Abstract
It has been appreciated over the past two decades that arterial remodelling, in addition to intimal hyperplasia, contributes significantly to the degree of restenosis that develops following revascularization procedures. Remodelling appears to be an adventitia-based process that is contributed to by multiple factors including cytokines and growth factors that regulate extracellular matrix or phenotypic transformation of vascular cells including myofibroblasts. In this review, we summarize the currently available information from animal models as well as clinical investigations regarding arterial remodelling. The factors that contribute to this process are presented with an emphasis on potential therapeutic methods to enhance favourable remodelling and prevent restenosis.
Keywords: Restenosis, Constrictive remodelling, Adaptive remodelling, ECM, EEL
1. Introduction
Atherosclerosis is pervasive and if untreated can lead to stroke, myocardial infarction, dialysis, or amputation. A frequent treatment of atherosclerosis is angioplasty; over two million percutaneous transluminal coronary angioplasties (PTCAs) are performed each year, representing one of the most common procedures in hospitals around the world. However, recurrent lumen narrowing (or restenosis) occurs in 30–50% of patients depending upon the artery treated, imposing a major limitation to the long-term success of these interventions.1,2 Restenosis post-vascular intervention is the sum of two processes: intimal hyperplasia, which is thickening of the tunica intima, and arterial remodelling, which results in a change in the size of the vessel. Arterial remodelling, which is the subject of this review, refers to a permanent change in artery diameter (as opposed to vasospasm or dilatation which produces a temporary change in artery size).
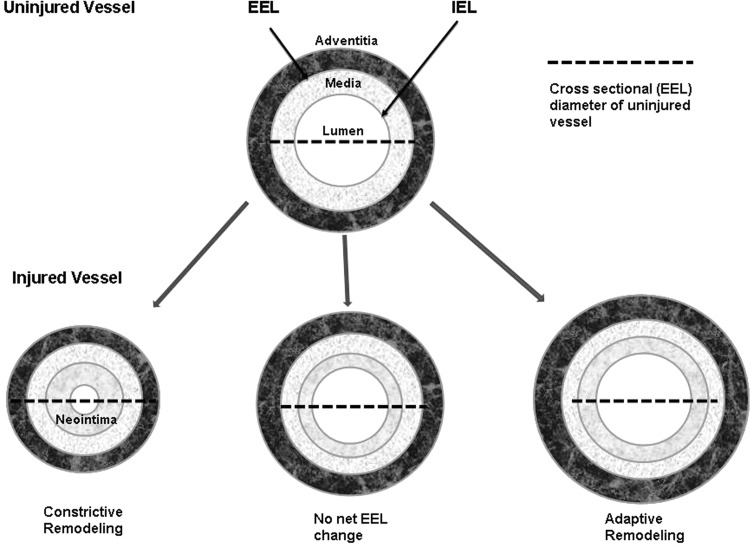
Innumerable studies have focused on the pathophysiology of intimal hyperplasia (see reviews).3–7 However, studies specifically dedicated to understanding the factors that produce arterial remodelling are less prevalent. Thus, the causes and pathophysiology of arterial remodelling have not been well delineated. 8 In this review, we attempt to report and reconcile currently available information on the molecular factors and possible pathways that lead to vessel remodelling. In the past, the term ‘remodelling’ has been used casually, in some cases referring to lumen narrowing caused by neointimal growth. In the current review, we have strictly defined arterial remodelling as a permanent (rather than reversible) geometric change in the vessel wall unrelated to the thickness of the neointima. Specifically, remodelling has been assessed by measuring the cross-sectional area within the external elastic lamina (EEL) or the EEL circumference (Figure 1).
Figure 1.
Definition of arterial remodelling following injury. In the studies cited in Tables 1–5, remodelling is often assessed by comparing the EEL (area, perimeter, or diameter) of the injured vessel in the presence and absence of a treatment that modulates a molecular factor.
Vascular remodelling may occur with de novo atherosclerosis or following vascular interventions such as angioplasty or bypass, or with transplant vasculopathy, or following the creation of an arteriovenous fistula. The underlying cause of remodelling following each of these interventions may be different.9 However, many of the causative factors may be similar. Therefore, while this review focuses primarily on post-angioplasty remodelling, pertinent evidence obtained from remodelling from other pathological processes will also be discussed.
Following arterial interventions, remodelling of the vessel wall can be either constrictive or adaptive. Constrictive, inward, or negative remodelling often accompanies intimal hyperplasia in patients treated with angioplasty. Both constrictive remodelling and intimal hyperplasia lead to luminal narrowing and the two together can greatly enhance the development of restenosis. Growing evidence indicates that constrictive remodelling may be as important or even a more important contributor to restenosis than intimal hyperplasia.10–14 Post et al.15 found that in both the rabbit and the hypercholesterolaemic Yucatan micropig, constrictive remodelling was the most important determinant of the late lumen loss. In the clinical setting, this finding has been reinforced by studies employing intracoronary ultrasound16,17 as well as histopathological analysis of specimens removed from patients treated with angioplasty.18
Alternatively, vessel enlargement, often denoted as adaptive, expansive, positive, or outward remodelling (Figure 1), has been observed in humans as a compensatory response to progressive growth of atherosclerotic plaques. This so-called Glagov phenomenon19 has stimulated widespread interest, since it is believed to postpone the development of a flow-limiting stenosis, although it is often inadequate to preserve luminal size. This same phenomenon is found in the setting of restenosis, as evidenced by an early study of an atherosclerotic rabbit model where vessel enlargement compensated for intimal formation following angioplasty.20 Prevention of lumen loss or even luminal enlargement after coronary balloon angioplasty has been achieved in animals by manipulating multiple factors including transforming growth factor beta (TGF-β1),21–25 matrix metalloproteinases (MMPs),26–28 oxidative stress,29,30 smad3,8 or VEGF.31 These discoveries have raised the prospect that manipulating these factors might lead in the clinical setting to outward arterial remodelling resulting in effective therapeutic methods to ameliorate restenosis.
In this review, we will describe current understanding of the factors and mechanisms that produce remodelling and the switch that influences whether this process is constrictive or adaptive. We hope to provide a useful guide for future investigations into this process with the goal of identifying techniques that can harness remodelling and provide more effective methods of treating restenosis in patients following vascular interventions. We apologize for the inability to reference all the relevant publications due to limited space.32–34
2. Current hypotheses regarding the pathophysiology of arterial remodelling
The events that control vascular remodelling remain poorly understood. While potentially all three layers of the vessel wall are involved, recent reports have suggested that remodelling is largely an adventitia-based process. The essential major players in arterial remodelling appear to be adventitial myofibroblasts as well as extracellular matrix (ECM).
The phenotypic conversion of fibroblasts to myofibroblasts is thought to be critical to this process and is considered by many as a hallmark of arterial remodelling following revascularization procedures.33–35 Myofibroblasts in turn produce and modify adventitial extracellular matrix. They also secrete pro-inflammatory factors, and alter tensile force. All of these are characteristic remodelling events.34 One hypothesis is that myofibroblasts interconnect by binding or ‘anchoring’ to ECM proteins such as collagen through integrins on the cell surface; thus, contraction of the myofibroblasts creates a constrictive band via their collagen interconnections that narrows the artery and the arterial lumen.33 Indeed, modulation of integrin expression has been reported to be associated with changes in vessel size.27 More investigations into the role of the myofibroblasts–ECM interaction in arterial remodelling are needed.
Because remodelling occurs well after the proliferation of myofibroblasts, it has been proposed that modification of the ECM plays an important role in injury-induced remodelling.14,32,34 The adventitial ECM is a reinforced composite of collagen and elastin fibres embedded in a viscoelastic gel of proteoglycans, hyaluronan, and water, together with a wide assortment of glycoproteins. These structurally varied components interact by entanglement and cross-linkages to form a bioactive polymer which, in part, regulates the biomechanical properties of the arterial wall.36 It is thus conceivable that changes either in the abundance, interaction, or organization of these ECM components may contribute to vascular remodelling.14
Collagen is a major ECM protein, which normally comprises 20–30% of the vascular protein content. Although both fibroblasts and smooth muscle cells (SMCs) produce collagen, fibroblasts, especially myofibroblasts, have been found to produce greater quantities of collagen than SMCs in balloon-injured arteries.10 Many studies have suggested that collagen plays an important role in arterial wall remodelling (see reviews14,32). Alterations in adventitial collagen content have been observed after angioplasty,37,38 which may result from both changes in synthesis as well as degradation.32
It has been hypothesized that excess collagen may form a constrictive band that shrinks the arterial wall.21 Indeed, in some studies, it has been observed that collagen is up-regulated in vessels affected by constrictive remodelling. In support of this hypothesis, several investigators have shown that down-regulation of collagen in vessels treated with angioplasty results in adaptive remodelling.21,24,25,39,40 However, the opposite finding has also been reported; that is, increased collagen levels in the vessel wall have been associated with adaptive remodelling after balloon injury.8,22,23,31 The accordant hypothesis is that collagen deposition in the ECM produces a scaffold holding the artery wall in place, thus preventing it from shrinking.22 Adding to the controversy are reports showing no change in collagen content associated with adaptive 41 or constrictive remodelling.22 Finally, there are examples of adventitial accumulation of collagen after vascular injury with no effect on vessel remodelling. In a study using an MMP-9 knockout mouse, elevated adventitial collagen content in the ligated carotid artery was associated with no change in the vessel EEL.42 These conflicting reports highlight the fact that the effect of collagen content on arterial remodelling remains undefined.
An alternative hypothesis is that not collagen content, but rather collagen cross-linking or the manner in which collagen molecules are compacted may be the determinant of arterial remodelling. In support of this hypothesis, administration of an inhibitor of collagen cross-linking (β-amino propionitrile) resulted in significant adaptive remodelling in the balloon-injured rabbit femoral vessel.39 Moreover, cystamine, an inhibitor of tissue transglutaminases (TTGs) which catalyze the crosslink of ECM proteins (including collagen), also produced enlargement of the EEL.43
There are multiple subtypes of collagen and thus collagen type may be another important factor influencing the effect of collagen on arterial remodelling. Among the collagen subtypes, collagen type 1 (CN1) and type 3 (CN3) are generally considered to be most relevant to arterial remodelling.8 Whereas CN1 is rigid in nature, CN3 is more elastic. Whether differential production of CN1 vs. CN3 plays an important role in this process remains to be elucidated. However, based on the aforementioned published data, it is reasonable to propose that the gross amount of collagen in the arterial wall is not the sole determinant of remodelling. Possibly following arterial injury, collective changes in collagen content, cross-linking, compaction of collagen fibrils, or also the distribution of collagen type may determine the final vessel geometry.
In addition to collagen, other ECM components, including fibronectin and elastin, have also been implicated as contributors to arterial remodelling. Application of an inhibitor of fibronectin polymerization to the ligated mouse carotid artery resulted in a significant diminution in the EEL.44 In a pig model of PTCA, VEGF165 gene transfer was associated with an increase in adventitial elastin and vessel enlargement.31
It has been well documented that the injury that follows vascular intervention such as angioplasty initiates an inflammatory response that constitutes an integral part of the remodelling processes.2,3 Also an important consequence of arterial injury is the production or activation of growth factors, cytokines, and a number of intracellular signalling pathways in both SMCs as well as fibroblasts. The consequence of at least some of these events may be the modification of adventitial ECM and stimulation of myofibroblasts leading to vessel remodelling (Figure 2). In the following section, we summarize the effects of various growth factors, proteolytic enzymes, and signalling molecules on injury-initiated arterial remodelling based on a broad range of published data. We have attempted to extract common themes about various factors that are particularly relevant to the remodelling process. Meanwhile, we also highlight areas of controversy that require additional study. It is clear from our analysis of the literature that the pathophysiology of arterial remodelling is far from completely defined.
Figure 2.
Schematic of the molecular factors that affect arterial remodelling (see text for details). For simplicity, the effect of these factors on intimal hyperplasia is not displayed, and the ECM proteins involved in remodelling are represented by collagen. TGF-β1, transforming growth factor β1; SMC, smooth muscle cell; ROS, reactive oxygen species; MMPs, matrix metaloproteinases; TTGs, tissue transglutaminases; EEL, external elastic lamina; IEL, internal elastic lamina.
3. Major factors participating in arterial remodelling
3.1. TGF-β1
It is generally accepted that the TGF-β family, especially TGF-β1, plays a pivotal role in arterial remodelling.2,8 TGF-β1 is a potent multifunctional regulator of a variety of vascular cellular activities, including SMC proliferation, ECM production, phenotypic conversion of adventitial fibroblasts to myofibroblasts, as well as others. Active TGF-β1 initiates cell signalling by binding to the TGF-β1 receptor type II (TβR-II), which then recruits TGF-β1 receptor type I (TβR-I). This heterotetrameric receptor complex results in activation of intracellular serine-threonine kinases on TβR-II and TβR-I, and in turn facilitates phosphorylation of Smad proteins, which represent the principal TGF-β1 signalling pathway.45 Phosphorylated Smad2 and Smad3 form a complex with Smad4, and this complex translocates to the nucleus regulating gene expression by interacting with transcription factors or binding directly to DNA. Alternatively, TGF-β1 may signal through Smad-independent pathways involving p38 MAPK, JNK, and protein kinase C.
A wealth of information is available regarding the mechanisms by which TGF-β1 regulates neo-intimal formation (see reviews3,46). In contrast, much less is known about the precise role of TGF-β signalling in post-angioplasty/injury arterial remodelling. TGF-β1 expression has been shown to be up-regulated in balloon catheter-injured carotid or coronary arteries in both animal models as well as in human restenotic vessels (see review2). Consequently, considerable effort has been invested in exploring the relationship between TGF-β1 and intimal hyperplasia (or vessel remodelling) by employing agonists or antagonists of TGF-β1 in experimental models of angioplasty. As summarized in Table 1, inhibition of TGF-β1 activity using a soluble form of TβR-II,21,23,24 or expression of TGF-β322 or Smad7,25 all antagonists of TGF-β1 signalling, has been found to attenuate constrictive remodelling. Consistent with these findings, overexpression of TGF-β1 resulted in a reduction in EEL in a porcine angioplasty model.22 These data strongly suggest that TGF-β1 is a potent contributor to constrictive remodelling.
Table 1.
Effects of TGF-β1 on remodelling
| Treatment | Model | Injury site | Method | Neo-intima | EEL/IEL | Lumen loss | CN | Remodelling | Reference |
|---|---|---|---|---|---|---|---|---|---|
| ⇓, Soluble TβR-II | Rat | Carotid | Balloon | ↓ | ↑EEL ↑IEL | ↓ | ↓CN | Adaptive | 21 |
| ⇓, Soluble TβR-II | Pig | Carotid | Balloon | ↓ | ↑EEL ↑IEL | ↓ | ↑CN | Adaptive | 23 |
| ⇓, Soluble TβR-II | Rat | Carotid | Balloon | ↓ | ↑ CSA | ↓ | ↓CN | Adaptive | 24 |
| ⇓, TGF-β3 expression | Pig | Coronary | Balloon | ↑ | ↑EEL ↑IEL | ↓ | ↑CN | Adaptive | 22 |
| ⇓, Smad7 expression | Rat | Carotid | Balloon | ↓ | ↑ CSA | ↓ | ↓CN | Adaptive | 25 |
| ⇓, Smad3 k/o | Mice | Femoral | Photo-Chem. | ↑ | ↑IEL | ↓ | ↔CN | Adaptive | 41 |
| ⇑, TGF-β1 expression | Pig | Coronary | Balloon | ↓ | ↓EEL ↓IEL | ↓ | ↔CN | Constrictive | 22 |
| ⇑, Smad3 expression | Rat | Carotid | Balloon | ↑ | ↑EEL | ↓ | ↑CN | Adaptive | 8 |
⇑ and ⇓, up and down regulation of the activity or expression of TGF-β1. TβR-II, TGF-β1 receptor type II. CSA, cross section area, which usually equates EEL area. K/O, knockout. CN, collagen. ‘↔’, no change in collagen content.
Throughout the tables, adaptive remodelling refers to an increase in EEL when compared with the experimental control.
Conversely, overexpression of Smad3, the primary signalling mediator for TGF-β1, in a rat carotid balloon injury model, resulted in arterial expansion rather than constriction.8 The authors postulated that this effect of Smad3 on adaptive remodelling may be mediated by connective tissue growth factor (CTGF), production of which is enhanced in response to TGF-β1/Smad3 signalling. In line with this hypothesis, periadventitial application of CTGF mimicked the effect of TGF-β1/Smad3 on adaptive remodelling.8 However, in a study where Smad3 knockout mice were used, arterial injury resulted in adaptive rather than constrictive remodelling.41 Of note in this model, Smad3 was universally deficient in all cells, whereas in the overexpression studies, Smad3 was manipulated in the arterial wall only. Nevertheless, the precise effect of Smad3 on remodelling remains unclear.
In sum, there is substantial evidence that the cytokine, TGF-β1, plays an active role in producing constrictive remodelling. However, in the presence of elevated levels of Smad3, this effect may be reversed. TGF-β1 has many downstream effects that have the potential to affect arterial remodelling (Figure 2). MMPs appear to be integral to remodelling, and accumulating evidence suggests that MMPs are downstream targets of the TGF-β1 signalling.2 However, very little information is currently available regarding the molecular details of the TGF-β1/MMP axis in arterial remodelling.
3.2. MMPs and TTGs
It is clear that adventitial extracellular matrix, particularly collagen, plays an important role in vascular remodelling. The family of MMPs is capable of degrading all components of the ECM, suggesting a potentially important role for MMPs in the remodelling process. The activity of MMPs is controlled at different levels, including transcription, activation of zymogens, and interaction with specific inhibitors, such as tissue inhibitor of metalloproteinases.47 Within the MMP family, MMP-2 and MMP-9 have attracted particular interest in relation to vascular remodelling, due to their expression by SMCs and their ability to breakdown components of the basement membrane and collagen. While expression of MMP-2 can be detected in the normal media, MMP-9 expression becomes apparent only after injury or an inflammatory stimulus.48
In a rat carotid balloon angioplasty model, MMP-9 overexpression was found to reduce lumen loss by promoting adaptive remodelling (Table 2).49 Consistent with this result, in a carotid ligation mouse model, in ApoE knockout mice vs. wild type, there was an increase in macrophage foam cells, enhanced MMP-9 activity, and also enhanced adaptive remodelling.50 These studies have led to the hypothesis that enhancement of MMPs accelerates breakdown of adventitial ECM, thus relieving the constraint provided by extracellular matrix on vessel enlargement. However, the reports have not been consistent. In a model of balloon angioplasty in the Yucatan micropig iliac artery26 or in a rat carotid artery injury model,27 administration of an MMP inhibitor, Batimastat, promoted adaptive rather than constrictive remodelling of these injured vessels. In a porcine femoral balloon injury model, a different MMP inhibitor (Marimastat) also promoted adaptive remodelling.28 Moreover, in a recent study in the balloon-injured rabbit iliac artery, suppression of MMP-2 activity by low-dose bacterial endotoxin resulted in adaptive remodelling.51 Specifically evaluating MMP-9, Galis et al.42 compared arterial remodelling in a carotid ligation model in MMP-9 knockout vs. wild-type mice. There was increased accumulation of adventitial collagen in knockout mice; however, arterial remodelling was unchanged in knockout vs. wild type. Thus, the question still remains as to whether MMPs through their effects on ECM lead to adaptive or constrictive remodelling. The discrepancy between these studies highlights the complexity of the relationship between the ECM and arterial remodelling, which defies an oversimplified theory.
Table 2.
Effects of MMPs and TTGs on remodelling
| Treatment | Model | Injury site | Method | Neo-intima | EEL/IEL | Lumen loss | CN | Remodelling | Reference |
|---|---|---|---|---|---|---|---|---|---|
| ⇑, MMP-9 expression | Rat | Carotid | Balloon | ↑ | ↑IEL | ↓ | Adaptive | 49 | |
| ⇑, ApoE k/oa | Mice | Carotid | Ligation | ↑ | ↑CSA | ↑ | Adaptive | 50 | |
| ⇓, Batimastatb | Pig | Iliac | Balloon | ↔ | ↑EEL | ↓ | Adaptive | 26 | |
| ⇓, Batimastatb | Rat | Carotid | Balloon | ↓ | ↑EEL | ↓ | Adaptive | 27 | |
| ⇓, Marimastatb | Pig | Femoral, Internal iliac | Balloon | ↔ | ↑CSA | ↓ | Adaptive | 28 | |
| ⇓, MMP-9 k/o | Mouse | Carotid | Ligation | ↓ | ↔EEL | ↓ | ↑ | ↔ | 42 |
| ⇓, Low dose LPSc | Rabbit | Iliac | Balloon | ↑ | ↑EEL | ↔ | Adaptive | 51 | |
| ⇓,Cystamine (TTG inhibitor) | Rat | Mesentric | Ligation | ↑EEL | Adaptive | 43 |
⇑ and ⇓, up and down regulation of the activity or expression of MMPs. aElevated MMP-9 activity due to the increase of macrophages. bMMP inhibitors. cLow dose of bacterial endotoxin suppressed the MMP-2 activity.
In contrast to the activity of MMPs, which enhance ECM degradation, TTGs catalyze protein cross-linking and ECM protein binding. Bakker et al.43 have shown that treatment with cystamine, a TTG blocker, resulted in increased EEL perimeter of the mesenteric artery in a rat ligation model. An interesting question that remains unsolved is whether TTG's effect on vascular remodelling in this model is through regulation of collagen cross-linking and organization.
The aforementioned studies suggest that both MMPs and TTGs play an important role in the composition and organization of vascular ECM and thus both have the potential to influence vascular remodelling. It is also known that growth factors such as TGF-β1 and PDGF modulate the activities of both of these proteins (see review32). Although the intermediates between growth factors and the ECM are not well understood, some signalling molecules, in particular nitric oxide (NO), are believed to play an important role.48 For example, NO has been shown to modulate the process of vessel remodelling by altering the production of both TTGs and MMP.52,53
3.3. Nitric oxide
The role of NO in arterial remodelling has been evaluated using balloon angioplasty, fistula as well as ligation models. These studies collectively suggest that NO promotes arterial remodelling in the form of vessel expansion.
In a rabbit carotid balloon injury model, Bosmans et al.54 have shown that perivascular application of l-arginine, which generates NO, results in an increase in EEL while also suppressing neointimal growth (Table 3). Moreover, an inhibitor of NO synthesis, nitro l-arginine methyl ester (NAME), has been reported to produce constrictive remodelling in a rabbit fistula model connecting the common carotid artery and the jugular vein.55 Reinforcing these findings and supporting a role for NO in vessel adaptive remodelling, studies conducted with either nNOS knockout56 or n/i/eNOS triple knockout mice57 revealed a decrease in the EEL area following carotid artery ligation. Moreover, a study has been carried out to compare differential roles of iNOS and eNOS in protection against restenosis using the carotid ligation model.58 Interestingly, in iNOS knockout mice, constrictive remodelling but not intimal hyperplasia was exacerbated when compared with the wild type, whereas in the eNOS knockout, intima thickening rather than constrictive remodelling was increased. The findings are not all consistent; in a rat carotid balloon injury model, an nNOS inhibitor, 7-nitroindazole, accentuated intimal hyperplasia but had no effect on arterial geometry.56 Nevertheless, the majority of studies have shown NO to be effective at suppressing intimal thickening while also promoting adaptive arterial remodelling.
Table 3.
Effects of NO on remodelling
| Treatment | Model | Injury site | Method | Neo-intima | EEL/IEL | Lumen loss | CN | Remodelling | Reference |
|---|---|---|---|---|---|---|---|---|---|
| ⇑, l-Arginine | Rabbit | Carotid | Balloon | ↓ | ↑EEL | ↓ | Adaptive | 54 | |
| ⇓, l-NAME | Rabbit | Carotid | Fistula | ↓CSA | ↑ | Constrictive | 55 | ||
| ⇓, nNOS k/o | Mice | Carotid | Ligation | ↑ | ↓ | ↑ | Constrictive | 56 | |
| ⇓, n,I,eNOS triple k/o | Mice | Carotid | Ligation | ↑ | ↓CSA | ↑ | Constrictive | 57 | |
| ⇓, nNOS inhibitora | Rat | Carotid | Balloon | ↑ | ↔ | ↑ | ↔ | 56 |
⇑ and ⇓, up and down regulation of NO production. l-NAME, nitro l-arginine methyl ester, an inhibitor for NO synthesis. a7-nitroindazole.
There is a great deal known about the mechanism behind NO's role as a vasodilator. In contrast, very little is known about the biological interplay of NO with the factors that lead to adaptive remodelling. It is conceivable that NO contributes to arterial remodelling through activation of MMPs, inhibition of TTG activity,52 or reaction with superoxide.59
3.4. Oxidative stress
Oxidative stress is a general term used to describe the steady-state level of oxidative damage in a cell, tissue, or organ, caused by reactive oxygen species (ROS). ROS levels in the adventitia of the porcine coronary artery increase substantially following balloon injury.60 Moreover, increased oxidative stress has correlated positively with the development of restenosis. Antioxidants have been shown to reduce restenosis; it has been demonstrated that the beneficial effects of antioxidants on restenosis are at least in part attributable to adaptive remodelling of the vessel wall. For example, Nunes et al.29 found that the combined use of vitamins C and E reduced the lumen loss without modifying the degree of intimal hyperplasia after balloon injury in a porcine model (Table 4). Using a rabbit angioplasty model, Durand et al.61 have shown that local expression of antioxidant enzymes, superoxide dismutase (SOD) and catalase, reduced ROS production and constrictive remodelling of the iliac artery. Importantly, based upon the data from patients treated with coronary balloon angioplasty, Probucol, a strong antioxidant agent which was given preoperatively, reduced restenosis by preventing constrictive remodelling.30 These studies together suggest a beneficial effect of antioxidants in that they promote adaptive remodelling or at minimum they prevent constrictive remodelling. Another interesting example is haem oxygenase-1 (HO-1), a vascular protective enzyme with potent anti-inflammatory and anti-oxidant effects. A recent study revealed a strong association between HO-1 promoter polymorphism and restenosis in patients undergoing femoropopliteal balloon angioplasty. This association was absent in the patients with stent implantation.1 Because restenosis after stenting is mainly due to in-stent neointimal hyperplasia,62 the authors speculated that the beneficial effects of HO-1 after balloon angioplasty were mainly due to an attenuation of constrictive remodelling. In another study in pigs, HO-1 gene transfer into the injured femoral artery effectively reduced intimal hyperplasia, but did not alter the EEL area when compared with control.63 Thus, more thorough investigations are needed to further elucidate the role of HO-1 in remodelling. Nevertheless, the role of antioxidants in the treatment of vascular disease remains controversial without a solidly demonstrable benefit. In terms of mechanism, it is worth noting that simultaneous production of superoxide and NO generates peroxynitrite that activates latent MMPs,59 suggesting a relationship between three of the factors that have been shown to regulate arterial remodelling.
Table 4.
Effects of oxidative stress on remodelling
| Treatment | Model | Injury site | Method | Neo-intima | EEL/IEL | Lumen loss | CN | Remodelling | Reference |
|---|---|---|---|---|---|---|---|---|---|
| ⇓, Vitamins C and E | Pig | Coronary | Balloon | ↔ | ↓ | Adaptive | 29 | ||
| ⇓, Probucol | Human | Coronary | Balloon | ↑EEMa | ↓ | Adaptive | 30 | ||
| ⇓, SOD/catalase expression | Rabbit | Iliac | Balloon | ↓ | ↑EEL | ↓ | ↓b | Adaptive | 61 |
⇓, reduction of oxidative stresses. aEEM, external elastic membrane, a parameter used in ultrasound studies that equates EEL. bDecrease of collagen density.
3.5. Other factors
Multiple factors have been evaluated with regard to their ability to affect restenosis. Most often, the primary outcome measured has been intimal thickness or intimal hyperplasia. Vessel size or arterial remodelling are less frequently assessed. We have, however, searched for additional factors beyond those already discussed, effects of which on arterial remodelling have been assessed (Table 5). In a pig PTCA model, VEGF165 gene transfer to the adventitia prevented the lumen loss by inducing adaptive remodelling.31 In several studies with angioplasty models, it has been reported that inhibition of PDGF reduces intimal hyperplasia, but no effect on vessel diameter has been observed.64,65 ADAMTS (a disintegrin and metalloproteinase with thrombospondin motifs) represents a family of zinc metalloproteinases that degrade ECM components such as versican and procollagen.32 It has been shown in a carotid ligation model using ApoE knockout mice that ADAMTS-1 overexpression stimulated intimal growth and also slightly increased vessel size.66 However, in another recent report, ADAMTS-7 knockdown in a balloon-injured rat carotid artery reduced intimal hyperplasia but did not produce a change in EEL.67 It will be worthwhile in the future to address whether ADAMTS subtypes have differential effects on remodelling. Two physiologically important plasminogen activators, the tissue type (tPA) and the urokinase type (uPA), have been identified, both up-regulated following balloon injury of the rat carotid artery. Interestingly, while perivascular administration of recombinant tPA to the injured vessel produced adaptive remodelling, recombinant uPA had an opposite effect.68
Table 5.
Miscellaneous factors
| Treatment | Model | Injury site | Method | Neo-intima | EEL/IEL | Lumen loss | CN | Remodelling | Reference |
|---|---|---|---|---|---|---|---|---|---|
| ⇑,VEGF | Pig | Coronary | Balloon | ↑EEL | ↓ | ↑ | Adaptive | 31 | |
| ⇓, Eplerenonea | Micro-pig | Coronary | Balloon | ↔ | ↑EEL | ↓ | ↓ | Adaptive | 40 |
| ⇓, (β-APN)b | Rabbit | Femoral | Balloon | ↓ | ↑EEL | ↓ | ↓ | Adaptive | 39 |
| ⇓, pUR4c | Mouse | Carotid | Ligation | ↓ | ↓EEL | ↑ | ↓ | Constrictive | 44 |
| ⇑, tPAd | Rat | Carotid | Balloon | ↓ | ↑EEL | ↑ | Adaptive | 68 | |
| ⇑, uPAe | Rat | Carotid | Balloon | ↑ | ↓EEL | ↓ | Constrictive | 68 | |
| ⇑, ADAMTS-1 | Mouse | Carotid | Ligation | ↑ | ↑CSA | ↔ | Adaptive | 66 |
aEplerenone reduces collagen content by inhibiting mineralocorticoid receptors. bβ-APN, β-amino propionitrile (inhibitor of collagen crosslinking). cpUR4, inhibitor of fibronectin polymerization. dTissue-type plasminogen activator. eUrokinase plasminogen activator.
There are a number of cytokines, growth factors, and enzymes that have the potential to alter the levels of MMPs, NO, and ROS, and theoretically any of these could affect arterial remodelling. For example, treatment of the injured rat carotid artery with IGF-1 has been found to stimulate eNOS expression.69 Thus, it is not unreasonable to speculate that IGF-1 may modulate arterial remodelling via the NO pathway. As more studies are performed to elucidate the specific contribution of the individual factors to arterial remodelling, additional targets are expected to emerge which will potentially afford new therapeutic solutions.
4. Potential opportunities and challenges in therapeutic targeting of arterial remodelling
Currently, the only clinically available effective treatments of restenosis are rapamycin- and paclitaxel-coated stents. However, when stents are used, arterial remodelling becomes irrelevant, since the stent fixes and prevents modification of the absolute vessel diameter.62 Other methods of drug delivery are rapidly coming to fruition including drug-coated balloons where adaptive remodelling could play an important role in the eventual outcome of these interventions. Moreover, external or perivascular application of drugs following surgical bypass or endarterectomy is an additional approach, through which the treatments that effect adaptive remodelling could be beneficial. Interestingly with this approach, drug is delivered directly to the vessel adventitia with the potential of having a profound effect on adaptive remodelling. Combination drug therapy as a treatment of restenosis is appealing, if two drugs with different and potentially synergistic effects can be combined. One could imagine a drug that inhibits intimal hyperplasia and a second that stimulates adaptive remodelling would have a powerful combined effect on restenosis.
It is worth noting that most of the therapeutic trials thus far have had the degree of intimal thickening as their primary target. Measures of adaptive or constrictive remodelling from the clinical setting are largely lacking. However, as the importance of remodelling in cardiovascular diseases is increasingly recognized, there is likely to be growing interest in targeting the regulatory factors to either reduce constrictive or promote adaptive remodelling. Locally modifying factors such as TGF-β1, MMPs, NO, or ROS may represent useful strategies to treat restenosis through attenuation of vessel constriction. Although currently there are no drugs that are clinically used to specifically target the remodelling process, encouraging studies have emerged, such as a report on Probucol, an antioxidant, has been shown to reduce constrictive remodelling following angioplasty when taken pre-operatively by patients.30 In addition, based upon animal studies, some TGF-β1-inhibiting agents and MMP-9 inhibitors, NO donors, and antioxidants should be considered possible therapeutics targeting arterial remodelling. In the future, more clinical trials are warranted to identify drugs that can positively and effectively influence the remodelling process.
In spite of the positive remodelling effects of treatments targeting the molecular factors listed in Tables 1–5, great challenges exist in translating positive pre-clinical results into clinically successful therapies.
For example, there is likely a strong relationship between intimal hyperplasia and vessel remodelling. In fact, vessel enlargement may be an adaptive response to intimal hyperplasia (i.e. the vessel's way of compensating for the luminal narrowing produced by intimal thickening). It may well be that adaptive remodelling occurs only after signals are released from the intimal plaque. Inevitably, the two processes are closely tied together; e.g. up-regulation of the TGF-β1 signalling protein, Smad3, has been shown to produce adaptive remodelling while also inducing intimal growth.8 It should also be appreciated that the molecular factors involved in arterial remodelling are often multifunctional and exert differential actions on many cell types throughout the arterial wall. Thus, either precisely controlled local drug delivery to the adventitia or drugs that discriminate vascular cell types may be critical in selective modification of vessel wall geometry. Lastly, crosstalk among pathways may play an important role in the remodelling process; manipulation of one portion of the process may affect another. For example, drugs that produce collagen breakdown have been shown to be favourable for adaptive remodelling in some angioplasty models.49 However, collagen degradation products are potent stimulants for monocytes and myofibroblasts, both of which contribute to constrictive remodelling.32 There is little doubt that arterial remodelling is a very complex process, the mechanism of which is far from defined. Consequently, we remain a distance away from translational therapies attaining beneficial vessel enlargement.
5. Conclusion
Growing evidence suggests that constrictive remodelling may be as much a culprit as intimal hyperplasia in producing permanent lumen loss after vascular interventions.10–14 In stark contrast to the wealth of information that is available regarding intimal hyperplasia, the data on remodelling are limited and often can only be extracted from studies of restenosis with a focus on intimal hyperplasia. Nevertheless, in studies where arterial modelling has been assessed, several factors have been identified that have the potential to regulate this process. There is a growing appreciation that arterial remodelling is an adventitial process that is affected by both myofibroblasts as well as a host of ECM proteins, including collagen.34 Current evidence indicates that multiple factors are involved in post-intervention arterial remodelling. Rather than acting independently, these factors are likely to be interlinked through crosstalk between different pathways. Still, a great deal of controversy remains and there are many conflicting studies. Thus, there is great need and opportunity for future research in this interesting and important pathophysiological process that contributes to recurrent vascular disease.
Funding
This work was supported by a Public Health Service Grant R01-HL-068673 (to K.C.K. and B.L.) from the National Heart, Lung, and Blood Institute.
Conflict of interest: none declared
References
- 1.Schillinger M, Exner M, Minar E, Mlekusch W, Mullner M, Mannhalter C, et al. Heme oxygenase-1 genotype and restenosis after balloon angioplasty: a novel vascular protective factor. J Am Coll Cardiol. 2004;43:950–957. doi: 10.1016/j.jacc.2003.09.058. doi:10.1016/j.jacc.2003.09.058. [DOI] [PubMed] [Google Scholar]
- 2.Khan R, Agrotis A, Bobik A. Understanding the role of transforming growth factor-beta1 in intimal thickening after vascular injury. Cardiovasc Res. 2007;74:223–234. doi: 10.1016/j.cardiores.2007.02.012. doi:10.1016/j.cardiores.2007.02.012. [DOI] [PubMed] [Google Scholar]
- 3.Suwanabol PA, Kent KC, Liu B. TGF-beta and restenosis revisited: a Smad link. J Surg Res. 2011;167:287–297. doi: 10.1016/j.jss.2010.12.020. doi:10.1016/j.jss.2010.12.020. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Tsai S, Butler J, Rafii S, Liu B, Kent KC. The role of progenitor cells in the development of intimal hyperplasia. J Vasc Surg. 2009;49:502–510. doi: 10.1016/j.jvs.2008.07.060. doi:10.1016/j.jvs.2008.07.060. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Weintraub WS. The pathophysiology and burden of restenosis. Am J Cardiol. 2007;100:3K–9K. doi: 10.1016/j.amjcard.2007.06.002. doi:10.1016/j.amjcard.2007.06.002. [DOI] [PubMed] [Google Scholar]
- 6.Ahanchi SS, Tsihlis ND, Kibbe MR. The role of nitric oxide in the pathophysiology of intimal hyperplasia. J Vasc Surg. 2007;45(Suppl. A):A64–A73. doi: 10.1016/j.jvs.2007.02.027. doi:10.1016/j.jvs.2007.02.027. [DOI] [PubMed] [Google Scholar]
- 7.Agrotis A, Kalinina N, Bobik A. Transforming growth factor-beta, cell signaling and cardiovascular disorders. Curr Vasc Pharmacol. 2005;3:55–61. doi: 10.2174/1570161052773951. doi:10.2174/1570161052773951. [DOI] [PubMed] [Google Scholar]
- 8.Kundi R, Hollenbeck ST, Yamanouchi D, Herman BC, Edlin R, Ryer EJ. Arterial gene transfer of the TGF-beta signalling protein Smad3 induces adaptive remodelling following angioplasty: a role for CTGF. Cardiovasc Res. 2009;84:326–335. doi: 10.1093/cvr/cvp220. doi:10.1093/cvr/cvp220. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Ward MR, Pasterkamp G, Yeung AC, Borst C. Arterial remodeling. Mechanisms and clinical implications. Circulation. 2000;102:1186–1191. doi: 10.1161/01.cir.102.10.1186. doi:10.1161/01.CIR.102.10.1186. [DOI] [PubMed] [Google Scholar]
- 10.Geary RL, Nikkari ST, Wagner WD, Williams JK, Adams MR, Dean RH. Wound healing: a paradigm for lumen narrowing after arterial reconstruction. J Vasc Surg. 1998;27:96–106. doi: 10.1016/s0741-5214(98)70296-4. discussion 106–108 doi:10.1016/S0741-5214(98)70296-4. [DOI] [PubMed] [Google Scholar]
- 11.Mintz GS, Popma JJ, Pichard AD, Kent KM, Satler LF, Hong MK. Intravascular ultrasound assessment of the mechanisms and predictors of restenosis following coronary angioplasty. J Invasive Cardiol. 1996;8:1–14. [PubMed] [Google Scholar]
- 12.Pasterkamp G, Galis ZS, de Kleijn DP. Expansive arterial remodeling: location, location, location. Arterioscler Thromb Vasc Biol. 2004;24:650–657. doi: 10.1161/01.ATV.0000120376.09047.fe. doi:10.1161/01.ATV.0000120376.09047.fe. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Gertz SD, Barry WL, Gimple LW, Banai S, Perez LS, McNamara CA. Predictors of luminal narrowing by neointima after angioplasty in atherosclerotic rabbits. Cardiovasc Res. 1997;36:396–407. doi: 10.1016/s0008-6363(97)00168-5. doi:10.1016/S0008-6363(97)00168-5. [DOI] [PubMed] [Google Scholar]
- 14.Faxon DP, Coats W, Currier J. Remodeling of the coronary artery after vascular injury. Prog Cardiovasc Dis. 1997;40:129–140. doi: 10.1016/s0033-0620(97)80005-9. doi:10.1016/S0033-0620(97)80005-9. [DOI] [PubMed] [Google Scholar]
- 15.Post MJ, Borst C, Kuntz RE. The relative importance of arterial remodeling compared with intimal hyperplasia in lumen renarrowing after balloon angioplasty. A study in the normal rabbit and the hypercholesterolemic Yucatan micropig. Circulation. 1994;89:2816–2821. doi: 10.1161/01.cir.89.6.2816. doi:10.1161/01.CIR.89.6.2816. [DOI] [PubMed] [Google Scholar]
- 16.Mintz GS, Popma JJ, Pichard AD, Kent KM, Satler LF, Wong C. Arterial remodeling after coronary angioplasty: a serial intravascular ultrasound study. Circulation. 1996;94:35–43. doi: 10.1161/01.cir.94.1.35. doi:10.1161/01.CIR.94.1.35. [DOI] [PubMed] [Google Scholar]
- 17.Mintz GS, Popma JJ, Pichard AD, Kent KM, Salter LF, Chuang YC. Intravascular ultrasound predictors of restenosis after percutaneous transcatheter coronary revascularization. J Am Coll Cardiol. 1996;27:1678–1687. doi: 10.1016/0735-1097(96)00083-6. doi:10.1016/0735-1097(96)00083-6. [DOI] [PubMed] [Google Scholar]
- 18.Sangiorgi G, Taylor AJ, Farb A, Carter AJ, Edwards WD, Holmes DR. Histopathology of postpercutaneous transluminal coronary angioplasty remodeling in human coronary arteries. Am Heart J. 1999;138:681–687. doi: 10.1016/s0002-8703(99)70183-3. doi:10.1016/S0002-8703(99)70183-3. [DOI] [PubMed] [Google Scholar]
- 19.Glagov S, Weisenberg E, Zarins CK, Stankunavicius R, Kolettis GJ. Compensatory enlargement of human atherosclerotic coronary arteries. N Engl J Med. 1987;316:1371–1375. doi: 10.1056/NEJM198705283162204. doi:10.1056/NEJM198705283162204. [DOI] [PubMed] [Google Scholar]
- 20.Kakuta T, Currier JW, Haudenschild CC, Ryan TJ, Faxon DP. Differences in compensatory vessel enlargement, not intimal formation, account for restenosis after angioplasty in the hypercholesterolemic rabbit model. Circulation. 1994;89:2809–2815. doi: 10.1161/01.cir.89.6.2809. doi:10.1161/01.CIR.89.6.2809. [DOI] [PubMed] [Google Scholar]
- 21.Smith JD, Bryant SR, Couper LL, Vary CP, Gotwals PJ, Koteliansky VE. Soluble transforming growth factor-beta type II receptor inhibits negative remodeling, fibroblast transdifferentiation, and intimal lesion formation but not endothelial growth. Circ Res. 1999;84:1212–1222. doi: 10.1161/01.res.84.10.1212. doi:10.1161/01.RES.84.10.1212. [DOI] [PubMed] [Google Scholar]
- 22.Kingston PA, Sinha S, Appleby CE, David A, Verakis T, Castro MG. Adenovirus-mediated gene transfer of transforming growth factor-beta3, but not transforming growth factor-beta1, inhibits constrictive remodeling and reduces luminal loss after coronary angioplasty. Circulation. 2003;108:2819–2825. doi: 10.1161/01.CIR.0000097068.49080.A0. doi:10.1161/01.CIR.0000097068.49080.A0. [DOI] [PubMed] [Google Scholar]
- 23.Kingston PA, Sinha S, David A, Castro MG, Lowenstein PR, Heagerty AM. Adenovirus-mediated gene transfer of a secreted transforming growth factor-beta type II receptor inhibits luminal loss and constrictive remodeling after coronary angioplasty and enhances adventitial collagen deposition. Circulation. 2001;104:2595–2601. doi: 10.1161/hc4601.099405. doi:10.1161/hc4601.099405. [DOI] [PubMed] [Google Scholar]
- 24.Ryan ST, Koteliansky VE, Gotwals PJ, Lindner V. Transforming growth factor-beta-dependent events in vascular remodeling following arterial injury. J Vasc Res. 2003;40:37–46. doi: 10.1159/000068937. doi:10.1159/000068937. [DOI] [PubMed] [Google Scholar]
- 25.Mallawaarachchi CM, Weissberg PL, Siow RC. Smad7 gene transfer attenuates adventitial cell migration and vascular remodeling after balloon injury. Arterioscler Thromb Vasc Biol. 2005;25:1383–1387. doi: 10.1161/01.ATV.0000168415.33812.51. doi:10.1161/01.ATV.0000168415.33812.51. [DOI] [PubMed] [Google Scholar]
- 26.de Smet BJ, de Kleijn D, Hanemaaijer R, Verheijen JH, Robertus L, van Der Helm YJ. Metalloproteinase inhibition reduces constrictive arterial remodeling after balloon angioplasty: a study in the atherosclerotic Yucatan micropig. Circulation. 2000;101:2962–2967. doi: 10.1161/01.cir.101.25.2962. doi:10.1161/01.CIR.101.25.2962. [DOI] [PubMed] [Google Scholar]
- 27.Margolin L, Fishbein I, Banai S, Golomb G, Reich R, Perez LS. Metalloproteinase inhibitor attenuates neointima formation and constrictive remodeling after angioplasty in rats: augmentative effect of alpha(v)beta(3) receptor blockade. Atherosclerosis. 2002;163:269–277. doi: 10.1016/s0021-9150(02)00035-7. doi:10.1016/S0021-9150(02)00035-7. [DOI] [PubMed] [Google Scholar]
- 28.Sierevogel MJ, Velema E, van der Meer FJ, Nijhuis MO, Smeets M, de Kleijn DP. Matrix metalloproteinase inhibition reduces adventitial thickening and collagen accumulation following balloon dilation. Cardiovasc Res. 2002;55:864–869. doi: 10.1016/s0008-6363(02)00467-4. doi:10.1016/S0008-6363(02)00467-4. [DOI] [PubMed] [Google Scholar]
- 29.Nunes GL, Sgoutas DS, Redden RA, Sigman SR, Gravanis MB, King SB., 3rd Combination of vitamins C and E alters the response to coronary balloon injury in the pig. Arterioscler Thromb Vasc Biol. 1995;15:156–165. doi: 10.1161/01.atv.15.1.156. doi:10.1161/01.ATV.15.1.156. [DOI] [PubMed] [Google Scholar]
- 30.Cote G, Tardif JC, Lesperance J, Lambert J, Bourassa M, Bonan R. Effects of probucol on vascular remodeling after coronary angioplasty. Multivitamins and Protocol Study Group. Circulation. 1999;99:30–35. doi: 10.1161/01.cir.99.1.30. doi:10.1161/01.CIR.99.1.30. [DOI] [PubMed] [Google Scholar]
- 31.Deiner C, Schwimmbeck PL, Koehler IS, Loddenkemper C, Noutsias M, Nikol S. Adventitial VEGF165 gene transfer prevents lumen loss through induction of positive arterial remodeling after PTCA in porcine coronary arteries. Atherosclerosis. 2006;189:123–132. doi: 10.1016/j.atherosclerosis.2005.12.008. doi:10.1016/j.atherosclerosis.2005.12.008. [DOI] [PubMed] [Google Scholar]
- 32.Osherov AB, Gotha L, Cheema AN, Qiang B, Strauss BH. Proteins mediating collagen biosynthesis and accumulation in arterial repair: novel targets for anti-restenosis therapy. Cardiovasc Res. 2011;91:16–26. doi: 10.1093/cvr/cvr012. doi:10.1093/cvr/cvr012. [DOI] [PubMed] [Google Scholar]
- 33.Forte A, Della Corte A, De Feo M, Cerasuolo F, Cipollaro M. Role of myofibroblasts in vascular remodelling: focus on restenosis and aneurysm. Cardiovasc Res. 2010;88:395–405. doi: 10.1093/cvr/cvq224. doi:10.1093/cvr/cvq224. [DOI] [PubMed] [Google Scholar]
- 34.Coen M, Gabbiani G, Bochaton-Piallat ML. Myofibroblast-mediated adventitial remodeling: an underestimated player in arterial pathology. Arterioscler Thromb Vasc Biol. 2011;31:2391–2396. doi: 10.1161/ATVBAHA.111.231548. doi:10.1161/ATVBAHA.111.231548. [DOI] [PubMed] [Google Scholar]
- 35.Sartore S, Chiavegato A, Faggin E, Franch R, Puato M, Ausoni S. Contribution of adventitial fibroblasts to neointima formation and vascular remodeling: from innocent bystander to active participant. Circ Res. 2001;89:1111–1121. doi: 10.1161/hh2401.100844. doi:10.1161/hh2401.100844. [DOI] [PubMed] [Google Scholar]
- 36.Wight TN. Arterial remodeling in vascular disease: a key role for hyaluronan and versican. Front Biosci. 2008;13:4933–4937. doi: 10.2741/3052. doi:10.2741/3052. [DOI] [PubMed] [Google Scholar]
- 37.Lafont A, Durand E, Samuel JL, Besse B, Addad F, Levy BI. Endothelial dysfunction and collagen accumulation: two independent factors for restenosis and constrictive remodeling after experimental angioplasty. Circulation. 1999;100:1109–1115. doi: 10.1161/01.cir.100.10.1109. doi:10.1161/01.CIR.100.10.1109. [DOI] [PubMed] [Google Scholar]
- 38.Strauss BH, Robinson R, Batchelor WB, Chisholm RJ, Ravi G, Natarajan MK. In vivo collagen turnover following experimental balloon angioplasty injury and the role of matrix metalloproteinases. Circ Res. 1996;79:541–550. doi: 10.1161/01.res.79.3.541. doi:10.1161/01.RES.79.3.541. [DOI] [PubMed] [Google Scholar]
- 39.Brasselet C, Durand E, Addad F, Al Haj Zen A, Smeets MB, Laurent-Maquin D. Collagen and elastin cross-linking: a mechanism of constrictive remodeling after arterial injury. Am J Physiol Heart Circ Physiol. 2005;289:H2228–H2233. doi: 10.1152/ajpheart.00410.2005. doi:10.1152/ajpheart.00410.2005. [DOI] [PubMed] [Google Scholar]
- 40.Ward MR, Kanellakis P, Ramsey D, Funder J, Bobik A. Eplerenone suppresses constrictive remodeling and collagen accumulation after angioplasty in porcine coronary arteries. Circulation. 2001;104:467–472. doi: 10.1161/hc3001.091458. doi:10.1161/hc3001.091458. [DOI] [PubMed] [Google Scholar]
- 41.Kobayashi K, Yokote K, Fujimoto M, Yamashita K, Sakamoto A, Kitahara M. Targeted disruption of TGF-beta-Smad3 signaling leads to enhanced neointimal hyperplasia with diminished matrix deposition in response to vascular injury. Circ Res. 2005;96:904–912. doi: 10.1161/01.RES.0000163980.55495.44. doi:10.1161/01.RES.0000163980.55495.44. [DOI] [PubMed] [Google Scholar]
- 42.Galis ZS, Johnson C, Godin D, Magid R, Shipley JM, Senior RM. Targeted disruption of the matrix metalloproteinase-9 gene impairs smooth muscle cell migration and geometrical arterial remodeling. Circ Res. 2002;91:852–859. doi: 10.1161/01.res.0000041036.86977.14. doi:10.1161/01.RES.0000041036.86977.14. [DOI] [PubMed] [Google Scholar]
- 43.Bakker EN, Pistea A, Spaan JA, Rolf T, de Vries CJ, van Rooijen N. Flow-dependent remodeling of small arteries in mice deficient for tissue-type transglutaminase: possible compensation by macrophage-derived factor XIII. Circ Res. 2006;99:86–92. doi: 10.1161/01.RES.0000229657.83816.a7. doi:10.1161/01.RES.0000229657.83816.a7. [DOI] [PubMed] [Google Scholar]
- 44.Chiang HY, Korshunov VA, Serour A, Shi F, Sottile J. Fibronectin is an important regulator of flow-induced vascular remodeling. Arterioscler Thromb Vasc Biol. 2009;29:1074–1079. doi: 10.1161/ATVBAHA.108.181081. doi:10.1161/ATVBAHA.108.181081. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Shi Y, Massague J. Mechanisms of TGF-beta signaling from cell membrane to the nucleus. Cell. 2003;113:685–700. doi: 10.1016/s0092-8674(03)00432-x. doi:10.1016/S0092-8674(03)00432-X. [DOI] [PubMed] [Google Scholar]
- 46.McCaffrey TA. TGF-beta signaling in atherosclerosis and restenosis. Front Biosci (Schol Ed) 2009;1:236–245. doi: 10.2741/s23. [DOI] [PubMed] [Google Scholar]
- 47.Whatling C, McPheat W, Hurt-Camejo E. Matrix management: assigning different roles for MMP-2 and MMP-9 in vascular remodeling. Arterioscler Thromb Vasc Biol. 2004;24:10–11. doi: 10.1161/01.ATV.0000100562.63144.C1. doi:10.1161/01.ATV.0000100562.63144.C1. [DOI] [PubMed] [Google Scholar]
- 48.Galis ZS, Khatri JJ. Matrix metalloproteinases in vascular remodeling and atherogenesis: the good, the bad, and the ugly. Circ Res. 2002;90:251–262. [PubMed] [Google Scholar]
- 49.Mason DP, Kenagy RD, Hasenstab D, Bowen-Pope DF, Seifert RA, Coats S. Matrix metalloproteinase-9 overexpression enhances vascular smooth muscle cell migration and alters remodeling in the injured rat carotid artery. Circ Res. 1999;85:1179–1185. doi: 10.1161/01.res.85.12.1179. doi:10.1161/01.RES.85.12.1179. [DOI] [PubMed] [Google Scholar]
- 50.Ivan E, Khatri JJ, Johnson C, Magid R, Godin D, Nandi S. Expansive arterial remodeling is associated with increased neointimal macrophage foam cell content: the murine model of macrophage-rich carotid artery lesions. Circulation. 2002;105:2686–2691. doi: 10.1161/01.cir.0000016825.17448.11. doi:10.1161/01.CIR.0000016825.17448.11. [DOI] [PubMed] [Google Scholar]
- 51.Epstein H, Grad E, Golomb M, Koroukhov N, Edelman ER, Golomb G. Innate immunity has a dual effect on vascular healing: suppression and aggravation of neointimal formation and remodeling post-endotoxin challenge. Atherosclerosis. 2008;199:41–46. doi: 10.1016/j.atherosclerosis.2007.10.034. doi:10.1016/j.atherosclerosis.2007.10.034. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Langille BL, Dajnowiec D. Cross-linking vasomotor tone and vascular remodeling: a novel function for tissue transglutaminase? Circ Res. 2005;96:9–11. doi: 10.1161/01.RES.0000153883.55971.81. doi:10.1161/01.RES.0000153883.55971.81. [DOI] [PubMed] [Google Scholar]
- 53.Tronc F, Mallat Z, Lehoux S, Wassef M, Esposito B, Tedgui A. Role of matrix metalloproteinases in blood flow-induced arterial enlargement: interaction with NO. Arterioscler Thromb Vasc Biol. 2000;20:E120–E126. doi: 10.1161/01.atv.20.12.e120. doi:10.1161/01.ATV.20.12.e120. [DOI] [PubMed] [Google Scholar]
- 54.Bosmans JM, Vrints CJ, Kockx MM, Bult H, Cromheeke KM, Herman AG. Continuous perivascular L-arginine delivery increases total vessel area and reduces neointimal thickening after experimental balloon dilatation. Arterioscler Thromb Vasc Biol. 1999;19:767–776. doi: 10.1161/01.atv.19.3.767. doi:10.1161/01.ATV.19.3.767. [DOI] [PubMed] [Google Scholar]
- 55.Tronc F, Wassef M, Esposito B, Henrion D, Glagov S, Tedgui A. Role of NO in flow-induced remodeling of the rabbit common carotid artery. Arterioscler Thromb Vasc Biol. 1996;16:1256–1262. doi: 10.1161/01.atv.16.10.1256. doi:10.1161/01.ATV.16.10.1256. [DOI] [PubMed] [Google Scholar]
- 56.Morishita T, Tsutsui M, Shimokawa H, Horiuchi M, Tanimoto A, Suda O. Vasculoprotective roles of neuronal nitric oxide synthase. FASEB J. 2002;16:1994–1996. doi: 10.1096/fj.02-0155fje. [DOI] [PubMed] [Google Scholar]
- 57.Furuno Y, Morishita T, Toyohira Y, Yamada S, Ueno S, Morisada N. Crucial vasculoprotective role of the whole nitric oxide synthase system in vascular lesion formation in mice: involvement of bone marrow-derived cells. Nitric Oxide. 2011;25:350–359. doi: 10.1016/j.niox.2011.06.007. doi:10.1016/j.niox.2011.06.007. [DOI] [PubMed] [Google Scholar]
- 58.Yogo K, Shimokawa H, Funakoshi H, Kandabashi T, Miyata K, Okamoto S. Different vasculoprotective roles of NO synthase isoforms in vascular lesion formation in mice. Arterioscler Thromb Vasc Biol. 2000;20:E96–E100. doi: 10.1161/01.atv.20.11.e96. doi:10.1161/01.ATV.20.11.e96. [DOI] [PubMed] [Google Scholar]
- 59.Rajagopalan S, Meng XP, Ramasamy S, Harrison DG, Galis ZS. Reactive oxygen species produced by macrophage-derived foam cells regulate the activity of vascular matrix metalloproteinases in vitro. Implications for atherosclerotic plaque stability. J Clin Invest. 1996;98:2572–2579. doi: 10.1172/JCI119076. doi:10.1172/JCI119076. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Shi Y, Niculescu R, Wang D, Patel S, Davenpeck KL, Zalewski A. Increased NAD(P)H oxidase and reactive oxygen species in coronary arteries after balloon injury. Arterioscler Thromb Vasc Biol. 2001;21:739–745. doi: 10.1161/01.atv.21.5.739. doi:10.1161/01.ATV.21.5.739. [DOI] [PubMed] [Google Scholar]
- 61.Durand E, Al Haj Zen A, Addad F, Brasselet C, Caligiuri G, Vinchon F. Adenovirus-mediated gene transfer of superoxide dismutase and catalase decreases restenosis after balloon angioplasty. J Vasc Res. 2005;42:255–265. doi: 10.1159/000085658. doi:10.1159/000085658. [DOI] [PubMed] [Google Scholar]
- 62.Farb A, Sangiorgi G, Carter AJ, Walley VM, Edwards WD, Schwartz RS. Pathology of acute and chronic coronary stenting in humans. Circulation. 1999;99:44–52. doi: 10.1161/01.cir.99.1.44. doi:10.1161/01.CIR.99.1.44. [DOI] [PubMed] [Google Scholar]
- 63.Duckers HJ, Boehm M, True AL, Yet SF, San H, Park JL. Heme oxygenase-1 protects against vascular constriction and proliferation. Nat Med. 2001;7:693–698. doi: 10.1038/89068. doi:10.1038/89068. [DOI] [PubMed] [Google Scholar]
- 64.Bilder G, Wentz T, Leadley R, Amin D, Byan L, O'Conner B. Restenosis following angioplasty in the swine coronary artery is inhibited by an orally active PDGF-receptor tyrosine kinase inhibitor, RPR101511A. Circulation. 1999;99:3292–3299. doi: 10.1161/01.cir.99.25.3292. doi:10.1161/01.CIR.99.25.3292. [DOI] [PubMed] [Google Scholar]
- 65.Fishbein I, Waltenberger J, Banai S, Rabinovich L, Chorny M, Levitzki A. Local delivery of platelet-derived growth factor receptor-specific tyrphostin inhibits neointimal formation in rats. Arterioscler Thromb Vasc Biol. 2000;20:667–676. doi: 10.1161/01.atv.20.3.667. doi:10.1161/01.ATV.20.3.667. [DOI] [PubMed] [Google Scholar]
- 66.Jonsson-Rylander AC, Nilsson T, Fritsche-Danielson R, Hammarstrom A, Behrendt M, Andersson JO. Role of ADAMTS-1 in atherosclerosis: remodeling of carotid artery, immunohistochemistry, and proteolysis of versican. Arterioscler Thromb Vasc Biol. 2005;25:180–185. doi: 10.1161/01.ATV.0000150045.27127.37. [DOI] [PubMed] [Google Scholar]
- 67.Wang L, Zheng J, Bai X, Liu B, Liu CJ, Xu Q. ADAMTS-7 mediates vascular smooth muscle cell migration and neointima formation in balloon-injured rat arteries. Circ Res. 2009;104:688–698. doi: 10.1161/CIRCRESAHA.108.188425. doi:10.1161/CIRCRESAHA.108.188425. [DOI] [PubMed] [Google Scholar]
- 68.Parfyonova Y, Plekhanova O, Solomatina M, Naumov V, Bobik A, Berk B. Contrasting effects of urokinase and tissue-type plasminogen activators on neointima formation and vessel remodelling after arterial injury. J Vasc Res. 2004;41:268–276. doi: 10.1159/000078825. doi:10.1159/000078825. [DOI] [PubMed] [Google Scholar]
- 69.Cittadini A, Monti MG, Castiello MC, D'Arco E, Galasso G, Sorriento D. Insulin-like growth factor-1 protects from vascular stenosis and accelerates re-endothelialization in a rat model of carotid artery injury. J Thromb Haemost. 2009;7:1920–1928. doi: 10.1111/j.1538-7836.2009.03607.x. doi:10.1111/j.1538-7836.2009.03607.x. [DOI] [PubMed] [Google Scholar]