Abstract
Necrotizing enterocolitis (NEC) remains the leading cause of death from gastrointestinal disease in premature infants and attacks the most fragile patients at a time when they appear to be the most stable. Despite significant advances in our overall care of the premature infant, NEC mortality remains stubbornly high. There is no specific treatment for NEC beyond broad-spectrum antibiotics and intestinal resection, and current efforts have focused on preventive strategies. Over the past decade, we have proposed a unifying hypothesis to explain the pathogenesis of NEC in premature infants that suggests that NEC develops in response to an imbalance between exaggerated proinflammatory signaling in the mucosa of the premature gut leading to mucosal injury, which is not countered effectively by endogenous repair processes, and in the setting of impaired mesenteric perfusion leads to intestinal ischemia and disease development. One of the most important pathways that mediates the balance between injury and repair in the premature intestine, and that plays a key role in NEC pathogenesis, is Toll-like receptor 4 (TLR4), which recognizes lipopolysaccharide on gram-negative bacteria. This review focuses on the role that the TLR4-mediated imbalance between proinflammatory and anti-inflammatory signaling in the premature intestinal epithelium leads to the development of NEC, and will explore how an understanding of the role of TLR4 in NEC pathogenesis has led to the identification of novel preventive or treatment approaches for this devastating disease.
Keywords: lneonate, Sepsis, Nutrition, Enterocyte, Microbiome, Probiotic
Abbreviations used in this paper: LPS, lipopolysaccharide; NEC, necrotizing enterocolitis; TLR, Toll-like receptor; TLR4, Toll-like receptor 4
Summary.
We describe the role of Toll-like receptor 4 (TLR4) in the pathogenesis of necrotizing enterocolitis, which is a major cause of morbidity and mortality in premature infants. Through regulation of the intestinal barrier and control of mesenteric perfusion, TLR4 signaling plays a key role in the mechanisms by which exaggerated bacterial signaling leads to ischemia in the premature gut. We now describe how the increased risk of necrotizing enterocolitis in the premature infant may be explained in part by the greater expression of TLR4 in the premature as compared with the full-term intestinal epithelium, which is a consequence of the important role of TLR4 in the regulation of normal intestinal epithelial differentiation. Thus, TLR4-based targeting strategies within the intestine of the premature infant may offer novel preventative or therapeutic approaches for this devastating disease.
If tuberculosis is the master masquerader, coronary artery disease the silent killer, and cancer the number one enemy, then necrotizing enterocolitis (NEC) has to be the doctor’s menace. Striking suddenly, attacking the most fragile of patients at a time when they appear to be the most stable, NEC remains the leading cause of death from gastrointestinal disease in premature infants. Despite significant advances in our overall care of the premature infant, the mortality among those affected by NEC remains stubbornly high.1, 2 Clinically, the presentation of infants with NEC often initially is quite subtle, yet over 24–48 hours progresses to abdominal distention, the passage of bloody stools, and systemic sepsis.3 At laparotomy, which is required in nearly half of all cases of NEC,4 patchy intestinal necrosis of the large and small intestine is detected,5 which occasionally can require extensive resection.6 In those infants who survive the initial onset of disease, long-term complications often develop, including severe inflammatory lung disease,7 which is more severe than the lung disease that develops in premature infants in the absence of NEC,8, 9 neurologic dysfunction,6, 10 and the presence of short-bowel syndrome,11 which is a devastating result of extensive intestinal resection. There is no specific treatment for NEC beyond broad-spectrum antibiotics and intestinal resection,12 and current efforts therefore have focused on preventive strategies,13, 14 which of course offer little solace to those who unfortunately develop the disease. On a positive note, work from a variety of investigators has begun to shed light on some of the key signaling pathways that lead to disease development, and that will form the basis of the current review. We begin by offering a unifying hypothesis for NEC development, which posits that NEC occurs in response to an imbalance between increased injury and reduced mucosal repair within the mucosa of the premature gut.
A Unifying Hypothesis for NEC Development: An Imbalance Between Injury and Repair in the Premature Gut
Over the past decade, we and others have proposed a unifying hypothesis to explain the pathogenesis of NEC in premature infants,15, 16 which is shown in Figure 1. In brief, as will be described in greater detail later, available evidence suggests that NEC develops in response to an imbalance between exaggerated proinflammatory signaling in the mucosa of the premature gut leading to mucosal injury, which is not countered effectively by endogenous repair processes, and in the setting of impaired mesenteric perfusion leads to intestinal ischemia and disease development. One of the most important pathways that mediates the balance between injury and repair in the premature intestine, and that plays a key role in NEC pathogenesis, is the Toll-like receptor (TLR) family of bacterial recognition receptors, specifically Toll-like receptor 4 (TLR4), which recognizes lipopolysaccharide (LPS) on gram-negative bacteria.17 Key evidence linking TLR4 with the pathogenesis of NEC include the findings that the expression of TLR4 in the intestinal epithelium is increased in mice and human beings with NEC,18, 19 activating mutations in TLR4 signaling pathways are seen in human NEC,20, 21, 22, 23 and novel TLR4 inhibitors prevent and treat NEC in animal models and attenuate proinflammatory signaling in human NEC tissue ex vivo,24 whereas mice lacking TLR4 in the intestinal epithelium are protected from NEC development.25 It is noteworthy that there are other pathways that also play a role in the pathogenesis of NEC, many of which are downstream of TLR4, and these have been reviewed extensively by us recently elsewhere,15 while other investigators have shown that the premature intestine is more prone to inflammation26 in part through the expression of innate immune response genes including TLR4 and its gene family members,27 which is supportive of this concept. This review focuses on the role that the TLR4-mediated imbalance between proinflammatory and anti-inflammatory signaling in the premature intestinal epithelium leads to the development of NEC, and explores how an understanding of the role of TLR4 in NEC pathogenesis has led to novel preventative or treatment approaches for this devastating disease.
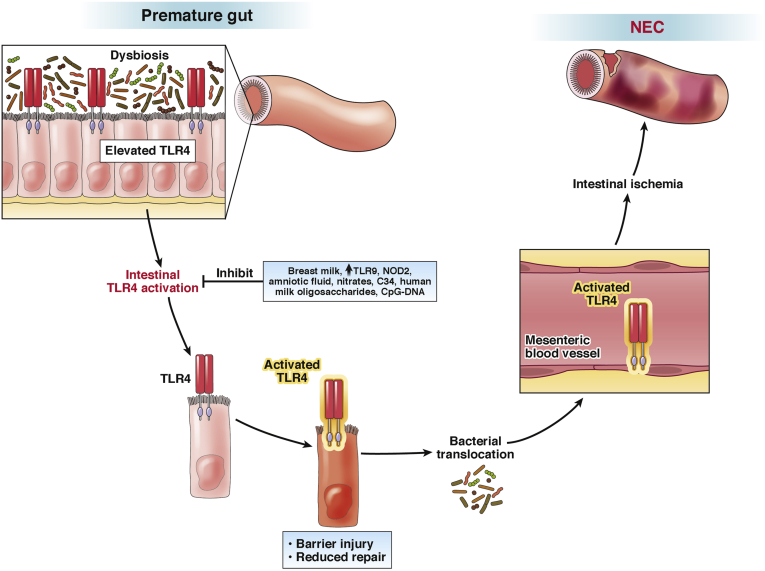
Figure 1.
The role of TLR4 in the pathogenesis of NEC. The premature infant gut is characterized by elevated expression of TLR4 on the intestinal epithelium, which is a function of the role of TLR4 in regulation of normal intestinal epithelial development. Activation of TLR4 by microbes within the intestinal lumen leads to barrier injury and impaired repair, resulting in translocation of luminal bacteria, which then interact with TLR4 on the lining of the mesenteric blood vessels, resulting in vasoconstriction and intestinal ischemia and NEC. Importantly, intestinal TLR4 is inhibited by factors including probiotic bacteria whose DNA can activate TLR9, as well as human milk oligosaccharides and other components of breast milk, while the provision of nitrates can induce mesenteric vasodilation and counter the negative effects of endothelial TLR4 activation on gut perfusion.
Clinical Risk Factors for NEC
To understand the cellular and biological processes that lead to NEC, we first review the clinical risk factors known to be associated with this disease, and then seek to correlate these clinical observations with the underlying biological pathways involved. In more than 90% of cases, NEC develops in premature infants (ie, those born before 37 weeks' gestational age), indicating that NEC is fairly specific to the underdeveloped gastrointestinal tract.2, 28 Intestinal bacteria are linked to the development of NEC because NEC occurs after colonization of the intestine has occurred, although NEC is treated with broad-spectrum antibiotics that target enteric microbes,29, 30, 31 suggesting that bacterial–host signaling plays a role in NEC development. Specific clinical risk factors for NEC include the administration of acid-suppressive H2 blockers,32, 33, 34 excessive antibiotic use,35 brief episodes of hypoxia,36 the presence of chorio-amnionitis (an infection of the lining of the uterine cavity during gestation),37 and the administration of formula feeds.38, 39 The administration of breast milk is highly protective against NEC,40, 41 a finding that has provided the rationale for the use of donor breast milk as a specific preventive strategy,42, 43 and that suggests that it may be the absence of breast milk rather than the presence of formula that is most important in NEC pathogenesis. It is noteworthy that each of the earlier-described clinical risk factors for NEC is linked indirectly by the induction or maintenance of a proinflammatory microenvironment in the newborn intestine. The premature intestine itself has been shown in ex vivo studies to exist in a proinflammatory state, as shown by the induction of a proinflammatory reaction to external bacteria as compared with the full-term bowel.26, 27, 44 Likewise, the presence of H2 blockers, chorioamnionitis, formula administration, and the use of broad-spectrum antibiotics all may be expected to contribute to the development of a dysbiotic microbiome, which has been linked to NEC development.31 Taken together, clinical risk factors for NEC each serve to induce a proinflammatory microenvironment in the premature host intestine, and in response to colonizing bacteria lead to NEC, through pathways that will be explored in additional detail later.
Why NEC Is Not Just Inflammatory Bowel Disease in Premature Infants
In seeking to understand the pathogenesis of NEC, and to develop novel approaches for the treatment of this devastating disease, it is important to understand not only what NEC is, but also what NEC is not. A common misconception is that NEC is quite simply Crohn's disease as seen in the premature infant. Although NEC does share some pathogenetic similarities with inflammatory bowel disease—including an associative role for a dysbiotic microbiome, an imbalance between proinflammatory and anti-inflammatory cells in the intestinal mucosa, a genetic predisposition, and a predilection for the terminal ileum and cecum45, 46, 47—the 2 diseases are very different. Specifically, Crohn's disease is characterized by the full-thickness involvement of parts of the small and large intestine, is a relapsing condition that may be associated with fistularization, is not associated with intestinal necrosis, and rarely is associated with sepsis or death.48, 49 By contrast, NEC is associated characteristically with necrosis of either the small or large intestine, is an acute disease, and leads to overwhelming sepsis and death in more than 30% of cases.50, 51, 52 Histologically, Crohn's disease is characterized by an influx of polymorphonuclear leukocytes and crypt abscesses in association with regions of fibrosis, although NEC is associated with an influx of lymphocytes and macrophages, vascular thrombosis, and mucosal edema.18, 53 In mouse models, the lack of TLR4 protects against experimental NEC,25 whereas mice lacking TLR4 have more severe colitis,54 reflecting differences in the molecular mechanisms that drive the disease. Thus, although Crohn's disease and NEC share certain clinical features, each is a unique intestinal inflammatory disease.
Toll-Like Receptor Activation Leads to NEC Development by Inducing Intestinal Injury and Reducing Mucosal Repair in the Premature Intestine
TLRs are innate immune receptors that contribute to host defense by initiating an inflammatory response to conserved microbial patterns that are expressed in both invading pathogens and commensal microorganisms.55 TLR4 on leukocytes is activated by LPS on the surface of gram-negative bacteria, which leads to the recruitment of the accessory molecules myeloid differentiation primary response 88 or Toll/interleukin 1–receptor domain–containing adapter inducing interferon β, the induction of the transcription factors nuclear factor-κ-light-chain–enhancer of activated B cells or interferon regulatory factor 3, and the eventual elimination of the invading microbe.56 Although TLR4 has a signature role in host defense through its expression on immune cells, we and others have shown that TLR4 also is expressed on the intestinal epithelium, where it regulates intestinal epithelial apoptosis and migration, and proliferation, and thus contributes to the pathogenesis of NEC.19, 22, 25, 57, 58, 59, 60, 61, 62, 63 Evidence for a role for TLR4 in human NEC from a variety of investigators includes the observations that levels of expression of TLR4 messenger RNA and protein are both significantly higher in the intestine of patients with NEC as compared with control patients, while activating mutations in the TLR4 signaling pathway are found in a greater proportion of premature infants with NEC as compared with those without this disease. These findings suggest but by no means prove the fact that TLR4 activation plays a role in NEC development. To interrogate the role of TLR4 in NEC development, we and others have turned to animal models, using mice, rats, and piglets. Induction of NEC in mice and rats typically requires daily administration of infant formula, often supplemented with bacteria in the setting of daily episodes of hypoxia and/or hypothermia, to mimic the clinical situation of apneas/bradycardic spells experienced by these neonates.64, 65 After 4 days, wild-type mice and rats develop patchy intestinal edema, inflammation, and necrosis, which closely resembles human NEC.19, 65, 66, 67, 68 By contrast, mice lacking TLR4, including either the TLR4-/- mouse and the C3H/HeJ mouse with an inactivating mutation in the TLR4 gene,19, 63 are protected from NEC development. Although the intermittent hypoxia/formula feeding model recapitulates some of the features of NEC, there are some limitations, including the fact that not all mice develop the disease, and the model is technically difficult to perform; we have modified the model by gavaging with stool from an infant with severe NEC to induce a more consistent and severe phenotype that replicates the human disease. Several investigators have provided an analysis of the various models for NEC,64, 65 which allows for an assessment of model selection appropriate to the experimental questions.
In seeking to determine whether TLR4 on the intestinal epithelium as opposed to other cell types is required for the pathogenesis of NEC, we have shown that mice lacking TLR4 on the intestinal epithelium, as opposed to other cell types, is required for the development of NEC because TLR4-:Δ-villin-/- deficient mice lacking TLR4 on the intestinal epithelium are protected from the development of NEC.25 TLR4 signaling on enterocytes leads to cell death via apoptosis,19, 62, 69 findings that were confirmed both in vitro and in vivo. Given that the induction of enterocyte apoptosis precedes intestinal injury in NEC,70 TLR4-induced cell death by apoptosis is thought to be an early event in the mucosal injury that characterizes this disease.71 Healing from mucosal injury in the intestine occurs first through the process of restitution, which involves the migration of healthy enterocytes to the injured site, followed by proliferation of new cells from stem cells housed within the intestinal crypts, which together restore the mucosal barrier.72 We have shown that TLR4 activation leads to a direct inhibition of mucosal repair via reduced enterocyte migration, through a mechanism that requires the activation of focal adhesions, and the induction of integrins.68, 73, 74 TLR4 activation also was found to lead to reduced proliferation of the Leucine-rich repeat-containing G-protein coupled receptor 5 (Lgr5) expressing stem cell pool in the intestinal crypts via mechanisms that involve the inhibition of β catenin signaling75 and the up-regulation of the proapoptotic mediator p53 up-regulated modulator of apoptosis76 directly on the stem cells. The intestine in mouse and human NEC was noted to be rich in proinflammatory T helper 17 cell (Th17) lymphocytes, whose influx into the newborn gut required enterocyte TLR4 signaling, and which were required for NEC development because lymphocyte-deficient Rag1-/- mice were protected from NEC, and transfer of intestinal lymphocytes from NEC-mice into naive mice induced intestinal inflammation.18 In further studies, we showed that the normal lymphocyte balance within the lamina propria of the intestine can be achieved by the administration of all-trans retinoic acid, which restored mucosal integrity by preventing the loss of intestinal stem cells, which richly express TLR4.77 These findings support earlier work, showing the importance of the adaptive immune system in the pathogenesis of NEC.78, 79, 80, 81
After mucosal injury, bacterial translocation leads to the entry of lipopolysaccharides into the bloodstream, where TLR4 signaling in the endothelium of the intestinal mesentery leads to a reduction in the expression of endothelial nitric oxide synthase, which is an enzyme responsible for the generation of the vasodilatory molecule nitric oxide, which contributed to the intestinal ischemia in NEC.82 The intestinal mesentery of the premature infant is not designed to receive food, given that the natural environment of the premature gut is still in utero. For this reason, its mesentery is relatively vasoconstricted in a process that involves the vasodilator nitric oxide (which is reduced in NEC) and the vasoconstrictor endothelin-1 (which is increased in NEC).83, 84, 85 It is noteworthy that breast milk is enriched in nitric oxide precursor sodium nitrates,82 suggesting one mechanism by which breast milk administration can prevent NEC, a mechanism that also is shared by human milk oligosaccharides, which are present in breast milk and whose absorption into the circulation can enhance nitric oxide release,86 thus counteracting the effects of TLR4 signaling on the mesenteric endothelium.
Taken together, these findings illustrate that TLR4 signaling in the intestinal mucosa leads to NEC through inducing mucosal injury and preventing mucosal repair. Although such observations provide insights into NEC pathogenesis, they also lead to several important questions, including why a receptor that has a role in host defense actually leads to disease development, and what pathways are in place within the host to prevent the exaggerated TLR4 signaling that leads to NEC. These questions are addressed in further detail later.
A Role for TLR4 in Intestinal Development
The earlier-described studies raise questions regarding why a receptor involved in host defense would lead to the development of disease. In addressing this seeming inconsistency, we investigated the expression of TLR4 on the intestine of mice during intestinal development, and noted a progressive increase in messenger RNA expression that peaked at the time of full-term gestation.16, 87 This is a surprising result given the fact that the intestine develops in the relatively sterile environment of the womb, and certainly in the absence of enteric microbes that only colonize the gut in the postnatal period.88 In a series of additional studies, we determined that TLR4 expression in the intestinal epithelium is required for normal gut development because TLR4-:Δ-villin-/- deficient mice lacking TLR4 on the intestinal epithelium show abnormal intestinal epithelial progeny, characterized by an abundance of goblet cells.25, 76 This finding is reflective of the observation that TLR4 is expressed predominantly in the Lgr5-positive intestinal stem cells where its activation leads to activation of Notch signaling and impaired differentiation of stem cells toward goblet cells.25, 76 It is noteworthy that human NEC is known to be characterized by a depletion of goblet cells in the intestinal epithelium, which is consistent with the exaggerated TLR4 activation that leads to NEC,89 and also with the finding that pharmacologic Notch inhibition restores goblet cells and attenuates NEC severity in mice cells.25 Taken together, these findings illustrate that TLR4 has a primary unexpected role in intestinal stem cell signaling and differentiation, and that the premature gut, which is still developing, expresses significantly higher levels of TLR4 as compared with its wild-type counterparts as a reflection of this increased expression. Subsequently, the delivery of the premature infant with expectedly higher levels of TLR4 in the intestinal epithelium, as a consequence of the ongoing gut development, results in activation of TLR4 by colonizing microbes, which then induces the imbalance between injury and repair that leads to NEC as described earlier. The observation that a receptor that is required for gut development also would recognize enteric microbes is consistent with findings in drosophila, where TLR4 was first identified, in which its homolog Toll was found to have a primary role in body wall development as well as in host immunity. These findings raise the question as to what curtails TLR4 signaling in the gastrointestinal tract, and further, suggests the possibility that therapeutic or preventative strategies for NEC may be developed based on limiting the extent of TLR4 signaling in the premature gut. These are discussed in greater detail later.
Restraining TLR4 Signaling in the Gastrointestinal Tract: nucleotide oligomerization domain-containing protein2, TLR9, and Amniotic Fluid
The finding that exaggerated TLR4 signaling in the intestinal epithelium leads to NEC raises the possibility that counter-regulatory pathways exist that limit the extent of TLR4 signaling in the newborn intestine, and thus reduce the propensity for NEC development. In support of this possibility, TLR9, a homologous receptor to TLR4 that is activated by bacterial DNA, can limit TLR4 signaling through activation of the inhibitory molecule interleukin-1 receptor associated kinase-m.90, 91, 92, 93 Human beings and mice with NEC have reduced expression of TLR9 in the gut (and increased TLR4), suggesting that a lack of protective TLR9 could lead to NEC.87 Furthermore, it is noteworthy that the administration of probiotic bacteria has been shown to limit the severity of NEC in mice and human beings,94 although additional studies have shown that mice lacking TLR9 did not show protection, whereas administration of bacterial DNA yielded similar protection in mice, raising the possibility that the protective mechanism of probiotic bacteria involved activation of TLR9 by bacterial DNA and reciprocal inhibition of TLR4.95 In additional studies, activation of nucleotide oligomerization domain-containing protein2, which has an essential role in familial Crohn's disease,96 reduced NEC severity by reducing TLR4 downstream pathways, and was reduced itself in the intestines of mice and human beings with NEC.97 It is interesting to note that in the developing intestine, the amniotic fluid that bathes the lumen of the fetal intestine was found to prevent TLR4 activation, and the administration of amniotic fluid in animal models reduced NEC severity, providing additional proof of concept of these findings.82 These findings support the over-riding precept that modulation of TLR4 signaling in the intestinal epithelium determines the balance between injury and repair in the pathogenesis of NEC.
Breast Milk and NEC
One of the most important strategies known to protect against the development of NEC is the administration of breast milk, which is protective when even small amounts are administered.98, 99, 100, 101 This observation has led to significant interest in seeking to understand the molecular components of breast milk that confer protection against NEC. Earlier studies have focused on the presence of immunoprotective IgA,102 lactoferrin,103 and erythropoietin.104 More recent studies have focused on probiotic bacteria within breast milk,105 and the nondigestible human milk oligosaccharides that are present in breast milk and reduce NEC through inhibition of bacterial enterocyte binding and enhanced mucosal perfusion.86, 106, 107, 108 More recently, we determined that breast milk contains powerful TLR4 inhibitory properties, including the major growth factor epidermal growth factor, which inhibits TLR4 signaling via activation of the phosphoinositide 3-K signaling pathway, suggesting an additional mechanism of NEC prevention.101 In support of this observation, treatment of mice with breast milk prevented NEC while administration of breast milk in which epidermal growth factor had been immune-depleted failed to offer protection. In addition, as mentioned earlier, breast milk is rich in sodium nitrates, which are important precursors of nitric oxide, whose administration leads to enhanced mesenteric perfusion and protection of the gut from ischemic injury.82 Taken together, these findings provide evidence regarding the mechanisms by which breast milk prevents NEC, provide additional evidence linking TLR4 activation to NEC pathogenesis, and provide support to the concept that NEC develops in a proinflammatory environment that can be reversed in part through factors present in breast milk.
Drug Discovery and NEC
The studies described earlier show not only an important role for TLR4 in the pathogenesis of NEC, but also raise possible approaches for either preventing or treating this disease. Based on the structure of TLR4 bound to the synthetic inhibitor E5564,109, 110 we conducted an in silico search for novel TLR4 inhibitors, and then evaluated their potential role in the prevention or treatment of NEC. Using a similarity search algorithm in conjunction followed by screening of small-molecule libraries, we identified a family of TLR4 inhibitors, many of which were detectable in breast milk.24 Importantly, our lead compound, C34, is a 2-acetamidopyranoside (molecular weight, 389) with the formula C17H27NO9, which reduced NEC in animal models and inhibited LPS signaling ex vivo in human ileum that was resected from infants with necrotizing enterocolitis.24 These findings identify C34 and the β-anomeric cyclohexyl analog C35 as novel leads for small-molecule TLR4 inhibitors that have potential therapeutic benefit for TLR4-mediated inflammatory diseases. Additional studies are underway to develop novel approaches to the prevention and treatment of NEC, based in part on the method of inhibition of TLR4 activation and its consequences.
Summary: What Is Next in NEC Research?
This review has sought to review the major role played by TLR4 signaling in the pathogenesis of NEC through its essential roles in the balance between injury and repair in the premature gut. Although other pathways play essential roles, and have been reviewed recently,15 the current studies provide a rationale for the development of NEC preventive strategies based on the modulation of TLR4 signaling. We also reviewed the potential reasons for which the premature infant is at risk for NEC development through an understanding of the increased expression of TLR4 in the intestinal epithelium, a consequence of the essential role played by TLR4 in normal intestinal development. These studies also provide a rationale for studying TLR4 inhibitory molecules as novel preventive or therapeutic approaches for NEC, and rely in part on the knowledge that breast milk is endowed with anti-TLR4 substrates, a fluid with an established role in NEC prevention. Future directions in NEC research may focus on factors that place the premature infant at risk for NEC development, a greater understanding of the genetic factors leading to NEC and how this information may be used to develop NEC treatment or prevention strategies, as well as focusing on more sensitive and specific diagnostic modalities for NEC, including appropriate serum or stool biomarkers, some of which may lie in TLR4 activation pathways. It is our hope that by focusing on these important questions, we will not only gain a greater understanding of NEC, but will reach a day when this disease is no longer the curse it currently is to these fragile patients and their families.
Footnotes
Author contributions David J. Hackam and Chhinder P. Sodhi both researched, wrote, edited, and revised the manuscript and Figure.
Conflicts of interest The authors disclose the following: David J. Hackam holds patents in the use of Toll-like receptor 4 antagonists in the prevention and treatment of necrotizing enterocolitis, and has received a research grant from Abbott Nutrition; Chhinder P. Sodhi holds patents in the use of Toll-like receptor 4 antagonists in the prevention and treatment of necrotizing enterocolitis.
Funding Supported by R01GM078238 and R01DK083752 from the National Institutes of Health (D.J.H.).
Supplementary Material
Supplemental Graphical Summary.
References
- 1.Boghossian N.S., Geraci M., Edwards E.M., Horbar J.D. Morbidity and mortality in small for gestational age infants at 22 to 29 weeks' gestation. Pediatrics. 2018;141:e20172533. doi: 10.1542/peds.2017-2533. [DOI] [PubMed] [Google Scholar]
- 2.Battersby C., Santhalingam T., Costeloe K., Modi N. Incidence of neonatal necrotising enterocolitis in high-income countries: a systematic review. Arch Dis Child Fetal Neonatal Ed. 2018;103:F182–F189. doi: 10.1136/archdischild-2017-313880. [DOI] [PubMed] [Google Scholar]
- 3.Sharma R., Hudak M.L. A clinical perspective of necrotizing enterocolitis: past, present, and future. Clin Perinatol. 2013;40:27–51. doi: 10.1016/j.clp.2012.12.012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Bhatt D., Travers C., Patel R.M., Shinnick J., Arps K., Keene S., Raval M.V. Predicting mortality or intestinal failure in infants with surgical necrotizing enterocolitis. J Pediatr. 2017;191:22–27.e3. doi: 10.1016/j.jpeds.2017.08.046. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Omarsdottir S., Agnarsdottir M., Casper C., Orrego A., Vanpee M., Rahbar A., Söderberg-Nauclér C. High prevalence of cytomegalovirus infection in surgical intestinal specimens from infants with necrotizing enterocolitis and spontaneous intestinal perforation: a retrospective observational study. J Clin Virol. 2017;93:57–64. doi: 10.1016/j.jcv.2017.05.022. [DOI] [PubMed] [Google Scholar]
- 6.Batra A., Keys S.C., Johnson M.J., Wheeler R.A., Beattie R.M. Epidemiology, management and outcome of ultrashort bowel syndrome in infancy. Arch Dis Child Fetal Neonatal Ed. 2017;102:F551–F556. doi: 10.1136/archdischild-2016-311765. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Laughon M., O'Shea M.T., Allred E.N., Bose C., Kuban K., Van Marter L.J., Ehrenkranz R.A., Leviton A. Chronic lung disease and developmental delay at 2 years of age in children born before 28 weeks' gestation. Pediatrics. 2009;124:637–648. doi: 10.1542/peds.2008-2874. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Ganapathy V., Hay J.W., Kim J.H., Lee M.L., Rechtman D.J. Long term healthcare costs of infants who survived neonatal necrotizing enterocolitis: a retrospective longitudinal study among infants enrolled in Texas Medicaid. BMC Pediatr. 2013;13:127. doi: 10.1186/1471-2431-13-127. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Fernandez R., D'Apremont I., Dominguez A., Tapia J.L. Survival and morbidity of very low birth weight infant in a South American neonatal network. Arch Argent Pediatr. 2014;112:405–412. doi: 10.5546/aap.2014.eng.405. [DOI] [PubMed] [Google Scholar]
- 10.Hintz S.R., Kendrick D.E., Stoll B.J., Vohr B.R., Fanaroff A.A., Donovan E.F., Poole W.K., Blakely M.L., Wright L., Higgins R. Neurodevelopmental and growth outcomes of extremely low birth weight infants after necrotizing enterocolitis. Pediatrics. 2005;115:696–703. doi: 10.1542/peds.2004-0569. [DOI] [PubMed] [Google Scholar]
- 11.Totonelli G., Tambucci R., Boscarelli A., Hermans D., Dall'Oglio L., Diamanti A., d'Aische A.D.B., Pakarinen M., Reding R., Morini F., Bagolan P., Fusaro F. Pediatric intestinal rehabilitation and transplantation registry: initial report from a European Collaborative Registry. Eur J Pediatr Surg. 2018;28:75–80. doi: 10.1055/s-0037-1605349. [DOI] [PubMed] [Google Scholar]
- 12.Valpacos M., Arni D., Keir A., Aspirot A., Wilde J.C.H., Beasley S., De Luca D., Pfister R.E., Karam O. Diagnosis and management of necrotizing enterocolitis: an international survey of neonatologists and pediatric surgeons. Neonatology. 2017;113:170–176. doi: 10.1159/000484197. [DOI] [PubMed] [Google Scholar]
- 13.Briana D.D. Enteral l-arginine supplementation for prevention of necrotizing enterocolitis in premature infants. J Matern Fetal Neonatal Med. 2018 doi: 10.1080/14767058.2018.1428552. Epub ahead of print. [DOI] [PubMed] [Google Scholar]
- 14.Gephart S.M., Hanson C., Wetzel C.M., Fleiner M., Umberger E., Martin L., Rao S., Agrawal A., Marin T., Kirmani K., Quinn M., Quinn J., Dudding K.M., Clay T., Sauberan J., Eskenazi Y., Porter C., Msowoya A.L., Wyles C., Avenado-Ruiz M., Vo S., Reber K.M., Duchon J. NEC-zero recommendations from scoping review of evidence to prevent and foster timely recognition of necrotizing enterocolitis. Matern Health Neonatol Perinatol. 2017;3:23. doi: 10.1186/s40748-017-0062-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Nino D.F., Sodhi C.P., Hackam D.J. Necrotizing enterocolitis: new insights into pathogenesis and mechanisms. Nat Rev Gastroenterol Hepatol. 2016;13:590–600. doi: 10.1038/nrgastro.2016.119. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Hackam D., Caplan M. Necrotizing enterocolitis: pathophysiology from a historical context. Semin Pediatr Surg. 2018;27:11–18. doi: 10.1053/j.sempedsurg.2017.11.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Kuzmich N.N., Sivak K.V., Chubarev V.N., Porozov Y.B., Savateeva-Lyubimova T.N., Peri F. TLR4 signaling pathway modulators as potential therapeutics in inflammation and sepsis. Vaccines (Basel) 2017;5:4. doi: 10.3390/vaccines5040034. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Egan C.E., Sodhi C.P., Good M., Lin J., Jia H., Yamaguchi Y., Lu P., Ma C., Branca M.F., Weyandt S., Fulton W.B., Niño D.F., Prindle T., Jr., Ozolek J.A., Hackam D.J. Toll-like receptor 4-mediated lymphocyte influx induces neonatal necrotizing enterocolitis. J Clin Invest. 2016;126:495–508. doi: 10.1172/JCI83356. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Leaphart C.L., Cavallo J.C., Gribar S.C., Cetin S., Li J., Branca M.F., Dubowski T.D., Sodhi C.P., Hackam D.J. A critical role for TLR4 in the pathogenesis of necrotizing enterocolitis by modulating intestinal injury and repair. J Immunol. 2007;179:4808–4820. doi: 10.4049/jimmunol.179.7.4808. [DOI] [PubMed] [Google Scholar]
- 20.Sampath V., Menden H., Helbling D., Li K., Gastonguay A., Ramchandran R., Dimmock D.P. SIGIRR genetic variants in premature infants with necrotizing enterocolitis. Pediatrics. 2015;135:e1530–e1534. doi: 10.1542/peds.2014-3386. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Fawley J., Cuna A., Menden H.L., McElroy S., Umar S., Welak S.R., Gourlay D.M., Li X., Sampath V. Immunoglobulin Interleukin-1-related receptor regulates vulnerability to TLR4-mediated necrotizing enterocolitis in a mouse model. Pediatr Res. 2018;83:164–174. doi: 10.1038/pr.2017.211. [DOI] [PubMed] [Google Scholar]
- 22.Wu W., Wang Y., Zou J., Long F., Yan H., Zeng L., Chen Y. Bifidobacterium adolescentis protects against necrotizing enterocolitis and upregulates TOLLIP and SIGIRR in premature neonatal rats. BMC Pediatr. 2017;17:1. doi: 10.1186/s12887-016-0759-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Ganguli K., Meng D., Rautava S., Lu L., Walker W.A., Nanthakumar N. Probiotics prevent necrotizing enterocolitis by modulating enterocyte genes that regulate innate immune-mediated inflammation. Am J Physiol Gastrointest Liver Physiol. 2013;304:G132–G141. doi: 10.1152/ajpgi.00142.2012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Neal M.D., Jia H., Eyer B., Good M., Guerriero C.J., Sodhi C.P., Afrazi A., Prindle T., Jr., Ma C., Branca M., Ozolek J., Brodsky J.L., Wipf P., Hackam D.J. Discovery and validation of a new class of small molecule Toll-like receptor 4 (TLR4) inhibitors. PLoS One. 2013;8:e65779. doi: 10.1371/journal.pone.0065779. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Sodhi C.P., Neal M.D., Siggers R., Sho S., Ma C., Branca M.F., Prindle T., Jr., Russo A.M., Afrazi A., Good M., Brower-Sinning R., Firek B., Morowitz M.J., Ozolek J.A., Gittes G.K., Billiar T.R., Hackam D.J. Intestinal epithelial Toll-like receptor 4 regulates goblet cell development and is required for necrotizing enterocolitis in mice. Gastroenterology. 2012;143:708–718. doi: 10.1053/j.gastro.2012.05.053. e1–5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Nanthakumar N.N., Fusunyan R.D., Sanderson I., Walker W.A. Inflammation in the developing human intestine: a possible pathophysiologic contribution to necrotizing enterocolitis. Proc Natl Acad Sci U S A. 2000;97:6043–6048. doi: 10.1073/pnas.97.11.6043. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Nanthakumar N., Meng D., Goldstein A.M., Zhu W., Lu L., Uauy R., Llanos A., Claud E.C., Walker W.A. The mechanism of excessive intestinal inflammation in necrotizing enterocolitis: an immature innate immune response. PLoS One. 2011;6:e17776. doi: 10.1371/journal.pone.0017776. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Patel S., Chaudhari M., Kadam S., Rao S., Patole S. Standardized feeding and probiotic supplementation for reducing necrotizing enterocolitis in preterm infants in a resource limited set up. Eur J Clin Nutr. 2018;72:281–287. doi: 10.1038/s41430-017-0040-7. [DOI] [PubMed] [Google Scholar]
- 29.Patel R.M., Underwood M.A. Probiotics and necrotizing enterocolitis. Semin Pediatr Surg. 2018;27:39–46. doi: 10.1053/j.sempedsurg.2017.11.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Itani T., Ayoub Moubareck C., Melki I., Rousseau C., Mangin I., Butel M.J., Karam-Sarkis D. Preterm infants with necrotising enterocolitis demonstrate an unbalanced gut microbiota. Acta Paediatr. 2018;107:40–47. doi: 10.1111/apa.14078. [DOI] [PubMed] [Google Scholar]
- 31.Warner B.B., Deych E., Zhou Y., Hall-Moore C., Weinstock G.M., Sodergren E., Shaikh N., Hoffmann J.A., Linneman L.A., Hamvas A., Khanna G., Rouggly-Nickless L.C., Ndao I.M., Shands B.A., Escobedo M., Sullivan J.E., Radmacher P.G., Shannon W.D., Tarr P.I. Gut bacteria dysbiosis and necrotising enterocolitis in very low birthweight infants: a prospective case-control study. Lancet. 2016;387:1928–1936. doi: 10.1016/S0140-6736(16)00081-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Talavera M.M., Bixler G., Cozzi C., Dail J., Miller R.R., McClead R., Jr., Reber K. Quality improvement initiative to reduce the necrotizing enterocolitis rate in premature infants. Pediatrics. 2016;137:5. doi: 10.1542/peds.2015-1119. [DOI] [PubMed] [Google Scholar]
- 33.Romaine A., Ye D., Ao Z., Fang F., Johnson O., Blake T., Benjamin D.K., Jr., Cotten C.M., Testoni D., Clark R.H., Chu V.H., Smith P.B., Hornik C.P. Safety of histamine-2 receptor blockers in hospitalized VLBW infants. Early Hum Dev. 2016;99:27–30. doi: 10.1016/j.earlhumdev.2016.05.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Gane B., Bhat B.V., Adhisivam B., Joy R., Prasadkumar P., Femitha P., Shruti B. Risk factors and outcome in neonatal necrotising enterocolitis. Indian J Pediatr. 2014;81:425–428. doi: 10.1007/s12098-013-1311-5. [DOI] [PubMed] [Google Scholar]
- 35.Tzialla C., Borghesi A., Perotti G.F., Garofoli F., Manzoni P., Stronati M. Use and misuse of antibiotics in the neonatal intensive care unit. J Matern Fetal Neonatal Med. 2012;25(Suppl 4):35–37. doi: 10.3109/14767058.2012.714987. [DOI] [PubMed] [Google Scholar]
- 36.Chen Y., Chang K.T., Lian D.W., Lu H., Roy S., Laksmi N.K., Low Y., Krishnaswamy G., Pierro A., Ong C.C. The role of ischemia in necrotizing enterocolitis. J Pediatr Surg. 2016;51:1255–1261. doi: 10.1016/j.jpedsurg.2015.12.015. [DOI] [PubMed] [Google Scholar]
- 37.Lee J.Y., Park K.H., Kim A., Yang H.R., Jung E.Y., Cho S.H. Maternal and placental risk factors for developing necrotizing enterocolitis in very preterm infants. Pediatr Neonatol. 2017;58:57–62. doi: 10.1016/j.pedneo.2016.01.005. [DOI] [PubMed] [Google Scholar]
- 38.Pammi M., Suresh G. Enteral lactoferrin supplementation for prevention of sepsis and necrotizing enterocolitis in preterm infants. Cochrane Database Syst Rev. 2017;6:CD007137. doi: 10.1002/14651858.CD007137.pub5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Good M., Sodhi C.P., Hackam D.J. Evidence-based feeding strategies before and after the development of necrotizing enterocolitis. Exp Rev Clin Immunol. 2014;10:875–884. doi: 10.1586/1744666X.2014.913481. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Patel A.L., Kim J.H. Human milk and necrotizing enterocolitis. Semin Pediatr Surg. 2018;27:34–38. doi: 10.1053/j.sempedsurg.2017.11.007. [DOI] [PubMed] [Google Scholar]
- 41.Cortez J., Makker K., Kraemer D.F., Neu J., Sharma R., Hudak M.L. Maternal milk feedings reduce sepsis, necrotizing enterocolitis and improve outcomes of premature infants. J Perinatol. 2018;38:71–74. doi: 10.1038/jp.2017.149. [DOI] [PubMed] [Google Scholar]
- 42.Buckle A., Taylor C. Cost and cost-effectiveness of donor human milk to prevent necrotizing enterocolitis: systematic review. Breastfeed Med. 2017;12:528–536. doi: 10.1089/bfm.2017.0057. [DOI] [PubMed] [Google Scholar]
- 43.Adhisivam B., Vishnu Bhat B., Banupriya N., Poorna R., Plakkal N., Palanivel C. Impact of human milk banking on neonatal mortality, necrotizing enterocolitis, and exclusive breastfeeding - experience from a tertiary care teaching hospital, south India. J Matern Fetal Neonatal Med. 2017 doi: 10.1080/14767058.2017.1395012. Epub ahead of print. [DOI] [PubMed] [Google Scholar]
- 44.Claud E.C., Walker W.A. Hypothesis: inappropriate colonization of the premature intestine can cause neonatal necrotizing enterocolitis. FASEB J. 2001;15:1398–1403. doi: 10.1096/fj.00-0833hyp. [DOI] [PubMed] [Google Scholar]
- 45.Weimers P., Munkholm P. The natural history of IBD: lessons learned. Curr Treat Options Gastroenterol. 2018;16:101–111. doi: 10.1007/s11938-018-0173-3. [DOI] [PubMed] [Google Scholar]
- 46.Li N., Shi R.H. Updated review on immune factors in pathogenesis of Crohn's disease. World J Gastroenterol. 2018;24:15–22. doi: 10.3748/wjg.v24.i1.15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Jiang H., Shen J., Ran Z. Epithelial-mesenchymal transition in Crohn's disease. Mucosal Immunol. 2018;11:294–303. doi: 10.1038/mi.2017.107. [DOI] [PubMed] [Google Scholar]
- 48.Wibmer A.G., Kroesen A.J., Grone J., Buhr H.J., Ritz J.P. Comparison of strictureplasty and endoscopic balloon dilatation for stricturing Crohn's disease–review of the literature. Int J Colorectal Dis. 2010;25:1149–1157. doi: 10.1007/s00384-010-1010-x. [DOI] [PubMed] [Google Scholar]
- 49.Ma C., Moran G.W., Benchimol E.I., Targownik L.E., Heitman S.J., Hubbard J.N., Seow C.H., Novak K.L., Ghosh S., Panaccione R., Kaplan G.G. Surgical rates for Crohn's disease are decreasing: a population-based time trend analysis and validation study. Am J Gastroenterol. 2017;112:1840–1848. doi: 10.1038/ajg.2017.394. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Neu J., Pammi M. Pathogenesis of NEC: impact of an altered intestinal microbiome. Semin Perinatol. 2017;41:29–35. doi: 10.1053/j.semperi.2016.09.015. [DOI] [PubMed] [Google Scholar]
- 51.Frost B.L., Modi B.P., Jaksic T., Caplan M.S. New medical and surgical insights into neonatal necrotizing enterocolitis: a review. JAMA Pediatr. 2017;171:83–88. doi: 10.1001/jamapediatrics.2016.2708. [DOI] [PubMed] [Google Scholar]
- 52.Moss R.L., Dimmitt R.A., Barnhart D.C., Sylvester K.G., Brown R.L., Powell D.M., Islam S., Langer J.C., Sato T.T., Brandt M.L., Lee H., Blakely M.L., Lazar E.L., Hirschl R.B., Kenney B.D., Hackam D.J., Zelterman D., Silverman B.L. Laparotomy versus peritoneal drainage for necrotizing enterocolitis and perforation. N Engl J Med. 2006;354:2225–2234. doi: 10.1056/NEJMoa054605. [DOI] [PubMed] [Google Scholar]
- 53.Choi E.K., Appelman H.D. Chronic colitis in biopsy samples: is it inflammatory bowel disease or something else? Surg Pathol Clin. 2017;10:841–861. doi: 10.1016/j.path.2017.07.005. [DOI] [PubMed] [Google Scholar]
- 54.Rakoff-Nahoum S., Paglino J., Eslami-Varzaneh F., Edberg S., Medzhitov R. Recognition of commensal microflora by Toll-like receptors is required for intestinal homeostasis. Cell. 2004;118:229–241. doi: 10.1016/j.cell.2004.07.002. [DOI] [PubMed] [Google Scholar]
- 55.Takeda K., Akira S. TLR signaling pathways. Semin Immunol. 2004;16:3–9. doi: 10.1016/j.smim.2003.10.003. [DOI] [PubMed] [Google Scholar]
- 56.Lu Y.C., Yeh W.C., Ohashi P.S. LPS/TLR4 signal transduction pathway. Cytokine. 2008;42:145–151. doi: 10.1016/j.cyto.2008.01.006. [DOI] [PubMed] [Google Scholar]
- 57.Shi Y., Liu T., Zhao X., Yao L., Hou A., Fu J., Xue X. Vitamin D ameliorates neonatal necrotizing enterocolitis via suppressing TLR4 in a murine model. Pediatr Res. 2018 doi: 10.1038/pr.2017.329. Epub ahead of print. [DOI] [PubMed] [Google Scholar]
- 58.Huang K., Mukherjee S., DesMarais V., Albanese J.M., Rafti E., Draghi A., Maher L.A., Khanna K.M., Mani S., Matson A.P. Targeting the PXR-TLR4 signaling pathway to reduce intestinal inflammation in an experimental model of necrotizing enterocolitis. Pediatr Res. 2018 doi: 10.1038/pr.2018.14. Epub ahead of print. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Zhou Y., Li Y., Zhou B., Chen K., Lyv Z., Huang D., Liu B., Xu Z., Xiang B., Jin S., Sun X., Li Y. Inflammation and apoptosis: dual mediator role for Toll-like receptor 4 in the development of necrotizing enterocolitis. Inflamm Bowel Dis. 2017;23:44–56. doi: 10.1097/MIB.0000000000000961. [DOI] [PubMed] [Google Scholar]
- 60.Meng D., Zhu W., Shi H.N., Lu L., Wijendran V., Xu W., Walker W.A. Toll-like receptor-4 in human and mouse colonic epithelium is developmentally regulated: a possible role in necrotizing enterocolitis. Pediatr Res. 2015;77:416–424. doi: 10.1038/pr.2014.207. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Zhou W., Li W., Zheng X.H., Rong X., Huang L.G. Glutamine downregulates TLR-2 and TLR-4 expression and protects intestinal tract in preterm neonatal rats with necrotizing enterocolitis. J Pediatr Surg. 2014;49:1057–1063. doi: 10.1016/j.jpedsurg.2014.02.078. [DOI] [PubMed] [Google Scholar]
- 62.Afrazi A., Branca M.F., Sodhi C.P., Good M., Yamaguchi Y., Egan C.E., Lu P., Jia H., Shaffiey S., Lin J., Ma C., Vincent G., Prindle T., Jr., Weyandt S., Neal M.D., Ozolek J.A., Wiersch J., Tschurtschenthaler M., Shiota C., Gittes G.K., Billiar T.R., Mollen K., Kaser A., Blumberg R., Hackam D.J. Toll-like receptor 4-mediated endoplasmic reticulum stress in intestinal crypts induces necrotizing enterocolitis. J Biol Chem. 2014;289:9584–9599. doi: 10.1074/jbc.M113.526517. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Jilling T., Simon D., Lu J., Meng F.J., Li D., Schy R., Thomson R.B., Soliman A., Arditi M., Caplan M.S. The roles of bacteria and TLR4 in rat and murine models of necrotizing enterocolitis. J Immunol. 2006;177:3273–3282. doi: 10.4049/jimmunol.177.5.3273. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Ares G.J., McElroy S.J., Hunter C.J. The science and necessity of using animal models in the study of necrotizing enterocolitis. Semin Pediatr Surg. 2018;27:29–33. doi: 10.1053/j.sempedsurg.2017.11.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Lu P., Sodhi C.P., Jia H., Shaffiey S., Good M., Branca M.F., Hackam D.J. Animal models of gastrointestinal and liver diseases. Animal models of necrotizing enterocolitis: pathophysiology, translational relevance, and challenges. Am J Physiol Gastrointest Liver Physiol. 2014;306:G917–G928. doi: 10.1152/ajpgi.00422.2013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Cetin S., Leaphart C.L., Li J., Ischenko I., Hayman M., Upperman J., Zamora R., Watkins S., Ford H.R., Wang J., Hackam D.J. Nitric oxide inhibits enterocyte migration through activation of RhoA-GTPase in a SHP-2-dependent manner. Am J Physiol Gastrointest Liver Physiol. 2007;292:G1347–G1358. doi: 10.1152/ajpgi.00375.2006. [DOI] [PubMed] [Google Scholar]
- 67.Zamora R., Grishin A., Wong C., Boyle P., Wang J., Hackam D., Upperman J.S., Tracey K.J., Ford H.R. High-mobility group box 1 protein is an inflammatory mediator in necrotizing enterocolitis: protective effect of the macrophage deactivator semapimod. Am J Physiol Gastrointest Liver Physiol. 2005;289:G643–G652. doi: 10.1152/ajpgi.00067.2005. [DOI] [PubMed] [Google Scholar]
- 68.Qureshi F.G., Leaphart C., Cetin S., Li J., Grishin A., Watkins S., Ford H.R., Hackam D.J. Increased expression and function of integrins in enterocytes by endotoxin impairs epithelial restitution. Gastroenterology. 2005;128:1012–1022. doi: 10.1053/j.gastro.2005.01.052. [DOI] [PubMed] [Google Scholar]
- 69.Afrazi A., Sodhi C.P., Good M., Jia H., Siggers R., Yazji I., Ma C., Neal M.D., Prindle T., Grant Z.S., Branca M.F., Ozolek J., Chang E.B., Hackam D.J. Intracellular heat shock protein-70 negatively regulates TLR4 signaling in the newborn intestinal epithelium. J Immunol. 2012;188:4543–4557. doi: 10.4049/jimmunol.1103114. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Jilling T., Lu J., Jackson M., Caplan M.S. Intestinal epithelial apoptosis initiates gross bowel necrosis in an experimental rat model of neonatal necrotizing enterocolitis. Pediatr Res. 2004;55:622–629. doi: 10.1203/01.PDR.0000113463.70435.74. [DOI] [PubMed] [Google Scholar]
- 71.Liu Y., Zhu L., Fatheree N.Y., Liu X., Pacheco S.E., Tatevian N., Rhoads J.M. Changes in intestinal Toll-like receptors and cytokines precede histological injury in a rat model of necrotizing enterocolitis. Am J Physiol Gastrointest Liver Physiol. 2009;297:G442–G450. doi: 10.1152/ajpgi.00182.2009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Sturm A., DA Epithelial restitution and wound healing in inflammatory bowel disease. World J Gastroenterol. 2008;14:348–353. doi: 10.3748/wjg.14.348. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Mi Q., Swigon D., Rivière B., Cetin S., Vodovotz Y., Hackam D.J. One-dimensional elastic continuum model of enterocyte layer migration. Biophys J. 2007;93:3745–3752. doi: 10.1529/biophysj.107.112326. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Cetin S., Ford H.R., Sysko L.R., Agarwal C., Wang J., Neal M.D., Baty C., Apodaca G., Hackam D.J. Endotoxin inhibits intestinal epithelial restitution through activation of Rho-GTPase and increased focal adhesions. J Biol Chem. 2004;279:24592–24600. doi: 10.1074/jbc.M313620200. [DOI] [PubMed] [Google Scholar]
- 75.Sodhi C.P., Shi X.H., Richardson W.M., Grant Z.S., Shapiro R.A., Prindle T.J., Branca M., Russo A., Gribar S.C., Ma C., Hackam D.J. Toll-like receptor-4 inhibits enterocyte proliferation via impaired beta-catenin signaling in necrotizing enterocolitis. Gastroenterology. 2010;138:185–196. doi: 10.1053/j.gastro.2009.09.045. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Neal M.D., Sodhi C.P., Jia H., Dyer M., Egan C.E., Yazji I., Good M., Afrazi A., Marino R., Slagle D., Ma C., Branca M.F., Prindle T., Jr., Grant Z., Ozolek J., Hackam D.J. Toll-like receptor 4 is expressed on intestinal stem cells and regulates their proliferation and apoptosis via the p53 up-regulated modulator of apoptosis. J Biol Chem. 2012;287:37296–37308. doi: 10.1074/jbc.M112.375881. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Nino D.F., Sodhi C.P., Egan C.E., Zhou Q., Lin J., Lu P., Yamaguchi Y., Jia H., Martin L.Y., Good M., Fulton W.B., Prindle T., Jr., Ozolek J.A., Hackam D.J. Retinoic acid improves incidence and severity of necrotizing enterocolitis by lymphocyte balance restitution and repopulation of LGR5+ intestinal stem cells. Shock. 2017;47:22–32. doi: 10.1097/SHK.0000000000000713. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Weitkamp J.H., Rosen M.J., Zhao Z., Koyama T., Geem D., Denning T.L., Rock M.T., Moore D.J., Halpern M.D., Matta P., Denning P.W. Small intestinal intraepithelial TCRgammadelta+ T lymphocytes are present in the premature intestine but selectively reduced in surgical necrotizing enterocolitis. PLoS One. 2014;9:e99042. doi: 10.1371/journal.pone.0099042. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Liu Y., Fatheree N.Y., Mangalat N., Rhoads J.M. Lactobacillus reuteri strains reduce incidence and severity of experimental necrotizing enterocolitis via modulation of TLR4 and NF-kappaB signaling in the intestine. Am J Physiol Gastrointest Liver Physiol. 2012;302:G608–G617. doi: 10.1152/ajpgi.00266.2011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Dingle B.M., Liu Y., Fatheree N.Y., Min J., Rhoads J.M., Tran D.Q. FoxP3(+) regulatory T cells attenuate experimental necrotizing enterocolitis. PLoS One. 2013;8:e82963. doi: 10.1371/journal.pone.0082963. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Weitkamp J.H., Koyama T., Rock M.T., Correa H., Goettel J.A., Matta P., Oswald-Richter K., Rosen M.J., Engelhardt B.G., Moore D.J., Polk D.B. Necrotizing enterocolitis is characterised by disrupted immune regulation and diminished mucosal regulatory (FOXP3)/effector (CD4, CD8) T cell ratios. Gut. 2013;62:73–82. doi: 10.1136/gutjnl-2011-301551. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 82.Yazji I., Sodhi C.P., Lee E.K., Good M., Egan C.E., Afrazi A., Neal M.D., Jia H., Lin J., Ma C., Branca M.F., Prindle T., Richardson W.M., Ozolek J., Billiar T.R., Binion D.G., Gladwin M.T., Hackam D.J. Endothelial TLR4 activation impairs intestinal microcirculatory perfusion in necrotizing enterocolitis via eNOS-NO-nitrite signaling. Proc Natl Acad Sci U S A. 2013;110:9451–9456. doi: 10.1073/pnas.1219997110. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Nowicki P.T., Caniano D.A., Hammond S., Giannone P.J., Besner G.E., Reber K.M., Nankervis C.A. Endothelial nitric oxide synthase in human intestine resected for necrotizing enterocolitis. J Pediatr. 2007;150:40–45. doi: 10.1016/j.jpeds.2006.09.029. [DOI] [PubMed] [Google Scholar]
- 84.Nowicki P.T., Dunaway D.J., Nankervis C.A., Giannone P.J., Reber K.M., Hammond S.B., Besner G.E., Caniano D.A. Endothelin-1 in human intestine resected for necrotizing enterocolitis. J Pediatr. 2005;146:805–810. doi: 10.1016/j.jpeds.2005.01.046. [DOI] [PubMed] [Google Scholar]
- 85.Reber K.M., Nankervis C.A., Nowicki P.T. Newborn intestinal circulation. Physiology and pathophysiology. Clin Perinatol. 2002;29:23–39. doi: 10.1016/s0095-5108(03)00063-0. [DOI] [PubMed] [Google Scholar]
- 86.Good M., Sodhi C.P., Yamaguchi Y., Jia H., Lu P., Fulton W.B., Martin L.Y., Prindle T., Nino D.F., Zhou Q., Ma C., Ozolek J.A., Buck R.H., Goehring K.C., Hackam D.J. The human milk oligosaccharide 2′-fucosyllactose attenuates the severity of experimental necrotising enterocolitis by enhancing mesenteric perfusion in the neonatal intestine. Br J Nutr. 2016;116:1175–1187. doi: 10.1017/S0007114516002944. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87.Gribar S.C., Sodhi C.P., Richardson W.M., Anand R.J., Gittes G.K., Branca M.F., Jakub A., Shi X.H., Shah S., Ozolek J.A., Hackam D.J. Reciprocal expression and signaling of TLR4 and TLR9 in the pathogenesis and treatment of necrotizing enterocolitis. J Immunol. 2009;182:636–646. doi: 10.4049/jimmunol.182.1.636. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88.Perez-Munoz M.E., Arrieta M.C., Ramer-Tait A.E., Walter J. A critical assessment of the "sterile womb" and "in utero colonization" hypotheses: implications for research on the pioneer infant microbiome. Microbiome. 2017;5:48. doi: 10.1186/s40168-017-0268-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 89.McElroy S.J., Prince L.S., Weitkamp J.H., Reese J., Slaughter J.C., Polk D.B. Tumor necrosis factor receptor 1-dependent depletion of mucus in immature small intestine: a potential role in neonatal necrotizing enterocolitis. Am J Physiol Gastrointest Liver Physiol. 2011;301:G656–G666. doi: 10.1152/ajpgi.00550.2010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Lee J., Rachmilewitz D., Raz E. Homeostatic effects of TLR9 signaling in experimental colitis. Ann N Y Acad Sci. 2006;1072:351–355. doi: 10.1196/annals.1326.022. [DOI] [PubMed] [Google Scholar]
- 91.Rachmilewitz D., Katakura K., Karmeli F., Hayashi T., Reinus C., Rudensky B., Akira S., Takeda K., Lee J., Takabayashi K., Raz E. Toll-like receptor 9 signaling mediates the anti-inflammatory effects of probiotics in murine experimental colitis. Gastroenterology. 2004;126:520–528. doi: 10.1053/j.gastro.2003.11.019. [DOI] [PubMed] [Google Scholar]
- 92.Kumagai Y., Takeuchi O., Akira S. TLR9 as a key receptor for the recognition of DNA. Adv Drug Deliv Rev. 2008;60:795–804. doi: 10.1016/j.addr.2007.12.004. [DOI] [PubMed] [Google Scholar]
- 93.Hemmi H., Takeuchi O., Kawai T., Kaisho T., Sato S., Sanjo H., Matsumoto M., Hoshino K., Wagner H., Takeda K., Akira S.A. Toll-like receptor recognizes bacterial DNA. Nature. 2000;408:740–745. doi: 10.1038/35047123. [DOI] [PubMed] [Google Scholar]
- 94.Neu J. Probiotics and necrotizing enterocolitis. Clin Perinatol. 2014;41:967–978. doi: 10.1016/j.clp.2014.08.014. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 95.Good M., Sodhi C.P., Ozolek J.A., Buck R.H., Goehring K.C., Thomas D.L., Vikram A., Bibby K., Morowitz M.J., Firek B., Lu P., Hackam D.J. Lactobacillus rhamnosus HN001 decreases the severity of necrotizing enterocolitis in neonatal mice and preterm piglets: evidence in mice for a role of TLR9. Am J Physiol Gastrointest Liver Physiol. 2014;306:G1021–G1032. doi: 10.1152/ajpgi.00452.2013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96.Kevans D., Silverberg M.S., Borowski K., Griffiths A., Xu W., Onay V., Paterson A.D., Knight J., Croitoru K. IBD genetic risk profile in healthy first-degree relatives of Crohn's disease patients. J Crohns Colitis. 2016;10:209–215. doi: 10.1093/ecco-jcc/jjv197. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 97.Richardson W.M., Sodhi C.P., Russo A., Siggers R.H., Afrazi A., Gribar S.C., Neal M.D., Dai S., Prindle T., Jr., Branca M., Ma C., Ozolek J., Hackam D.J. Nucleotide-binding oligomerization domain-2 inhibits Toll like receptor-4 signaling in the intestinal epithelium. Gastroenterology. 2010;139:904–917. doi: 10.1053/j.gastro.2010.05.038. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 98.Patel A.L., Panagos P.G., Silvestri J.M. Reducing incidence of necrotizing enterocolitis. Clin Perinatol. 2017;44:683–700. doi: 10.1016/j.clp.2017.05.004. [DOI] [PubMed] [Google Scholar]
- 99.Hair A.B., Peluso A.M., Hawthorne K.M., Perez J., Smith D.P., Khan J.Y., O'Donnell A., Powers R.J., Lee M.L., Abrams S.A. Beyond necrotizing enterocolitis prevention: improving outcomes with an exclusive human milk-based diet. Breastfeed Med. 2016;11:70–74. doi: 10.1089/bfm.2015.0134. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 100.Chowning R., Radmacher P., Lewis S., Serke L., Pettit N., Adamkin D.H. A retrospective analysis of the effect of human milk on prevention of necrotizing enterocolitis and postnatal growth. J Perinatol. 2016;36:221–224. doi: 10.1038/jp.2015.179. [DOI] [PubMed] [Google Scholar]
- 101.Good M., Sodhi C.P., Egan C.E., Afrazi A., Jia H., Yamaguchi Y., Lu P., Branca M.F., Ma C., Prindle T., Jr., Mielo S., Pompa A., Hodzic Z., Ozolek J.A., Hackam D.J. Breast milk protects against the development of necrotizing enterocolitis through inhibition of Toll-like receptor 4 in the intestinal epithelium via activation of the epidermal growth factor receptor. Mucosal Immunol. 2015;8:1166–1179. doi: 10.1038/mi.2015.30. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 102.Caplan M.S., MacKendrick W. Necrotizing enterocolitis: a review of pathogenetic mechanisms and implications for prevention. Pediatr Pathol. 1993;13:357–369. doi: 10.3109/15513819309048223. [DOI] [PubMed] [Google Scholar]
- 103.Pammi M., Abrams S.A. Oral lactoferrin for the prevention of sepsis and necrotizing enterocolitis in preterm infants. Cochrane Database Syst Rev. 2015;2 doi: 10.1002/14651858.CD007137.pub4. [DOI] [PubMed] [Google Scholar]
- 104.Ledbetter D.J., Juul S.E. Erythropoietin and the incidence of necrotizing enterocolitis in infants with very low birth weight. J Pediatr Surg. 2000;35:178–181. doi: 10.1016/s0022-3468(00)90006-x. discussion 182. [DOI] [PubMed] [Google Scholar]
- 105.Hidalgo-Cantabrana C., Delgado S., Ruiz L., Ruas-Madiedo P., Sanchez B., Margolles A. Bifidobacteria and their health-promoting effects. Microbiol Spectr. 2017;5:3. doi: 10.1128/microbiolspec.bad-0010-2016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 106.Autran C.A., Schoterman M.H., Jantscher-Krenn E., Kamerling J.P., Bode L. Sialylated galacto-oligosaccharides and 2′-fucosyllactose reduce necrotising enterocolitis in neonatal rats. Br J Nutr. 2016;116:294–299. doi: 10.1017/S0007114516002038. [DOI] [PubMed] [Google Scholar]
- 107.Underwood M.A., Gaerlan S., De Leoz M.L., Dimapasoc L., Kalanetra K.M., Lemay D.G., German J.B., Mills D.A., Lebrilla C.B. Human milk oligosaccharides in premature infants: absorption, excretion, and influence on the intestinal microbiota. Pediatr Res. 2015;78:670–677. doi: 10.1038/pr.2015.162. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 108.Armanian A.M., Sadeghnia A., Hoseinzadeh M., Mirlohi M., Feizi A., Salehimehr N., Saee N., Nazari J. The effect of neutral oligosaccharides on reducing the incidence of necrotizing enterocolitis in preterm infants: a randomized clinical trial. Int J Prev Med. 2014;5:1387–1395. [PMC free article] [PubMed] [Google Scholar]
- 109.Lien E., Chow J.C., Hawkins L.D., McGuinness P.D., Miyake K., Espevik T., Gusovsky F., Golenbock D.T. A novel synthetic acyclic lipid A-like agonist activates cells via the lipopolysaccharide/toll-like receptor 4 signaling pathway. J Biol Chem. 2001;276:1873–1880. doi: 10.1074/jbc.M009040200. [DOI] [PubMed] [Google Scholar]
- 110.Tidswell M., Tillis W., Larosa S.P., Lynn M., Wittek A.E., Kao R., Wheeler J., Gogate J., Opal S.M. Phase 2 trial of eritoran tetrasodium (E5564), a Toll-like receptor 4 antagonist, in patients with severe sepsis. Crit Care Med. 2010;38:72–83. doi: 10.1097/CCM.0b013e3181b07b78. [DOI] [PubMed] [Google Scholar]