Abstract
The aim of this study was to investigate the attitude of dentists in Kuwait toward the use of nitrous oxide sedation as a behavior management technique (BMT) for pediatric patients and assess their training in nitrous oxide sedation. In addition, we assessed parents' knowledge of and attitude toward the use of nitrous oxide as a BMT for their children. The objective was to determine if nitrous oxide sedation is being provided and utilized as a means to enhance dental care for pediatric patients. A cross-sectional survey was randomly distributed to both groups of interest: parents accompanying their children to the dentist and licensed dentists in Kuwait. Participants had to meet certain inclusion criteria to be included in the survey and had to complete the entire questionnaire to be part of the analysis. A total of 381 parents completed the questionnaires. The majority of parents responded that they were unaware of nitrous oxide sedation and were not aware of it as a BMT (79%). Two thirds of the parent would accept nitrous oxide sedation if recommended by a dentist treating their children. Two hundred and one dentists completed the survey and met the inclusion criteria. The majority (74.5%) of dentists were willing to use nitrous oxide as a BMT. However, only 6% were utilizing nitrous oxide sedation and providing it to their child patient if indicated. The main reasons for this huge gap are lack of facilities/equipment and lack of training as indicated by the dentists. This study showed that parents are accepting nitrous oxide sedation as a BMT for their children. It also showed the willingness of the dentists to provide such BMT to their patients. The lack of training and lack of equipment are the main barriers to providing such service to the patients. More training courses and more facilities should be provided to eliminate such barriers.
Key Words: Nitrous oxide, Kuwait, Minimal sedation
Managing a child's behavior during dental treatment is an important factor in delivering safe and effective dental care. Various nonpharmacological and pharmacological techniques are recommended by the American Academy of Pediatric Dentistry to enable the dental practitioner to perform quality oral health care for the uncooperative pediatric patient, and at the same time alleviate fear and anxiety, guide the child to be cooperative, and nurture a positive dental attitude in him/her.1 In addition to tailoring various behavior management techniques (BMTs) to the individual child, it is also important for dental practitioners to utilize techniques consistent with their level of professional education and clinical experience.2
Nitrous oxide sedation has a long history of safe use in dentistry and offers the clinician predictable clinical outcomes.3 It is considered a preferred technique for the pharmacological management of anxiety in pediatric dental patients in the dental office.4,5
Nitrous oxide sedation has been accepted as a popular pharmacological BMT in many Western countries, including the United States.6,7 In 1996, a survey of the American Academy of Pediatric Dentistry membership revealed that 89% of pediatric dentists utilize nitrous oxide sedation, with most of them using it more than 5 times per week.8 Moreover, this sedation technique is the second most accepted BMT by parents in the United States.9 On the contrary, several studies showed that the majority of parents in Middle East countries did not accept nitrous oxide sedation as a BMT. One study, which was conducted in 2009, demonstrated that most parents in Kuwait prefer nonpharmacological techniques over pharmacological ones, and nitrous oxide sedation was rated as one of the least acceptable techniques.10 Similar findings were found by Al-Shalan and Alammouri for Saudi Arabian and Jordanian parents, respectively.11,12
In 2010, nitrous oxide sedation was officially approved and regulated by the Kuwaiti Dental Board. Prior to that date, dentists were unable to administer nitrous oxide in their dental offices despite training in its use. Many dentists referred patients to have general anesthesia if the patient needed pharmacological anxiety management. Therefore, 3 years after the approval of its use by dentists, the aim was to investigate the attitude of dentists in Kuwait toward the use of nitrous oxide sedation as a BMT for pediatric patients and assess their training in nitrous oxide sedation. In addition, parents' knowledge and attitude toward the use of nitrous oxide as a BMT for their children was also assessed.
METHODS
Parents
After approval by the Health Sciences Center's Ethical Committee, 400 precoded questionnaires were distributed among a random sample of parents who accompanied their children to (a) the Kuwait University Dental Center, (b) pediatric dental clinics at the specialty dental centers (Al-Amiri, Benaid Al-Gar, Al-Farwaniya, Adan, and Al-Jahra), (c) pediatric dental clinics at the general practice dental centers (polyclinics) (Al-Salmiya Al-Garby, Fahad Al-Ahmad, and Al-Nezha), and (d) 4 private clinics advertising for pediatric dental care. Parents were randomly recruited from the waiting room of those dental clinics. Inclusion criteria included parenthood of the accompanying child, literacy for the questionnaire, and minimum age of 21 years.
All parents who agreed to participate received verbal and written information about the nature and purposes of the study. Upon their approval to participate, an informed consent was obtained from each subject. Participants were handed a self-administered questionnaire, and were instructed to answer all questions, which involved the following independent variables: (a) demographic data of the child and the accompanying parent such as age, gender, nationality, government (administrative districts in Kuwait), and child's birth order in the family; (b) parent's educational and income levels; (c) reason for the dental visit and child's usual behavior; and (d) parent's knowledge and attitude toward the use of nitrous oxide as a BMT for their children.
Dentists
A cross-sectional survey of the licensed dentists in the country was approved by the Health Sciences Center's Ethical Committee. Two hundred eighty precoded questionnaires were distributed among a random sample of the 1723 licensed dentists in Kuwait. The dentists were practicing in specialty practices located in the following: (a) Kuwait University Dental Center; (b) specialty dental centers (Al-Amiri, Benaid Al-Gar, Al-Farwaniya, Adan, and Al-Jahra); (c) 5 randomly selected polyclinics, 1 from each of the residential areas in which the specialty centers were located; and (d) 5 randomly selected private dental clinics advertising for pediatric dental care. The inclusion criteria for this group were dentist with a valid dental license, currently residing and practicing in Kuwait, minimum age of 21 years, and treating pediatric patients.
All dentists who agreed to participate received verbal and written information about the nature and purposes of the study. Upon their approval to participate, an informed consent was obtained from each subject. Participants were handed self-administered questionnaires, and were instructed to answer all questions, which involved the following independent variables: (a) demographic data such as age, gender, nationality, and marital status, (b) years of dental practice, specialty, and level of training; (c) training in nitrous oxide sedation; and (d) attitude and knowledge toward the use of nitrous oxide sedation as a BMT for pediatric patients. Data entry, management, analysis, and presentation of results were performed using statistical software, Statistical Package for Social Sciences (SPSS) version 20. A probability value of <.05 was used as the cutoff level for statistical significance. Frequency, percentage, mean ± SD, and range were used to present descriptive statistics. Pearson's chi-square was used to assess the association of different characteristics with parents' or dentists' attitudes.
RESULTS
Parent BMT Survey
A total of 381 parents completed the questionnaire with a response rate of 95.25%; 5 respondents did not complete the questionnaire and were omitted from data analysis. The profile of the parents and their child-patients are summarized in Tables 1 and 2 respectively. Parents' mean age was 35.7 years, ranging between 23 and 65 years. Mothers and fathers accompanied the child-patient in almost equal numbers (male to female ratio = 0.9 : 1). Half of the parents (50.3%) had university education, followed by high school (29.8%); higher education degrees, ie, master, PhD (12%); and less than high school (8%). The mean age of the child-patient was 5.9 years, ranging between 1 and 15 years, with almost equal number of boys and girls (male to female ratio = 0.9 : 1). More than half of the children (68.6%) were seeking dental clinic for restorative treatment. The parents rated their child as usually highly cooperative or cooperative (71.5%) but at the same time usually fearful, anxious, or apprehensive (87.4%) regarding dental treatment.
Table 1. .
Demographics of Parents (N = 376)*

Table 2. .
Demographics of Child-Patient (N = 376)

The majority of parents in this study were neither aware of nitrous oxide sedation (79%) nor aware that it was an option as a BMT (75%). The majority were also unaware of its recent acceptance as a BMT for dental pediatric patients in Kuwait (86%).
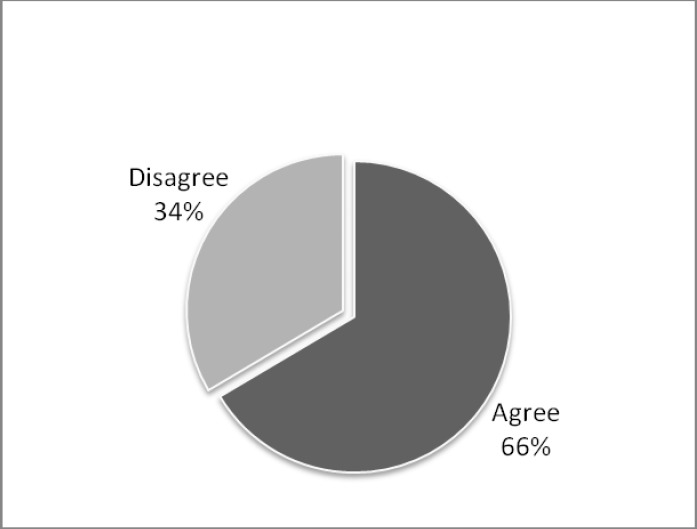
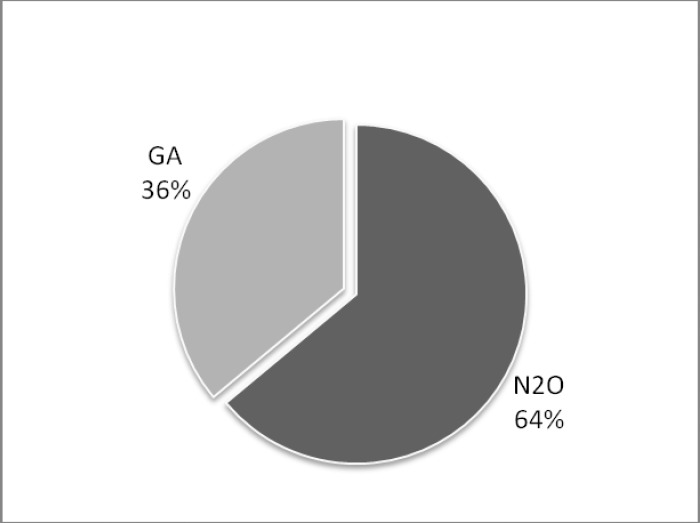
More than half of parents (66%) in our study would accept nitrous oxide sedation as a BMT for their children if it was recommended by the treating dentist (Figure 1). In addition, a similar percentage of them would prefer nitrous oxide over general anesthesia if both were suggested by the treating dentist (Figure 2).
Figure 1. .
Parental acceptance of nitrous oxide (N2O) sedation as a behavioral management technique.
Figure 2. .
Parental preference.
Nineteen pediatric patients (5%) had undergone nitrous oxide sedation with dental treatments during this analysis. Table 3 shows that the majority of parents were satisfied about their child's experience of this sedation technique.
Table 3. .
Parents' Attitude Toward N2O Sedation Experience as a BMT for Their Child-Patient (N = 19)*

Table 4 demonstrates the association of different parental and child characteristics with parents' acceptance of nitrous oxide sedation. A significant declining trend in parental acceptance was noticed with increasing age of parents (P = .001). Parental education also showed a significant association with their acceptance of this sedation technique: the higher their education level, the more accepting parents were toward the use of nitrous oxide sedation for their children (P = .031). Moreover, gender had a significant association, as mothers accepted this BMT slightly more compared to fathers (P = .006). Nationality had no significant effect on acceptance of nitrous oxide as a BMT (P = .085). Furthermore, as income of parents increased, their acceptance of nitrous oxide sedation seemed to increase only slightly, and this was not significant (P = .573). It was also found that parents seeking private-sector dental treatment of their children tended to accept this sedation more than those seeking public-sector treatment; this association was significant (P = .006). No association was found between parents' acceptance and child-patient's age, gender, birth order, usual cooperation, or usual behavior.
Table 4. .
Characteristics of Parents and Child-Patient and Parental Acceptance of N2O Sedation as a BMT

Provider BMT Survey
Of 280 dentists, 238 responded to the study questionnaire (response rate: 85%); of those, 201 respondents met the inclusion criteria. As demonstrated in Table 5, the greatest percentage of respondent dentists in this study were 20 to 29 years old (40.3%), with slightly more male (57.2%) than female dentists (42.8%). Most respondents had been practicing dentistry more than 10 years (38%) and categorized themselves as general dentists (59.2%). Overall, 60.5% of dentists stated that they treated 1 to 5 pediatric patients per week, with 49.5% of respondents reporting seeing 1 to 5 uncooperative pediatric patients per week (Table 5).
Table 5. .
Demographics of Dentists (N = 201)*

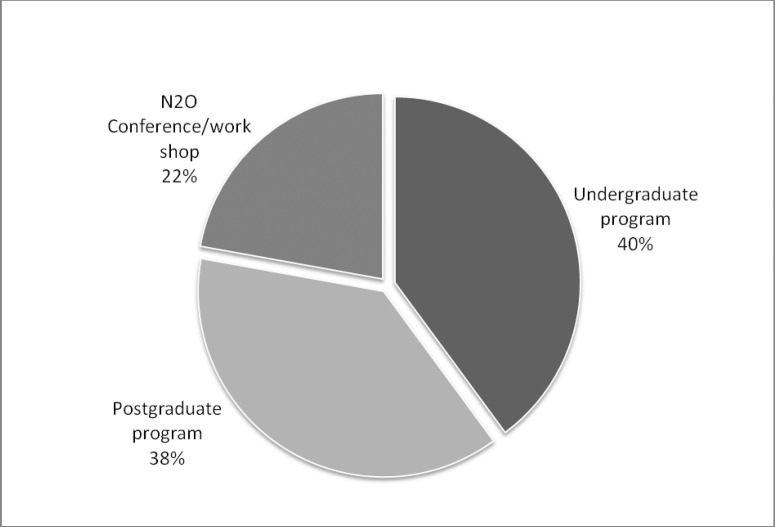
Table 6 assesses the respondent dentists' knowledge and attitude toward nitrous oxide sedation as a BMT. More than half of the dentists in this study were aware of the acceptance of nitrous oxide sedation as a BMT in Kuwait. Despite the fact that 94% of dentists did not use nitrous oxide sedation as a BMT for their pediatric patients, 74.5% were willing to use it. However, dentists who did not have appropriate training for the use of nitrous oxide (64.2%) significantly outnumbered dentists who did (35.8%). Figure 3 demonstrates the types of training respondents received. Although only 23.9% of dentists were aware of regulations about nitrous oxide sedation usage for pediatric patients in Kuwait, over half (55.2%) were aware of regulations about its usage internationally. When dentists were asked about the main reasons for lack of nitrous oxide use in Kuwait, the majority of respondents answered lack of facilities/equipment and lack of training/knowledge. Moreover, the majority of dentists in this study (73.1%) thought that parents were not aware of nitrous oxide sedation as a BMT for their children.
Table 6. .
Dentists' Knowledge and Attitude Toward N2O Sedation as a BMT (N = 201)*

Figure 3. .
Types of nitrous oxide (N2O) training.
When cross-tabulation was done (Table 7), female dentists seemed to be significantly more willing to use nitrous oxide sedation than males (P = .001). In addition, the willingness of the dentists to use nitrous oxide sedation increased with higher numbers of uncooperative patients being treated (P = .00001). Moreover, the dentists who had been trained to use nitrous oxide sedation were more willing to utilize it (P = .00001). Furthermore, the surveyed dentists in different specialties were more willing to utilize nitrous oxide sedation, except in orthodontics, where none showed willingness (P = .00001).
Table 7. .
Characteristics of Dentists and Their Willingness to Use N2O as a BMT

There was no significance with regards to dentists' age, nationality, years of dental practice, main practice setting, or treated pediatric patient nationality toward the willingness to use nitrous oxide sedation. Dentists who worked in Hawalli showed a trend to be more willing to use nitrous oxide sedation than those in other governments (P = .059).
DISCUSSION
This study showed that the majority of parents in Kuwait are unaware of nitrous oxide sedation as a BMT or the recent approval and regulation of the agent in dental practice. When this BMT is recommended by the treating dentist, more than half of parents would accept its usage for their children. Younger parents and increasing education level were the main factors associated with improved acceptance rates. Almost all parents in our study who reported that their child had had nitrous oxide sedation before were pleased with their child's experience. Thus, dentists treating pediatric patients should be encouraged to educate and inform parents of nitrous oxide as a BMT and offer it as a service to pediatric patients whenever it is suitable and indicated. This study also demonstrated that parental acceptance of nitrous oxide sedation is higher compared to previous studies conducted in Middle East countries including Kuwait.10–12 This might be due to differences in the method by which these studies were conducted and the sample size used in each study.
Although nitrous oxide sedation has become a routine BMT for pediatric patients in contemporary American dental practice,8 only 12 out of 201 (6%) surveyed dentists in Kuwait utilize it. Nitrous oxide is not commonly used in Kuwait because of a shortage of facilities/equipment and lack of dentist training/knowledge.13 Concerning nitrous oxide sedation safety, the majority of dentists agreed on its safety, which is consistent with previously published reports.14,15 An analysis completed by Hulland et al16 revealed that on the basis of a 10-year retrospective study, the utilization of nitrous oxide–oxygen sedation as a single agent provides effective and safe conscious sedation for pediatric patients. Possible reasons for its effectiveness are that nitrous oxide sedation calms agitated pediatric patients, suppresses their anxiety, and decreases unpleasant dental care memories.16 In addition, the dentist can work more quickly and in a more focused manner, diminishing the chance of mechanical error and improving the quality of dental care; consequently, there are fewer dental appointments and fewer missed school days for the child.15
Dental providers in Kuwait have used general anesthesia as their main means of pharmacologic behavior management for the administration of dental procedures.13,17 This process requires a hospital operating theater, bears substantial cost on the Kuwaiti health care system, and can act as a barrier to care because of limited access for appointment times. The need for sedation services for dental care in Kuwait was demonstrated by a recent study that found a significant portion of the population, 60%, preferred a method in which anxiety and fear can be reduced for dental appointments.13 Given that nitrous oxide has the highest safety margin of any anxiolysis or sedation modality in dentistry and has a long history of efficacy, the use of this modality by Kuwaiti dental providers may improve access to care and the patient experience.18
CONCLUSION
This study demonstrated that most parents in Kuwait are unaware of nitrous oxide sedation as a BMT, but more than half of them accept its usage for their children upon their dentist's advice and recommendation. In addition, it showed that the vast majority of dentists treating pediatric patients in Kuwait are willing to use nitrous oxide sedation as a BMT, but more than half of them lack the training and equipment. This indicates that there is a need to provide nitrous oxide sedation as a BMT for pediatric patients and that the lack of training and equipment are barriers. Therefore, training courses on the use of nitrous oxide sedation should be offered to the dental community and the needed equipment should be provided in the clinics.
REFERENCES
- 1.American Academy of Pediatric Dentistry (AAPD) Guideline on Behavior Guidance for the Pediatric Dental Patient. Chicago, Ill: American Academy of Pediatric Dentistry (AAPD); 2011. [Google Scholar]
- 2.American Dental Association (ADA) Guidelines for the Use of Sedation and General Anesthesia by Dentists. Chicago, Ill: American Dental Association (ADA); 2012. [Google Scholar]
- 3.American Academy of Pediatric Dentistry (AAPD) Guideline on Use of Nitrous Oxide for Pediatric Dental Patients. Chicago, Ill: American Academy of Pediatric Dentistry (AAPD); 2013. [Google Scholar]
- 4.Hosey MT. UK National Clinical Guidelines in Paediatric Dentistry. Managing anxious children: the use of conscious sedation in paediatric dentistry. Int J Paed Dent. 2002;12:359–372. doi: 10.1046/j.1365-263x.2002.03792.x. [DOI] [PubMed] [Google Scholar]
- 5.Council of European Dentists. The Use of Nitrous Oxide Inhalation Sedation in Dentistry. Bruxelles, Belgium: Council of European Dentists; 2012. [Google Scholar]
- 6.Hallonsten A-L, Jensen B, Raadal M, Veerkamp J, Hosey MT, Poulsen S. European Academy of Paediatric Dentistry: Guidelines on Sedation in Paediatric Dentistry. Athens, Greece: European Academy of Paediatric Dentistry; 2005. [Google Scholar]
- 7.Levering N, Welie J. Current status of nitrous oxide sedation as a behavior management practice routine in pediatric dentistry. J Dent Child. 2011;78:24–30. [PubMed] [Google Scholar]
- 8.Wilson S. A survey of the American Academy of Pediatric Dentistry membership: nitrous oxide and sedation. Pediatr Dent. 1996;18:87–93. [PubMed] [Google Scholar]
- 9.Scott M, Srephen W, William F. Parental attitudes toward behavior management techniques used in pediatric dentistry. Pediatr Dent. 1991;13:151–155. [PubMed] [Google Scholar]
- 10.Muhammad S, Shyama M, Al-Mutawa SA. Parental attitude toward behavioral management techniques in dental practice with schoolchildren in Kuwait. Med Princ Pract. 2011;20:350–355. doi: 10.1159/000323758. [DOI] [PubMed] [Google Scholar]
- 11.Al-Shalan TA. Factors affecting Saudi parents' perception of their children's first dental visit. J Contemp Dent Pract. 2003;4:54–66. [PubMed] [Google Scholar]
- 12.Alammouri M. The attitude of parents toward behavior management techniques in pediatric dentistry. J Clin Pediatr Dent. 2006;30:310–313. doi: 10.17796/jcpd.30.4.m73568r0t74962m3. [DOI] [PubMed] [Google Scholar]
- 13.Abdulwahab M, Al-Sayegh F, Boynes SG. Assessing the need for anesthesia and sedation services in Kuwaiti dental practice. Anesth Prog. 2010;57:91–95. doi: 10.2344/0003-3006-57.3.91. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Levering N, Welie J. Ethical considerations in the use of nitrous oxide in pediatric dentistry. Am Soc Dent Ethics. 2010;77:40–47. [PubMed] [Google Scholar]
- 15.Primosch R, Buzzi I, Jerrell G. Effect of nitrous oxide-oxygen inhalation with scavenging on behavioral and physiological parameters during routine pediatric dental treatment. Pediatr Dent. 1999;21:417–420. [PubMed] [Google Scholar]
- 16.Hulland S, Freilich M, Sàndor G. Nitrous oxide–oxygen or oral midazolam for pediatric outpatient sedation. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2002;93:643–646. doi: 10.1067/moe.2002.124763. [DOI] [PubMed] [Google Scholar]
- 17.Ibricevic H, Al-Jame Q, Honkala S. Pediatric dental procedures under general anesthesia at the Amiri Hospital in Kuwait. J Clin Pediatr Dent. 2001;25:337–342. doi: 10.17796/jcpd.25.4.fl062x558qtt4v69. [DOI] [PubMed] [Google Scholar]
- 18.Boynes SG, Lewis CL, Moore PA, Zovko J, Close J. Complications associated with anesthesia administered for dental treatment. Gen Dent. 2010;58:e20–e25. [PubMed] [Google Scholar]