Abstract
Background: Gender affirming surgeries are increasingly accessible to transgender and non-binary individuals due to changes in health care coverage policies and rising numbers of trained providers. Improved access to care has led to an increase in the number of individuals pursuing gender affirming surgeries. Little is known about how to optimally prepare patients for these surgeries.
Aims: This evaluation examined attendees’ assessment of a four-hour single-session class developed to prepare transgender and non-binary patients and their caregivers for gender affirming surgeries in a multi-disciplinary transgender clinic within an integrated health care system.
Methods: A multi-disciplinary group of providers within a health maintenance organization in Northern California designed and facilitated two separate curricula, one for patients preparing for metoidioplasty/phalloplasty and the other preparing for vaginoplasty. Between November 2015 and June 2017, 214 patients and caregivers took one of the two versions of the class and completed the post-class survey evaluating perceived favorability of the class and preparedness regarding surgery options, complications and postoperative care. Descriptive statistics were used to summarize the Likert scale questions, with 1 showing the least improvement and 5 showing the most.
Results: Of the 214 patients and caregivers that completed the survey, the majority reported that they were better informed about their surgical options (mean: 4.4, SD: 0.7), more prepared for surgery (mean: 4.5, SD: 0.6), better informed about possible complications (mean: 4.5, SD: 0.7), and better understood their postoperative care needs (mean: 4.6, SD: 0.6). Of the respondents, 204 (95%) reported they would recommend the course to a friend preparing for gender affirming surgery.
Discussion: Our findings demonstrate that a single-session class is a favorable method for preparing transgender and non-binary patients to make informed decisions regarding the perioperative gender affirming surgical process, from preoperative preparedness, to surgical complications, and postoperative care.
Keywords: Gender affirming surgery, informed consent, nonbinary, patient education, transgender health
Introduction
The population of transgender individuals in the United States (US) is estimated to be 0.4–0.6% of the population, or between 1 and 1.4 million individuals (Flores, Herman, Gates, & Brown, 2016; Meerwijk & Sevelius, 2017). Population estimates for numbers of individuals who identify as non-binary are more difficult to capture. Data on the prevalence of hormonal or surgical treatment for gender affirmation in the US transgender population is limited, but growing. According to the 2015 US Transgender Survey, the nation’s largest survey on transgender health, approximately half of respondents had undergone hormone therapy and/or gender affirming surgery, with 25% reporting having completed one or more transition-related surgery (James et al., 2016).
The World Professional Association for Transgender Health (WPATH) publishes Standards of Care (SOC) for the health of transgender and gender nonconforming people. In its seventh and most current iteration, the SOC delineate recommended criteria for transgender patients undergoing genital surgery for gender affirmation (Coleman et al., 2012). These standards are consulted worldwide for guidance on providing treatment to transgender and non-binary patients seeking surgery.
The number of gender affirming procedures in the US has risen as insurance coverage for gender affirming healthcare has expanded. In 2014, the US Department of Health and Human Services overturned Medicare’s exclusion of coverage for transgender surgical treatment, a decision likely responsible for the three-fold increase in Medicare- and Medicaid-covered patients seeking gender affirming procedures from 2012–2013 to 2014 as recently reported by Canner et al (2018). An increasing number of state legislatures have passed similar laws banning transgender care exclusions among their third-party payers. The American Society of Plastic Surgeons (ASPS) reported a 20% rise in transgender-related surgeries from 2015 to 2016 (ASPS, 2017). These numbers must be interpreted in the context of surgery and surgeon availability, procedure cost and insurance coverage limitations for transgender individuals, discrimination by medical providers, and other barriers to care, and likely reflect a low estimate of the number of people who would pursue gender affirming surgeries if access barriers were reduced.
As demand and availability of gender affirmation treatments including genital surgery increase, there is a need to establish best health care practice models to provide optimal informed consent, patient counseling, and surgical outcomes for patients undergoing gender affirmation procedures (Berli et al., 2017; Reisner, Radix, & Deutsch, 2016; Wylie et al., 2016). While the SOC specify that surgeons performing gender affirmation procedures should engage in “at length” consultation with both their patients and interdisciplinary health care team so that they are equipped to provide coordinated care to their transgender clientele, the SOC do not provide guidelines for how best to prepare patients for surgery.
To date, there are no published studies on strategies that effectively optimize the informed consent process among patients seeking to undergo gender affirming surgery. Preoperative patient education programs for bariatric surgery and hip or knee replacement have been shown to be effective (Groller 2017; Kennedy et al., 2017). However, no studies have been published on similar programs for gender affirming surgery. These surgeries can be complicated and involve multiple stages; therefore, as with any complex surgical process, patients must understand the risks, benefits and time course of their desired procedures before proceeding.
This project aimed to provide insight into the favorability of a surgery readiness class to inform and prepare transgender and non-binary patients and their caregivers for gender affirmation surgery within an integrated, multi-specialty transgender care clinic.
Methods
The surgery readiness class was developed at a multi-specialty clinic providing integrated services for transgender and non-binary patients within a health maintenance organization in Northern California. The department, a major referral center for gender affirming surgery throughout Northern California, includes internal medicine and obstetrics and gynecology physicians, social workers, mental health specialists, nurses, plastic surgeons, and urologists, all with expertise and experience providing culturally competent care to transgender and gender non-binary patients.
In November 2015, a multidisciplinary team of clinic providers developed a monthly single-session, four-hour curriculum for patients preparing to undergo gender affirming surgery and their caregivers. Two iterations of the curriculum were developed, one focusing on vaginoplasty and the other on metoidioplasty/phalloplasty, and each was implemented on alternating months. The course covered four primary content areas: anatomy and surgical options, preparation and readiness for surgery including complications, postoperative care and recovery, and mental health and wellness (Figure 1) and was facilitated by culturally sensitive providers. The content and organization of classes were informed by feedback provided to clinic staff by participants in prior classes as well as key patient informants invited to participate in the initial classes.
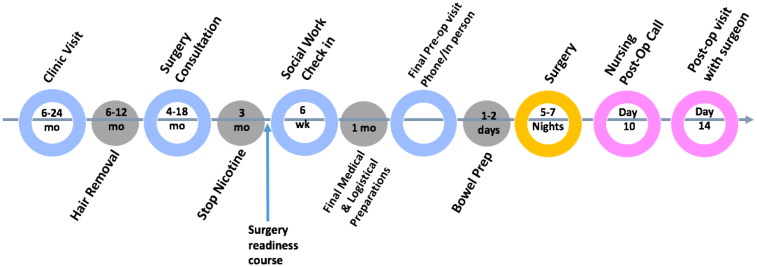
Figure 1.
Sample timeline for phalloplasty preparation.
Those eligible to attend the class included patients receiving care at the clinic who were either scheduled for or considering surgery and the caregivers of said patients. Attendance was limited to 10–20 participants each month. Due to high demand and attendance constraints, patients who had scheduled surgeries within two to three months were prioritized for class attendance as well as patients earlier in their referral process who were identified by their gender therapist as needing more information for surgical decision-making. These patients included those who were still in the process of deciding whether or not to undergo gender affirming surgery as well as those who had inaccurate information about anatomy, recovery or surgical outcomes. An estimated 20% of patients served at the multi-specialty clinic were referred to the course.
As part of the educational program, anonymous evaluation surveys were distributed at the end of each class to assess patient and caregiver satisfaction and knowledge acquisition. No identifying information was collected. The survey included multiple yes/no, five-point Likert scale (1 showing the least improvement and 5 showing the most) and open-ended questions. Quantitative data were aggregated and analyzed using descriptive statistics to create summary scores related to course favorability and attendee knowledge acquisition. This project was deemed exempt from review by the clinic’s supervising Institutional Review Board as there were no patient identifiers in the surveys received.
Results
From November 2015 to June 2017, 214 course evaluations were completed by patients and caregivers. Fifty-five percent (n = 118) of the evaluations corresponded to the metoidioplasty/phalloplasty curriculum and 45% (n = 96) to the vaginoplasty curriculum. Of the respondents, 64 (30%) were patients anticipating surgery, 43 (20%) were caregivers of patients, and 107 (50%) did not indicate whether they were patients or caregivers.
After attending the class, participants reported that they were better informed about their surgical options (mean: 4.4, SD: 0.7), more prepared for surgery (mean: 4.5, SD: 0.6), better informed about possible complications (mean: 4.5, SD: 0.7), and better understood their postoperative care needs (mean: 4.6, SD: 0.6) (Table 1).
Table 1.
Likert scale evaluation of surgery readiness course (n = 214).a
| After attending this class | Mean (standard deviation) |
|---|---|
| I better understand surgical options | 4.4 (0.7) |
| I better understand complications | 4.5 (0.7) |
| I better understand what to expect before surgery | 4.6 (0.6) |
| I better understand what care I will need after surgery | 4.6 (0.6) |
1 = Strongly disagree, 5 = Strongly agree.
When asked if they would recommend the class to a friend, 204 (95.3%) respondents said they would; 172 (80.4%) believed the length of the class was appropriate and 151 (70.5%) believed that the class time, date, and location were convenient. When given a list of options for ways to receive information about preparing for surgery in the future, 116 (54.2%) opted to continue receiving information in the form of an in-person class, 57 (26.6%) preferred the use of online tools and resources and 57 (26.6%) preferred one-on-one in-person coaching.
Respondents gave suggestions for how to improve the class which included additional pictures of previous gender affirming surgeries performed by the specific surgeons they were considering, example photographs of typical and unexpected wound healing, the inclusion of a list of materials to have ready for the postoperative recovery and wound healing process and a discussion of the statistical likelihood of complications that may arise and a more detailed description of those complications.
A common suggestion in the initial months of the course’s implementation was to include a panel of patients who had undergone gender affirming surgery and could speak about their experience. This suggestion was implemented in April 2016 and was well received by attendees thereafter, resulting in increased mean scores on each of our evaluation measures after the panels were initiated. Statistically significant increases in mean participant responses were found in the measures indicating better understanding of surgical options (from 4.3 to 4.5, p = .05) and better understanding of what to expect before surgery (from 4.4 to 4.6, p = .02).
Discussion
This four-hour single-session class, providing information on the perioperative process for transgender and non-binary patients preparing for gender affirming surgery, received high favorability ratings from attendees. Attendees reported increased knowledge regarding surgical options, preparedness, and recovery, thus bolstering informed consent.
This knowledge acquisition may not only impact the consent process and preoperative preparation, but according to WPATH SOC’s, having a realistic understanding of the postoperative outcomes may help patients “in achieving a result that will alleviate their gender dysphoria” (Coleman et al., 2012), thereby affecting the patients’ postoperative satisfaction as well.
In lieu of a surgery preparation course or adequate preoperative counseling time with a surgeon, patients may turn to the Internet for information about their desired surgeries. However, online medical information regarding gender affirming surgery is at a reading level higher than is recommended for healthcare information dissemination (Kiwanuka, Mehrzad, Prsic, & Kwan, 2017). Anecdotally, many patients may seek online information from various community forums and message boards which, while written in plain language, may not be medically accurate. Surgeons performing gender affirming procedures are increasingly recognizing the need to establish realistic expectations and thorough understanding of postoperative care with their patients, emphasizing preoperative informed consent and the importance of postoperative follow-up with a multidisciplinary team (Weissler et al., 2018). Our evaluation of this course suggests the possibility that the attendance of a class that provides comprehensive information on key perioperative topics may help streamline preoperative consultations with the physicians, bolster the informed consent process and contribute to optimal physical and psychological outcomes.
Attendees’ suggestions to include more example photographs as part of the preoperative educational process is consistent with other projects that have evaluated patient education courses prior to surgical procedures (Webb, Sharma, & Temple-Oberle, 2018). Specifically, attendees requested postoperative photographs of the various gender affirming procedures, including procedures that had been performed by local surgeons who may perform their procedures and photographs depicting normal versus pathological healing of surgical sites. When available, the photographs included in our presentation were sourced from the public-facing websites of the surgeons contracted to perform operations for patients served by our organization. As more surgeries became internalized within our institution we worked to obtain patient consent to take intraoperative and postoperative photographs of surgical procedures, and hope to expand our library of photographs that can be made available to our patients considering surgery. While a potential barrier may be compliance with HIPAA regulations around identifying information in surgical photographs, efforts should be made to develop resources for transgender patients that include visual examples of their surgical options.
Unlike the attendees of this class, largely a health-literate and insured patient population, the majority of transgender and gender nonconforming patients in the US face numerous barriers to care (James et al., 2016; Safer et al., 2016) and are not able to access gender affirming surgery (Beckwith, Reisner, Zaslow, Mayer, & Keuroghlian, 2017). According to the most recent US Transgender Survey, 13% of respondents reported lack of health insurance compared to 10% of the general population (James et al, 2016). Of the insured, 55% were denied coverage for transition surgery. In addition, 33% of the US Transgender Survey respondents reported having at least one negative experience with a health care provider.
To our knowledge, this is the first program to directly evaluate the favorability of a surgery readiness class to inform and prepare transgender and non-binary patients and their caregivers for gender affirmation surgery. The course increased access to comprehensive information and the positive feedback suggests it was useful in providing guidance to patients regarding their surgical pathway. In future years, we hope to move beyond this initial evaluation and assess the association between preoperative education measures and postoperative outcomes, helping to provide more generalizable information on the universality of such an education class. The potential to expand the course to non-health maintenance organization models of health care may help reduce disparities in health experienced by transgender and gender non-conforming individuals. It is imperative to support the momentum of current interdisciplinary interventions focused on transgender health, like ours, that can inform efforts to provide accessible and effective care to transgender and non-binary people throughout the US.
Disclosure statement
No potential conflict of interest was reported by the authors.
Ethical approval
For this type of study formal consent is not required.
References
- American Society of Plastic Surgeons. (2017). Gender confirmation surgeries rise 20% in first ever report [Press Release]. Retrieved from https://www.plasticsurgery.org/news/press-releases/gender-confirmation-surgeries-rise-20-percent-in-first-ever-report.
- Beckwith N., Reisner S. L., Zaslow S., Mayer K. H., & Keuroghlian A. S (2017). Factors associated with gender-affirming surgery and age of hormone therapy initiation among transgender adults. Transgender Health, 2(1), 156–164. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Berli J. U., Knudson G., Fraser L., Tangpricha V., Ettner R., Ettner F. M., … Schechter L (2017). What surgeons need to know about gender confirmation surgery when providing care for transgender individuals: A review. JAMA Surgery, 152(4), 394–400. [DOI] [PubMed] [Google Scholar]
- Canner J. K., Harfouch O., Kodadek L. M., Pelaez D., Coon D., & Offodile A. C (2018). Temporal trends in gender-affirming surgery among transgender patients in the United States. JAMA Surgery [Online]. doi: 10.1001/jamasurg.2017.6231 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Coleman E., Bockting W., & Botzer M, Cohen-Kettenis P., DeCuypere G., … Zucker K (2012). Standards of care for the health of transsexual, transgender and gender-nonconforming people, version 7. International Journal of Transgender, 13, 165–232. [Google Scholar]
- Flores A. R., Herman J. L., Gates G. J., & Brown T. N. T (2016). How many adults identify as transgender in the United States? Los Angeles, CA: The Williams Institute; Retrieved from http://williamsinstitute.law.ucla.edu/wp-content/uploads/How-Many-Adults-Identify-as-Transgender-in-the-United-States.pdf [Google Scholar]
- Groller K. D. (2017). Systematic review of patient education practices in weight loss surgery. Surgery for Obesity and Related Diseases: Official Journal of the American Society for Bariatric Surgery, 13(6), 1072–1085. [DOI] [PubMed] [Google Scholar]
- James S. E., Herman J. L., Rankin S., Keisling M., Mottet L., & Ana M (2016). The report of the 2015 U.S. transgender survey. Washington, DC: National Center for Transgender Equality. [Google Scholar]
- Kennedy D., Wainwright A., Pereira L., Robarts S., Dickson P., Christian J., & Webster F (2017). A qualitative study of patient education needs for hip and knee replacement. BMC Musculoskeletal Disorders, 18(1), 413. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kiwanuka E., Mehrzad R., Prsic A., & Kwan D (2017). Online patient resources for gender affirmation surgery: An analysis of readability. Annals of Plastic Surgery, 79(4), 329–333. [DOI] [PubMed] [Google Scholar]
- Meerwijk E. L., & Sevelius J. M (2017). Transgender population size in the United States: A meta-regression of population-based probability samples. American Journal of Public Health, 107(2), e1–e8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Reisner S. L., Radix A., & Deutsch M. B (2016). Integrated and gender-affirming transgender clinical care and research. Journal of Acquired Immune Deficiency Syndrome, 72, S235–S242. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Webb C., Sharma V., & Temple-Oberle C (2018). Delivering breast reconstruction information to patients: Women report on preferred information delivery styles and options. Plastic Surgery, 26(1), 26–32. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Weissler J. M., Chang B. L., Carney M. J., Rengifo D., Messa C. A., Sarwer D. B., & Percec I (2018). Gender-affirming surgery in persons with gender dysphoria. Plastic and Reconstructive Surgery, 141(3), 388e–396e. [DOI] [PubMed] [Google Scholar]
- Wylie K., Knudson G., Khan S. I., Bonierbale M., Watanyusakul S., & Baral S (2016). Serving transgender people: Clinical care considerations and service delivery models in transgender health. Lancet, 388(10042), 401–411. [DOI] [PubMed] [Google Scholar]
- Safer J. D., Coleman E., Feldman J., Garofalo R., Hembree W., Radix A., & Sevelius J (2016). Barriers to healthcare for transgender individuals. Current Opinion in Endocrinology, Diabetes, and Obesity, 23(2), 168–171. [DOI] [PMC free article] [PubMed] [Google Scholar]