Abstract
Study Objective
To determine the association between Anticholinergic Cognitive Burden (ACB) score and both cognitive impairment and health care utilization among a diverse ambulatory older adult population.
Design
Retrospective cohort study.
Data Source
Medication exposure and other clinical data were extracted from the Regenstrief Medical Record System (RMRS), and cognitive diagnosis was derived from a dementia screening and diagnosis study.
Patients
A total of 3344 community-dwelling older adults (age 65 yrs and older) who were enrolled in a previously published dementia screening and diagnosis study; of these, 3127 were determined to have no cognitive impairment, and 217 were determined to have cognitive impairment.
Measurements and Main Results
The study followed a two-phase screening and comprehensive neuropsychiatric examination to determine a cognitive diagnosis, which defined cognitive impairment as dementia or mild cognitive impairment. The ACB scale was used to identify anticholinergics dispensed in the 12 months prior to screening. A total daily ACB score was calculated by using pharmacy dispensing data from RMRS; each anticholinergic was multiplied by 1, 2, or 3 consistent with anticholinergic burden defined by the ACB scale. The sum of all ACB medications was divided by the number of days with any medication dispensed to achieve the total daily ACB score. Health care utilization included visits to inpatient, outpatient, and the emergency department, and it was determined by using visit data from the RMRS. The overall population had a mean age of 71.5 years, 71% were female, and 58% were African American. Each 1-point increase in mean total daily ACB score was associated with increasing risk of cognitive impairment (odds ratio [OR] 1.13, 95% confidence interval [CI] 1.004–1.27, p=0.043). Each 1-point increase in mean total daily ACB score increased the likelihood of inpatient admission (OR 1.11, 95% CI 1.02–1.29, p=0.014) and number of outpatient visits after adjusting for demographic characteristics, number of chronic conditions, and prior visit history (estimate 0.382, standard error [SE] 0.113; p=0.001). The number of visits to the emergency department was also significantly different after similar adjustments (estimate 0.046, SE 0.023, p=0.043).
Conclusion
Increasing total ACB score was correlated with an increased risk for cognitive impairment and more frequent health care utilization. Future work should study interventions that safely reduce ACB and evaluate the impact on brain health and health care costs.
Keywords: anticholinergic, cognitive impairment, health care utilization
Older adults are often prescribed a high number of medications to manage multiple acute and chronic medical comorbidities, with population estimates ranging from five to nine prescription medications each day.1, 2 Some of these medications may be prescribed for their clinical anticholinergic effects, whereas others have unintended anticholinergic properties not related to its mechanism of action (e.g., paroxetine) or have anticholinergic properties identified through in vitro data.3 More than 50% of ambulatory older adults use at least one medication with anticholinergic effects that is prescribed for a variety of complaints including mood, pain, incontinence, allergies, anxiety, and insomnia.4, 5 A 2013 study conducted in American women older than 75 years suggests that exposure to anticholinergic agents is increasing over time.6
Medications with anticholinergic properties have been associated with adverse cognitive effects in a number of observational studies.5, 7–9 We previously developed the Anticholinergic Cognitive Burden (ACB) scale and showed that users of anticholinergics identified by the scale were associated with an increased risk of cognitive impairment.5, 7 However, the ACB scale has not been used to calculate a cumulative score using prescription dispensing or claims databases. We hypothesized that the adverse cognitive effects of anticholinergic medications not only increase the risk of cognitive impairment but also increase health care utilization that may represent a decline in the ability to self-manage comorbid disease.
Pharmacy databases have been used previously to evaluate relationships between certain anticholinergic and sedative medications and hospital admissions. Existing literature is limited by the inclusion of a select number of anticholinergic medications8, 10, 11 or has limited generalizability to U.S. populations due to methodologic or demographic differences.12–14 Specifically, populations with low socioeconomic status are poorly represented in prior work and are at higher risk for dementia.15, 16 Therefore, the objective of this study was to determine the relationship between the mean total daily ACB score and both cognitive impairment and health care utilization among a diverse ambulatory older adult population.
Methods
Study Design, Setting, and Patient Population
In this retrospective cohort study, the patients were enrolled in a dementia screening and diagnosis study conducted between 2001 and 2004 within Eskenazi Health (formerly known as Wishard Health; Indianapolis, IN).17 Eskenazi Health is among the five largest safety-net health care systems in the United States and is responsible for the care of indigent, uninsured, or underinsured people in Indianapolis. Eskenazi Health provides care through a centrally located hospital and eight affiliated primary care clinics within the city of Indianapolis.
As mentioned earlier, the patients available for this analysis were selected from a dementia screening study conducted in Indianapolis, Indiana.17 Inclusion criteria for this analysis were age 65 years and older at time of enrollment (2001–2004), at least one visit to a primary care provider in the year prior to enrollment, at least one dispensed prescription medication in the year prior to enrollment, and at least one inpatient, outpatient, or emergency department visit recorded in the 12 months following enrollment. Patients were excluded if dispensing or visit data were not available from their electronic medical records.
Comorbidity and Other Variables
Regenstrief Institute previously developed identification terms derived from International Classification of Diseases, Ninth Revision codes from the Regenstrief Medical Record System (RMRS) to identify common comorbid conditions among older adults. For this study, we reported the following nine conditions that have been identified as common comorbidities in community-dwelling older adults: congestive heart failure, coronary artery disease, stroke, arthritis, diabetes mellitus, liver failure, kidney failure, chronic obstructive pulmonary disease, and cancer.18, 19 Hypertension has also been recognized as a common chronic condition in this previous work; however, we did not include it in the models because 98% of the population was identified as having the disease. Demographic characteristics including sex, age, and race were also available from the RMRS. Lastly, visit data and dates of visits were categorized as inpatient, emergency department (ED), and out-patient (primary care and specialty care) visits.
Cognitive Assessment
The cognitive screening took place in two phases, with the first phase occurring on the index date of this analysis. The first phase of cognitive screening included the 6-point screening instrument that consists of four questions: three items assessed temporal orientation and one item assessed recall. Patients who made one or more mistakes were asked to complete the second stage of screening. In prior work in a community-based population, this instrument had a sensitivity of 97.7% and a specificity of 49.2% for a diagnosis of dementia.20 Those who made no errors on this instrument were excluded from further evaluation and considered to have no cognitive impairment. The second stage of screening included the Community Screening Interview for Dementia (CSI-D) that evaluates cognitive function across multiple domains with no requirement for reading ability. The CSI-D includes 28 items with a score ranging from 0–34; a cut-off score of 24 or lower has a sensitivity of 87% and a specificity of 83.1% for a diagnosis of dementia.21, 22 The CSI-D was designed for populations with low educational attainment to avoid educational bias. Patients who made at least one error on the six-item screener and subsequently scored 24 points or less on the CSI-D were considered to screen positive for cognitive impairment.
Patients who screened positive in phase 1 were invited to a comprehensive diagnostic assessment (phase 2) that included a neuropsychological evaluation using the Consortium to Establish a Registry for Alzheimer’s Disease neuropsychological battery; and a semistructured interview with an informant. In addition, RMRS records were reviewed for the presence of all comorbid medical conditions, current medications, relevant laboratory data, and brain imaging. Data from all components of the assessment just described were reviewed by a consensus diagnosis panel including a psychologist, neuropsychologist, geriatrician, and geriatric psychiatrist. The team used standardized criteria to diagnose mild cognitive impairment, dementia, Alzheimer disease, and vascular dementia.23
For this analysis, cognitive impairment included the diagnosis of mild cognitive impairment or dementia. Those who screened positive in phase 1 but were diagnosed as cognitively normal in phase 2 were considered normal. Those who screened positive in phase 1 but did not undergo diagnostic assessment (phase 2) were excluded from the analysis because we could not determine their cognitive status.
Exposure Measurement
Dispensing data captured from the RMRS were used as the source of exposure measurement. The RMRS captures clinical data from the entire Eskenazi Health Network including inpatient and outpatient registration records (demographics), medication and treatment orders, and laboratory, imaging, and encounter data. Most important for this study, RMRS captures pharmacy dispensing data from eight outpatient pharmacies within the network. Pharmacy data include medication name, dosage, quantity, days supplied, and dates of dispensing for each medication. Although patients in the network are not limited to using these pharmacies, benefits of low-income subsidy programs reduce costs for medications dispensed from network pharmacies.
Regenstrief Institute and its research partners previously developed the ACB scale to determine the anticholinergic activity of medications in pharmacoepidemiologic analyses.3, 7 An interdisciplinary team categorized medications as mild (ACB score 1), moderate (ACB score 2), or severe (ACB score 3) anticholinergics based on the literature and clinical expertise. The ACB medications in this analysis do not include topical or inhaled products. We calculated cumulative exposure to anticholinergics using a total daily ACB score for each patient. The example here provides a sample calculation for a patient taking anticholinergic drugs “A,” “B,” and so on (X) to calculate the total daily ACB score as follows:
The number of days supplied during the exposure period was used to quantify duration of exposure for each anticholinergic drug recognized in the ACB scale. We chose the number of days from first prescription date to the index date (date of cognitive screening) as the denominator because patients may not have been active in the network or used prescription medications for the full 365 days of the exposure window. Overall 77% of the population had 365 days with active prescription activity. For this analysis, mean total daily values of 0–0.49 were categorized as ACB score of 0, values of 0.50–1.49 were categorized as ACB score of 1, values of 1.50–2.49 were categorized as ACB score of 2, and so on.
Statistical Analysis
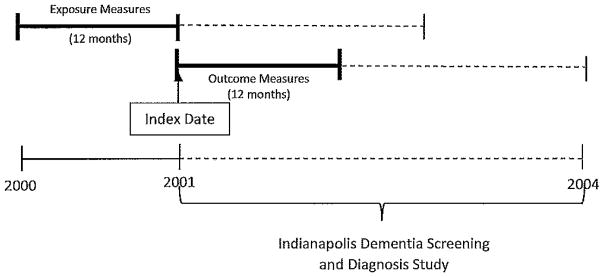
Figure 1 describes the approach to measuring exposure and outcome variables in this study. Exposure to anticholinergics and other medications was captured in the 12 months prior to enrollment in the screening study, and outcome measures of cognitive screening and health care utilization were measured at index date (date of cognitive screening) and during the 12 months following enrollment (health care utilization).
Figure 1.
Description of the study design. Exposure to anticholinergics and other medications was captured in the 12 months prior to enrollment in the screening study, and outcome measures of cognitive screening and health care utilization were measured at the index date (cognitive screening) and during the 12 months following enrollment (health care utilization).
Means and standard deviations (SDs) are reported for numerical data, and proportions are reported for categorical data, with the differences between groups evaluated by t tests and χ2 tests, respectively. Comparisons of mean total daily ACB score, number of ED visits, and number of outpatient visits by categorical variables were evaluated by using the Wilcoxon rank sum test due to the skewness of these variables. We used logistic regression to evaluate the relationship of cognitive impairment with mean total daily ACB score while adjusting for age, sex, race, and number of chronic conditions. Two different sets of models were used to evaluate the relationship between health care utilization and ACB exposure adjusting for age, sex, race, and number of chronic conditions. The number of inpatient admissions was recoded to a binary outcome due to the small number of patients having an admission (18%) and an even smaller number having multiple admissions (6%). Therefore, we used logistic regression to evaluate the relationship between ACB exposure and any inpatient admission. We used linear regression models for the ED visits and outpatient visits because these two health care utilization measures were continuous and not recoded to a binary outcome. In addition, we performed sensitivity analyses for the ED visit and outpatient visit models. Due to skewness, we used Poisson regression models and linear regression models using log(visits+1). Results were similar for all models; therefore, we reported the linear regression results with crude visit rates as the dependent variables. Because similar studies have not consistently adjusted for prior health care utilization when evaluating health care utilization as an outcome, we presented models with and without adjustments for prior utilization for ED and outpatient visits to compare our results with these studies. All models were also adjusted for age, sex, race, and number of chronic conditions.
Results
The population included 3344 older adults with medication dispensing and visit data available for this analysis. The population had a mean age of 71 years, 71% were female, and 58% were African American. A total of 38% of the population had a mean total daily ACB score of 0; 33% had a mean total daily ACB score of 1; 16% had a mean total daily ACB score of 2; 8% had a mean total daily ACB score of 3, and 6% had a mean total daily ACB score of 4 or more. Table 1 presents the demographic and clinical characteristics for the overall cohort as well as those with and without cognitive impairment. In addition to differences in demographic characteristics by cognitive status, differences in mean total daily ACB score were evident in this population. Women had a significantly higher mean total daily ACB score than men (mean ± SD for women 1.2 ± 1.3 and men 0.9 ± 1.1; Wilcoxon rank sum p<0.001). African Americans had significantly lower mean total daily ACB scores than whites and other races (mean ± SD for whites 1.4 ± 1.4, African Americans 0.9 ± 1.1, and other races 1.3 ± 1.5; Wilcoxon rank sum p<0.001).
Table 1.
Comparison of Demographic and Clinical Characteristics and Anticholinergic Cognitive Burden Score in the Two Study Cohorts
| Variable | Entire cohort (n=3344) | No cognitive impairment cohort (n=3127) | Cognitive impairment cohort (n=217) | p value |
|---|---|---|---|---|
| Age, yrs | 71.5 ± 5.7 | 71.3 ± 5.7 | 74.9 ± 6.6 | < 0.001 |
| Female | 2373 (71.0) | 2232 (71.4) | 141 (65.0) | 0.047 |
| White | 1322 (39.5) | 1256 (40.2) | 66 (30.4) | 0.005 |
| African American | 1932 (57.8) | 1787 (57.2) | 145 (66.8) | 0.006 |
| No. of chronic disease conditions | 2.7 ± 1.7 | 2.6 ± 1.7 | 2.9 ± 1.6 | 0.011 |
| Arthritis | 795 (23.8) | 739 (23.6) | 56 (25.8) | 0.467 |
| Cancer | 835 (25.0) | 786 (25.1) | 49 (22.6) | 0.400 |
| CAD | 1250 (37.4) | 1165 (37.3) | 85 (39.2) | 0.573 |
| CHF | 1192 (35.6) | 1110 (35.5) | 82 (37.8) | 0.496 |
| COPD | 1133 (33.9) | 1061 (33.9) | 72 (33.2) | 0.821 |
| Diabetes mellitus | 2013 (60.2) | 1878 (60.1) | 135 (62.2) | 0.531 |
| Liver disease | 141 (4.2) | 132 (4.2) | 9 (4.2) | 0.958 |
| Renal disease | 570 (17.0) | 521 (16.7) | 49 (22.6) | 0.025 |
| Stroke | 978 (29.2) | 878 (28.1) | 100 (46.1) | < 0.001 |
| No. of non-anticholinergic drugs in prior year | 7.9 ± 5.3 | 7.9 ± 5.3 | 7.6 ± 4.3 | 0.852 |
| No. of inpatient stays in prior year | 0.2 ± 0.6 | 0.2 ± 0.6 | 0.2 ± 0.6 | 0.352 |
| No. of ED visits in prior year | 0.9 ± 1.6 | 0.9 ± 1.5 | 1.1 ± 1.8 | 0.163 |
| No. of outpatient visits in prior year | 8.7 ± 8.0 | 8.7 ± 8.1 | 8.0 ± 6.3 | 0.857 |
| Inpatient stay | 589 (17.6) | 544 (17.4) | 44 (20.3) | 0.276 |
| No. of ED visits | 0.9 ± 1.7 | 0.9 ± 1.7 | 1.2 ± 1.7 | 0.012 |
| No. of outpatient visits | 9.5 ± 8.5 | 9.6 ± 8.6 | 9.0 ± 7.3 | 0.955 |
| Total daily ACB score | 1.1 ± 1.3 | 1.1 ± 1.3 | 1.3 ± 1.3 | 0.122 |
ACB = Anticholinergic Cognitive Burden; CAD = coronary artery disease; CHF = congestive heart failure; COPD = chronic obstructive pulmonary disease; ED = emergency department.
Data are mean ± SD values or no. (%) of patients.
Table 2 shows that, after adjusting for demographic variables and number of chronic diseases, each 1-point increase in the mean total daily ACB score was associated with an increased risk of cognitive impairment by 13% (odds ratio [OR] 1.13, 95% confidence interval [CI] 1.004–1.27, p=0.043). Age was also associated with an increased risk of cognitive impairment, and female sex was protective against cognitive impairment. As shown in Table 3, the likelihood of any inpatient admission was associated with a 1-point increase in the mean total daily ACB score (OR 1.11, 95% CI 1.02–1.29, p=0.014) even after adjusting for prior health care utilization. Age, number of chronic conditions, and prior visit history were also correlated with higher risk of any inpatient admission.
Table 2.
Relationship Between Anticholinergic Cognitive Burden Total Score and Cognitive Impairment Adjusted for Demographic and Clinical Characteristics
| Variable | Unadjusted for prior health care utilization | Adjusted for prior health care utilization | ||
|---|---|---|---|---|
|
|
|
|||
| OR (95% CI) | p value | OR (95% CI) | p value | |
| Age | 1.09 (1.07–1.12) | < 0.001 | 1.09 (1.07–1.12) | < 0.001 |
| Female | 0.61 (0.45–0.83) | 0.002 | 0.64 (0.47–0.88) | 0.005 |
| White | 0.80 (0.33–1.94) | 0.627 | 0.83 (0.34–2.00) | 0.679 |
| African American | 1.09 (0.46–2.58) | 0.843 | 1.12 (0.47–2.66) | 0.800 |
| Arthritis | 1.05 (0.75–1.46) | 0.783 | 1.10 (0.79–1.53) | 0.586 |
| Cancer | 0.78 (0.56–1.09) | 0.148 | 0.81 (0.58–1.14) | 0.222 |
| CAD | 0.98 (0.72–1.35) | 0.918 | 1.03 (0.75–1.42) | 0.846 |
| CHF | 0.79 (0.57–1.10) | 0.159 | 0.81 (0.58–1.13) | 0.221 |
| COPD | 1.00 (0.73–1.37) | 0.985 | 1.02 (0.74–1.41) | 0.885 |
| Diabetes mellitus | 1.03 (0.76–1.39) | 0.857 | 1.07 (0.79–1.45) | 0.657 |
| Liver disease | 1.06 (0.52–2.15) | 0.880 | 1.07 (0.53–2.18) | 0.854 |
| Renal disease | 1.13 (0.79–1.61) | 0.496 | 1.15 (0.81–1.64) | 0.440 |
| Stroke | 2.00 (1.50–2.67) | < 0.001 | 2.04 (1.52–2.74) | < 0.001 |
| No. of non-anticholinergic drugs | – | – | 0.99 (0.95–1.02) | 0.408 |
| Prior inpatient admissions | – | – | 1.06 (0.80–1.40) | 0.687 |
| Prior ED visits | – | – | 1.07 (0.98–1.16) | 0.160 |
| Prior outpatient visits | – | – | 0.98 (0.95–1.00) | 0.049 |
| Mean total daily ACB scorea | 1.13 (1.004–1.27) | 0.043 | 1.16 (1.03–1.31) | 0.014 |
ACB = Anticholinergic Cognitive Burden; CAD = coronary artery disease; CI = confidence interval; CHF = congestive heart failure; COPD = chronic obstructive pulmonary disease; ED = emergency department; OR = odds ratio.
OR reflects increase in odds of cognitive impairment for every 1-point increase in total daily ACB score.
Table 3.
Relationship Between Anticholinergic Cognitive Burden Total Score and Any Inpatient Admission Adjusted for Demographic and Clinical Characteristics
| Variable | Unadjusted for prior health care utilization | Adjusted for prior health care utilization | ||
|---|---|---|---|---|
|
|
|
|||
| OR (95% CI) | p value | OR (95% CI) | p value | |
| Age | 1.02 (0.99–1.03) | 0.067 | 1.02 (1.003–1.04) | 0.022 |
| Female | 0.99 (0.80–1.22) | 0.925 | 1.01 (0.81–1.26) | 0.923 |
| White | 1.04 (0.56–1.93) | 0.907 | 1.12 (0.59–2.12) | 0.738 |
| African American | 1.07 (0.58–1.98) | 0.835 | 1.13 (0.60–2.12) | 0.709 |
| Arthritis | 1.11 (0.89–1.38) | 0.363 | 1.06 (0.85–1.33) | 0.611 |
| Cancer | 1.53 (1.25–1.88) | < 0.001 | 1.50 (1.22–1.85) | < 0.001 |
| CAD | 1.18 (0.96–1.45) | 0.120 | 1.12 (0.91–1.39) | 0.282 |
| CHF | 1.82 (1.48–2.24) | < 0.001 | 1.69 (1.36–2.09) | < 0.001 |
| COPD | 1.83 (1.50–2.23) | < 0.001 | 1.67 (1.36–2.05) | < 0.001 |
| Diabetes mellitus | 1.58 (1.28–1.96) | < 0.001 | 1.47 (1.18–1.82) | 0.001 |
| Liver disease | 1.60 (1.07–2.41) | 0.023 | 1.50 (0.99–2.28) | 0.059 |
| Renal disease | 1.45 (1.15–1.82) | 0.002 | 1.38 (1.09–1.75) | 0.008 |
| Stroke | 1.80 (1.48–2.18) | < 0.001 | 1.55 (1.27–1.90) | < 0.001 |
| No. of non-anticholinergic drugs | – | – | 0.99 (0.97–1.01) | 0.499 |
| Prior inpatient admissions | – | – | 1.39 (1.18–1.64) | < 0.001 |
| Prior ED visits | – | – | 1.18 (1.10–1.26) | < 0.001 |
| Prior outpatient visits | – | – | 1.01 (0.99–1.03) | 0.065 |
| Mean total daily ACB score | 1.13 (1.05–1.22) | 0.001 | 1.11 (1.02–1.29) | 0.014 |
ACB = Anticholinergic Cognitive Burden; CAD = coronary artery disease; CHF = congestive heart failure; CI = confidence interval; COPD = chronic obstructive pulmonary disease; ED = emergency department; OR = odds ratio.
The number of visits to the ED was associated with increasing mean total daily ACB score (parameter estimate 0.046, standard error [SE] 0.023, p=0.043) after adjusting for demographic characteristics, number of chronic conditions, and prior visit history (Table 4). The number of outpatient visits was also higher with each 1-point increase in mean total daily ACB score (parameter estimate 0.382, SE 0.113, p=0.001) after similar adjustments. All utilization models (inpatient, ED, and outpatient visits) were repeated with cognitive diagnosis included as a binary variable; cognitive impairment was not associated with utilization in any of these models and was therefore not included in the final tables presented.
Table 4.
Relationship Between Anticholinergic Cognitive Burden Total Score and Number of Emergency Department Visits Adjusted for Demographic and Clinical Characteristics
| Variable | Unadjusted for prior health care utilization | Adjusted for prior health care utilization | ||
|---|---|---|---|---|
|
|
|
|||
| Estimate (SE) | p value | Estimate (SE) | p value | |
| Age | −0.004 (0.005) | 0.385 | −0.001 (0.005) | 0.827 |
| Female | 0.028 (0.063) | 0.652 | 0.020 (0.059) | 0.731 |
| White | 0.042 (0.176) | 0.812 | 0.135 (0.162) | 0.405 |
| African American | 0.248 (0.175) | 0.157 | 0.277 (0.161) | 0.085 |
| Arthritis | 0.281 (0.067) | < 0.001 | 0.177 (0.062) | 0.004 |
| Cancer | 0.119 (0.065) | 0.069 | 0.047 (0.060) | 0.440 |
| CAD | 0.261 (0.063) | < 0.001 | 0.169 (0.059) | 0.004 |
| CHF | 0.295 (0.066) | < 0.001 | 0.196 (0.061) | 0.001 |
| COPD | 0.397 (0.062) | < 0.001 | 0.236 (0.058) | < 0.001 |
| Diabetes mellitus | 0.263 (0.060) | < 0.001 | 0.169 (0.059) | 0.002 |
| Liver disease | 0.462 (0.140) | 0.001 | 0.326 (0.129) | 0.011 |
| Renal disease | 0.167 (0.077) | 0.031 | 0.134 (0.071) | 0.060 |
| Stroke | 0.329 (0.063) | < 0.001 | 0.162 (0.059) | 0.006 |
| No. of non-anticholinergic drugs | – | – | 0.019 (0.006) | 0.003 |
| Prior inpatient admissions | – | – | −0.082 (0.053) | 0.125 |
| Prior ED visits | – | – | 0.417 (0.019) | < 0.001 |
| Prior outpatient visits | – | – | 0.0004 (0.004) | 0.916 |
| Mean total daily ACB score | 0.094 (0.024) | < 0.001 | 0.046 (0.023) | 0.043 |
ACB = Anticholinergic Cognitive Burden; CAD = coronary artery disease; CHF = congestive heart failure; COPD = chronic obstructive pulmonary disease; ED = emergency department; SE = standard error.
Discussion
Our results suggest that increasing mean total daily ACB score is associated with higher odds of cognitive impairment and inpatient, ED, and outpatient visits. With average costs for outpatient visits, ED visits, and hospital admissions at $209, $1355, and $13,442, respectively (in 2014 dollars),24–27 additional costs due to ACB exposure are important considerations from the societal and insurer perspectives.
Our results resemble those of a number of recent studies that show a relationship between anticholinergic exposure and health care utilization.10–13, 28 In a design similar to that of our study, one report used the mean total daily ACB score (as well as other anticholinergic scales) to find an OR of 1.231 (95% CI 1.209–1.253) for hospital admissions and 1.055 (95% CI 1.052–1.057) for general practitioner visits among older adults in New Zealand.12 This population differed from our population by having a lower mean ± SD total daily ACB score of 0.33 ± 0.61 compared with 1.1 ± 1.3 in our population, as well as in racial diversity, which included a large proportion of European and Polynesian patients (79.1% and 4.7%, respectively) compared with our distribution of white and African Americans (39.5% and 57.8%, respectively). In addition, the authors did not account for prior visit data as a confounding variable in their regression models.
One study published results from a Finnish population that were similar to those of our study, with similar racial and methodologic differences.14 Another study reported a higher rate of fall-related hospitalizations (incident rate ratio 1.56, 95% CI 1.47–1.65) and general practice visits (incident rate ratio 1.13, 95% CI 1.12–1.13) among older adults using medications identified in the Drug Burden Index.10 Medications included in this exposure variable reflect the combination of both anticholinergic and sedative agents. A second study reported specifically hospital visits for confusion or altered mental status, showing an increased risk among users of at least two anticholinergic medications.14 Our results report higher health care utilization by incremental increase in total daily ACB score and included a diverse population of older adults from a safety-net health care system with ~60% African Americans and a significant burden of comorbid disease.
The correlation between total daily ACB score and cognitive impairment is in a similar direction as that in several other reports.5–10 However, few of these studies calculated ACB exposure with pharmacy dispensing records and included medications with mild anticholinergic properties. In addition, the proportion of the variance predicted in our models was similar to other reports evaluating anticholinergic and sedative exposure with cognitive and physical function.11 Our results suggest that each 1-point increase in mean total daily ACB score increases the risk of cognitive impairment by 13%. This risk can be interpreted as the additional risk among patients taking a strong anticholinergic for as little as 4 months (out of 12 mo) or one mild anticholinergic every day for 12 months compared with those who do not take an anticholinergic medication. Further increases in mean total daily ACB score resulted in higher risk: a patient taking one strong anticholinergic every day for 12 months would correlate with a 39% increased risk of cognitive impairment compared with those not exposed to anticholinergics. With dementia prevalence already expected to surpass 7 million individuals in the United States by 2025,29 the importance of identifying and testing the reversibility of medications that increase the risk becomes particularly important.30
Limitations of this work are worth noting. First, the use of medication dispensing records to measure exposure assumes consumption of all medications dispensed. This method, however, minimizes recall bias by constructing exposure variables from objective data and is preferred over the use of self-reporting or medication orders to measure medication exposure. A second limitation is the length of time between the analysis and the data collection period. Although recent reports suggest that exposure to anticholinergics has not changed,1, 2, 4, 7 the lag time may introduce temporal bias that may introduce changes in prescribing or visit patterns. Third, evaluating medication exposure prior to cognitive assessment may introduce protopathic bias that may account for our findings.30, 31 In addition, although we included a number of variables in the regression models, there may be unmeasured variables that could explain our findings. Fourth, although the populations included in this study were cared for by a safety-net health care system that provides continuous acute and chronic care services, visits outside of the system may not have been captured, and 23% of the population did not have 365 days of dispensing records available. This gap may be due to relocation (patients leaving the system) or receiving medications outside the data catchment area. It is unknown whether more complete data would have altered our results. Lastly, the method used to quantify anticholinergic exposure assumes that the contribution of anticholinergics to the study outcomes is similar; due to the relatively small sample size, we could not test whether each anticholinergic class was associated with study outcomes to a similar degree.
Conclusion
This study showed an increased rate of health care utilization with increasing total daily ACB score among a diverse population of older adults with multiple chronic conditions. Increasing total daily ACB score also increased the risk of cognitive impairment. Future work should develop safe, effective approaches to reducing exposure to anticholinergic medications and evaluate the impact on financial and patient safety outcomes.
Table 5.
Relationship Between Anticholinergic Cognitive Burden Total Score and Number of Outpatient Visits Adjusted for Demographic and Clinical Characteristics
| Variable | Unadjusted for prior health care utilization | Adjusted for prior health care utilization | ||
|---|---|---|---|---|
|
|
|
|||
| Estimate (SE) | p value | Estimate (SE) | p value | |
| Age | −0.068 (0.025) | 0.007 | −0.049 (0.023) | 0.034 |
| Female | 1.161 (0.313) | < 0.001 | 0.712 (0.292) | 0.015 |
| White | 0.505 (0.877) | 0.564 | 0.472 (0.808) | 0.559 |
| African American | 0.666 (0.868) | 0.443 | 0.532 (0.800) | 0.506 |
| Arthritis | 0.696 (0.333) | 0.037 | 0.130 (0.309) | 0.674 |
| Cancer | 2.004 (0.324) | < 0.001 | 1.201 (0.300) | < 0.001 |
| CAD | 0.567 (0.314) | 0.072 | −0.034 (0.292) | 0.906 |
| CHF | 2.135 (0.326) | < 0.001 | 1.598 (0.303) | < 0.001 |
| COPD | 0.819 (0.310) | 0.008 | 0.327 (0.290) | 0.260 |
| Diabetes mellitus | 1.128 (0.294) | < 0.001 | 0.533 (0.274) | 0.052 |
| Liver disease | 3.278 (0.696) | < 0.001 | 2.854 (0.641) | < 0.001 |
| Renal disease | 1.386 (0.385) | < 0.001 | 0.937 (0.355) | 0.008 |
| Stroke | 1.668 (0.312) | < 0.001 | 0.789 (0.292) | 0.007 |
| No. of non-anticholinergic drugs | – | – | −0.004 (0.031) | 0.911 |
| Prior inpatient admissions | – | – | −0.148 (0.265) | 0.575 |
| Prior ED visits | – | – | 0.295 (0.095) | 0.002 |
| Prior outpatient visits | – | – | 0.410 (0.020) | < 0.001 |
| Mean total daily ACB score | 0.841 (0.119) | < 0.001 | 0.382 (0.113) | 0.001 |
ACB = Anticholinergic Cognitive Burden; CAD = coronary artery disease; CHF = congestive heart failure; COPD = chronic obstructive pulmonary disease; ED = emergency department; SE = standard error.
Acknowledgments
Study concept, acquisition of data, conduct of the collection, management and analysis of the study was conducted by Drs. Campbell and Boustani and Mr. Perkins; design and interpretation of results were executed by Drs. Campbell, Boustani, Bradt, Perk, and Ng, and Mr. Wielage and Mr. Perkins. Preparation of the manuscript was conducted by Dr. Campbell and Mr. Perkins, with revisions and approval performed by Drs. Campbell, Boustani, Bradt, Perk, and Ng, and Mr. Wielage and Mr. Perkins. Dr. Campbell and Mr. Perkins had full access to all of the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
Footnotes
Conflict of Interest: This work was supported by a research grant from Astellas Pharma Global Development, U.S. The study design, analysis, and manuscript were developed by the Regenstrief Institute Inc., and Medical Decision Modeling, Inc. Dr. Campbell and Mr. Perkins assume responsibility for the content and validity of the analysis. Research reported in this publication was also supported by the National Institute on Aging of the National Institute of Health award no. K23AG044440 [principal investigator: Noll Campbell] The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
References
- 1.Schubert CC, Boustani M, Callahan CM, et al. Comorbidity profile of dementia patients in primary care: are they sicker? J Am Geriatr Soc. 2006;54:104–9. doi: 10.1111/j.1532-5415.2005.00543.x. [DOI] [PubMed] [Google Scholar]
- 2.Buck MD, Atreja A, Brunker CP, et al. Potentially inappropriate medication prescribing in outpatient practices: prevalence and patient characteristics based on electronic health records. Am J Geriatr Pharmacother. 2009;7(2):84–92. doi: 10.1016/j.amjopharm.2009.03.001. [DOI] [PubMed] [Google Scholar]
- 3.Campbell N, Boustani M, Limbil T, et al. The cognitive impact of anticholinergics: a clinical review. Clin Interv Aging. 2009;4:225–33. doi: 10.2147/cia.s5358. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.West T, Pruchnicki MC, Porter K, Emptage R. Evaluation of anticholinergic burden of medications in older adults. J Am Pharm Assoc (Wash) 2013;53:496–504. doi: 10.1331/JAPhA.2013.12138. [DOI] [PubMed] [Google Scholar]
- 5.Cai X, Campbell N, Khan B, Callahan C, Boustani M. Long-term anticholinergic use and the aging brain. Alzheimers Dement. 2013;9:377–85. doi: 10.1016/j.jalz.2012.02.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Koyama A, Steinman M, Ensrud K, Hillier TA, Yaffe K. Ten-year trajectory of potentially inappropriate medications in very old women: importance of cognitive status. J Am Geriatr Soc. 2013;61:258–63. doi: 10.1111/jgs.12093. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Campbell NL, Boustani MA, Lane KA, et al. Use of anticholinergics and the risk of cognitive impairment in an African American population. Neurology. 2010;75:152–9. doi: 10.1212/WNL.0b013e3181e7f2ab. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Gray SL, Anderson ML, Dublin S, et al. Cumulative use of strong anticholinergics and incident dementia: a prospective cohort study. JAMA Intern Med. 2015;175:401–7. doi: 10.1001/jamainternmed.2014.7663. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Fox C, Smith T, Maidment I, et al. Effect of medications with anti-cholinergic properties on cognitive function, delirium, physical function and mortality: a systematic review. Age Ageing. 2014;43:604–15. doi: 10.1093/ageing/afu096. [DOI] [PubMed] [Google Scholar]
- 10.Nishtala PS, Narayan SW, Wang T, Hilmer SN. Associations of drug burden index with falls, general practitioner visits, and mortality in older people. Pharmacoepidemiol Drug Saf. 2014;23:753–8. doi: 10.1002/pds.3624. [DOI] [PubMed] [Google Scholar]
- 11.Kalisch Ellett LM, Pratt NL, Ramsay EN, Barratt JD, Roughead EE. Multiple anticholinergic medication use and risk of hospital admission for confusion or dementia. J Am Geriatr Soc. 2014;62:1916–22. doi: 10.1111/jgs.13054. [DOI] [PubMed] [Google Scholar]
- 12.Salahudeen MS, Hilmer SN, Nishtala PS. Comparison of anticholinergic risk scales and associations with adverse health outcomes in older people. J Am Geriatr Soc. 2015;63:85–90. doi: 10.1111/jgs.13206. [DOI] [PubMed] [Google Scholar]
- 13.Myint PK, Fox C, Kwok CS, Luben RN, Wareham NJ, Khaw KT. Total anticholinergic burden and risk of mortality and cardiovascular disease over 10 years in 21,636 middle-aged and older men and women of EPIC-Norfolk prospective population study. Age Ageing. 2015;44:219–25. doi: 10.1093/ageing/afu185. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Gnjidic D, Hilmer SN, Hartikainen S, et al. Impact of high risk drug use on hospitalization and mortality in older people with and without Alzheimer’s disease: a national population cohort study. PLoS One. 2014;9:e83224. doi: 10.1371/journal.pone.0083224. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Yaffe K, Falvey C, Harris TB, et al. Effect of socioeconomic disparities on incidence of dementia among biracial older adults: prospective study. BMJ. 2013;347:f7051. doi: 10.1136/bmj.f7051. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Glymour MM, Manly JJ. Lifecourse social conditions and racial and ethnic patterns of cognitive aging. Neuropsychol Rev. 2008;18(3):223–54. doi: 10.1007/s11065-008-9064-z. [DOI] [PubMed] [Google Scholar]
- 17.Boustani M, Callahan CM, Unverzagt FW, et al. Implementing a screening and diagnosis program for dementia in primary care. J Gen Intern Med. 2005;20:572–7. doi: 10.1111/j.1525-1497.2005.0126.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.McDonald CJ, Tierney WM, Overhage JM, Martin DK, Wilson GA. The Regenstrief Medical Record System: 20 years of experience in hospitals, clinics, and neighborhood health centers. MD Comput. 1992;9:206–17. [PubMed] [Google Scholar]
- 19.McDonald CJ, Overhage JM, Tierney WM, et al. The Regenstrief Medical Record System: a quarter century experience. Int J Med Inform. 1999;54:225–53. doi: 10.1016/s1386-5056(99)00009-x. [DOI] [PubMed] [Google Scholar]
- 20.Callahan CM, Unverzagt FW, Hui SL, Perkins AJ, Hendrie HC. Six-item screener to identify cognitive impairment among potential subjects for clinical research. Med Care. 2002;40:771–81. doi: 10.1097/00005650-200209000-00007. [DOI] [PubMed] [Google Scholar]
- 21.Hall KS, Gao S, Emsley CL, Ogunniyi AO, Morgan O, Hendrie HC. Community screening interview for dementia (CSI ‘D’); performance in five disparate study sites. Int J Geriatr Psychiatry. 2000;15:521–31. doi: 10.1002/1099-1166(200006)15:6<521::aid-gps182>3.0.co;2-f. [DOI] [PubMed] [Google Scholar]
- 22.Morris JC, Mohs RC, Rogers H, Fillenbaum G, Heyman A. Consortium to establish a registry for Alzheimer’s disease (CERAD) clinical and neuropsychological assessment of Alzheimer’s disease. Psychopharmacol Bull. 1988;24:641–52. [PubMed] [Google Scholar]
- 23.Spitzer R. Diagnostic and statistical manual of mental disorders. 3. 1987. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Caldwell N, Srebotnjak T, Wang T, Hsia R. “How much will I get charged for this?” Patient charges for top ten diagnoses in the emergency department. PLoS One. 2013;8:e55491. doi: 10.1371/journal.pone.0055491. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Noe L, Becker R, Williamson T, Chen D. A pharmacoeconomic model comparing two long-acting treatments for overactive bladder. J Manag Care Pharm. 2002;8:343–52. doi: 10.18553/jmcp.2002.8.5.343. [DOI] [PubMed] [Google Scholar]
- 26.American Medical Association. [Accessed April 14, 2014];Physician Fee Schedule Search. 2014 Available from https://www.cms.gov/apps/physician-fee-schedule/license-agreement.aspx.
- 27.Kaiser Family Foundation. [Accessed July 15, 2016];Health Costs and Budget Indicators. 2014 data. Available from http://kff.org/state-category/health-costs-budgets/
- 28.Hilmer SN, Mager DE, Simonsick EM, et al. A drug burden index to define the functional burden of medications in older people. Arch Intern Med. 2007;167:781–7. doi: 10.1001/archinte.167.8.781. [DOI] [PubMed] [Google Scholar]
- 29.Alzheimer’s Association. 2016 Alzheimer’s disease facts and figures. Alzheimers Dement. 2016;12(4) doi: 10.1016/j.jalz.2016.03.001. [DOI] [PubMed] [Google Scholar]
- 30.Campbell NL, Boustani MA. Adverse cognitive effects of medications: turning attention to reversibility. JAMA Intern Med. 2015;175:408–9. doi: 10.1001/jamainternmed.2014.7667. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Amieva H, Le Goff M, Millet X, et al. Prodromal Alzheimer’s disease: successive emergence of the clinical symptoms. Ann Neurol. 2008;64:492–8. doi: 10.1002/ana.21509. [DOI] [PubMed] [Google Scholar]