDR age-standardized death rate.
Fig. 2.
The global disease burden of pancreatitis in older adults consumption for both genders in 204 countries and territories from 1990 to 2019. A AAPC of ASDR for pancreatitis; B AAPC of age-standardized DALY rate for pancreatitis. AAPC average annual percentage change; DALYs disability-adjusted life-years; ASDR age-standardized death rate.
3.2. Age composition of pancreatitis burden in older adults
Globally, pancreatitis deaths and DALYs in older adults increased over time in all age groups, with the 65–74 age group being slightly higher than the 75–84 age group (Fig. S1A, B). Both ASDR and age-standardized DALYs rates for pancreatitis in older adults were highest in the 85 + age group. ASDR remained essentially flat in all three age groups from 1990 to 2019, but age-standardized DALYs rates declined. In 2019, the 65–74 age group had the highest number of deaths and DALYs among the elderly in most regions (Fig. S2A, B). The age composition of burden growth in Eastern Europe was quite different from the other regions, with the 85 + age group playing a key role (Fig. S3A,B).
3.3. Sex disparity of the burden of pancreatitis in older adults
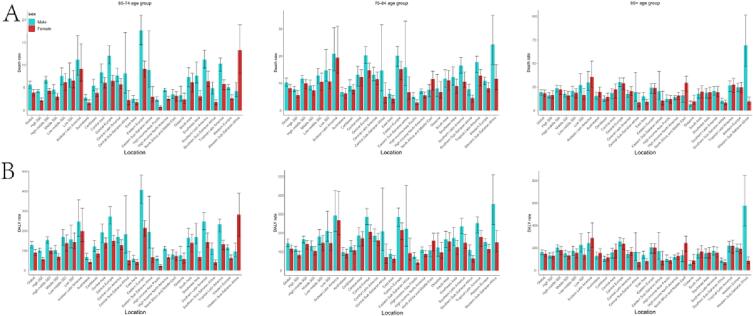
There were differences between males and females in the burden of pancreatitis in older adults (Fig. 3). Globally, elderly females accounted for 50.70 % (26672.2 cases) of pancreatitis deaths in 2019, compared with 49.30 % (25932.8 cases) in males (Table 1). DALYs for pancreatitis in elderly females accounted for 47.95 % compared to 52.05 % in males. However, in terms of ASDR and DALYs rates, the burden is greater for elderly males than for females globally in all age groups (Fig. 3A,B). With the exception of North Africa and the Middle East, Oceania, and Western Sub-Saharan Africa, death and DALYs rates for pancreatitis are higher in older males than in females in all other regions of the world (Table S3, S4).
Fig. 3.
The death and DALY rate of pancreatitis in older adults in global, SDI regions, and 21 GBD regions in 2019 by age group and sex. A The death rate of pancreatitis in older adults; B The DALY rate of pancreatitis in older adults. The first column represents the 65–74 age group; the second column represents the 75–84 age group; the third column represents the 85 + age group. SDI socio-demographic index; GBD Global Burden of Diseases, Injuries, and Risk Factors Study; DALYs disability-adjusted life-years.
3.4. Attributable risk factors for death from pancreatitis in older adults
In 2019, the estimated number of alcohol-related pancreatitis deaths among older adults globally is 12,241.9, accounting for 23.3 % of all pancreatitis deaths (Table S5). The proportion for males was 35.6 %, compared with 11.3 % for females. The burden of alcohol-related pancreatitis deaths in older adults was generally greater in males than in females in all regions (Figure S4). By further looking at different regions, we found that the burden of disease caused by alcohol use was heaviest in Western Europe, Southern Latin America, Central Europe and Australasia. And more than 50 % of pancreatitis deaths among males in these regions were alcohol-related.
3.5. Cross-national inequalities in the burden of pancreatitis in older adults
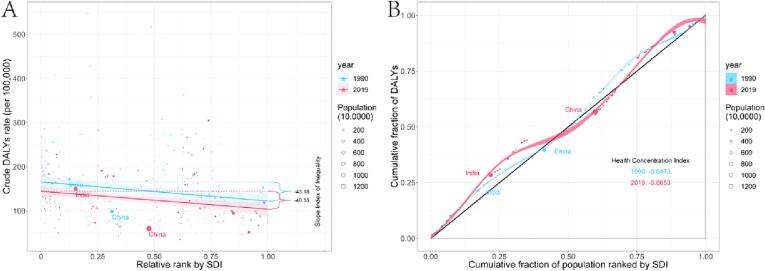
Across the 204 countries analysed, significant absolute and relative SDI-related inequalities in pancreatitis in older adults were observed, with a disproportionately high burden borne by countries with low SDI (Fig. 4A,B). As shown by the slope index of inequality, the the gap in DALYs rate between countries with the highest and lowest SDI were −43.18 (95 % CI: −74.31 to −12.05) and −40.55 (95 % CI: −62.61 to −18.50) DALYs per 100,000 population in 1990 and 2019, respectively, showing a negative association between the DALY rate and SDI. This decline suggests that inequalities in the burden of pancreatitis in older adults between high and low SDI countries have narrowed over the past three decades. By contrast, relative inequality analysis showed that the health concentration index remained nearly constant between 1990 (−0.0473, 95 % CI − 0.0793 to − 0.0154) and 2019 (−0.0653, 95 %CI − 0.1066 to − 0.0240) (Table S6).
Fig. 4.
Health inequality regression curves and concentration curves for the DALYs of pancreatitis in older adults worldwide, 1990 and 2019. A Slopes index of pancreatitis in older adults globally, 1990 and 2019; B Health concentration index of pancreatitis in older adults globally, 1990 and 2019. The slope index of inequality, shown as the slope of the regression line, represents the absolute difference in pancreatitis in older adults burden between countries or territories with the highest and lowest SDI. Concentration curves (Lorenz curves) graphed by plotting the cumulative fraction of population ranked by SDI (x-axis) against the cumulative fraction of pancreatitis in older adults burden ranked by age-standardised DALY (y-axis). The concentration index, calculated as twice the area between the 45° diagonal line and the Lorenz curve, representing the relative extent to which the pancreatitis in older adults burden is concentrated among the poor (negative value) or the rich (positive value). Dots representing countries or territories, with different sizes representing the population sizes. DALYs disability-adjusted life-years; SDI socio-demographic index.
3.6. The prediction of pancreatitis burden in older adults
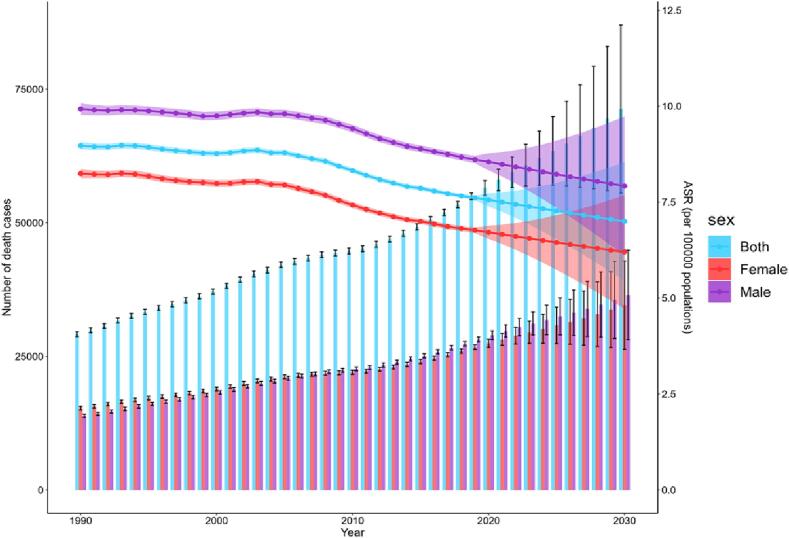
From 2020 to 2030, global deaths from pancreatitis in older adults will continue to increase, with males slightly outnumbering females (Fig. 5). The number of female deaths was projected to increase from 0.027 million in 2019 to 0.035 million in 2030, and the number of male deaths was projected to increase from 0.028 million to 0.036 million (Table S7). Although deaths from pancreatitis in older adults were projected to continue to increase, the global ASDR was expected to decline each year (Table S8).
Fig. 5.
The observation and prediction of the number of deaths and mortality from pancreatitis in older adults from 1990 to 2030. Each lines represent death/ DALY rates for age group, and each bars represent the number of deaths/DALYs. DALYs disability-adjusted life-years.
4. Discussion
In this study, we conducted secondary analyses of the 2019 GBD data to provide an up-to-date overview of the global epidemiology of pancreatitis in older adults, along with projections for the next 11 years. Additionally, we identified the major risk factor for pancreatitis, which is the proportion of alcohol consumption contributing to pancreatitis-related deaths in different regions. Furthermore, by calculating the slope index and concentration index of health inequality, we revealed the phenomenon and changes in health inequality associated with pancreatitis among older adults globally over the past 30 years.
As the population continues to grow and age, it is inevitable that the number of pancreatitis-related deaths and DALYs in older adults increases. However, there is positive news as the ASDR and age-standardized DALY rates for pancreatitis have shown a decline. This downward trend is projected to persist until 2030. A study has highlighted that alcohol consumption plays a significant role in contributing to pancreatitis. The proportion of patients with acute pancreatitis attributed to alcohol use ranges from 19 % to 32 %, while the proportion of patients with chronic pancreatitis ranges from 55 % to 70 % (Yadav and Whitcomb, 2010). In our study, 23.3 % of pancreatitis deaths in the elderly worldwide were attributable to alcohol consumption. In developing countries, about 35 % of acute pancreatitis cases are associated with alcohol abuse (Wang et al., 2009). Most alcoholic pancreatitis presents as acute pancreatitis, but alcoholic acute pancreatitis is more likely to progress to chronic pancreatitis, which is an important factor in its prevalence (Petrov and Yadav, 2019). In addition, one study confirmed a dose–response relationship between alcohol consumption and risk of pancreatitis (Irving et al., 2009). It is encouraging to note that the introduction of multidisciplinary and individualized treatment has greatly improved the prognosis of acute pancreatitis in the past decade (Boxhoorn et al., 2020). In addition, advances in early diagnostic methods, the use of minimally invasive endoscopy, advances in the treatment of pancreatic and peripancreatic necrosis, and improvements in the management of critically ill patients have contributed to a reduction in pancreatitis mortality rates (Baron et al., 2020, Bang et al., 2019, Nathens et al., 2004).
Additionally, the regional heterogeneity of pancreatitis burden in older adults is equally noteworthy. Among the 21 GBD regions, the largest increases in ASDR and age-standardized DALYs rate were in Eastern Europe and Tropical Latin America. These conditions are largely attributed to the distribution of alcohol consumption in these regions (GBD 2016 Alcohol Collaborators, 2018). Globally, Eastern Europe has been repeatedly identified as the region with the highest alcohol-related health risks (Jasilionis et al., 2020). Although the alcohol-related burden in Eastern Europe has declined following the implementation of a series of alcohol-related policies, the prevalence of harmful alcohol consumption in Eastern Europe is still on the rise in recent studies (NCD Countdown 2030 Collaborators, 2018, GBD 2020 Alcohol Collaborators, 2022). This means that Eastern Europe still has a long way to go in controlling alcohol.
In our research, the burden of pancreatitis was higher in males than in females in 1990 and 2019. Gender differences in the epidemiology of pancreatitis may be related to etiology. Pancreatitis in females was more closely associated with gallstones, autoimmune diseases or idiopathic pancreatitis, whereas alcohol-related pancreatitis was more common in males (Yadav and Lowenfels, 2013, Kleeff et al., 2017). Our study also confirms that deaths from pancreatitis in older males attributed to alcohol are much greater than in females. On the one hand, many females are lifelong abstainers from alcohol and are less likely to develop alcohol-related diseases compared to males (Erol and Karpyak, 2015). On the other hand, the global prevalence of smoking among males is 36.7 %, much higher than the 7.8 % among females (World HO, 2021). However, the relationship between gender differences and pancreatitis at the molecular and genetic levels needs to be further investigated. In addition, advanced age is associated with an increased risk of death in patients with pancreatitis (Moran et al., 2018). Overall, the older adults have one of the highest burdens of pancreatitis, especially in the age group ≥ 85 years. Considering that the world is facing an unavoidable aging population, the prevention and treatment of pancreatitis in older adults should receive more attention. Therefore, it is important to increase awareness and education about pancreatitis and its risk factors, especially in the older adults.
In terms of health inequalities inequalities between countries, we calculated the slope index and the health concentration index, which depend on the cross-country health gradient and SDI rankings. Typically, the prevalence of alcohol use, a major risk factor for pancreatitis, is highest in high SDI regions (GBD 2016 Alcohol Collaborators, 2018). However, we found that the burden of pancreatitis in older adults is negatively associated with national SDI levels, and this inequality has decreased slightly over the last 30 years for the absolute measure (slope index) and remained low for the relative measure (health concentration index). One possible explanation for this is that high SDI regions produce a lower burden of disease per litre of alcohol consumed compared to low SDI regions (Shield and Rehm, 2021). In addition, in low SDI countries, environmental and other risk factors such as smoking also increase the harm caused by alcohol (Stringhini et al., 2017). In general, the prevalence of alcohol consumption has increased as socioeconomic levels have risen (GBD 2016 Alcohol Collaborators, 2018). Therefore, as a potential variable risk factor, health education and public health strategies to control alcohol may help to reduce the disease burden of pancreatitis in older adults.
There are some limitations to this study: (1) In some regions and countries, especially low-income areas, there is a lack of high-quality and detailed data. Only a few countries or territories provide actual national data from around the world, so burden estimates heavily rely on modeling data rather than typical data from individual population studies. Therefore, national-level burdens should be interpreted with caution. If possible, it is encouraged to conduct more health surveys at the national level to obtain more detailed and representative data from each country. (2) Data limitations prevented us from further exploring specific types of pancreatitis, such as acute and chronic pancreatitis; moreover, acute and chronic pancreatitis are two distinct diseases with some overlap in a small proportion of patients. To better understand the true burden of pancreatitis, it is suggested to categorize pancreatitis types in the future, especially based on histology. (3) Similarly, risk factors such as gallstones and hypertriglyceridemia also play an important role in the pathogenesis of pancreatitis (Yang and McNabb-Baltar, 2020). However, the GBD2019 did not support our analysis of the burden of disease due to these meaningful risk factors. In addition, future research should focus on assessing common risk factors and lifestyles that influence the incidence, mortality, and DALYs of pancreatitis, especially in countries and regions with large populations or high alcohol consumption levels.
5. Conclusion
Overall, the burden of pancreatitis in older adults is higher in less developed regions, while developed regions exhibit a decreasing trend in the burden of pancreatitis among older adults. Globally, there has been a gradual increase in the number of deaths and DALYs attributed to pancreatitis in older adults. However, there has been a corresponding decline in ASDR and age-standardized DALY rates. This trend is expected to persist until 2030. Alcohol consumption is a contributing factor to the high global burden of pancreatitis in older adults. Therefore, based on our findings, it is crucial to strengthen and improve measures targeting alcohol consumption through effective national policies that consider different genders, age groups, and regions. Additionally, there is a need to develop pancreatitis surveillance and treatment programs in less developed regions to alleviate the burden of alcohol-induced pancreatitis.
6. Funding
This study was supported by the project of the Institute of Hospital Management, National Health Care Commission (YLZLXZ22G026), the Self-funded Science and Technology Program of Fuyang City (FK202081016), and Anhui Province Clinical Medical Research Translation Special Programme (202204295107020054).
CRediT authorship contribution statement
Jiangtao Yu: Writing – original draft, Validation. Chunlong Liu: Investigation, Data curation. Jian Zhang: Visualization, Software. Xiangyu Wang: Visualization, Resources. Kun Song: Validation, Project administration. Panpan Wu: Validation, Data curation. Fubao Liu: Software, Resources.
Declaration of competing interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Acknowledgments
We acknowledge GBD2019 collaborators whose outstanding contributions have enabled us to complete this study.
Footnotes
Supplementary data to this article can be found online at https://doi.org/10.1016/j.pmedr.2024.102722.
Appendix A. Supplementary data
The following are the Supplementary data to this article:
Data availability
I explain the source of my data in the text.
References
- Bang J.Y., Arnoletti J.P., Holt B.A., Sutton B., Hasan M.K., Navaneethan U., Feranec N., Wilcox C.M., Tharian B., Hawes R.H., et al. An Endoscopic Transluminal Approach, Compared With Minimally Invasive Surgery, Reduces Complications and Costs for Patients With Necrotizing Pancreatitis. Gastroenterology. 2019;156(4):1027–1040. doi: 10.1053/j.gastro.2018.11.031. [DOI] [PubMed] [Google Scholar]
- Baron T.H., DiMaio C.J., Wang A.Y., Morgan K.A. American Gastroenterological Association Clinical Practice Update: Management of Pancreatic Necrosis. Gastroenterology. 2020;158(1):67–75. doi: 10.1053/j.gastro.2019.07.064. [DOI] [PubMed] [Google Scholar]
- Bottazzi B., Riboli E., Mantovani A. Aging, inflammation and cancer. Semin Immunol. 2018;40:74–82. doi: 10.1016/j.smim.2018.10.011. [DOI] [PubMed] [Google Scholar]
- Boxhoorn L., Voermans R.P., Bouwense S.A., Bruno M.J., Verdonk R.C., Boermeester M.A., van Santvoort H.C., Besselink M.G. Acute pancreatitis. Lancet. 2020;396(10252):726–734. doi: 10.1016/S0140-6736(20)31310-6. [DOI] [PubMed] [Google Scholar]
- Du Z., Chen W., Xia Q., Shi O., Chen Q. Trends and projections of kidney cancer incidence at the global and national levels, 1990–2030: a Bayesian age-period-cohort modeling study. Biomark Res. 2020;8:16. doi: 10.1186/s40364-020-00195-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Erol A., Karpyak V.M. Sex and gender-related differences in alcohol use and its consequences: Contemporary knowledge and future research considerations. Drug Alcohol Depen. 2015;156:1–13. doi: 10.1016/j.drugalcdep.2015.08.023. [DOI] [PubMed] [Google Scholar]
- GBD 2016 Alcohol Collaborators Alcohol use and burden for 195 countries and territories, 1990-2016: a systematic analysis for the Global Burden of Disease Study 2016. LANCET. 2018;392(10152):1015–1035. doi: 10.1016/S0140-6736(18)31310-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- GBD 2019 Diseases and Injuries Collaborators Global burden of 369 diseases and injuries in 204 countries and territories, 1990-2019: a systematic analysis for the Global Burden of Disease Study 2019. LANCET. 2020;396(10258):1204–1222. doi: 10.1016/S0140-6736(20)30925-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- GBD 2019 Risk Factors Collaborators Global burden of 87 risk factors in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. LANCET. 2020;396(10258):1223–1249. doi: 10.1016/S0140-6736(20)30752-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- GBD 2020 Alcohol Collaborators Population-level risks of alcohol consumption by amount, geography, age, sex, and year: a systematic analysis for the Global Burden of Disease Study 2020. LANCET. 2022;400(10347):185–235. doi: 10.1016/S0140-6736(22)00847-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gloor B., Ahmed Z., Uhl W., Buchler M.W. Pancreatic disease in the elderly. Best Pract Res Cl Ga. 2002;16(1):159–170. doi: 10.1053/bega.2002.0272. [DOI] [PubMed] [Google Scholar]
- Howe L.D. Handbook on Health Inequality Monitoring. Int J Epidemiol. 2014;43(4):1345–1346. [Google Scholar]
- Institute for Health Metrics and Evaluation (IHME) Global Burden of Disease Study. (GBD 2019) Socio-Demographic Index (SDI) 1950–2019. In.; 2019.
- Irving H.M., Samokhvalov A.V., Rehm J. Alcohol as a risk factor for pancreatitis. A systematic review and meta-analysis. J Pancreas. 2009;10(4):387–392. [PMC free article] [PubMed] [Google Scholar]
- Jasilionis D., Leon D.A., Pechholdova M. Impact of alcohol on mortality in Eastern Europe: trends and policy responses. Drug Alcohol Rev. 2020;39(7):785–789. doi: 10.1111/dar.13167. [DOI] [PubMed] [Google Scholar]
- Jiang W., Du Y., Xiang C., Li X., Zhou W. Age-period-cohort analysis of pancreatitis epidemiological trends from 1990 to 2019 and forecasts for 2044: a systematic analysis from the Global Burden of Disease Study 2019. Front Public Health. 2023;11:1118888. doi: 10.3389/fpubh.2023.1118888. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kleeff J., Whitcomb D.C., Shimosegawa T., Esposito I., Lerch M.M., Gress T., Mayerle J., Drewes A.M., Rebours V., Akisik F., et al. Chronic pancreatitis. Nat Rev Dis Primers. 2017;3 doi: 10.1038/nrdp.2017.60. [DOI] [PubMed] [Google Scholar]
- Knoll M., Furkel J., Debus J., Abdollahi A., Karch A., Stock C. An R package for an integrated evaluation of statistical approaches to cancer incidence projection. Bmc Med Res Methodol. 2020;20(1):257. doi: 10.1186/s12874-020-01133-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Liu Z.Y., Tian L., Sun X.Y., Liu Z.S., Hao L.J., Shen W.W., Gao Y.Q., Zhai H.H. Development and validation of a risk prediction score for the severity of acute hypertriglyceridemic pancreatitis in Chinese patients. World J Gastroentero. 2022;28(33):4846–4860. doi: 10.3748/wjg.v28.i33.4846. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Liu C., Zhu S., Zhang J., Wu P., Wang X., Du S., Wang E., Kang Y., Song K., Yu J. Global, regional, and national burden of liver cancer due to non-alcoholic steatohepatitis, 1990–2019: a decomposition and age-period-cohort analysis. J Gastroenterol. 2023 doi: 10.1007/s00535-023-02040-4. [DOI] [PubMed] [Google Scholar]
- Moran R.A., Garcia-Rayado G., de la Iglesia-Garcia D., Martinez-Moneo E., Fort-Martorell E., Lauret-Brana E., Concepcion-Martin M., Ausania F., Prieto-Martinez C., Gonzalez-de-Cabo M., et al. Influence of age, body mass index and comorbidity on major outcomes in acute pancreatitis, a prospective nation-wide multicentre study. United Eur Gastroent. 2018;6(10):1508–1518. doi: 10.1177/2050640618798155. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mujica O.J., Moreno C.M. From words to action: measuring health inequalities to “leave no one behind”Da retorica a acao: mensurar as desigualdades em saude para nao deixar ninguem atras. Rev Panam Salud Publ. 2019;43:e12. doi: 10.26633/RPSP.2019.12. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Nathens A.B., Curtis J.R., Beale R.J., Cook D.J., Moreno R.P., Romand J.A., Skerrett S.J., Stapleton R.D., Ware L.B., Waldmann C.S. Management of the critically ill patient with severe acute pancreatitis. Crit Care Med. 2004;32(12):2524–2536. doi: 10.1097/01.ccm.0000148222.09869.92. [DOI] [PubMed] [Google Scholar]
- Nations U . United Nations; 2019. World Population Prospects 2019: Highlights. [Google Scholar]
- NCD Countdown 2030 Collaborators NCD Countdown 2030: worldwide trends in non-communicable disease mortality and progress towards Sustainable Development Goal target 3.4. LANCET. 2018;392(10152):1072–1088. doi: 10.1016/S0140-6736(18)31992-5. [DOI] [PubMed] [Google Scholar]
- Ouyang G., Pan G., Liu Q., Wu Y., Liu Z., Lu W., Li S., Zhou Z., Wen Y. The global, regional, and national burden of pancreatitis in 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Bmc Med. 2020;18(1):388. doi: 10.1186/s12916-020-01859-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pendharkar S.A., Mathew J., Zhao J., Windsor J.A., Exeter D.J., Petrov M.S. Ethnic and geographic variations in the incidence of pancreatitis and post-pancreatitis diabetes mellitus in New Zealand: a nationwide population-based study. New Zeal Med J. 2017;130(1450):55–68. [PubMed] [Google Scholar]
- Pendharkar S.A., Mathew J., Petrov M.S. Age- and sex-specific prevalence of diabetes associated with diseases of the exocrine pancreas: A population-based study. Digest Liver Dis. 2017;49(5):540–544. doi: 10.1016/j.dld.2016.12.010. [DOI] [PubMed] [Google Scholar]
- Petrov M.S., Yadav D. Global epidemiology and holistic prevention of pancreatitis. Nat Rev Gastro Hepat. 2019;16(3):175–184. doi: 10.1038/s41575-018-0087-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pilleron S., Sarfati D., Janssen-Heijnen M., Vignat J., Ferlay J., Bray F., Soerjomataram I. Global cancer incidence in older adults, 2012 and 2035: a population-based study. Int J Cancer. 2019;144(1):49–58. doi: 10.1002/ijc.31664. [DOI] [PubMed] [Google Scholar]
- Riebler A., Held L. Projecting the future burden of cancer: Bayesian age-period-cohort analysis with integrated nested Laplace approximations. Biometrical J. 2017;59(3):531–549. doi: 10.1002/bimj.201500263. [DOI] [PubMed] [Google Scholar]
- Sadighi A.A. Aging and the immune system: an overview. J Immunol Methods. 2018;463:21–26. doi: 10.1016/j.jim.2018.08.005. [DOI] [PubMed] [Google Scholar]
- Shield K.D., Rehm J. Societal development and the alcohol-attributable burden of disease. Addiction. 2021;116(9):2326–2338. doi: 10.1111/add.15441. [DOI] [PubMed] [Google Scholar]
- Stringhini S., Carmeli C., Jokela M., Avendano M., Muennig P., Guida F., Ricceri F., D'Errico A., Barros H., Bochud M., et al. Socioeconomic status and the 25 x 25 risk factors as determinants of premature mortality: a multicohort study and meta-analysis of 1.7 million men and women. Lancet. 2017;389(10075):1229–1237. doi: 10.1016/S0140-6736(16)32380-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Trikudanathan G., Wolbrink D., van Santvoort H.C., Mallery S., Freeman M., Besselink M.G. Current concepts in severe acute and necrotizing pancreatitis: an evidence-based approach. Gastroenterology. 2019;156(7):1994–2007. doi: 10.1053/j.gastro.2019.01.269. [DOI] [PubMed] [Google Scholar]
- Wang G.J., Gao C.F., Wei D., Wang C., Ding S.Q. Acute pancreatitis: etiology and common pathogenesis. World J Gastroentero. 2009;15(12):1427–1430. doi: 10.3748/wjg.15.1427. [DOI] [PMC free article] [PubMed] [Google Scholar]
- World HO . World Health Organization; Geneva: 2013. Handbook on health inequality monitoring with a special focus on low- and middle-income countries. [Google Scholar]
- World HO . World Health Organization; Geneva: 2021. WHO global report on trends in prevalence of tobacco use 2000–2025. [Google Scholar]
- Xiao A.Y., Tan M.L., Wu L.M., Asrani V.M., Windsor J.A., Yadav D., Petrov M.S. Global incidence and mortality of pancreatic diseases: a systematic review, meta-analysis, and meta-regression of population-based cohort studies. Lancet Gastroenterol. 2016;1(1):45–55. doi: 10.1016/S2468-1253(16)30004-8. [DOI] [PubMed] [Google Scholar]
- Yadav D., Lowenfels A.B. The epidemiology of pancreatitis and pancreatic cancer. Gastroenterology. 2013;144(6):1252–1261. doi: 10.1053/j.gastro.2013.01.068. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Yadav D., Whitcomb D.C. The role of alcohol and smoking in pancreatitis. Nat Rev Gastro Hepat. 2010;7(3):131–145. doi: 10.1038/nrgastro.2010.6. [DOI] [PubMed] [Google Scholar]
- Yang A.L., McNabb-Baltar J. Hypertriglyceridemia and acute pancreatitis. Pancreatology. 2020;20(5):795–800. doi: 10.1016/j.pan.2020.06.005. [DOI] [PubMed] [Google Scholar]
- Yu L., Xie F., Luo L., Lei Y., Huang X., Yang X., Zhu Y., He C., Li N., He W., et al. Clinical characteristics and risk factors of organ failure and death in necrotizing pancreatitis. Bmc Gastroenterol. 2023;23(1):19. doi: 10.1186/s12876-023-02651-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Yu J., Yang X., He W., Ye W. Burden of pancreatic cancer along with attributable risk factors in Europe between 1990 and 2019, and projections until 2039. Int J Cancer. 2021;149(5):993–1001. doi: 10.1002/ijc.33617. [DOI] [PubMed] [Google Scholar]
- Zhang J., Zhu S., Liu C., Xiao X., Xie H., Zhang Y., Hong Y. Colorectal cancer and its attributable risk factors in East Asia, 1990-2030. J Gastroen Hepatol. 2024 doi: 10.1111/jgh.16467. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
I explain the source of my data in the text.