Abstract
The robotic nurse plays an essential role in a successful robotic surgery. As part of the robotic surgical team, the robotic nurse must demonstrate a high level of professional knowledge, and be an expert in robotic technology and dealing with robotic malfunctions. Each one of the robotic nursing team “nurse coordinator, scrub-nurse and circulating-nurse” has a certain job description to ensure maximum patient's safety and robotic surgical efficiency. Well-structured training programs should be offered to the robotic nurse to be well prepared, feel confident, and maintain high-quality of care.
Keywords: Nurses, Perioperative nursing, Robotics, Robotic nurse, Urology
1. Introduction
Since its introduction in 2001, the use of robotic surgery is expanding rapidly in all surgical fields and subspecialties such as thoracic, colorectal, hepatobiliary, gynecological, and urological surgeries. Subsequently, both the facilities purchasing robotic systems and the number of surgeons using them are increasing, which creates many challenges in terms of cost, training and safety.
Robotic surgery has many advantages for the patients, surgeons and nurses. It provides benefit of minimal invasive surgery (e.g. less blood loss, lower transfusion rate, and shorter recovery time), minimizes the inconvenience, enhances visualization through three-dimension high-definition binocular lens, better ergonomics, and motion scaling. For nurses, it provides better visualization in vision cart which make surgery more easy and clear. And as operating nurses, it allows them to have experience of new technologies and roles. Moreover, they can establish territory as a clinical expert and expand roles as professional nurses.
Accomplishment of successful robotic surgery requires a comprehensive skillful teamwork that could play together in a harmony like orchestra symphony, while maintaining the maximum safety of the patient and quality of care. The robotic surgery team work inside the operating room is composed of the main robotic surgeon, bed-side assistant, robotic nurse, and anesthesia team.
Among this team, the robotic nurses' role has gained a rapid development and was discussed in many previous reports which emphasized on the great importance of their role during surgery [1], [2], [3], [4]. The robotic nurse is capable of building a comprehensive picture of how, why, and when the robotic system is being used. Subsequently, the nurse configures the optimal use of equipment, instruments, and supplies. Having a properly trained robotic nurse team could reduce the cost of robotic surgery [5]. Moreover, the robotic nurse allows fast and accurate solving for problems with the robotic equipment and instruments [1]. Kang et al. [2] categorized robotic nurses work experience of major hospitals in South Korea into four main themes: (a) checking patients' safety and the robot's functions; (b) dealing with any unexpected robotic machine malfunctions; (c) feelings of burden in a robotic surgical team; and (d) need for more education and training. They recommended that offering more support for nurses involved in robotic surgery should be a priority to empower them to play an extended role in robotic surgery.
The present article describes in details the role of robotic nurse in Severance Hospital since the introduction of robotic surgery in our urology department, and its evolution until the present time.
2. History of robotic surgery in South Korea
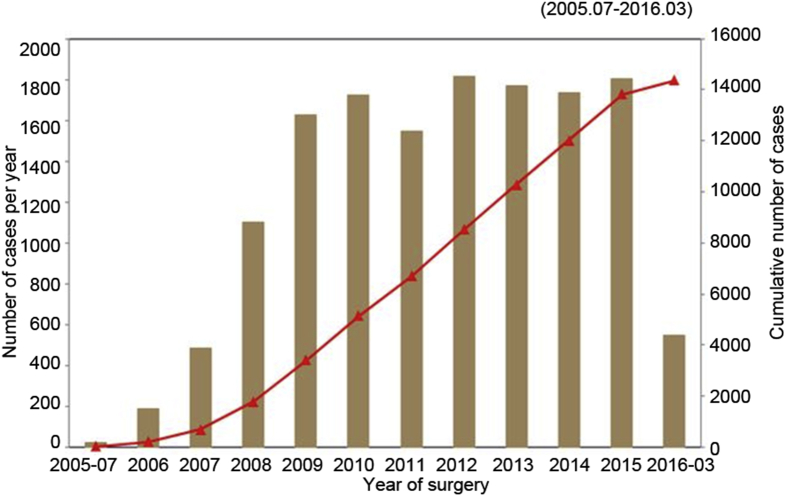
The Korean Ministry of Food and Drug Safety approved da Vinci robotic surgery (Intuitive Surgical, Inc., Sunnyvale, CA, USA) on 13th of July 2005. After approval and up-to-date, a total of 53 da Vinci surgical systems had been installed in 40 institutions in South Korea. Severance Hospital was honored to launch the start of robotic surgery in South Korea when the first robotic-assisted cholecystectomy was carried out in July 2005. From 2005 to 2014, more than 16,000 urological robotic procedures were performed in South Korea (Fig. 1); of these cases more than 3400 were in the year 2014 only. Subsequently, many Korean studies entitling different robotic procedures were published. Cho et al. [6] reported that robotic-assisted radical prostatectomy (RARP) (n = 60) had better results in operating time, estimated blood loss, hospital stay, and urinary catheterization duration compared to the laparoscopic approach (n = 60). While there was no difference regarding the trifecta achievement. On the other hand, Jang et al. [7] compared the perioperative outcomes of robotic-assisted partial nephrectomy RAPN (n = 89) and laparoscopic partial nephrectomy (n = 38) for tumors with R.E.N.A.L. score ≥7. They found no significant differences in warm ischemic time blood loss, intraoperative complications, or operation time between groups. Interestingly, Kang et al. [8] presented a developed technique of robotic-assisted radical cyctectomy (RARC) with complete intracorporeal urinary diversion, and concluded that their technique is a feasible procedure with less blood loss and earlier recovery.
Figure 1.
Number of urologic robotic surgeries (Y-axis) from the year 2005–2014 in South Korea (data from Intuitive Surgical Korea) adapted from Seo Y. 2015 [25]. RALPP, robot-assisted laparoscopic pyeloplasty; RALRC, robot assisted laparoscopic radical cystectomy; RALRN, robot-assisted laparoscopic radical nephrectomy; RALPN, robot-assisted laparoscopic partial nephrectomy; RALRP, robot-assisted laparoscopic radical prostatectomy.
2.1. History of robotic surgery in Severance Hospital
Severance Hospital contains 10 robotic surgical systems: 6 da Vinci Si and 4 da Vinci Xi. The first RARP was performed by Dr. Koon Ho Rha in July 2005, using the da Vinci Standard surgical system in Severance Hospital [9]. By that time, the number of da Vinci surgical procedures in Severance Hospital has been increased dramatically, and from July 2005 to March 2016 the total number of robotic procedures has reached 14,371, representing the largest robotic volume among all Korean hospitals. The main subjects in our robotic procedures are general and urologic surgeries. The general surgery is interestingly more frequent than urologic surgery procedures (7743 vs. 4780), respectively (Fig. 2). Recently, we reported the largest Asian cohort (n = 800) of RARP with the longest follow-up period (median 5 years). And we concluded that RARP confers excellent oncological outcomes even in high-risk prostate cancer patients [10]. Furthermore, Abdel Raheem et al. [11] reported the largest series (n = 121) of high-complex renal tumors (PADUA score ≥10) treated by RAPP in Severance Hospital and found that high-complex PADUA tumors are associated with higher perioperative complications and a lower rate of trifecta achievement with equivalent long-term oncological and functional outcomes to intermediate and low-complex tumors.
Figure 2.
Number of overall robotic procedures in Severance Hospital in each department from July 2005 to March 2016. ENT, ear and nose; GS, general surgery; GYN, gynecology; NS, neurosurgery; URO, urology.
3. Severance Robotic Surgery Training Center
In 2008, the Severance Hospital opened Korea's first Minimally Invasive Surgery (MIS) and Robotic Training Center (RC), where doctors can learn about da Vinci robots. Since then, Severance Hospital, which is affiliated with Yonsei University College of Medicine, has cemented its position as the hub for those who want to receive robotic surgery and those who want to learn it. MIS/RC has trained medical doctors including main operators and fellows, nurses, and coordinators. It offers several training programs including basic training using a porcine model, wet lab, and advanced training courses. Moreover, it presents an advanced robotic training course using a cadaver. The training centers focus on general surgery, cardiothoracic surgery, gynecology, and urology. Additionally, the Severance center MIS/RC had carried out more than 313 basic training sessions, as well as, many doctors, including 500 from other countries, have received training at our training center.
4. Robotic urological procedures in Severance Hospital
Since the introduction of da Vinci in Severance Hospital, there is progressive increase in the number of urological robotic surgeries, with subsequent decline in the open surgical procedures (Fig. 3). Nowadays, most oncological surgeries are carried out by the robot. Even in cases of multiple urinary tract malignancies, surgical management by robotic surgery in single session is easily performed. Recently, we reported the safety and feasibility of simultaneous retzius-sparing RARP and RAPN in treatment of a 61-year-old man who had synchronous prostate cancer and renal cell carcinoma [12].
Figure 3.
Shows the trend of robotic procedures (Y-axis represent the number of surgeries) from the year 2005–2015.
Various types of robotic surgery are performed in our department: (a) Radical prostatectomy (transperitoneal, extraperitoneal and retzius-sparing techniques); (b) radical nephrectomy, partial nephrectomy (transperitoneal and retroperitoneal), radical nephroureterctomy with bladder cuff excision; and (c) radical cystectomy with intracorporeal urinary diversion.
For this reason, our robotic nurses have a great experience with robotic surgery, since our hospital is considered one of the biggest tertiary robotic centers in South Korea and Asia.
5. Robotic urology nursing staff
In our urology department, we have two robotic nursing teams: the main hospital has 8 robotic nurses serving in two operating rooms (ORs), and the cancer hospital has 9 robotic nurses serving in three ORs (Fig. 4).
Figure 4.
Robotic team in the main hospital: Chief coordinator “in the middle” and robotic nurse's specialists.
6. Recruitment of new robotic nurse
There is a rule to hire a new robotic nurse in our hospital. There is a minimum level of requirements and qualification for recruiting robot nurses. Each nurse must have at least three full years of work experience in the OR. In addition, those nurses should have multiple-specialty training in at least two departments which entails robotic surgery. Moreover, their yearly evaluation reports should be commendable. Furthermore, during the initial recruitment interview they should show enthusiasm, competency and good working habit to meet the challenging needs of patients undergoing robotic surgery.
After initial recruitment, each nurse passes through the standardized training process to become robotic nurse. First, the robotic nurse should undergo a basic training in our MIS/RC, entailing the da Vinci surgical system i.e. setting-up, turn-on, shut-down, connections, positioning of the robotic table and console, docking and undocking, malfunction and errors management, etc. This process lasts for 2 weeks, 4 h per day and in the end the nurse receives a training certificate. Subsequently, after her dry laboratory training, the nurse receives an intensive OR training for 6 weeks. During this apprenticeship, the nurse acts as a second scrub-nurse in 2–3 robotic procedures daily. A thorough evaluation is performed during this period by the nurse coordinator and the whole robotic nurse team to assess the progress of his/her understanding of each procedural step, troubleshooting and maintaining patient's safety. The final recommendation is decided upon by nurse coordinator and the team. After a successful apprenticeship, she becomes part of the team as an independent robotic nurse.
7. Duties of the robotic nurse inside the OR
The job description of the robotic nurse designated her/his role to be an expert staff for clinical care of patients undergoing robotic-assisted surgery. Robotic nurses are divided into three groups inside the OR; nurse coordinator (chief robotic nurse), scrub-nurse and circulating-nurse.
7.1. Duties of da Vinci coordinator
The nurse coordinator is the most expert in robotic surgery among nurses. She/he engages in many scientific activities that develop and maintain clinical expertise and professional skills. The nurse coordinator has the following duties and responsibilities:
-
1.
Schedule management: The nurse coordinator coordinates the daily operation schedule to avoid discrepancy between different departments, and allow sufficient time between subsequent robotic surgeries and the following one for OR and robot set-up.
-
2.
System operating and management: The nurse coordinator is responsible for maintaining accuracy of the operating system and management ability including inventory management.
-
3.
Clinical support: The nurse coordinator supervises the robot set-up, progression of patient preparation, nurse's performance during the whole procedure, could offer help and advice for any problems encountered during robotic surgery.
-
4.
Education and training: The nurse coordinator plays an important role in orientation of the new personnel, training existing personnel, ensuring completion of competencies for all new members, and assists in setting up educational programs for medical students, urology residents, nurses, fellows and surgeons.
7.2. Duties of da Vinci scrub and circulating-nurses
The robotic nurse must keep OR skills up-to-date to maintain the necessary skills, and to provide high quality patient care in the OR [1]. The ability to function as a circulating or scrub-nurse gives the robotic nurse better chance for proper assessment and use of all the robotic equipment, instruments, and supplies. Simply, they are responsible for the following:
7.2.1. Patient safety
Patients' safety comes first. Nurses check the instruments before surgery to be sure that it works properly. All connection of electrical cables, pads, tubes, and CO2 gas tube are checked before surgery to ensure safe connection. After the robot setup, nurses check whether the instruments are in its correct position. They must be familiar with the robotic instruments needed for each type of procedure, including how to properly load and handle it. The robotic supply cart is located outside the OR. It should contain all the required robotic instruments and supplies, which helps to maintain flexibility in the OR. To enhance the robotic cost effectiveness, the procedure starts with only the essential instruments and supplies, after which extra items can be added in a timely manner if needed.
7.2.2. Patient positioning
Nurses are oriented with different patient positions of each robotic procedure e.g. steep Trendlenberg position for pelvic surgery such as prostate or bladder, and lateral flank position for renal surgeries. All pressure points must be protected using verified safety devices e.g. air-inflated positioning devices and high-density foam padding to avoid skin pressure, neuromuscular injuries, and venous thrombosis owing to improper patient positioning and padding before surgery [13]. Moreover, they must be proficient in the undocking procedures for any unexpected emergency situation [14].
7.2.3. Robot draping and docking
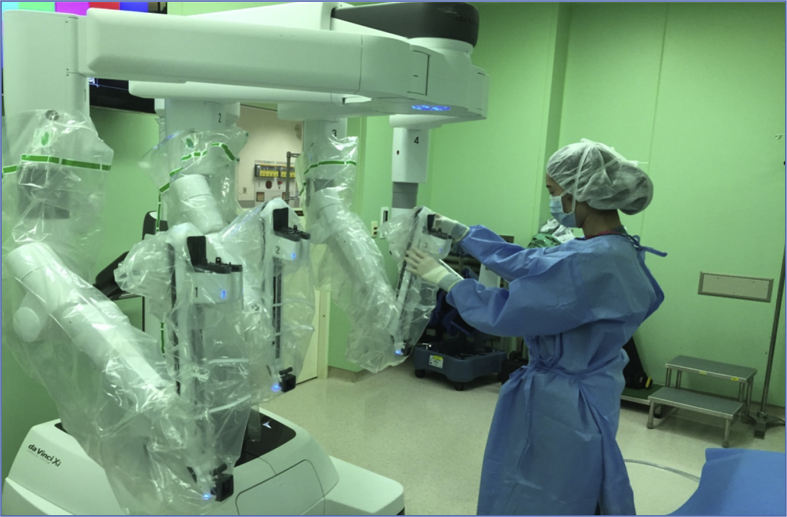
The robotic nurse prepares the robot before surgery by testing it for safety, function, assembling the arm, draping the machine in sterile technique, and keeps it covered to avoid contamination until start the docking process (Fig. 5). Once the robot is introduced into the surgical field, they help the bed-side assistant in moving and docking the robotic arms to the ports, install and manage the camera.
Figure 5.
Robotic system sterile draping.
7.2.4. During surgery
While surgery is in progress, scrub and circulating nurses continuously monitor the patient safety, check the robotic system, robotic arms movement, CO2 level, and whether the machine is pressing against the patient to avoid their injury, and look for any signs of robotic malfunction. They must be able to assist intraoperatively in all robotic surgical procedures, and clean the robotic instruments during the surgery using brush tools, sometimes they interpret message from robot system. The ability of the nursing personnel to interpret and react to messages displayed on the robotic television monitor is critically important to the flow and success of the procedure, and allows the surgeons to focus fully on the surgical procedure.
Moreover, the robotic nurse specialist registers the frequency of use of each instrument during surgery to alert the next scrub person when the instrument needs to be discarded. Therefore, she/he is responsible for tracking the “robotic instruments life” (i.e. number of times that the instrument still can be used). This could be carried out through either writing on the instrument with an indelible marker or registering on the specified instrument log.
7.2.5. Robot malfunctions
Robotic system errors or malfunctions may occur at any time. Several studies have reported robotic malfunctions at the time of robotic surgery [15], [16], resulting in delay, postponement, or conversion to open or laparoscopic surgery [17], [18], and rarely may result in patient injuries [13].
To prevent user error and rapidly recognize device failure, all health care team members must thoroughly understand robotic surgery and their role in the procedure [19], [20], [21]. Furthermore, providing the robotic nurse with the proper knowledge regarding the system troubleshoots use and not just follow a series of setup instructions, is a paramount step to establish a good general medical robotic system background. Only oriented robotic nurses are assigned to setup the robot, run it, solve problems that arise, and handle the emergency situations.
To manage the instrument and system, the robotic nurse has to know the route to claim the error. When nurses become aware of an error message, they will be able to act immediately. For instrument claim (i.e. broken, malfunction or miscount of life), customer service or clinical sales representative take charge of this. It also would be helpful to record any complaints about the instrument or difficulty in using it.
7.2.6. After surgery
When one surgery ends, nurses help in undocking of the robot, along with the surgical technicians are responsible for completing the medical charts, and doing an inventory of the robotic instruments, then cleaning-up and setting-up for the next case.
The robotic instruments can be sterilized individually. When body tissue or fluids “i.e. blood” are still attached to the instrument's ends, they should be cleaned on the sterile field through the manufacturer's designated ports, and before sending for terminal cleaning and sterilization. Seldom-used instruments are sterilized separately and are kept ready for use when needed on the support cart.
7.2.7. Research filed
Robotic nurses should demonstrate reasonable proficiency in basic computer software applications, basic data collection knowledge, research approaches, and protocol types. Moreover, they could be able to participate in developing a research through ensuring adequate data management and dissemination.
8. Instruments check-list before robotic procedure
The robotic nurses are responsible for preparation of the surgical field of each robotic procedure, and should be fully oriented which instruments will be used before the start of surgery. They arrange the instruments over the surgical tables in a standardized manner, and revise the instruments “Check-list” (Fig. 6). The development and use of surgical checklists could improve patients' safety by detection of potential safety hazards, lowering the surgical complications, and improving the patient outcomes and the surgical team communication [22], [23]. Each robotic procedure has its own instruments “Check-list”; examples of the RARP and RAPN are illustrated in Table 1, Table 2.
Figure 6.

Instruments check-lists for robot-assisted radical prostatectomy.
Table 1.
Instruments check-list for robot-assisted radical prostatectomy.
| Application | Number | Recommended robotic instrumentations |
|---|---|---|
| Dissection and monopolar coagulation for mobilizing colon, exposing prostate and division of urethra | 1 | Hot shear™ monopolar curved scissor |
| Grasping, retraction, blunt-tip dissection and bipolar cautery for mobilizing colon, dissecting and manipulating tissue | 1 | Maryland bipolar forceps |
| Suturing for vesicourethral anastomosis, bladder neck repair and peritoneal closure | 2 | Large needle drivers |
| Non-energized instrument with similar features with similar features to the fenestrated bipolar forceps | 1 | ProGrasp™ forceps |
| 1 | Intuitive surgical camera head | |
| 1 | Intuitive surgical 12 mm 0° and 30° lens | |
| Recommended laparoscopic accessories and instrumentations | ||
| Retrieval of margin specimens | 1 | 5 mm laparoscopic grasper |
| Provide and remove sutures | 5 mm laparoscopic needle driver | |
| Cut the suture end | 1 | 5 mm laparoscopic scissor |
| Control bleeding | 2 | 10 mm metal cips (test function preoperatively) LIGACLIP, ethicon |
| Control bleeding | 2 | 5 mm metal cips (test function preoperatively) LIGACLIP, ethicon |
| Support vesicourehral anastomosis suturing | 2 | Lapra-Ty clip (test function preoperatively) |
| Applied on anastomotic end | 1 | Greenplast (fibrin glue) |
| Judicious placement | Surgicel® | |
| Specimen retrieval | 2–3 | Lap bag medium or large |
| 1 | Drain | |
| Suction and irrigation | 1 | Suction tip/irrigation system |
| Applied before closure of peritoneal incision | 1 | Guardix |
| Recommended sutures | ||
| DVC control Back-bleeding stitch/handle | 3 | 0 Vicryl on CT-1 |
| Back-bleeding stitch/handle | 3 | 2-0 Vicryl on SH |
| Vesicourehral anastomosis running suture | 3 | 3-0 V-Loc |
| Bladder neck repair vesicourehral anastomosis interrupted suture | 3 | 2-0 or 3-0 vicryl/monocryl on RB-1/SH |
CT, circle taper; DVC, deep vein complex; RB, renal bypass; SH, small half.
Table 2.
Instruments check-list for robot-assisted partial nephrectomy.
| Application | Number | Recommended robotic instrumentations |
|---|---|---|
| Dissection and monopolar coagulation for mobilizing colon, dissecting hilum and expose tumor | 1 | Hot Shear™ monopolar curved scissor |
| Grasping, retraction, blunt-tip dissection and bipolar cautery for mobilizing colon, dissecting hilum and manipulating tissue | 1 | Fenestrated bipolar forceps |
| Suturing for collecting system, parenchymal reconstruction and Gerota's fascia | 2 | Large needle drivers |
| Non-energized instrument with similar features with similar features to the fenestrated bipolar forceps | 1 | ProGrasp™ forceps |
| 1 | Intuitive surgical camera head | |
| 1 | Intuitive surgical 12 mm 0° and 30° lens | |
| Firefly fluorescence imaging system (for Si) | ||
| Recommended laparoscopic accessories and instrumentations | ||
| Retrieval of margin specimens | 1 | 5 mm laparoscopic grasper |
| Provide and remove sutures | 5 mm laparoscopic needle driver | |
| Cut the suture end | 1 | 5 mm laparoscopic scissor |
| Liver retraction | 1 | 5 mm laparoscopic toothed grasper |
| Prepare and secure sutures for renal defect closure | 2 | 5 mm automatic endoscopic hem-o-lok Applier (Auto endo5® hem-o-lok®, WECK) |
| Control the renal hilar vessels | Laparoscopic bulldog clamps | |
| 2 | Short straight | |
| 2 | Short curved | |
| 2 | Long straight | |
| 2 | Long curved | |
| Tumor margins and depth assessment | 1 | Laparoscopically controlled ultrasound probe from the bedside |
| Control bleeding | 2 | 10 mm metal cips (test function preoperatively) LIGACLIP, ethicon |
| Control bleeding | 2 | 5 mm metal cips (test function preoperatively) LIGACLIP, ethicon |
| Support vesicourehral anastomosis suturing | 2 | Lapra-Ty clip (test function preoperatively) |
| Applied on renorraphy site | 1 | Greenplast (Fibrin glue) |
| Applied on renal defect after closure | 1 | Floaseal (hemostatic matrix), baxter |
| Judicious placement | Surgicel® | |
| Determine renal blood flow | 1 amp | Indocyanine green (ICG) |
| Specimen retrieval | 2–3 | Lap bag medium or large |
| Drainage | 1 | Drain |
| Suction and irrigation | 1 | Suction tip/irrigation system |
| Recommended sutures | ||
| Inner layer or deep closures | 3 | 3-0 vicryl on SH needle |
| Renal capsule closure | 3 | 2-0 vicryl on SH needle |
SH, small half.
9. Nurse education and training
Although more educational programs for robotic nurses are urgently needed, however, majority of them suffer from the lack of updated information, training programs, and learning opportunities. Most conferences and continuing education are only for surgeons. Well-structured training programs including hands-on training, what to do when an emergency situation arises [14], and multidisciplinary team training for the resuscitation during robotic-assisted surgery [24] should be offered to nurses involved in robot surgery. This will contribute to ensuring patient's safety and quality of care and empower nurses to feel well confident and prepared during robotic surgery [14], [24].
In our urology department, we are responsible for helping the robotic nurses in their education, and present to them the recent update of clinical robotic knowledge system maintenance and upgrade (i.e. Si, smart pedal, vessel sealer, single site, firefly, etc.) through our regular monthly conference.
10. Conclusion
Since the introduction of da Vinci surgical system last decade, the robotic nurse role has been evolved rapidly, and became of great importance during the robotic surgery. A skilled robotic nurse is an essential part of an effective robotic surgery team. Roles and duties of the robotic nurse have been changed over time, and they are considered a vital bridge between the console surgeon, bed-side assistant and the patient. The robotic nurse should acquire and maintain current knowledge on best-practice nursing rules for robotic surgery to understand the operation, improve the overall flow, and management of unanticipated circumstances, in order to maintain high-quality of care and patient's safety.
Conflicts of interest
The authors declare no conflict of interest.
Footnotes
Peer review under responsibility of Second Military Medical University.
References
- 1.Francis P. Evolution of robotics in surgery and implementing a perioperative robotics nurse specialist role. AORN J. 2006;83:630–642. doi: 10.1016/s0001-2092(06)60191-9. [DOI] [PubMed] [Google Scholar]
- 2.Kang M., De Gagne J.C., Kang H.S. Perioperative nurses' work experience with robotic surgery: a focus group study. Comput Inf Nurs. 2016;34:152–158. doi: 10.1097/CIN.0000000000000224. [DOI] [PubMed] [Google Scholar]
- 3.Thomas C.C. Role of the perioperative nurse in robotic surgery. Perioper Nurs Clin. 2011;6:227–234. [Google Scholar]
- 4.Francis P., Winfield H.N. Medical robotics: the impact on perioperative nursing practice. Urol Nurs. 2006;26:99–108. [PubMed] [Google Scholar]
- 5.Nayeemuddin M., Daley S.C., Ellsworth P. Modifiable factors to decrease the cost of robotic-assisted procedures. AORN J. 2013;98:343–352. doi: 10.1016/j.aorn.2013.08.012. [DOI] [PubMed] [Google Scholar]
- 6.Cho J.W., Kim T.H., Sung G.T. Laparoscopic radical prostatectomy versus robot-assisted laparoscopic radical prostatectomy: a single surgeon's experience. Korean J Urol. 2009;50:1198–1202. [Google Scholar]
- 7.Jang H.J., Song W., Suh Y.S., Jeong U.S., Jeon H.G., Jeong B.C. Comparison of perioperative outcomes of robotic versus laparoscopic partial nephrectomy for complex renal tumors (RENAL nephrometry score of 7 or higher) Korean J Urol. 2014;55:808–813. doi: 10.4111/kju.2014.55.12.808. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Kang S.G., Ko Y.H., Jang H.A., Kim J., Kim S.H., Cheon J. Initial experience of robot-assisted radical cystectomy with total intracorporeal urinary diversion: comparison with extracorporeal method. J Laparoendosc Adv Surg Technol A. 2012;22:456–462. doi: 10.1089/lap.2011.0249. [DOI] [PubMed] [Google Scholar]
- 9.Lee Y.S., Han W.K., Yang S.C., Rha K.H. Robot-assisted laparoscopic radical prostatectomy. Korean J Urol. 2006;47:206–210. [Google Scholar]
- 10.Abdel Raheem A., Kim D.K., Santok G.D., Alabdulaali I., Chung B.H., Choi Y.D. Stratified analysis of 800 Asian patients after robot-assisted radical prostatectomy with a median 64 months of follow up. Int J Urol. 2016;23:765–774. doi: 10.1111/iju.13151. [DOI] [PubMed] [Google Scholar]
- 11.Abdel Raheem A., Alatawi A., Kim D.K., Sheikh A., Alabdulaali I., Han W.K. Outcomes of high-complexity renal tumours with a Preoperative Aspects and Dimensions Used for an Anatomical (PADUA) score of ≥10 after robot-assisted partial nephrectomy with a median 46.5-month follow-up: a tertiary centre experience. BJU Int. 2016;118:770–778. doi: 10.1111/bju.13501. [DOI] [PubMed] [Google Scholar]
- 12.Raheem A.A., Santok G.D., Kim D.K., Troya I.S., Alabdulaali I., Choi Y.D. Simultaneous Retzius-sparing robot-assisted radical prostatectomy and partial nephrectomy. Invest Clin Urol. 2016;57:146–149. doi: 10.4111/icu.2016.57.2.146. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Sutton S., Link T., Makic M.B. A quality improvement project for safe and effective patient positioning during robot-assisted surgery. AORN J. 2013;97:448–456. doi: 10.1016/j.aorn.2013.01.014. [DOI] [PubMed] [Google Scholar]
- 14.Zender J., Thell C. Developing a successful robotic surgery program in a rural hospital. AORN J. 2010;92:72–86. doi: 10.1016/j.aorn.2009.10.024. [DOI] [PubMed] [Google Scholar]
- 15.Kaushik D., High R., Clark C.J., LaGrange C.A. Malfunction of the da Vinci robotic system during robot-assisted laparoscopic prostatectomy: an international survey. J Endourol. 2010;24:571–575. doi: 10.1089/end.2009.0489. [DOI] [PubMed] [Google Scholar]
- 16.Tugcu V., Mutlu B., Canda A.E., Sonmezay E., Tasci A.I. Robotic malfunction during live robotic urologic surgery: live surprise in a robotic surgery congress. Arch Ital Urol Androl. 2012;84:211–213. [PubMed] [Google Scholar]
- 17.Borden L.S., Jr., Kozlowski P.M., Porter C.R., Corman J.M. Mechanical failure rate of da Vinci robotic system. Can J Urol. 2007;14:3499–3501. [PubMed] [Google Scholar]
- 18.Lucas S.M., Pattison E.A., Sundaram C.P. Global robotic experience and the type of surgical system impact the types of robotic malfunctions and their clinical consequences: an FDA MAUDE review. BJU Int. 2012;109:1222–1227. doi: 10.1111/j.1464-410X.2011.10692.x. [DOI] [PubMed] [Google Scholar]
- 19.Aconnor M., Areinbolt J., Handley P.J. Perioperative nurse training in cardiothoracic surgical robotics. AORN J. 2001;74:851–857. doi: 10.1016/s0001-2092(06)61503-2. [DOI] [PubMed] [Google Scholar]
- 20.Falcone T., Goldberg J.M. Robotic surgery. Clin Obstetrics Gynecol. 2003;46:37–43. doi: 10.1097/00003081-200303000-00007. [DOI] [PubMed] [Google Scholar]
- 21.Russ S., Rout S., Sevdalis N., Moorthy K., Darzi A., Vincent C. Do safety checklists improve teamwork and communication in the operating room? A systematic review. Ann Surg. 2013;258:856–871. doi: 10.1097/SLA.0000000000000206. [DOI] [PubMed] [Google Scholar]
- 22.Tang R., Ranmuthugala G., Cunningham F. Surgical safety checklists: a review. ANZ J Surg. 2014;84:148–154. doi: 10.1111/ans.12168. [DOI] [PubMed] [Google Scholar]
- 23.Treadwell J.R., Lucas S., Tsou A.Y. Surgical checklists: a systematic review of impacts and implementation. BMJ Qual Saf. 2014;23:299–318. doi: 10.1136/bmjqs-2012-001797. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Huser A.S., Müller D., Brunkhorst V., Kannisto P., Musch M., Kröpfl D. Simulated life-threatening emergency during robot-assisted surgery. J Endourol. 2014;28:717–721. doi: 10.1089/end.2013.0762. [DOI] [PubMed] [Google Scholar]
- 25.Seo Y. Urologic robotic surgery in Korea: past and present. Korean J Urol. 2015;56:546–552. doi: 10.4111/kju.2015.56.8.546. [DOI] [PMC free article] [PubMed] [Google Scholar]