Abstract
Purpose
Thoracic disc herniations are uncommon and carry a high risk for neurological deterioration. Traditional surgical approaches include thoracotomy, costotransversectomy or posterior approaches with considerable morbidity. In this technical note with case series, we describe a minimally invasive tubular retractor–assisted retropleural approach for simple and less invasive microsurgical exploration of thoracic disc herniations from a lateral angle.
Methods
Surgical technique consisted of partial rib resection and retropleural dissection followed by the placement of a tubular retractor (METRx Tubes, Medtronic) for an anterior-lateral exposure of the disc and neuroforamen. Epidemiological, clinical and surgical patient data were acquired.
Results
Between 2017 and 2020, six patients were surgically treated using the minimally invasive tubular retractor–assisted retropleural approach. Microsurgical exposure of the disc and neural structures was achieved from a lateral direction without requiring thoracotomy or lung deflation. Control imaging confirmed resection in all cases without relevant residuum. As postoperative complications, one dural injury and one postoperative pneumothorax occured. No neurologic deterioration or recurrence occurred during a median follow-up of 3 months.
Conclusion
The described tubular retractor–assisted retropleural exposure serves as a feasible minimally invasive microsurgical approach to the anterior-lateral thoracic spine.
Keywords: Thoracic disc herniation, Minimally invasive spine surgery, Thoracic spine surgery, Tubular retractor–assisted surgical approach, Retropleural dissection
Introduction
Symptomatic disc herniations in the thoracic spine are uncommon and occur only in up to 3% of all patients suffering from disc herniations [8, 9]. Mainly, they are located in the mid- to lower thoracic spine and are prone to neurological deficits in up to 60% [6, 8, 19, 23]. To surgically treat thoracic disc herniations, anterior, posterior, and lateral approaches are available. Common anterior approaches include transthoracic, transsternal and thoracoscopic approaches, whilst common posterior approaches are transpedicular and trans-facet pedicle sparing approaches, and traditional lateral approaches include lateral extracavitary approaches and costotransversectomy [2, 4, 8, 24]. Lateral retropleural approaches to the thoracic spine give the advantage of using the shortest way to the anterior-lateral thoracic spine without opening the pleural cavity [1, 13, 16, 24]. In the past years, case series described refinements of this lateral approach to the thoracic spine for the treatment of thoracic disc herniations, combining the technique with neuronavigation, videoendoscopy, or retractor-assisted approaches using an X-LIF retractor system, allowing for an enhanced exposure of thoracic disc herniations whilst decreasing surgical morbidity [1, 8, 13, 17, 22, 24]. With this report, we describe a minimally invasive tubular retractor–assisted retropleural approach which allows for a microsurgical exploration and resection of thoracic disc herniations from a lateral angle in a series of six patients.
Materials and methods
Clinical and surgical data
Patients with symptomatic one-level thoracic disc herniations surgically treated between 2017 and 2020 using a new minimally invasive tubular retractor–assisted approach were included in this case series. Patient recruitment and surgery were performed at two academic institutions. Included patients suffered from symptomatic one-level disc herniations at the mid– to lower thoracic level (Th6/7—Th10/11) which were lateralized and at least partially calcified. Clinical, surgical and imaging data was analyzed restropectively. Patients received postoperative routine treatment including early mobilisation and physiotherapy. Postoperative control imaging was performed to assess disc herniation removal using MRI or CT. All patients received routine clinical follow-up.
Ethical statement.
This case series was conducted according to the World Medical Association Declaration of Helsinki. The study was approved by the local ethics committee and informed patient consent was waived due to the retrospective nature of the study (Ethics committee approval by the Charité-Universitätsmedizin Berlin, Germany, number EA4/064/20).
Data management
Data management was performed using Microsoft Excel and internal file servers. Descriptive statistical analysis was performed using GraphPad Prism 8 (GraphPad Software, La Jolla, CA, USA).
Results
Technical note to the surgical technique
Surgery was performed under general anesthesia. A double lumen tube for respiration was inserted to allow for unilateral lung deflation during retropleural dissection. Antibiotic prophylaxis via single-shot infusion of Cefazolin (2 g) was applied 30 min prior to the skin incision. The patient was positioned laterally on an X-ray transparent operating table (Trumpf Carbon Spine tabletop, Trumpf Medical), using a deflatable mattress. The side of the herniated disc was facing up. The arm was elevated and positioned at 90° from the thorax. Fluoroscopic localization of the index level was performed anterior-posteriorly and laterally and the thus localized index level was marked on the skin using a water-proof marker. A 3 cm skin incision was applied at about 12 cm paramedian on the side of the herniated disc. Following retractor-insertion under fluoroscopic control, the caudal rib of the index segment was partially resected using a diamond drill (Fig. 1a). Retropleural dissection under short apnea and unilateral lung deflatation was performed to expose the head of the caudal rib and the neuroforamen of the index segment. Next, a tubular retractor (METRx Tubes, Medtronic) was placed through this retropleural corridor using fluoroscopic control (Fig. 1b). The tubular retractor was placed over the disc and the neuroforamen (Fig. 1b, Fig. 2a, b). This approach allows for the microsurgical exploration and removal of the disc herniation whilst providing an excellent view of the disc and the neural structures from an anterior-lateral view (Fig. 2c, d). Following the removal of the disc herniation and meticulous hemostasis, the tubular retractor was removed without the necessity for another apnoe episode and the skin was closed in a layering fashion, with dermabond skin glue applied for external closure (Fig. 2e) (surgical steps: Fig. 2, Table 1).
Fig. 1.
Schematic illustration of partial resection of the lower rib (a) and positioning of the tubular retractor (b) for the retropleural, retractor-assisted approach to thoracic disc herniations
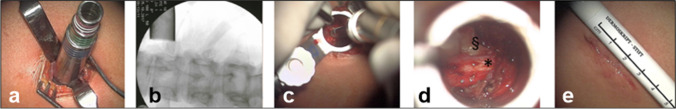
Fig. 2.
Insertion of the tubular retractor (a) with the aid of intraoperative fluoroscopy at the level Th 10/11 (b) and drilling of the head of the rib and posterior lateral part of the disc (c) allows removal of the disc herniation with optimal anterior/lateral exposure of the disc space (d,§) and dura (d,*). (e) illustrates the wound after closure
Table 1.
The nine surgical steps of the minimally invasive tubular retractor–assisted retropleural approach for the thorough exploration and removal of thoracic disc herniations from an anterior-lateral direction
| Surgical step | Description |
|---|---|
| 1. Patient positioning | The patient is positioned laterally, with the affected side facing up |
| 2. Index localization | Localization of the index level is performed using fluoroscopic control |
| 3. Skin incision | A skin incision measuring approximately 3 cm is applied at approximately 12 cm paramedian |
| 4. Partial rib resection | The caudal rib of the index segment is resected using a diamond drill. (Fig. 1a) Beforehand, fluoroscopic control confirms the right level |
| 5. Retropleural dissection | Retropleural dissection and exposure of the ipsilateral head of the caudal rib and the neuroforamen is performed |
| 6. Tubular retractor insertion | The tubular retractor is inserted and positioned through the site of the partially resected lower rib using fluoroscopic control and is placed over the disc and neuroforamen during a short apnea and deflation of the ipsilateral lung. (Fig. 1b, Fig. 2a,b) |
| 7. Exposure | Excellent exposure of the disc and neural structures is achieved from an anterior-lateral direction. (Fig. 2) |
| 8. Exploration and Removal | The disc herniation can be thoroughly explored and removed from anterior-laterally |
| 9. Closure | Following thorough hemostasis, wound closure is performed in a layering fashion with the skin closed using Dermabond® skin glue |
Case series
Between 2017 and 2020, six patients were surgically treated with symptomatic one-level thoracic disc herniations using the minimally invasive tubular retractor–assisted retropleural approach. All patients suffered from a symptomatic uni-level thoracic disc herniation at the mid- to lower thoracic level (Th6/7—Th10/11) which was lateralized and at least partially calcified. One patient suffered from a recurrent thoracic disc herniation and was previously surgically treated via posterior laminotomy. All patients suffered from lateralized radicular pain and 4/6 patients from neurological deficits. In most patients, symptoms persisted for more than 1 month (detailed data on epidemiology and clinical presentation: Table 2). The median duration of surgery was 159 (58–211) minutes. Perioperative blood loss was minimal and transfusion was not necessary (surgical data: Table 3). One patient suffered from an intraoperative dural injury which was fixed intraoperatively with primary dural suture, but was associated with the necessity of a lumbar drainage for four consecutive days to prevent dural fistula. Another patient suffered a postoperative pneumothorax with the necessity of a temporary chest tube which could be removed without complications within 3 days following surgery. Other common postoperative complications like surgical site infections or hematomas did not occur. Two patients complained of slight postoperative thoracalgia and skin irritation on the side of the approach, decreasing over the first postoperative days. Neurological deterioration did not occur and postoperative pain was improved. Postoperative MRI or CT was routinely performed to confirm the near total removal of the thoracic disc herniation, defined as no residual spinal canal stenosis or nerve root compression in postoperative imaging (example: Fig. 3). No neurological deterioration and no recurrent disc herniation occurred at a median follow-up of 3 months (detailed data on postoperative course and follow-up: Table 3).
Table 2.
Epidemiological and clinical data of the enrolled patients
| Patient No | Age (years) | Sex | BMI (kg/m2) | Level of disc herniation | Calcified | Lateralized | Previous surgery | Radicular pain | Neurological deficits | Acuteness of symptoms | Preoperative neurological scoring |
|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 40 | F | 24 | Th 10/11 | Yes | Left | No | Yes | None | Non-acute | AIS E, mJOA 18 |
| 2 | 55 | F | 25 | Th 7/8 | Yes | Left | No | Yes | None | Non-acute | AIS E, mJOA 18 |
| 3 | 52 | M | 33 | Th 6/7 | Yes | Left | Yes | Yes | Ataxia | Non-acute | AIS D, mJOA 15 |
| 4 | 60 | F | 23 | Th 9/10 | Yes | Left | No | Yes | Ataxia | Non-acute | AIS D, mJOA 15 |
| 5 | 31 | M | 23 | Th 7/8 | Yes | Left | No | Yes | Hypesthesia | Acute | AIS E, mJOA 17 |
| 6 | 54 | F | 36 | Th 10/11 | Yes | Right | No | Yes | Dysesthesia | Non-acute | AIS E, mJOA 18 |
AIS, ASIA (American Spinal Injury Association) Impairment Scale; BMI, body mass index; F, female; M, male; mJOA, modified Japanese Orthopedic Association score; Th, thoracic vertebra
Table 3.
Surgical and outcome data of the enrolled patients
| Patient No | Duration of surgery (min) | Blood transfusion | Perioperative complications | Chest tube (duration) | Clinical deterioration | Postoperative MRI/CT | Hospital stay (days) | Postoperative pain | Postoperative neurological scoring | Follow-up (months) |
|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 91 | No | None | No | No | No residuum | 4 | Improved | AIS E, mJOA 18 | 2 |
| 2 | 180 | No | None | No | No | No residuum | 6 | Improved | AIS E, mJOA 18 | 2 |
| 3 | 162 | No | Pneumothorax | Yes (3 days) | No | No residuum | 16 | Improved | AIS E, mJOA 18 | 28 |
| 4 | 58 | No | None | No | No | No residuum | 6 | No pain | AIS D, mJOA 15 | 12 |
| 5 | 155 | No | None | No | No | No residuum | 5 | No pain | AIS E, mJOA 17 | 3 |
| 6 | 211 | No | Dural injury | No | No | No residuum | 12 | Improved | AIS E, mJOA 18 | 1 |
AIS, ASIA (American Spinal Injury Association) Impairment Scale; mJOA, modified Japanese Orthopedic Association score; MRI, magnetic resonance imaging; CT, computed tomography
Fig. 3.
Preoperative (a–d) and postoperative (e–f) MRI of patient No. 5 with a mediolateral left-sided, partially calcified disc herniation at level Th 7/8 causing relevant spinal cord compression, with spinal cord and radicular compression completely removed in (e) and (f)
Discussion
Symptomatic thoracic disc herniations are rare. If symptomatic, a high rate of neurological deficits and progressive myelopathy is common. However, surgery for thoracic disc herniations only makes up for 1–4% of all disc herniation surgeries and is technically challenging and thus associated with a relevant morbidity [3, 4, 6–8, 12]. The anatomy of the thoracic spine hinders an easy access to the anterior-lateral spinal canal, and retraction of the thoracic spinal cord has deleterious consequences [4, 15, 24]. Therefore, access through posterior approaches to thoracic disc herniations remains limited [5, 19]. Traditional anterior approaches like open thoracotomy allow good access to the thoracic anterior-lateral spinal canal [3, 4, 6, 8, 12, 24].
Over the past years, the trend developed towards more minimally invasive surgical approaches using thoracoscopy, which showed a lower complication rate than the before-mentioned more traditional surgical approaches [11, 20, 21]. However, they go with a relevant learning curve of the surgeon. Retropleural approaches to the thoracic spine allow for the shortest way to access the thoracic spinal canal from anterior-laterally, without the necessity for opening the pleural cavity [1, 16]. Combined with endoscopy, they can provide a good access to the spinal canal without the necessity of permanent lung deflation and with a reduced surgery-related morbidity [22, 24]. In a case series of seven patients, a retropleural X-LIF retractor-assisted approach showed feasible without the utilization of neuronavigation or endoscopy, with only minor morbidity [13].
Likewise, the minimally invasive tubular retractor–assisted retropleural approach described in this report allows for a microsurgical retropleural exploration and resection of thoracic disc herniations in a two-center series of six patients. With regard to the most common symptoms of thoracic disc herniations leading to surgical treatment, back and radicular pain did improve and there occurred no neurological deterioration. As surgical complications, a temporary pneumothorax necessitating a postoperative chest tube, and a dural injury necessitating a temporary lumbar drain occurred. Whatsoever, the minimally invasive retropleural exploration with this approach might lower the risk for pleural injury when compared to open approaches.
To ameliorate the safety and feasibility of the described tubular retractor–assisted retropleural approach, the combination with advanced intraoperative state-of-the-art imaging like intraoperative CT, Cone Beam CT (CBCT) or robotic CBCT combined with neuronavigation could prove beneficial in the future [10, 14, 18]. Thus, a safer identification of the anatomical structures could be possible, and the safety of the retropleural preparation might be ameliorated through real-time-control of the right surgical canal. Moreover, the intraoperative assessment of a relevant residual calcified disc herniation following resection is possible with intraoperative CT or CBCT imaging.
The retropleural approach described in this series showed feasible even without the usage of neuronavigation and intraoperative CT imaging. Thus, the approach is not only limited to centres with available intraoperative navigation or advanced intraoperative imaging systems and can be performed broadly with the usage of fluorescence imaging. In summary, a good microsurgical exposure of the disc and neural structures can be achieved minimally invasively from an anterior-lateral direction without the need for an open thoracotomy and permanent lung deflation.
Conclusion
Using the tubular retractor–assisted retropleural approach, a good microsurgical exposure of the disc and neural structures can be achieved from an anterior-lateral direction without the need for open thoracotomy and permanent lung deflation. In the six treated patients in this case series, control-imaging showed the disc herniation to be removed near complete in all cases without relevant residuum and without residual compression of the neural structures.
Abbreviations
- AIS
ASIA Impairment Scale
- ASIA
American Spinal Injury Association
- BMI
Body mass index
- CBCT
Cone beam computed tomography
- CT
Computed tomography
- Hb
Hemoglobin
- Hct
Hematocrit
- ICU
Intensive care unit
- mJOA
Modified Japanese Orthopedic Association score
- MRI
Magnetic resonance imaging
- Th
Thoracic vertebra
- X-LIF
Extreme lateral interbody fusion
Author contribution
JW and VH designed the study concept. VH, PS, FM, JO, UCS, NH MC, PV and JW participated in data acquisition. VH and JW performed data analysis and wrote the manuscript. MC, NH and PV revised the manuscript and contributed to data analysis.
Funding
Open Access funding enabled and organized by Projekt DEAL.
Data availability
Supporting data is available from the corresponding author upon reasonable request.
Declarations
Ethics approval
The study was approved by the ethics committee of the Charité-Universitätsmedizin Berlin, Germany (EA4/064/20).
Competing interests
No competing interests exist in the submission of the manuscript and the manuscript is approved by all authors for publication. No special funding was received for this study. VH ist funded by the BIH Charité Clinician Scientist program. NH is Berlin Institute of Health (BIH) clinical fellow, funded by Stiftung Charité.
Footnotes
This article is part of the Topical Collection on Spine degenerative
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Angevin P, McCormick P. Retropleural thoracotomy. Technical note. Neurosurg Focus. 2001 doi: 10.3171/FOC.2001.10.1.9. [DOI] [PubMed] [Google Scholar]
- 2.Arts M, Bartels R. Anterior or posterior approach of thoracic disc herniation? A comparative cohort of mini-transthoracic versus transpedicular discectomies. Spine J. 2014;14(8):1654–1662. doi: 10.1016/j.spinee.2013.09.053. [DOI] [PubMed] [Google Scholar]
- 3.Ayhan S, Nelson C, Gok B, Petteys RJ, Wolinsky JP, Witham TF, Bydon A, Gokaslan ZL, Sciubba DM. Transthoracic surgical treatment for centrally located thoracic disc herniations presenting with myelopathy: a 5-year institutional experience. J Spinal Disord Tech. 2010;23(2):79–88. doi: 10.1097/BSD.0b013e318198cd4d. [DOI] [PubMed] [Google Scholar]
- 4.Bilsky MH. Transpedicular approach for thoracic disc herniations. Neurosurg Focus. 2000 doi: 10.3171/foc.2000.9.4.4. [DOI] [PubMed] [Google Scholar]
- 5.Börm W, Bäzner U, König RW, Kretschmer T, Antoniadis G, Kandenwein J. Surgical treatment of thoracic disc herniations via tailored posterior approaches. Eur Spine J. 2011;20(10):1684–1690. doi: 10.1007/s00586-011-1821-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Bouthors C, Benzakour A, Court C. Surgical treatment of thoracic disc herniation: an overview. Int Orthop. 2019 doi: 10.1007/S00264-018-4224-0. [DOI] [PubMed] [Google Scholar]
- 7.Chen TC. Surgical outcome for thoracic disc surgery in the postlaminectomy era. Neurosurg Focus. 2000 doi: 10.3171/foc.2000.9.4.12. [DOI] [PubMed] [Google Scholar]
- 8.Court C, Mansour E, Bouthors C. Thoracic disc herniation: surgical treatment. Orthop Traumatol Surg Res. 2018;104(1):S31–S40. doi: 10.1016/j.otsr.2017.04.022. [DOI] [PubMed] [Google Scholar]
- 9.Dimopoulos MA, Gay F, Schjesvold F, et al. Oral ixazomib maintenance following autologous stem cell transplantation (TOURMALINE-MM3): a double-blind, randomised, placebo-controlled phase 3 trial. Lancet. 2019;393(10168):253–264. doi: 10.1016/S0140-6736(18)33003-4. [DOI] [PubMed] [Google Scholar]
- 10.Hecht N, Kamphuis M, Czabanka M, Hamm B, König S, Woitzik J, Synowitz M, Vajkoczy P. Accuracy and workflow of navigated spinal instrumentation with the mobile AIRO® CT scanner. Eur Spine J. 2016 doi: 10.1007/s00586-015-3814-4. [DOI] [PubMed] [Google Scholar]
- 11.Johnson JP, Filler AG, Mc Bride DQ (2000) Endoscopic thoracic discectomy. Neurosurg Focus 9(4):e11 [PubMed]
- 12.Kapoor S, Amarouche M, Al-obeidi F, U-King-im JM, Thomas N, Bell D. Giant thoracic discs: treatment, outcome, and follow-up of 33 patients in a single centre. Eur Spine J. 2018;27(7):1555–1566. doi: 10.1007/s00586-017-5192-6. [DOI] [PubMed] [Google Scholar]
- 13.Kasliwal M, Deutsch H. Minimally invasive retropleural approach for central thoracic disc herniation. Minim Invasive Neurosurg. 2011;54(4):167–171. doi: 10.1055/s-0031-1284400. [DOI] [PubMed] [Google Scholar]
- 14.Kendlbacher P, Tkatschenko D, Czabanka M, Bayerl S, Bohner G, Woitzik J, Vajkoczy P, Hecht N. Workflow and performance of intraoperative CT, cone-beam CT, and robotic cone-beam CT for spinal navigation in 503 consecutive patients. Neurosurg Focus. 2022 doi: 10.3171/2021.10.FOCUS21467. [DOI] [PubMed] [Google Scholar]
- 15.Logue V. Thoracic intervertebral disc prolapse with spinal cord compression. J Neurol Neurosurg Psychiatry. 1952;15(4):227. doi: 10.1136/jnnp.15.4.227. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.McCormick PC. Retropleural approach to the thoracic and thoracolumbar spine. Neurosurgery. 1995;37(5):908–914. doi: 10.1227/00006123-199511000-00009. [DOI] [PubMed] [Google Scholar]
- 17.Nacar OA, Ulu MO, Pekmezci M, Deviren V. Surgical treatment of thoracic disc disease via minimally invasive lateral transthoracic trans/retropleural approach: analysis of 33 patients. Neurosurg Rev. 2013;36(3):455–465. doi: 10.1007/s10143-013-0461-2. [DOI] [PubMed] [Google Scholar]
- 18.Tkatschenko D, Kendlbacher P, Czabanka M, Bohner G, Vajkoczy P, Hecht N. Navigated percutaneous versus open pedicle screw implantation using intraoperative CT and robotic cone-beam CT imaging. Eur Spine J. 2020 doi: 10.1007/s00586-019-06242-4. [DOI] [PubMed] [Google Scholar]
- 19.Vanichkachorn J, Vaccaro A. Thoracic disk disease: diagnosis and treatment. J Am Acad Orthop Surg. 2000;8(3):159–169. doi: 10.5435/00124635-200005000-00003. [DOI] [PubMed] [Google Scholar]
- 20.Vollmer D, Simmons N. Transthoracic approaches to thoracic disc herniations. Neurosurg Focus. 2000 doi: 10.3171/FOC.2000.9.4.8. [DOI] [PubMed] [Google Scholar]
- 21.Wait S, Fox D, Kenny K, Dickman C. Thoracoscopic resection of symptomatic herniated thoracic discs: clinical results in 121 patients. Spine (Phila Pa 1976) 2012;37(1):35–40. doi: 10.1097/BRS.0b013e3182147b68. [DOI] [PubMed] [Google Scholar]
- 22.Yanni DS, Connery C, Perin NI. Video-assisted thoracoscopic surgery combined with a tubular retractor system for minimally invasive thoracic discectomy. Neurosurgery. 2011;68(SUPPL. 1):138–143. doi: 10.1227/NEU.0b013e318209348c. [DOI] [PubMed] [Google Scholar]
- 23.Yoon WW, Koch J. Herniated discs: when is surgery necessary? EFORT Open Rev. 2021;6(6):526–530. doi: 10.1302/2058-5241.6.210020. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Yoshihara H. Surgical treatment for thoracic disc herniation: an update. Spine (Phila Pa 1976) 2014 doi: 10.1097/BRS.0000000000000171. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
Supporting data is available from the corresponding author upon reasonable request.